Overall, the Medicare Advantage program (MA)—a system of competing health plans and the only viable alternative to enrollment in traditional Medicare—has been a success. Enrollment has grown rapidly. It is obviously a program that seniors know and like, and it has long enjoyed strong bipartisan support in both houses of Congress. Nonetheless, it costs more than it should and delivers less than it can.
When MA was created in 2003, private health plan enrollment was 5.3 million beneficiaries—just 13 percent of those covered by Medicare.[REF] Today, 33.6 million beneficiaries are enrolled in private plans—54 percent of the total Medicare population.[REF] The reasons for this phenomenal growth are obvious. Choosing an MA plan is convenient and supremely attractive. Most beneficiaries pay no more than one premium (the standard Medicare Part B premium) for one comprehensive plan, with a rich menu of benefits and, unlike traditional Medicare, the program provides guaranteed protection against the financial devastation of catastrophic illness.
Better Benefits
Virtually all Medicare beneficiaries have access to a private health plan, and nationwide there are literally thousands of options from which to choose, including employer-sponsored MA plans and “special needs plans” for patients suffering from complex medical conditions. In terms of care quality, MA plans focus heavily on preventive care, coordinated care and case management, and perform better than traditional Medicare on a variety of metrics, including fewer hospitalizations, emergency room visits, and complications from diabetes.[REF]
According to a detailed Kaiser Family Foundation analysis, this year 67 percent of MA plans with prescription drug coverage charge no extra premium for that coverage; 32 percent offer reductions in the standard Medicare Part B premium that finances their MA coverage; and 97 percent offer vision, dental, and auditory coverage. Plans also offer a wide range of supplemental health benefits, everything ranging from coverage for common over-the-counter medical products and transportation assistance to fitness programs and in-home support services.[REF] In a large survey, more than nine of 10 beneficiaries said that such supplemental benefits can improve their health and save them money.[REF]
Benefit options have steadily improved in recent years, and premiums have remained relatively stable, guaranteeing senior and disabled citizens access to affordable coverage. The imposition of a cap on prescription out-of-pocket costs, a measure long supported by both liberal and conservative analysts, will also enable patients to secure thousands of dollars in new savings each year.[REF] For taxpayers, spending for coverage for MA enrollees is indeed higher than spending for the coverage of beneficiaries in traditional Medicare, but MA also provides benefits and other advantages that traditional Medicare does not. This difference in government spending, in other words, is not a measure of value.[REF]
Fixable Flaws
Despite its popularity with seniors, Medicare Advantage has serious but fixable flaws; problems resulting directly from policy—not market—failures. For example, MA’s payment system, including its risk-adjustment component, is complex, cumbersome, and excessively costly. The program’s benefit gaps—ranging from restrictions on hospice care to health savings accounts to direct primary care options—make little or no sense. Health plans’ use of prior authorization for medical treatments and procedures is too often excessive, resulting in frustrating delays and even denials of care. Moreover, the Centers for Medicare and Medicaid Services (CMS) does not provide Medicare beneficiaries with clear comparative information on the programs’ performance on quality metrics, or the true costs and benefits of MA versus Medicare Fee for Service (FFS).
Focused on MA’s rising costs, the Biden Administration made several payment and regulatory changes, including a reduction in the 2025 Medicare Advantage benchmark payment well below medical inflation, tougher quality rating standards, and a major reduction in the diagnostic codes for risk-adjusted payments to the plans. Since then, the Trump Administration has stabilized the basic MA rates, following two years of rate payment declines. However, Trump Administration officials are also concerned about rising MA spending and announced that they would annually audit every MA plan to determine whether plans were abusing the risk-adjustment system to secure higher reimbursement, while investigating the practices of United Health Group, one of the largest MA insurers.[REF]
Administrative or regulatory changes, however, are an insufficient response to MA’s fundamental problems. Congressional intervention, ideally with White House support, should improve the program through statutory changes that are necessary and long overdue.
Improving Medicare Advantage: A 14-Step Program
Congress can correct MA’s specific flaws with targeted reforms and build on its best features—consumer choice and market competition—to guarantee a superior Medicare Advantage program for the future. Congress should take 14 specific steps and:
1. Reform the Health Plan Payment System. Today, the federal government pays health plans based on a complex formula combining Medicare’s administrative price setting and a flawed process of county-based competitive bidding among health plans to offer the standard Medicare Part A (hospitalization) and Part B (outpatient services) benefits.[REF] This health plan payment process is complex, inherently costly and unnecessarily cumbersome.
