Plan year 2021 is the eighth year of operation for the health insurance exchanges created by the Affordable Care Act (ACA, or Obamacare). It also marks the third consecutive year of increased insurer participation at both the state and county levels—a reversal of the prior trend of decreasing insurer participation during plan years 2016–2018.
State-Level Insurer Competition in the Exchanges
One way to measure insurer competition is to assess insurer participation on a state-by-state basis. Table 1 shows the number of carriers in each state and the District of Columbia in the individual market in 2013 and in the exchanges each year since they began in 2014. Insurers that offer exchange coverage through more than one subsidiary in a state are counted as one carrier (the parent company), while insurers that offer coverage in more than one state are counted for each state (as exchange participation is a state-level decision).
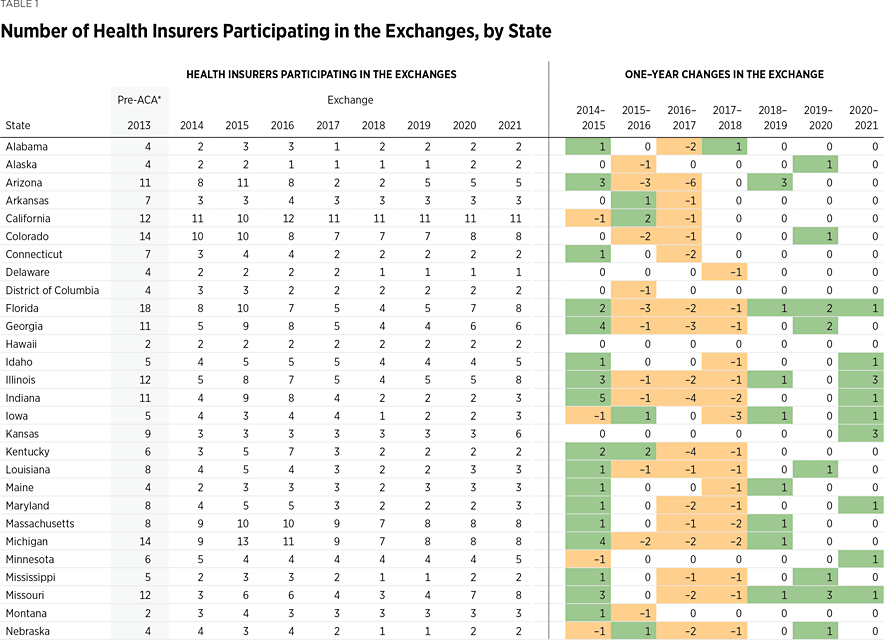
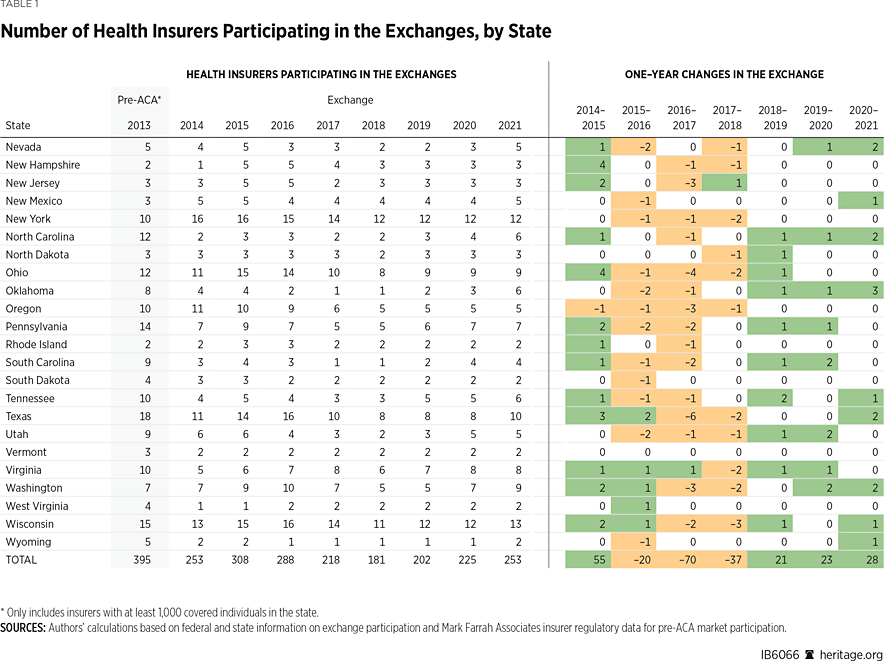
In 2013, the last year before Obamacare’s implementation, 395 insurers sold coverage in the individual market across all states and the District of Columbia. For 2021, 253 insurers offer coverage in the Obamacare exchanges. That is an increase of 72 insurers over the low of 181 in 2018, but it still leaves the 2021 exchanges 36 percent less competitive than the individual market was before the implementation of Obamacare.
