The recently enacted American Rescue Plan Act (ARPA) spent an estimated $90 billion in subsidizing free health insurance to the unemployed and making some of the nation’s highest-paid workers eligible for government premium assistance.
According to an analysis by the Congressional Budget Office (CBO), this money did little to increase the number of people with coverage. It did, however, increase the amount the government pays to health insurers on behalf of millions of people who already have subsidized coverage. And it induced millions more people who had insurance to shift to government-subsidized coverage.
These provisions are temporary. Some expire later this year, others at the end of 2022. With the American Families Plan (AFP), President Biden has proposed to enlarge the premium assistance program in the Affordable Care Act (ACA) to make bigger payments to insurance companies on behalf of those who already have subsidized coverage. He has also proposed a permanent entitlement to government assistance for everyone, including those in the top two income quintiles.
Congress should not have enacted these temporary expansions. It would be worse to make them permanent. Doing so would do little to increase health insurance coverage. Instead, it would establish an entitlement to premium assistance for the wealthiest households and funnel hundreds of billions of additional taxpayer money to insurance companies on behalf of people who already have coverage. It would also create perverse incentives that could further increase premiums and induce employers to stop sponsoring coverage for their workers.
ACA Premium Subsidies Before ARPA
The ACA created premium subsidies for certain people who did not qualify for employer-sponsored coverage or other federal health care programs. The ACA provided government subsidies only to those with incomes between 100 percent and 400 percent of the federal poverty level (FPL)—that is, $12,880–$51,520 for an individual in 2021.REF
The subsidies limit the amount an individual must pay for premiums for the benchmark plan, which is the second-lowest-cost Silver plan in the region. For example, in 2021, the average premium for benchmark ACA coverage is $452.REF An individual with income at 100 percent of the FPL would pay no more than 2.07 percent of income for this plan. That would mean a $22 per month premium, with the federal government paying the balance of $430 to the individual’s insurance company. An individual with income at 250 percent of the FPL ($32,200) would pay a monthly premium of $224 (8.33 percent of income).
ARPA Temporarily Increased Premium Subsidies
ARPA, enacted in March 2021, temporarily enlarged the ACA premium subsidies in two ways.REF First, it increased subsidy checks sent by the federal government to insurance companies. It did so on behalf of those who already had subsidized coverage (i.e., those with incomes between 100 percent and 400 percent of the FPL). Second, it made people whose earnings exceed 400 percent of the FPL eligible for subsidies. Both expansions expire on December 31, 2022.
Table 1 compares premium subsidies under the ACA and ARPA . The first column presents income categories as a percentage of the FPL. The ACA bars federal premium subsidies to individuals with income below the poverty line, a ban that ARPA retains.REF Before ARPA, an individual with income between 100 percent and 150 percent of the FPL would spend no more than 2.07 percent of income for benchmark coverage. A person with income at 300 percent of the FPL would pay no more than 9.83 percent of that income for benchmark coverage. Those with incomes above 400 percent of the FPL were ineligible for subsidies.
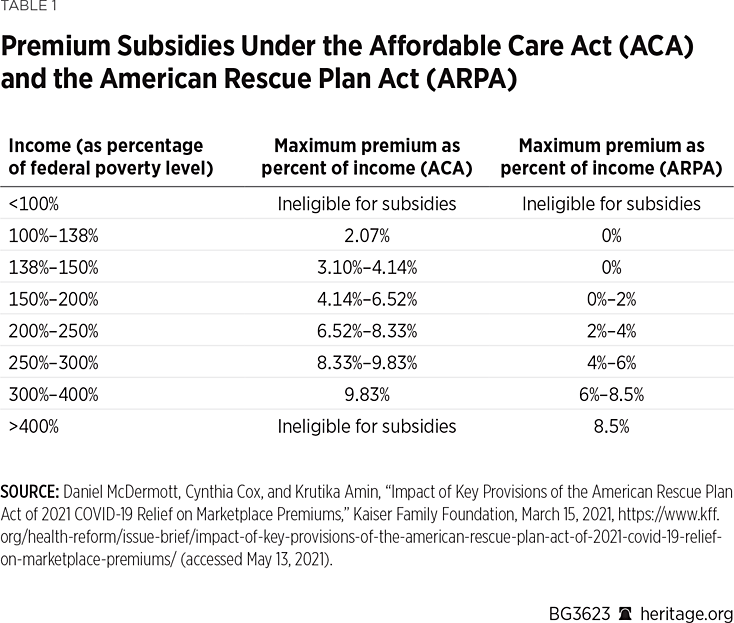
Under ARPA, a person with income between 100 percent and 150 percent of the FPL would get a free benchmark policy, while someone at 300 percent of the FPL would pay no more than 6 percent of income for benchmark coverage. Table 2 compares the premium subsidies for individual health insurance before and after ARPA, using dollar figures rather than percentages of the FPL.

