There is a deepening crisis in America's hospital emergency rooms. More and more patients are showing up for care without the ability to pay for it. The burden on taxpayers and private insurance policy holders is increasing, and doctors and nurses are often overworked while operating in an environment of complex and confusing overregulation, increased litigation, and rising costs.
Moreover, the main federal law that governs the provision of emergency medicine is outdated and counterproductive. It undermines the provision of efficient medical care for all patients, especially for those who are uninsured or underinsured—the very group the law was meant to protect.
The problems confronting the nation's emergency medical system are likely to get worse, especially considering the gravity of the challenges, most notably the threat of a pandemic or a major terrorist attack using biological or nuclear weapons. America's emergency medical system is not prepared for such a disaster.
Current Law
The Emergency Medical Treatment and Active Labor Act (EMTALA)[1] is another example of federal legislation that hurts the very people that it was meant to protect: low-income patients in need of emergency medical services. Enacted in 1986, the law is a congressional response to well-publicized cases in which patients were refused immediate medical treatment based on their inability to pay.
However, EMTALA does not even begin to address the underlying causes of the problem, such as the lack of affordable health insurance and the substandard performance of Medicaid as a health care delivery program for the poor and the indigent. Even after several rounds of additional regulation and clarification, EMTALA remains a poorly understood, inconsistently enforced, unfunded mandate. Worse, the law itself is a major barrier to timely and appropriate emergency medical care.
Policymakers need to undertake urgent reform of the emergency medical system, especially in the face of an increasing need for disaster preparedness.
A Better Policy
For a variety of reasons, the outright repeal of EMTALA is highly unlikely. Nonetheless, federal and state policymakers can mitigate the law's deficiencies and transcend the problems that it was originally designed to resolve.
For example, Congress can diminish the adverse effects on doctors and other medical professionals by providing relief from medical malpractice lawsuits for those who deliver medical care in hospital emergency departments. Congress could also target a portion of Medicare funds to emergency departments to ease the pressures confronting emergency personnel.
More promising than these short-term fixes, however, would be a serious effort to reduce the number of Americans without health insurance coverage. One way to do this would be for state and federal officials to take the funds for existing public subsidies to hospitals and other public facilities that offset the costs of uncompensated care and redirect those funds into a pool to provide health care vouchers or "premium assistance" for low-income families to secure private health insurance coverage. This innovative approach, originally developed by analysts at the National Center for Policy Analysis, could significantly reduce the reliance of so many Americans on the nation's already overcrowded emergency rooms for primary care. A variant of this approach was incorporated into the 2006 Massachusetts health care reform.
Policymakers can stop the continued erosion of quality care in the nation's emergency departments (EDs) and reverse the adverse effects of two decades of ineffective law and misguided regulation on the provision of emergency medical services.
How Congress Regulates Emergency Rooms
American hospitals traditionally have included charity care as part of their mission. In the mid-19th century, only the truly indigent would enter hospitals voluntarily. By the early 20th century, nonprofit and voluntary hospitals became more dependent on patient fees and began to compete for paying patients.[2] With this change in health care financing came the phenomenon of "patient dumping," the practice of transferring non-paying patients from private and nonprofit hospitals to public hospitals before they were adequately stabilized or treated.
The Hill–Burton Hospital Survey and Construction Act of 1946 was an early but largely ineffective attempt to prevent patient dumping. The law required hospitals, as a condition of receiving government funds for construction or modernization, to provide emergency services to all patients, regardless of their ability to pay.
Initially, hospitals could rely on internal subsidization, using surpluses obtained from affluent patients (as well as philanthropic contributions and government subsidies) to offset the costs of services for which they were not paid. However, further changes in health care financing in the 1980s, such as the Medicare diagnosis-related group (DRG)[3] prospective payment system and the rise of managed care, severely limited hospitals' ability to generate the surpluses needed for cross-subsidization. Predictably, this gave hospitals greater incentive to avoid non-paying patients and resulted in a sudden and dramatic increase in reports of inappropriate transfers.[4] Growing public awareness of these cases led to increased pressure to address the problem, and Congress responded with EMTALA, an amendment to the Consolidated Omnibus Budget Reconciliation Act (COBRA) of 1985.
