The Senate health care bill passed on December 24 does not contain an explicit “public option.” It does, however, still include provisions that could put private health plans out of business. Specially, the bill would:
- Give federal regulators the power to define minimum benefit packages;
- Specify by law the minimum amount that health plans must spend on medical claims; and
- Impose new taxes that will not count toward those minimums.
These three particular provisions could combine to make it impossible for private health plans to simultaneously meet all of the bill’s requirements, thereby allowing appointed officials, by accident or intention, to create regulatory “squeeze” that could, if taken far enough, put private health plans out of existence. This might make a government-run public “option” appear necessary to respond to an artificially created “crisis.”
The Three Regulations at Issue
1. Excise Tax on “Cadillac” Health Plans. The bill imposes a 40 percent excise tax on health plans with total premiums (including both employer and employee shares, if applicable) that exceed certain limits—initially $8,500 for single plans and $23,000 for family plans.[1]
These thresholds would be indexed to consumer inflation, not health insurance premiums, so if premiums continue to rise faster than inflation (as they have over the past four decades), more and more Americans would find that their health plans are subject to this tax.[2]
The tax would apply to the amount by which premiums exceed the threshold, and though it would formally be paid by the insurer, this “excess premium tax,” like sales taxes, would be passed on to the consumer in the form of even higher premiums.
2. Federally Defined Minimum Medical Loss Ratio. The bill also specifies a minimum medical loss ratio (MLR) of 85 percent.[3] This MLR requires insurers to spend at least 85 percent of the premiums they collect to pay claims to health care providers; leaving no more than 15 percent for taxes, administrative expenses, and directly provided services such as chronic disease management.
If medical costs turn out to be less than 85 percent of premiums, insurers would be required to rebate the difference to their policyholders. However, they might prefer to increase their medical expenditures, which—because the spending requirement is expressed as a percentage—would allow them to keep more profit (measured in absolute dollars, rather than as a percentage).
3. Federally Defined Health Benefits. The bill directs the Secretary of Health and Human Services to issue regulations defining specific benefits for all health plans.[4] While the bill does require coverage of broad categories such as “hospitalization” and “physician services,” it directs the secretary to define what those terms mean and what specific services would be covered under what conditions.
The bill also requires a few specific services. For example, the U.S. Preventative Services Task Force (USPSTF) now makes recommendations on what preventive care should be offered to patients, ranking “recommended” services as an “A” or a “B” and services that they do not recommend or recommended against as an “C” or “D,” respectively.[5]
Under the Senate bill, these recommendations would carry the force of law, and coverage of any service rated “A” or “B” would be required without any deductible or copay. The power to make these determinations would fall in the hands of members of this panel who are not held accountable to the voters and are free to promote their own agendas and change their recommendations every year.
Setting a Maximum on Premiums
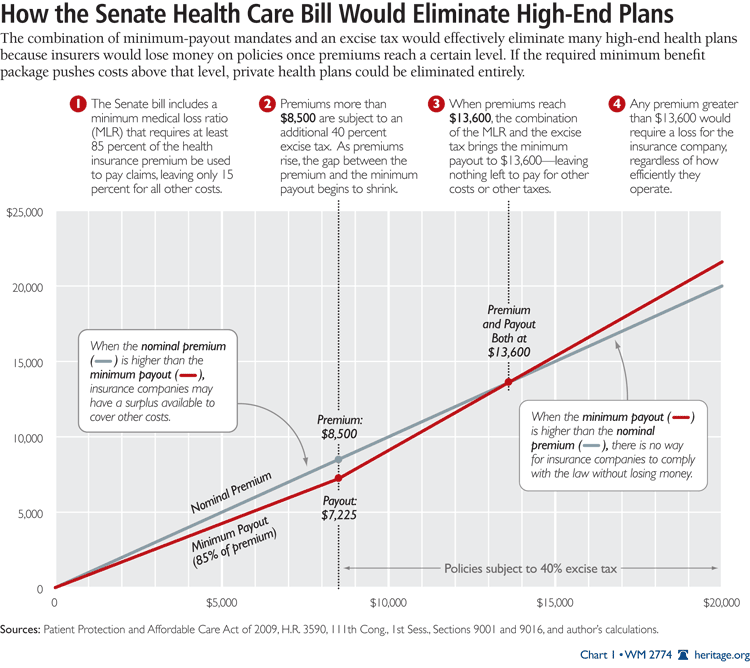
By establishing both an excise tax on high-value health plans and a minimum MLR, the bill creates an implicit maximum legal premium that insurers can charge. With an 85 percent MLR and a 40 percent excise tax on the “excess” premiums, simple algebra shows that if the premium exceeds 1.6 times the taxable threshold, then it is impossible for insurers to both meet the required medical loss ratio and pay the excise tax.