It is important to note that Table 2 presents average premiums for benchmark coverage. Those premiums—and, thus, subsidies—vary geographically. In places where the premium for benchmark coverage is higher, subsidies are higher. The subsidy equals the difference between the benchmark plan premium and a percentage of the beneficiary’s income. For example, under ARPA, an individual with income at 300 percent of the FPL ($38,640) living in an area where the benchmark plan cost $452 would get a monthly subsidy of $194 ($452–$258). The recipient can apply that $194 subsidy to any plan sold on the exchange, including policies that cost less than the benchmark plan.REF
Table 2 also shows that ARPA now provides full subsidies to people with incomes below 150 percent of the FPL ($32,200) who enroll in benchmark plans. Instead of paying $67 per month for benchmark coverage, an individual at 150 percent of the FPL ($19,320) now gets free health insurance. It is free because the government gives more money to the insurance company—in this case, $452 instead of $385.
Thus, one significant effect of ARPA was to enlarge government payments to insurance companies on behalf of people who already have subsidized coverage. Insurance companies, already profiting from tens of billions in federal cash, are the biggest beneficiaries of the temporary increases in those payments.
A second major effect was to make people in the top two income quintiles eligible for subsidized health insurance.REF The ACA did not provide premium assistance to the wealthiest households. ARPA removed the income limit, making 3.5 million people in the top two income quintiles eligible for premium subsidies.REF Of these, 1.1 million have incomes above 600 percent of the FPL (incomes of at least $77,280 for individuals and $159,000 for families of four).REF
The Kaiser Family Foundation report also finds that people in the top two income quintiles derive the highest average subsidies from the expansion, as Chart 1 illustrates.
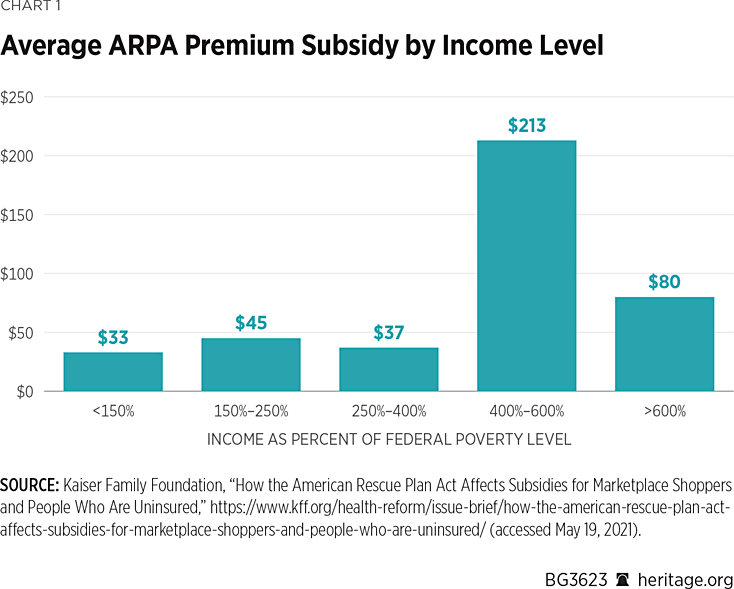
In addition to accounting for 40 percent of new exchange enrollees, people in the top two quintiles collect ARPA’s largest average premium subsidies.REF Those with incomes between 400 percent and 600 percent of the FPL receive average monthly ARPA subsidies of $213, a figure that is nearly seven times as high as the increased subsidy provided by ARPA to those with incomes less than 150 percent of the FPL. The wealthiest recipients—those with incomes exceeding 600 percent of the FPL—get average ARPA subsidies nearly two-and-a-half times as large as the lowest-income recipients.REF
These temporary expansions come at great cost to the federal government. The CBO estimates the combined revenue and outlay effects of the premium subsidies at $34.2 billion, with the bulk of the spending occurring during fiscal year (FY) 2022.REF
Most of that new spending, as noted above, will come in the form of federal payments to insurance companies on behalf of people who already have health insurance. The CBO estimates that the subsidies will cost a total of $21.9 billion in spending and forgone revenues in FY 2022 and cover 1.3 million previously uninsured people.REF That works out to an average of $16,825 per newly insured person.
The AFP Would Make ARPA Subsidy Increases Permanent
The AFP would make the ARPA premium subsidies permanent.REF In a fact sheet advancing the proposal, the Administration makes two dubious claims: that it would reduce the number of uninsured people by 4 million and that it would cost the federal government $200 billion (presumably over 10 years).
The Administration’s estimate of the coverage effect of the AFP is more than three times higher than the CBO’s estimate for ARPA. It seems highly unlikely that permanently extending the ARPA subsidies would reduce the number of uninsured by that amount.
