Abstract: Rapidly rising Medicare spending is a major cause of the federal government’s budget problems. Proposals to reform Medicare and slow its spending fall into one of two categories: more government micromanagement or empowerment of health care consumers in a functioning marketplace. Those who promote top-down spending controls optimistically assume that federal regulators can accomplish now something that has eluded Medicare’s administrators for more than 40 years. In contrast, the market-based approach to reform would harness the power of financial incentives to encourage health care consumers to choose the best, most efficient means of getting services and would reward providers for finding ways to deliver more for less.
Rapidly rising health care costs threaten to push the federal budget past the breaking point. In 1975, total federal spending on Medicare and Medicaid was 1.3 percent of gross domestic product (GDP). In 2010, it was 5.5 percent. The Congressional Budget Office (CBO) expects spending on these programs, together with spending on the entitlement expansions in the 2010 health law, to reach 9.7 percent of GDP by 2030.[1]
At the heart of the budget and entitlement problem is Medicare, the health insurance program for those who are age 65 and older as well as millions of disabled Americans. With spending of $525 billion in 2010, Medicare is the largest payer for medical services in the United States. Its size and market dominance heavily influence how all of American health care is organized.
Analysts who have offered proposals to slow the pace of rising Medicare costs tend to fall into one of two competing camps. The first camp believes that central government management of prices and government reengineering of how services are delivered by doctors and hospitals can control Medicare’s costs—as well as costs in the wider health system—without harming the quality of care. The other camp argues that strong competition in a functioning marketplace will work far better than more government micromanagement to improve quality and reduce costs.
Government Control Versus Market Forces
The gulf between these two camps is deep. They represent completely different approaches to resource allocation—one centered on government control and the political process and the other on consumer choice. The divide is so deep that it is widely viewed on both sides as unbridgeable. As a result, every health care debate tends to become deeply polarized.
Over the past three decades, the camp that favors government control and regulation has been calling the shots in the Medicare program, without success. Medicare spending has continued to rise very rapidly, and the program is now projected to become insolvent in 2024 due to mounting costs.[2]
The alternative to top-down cost control is the financial discipline of a functioning marketplace, which holds costs in check in other sectors of the American economy—something that most Americans understand from buying groceries, electronics, and services.
Recently, proposals have been advanced that would bring market discipline to Medicare by converting the program into fixed premium assistance instead of an open-ended, defined-benefit entitlement.[3] These reforms are designed to harness the power of competition to increase efficiency in the Medicare program.
These reform plans have met with fierce criticism in some quarters. A primary argument of opponents is that government-led efforts will work better than competition to control costs without compromising the quality of care for patients. However, a careful review of the history of Medicare and other programs shows that this criticism is wrong. Competition can bring more discipline to the program, whereas the alternative—top-down price controls—will seriously erode the quality of care that seniors and other patients receive.
Medicare’s Relationship to the Broader Health System
Most often, those who believe that more forceful central management of the health system is the solution to rising costs have viewed Medicare as something like a railcar hooked onto a runaway freight train; The only way to slow down Medicare would be to slow down the whole train. Thus, their solutions tend to aim at containing costs systemwide with more government control, such as a global budget or an all-payer rate-setting system in which public and private insurers alike pay the same government-set prices for services.
Of course, those who believe in building a marketplace for health care reject these kinds of reforms. Their solutions would move Medicare and the rest of the health system toward more cost-conscious consumption.
Interestingly, in the debate over the recently enacted health law, a subtle shift occurred in the thinking among some of those who favor more government control. Instead of viewing Medicare as an innocent bystander in the cost-escalation problem, these analysts began to see that Medicare, as currently constituted, is a primary cause of the cost problem for all of American health care.
Most of those who hold this view, especially those who supported passage of the Patient Protection and Affordable Care Act (PPACA), have not acknowledged and probably will not acknowledge this shift in their point of view, but they do not need to acknowledge it, because it is obvious in the remedies that they pushed in the health care law. PPACA proponents argued repeatedly throughout the legislative process that “delivery system reform” would be the only way to slow cost growth and build a more efficient health sector. In other words, they supported reforms that would alter the ways in which physicians and hospitals provide services to patients. To bring about this “reform of the delivery system,” they argued that Medicare must change how it pays for services for its enrollees.