As a condition of participating in the Medicare program, hospitals with designated EDs must initially screen all patients who present themselves to the ED. If an emergency condition is found, the patient must be treated or stabilized before being transferred to another institution. Hospitals and individual providers that violate this law can face severe financial and professional penalties. Application of the statute depends on a hospital's participation in Medicare, but its protection extends to all persons presenting themselves to the ED of a Medicare-funded hospital.[5]
In this way, EMTALA provided a politically expedient response to patient dumping. However, it failed to address the underlying causes of the problem— especially the increase in the number of uninsured patients and growing financial pressures on hospitals.
Metastasizing Regulation. Even EMTALA's most ardent congressional champions were aware of its limitations. The law did not address the growing financial pressures on hospitals in a changing marketplace. It was not a cure-all, but a "modest policy," and most policymakers recognized that further measures would likely be needed.[6]
The legislation was also frustratingly vague, and a number of key elements were poorly defined, such as the meaning of "emergency condition," what constitutes an "emergency department," whether "off-campus" facilities need to comply, and the requirements to provide on-call emergency specialty services. Moreover, EMTALA makes no provision for compensating hospitals or individual providers for the "free" care effectively mandated by Congress.
This statutory ambiguity fueled further regulation. New federal rules and regulations were crafted in an attempt to make EMTALA better understood among medical professionals and easier to implement for hospital officials. In 1994, the U.S. Department of Health and Human Services (HHS) issued supplementary regulations explaining the Medicare agreement in more detail and defining terms such as "emergency medical condition" and "appropriate transfer."[7]
In 1998, federal officials added interpretive guidelines to detail the administrative requirements for compliance with the law and to address the dilemma that hospitals face when treating managed care patients in the emergency room. For example, managed care organizations can retrospectively deny payment for services to patients that they deem "medically unnecessary," and they often require "pre-authorization" for medical services that they do cover. This creates a classic bureaucratic conundrum for the emergency department staff. Delaying an evaluation or treatment to verify that the medical services are authorized by a managed care organization could result in an EMTALA violation.[8]
In 2003, the Centers for Medicare and Medicaid Services (CMS) issued its "final rule" regarding policy clarifications of EMTALA. This set of clarifications defined "dedicated emergency department" and further refined the requirement that hospitals have written policies regarding the provision of emergency services. The rule also attempted to clarify the responsibilities of on-call medical specialists.[9] In spite of these administrative clarifications, EMTALA remains poorly understood and unevenly enforced.
How Washington Enforces EMTALA
It should not be surprising that a hastily enacted law would fail to address the root cause of the problem and create even more difficulties than it was designed to eliminate. EMTALA is a federal statute that attempts to deal with a complex problem that varies greatly in magnitude among states and communities. The federal EMTALA mandate was never meant to supersede state laws and regulations focused on eliminating or reducing the provision of substandard medical care. However, the federal law and its subsequent regulations added yet another layer of complexity to the problem without yielding a stronger benefit in terms of better enforcement or deterrence of undesirable behavior by doctors and hospitals.