Congress should break the link between MA plan payment and administrative payment in the Medicare FFS program. The right solution is summarized by James Capretta, senior fellow at the American Enterprise Institute (AEI) and a former associate director of the Office of Management and Budget (OMB): “The most effective approach would be to set payments based on bids submitted by the plans rather than administratively set benchmarks which invite political manipulation and abuse.”[REF]
By basing health plan payment on a new system of market-based competitive bidding, lawmakers would harness the great power of the free market forces of supply and demand. Direct market-based bidding among competing health plans to offer the standard Medicare benefits would intensify price competition and reflect the real conditions in the health insurance market. Today, MA plans offer bids to provide standard benefits in Medicare Parts A and B. In a new system, the benefit base for competitive bidding could be expanded to include the standard Medicare Part D drug benefit, thus integrating drug coverage into the payment setting for comprehensive health coverage.
Congress would have to address several key issues. Paramount among them, of course, would be the formula governing the bidding that determines health plan payment. Lawmakers should consider at least three possibilities.
First, Congress could adopt the weighted average plan premium (weighted by plan enrollment) among plans bidding in the competitive area, the basic formula used today to set government payment to competing health plans in the Federal Employees Health Benefit Program (FEHBP) and Medicare Part D. Using the average bid would enable the beneficiaries to directly reap the savings of choosing any plan offering coverage under the plan’s payment. Like today, if an MA plan’s coverage cost more than the government payment, then the plan could charge a premium to compensate for the difference. If the plan’s coverage were to cost less, then the beneficiary should be able to pocket 100 percent of the differential in personal savings, either in tax-free cash or in deposit in a health savings account.[REF]
Second, Congress could consider basing plan payment on the bid of the second lowest-cost health plan in each competitive (county) area, which is the formula used today under the Affordable Care Act (ACA) for paying health plans in the program’s health insurance exchanges. Alternatively, Congress could consider using the average enrollment weighted bid of the three lowest-cost health plans in the competitive area.[REF]
In all three scenarios, MA beneficiaries could enroll, as they do today, in a “zero” premium health plan, meaning no additional payment beyond the standard Part B Medicare premium.
Congress should also redefine the competitive area for an updated bidding process. Today, government payment to MA plans is based on the insurers’ bids offered in more than 3,000 counties throughout the United States. Instead, Congress should authorize competitive bidding on a regional basis, smoothing out the sharp local disparities in providers’ payment while reflecting the fact that modern care delivery is also more regionally based.[REF]
Finally, Congress should provide a transition period in creating a new MA competitive-bidding program. Though strongly supportive of a new bidding system, AEI’s Capretta, as well as Paul Ginsburg and Steven Lieberman, analysts with the Schaeffer Center at the University of Southern California, warn that any precipitous change could prove disruptive to MA enrollees, resulting in less generous benefits in some areas or higher costs in others. Congress can effectively address this problem by phasing in the new system over a period of years with special rules to minimize any disruption.[REF] Three to five years, for example, would be an appropriate transition period.
Meanwhile, the Trump Administration can contribute to this reform effort by requiring the Center for Medicare and Medicaid Innovation (CMMI) to evaluate the effectiveness of the different payment formulas. Assessing these formulas in regional demonstrations would enable policymakers to determine the best option to secure continued patient affordability for coverage while ensuring the stability of the market. Competitive bidding works, and the continuing success of the FEHBP’s six decades of experience is a clear proof of the concept.
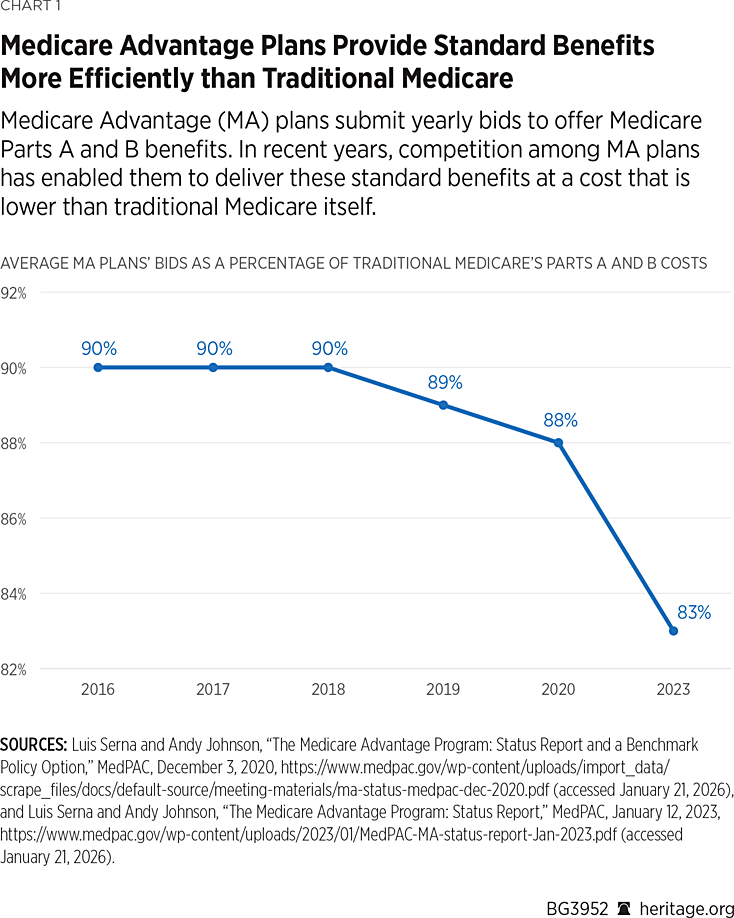