This is an important development. It does not bridge the huge divide between the governmentalists and those who support market-based reforms, but it does reveal a growing understanding that Medicare’s current design not only is not the solution to America’s health care problems, but actually is the source of many of those problems. Other factors also drive up costs, including unreformed medical malpractice laws, open-ended federal tax subsidization of job-based insurance, perverse incentives in the federal–state matching program for Medicaid, lack of price transparency, and the growing demand for better medical care that comes with increasing wealth and higher incomes. However, Medicare is the most important reason that health care is expensive and needlessly inefficient in the United States.
Outdated Model
American health care has its virtues. The system of job-based insurance for working-age people and Medicare for retirees provides ready access to care for most citizens, although the poor have more problems accessing care through Medicaid. Americans have highly skilled physicians and capital-intensive inpatient institutions that can deliver medical miracles for the sickest. U.S. health care is also open to medical innovation in ways that other health systems around the world are not.
Yet health care in the U.S. is often highly inefficient, and the system is extremely fragmented. Physicians, hospitals, clinics, labs, and pharmacies are autonomous, financially independent units. They bill separately when they render services, with very little coordination of care, which leads to a disastrous level of duplicative services and low-quality care that is dangerous for the patient. The bureaucracy is maddening, the paperwork is burdensome and excessive, and providers have little regard for making the care experience convenient and pleasant.
Indeed, the pervasiveness of these problems has led numerous analysts and scholars to recommend that U.S. health care move toward a true consumer marketplace. Mark Pauly of the University of Pennsylvania and Joseph Antos of the American Enterprise Institute have proposed using marketplace incentives to create a system that is more responsive to patients even as it achieves communitywide objectives, such as better coverage for low-income households and those with chronic health conditions.[4]
The Medicare Fee-for-Service Failure
At the heart of all of this dysfunction is Medicare—more precisely, Medicare’s dominant fee-for-service (FFS) insurance structure.
In a June 2009 article in The New Yorker, Atul Gawande contrasted the high-use, high-cost care provided in McAllen, Texas, to the less costly and higher quality care provided in other cities, such as El Paso, Texas, and at institutions such as the Mayo Clinic.[5] However, as Robert Book pointed out in a Heritage Foundation blog post, the real lesson from the Gawande study may be quite different from what most assumed initially.[6] At the time, the President and others cited it as an example of how physician culture and practice patterns have run amok in certain regions of the country and why “bending the cost curve” would require addressing these problems.
Yet upon closer inspection, it became clear that the cost differences between McAllen and El Paso were largely confined to Medicare. For the non-Medicare population, the cost differential between the two cities was practically nonexistent.[7]
As Book explained, this suggests that Gawande uncovered a problem with Medicare in McAllen, not a problem with medical practice in McAllen. Indeed, Gawande never really explained that Medicare was paying for the expansive volume-driven delivery structure. Without Medicare fee-for-service payments for every physician-prescribed diagnostic test and surgical procedure, the expensive infrastructure in McAllen would never have been viable.
Medicare’s FFS insurance is the largest and most influential payer in most markets. As the name implies, FFS pays any licensed health care provider when a Medicare patient uses services—no questions asked. More than 75 percent of Medicare’s 35 million enrollees are in the FFS program.[8] Physicians, hospitals, clinics, and other care organizations most often set up their operations to maximize revenue from Medicare FFS payments.
For FFS insurance to make any economic sense at all, patients must pay some of the cost when they receive health care services. Otherwise, there is no financial check against the understandable inclination to agree to all of the tests, consultations, and procedures that could be possible, but not guaranteed, steps to better health.[9]
However, Medicare’s FFS does not have effective cost-sharing at the point of service. The program requires cost-sharing, including 20 percent coinsurance to see a physician, but more than 90 percent[10] of FFS beneficiaries have additional insurance in the form of Medigap coverage, retiree wraparound plans, or Medicaid that pays for nearly all costs not covered by FFS. Further, Medicare’s rules require providers to accept the Medicare reimbursement rates as payment in full, effectively precluding any additional billing to the patient.