Enforcement of EMTALA regulations can be both protracted and complicated, involving state regulatory bodies, CMS regional offices, HHS, the HHS Office of Inspector General (OIG), the Office of Civil Rights, and local peer review organizations. The process is routinely compromised by extensive delays, inadequate feedback, wide regional and year-to-year variations in investigation results and disposition of cases, and numerous errors and omissions in tracking violations. Whereas state agencies can investigate and resolve cases in 15–20 days on average, regional CMS offices regularly take 65 days or longer to complete the process.[10]
A descriptive CMS study of EMTALA citations issued in 2000 showcased several important findings:
- Refusals to screen patients still occur in spite of the federal regulation,
- A majority of citations did not contain evidence of deliberate denial of care, and
- A small but increasing number of cases involved problems in providing on-call specialist services.[11]
Congress responded to these deficiencies in the standard fashion: by adding yet another layer of bureaucratic complexity to the system. As part of the Medicare Modernization Act (MMA) of 2003— the law expanding the Medicare entitlement and creating the Part D drug program—Congress established the EMTALA Technical Advisory Group (TAG) to advise CMS on EMTALA-related issues, including implementation, enforcement, reimbursement, and liability.[12] At its most recent meeting, the TAG reported 774 EMTALA complaints for 2006 nationwide, with wide geographic variation and only a 38 percent substantiation rate overall.[13]
How Current Law Affects Patients
The Institute of Medicine (IOM) recently issued a major report that details the deficiencies of America's emergency medical system, not only on a day-to-day basis, but also in the ability to meet specialized demands for medical care under critical conditions. In other words, the system lacks surge capacity.[14]
Not surprisingly, EMTALA is one of the factors contributing to the erosion of doctors' and hospitals' ability to provide timely access to emergency care to both paying and non-paying patients. Because it is an unfunded federal mandate, the provisions governing EMTALA-related care have been predicated on the ability of providers to cross-subsidize care for the uninsured through revenues from other payers and revenue sources. However, research demonstrates that funding EMTALA through internal cost-shifting is an increasingly bankrupt financing strategy. Emergency departments face growing economic pressure because of a relative decline in overall reimbursement. The reasons for the financial instability of EDs extend beyond the delivery of uncompensated care to the uninsured and include other factors that aggravate the problem, such as inadequate Medicaid reimbursement and the reduction or denial of payment by private insurers.[15]
These financial pressures on hospital EDs coincide with several other statistical trends that have ominous implications for patient access to emergency care. From 1994 through 2004, the number of ED visits increased 18 percent from 93.4 million to 110.2 million visits annually. This is an average increase of more than 1.5 million visits per year spread over all age groups.[16] During roughly the same period, the United States also experienced a net loss of 703 hospitals, 198,000 hospital beds, and 425 EDs, mainly in response to rising costs of care and lower reimbursements by managed care organizations and other payers, including Medicare and Medicaid. (See Chart 1.)
There is also convincing evidence that hospital restructuring in response to financial pressures has been a major contributor to ED overcrowding.[17] The diminished capacity of inpatient and specialty units is especially worrisome because this is the reason most often given for ambulance diversions and patient boarding, the practice of caring for admitted patients in the ED until an inpatient bed becomes available. In a 2006 American Hospital Association survey of hospital chief executive officers, 50 percent of responders reported the perception that their EDs were at or over operating capacity.[18]
The problem is more prominent at urban hospitals (68 percent) and most acute at teaching hospitals (75 percent). These hospitals also report a higher rate of ambulance diversion and patient boarding. In EDs that are at or over capacity, the wait times for patients to be seen are roughly twice the wait times in EDs that are not at capacity.[19] In addition, hospital total operating and patient care margins showed significant declines in 2004 compared to 1997—the year when Congress enacted the Balanced Budget Act and made major changes in Medicare reimbursement—limiting hospitals' ability to cross-subsidize less profitable activities.[20]
Because low-income patients are more likely to lack access to regular primary care and preventive services, they tend to interact with the health care system when they are sicker and are often cared for in the ED. Results from an Emergency Medicine Patients' Access to Healthcare (EMPATH) study suggest that economic barriers to health care access disproportionately affect minority patients and increase their reliance on the ED for care.[21]
The ED visit rate for the uninsured is significantly higher than the rate for those with private insurance, and public programs place even more of a burden on emergency rooms. In fact, Medicaid/ State Children's Health Insurance Program (SCHIP) enrollees use the ED at twice the rate of the uninsured and five times the rate of persons with private insurance and are much more likely to visit the ED for non-urgent and semi-urgent problems[22] than are persons in other payer groups, including the uninsured.[23]
How Current Law Affects Doctors Providing Emergency Care
Although the direct effect on individual doctors is difficult to quantify, EMTALA affects both emergency physicians and on-call specialists. According to the American Medical Association's 2001 Patient Care Physician Survey:
- More than 95 percent of emergency department physicians and more than 30 percent of physicians overall provide care covered by EMTALA in a typical week of practice.