Straight market-based bidding among health plans to set the annual government payment also promises to secure significant savings. The reason: The yearly Medicare Advantage bids to provide traditional Medicare benefits routinely come in well below the cost of traditional Medicare in delivering those benefits, according to the Medicare Payment Advisory Commission (MedPAC), the agency that advises Congress on provider reimbursement. In 2023, for example, the health plans’ bids, on average, were 17 percent below traditional Medicare’s cost.[REF] For 2025, MedPAC reported that almost all MA plan bids came under the traditional Medicare benchmark cost.[REF] In short, MA can and does deliver traditional Medicare benefits cheaper and more efficiently than traditional Medicare itself.
Commenting on this superior performance, Capretta remarked, “If an MA bidding system led to a reduction in payments comparable to a 10 percent cut (which is realistic based on MedPAC’s research), the savings over a decade would be close to $500 billion.”[REF] It is worth noting that former Presidents Bill Clinton and Barack Obama also understood the potential of straight competitive bidding to reduce MA costs and included the reform in their budget proposals in 2000 and 2009, respectively. In fact, when President Obama submitted his 2009 budget proposal, he estimated that his competitive bidding reform would yield savings of $177 billion over 10 years.[REF]
2. Reform the Risk-Adjustment System. In tandem with MA payment reform based on competitive bidding, Congress should improve reimbursement of plans for enrolling sicker beneficiaries with higher-than-average medical needs. As Capretta observes, “The current system has several flaws that might be addressed. But the basic problem is too much reliance on the data submitted by the plans which can lead directly to higher revenue.”[REF]
Today, the government adjusts plan payment to MA plans to account for enrollees’ age, sex, institutional and Medicaid status. For payment setting, for prospectively assessing risks, this demographic set of risk projections works fairly well. The problem arises in determining beneficiaries’ health status. While the current system accounts for health status, it does so prospectively using past claims data. While that approach can produce reasonably accurate cost projections for beneficiaries with well-understood chronic conditions, it cannot predict unexpected costs or sudden changes in a beneficiary’s health status.
The current system also invites what MedPAC officials call “coding intensity”—assigning an excessive number of diagnostic codes to secure higher plan reimbursement. To be clear: MA plans, under law and regulation, are required to use diagnostic codes to identify the medical conditions of their enrollees to estimate “health risk” for plan reimbursement. This is very different from FFS Medicare, where doctors submit diagnostic codes for payment for the provision of a specific medical treatment or procedure. In MA, the more diagnostic codes that plans submit, the higher their reimbursement from the government. In its 2024 report, MedPAC reported that this “coding intensity” plus “favorable selection” (MA’s attraction of younger, healthier enrollees) are the main drivers of higher government payments for MA enrollees.
MA’s “favorable selection” is, once again, a problem rooted in the status quo. Medicare’s administrative payment system requires health plan payment to be based on the “average” FFS cost of Medicare beneficiaries. Assuming that MA beneficiaries are healthier than average, thus costing less, the system automatically pays MA plans more than is warranted. If the government payment reflected the real cost of MA beneficiaries, allegedly healthier than their counterparts in traditional FFS Medicare, then obviously the MA costs would be lower.
It should be noted, however, that the degree of MA’s “favorable selection” is rightly a hot point of contention. The reason: The MA program, heavily populated with lower income beneficiaries, attracts patients with “special needs” (more complex medical conditions) and, in recent years, has enrolled patients with end-stage renal disease (ESRD), a particularly costly sub-group of the Medicare population. Dr. Brian J. Miller of Johns Hopkins University, a member of MedPAC, along with his colleagues, have called attention to these facts, noting also that MA coding requirements have no parallel in FFS Medicare, suggesting the need for a more balanced evaluation of the program.[REF]
Nonetheless, MedPAC concludes that the combination of these two factors—“coding intensity” and “favorable selection” result in MA program costs that are 22 percent higher ($83 billion) than they would have been had these enrollees been confined to traditional Medicare.[REF] Of course, if these beneficiaries were confined to traditional FFS Medicare, they would not have access to the additional benefits that MA plans provide and would be required to buy increasingly expensive supplemental coverage to fill in the crucial gaps in FFS Medicare, including protection from the financial devastation of catastrophic illness.