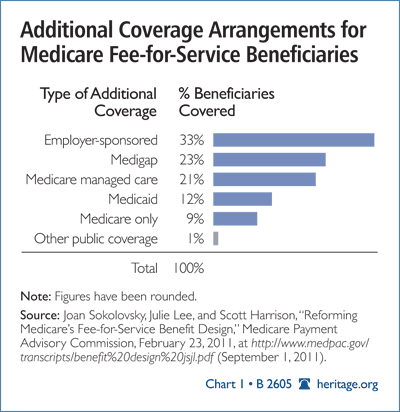
In the vast majority of cases, FFS enrollees incur no additional cost when they use more services, and health care providers earn more only when service use rises. Given these parameters, it is not surprising that the volume of services used by FFS participants has exploded over the years. To make matters worse, the taxpayers pay 80 percent of the increased cost induced by Medigap coverage. Medigap premiums cover only the 20 percent (coinsurance and deductibles) that Medicare does not pay. This serious price distortion leads to overconsumption of Medigap coverage.
The CBO reports that the average beneficiary used 40 percent more physician services in 2005 than in 1997, just eight years earlier.[11] Similarly, according to the Medicare Payment Advisory Commission, spending for physician-administered imaging and other tests was up approximately 40 percent from 2002 to 2007.[12]
Medicare’s dominant FFS design also stifles much-needed innovation in service delivery. As Mark McClellan, former Administrator of the Centers for Medicare and Medicaid Services (CMS), stated:
In traditional FFS Medicare, benefits are determined by statute and cannot easily include many innovative approaches to benefit design, provider payment, care coordination services, and personalized support for beneficiaries.… When providers are paid more when patients have more duplicative tests and more preventable complications—as is the case in FFS payment systems—it is more challenging to take steps like adopting health IT or reorganizing practices in other ways to deliver care more effectively.[13]
Moreover, many of the payment regulations reward higher use of last year’s services, offered by last year’s list of qualified providers. New service delivery organizations, pricing approaches, and ways of caring for a patient—such as over the Internet and phone—are simply not accommodated by payment rules, many of which were written a decade ago. Even marginal changes can take years to implement, often after a multiyear test. Providers are thus understandably reluctant to invest in new approaches, no matter how promising, that will pay off only if Medicare accommodates the change. The result is today’s fragmented and dysfunctional system, which is virtually frozen in place for all users of U.S. health care, not just Medicare beneficiaries.
Medicare administrators have understood the problems created by Medicare’s FFS payment systems for many years. Despite the rising volume, they have tried to control costs by increasing scrutiny of the payment rates per service. Indeed, the ongoing maintenance of the arcane and complex payment systems for hospitals, physicians, nursing homes, and other provider categories is an all-consuming enterprise for the Medicare bureaucracy and the provider groups that watch the bureaucracy’s every move.
Despite curbing some abuses, these payment systems have not controlled Medicare costs. As often happens, the regulated have learned how to work the regulator. Politicians and program officials do not want to be accused of disrupting how and where seniors get care, so care providers naturally use exactly that threat—closed facilities and reduced service—to narrow the range of possible payment changes from year to year. The yearly ritual of keeping physician fees at least level with the prior year’s fees is just one example of this phenomenon. With an effective “political” floor on their Medicare payments, many health care providers see no reason to move away from their autonomous structures and integrate with others in a more organized system of care.
The Centrally Planned “Solution”
Although there is growing recognition of the problems in Medicare’s current design, the opposing sides are proposing very different solutions.
Proponents of the 2010 health care law observed the problem and concluded that better technocratic solutions were needed. They argue incorrectly that today’s arrangements—with all of the distortions that come from open-ended taxpayer subsidization of third-party insurance—are the result of a “private” market that has not worked. They then conclude that, because the market has failed and cannot fix the prevalent problems in health care, the solution is more intensive government regulation. From their perspective, the antidote to today’s inefficient delivery arrangements is a top-down payment reform program in which the federal government uses the leverage of Medicare payment policy to build essentially new organizational arrangements for providing care to patients.