Table 1 shows that choice and competition in the state exchanges dropped significantly over the three plan years of 2016–2018 but largely rebounded over the subsequent three years (2019–2021). One consequence of insurers returning to the exchanges was that the number of states with only one insurer offering coverage declined from eight in 2018 to five in 2019 to two in 2020. For 2021, only Delaware still has just one exchange insurer.
Over the past three plan years, the number of insurers offering exchange coverage increased by one insurer each in 16 states, by two insurers in six states, by three insurers in six states, by four insurers in four states, and by five insurers in two states (Missouri and Oklahoma), while remaining the same in 16 states and the District of Columbia. The year-to-year pattern of insurers entering and exiting the exchanges is shown in Chart 1.
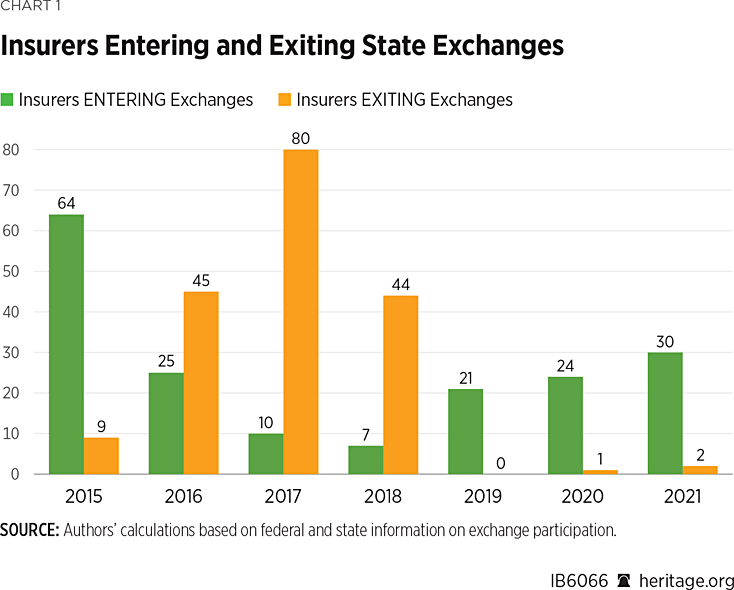
Yet even with the increase in insurer participation over the past three years, only five states have more insurers offering Obamacare exchange coverage in 2021 than before the ACA, while seven states have the same number, and 38 states and the District of Columbia have fewer. Indeed, as Table 1 shows, state-level choice and competition in the Obamacare exchanges in 2021 is essentially back to where it started out in 2014.
2021 County-Level Insurer Competition in the Obamacare Exchanges
Though state-level data are informative, the most tangible measure of competition for consumers is data at the county level. That is because health plans are offered, and priced, locally. Also, because some insurers offer Obamacare exchange coverage only in certain parts of a state, county-level data provides a more precise picture of the actual choices available to consumers.
While information on county-level insurer participation is not included in insurer regulatory filings, it is part of the data sets for exchange coverage and thus has been available for that subset of the market since 2014.
The state-level pattern of three years of decreasing insurer participation, followed by increasing participation over the past three years, was echoed at the county level.
As Chart 2 shows, insurer exits resulted in the share of U.S. counties with only one or two carriers offering exchange plans increasing from 36 percent in 2016 to nearly 82 percent in 2018. Over the past three years, the return of insurers to the exchanges has brought the share of counties with an insurer monopoly or duopoly back down to 53 percent for 2021.