Beyond the issue of “favorable selection,” the degree of MA plans’ “coding intensity” is also a legitimate point of contention. As The Wall Street Journal observes,
MedPAC claims that seniors in Medicare Advantage are healthier than those in fee-for-service because they incur less spending. Ergo, insurers must be coding them as being sicker than they are. Maybe. But that’s hard to square with the fact that Medicare Advantage enrollees are also more likely to be low income and have poor self-reported health status.[REF]
Lawmakers should also be aware of the recent discrepancy in estimates of the impact of MA “coding intensity” between MedPAC analysts and those with the CMS. Based on 2022 data, MedPAC estimated, after making statutorily required adjustments, that “coding intensity” resulted in MA payments for beneficiaries being 10 percent higher than Medicare, but the CMS analysts, relying on an updated methodology, estimated the differential impact between 1.5 percent and 2 percent.[REF] Such a disparity merits further congressional inquiry.
Looking toward the future, Congress should take the guesswork out of projecting an MA plan’s cost from enrolling sicker patients. There is a much better option: paying plans for the actual costs they incur. Thus, a retrospective (look-back) system would reimburse plans for the actual costs of enrolling a disproportionate number of beneficiaries with higher medical costs. Such reimbursements would come from a common pool, funded by the plans themselves, through which MA plans would share the costs of expensive enrollees. Such retrospective risk-transfer pools should be organized on a state or regional basis, with funding from all participating MA plans, and should be designed and managed by the plans themselves under the direct supervision of state insurance regulators.
Such a retrospective system would not only be more accurate but would also reduce or eliminate the real problem of insurer gaming of the current MA payment system at the expense of the taxpayer. Commenting on this Heritage Foundation proposal, Stanford University’s Alain Enthoven, one of the nation’s top health economists, observed, “In this model, costs would not need to be predicted. The pool payments would be settled after the fact. This would take place under the supervision of state insurance departments, which already have experience with pooling arrangements in different lines of insurance.”[REF]
As with health plan payment formulas, the Trump Administration may wish to conduct a demonstration of such a risk-adjustment reform to ensure that reform would maintain market stability and an equitable distribution of year-end payments to participating plans. A well-designed risk-adjustment system can also secure guaranteed access to affordable coverage for the most medically vulnerable beneficiaries.[REF]
3. Allow MA Medical Savings Account Plans to Offer Drug Coverage. Medical Savings Account (MSA) plans are the closest equivalent to health savings account (HSA) plans in the private sector, and, as a rule, they do not have networks of physicians or hospitals. The plans deposit funds into a beneficiary’s account, and beneficiaries draw upon this account to meet their medical expenses. Congress should allow MSA plans to offer prescription drug coverage just like all other MA plans. Today, they cannot. If a Medicare patient who is enrolled in an MSA plan wants access to drug coverage, that patient must enroll in a separate Medicare Part D drug plan and pay an additional premium. This is an anti-competitive feature of the program, which discourages enrollment in these plans. A level playing field among health plans is essential to secure rational beneficiary choice in a normal, functioning market.[REF]
4. Allow MA to Offer Hospice Coverage. Under current law, beneficiaries in MA plans must secure their hospice benefits under the traditional Medicare program. Congress should eliminate this counterproductive restriction and allow MA beneficiaries to enjoy a full continuum of care, including end-of-life care if needed, through their private plans.[REF] There should be no benefit mandate, of course; health plans can and should decide for themselves if they wish to extend palliative care, which many offer today, into hospice coverage for the full continuum of patient care. MA plans should be allowed to offer such coverage, and MA beneficiaries should be permitted to take advantage of this benefit option.
5. Allow Medicare Beneficiaries to Continue to Make Contributions to HSAs. Under current law, Medicare beneficiaries cannot continue to make tax-free contributions to their health savings accounts. Congress should also revisit (and raise) the current HSA contribution limits and consider making these accounts free-standing savings vehicles for medical care, regardless of insurance coverage. Facing much higher per capita health costs than incurred by younger and healthier people, as well as far more complex medical conditions, Medicare patients generally rely on an even greater variety of medical services. They also must rely on a much broader range of medical specialists than the younger working Americans who use HSAs to offset their much lower health care costs.