Accountable Care Organizations. Two Administration initiatives in this regard are particularly noteworthy. The first is a new Health and Human Services program to establish accountable care organizations (ACOs) in Medicare.
An ACO allows doctors and hospitals to join voluntarily with others in new legal entities that are accountable for providing care across institutional and outpatient settings. The idea is to put physicians and hospitals in new organizational arrangements in which they share revenue and keep the savings if they provide quality care at less cost than FFS Medicare would normally pay. The physicians and hospitals participating in an ACO would keep a substantial portion of the resulting savings. In effect, ACOs are the latest in a long series of efforts to persuade physicians and hospitals to form provider-run—as opposed to insurance-driven—managed care entities.
Interestingly, a five-year pilot project on ACOs came up short. According to The Washington Post’s Amy Goldstein, “In 2010, the final year, just four of the 10 sites, all long-established groups run by doctors, slowed their Medicare spending enough to qualify for a bonus, according to an official evaluation not yet made public.”[14]
The key to understanding the ACO concept is that beneficiaries play no role in selecting where they obtain care. Medicare’s enrollees are automatically assigned to the ACO that their primary care physician has agreed to join.
This approach to building an ACO is based on an implausible assumption, to say the least. ACOs will be effective at reducing costs only by becoming a more integrated and closed network of providers who follow data-driven protocols for care. That means they cannot let their beneficiaries see just any specialist. The ACO needs patients to see only its preferred list of specialists, but that will be nearly impossible to enforce if beneficiaries have never agreed to become part of the ACO’s managed care environment in the first place.
The proposed ACO regulations, issued by the Department of Health and Human Services in March 2011, provide a window into why centrally planned solutions have never worked in the past and almost certainly will not work this time. The department’s regulators clearly had several competing objectives in mind when drafting the new rule. First among them was saving money for the program, as promised when it was enacted, without harming beneficiaries. To meet this objective, they wrote a 127-page regulation that imposes enormous financial risks on providers to deliver lower-cost care even as it imposes scores of onerous rules and regulations in the name of “consumer protection.”[15]
The result is a regulatory monstrosity that the medical community has nearly unanimously denounced as completely unworkable. Even the integrated health plans that are the supposed ACO prototypes have said that they will not participate in the program as currently conceived.[16] The Department of Health and Human Services may choose to delay the rule and financial burdens in the next round, but that will almost certainly mean that the concept will not save any money either.
Independent Payment Advisory Board. The other prominent Medicare reform pushed by the Administration in the health law is the Independent Payment Advisory Board (IPAB). The IPAB is a 15-member independent panel appointed by the President, confirmed by the Senate, and charged with enforcing an upper limit on annual Medicare spending growth. The IPAB has been given the authority to make recommendations for further cuts in Medicare’s costs, which will automatically take effect unless Congress overrides them.
However, the IPAB is strictly limited in what it can recommend and implement. It cannot change cost-sharing for covered Medicare services, the nature of the Medicare entitlement, the rules governing Medigap insurance, or any aspect of the beneficiary’s relationship to the program. It can really only cut Medicare payment rates for a narrow set of service providers or perhaps deny Medicare coverage altogether for certain types of therapies and procedures.[17]
To deny coverage, the IPAB presumably would need to rely on clinical evidence developed under the “comparative effectiveness research” initiative, which was funded in the stimulus legislation, or other public or private research that provides some evidence of clinical outcomes weighted by the associated cost of alternative interventions. Yet many Americans would distrust these kinds of analyses because they would necessarily mean that a small, unaccountable group of academics would be making important clinical decisions on matters of life and death for Medicare participants based in part on assessments of how much government values an added year of life. This kind of “cost-effectiveness” analysis is highly controversial in other countries and would be completely alien in the U.S.
The flaw in both the ACO and IPAB concepts is that they assume the federal government will be able to enforce a vision for cost control that has eluded Medicare’s administrators for more than 40 years. The private-sector delivery models that are so admired—such as Geisinger, the Cleveland Clinic, and Intermountain Health Care—operate on a principle of provider exclusivity. They do not take just any licensed provider into their fold. They operate highly selective, if not totally closed, networks, which allows them to control the delivery system. Low-quality performers are dropped or avoided altogether, and tight processes are established to streamline care and eliminate unnecessary steps.