- On average, emergency medicine physicians provide 22.9 hours and surgeons provide 9.7 hours of EMTALA-mandated care per week.
- Among self-employed physicians, 42 percent reported that a significant portion of their bad debt was attributable to EMTALA-related services, accounting for 13.7 percent of all bad debt. This amounts to an estimated $12,300 per provider and an aggregate $4.2 billion annually.[24]
EMTALA provisions have also been cited as a major reason for the lack of availability of medical specialists to provide on-call emergency services. In a 2004 survey of ED directors conducted by the American College of Emergency Physicians, 65.9 percent reported a problem with inadequate on-call specialist coverage. Uncompensated care was reported as the most common reason for the problem, and EMTALA was listed as one of the most frequent concerns.[25]
Costs of the Uninsured. A lack of easy access to primary care, especially among the uninsured and underinsured, contributes significantly to the crisis in emergency medicine, specifically in terms of overcrowding and inappropriate and inefficient use of resources. Estimating the financial costs of providing non-emergent care in the ED is difficult, largely because of disagreement among patients, physicians, and payers about the "prudent definition" of an emergent medical condition.
Perhaps the most important standard for evaluating the appropriateness of ED use is patients' own views of the severity of their medical conditions. Even when viewed from the patients' perspective, a significant portion of ED use is clearly inappropriate. For example, many patients simply prefer the ED to other primary care venues or are unaware of the availability of alternative after-hours care.[26]
In a study that questioned patients waiting to be seen in the ED, one-third of patients considered their problems of no or only minor seriousness. More than one-third expressed a willingness to wait one day to three days for a clinic appointment.[27] However, once these patients arrive at the ED, they must at the very least be evaluated, according to the EMTALA mandate.
Future Disasters. In addition, EMTALA complicates the growing need of the emergency medical system to prepare for a medical disaster, whether natural or manmade, such as a terrorist attack. Disaster response will require rapid and efficient triage, transport, evaluation, and treatment of large numbers of patients. In those circumstances, current law is not helpful, and many policymakers agree that EMTALA regulations would need to be suspended during such a disaster.[28]
What Policymakers Should Do
According to surveys on the subject, the American people are becoming aware of the crisis in the nation's emergency medical system. A majority of Americans favor legislation that would address various facets of the problem.
For example, 62 percent of Americans favor legal protection for physicians who care for uninsured patients in the emergency room, similar to the legal protections given to physicians who treat patients in community health centers. In addition, 71 percent of Americans favor providing additional funding to hospitals to alleviate the problem of patient boarding, and 62 percent favor recognizing emergency care as an essential public service and would support increasing physician and hospital Medicare payments to help to pay for emergency medical services.[29]
On EMTALA itself, there does not appear to be any public support, much less congressional interest, in repealing the law. Appropriately, the public does not endorse denying emergency care to patients because of their financial incapacity to pay for it. Moreover, under traditional medical ethics, physicians must put the welfare of patients first, above all other considerations including financial concerns.
Therefore, the best option, rather than trying to repeal EMTALA, is to transcend it. Specifically, policymakers can mitigate EMTALA's adverse effects in three ways:
- Provide relief from medical liability to physicians who provide emergency care.
Increased liability exposure is one of the most burdensome problems facing emergency physicians and one of the most common reasons why specialists are increasingly unwilling to provide on-call ED coverage. Part of specialists' growing reluctance to take emergency calls is a genuine concern that ED patients will sue. Surveys by the American College of Surgeons and the American Association of Neurological Surgeons/Congress of Neurological Surgeons revealed that more than one-third of respondents had been sued by a patient who was first seen in the hospital ED. A 2005 hospital ED administration survey also lists "malpractice concerns" as a principal factor discouraging specialists from providing ED coverage.