6. Reform MA Prior Authorization. There is virtually no prior authorization for access to medical services under the traditional Medicare FFS program.[REF] Doctors are reimbursed for providing a covered service, and the perennial problem is that volume increases in the delivery of medical services do not necessarily reflect their value to the patient. Unsurprisingly, the Centers for Medicare and Medicaid Services estimates that in fiscal year 2024 alone, the total cost of improper FFS payments amounted to $31.7 billion.[REF]
The situation is vastly different in Medicare Advantage. Almost all MA enrollees are members of plans that require prior authorizations for medical services, treatments, or procedures, though the extent varies from plan to plan. Focused on 2023 data, Kaiser Family Foundation analysts conducted a comprehensive study of MA prior-authorization practices. They found that in 2023 health plans made almost 50 million such determinations and more than 90 percent of them were positive, meaning that the requests were “fully” favorable.[REF] Only 6.4 percent of requests were “fully or partially” denied, but 81.7 percent of the denied requests for authorization were “partially or fully” overturned on appeal. As the Kaiser analysts observed, however, “These requests represent medical care that was ordered by a health care provider and ultimately deemed necessary but was potentially delayed because of the additional step of appealing the initial prior authorization decision. Such delays may have negative effects on a person’s health.”[REF]
For doctors and their patients, the process itself is often profoundly frustrating, aggravated by outdated paperwork and fax communications, that unnecessarily contribute to care and payment delays.
To its credit, the Trump Administration has already taken steps to address the problem. During his Senate confirmation hearing, CMS Administrator Dr. Mehmet Oz (the CMS administers Medicare), said that there should be a regulatory limit on the number of treatments or procedures subject to prior authorization, reducing the total number from 5,500 to 1,000.[REF] In June 2025, Secretary of Health and Human Services (HHS) Robert F. Kennedy, Jr., and Dr. Oz announced a breakthrough agreement with major MA insurers. The insurers pledged to address the problem by, among other things, standardizing electronic submissions and providing “real-time” decisions, reducing the number of prior authorization requests, and ensuring that a medical professional would review any clinical denials.[REF]
These voluntary efforts should be given appropriate time, say, a year, to work. If these administrative and regulatory efforts fail to resolve the problem of excessive prior authorization, however, Congress should pursue a bipartisan legislative remedy. Senator Roger Marshall (R–TN) and Representative Ami Bera (D–CA) have co-sponsored the Improving Seniors’ Timely Access to Care Act (S. 1816/H.R. 3514) that would, among other things, require MA plans to adopt an expedited process of electronic prior authorization; expedite determination for routine items and services in real time; and provide full transparency of MA plan justifications for their decisions.
Given the determination of the Trump Administration to resolve the problem plus the fact that the Marshall–Bera legislation has already attracted strong bipartisan support in Congress, doctors and patients are likely, one way or another, to secure significant relief.
7. Allow MA Plans to Fund Direct Primary Care Through a Roth HSA. Today seniors’ Medicare premiums and out-of-pocket payments are made with after-tax dollars, but Medicare benefits are untaxed. Congress could allow MA plans to make after-tax deposits into a beneficiary’s Roth-style HSA, as John Goodman suggests,[REF] and these funds would be untaxed when withdrawn. While some direct primary care (DPC) doctors do not accept third-party payment (including Medicare), Medicare beneficiaries with a Roth HSA should be able to use those funds to engage both non-Medicare doctors and Medicare doctors. By depositing funds into a Roth HSA, they would be allowing patients to directly manage their primary care. This flexibility would enable patients to use emerging and innovative primary care services, including telehealth, fostering better and more cost-effective care.[REF]
8. Create a “Cash and Counseling” Option for Chronically Ill or Disabled Seniors. Like the successful “cash and counseling” programs for low-income disabled persons in Medicaid, Congress could create a “cash and counseling” program in Medicare for low-income seniors with physical and mental disabilities. MA plans could deposit funds into a special account that these seniors and their caregivers could use for a wide variety of specialized services that they or their caregiver determine is best for them.[REF]
9.Require Clear Side-by-Side, Direct Out-of-Pocket Cost Comparisons Between Medicare Advantage and Traditional Medicare. Each year, the CMS publishes a booklet, Medicare and You, which discusses the options for senior citizens, including the benefits and costs of both programs. This is a helpful guide, but the provision of comparative information could be improved. As Walton Francis, an independent economist specializing in health insurance, has observed, the “CMS has never adopted the simple lesson from the FEHBP of requiring plans to create brochures in a standard format that makes it easy and convenient for enrollees to compare plans and to be assured that there are few or no ‘gotcha’ omissions or descriptions.”[REF]
While MA plans are all required to cap annual out-of-pocket costs, traditional Medicare has no such cap, and patients must buy private supplemental coverage, such as a Medigap plan to fill in crucial coverage gaps, including the cost of catastrophic events. The result is that beneficiaries in the traditional program must pay at least two premiums, almost doubling their monthly premium cost for comprehensive coverage. At the same time, while MA plans have a cap, there are times when MA plans’ out-of-pocket costs are much higher than beneficiaries anticipated, especially if they pay for out-of-network medical services.