The federal government has never shown any capacity to enforce what might be called a Medicare “preferred provider network.” Indeed, the whole point of the Medicare FFS model that Congress has protected so jealously over the years is that beneficiaries may see any licensed provider of their choosing, to whom Medicare pays a fixed reimbursement rate, irrespective of quality. Past attempts to steer patients toward preferred physicians or hospitals have failed miserably because politicians and regulators find it impossible to make distinctions among hospitals and physician groups based on quality measures that can be disputed.
Recently, CBO Director Doug Elmendorf confirmed this pessimism about the government’s ability to reengineer health care delivery through Medicare. In a forthcoming analysis, the CBO assesses such efforts over the past 20 years and essentially concludes that they have done little or nothing to bend the cost curve. According to Elmendorf:
The demonstration projects that Medicare has done in this and other areas are often disappointing. It turns out to be pretty hard to take ideas that seem to work in certain contexts and proliferate that throughout the health care system. The results are discouraging.[18]
Instead, Congress and Medicare’s regulators have cut costs with across-the-board payment rate reductions that apply to every licensed provider without regard to any measures of quality or efficient performance. Tellingly, the recent health law uses this approach to achieve most of its Medicare savings. The big reductions come from arbitrary cuts in payment updates for institutional providers of care. When push comes to shove, the IPAB will almost certainly fall into the same trap. To cut spending fast and with certainty, the preferred solution will always be deeper reductions in payment rates.
Premium Support Can Transform Health Care Delivery
The alternative to the failed top-down approach of government micromanagement is to create the supportive environment for a properly functioning marketplace in Medicare. Medicare does not operate that way today, which is why the program needs reform. The most important feature of such a marketplace system is cost-conscious consumers choosing among competing insurers and delivery systems based on price and quality. That is the basis for The Heritage Foundation’s Medicare proposal in Saving the American Dream and the proposal that was included in the House budget resolution for fiscal year 2012.[19]
Of course, both the Heritage plan and the House-passed budget are much more than plans for Medicare reform. They are comprehensive plans to put the nation’s finances on a sustainable trajectory with policies that will promote economic growth and prosperity.
Yet both plans hinge on converting Medicare into a premium-support program for new entrants below a certain age. Instead of a defined-benefit entitlement, new Medicare beneficiaries would decide how to use a fixed-dollar contribution provided by Medicare. In general, the beneficiaries would decide which insurance plans they preferred. If the premiums for their plans were higher than the Medicare contribution, they would pay the difference out of their own resources. If they chose less expensive plans, they would pay lower premiums and keep the savings. This structure would provide a powerful incentive for the program’s participants to find high-value plans that charge low premiums.
Critics argue that this type of reform would not control health care costs, but would only shift the burden and risk of rapidly rising costs onto individuals because the government’s financial support for Medicare would no longer keep pace with premium growth. However, this is the wrong way to look at these reforms because it ignores the evidence that functioning markets, not top-down regulation and planning, are the key to obtaining value for money and restraining spending. The goal is not to shift rising premium costs from the government onto the beneficiaries, but to move away from the cost-increasing incentives of Medicare FFS and create an entirely different market dynamic to achieve greater efficiency and cost-effectiveness. In time, implementation of a premium-support model would convert millions of passive Medicare participants into cost-conscious consumers of insurance and alternative models for securing needed medical services.
With cost-conscious consumers looking for the best value for their money, cost-cutting innovations would be rewarded, not punished as they are today. Physicians and hospitals would have strong financial incentives to reorganize themselves to increase productivity and efficiency in order to capture a larger share of what would become a highly competitive marketplace. This is the way to slow the growth of health care costs. Indeed, it is the only way to slow growing costs without harming the quality of care.