In addition to the effects on access, apprehension about exposure to malpractice appears to affect the quality of medical care. In a 2005 study conducted by Common Good, a bipartisan coalition dedicated to legal reform, 76 percent of doctors said that fear of liability has hurt the quality of their care in recent years, 55 percent of the public said that litigation and doctors' fear of it has hurt the quality of care, and 61 percent of medical students worry that the current liability crisis may hurt the quality of care.[30]
Some specialists tend to view EMTALA as a mandate to provide uncompensated care around the clock, and the law is widely believed to be a primary factor behind practice behavior changes that are taking specialists away from hospitals and EDs. In addition, the American College of Emergency Physicians noted in a recent report that EMTALA may actually encourage uninsured patients to seek ED care in increasing numbers because they are aware of the federal mandate to provide screening and stabilizing care. Furthermore, because liability premiums have outpaced payments for their services, some specialists have concluded that they simply cannot afford the added liability risk involved in providing care that is often uncompensated.[31]
Medical malpractice reform is fundamentally a state issue, not a federal issue, and states can implement a variety of innovative measures to relieve physicians from the burden of unreasonable liability.[32] EMTALA was never meant as a substitute for state medical malpractice laws, and reform attempts should in no way supersede state legislation or a more comprehensive reform of the tort system. However, as a federal mandate, EMTALA has become the government instrument that guarantees uninsured patients the same care in the ED that patients who are fully insured receive, thereby making the provision of emergency medical care in emergency departments a de facto public service. Congress has a responsibility to act quickly to prevent further erosion of the services that EMTALA promises.
Several legislative proposals attempt to address this issue, including the Access to Emergency Medical Services Act of 2005 (H.R. 3875), sponsored by Representative Barton Gordon (D–TN); the Ensuring Access to Emergency Rooms Act of 2005 (H.R. 2729), sponsored by Representative John Shadegg (R–AZ); and the Access to Emergency Medical Services Act of 2006 (S. 2750) sponsored by Senator Jim DeMint (R–SC).
These bills would amend the Public Health Service Act so that hospitals, emergency rooms, physicians, and physician groups that provide emergency care to uninsured individuals would be considered employees of the Public Health Service for purposes of any civil action that may arise due to items and services furnished to those patients. However, they promise only limited relief and may actually conflict with existing state medical malpractice legislation.
- Increase payment for doctors providing emergency care.
While the Medicare physician payment system is profoundly flawed and in desperate need of a thorough overhaul, there is an urgent need to adjust the physician payment system for doctors who provide emergency medical services. H.R. 3875 and S. 2750 suggest funding these payments from the Federal Supplementary Insurance Trust Fund through an amendment to the Medicare legislation (Title XVIII of the Social Security Act).
These bills would increase Medicare payments for physician services provided to a Medicare recipient in the emergency department or critical access hospital to offset the costs of EMTALA-mandated uncompensated care. However, the intended funding for these proposals is not budget-neutral and will only increase the already unsustainable financial burden on the Medicare system unless funds are redirected from sources that are already in the system.[33]
- Redirect existing government funding for uncompensated care from hospitals to patients in the form of health care vouchers or premium assistance programs.
A more comprehensive solution would address the fundamental problem that led to the enactment of EMTALA: the large and growing number of Americans without adequate health insurance. In principle, a program for covering the uninsured would remove incentives for patient dumping, thus making EMTALA irrelevant.