Congress has already taken some steps to address these problems, enacting the No Surprises Act in 2020. In 2023, the House of Representatives (though not the Senate) also passed groundbreaking price-transparency legislation that would apply to MA plans as well as private health plans in the commercial markets. Congress can reinforce these efforts by requiring the CMS to provide beneficiaries clear, easy to understand, side-by-side comparisons of the true costs, including both premium costs and out-of-pocket costs, that they will likely face in both programs.[REF]
10. Establish Site Neutrality in Medicare Payment. Medicare, representing about 12 percent of the federal budget, accounts for more than one-fifth of all American health care spending, and it is growing.[REF] Not surprisingly, Medicare payment policy thus has an enormous influence on private-sector insurance and payment for physicians and other medical professionals. While MA can largely set its own payment rates for in-network provider payments, MA is not entirely independent of traditional Medicare. At a minimum, for example, the law requires MA plans to pay the traditional Medicare FFS rate for out-of-network providers. Under the existing Medicare FFS system, Medicare payments to hospitals for a medical service are generally higher than payments for providers delivering that service outside a hospital setting.
The principle is simple: Medicare should pay the same rate for a medical service or procedure whether it is provided in a hospital setting, a clinic, or in a physician’s office. In short, the payment would be site neutral. Aligning physician and hospital rates could achieve significant savings and blunt impending physician pay cuts without worsening the financial condition of the Medicare hospital insurance (HI) trust fund. The Trump Administration’s Office of Management and Budget analysts projected that implementing site neutrality could lead to significant savings between 2021 and 2030. They estimated that paying hospital-owned physician offices located off-campus at the same rate as independent physician offices would save $47.2 billion over this period. Additionally, they calculated that paying on-campus hospital outpatient departments at the physician office rate for certain services would result in even greater savings of $117.2 billion from 2021 to 2030.[REF]
More recently, Congressional Budget Office (CBO) analysts, in “Options for Reducing the Deficit: 2025–2034,”[REF] have estimated a 10-year savings of $156.9 billion by applying the site-neutral payment formula to almost all Medicare services. Medicare payment changes have an outsized impact (a “spill-over” effect) on the private-sector health markets. That is why analysts with the Blue Cross Blue Shield Association have estimated that a full Medicare site-neutral payment reform would save an estimated $471 billion for both patients and taxpayers from 2024 to 2033.[REF] Further, Medicare beneficiaries would have a greater selection of providers from which to choose. As former HHS Secretaries Alex Azar, serving in the Trump Administration, and Kathleen Sebelius, serving in the Obama Administration, have recently argued, “Site-neutral payments represent a commonsense policy that will reduce costs for patients and taxpayers. It will diminish perverse incentives for consolidation and incentivize care delivery in the right place for the right price. It’s a no-brainer that we believe could reduce costs for patients and payers.”[REF]
11. Repeal the ACA Restrictions on Medicare and Medicaid Payment to Physician- Owned and Certain Specialty Hospitals. Section 6001 of the ACA was—and remains—a direct assault on emerging-market competition, and is yet another contributor to the unhealthy growth of large-scale hospital market consolidation.[REF] Current law imposes this special-interest restriction, even though a large body of data and findings in the professional literature demonstrate conclusively that these physician-owned or physician-managed hospitals, especially specialty hospitals (such as orthopedic facilities) generally outperform general community hospitals on metrics of quality and cost.[REF] The right policy is to open the markets, end the restrictions, and encourage increased innovation in the delivery of quality care, especially specialized care for beneficiaries who suffer from certain complex medical conditions.
12. Allow Retirees Living Overseas to Access Medicare Advantage Plans. In a comprehensive comparison of health insurance options for beneficiaries of Medicare and the FEHBP, Walton Francis notes that federal retirees, especially those enrolled in FEHBP national FFS plans, enjoy “worldwide” health care coverage:
Outside of the United States, FFS coverage extends worldwide in every national plan, and some plans (including the Blue Cross Standard Option) market themselves as providing excellent service and coverage everywhere in the world. Original Medicare offers no coverage abroad, not even emergency care, with minor exceptions in nearby Canada and Mexico.[REF]
Retired Americans living abroad (well over 600,000) receive Social Security, but their earned Medicare benefits are unavailable. Practically speaking, Medicare law, as Francis notes, “denies Medicare benefits entirely to hundreds of thousands of retirees who live abroad, unless they make a special trip to the United States. With the diminished value of Part B, and the cost of travel, those retirees would essentially pay an exorbitant tax to remain in Medicare, and most do not.”[REF] As for MA plans, they do not generally provide coverage to overseas residents and thus differ from the standard-practice FEHBP national plans.