Prominent health analysts have been making the case that competition in health care could produce much higher value and lower costs than are produced by heavy-handed government payment regulation. Alain Enthoven, one of the original architects of the managed competition theory of health care reform, has written numerous articles on the benefits of competition in various health care markets, including the California public employees system. He and Mark Pauly of the University of Pennsylvania have been among the most prominent and respected economists who have championed vigorous price competition in Medicare as the solution to the cost problem.[20]
Their view that competition can bring more discipline to Medicare spending is supported by experience with the Medicare prescription drug benefit and the Federal Employees Health Benefits Program (FEHBP). It is also supported by official cost estimates of the effects of premium support. Most important, the Chief Actuary of the Medicare program, the official most responsible for assessing Medicare’s future financial viability, shares this view.
The Benefits of Competition in Medicare Part D
Medicare Part D, the prescription drug benefit, was enacted in 2003 and fully implemented in 2006. It provides strong evidence that competition and consumer choice can control the growth of health care costs for Medicare beneficiaries.
The new drug benefit was designed to harness the power of consumers looking for value. There is no government-sponsored plan or option in Medicare Part D. It is delivered entirely through private plans that submit bids to the federal government based on the premium amounts that they will charge for providing drug coverage. The government then calculates what it will pay on a regional basis, based on a weighted average of those bids.
Importantly, the government’s contributions do not vary depending on the plans selected by the beneficiaries. In this way, the government’s contribution toward drug coverage becomes a defined contribution payment on behalf of the Medicare beneficiaries. If a beneficiary selects a plan that costs more than the Medicare contribution, he or she pays the difference out of pocket. Conversely, selection of a relatively less expensive plan would reduce out-of-pocket premium payments from the enrollee.
At the time of enactment, the competitive drug benefit design had many critics.[21] Some argued that the program would not work because private plans would decline to participate without a guaranteed share of the market. Others said that beneficiaries would not sign up for it because the competitive structure was too complex to navigate. Others said that program costs would explode without government-regulated price controls.
All of these predictions proved to be wrong. Now in its sixth year of implementation, the program has exceeded all expectations. Some 90 percent of Medicare participants are in secure drug coverage of some sort, and public opinion surveys show that they are very satisfied with their insurance.[22] Most important, the program is coming in way under budget, with costs over the first decade running 42 percent below estimates at the time of enactment.[23]
Yet the critics persist. They now say that this cost discipline in Part D is either a mirage or unrelated to the competitive design of the program. For instance, Washington Post columnist Ezra Klein has simultaneously argued that Part D premiums are up 57 percent in 2011 compared to 2006 and that prescription drug spending overall (not just for Medicare) is down 35 percent compared to estimates from 2003.[24]
Klein’s criticisms are completely off the mark. First, projected drug spending for the first decade of the Medicare drug benefit dropped 31 percent between forecasts made in 2004 and 2010.[25] Moreover, when the forecasts are adjusted by removing the portion attributable to the elderly (approximately one-third of all drug spending), the drop is just 26 percent.[26] Thus, the drop in expected drug costs for the elderly—42 percent since 2004—far exceeds the drop for the rest of the population.
Moreover, as the Obama Administration and others often contend, the drop in drug spending for the non-elderly may have been heavily influenced by the outsized influence of Medicare. For instance, the movement toward higher use of generic drugs among seniors may have spilled over into the non-elderly market through changed practices among physicians and pharmacies.
Furthermore, the evidence does not support Klein’s assertion that premiums have risen sharply in Part D. The citation used by Klein is flawed because it erroneously assumes that seniors in 2011 did not move to plans with lower premiums when their plans experienced relatively large premium increases. Moreover, it completely excludes the premium experience of those receiving drug coverage through Medicare Advantage plans or former employers.