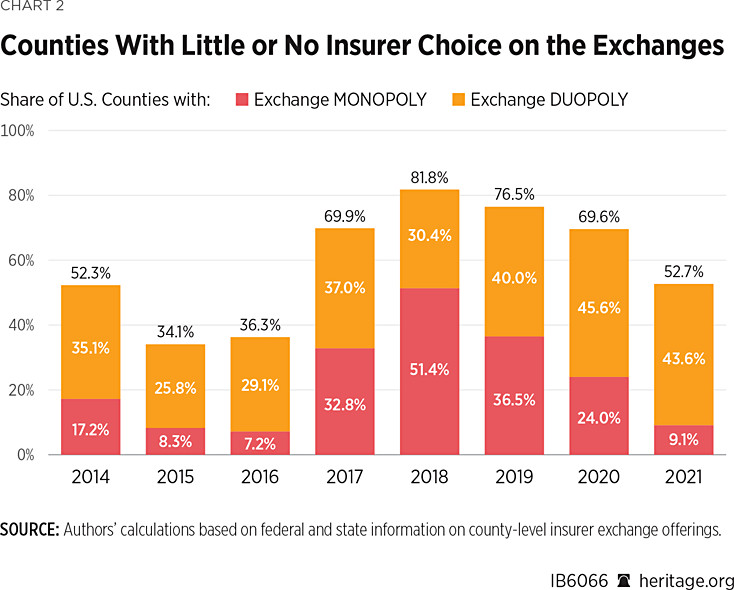
That reversal was driven mainly by changes in the share of counties with only one insurer, which peaked at over half of all counties (51.4 percent) in 2018 but is now down to only 9.1 percent for 2021—about the same level it was at back in 2015 (8.3 percent).REF However, Chart 2 also shows that the share of counties with just two insurers actually increased over the past three years.
Thus, at the county level, the principal effect of insurers returning to the exchanges was that roughly one-quarter of U.S. counties shifted from having an insurer monopoly to a duopoly.REF A secondary effect was a marginal increase in competition among the 572 counties that still had three or more insurers in 2018. As of 2021, roughly one-third of those counties (199 of the 572, or 34.7 percent) had also gained one or more additional insurers.
Patterns of Insurer Exchange Participation
The pattern over the past three years consisted mainly of new or returning insurers selectively offering coverage in portions of states rather than statewide.
During the three-year period 2019–2021, there were 25 instances of insurers reentering state exchanges that they had previously dropped out of, but in only four of those does the insurer currently offer coverage on a statewide basis. Over the same period there were also 49 instances of insurers expanding into states where they had not previously offered exchange coverage, but in only six of those cases did the new entrant offer coverage statewide.
For instance, while Anthem returned to the exchanges in Indiana, Maine, Nevada, Ohio, and Wisconsin, in only two of those states (Maine and Nevada) does it currently offer coverage in all counties. Similarly, United reentered the exchanges in seven states, but in none of them does it currently offer coverage statewide.REF
In general, most of the increase in competition came from smaller, local, or regional insurers and from carriers that focus on offering coverage in targeted metropolitan areas, such as Cigna and Oscar.
Market Stabilization
In part, the rebound in insurer competition reflects a number of actions taken by Trump Administration officials to stabilize the exchange market—such as limiting the ability of medical providers and enrollees to “game” the system and saddle carriers with significant losses.
The Trump Administration also eliminated the payment to insurers of separate “cost-sharing reduction” subsidies. Congress never appropriated funding for those separate payments, and their elimination forced insurers to include those costs in their base premiums for Silver plans.REF That not only made the true cost of Silver plans transparent but also increased the ACA’s “premium tax credits,” which are pegged to the second-lowest-cost Silver plan available to the subsidy-eligible enrollee. Thus, for subsidized enrollees—who overwhelmingly choose Silver plans—the increase in premiums was offset by an increase in subsidies, while premiums for other plans were unaffected by the change.
In addition, the Trump Administration approved “Section 1332” waivers in 15 states, which gave those states regulatory relief from some of Obamacare’s mandates in order to better align federal subsidy dollars with enrollee need using state-based “reinsurance” programs. As a result, insurers in those states were able to maintain, or even reduce, premiums in general. That particularly benefited unsubsidized exchange customers—who primarily choose Bronze plans.REF
Conclusion
As the Obamacare exchange market has stabilized over the past three plan years, more insurers have resumed or expanded their offering of exchange coverage. The result is that, at both the state and county levels, insurer choice and competition in the Obamacare exchanges in 2021 is essentially back to where it started out in 2014. Improvements (especially to premiums) are due to the Trump Administration’s efforts to stabilize the market through actions such as limiting the ability of medical providers and enrollees to “game” the system and saddle carriers with significant losses and allowing states to waive some of Obamacare’s mandates in order to better align federal subsidy dollars with enrollee need using state-based “reinsurance” programs. Despite improvements, the exchanges in 2021 are still one-third less competitive than the individual market was before the implementation of Obamacare.
Edmund F. Haislmaier is Preston A. Wells, Jr. Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Abigail Slagle is a Research Assistant in Domestic Policy Studies.