A May 2021 analysis of the Administration’s proposal by the Penn Wharton School Budget Model estimates the 10-year costs of extending the premium subsidy at $378 billion, a figure nearly twice the Administration’s estimate.REF The CBO has not yet estimated the cost or coverage effects of these provisions.
Why Congress Should Not Make the ARPA Subsidy Increases Permanent
Congress should reject the Administration’s proposal to make the ARPA subsidy increases permanent. Here are six reasons why.
1. Costly Solution in Search of a Problem
The pandemic and government policies that shuttered schools, businesses, and churches were widely believed to have massively increased the number of uninsured. A July 2020 Urban Institute report, for example, estimated that 10.1 million people would lose coverage tied to a job and that 3.5 million of them would not find another source of insurance.REF Such forecasts motivated Congress to enact the temporary expansion of premium subsidies in ARPA.
We now know that such forecasts of a surge in uninsurance were erroneous. An analysis by Heritage Foundation experts of administrative data on actual coverage during 2020 found that 5.7 million more people had coverage in December 2020 than in December 2019.REF Net enrollment in private coverage (group and non-group) decreased by 2 million individuals, or 1.2 percent, while enrollment in public coverage (Medicaid and the Children’s Health Insurance Program) increased by 7.8 million individuals, or 10.9 percent.REF Furthermore, the analysis found that enrollment in individual market plans increased by 605,000 individuals (or 4.4 percent)—an increase that occurred before Congress increased ACA premium subsidies.
Thus, the underlying premise of the temporary subsidies was faulty. Congress has committed tens of billions of dollars in unnecessary temporary spending that has done little to increase coverage. It should not double down on its error by making the subsidies permanent.
2. Benefits for the Already Insured
Of the new deficit spending authorized by ARPA, $22.5 billion would go to people already enrolled in marketplace plans.REF The remaining $13 billion would go to new enrollees, many of whom would migrate from some other form of coverage.
For example, a 30-year-old couple with two children and income at 500 percent of the FPL ($132,500) currently buying an unsubsidized insurance policy now qualifies for a subsidy of $4,433.REF Subsidizing the already insured is an inefficient use of federal money.
3. Benefits for the Wealthy
ARPA made the wealthiest people eligible for subsidized coverage and gave them the biggest average benefits.
This temporary provision has disproportionately benefited high-income earners, particularly those in their 50s and 60s. Because ACA premiums vary by age and family composition, middle-aged and older workers qualify for the most significant subsidies, even when their income is quite high.
Under ARPA, a family of four headed by a 45-year-old couple and with income of around $106,000 qualifies for a $10,000 premium subsidy.REF A 60-year-old couple with the same family composition and income receives more than $20,000 in government premium subsidies.REF That couple still gets a $10,000 subsidy if its income rises above $230,000. Even at $318,000 of income, the household would qualify for a subsidy of nearly $1,900.REF
Congress should not have provided subsidies, even temporarily, to the wealthiest households, most of whom already had health insurance.
4. Boon for Insurance Companies
While the government pays subsidies on behalf of people who enroll in exchange-based coverage, the government pays those subsidies to insurance companies. And since subsidies rise dollar for dollar with benchmark premiums, the higher the premiums, the more government money insurers pocket.
It is no coincidence, then, that the ACA touched off an upward spiral in premiums. Nationally, the average premium paid for individual coverage rose by 129 percent—or more than doubled—between 2013 and 2019.REF
Not surprisingly, profits rose with those premiums. Average monthly per-enrollee gross margins for insurers in the individual market was $158 through the first nine months of 2020. That was far higher than the $92 monthly margin insurers made on their group business.REF
Unlike their group business, the lion’s share of insurance company revenue in the exchange-based individual market comes from the government, not enrollees.
Table 3 is based on a Centers for Medicare and Medicaid Services (CMS) analysis of enrollment in exchange-based coverage through the first half of 2020.REF

According to the CMS, more than 10.5 million people had exchange-based coverage during the first half of 2020. Of those, 9.1 million received premium subsidies. Premiums averaged $575, while premium subsidies averaged $491.
Table 3 presents the monthly premium revenue for exchange-based coverage by multiplying the average premium by the number of enrollees. The monthly subsidy revenue is calculated by multiplying the number of subsidy recipients by the average value of the subsidy.
As of June 2020, monthly insurance company revenue from exchange-based coverage averaged $6.1 billion, while monthly government subsidies paid to insurers were just under $4.5 billion. Thus, insurers that sold through the exchanges derived 73.8 percent of their revenue from direct payments from the federal treasury.REF
By increasing subsidies to people who already receive them and extending them to higher-income households, ARPA will increase government payments to certain insurers for certain government-approved products—and so increase the share of revenue those companies derive from those federal payments.