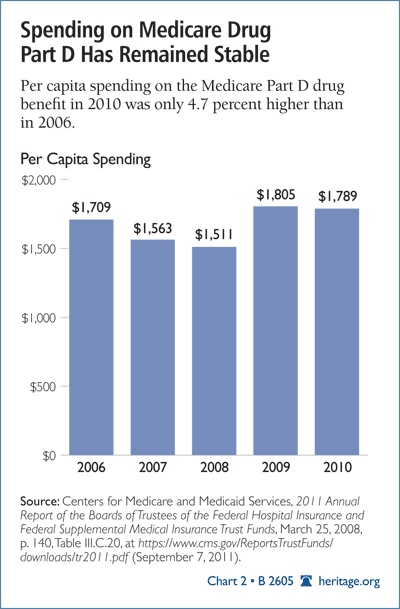
A more comprehensive look at overall per capita costs shows an entirely different and positive picture. As shown in Chart 2, on an “all in” basis, the per capita costs for Part D coverage have risen by only 4.7 percent from 2006 to 2010—less than 1.2 percent per year, which is far below the 4 percent per capita annual cost increase for the rest of Medicare.
The drug benefit is working because it engages the consumer in cost cutting. Seniors want the best value for their Part D premium, which means looking for plans that keep drug prices low and offer favorable terms for using low-cost generics. The result has been a record of cost control that government micromanagement of the rest of the Medicare cannot match.
The Federal Employees Health Benefits Program
Although the drug benefit provides the most direct evidence that competition can work in the Medicare program, additional data indicate the potential for competition to dent the cost curve.
For instance, the premium-support framework proposed for Medicare in Saving the American Dream and the House budget plan is structured like the Federal Employees Health Benefits Program. The FEHBP provides private health insurance coverage for federal employees and retirees and their families based on a consumer choice model. The government makes a premium assistance payment, equal to 72 percent of the weighted-average premium cost of all the competing health plans, to the private insurance plan of beneficiary’s choice, and the worker or retiree pays the balance.[27]
Many studies over the past two decades have compared the costs of the FEHBP and Medicare. The findings are mixed, in large part because the studies used different methodologies to compare costs. As Walton Francis points out, to compare the programs properly on an “apples to apples” basis, some adjustments are necessary to remove the higher costs in the FEHBP for steadily expanded insurance benefits. After this adjustment, the FEHBP has clearly controlled costs better than Medicare has over the past two decades. As Francis put it, “The FEHBP has demonstrably outperformed Medicare in cost control over most of the history of these two programs, simply taking into account benefit improvements in the FEHBP.”[28]
Other researchers have confirmed Francis’s analysis. While at the Joint Economic Committee, Michael O’Grady conducted research showing that, although costs in the FEHBP and Medicare grew at comparable rates, this was not an “apples to apples” comparison because the rising costs of prescription drugs, along with other factors, increased costs faster for private coverage.[29] O’Grady’s analysis, which adjusted for enrollment growth and difference in benefits, showed that Medicare did not contain costs better than the FEHBP did, despite not including drug coverage or providing as generous coverage as private plans provided. Indeed, Medicare offered the least generous coverage of all of the forms of insurance in O’Grady’s analysis, and the FEHBP offered more generous benefits but delivered similar control in cost growth.
Joseph Antos of the American Enterprise Institute reached a similar conclusion. He compared Medicare and private health insurance spending, focusing only on hospital and physician services, thereby excluding prescription drugs and other costs that Medicare did not cover until 2006.[30] His analysis showed that private health insurance performed better than Medicare in containing costs. Spending in the private sector grew more quickly, but the value of coverage increased simultaneously. The share of total private spending covered by insurance grew from 59.6 percent in 1970 to 85.4 percent in 1999, reflecting a decline in out-of-pocket costs for beneficiaries. The cost per unit of private coverage grew more slowly over the same 30 years. Between 1977 and 1996, the generosity of coverage for those under 65 increased by 41.5 percent, compared to just 22.2 percent for Medicare.
Although helpful, even these comparisons do not demonstrate the full potential of competition to slow the pace of rising costs, because the FEHBP and the larger system of employer-sponsored private insurance are not structured properly for cost control. The government’s contribution toward FEHBP plan costs rises with the expense of the plan up to a maximum. Similarly, the tax preference for employer plans rises with premiums. Thus, a large number of workers and retirees can receive a higher FEHBP contribution or tax subsidy by selecting a more expensive offering. This feature of today’s arrangements substantially undermines the incentive for selecting less expensive premium plans.
The Clinton Medicare Commission’s View of Premium Support
Previous official analyses of the premium-support model for Medicare reform have recognized its potential to slow the pace of rising Medicare costs by stimulating competition within a defined contribution framework.