Congress should rectify this inequity. In 2023, Representative Adriano Espaillat (D–NY) took a step in this direction by sponsoring the Earned Benefits Equality and Family Reunification Act (H.R. 5299) that would establish a demonstration program for international coverage for beneficiaries living abroad under the MA program. The demonstration would be conducted among a select group of countries where these Americans reside. The HHS Secretary would conduct the proposed demonstration and allow up to 150,000 Medicare beneficiaries to participate voluntarily. These MA enrollees would be able to access medical services provided by the countries’ national health insurance systems using their MA premiums and benefit coverage, and the Secretary would make payment on behalf of the beneficiaries for the federal government’s share of the costs of these medical items and services.
Private-sector interest in such a program already exists. In fact, the Redbridge Insurance Company, a firm managing health benefits for U.S. Civil Service retirees in Panama, has expressed strong interest in the proposed demonstration project and claims that it can secure significant savings on behalf of the American beneficiaries and taxpayers.[REF] Because medical costs in other countries are generally lower than in the United States, such a claim is eminently reasonable; an assessment that can and should be easily verifiable by the CBO.
13. Allow MA Plans to Compete Directly with Medicare’s Accountable Care Organizations (ACOs) on a Level Playing Field. Congress created the Medicare Shared Savings Program (MSSP) as part of the ACA in 2010. Within the traditional Medicare FFS system, the program authorizes doctors, hospitals, and medical professionals to come together in accountable care organizations (ACOs) to accept financial risk for the care of Medicare patients, with the goal of securing high-quality care at lower cost. By contrast, traditional Medicare FFS pays doctors and other medical professionals an administratively set fee for the delivery of each medical treatment and procedure. The economic incentive, therefore, is for medical professionals to increase the volume of medical services or procedures and secure higher reimbursement with insufficient attention to their quality or outcome. Working with the Obama Administration, Congress designed the ACO program to remedy that deficiency and reward practitioners for improving quality. It is Medicare’s primary “value-based” payment reform. In January 2024, traditional Medicare’s ACO program had 13.7 million beneficiaries.[REF]
This is how the program works. The CMS sets a benchmark spending target for an ACO based on the estimated cost of providing care to the relevant Medicare population. In this financing arrangement, there are two major types of ACO contracts: “upside” risk contracts and “downside” risk contracts. In “upside” risk contracts, if an ACO delivers care at a cost below the CMS benchmark—while maintaining or improving the quality of care according to CMS metrics—the organization reaps a financial reward and shares in the savings achieved with the Medicare program. If the ACO cost of care delivery is higher than the CMS benchmark, then the ACO obviously collects no “shared savings,” but the organization is not financially penalized for excess cost of care. In a “downside” risk contract, if an ACO achieves care delivery at a cost below the CMS benchmark; the ACO qualifies for “shared savings.” If an ACO’s cost exceeds the CMS benchmark, then the ACO may have to pay a financial penalty for incurring the excess costs. Historically, most ACOs have opted for “upside” risk contracts.
While ACOs have achieved high scores on certain quality metrics, their history on securing total program savings has been mixed. In 2018, for example, the CMS reported that the program increased “net” spending since the program’s implementation in 2012, attributing this failure to insufficient uptake of “downside” risk contracts.[REF] In recent years, however, there has been an uptick in total program savings. In 2023, for example, the ACO program achieved a hefty $2.1 billion in savings.[REF]
To enable ACOs to reach their full potential in securing savings as well as improving care quality, Joseph Antos and James Capretta, senior health policy specialists at AEI, have proposed a bold remedy: establish direct competition between ACOs and Medicare Advantage plans on a level playing field.[REF]
In making their case for maximizing competition, they cite the ACO program’s central weakness: It is devoid of informed patient choice. Instead, the Medicare patient chooses an ACO-affiliated doctor. But Medicare patients do not know, nor are they informed, that they are also being enrolled in an ACO. Medicare patients are thus “attributed” to these organizations, and indeed the patients may not even realize that they have been so assigned or even switched from one ACO to another. It is worth noting that the degree of patient “switching” among ACOs may have contributed to the program’s previous problems in generating savings.[REF]
In a reversal of these dynamics, Antos and Capretta propose that ACOs become “provider-driven health plans” and become another valuable option in the MA program. Patients would henceforth choose an ACO in a fully transparent, open market, where provider cost and quality performance would become easily accessible information. Like MA plans, ACOs would participate in the MA program’s annual competitive bidding and payment process. They would obviously have to provide standard Parts A and B medical benefits and services, and they would also be eligible to secure rebates from the government if their bids for offering standard package of benefits come in below the annual CMS benchmarks, thus enabling them to lower beneficiary costs or enhance enrollees’ benefit offerings. ACOs could also offer standard Part D prescription drug coverage, as most MA plans do today. And most important, they would be required to offer Medicare patients protection from the financial devastation of catastrophic illness—a hard limit on Medicare patients’ out-of-pocket costs—a crucial benefit that does not exist in the traditional FFS Medicare program. ACOs could, of course, contract with a health reinsurance company to protect the organization from excessive financial risk.