Perhaps the quickest way to accomplish this objective is to redirect existing government funds that offset the costs of uncompensated care in hospitals and other institutions into a pool for direct assistance to individuals and families toward the purchase of private health insurance. This innovative policy was developed initially by health policy analysts at the National Center for Policy Analysis, and a variant of this proposal was successfully advanced by Governor Mitt Romney (R) as part of a comprehensive Massachusetts health care reform signed into law in April 2006. With waivers from HHS, Massachusetts officials are transforming an estimated $1.3 billion in federal and state uncompensated care funds into a premium assistance program for uninsured persons to help them buy health insurance. Eligibility for the Massachusetts premium assistance program broadly tracks the income eligibility for federal individual health care tax credits originally proposed by President George W. Bush.[34]
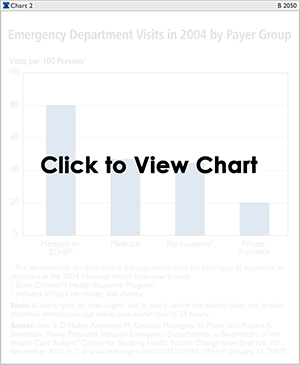
Curiously enough, private insurance seems to perform best in keeping Americans out of the emergency room. Emergency room overcrowding is compounded by the substandard performance of government health care programs. For example, in 2004, the ED visit rate for Medicaid/SCHIP patients (80.3 per 100 persons) was higher than the rates for other payer groups, including Medicare (47.1 per 100 persons); those with no health insurance (44.6 per 100 persons); and those with private health insurance (20.3 per 100 persons). (See Chart 2.)
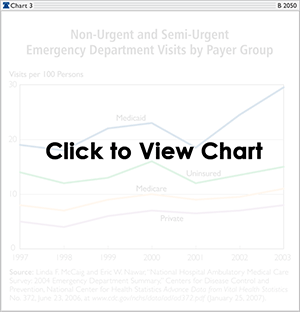
In addition, a greater portion of ED visits by Medicaid/SCHIP patients were classified as non-urgent or semi-urgent (35.7 percent), compared to visits by self-pay patients (23.7 percent).[35] The empirical record indicates that simply expanding Medicaid and SCHIP to the uninsured is unlikely to relieve the growing burden on the emergency medical system. It may even aggravate the problem. (See Chart 3.)
The best avenue for private health insurance expansion would be based on a defined contribution rather than a defined benefit structure, with subsidies to lower-income groups as needed. This would give individuals personal ownership and control of their health care resources, provide an incentive to become more involved in their own medical care decisions, and allow for greater portability of coverage. Under such an arrangement, patients with non-urgent problems would be more likely to seek care in less expensive venues than in hospital EDs.
Conclusion
In passing EMTALA, Congress responded to anecdotal evidence and crafted a politically expedient solution. As an unfunded mandate, EMTALA disproportionately burdens the hospitals and doctors that, as a part of their professional commitment, have traditionally provided most of the health care to patients who are unable to pay. EMTALA is emblematic of the ongoing financial and regulatory burden that is making hospitals and providers less able and increasingly less willing to provide such care.
Turning away bleeding patients and women in labor from hospital emergency rooms is not tolerated in a civilized society. However experience and the accumulation of data on the performance of the law have increasingly exposed the consequences of the existing legislation, and Congress should address them now.
If Americans could own and control their personal health insurance and carry it with them from job to job, uninsurance would rapidly decline, and uncompensated care resulting from uninsurance would be dramatically reduced, making EMTALA largely irrelevant. Assuming that EMTALA remains on the books for the foreseeable future, Congress could make changes in emergency care—by granting limited relief from medical liability and increasing the reimbursement for physicians who perform these services—that would ease the burden on doctors and hospitals that serve patients seeking urgent care under often difficult circumstances. State legislators could also relieve the medical liability of such medical personnel.
Meanwhile, state officials working with the U.S. Department of Health and Human Services could change how public funds are used to care for the uninsured, transforming uncompensated care subsidies to hospitals and other health care facilities into direct assistance to the uninsured that would enable them to buy private coverage that meets their personal needs.
Policymakers could shift health policy to a value-based system that emphasizes personal freedom and expands private health care coverage. Such a system, driven by free-market principles of consumer choice and competition, will yield much better value than one driven by reams of outdated regulation, misguided government subsidies, and the good will of doctors and other medical professionals who provide "free" care in today's professionally discouraging environment.
John S. O'Shea, M.D., is Health Policy Fellow in the Center for Health Policy Studies at The Heritage Foundation.