In 1999, the National Bipartisan Commission on the Future of Medicare closely examined the financial implications of a premium-support reform. A majority of the commission members favored such a reform, but not the supermajority necessary to advance the idea to legislative consideration.
During the deliberations, the commission staff issued a detailed analysis of what the concept would mean for Medicare costs in the future. They concluded that moving Medicare toward a competitive structure would lead to both short-term and long-term savings.
In particular, the commission staff believed that premium support would induce private plans to find ways to slow the growth of their premiums every year. Over the first decade, the savings from premium support would reach $65 billion. Over the longer run, the savings would increase, eventually reaching several hundred billion dollars annually, helping to extend the solvency of the program and ensure its viability for future retirees.[31]
Critics of competition sometimes assume that consumers are not as responsive to price signals in health care as they are to price signals in other sectors of the economy. Many studies have shown that this is a false assumption. The RAND Health Insurance Experiment carefully studied the use of higher cost sharing on use of services and found that consumers use health services less if they must pay for a portion of the cost and that the drop in health service utilization occurs without a noticeable deterioration in the health status of the patients. Countless other studies have essentially confirmed these findings over the past three decades.[32]
These studies put to rest the mistaken notion that health care is somehow so different from other parts of economic activity that economic incentives do not matter. Regrettably, this mistaken view has led to disastrous policies. Under the right circumstances, American consumers will demand higher performance from their health care providers. What they need is a public policy change that shifts control of limited resources, not just costs, away from the government and toward the patients.
The View of Medicare’s Chief Actuary
Perhaps the most important recent evidence that competition can work to slow Medicare cost growth was delivered in testimony by CMS Chief Actuary Richard Foster, who has examined scores of Medicare reform proposals in recent years. More than any other government official, he is responsible for assessing the state of Medicare’s financial health. In an appearance before the House Budget Committee on July 13, 2011, he clearly and unambiguously endorsed the cost-saving potential of the premium-support model for Medicare reform in an exchange with Chairman Paul Ryan (R–WI):
RYAN: Do you think a system set up along [premium support lines] can achieve savings in Medicare while continuing to provide for a basic Medicare benefit?
FOSTER: As a general rule, certainly.… If a plan can come through with more efficiency and at a lower cost, participants in that plan would get a cheaper premium. We’ve estimated for many years that competition among plans in a premium support setting like this could have advantages and lead to somewhat lower costs for Medicare. It can get you to the lowest cost consistent with good quality of care.[33]
Foster noted further that premium support could work because it would substantially change the incentives in the program. Today, innovation is aimed mainly at improving quality with higher costs. With premium support, those who deliver services would have strong incentives to invest in cost-reducing technology and redesign organizations to cut costs. For these reasons, he stated that he has somewhat higher confidence in the ability of premium support to control Medicare costs than in the regulatory approaches endorsed in the new health law.
Conclusion
No one, not even the CBO, knows for certain how much a reformed Medicare program based on consumer choice and competition would slow the pace of rising health care costs. The relevant data needed to estimate the effects of such a substantial change in incentives are difficult to find. At the end of the day, policymakers will need to judge the likelihood that such a reform would succeed. Policymakers need to decide which policy approach is most likely to lead to a virtuous cycle of productivity improvement and higher quality throughout the health sector. Given the track record, it is not reasonable to expect top-down reforms, such as those in the new health care law, to produce the desired improvements.
However, a well-functioning marketplace would set in motion the forces needed to transform American medical care, including in the Medicare context, into a model of efficient patient-centered care. Policymakers have good reason to conclude that American health care would benefit from the transformational power of the marketplace that has consistently improved products and services in other sectors of the U.S. and global economies.
The government can and should play an important oversight role in such a reformed system, but the difficult organizational changes and innovations needed to provide better care at lower cost must come from the bottom up, not from the top down. In other words, changes should come from those who are delivering services to patients, not from Congress, the Department of Health and Human Services, or an appointed board of remote and unaccountable “experts.”
—James C. Capretta is a Fellow at the Ethics and Public Policy Center.