By creating a competitive level playing field between MA plans and ACOs, not only would traditional Medicare patients benefit but so would patients in the MA program. As Antos and Capretta observe:
Direct competition would be good for both models. It would force ACOs to take on the organizational skills necessary for aggressively managing care for an enrolled population. It would force MA plans to compete in a market with local, provider driven options that are likely to be popular with many beneficiaries. Out of this competition would come better care and lower costs for beneficiaries and Medicare.[REF]
14. (Following Key MA Reforms), Make Medicare Advantage the Default Enrollment for New Medicare Beneficiaries. Today, under current law Social Security recipients are automatically enrolled in traditional Medicare Part B; it is the default enrollment for newly retired people. Throughout their working lives, today’s newly retired beneficiaries, as former Medicare Administrator Gail Wilensky observed, have been enrolled in employer-sponsored plans that broadly resemble the same kind of health plans that are offered today in MA, featuring comprehensive coverage, prescription drug benefits, and catastrophic protection. Because they are automatically enrolled in traditional Medicare, new beneficiaries must fill in coverage gaps and protect themselves by purchasing an additional supplemental, or Medigap, plan, as well as a prescription drug plan, paying as many as three separate premiums and most often higher out-of-pocket costs.
Assuming—and only assuming—crucial improvements to MA payment, risk adjustment, prior authorization, and benefit updates, policymakers could take another step. Given MA’s superior record (well documented in professional literature) in providing high-quality medical care, Congress should change the default enrollment from traditional Medicare to Medicare Advantage.[REF] As urged by Brian Miller and Gail Wilensky, Congress could require MA plans qualifying for automatic enrollment to meet certain quality and cost standards. Of course, Medicare beneficiaries would have the absolute right to re-enroll in traditional Medicare.
MA plans do not use medical underwriting to hike premiums or deny coverage to Medicare beneficiaries. This is not the case with Medicare supplemental coverage, like Medigap. Almost all beneficiaries who would choose to re-enroll in traditional Medicare would also have to buy a supplemental private plan to close crucial coverage gaps. This would mean that they would have to pay, as they do today, an additional monthly premium on top of the standard Part B Medicare premium. In the interest of fairness, Congress should also ensure that returning seniors are not penalized by medical underwriting by insurers offering Medigap or other supplemental coverage.
Conclusion
Overall, Medicare Advantage has been a success. The program has provided seniors with a personal choice of a broad range of health plans and options, including those tailored to their special needs and medical conditions. It has also provided senior and disabled citizens with additional benefits beyond the standard Medicare Part A and Part B benefits, including an impressive array of supplemental benefits. Furthermore, senior and disabled citizens have also found MA coverage affordable, as most Medicare enrollees pay only one premium, the standard Part B monthly premium. Most importantly, the program has succeeded in delivering high-quality medical care. In a review of the professional literature on the subject (48 studies), researchers writing in Health Affairs have found that MA has outperformed traditional Medicare in “most studies comparing quality of care metrics.”[REF]
The bad news is that MA is burdened with very specific and policy-generated flaws. Most significantly, its existing health plan payment system is inefficient and costly. It has unnecessary gaps in benefit coverage, physicians are rightly frustrated with health plan “prior authorization” practices, and patients are sometimes burdened with surprising out-of- pocket costs when they employ the services of out-of-network medical professionals. The good news is that these are all eminently fixable flaws, but solving these problems will require Congress, working closely with the White House, to craft targeted legislative remedies. Given the broad popularity of this enormous program, there is no reason why MA reform should not attract bipartisan support.
Americans deserve, and seniors need, bipartisan congressional cooperation on Medicare reform. Congressional leaders must work across the aisle to improve a vital program that literally impacts every American citizen, young and old alike.
Robert E. Moffit, PhD, is a Senior Research Fellow in the Center for Health and Welfare Policy at The Heritage Foundation.