This implies a maximum legal premium of $13,600 for single policies, assuming an $8,500 threshold. At that level, the premium would be entirely consumed by claims and the excise tax, leaving the insurer no funds to pay other taxes or administrative costs, let alone profit.
Of course, in reality it would become impossible to break even at a much lower premium, since there are additional taxes and there are always some administrative costs. The bill imposes an “annual fee” tax on health insurers based on market share, and most states impose premium taxes (usually around 2 percent) and other non-avoidable expenses for regulatory compliance.
Suppose the “annual fee” tax works out to $50 per covered person (this is an approximation for 2016, when the tax will be $10 billion and the CBO estimates about 200 million people will be covered by private insurance[6]) and administrative costs are $500 per person (similar to the current values for both Medicare and private plans[7]). This adds $550 per person to the expenses of the insurer.
In that case, the 40 percent excise tax and the $550 in expenses combined must make up no more than 15 percent of the premium to meet the required MLR. This implies a maximum attainable premium of $11,400, of which $9,690 must be spent on claims. By adding, for example, a fairly typical 2 percent state premium tax, and still assuming no other costs, the maximum premium drops to $10,555, and the maximum amount the insurer can spend on medical claims becomes $8,972.
Notice that every increase in taxes or administrative expenses decreases the amount legally “left over” to pay medical claims. Each increase of $1 in taxes or other expenses requires a reduction of $6.67 in medical claims. In addition to limiting profit and administrative costs, the bill would put an even more restrictive limit on how much insurers could spend to cover their beneficiaries’ medical costs. Spending more on benefits could put insurers out of business.
What Happens When the “Floor” Is Above the “Ceiling”?
While the excise tax and the MLR combine to set a maximum amount insurers would be able to spend on benefits, the Secretary of Health and Human Services is directed to specify a benefits package, which would imply a minimum level of health care spending. Since they are determined separately, the minimum required amount could exceed the maximum.
Currently, many states have mandated benefits that must be covered by all health plans in that state. These mandates are estimated to add 20 to 50 percent to premiums, depending on which mandates are included in a given state.[8]
The experience in these states is instructive: Typically, providers ask the state legislature to require that their services be included so as to increase demand for those services. The Senate bill would make benefit mandates even more pervasive by granting nearly unrestricted authority to appointed executive branch officials to mandate an entire benefits package, which may be expanded every year without further action by Congress.[9]
With every political incentive to increase benefits and little or no pressure to say no, it is quite likely—if not inevitable—that the required benefits would soon cost well above the maximum allowed by the taxes and the required medical loss ratio. In addition, limits on deductibles and copayments would increase use and, therefore, the cost of any particular benefits package.
Whether as the unintended result of a desire for ever more comprehensive coverage or a deliberate attempt to put private health plans out of business, this bill would likely result in a minimum benefit package cost that is high enough to make it literally impossible for private health plans to break even, let alone make a profit.
This would require average claims of $8,972 or more by 2016, which is only 17 percent higher than 2008 per capita health spending and well below the project per capita spending for 2016.[10] If private insurers could not both satisfy the new regulations and stay solvent, this would provide “justification” to institute a government-run public plan.
And if adding benefits did not do the trick, federal lawmakers and regulators could always add “exchange participation fees” or something similar, to cover their costs, which would burden private insurers even more—because every dollar of additional fees would bring plans $6.67 closer to insolvency.
The Complete Elimination of People’s Ability to Choose Private Health Plans
Though it may seem unlikely today that regulators would deliberately put all health plans out of business, the Senate health care bill provides ample authority for this scenario to develop without further congressional action.
By putting an inflexible ceiling on how much insurers can spend on medical costs and how much they can charge in premiums—without any limit on what cost they could be required to incur—this legislation opens the door to the complete elimination of people’s ability to choose private health plans.
Robert A. Book, Ph.D., is Senior Research Fellow in Health Economics in the Center for Data Analysis, and Kathryn Nix is a Research Assistant in the Center for Health Policy Studies, at The Heritage Foundation.