Enriching insurers without substantially increasing coverage is misguided as a temporary expedient. It is even more misguided as permanent law.
5. Inflationary Effect on Premiums
Federal premium subsidies rise dollar for dollar with the price of premiums for benchmark coverage. That likely contributed to the law’s inflationary effects.
The law also dulls consumer price sensitivity by limiting what a subsidized beneficiary pays in premiums for a benchmark policy to a percentage of income. Once that percentage is determined, a consumer has little incentive to worry about a plan’s premium, especially if he or she enrolls in the benchmark plan or one with a lower premium. That is especially true with ARPA, where subsidies equal 100 percent of the premium for a benchmark plan for millions of consumers.
The CMS presents this as a feature, not a bug. Its fact sheet on the ARPA premium subsidies states: “Four out of five enrollees will be able to find a plan for $10 or less/month after premium tax credits, and over 50% will be able to find a Silver plan for $10 or less.” The statement envisions two overlapping groups of people. More than half of those in the second group pay $10 or less for their exchanged-based insurance. That is mainly because those with incomes between 100 percent and 150 percent of the FPL now pay $0 for benchmark coverage. Since people with incomes in the 100 percent to 200 percent of the FPL range are disproportionately represented on the exchanges, it is easy to see how more than half the participants have such low premiums.REF
The reason 80 percent of participants can obtain coverage for less than $10 is that they can apply their subsidies to plans that cost less than the benchmark plan. As discussed above, the subsidy is computed by subtracting the maximum out-of-pocket premium contribution from the benchmark premium. For a person with earnings of 250 percent of the FPL, subtract $107 (4 percent of income) from the cost of the benchmark plan. Assuming the premium for the benchmark plan is at the national average ($452), the subsidy would equal $345 ($452–$107). The premium for the average Bronze plan is $328.REF If the individual chose a Bronze plan, the coverage would be less generous, but the premium would be $0. The value of the subsidy ($345) exceeds the cost of the policy ($328).REF
ARPA’s temporary expanded subsidies thus create perverse incentives for buyers and sellers alike. Many buyers will be less price sensitive, especially those whose subsidies are equal to or close to the benchmark coverage cost. Sellers have incentives to keep benchmark premiums high, as the larger the benchmark premium, the larger the subsidy.REF
Right now, that dynamic is temporary, affecting only bids for the 2022 plan year. If Congress makes the ARPA subsidy structure permanent, however, these inflationary effects would be much more likely.
6. Induces Employers to Drop Coverage
Under the ACA, individuals whose employers offer them health insurance that meets certain federal requirements may not receive subsidized exchange-based coverage.REF This so-called firewall—coupled with the high premiums, high cost-sharing, and narrow networks associated with ACA plans—has helped dissuade firms from dropping their plans. Moreover, employers with at least 50 full-time workers face tax penalties for failing to offer coverage to employees and their children or if the self-only insurance does not meet federal standards of minimum value and affordability.REF
The ARPA subsidies, according to the CBO, did not change this dynamic. In its analysis of the legislation, the CBO wrote that it did not “anticipate that many employers would change their decision to offer health insurance given the temporary nature of the enhanced subsidy.”
Making those subsidies permanent would change the calculus. Once employers know that government will subsidize coverage for workers regardless of their income, they may have fewer inhibitions about dumping their employees into the exchanges, where the government pays a portion of the premiums.
Smaller firms that are exempt from the employer mandate, especially those with older or lower-paid workers, will have strong incentives to discontinue job-based coverage. The ACA made group health insurance more expensive, and the government does not subsidize the premiums.REF Coverage among small firms dropped abruptly with the ACA’s enactment in 2010 and has never recovered. A permanently revamped federal subsidy program might induce firms that have continued to cover their workers to rethink that decision.
In addition to being more costly to the government, such a change would be a bad deal for workers, especially those with average or above average medical expenses. Employer-sponsored coverage is far more generous than ACA coverage, not only in terms of actuarial value but also in establishing broader networks of physicians and other medical providers.
Conclusion
The decision to temporarily increase federal premium subsidies was ill-considered. It was based on the false premise that millions of workers and their dependents had lost coverage due to government lockdowns. It poured almost all resources into subsidizing the premiums of people who already had insurance. It made the nation’s highest earners eligible for government premium assistance. It enlarged federal payments to insurance companies in one of their most profitable lines of business and created perverse incentives to inflate premiums. Making these subsidies permanent not only would double down on these bad policies but could also result in millions of Americans losing their employer-sponsored coverage.
Congress erred in enlarging premium subsidies last March. It should not compound that error by making that expanded subsidy structure permanent.
Doug Badger is Senior Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.


