Here’s the truth. Millions of Americans rely on Medicare in their retirement. And millions more will do so in the future. But with an aging population and rising health care costs, we are spending too fast to sustain the program. And if we don’t gradually reform the system while protecting current seniors, it won’t be there when future retirees need it. — President Barack Obama, Address to Congress, September 8, 2011.
Medicare as we know it is not sustainable. — Editorial, “Repairing Medicare,” The Washington Post, January 6, 2013.
Medicare is the cornerstone on which all other government health programs rest. Unfortunately, the deteriorating financial conditions of this program are threatening beneficiary access to its benefits. — Hon. Paul Ryan, Speaker, U.S. House of Representatives, 2015.
The Trustees recommend that Congress and the Executive branch work closely with a sense of urgency to address the depletion of the HI Trust Fund and the projected growth in HI (Part A) and SMI (Parts B and D) expenditures. — Medicare Board of Trustees, Annual Report, 2016.
The Great Medicare Challenge
2015 marked the 50th anniversary of the enactment of Medicare, the huge federal health program that serves senior and disabled citizens.[1] To preserve the program for future retirees, Congress and the new Administration must solve its recurrent problems and improve its performance.
Today, all Americans age 65 and older who have paid into Social Security or the Railroad Retirement program, as well as those who qualify as disabled and patients on dialysis, are entitled to Medicare enrollment: an estimated 57.1 million enrollees in 2016.[2] Half have annual incomes below 200 percent of the federal poverty level ($23,540 per person), and an estimated 45 percent have four or more chronic medical conditions.[3]
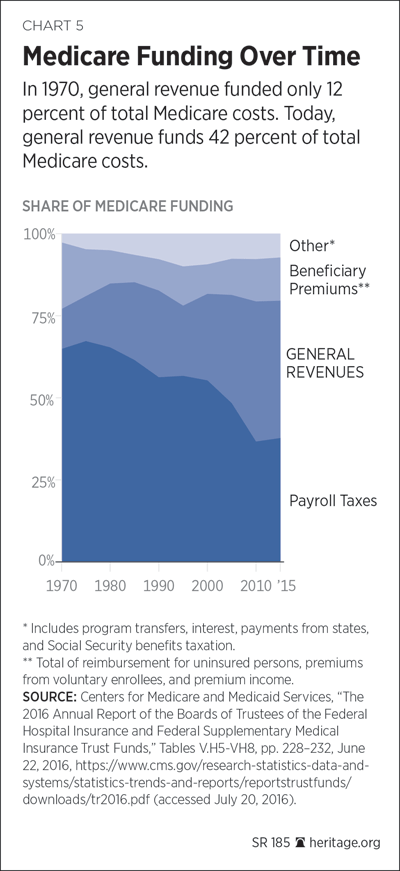
Current workers’ income taxes and payroll taxes finance 84 percent of Medicare’s annual cost.[4] The Medicare trustees estimate that the average per capita Medicare benefit is $12,559.[5] Beneficiary costs vary greatly, of course.[6] The most costly 25 percent of Medicare patients today account for 82 percent of Medicare spending.[7]
Then and Now. The World War II generation, with vivid memories of the Great Depression of the 1930s, cherished especially the financial security that the program delivered for themselves and their parents. At its inception, Medicare provided millions of retirees with continuous and affordable coverage regardless of their health status. At the very time when medical breakthroughs started arming medical professionals with powerful new weapons to combat disease, Medicare helped to finance medical services for a rapidly growing aged population. Not surprisingly, the program has enjoyed almost universal popularity among voters. In 2013, it was reported that among Americans aged 65 or older, 80 percent said that Medicare was “working well” for most seniors.[8]
Over the past 50 years, however, although Medicare delivered core coverage of hospital and physician services and financial security, it quickly deviated from Congress’s original fiscal intentions, with spending far outdistancing the government actuaries’ projections. Unanticipated spending also helped to fuel a giant surge in America’s overall medical costs.[9]
Medicare spending routinely has outpaced inflation, growth in the general economy, and growth in the federal budget, on top of which the program’s adoption of new medical treatments, procedures, or benefit designs, including alternative health insurance arrangements, has had to survive the pressure cooker of intense special-interest lobbying and partisan polarization. Too often, sound and serious change, no matter how beneficial or desirable for seniors, has been either highly politicized or long delayed. Meanwhile, the addition of new benefits and services has been accompanied by increasingly detailed conditions of reimbursement that have led to more intrusive bureaucracy and costly red tape for doctors, hospitals, and other medical professionals.
Challenges Ahead. Succeeding waves of Baby Boomer retirements will make Medicare’s recurrent challenges—demographic, financial, and structural—even tougher.[10] Members of the Baby Boom generation—the 77 million Americans born between 1946 and 1964—form a large and diverse patient population and are turning 65 at the rate of about 10,000 per day. Year after year, the Medicare trustees have warned Congress to act, sooner rather than later, to meet the challenge of providing this group Medicare coverage. Innovative financing and delivery of high-quality care for this huge cohort should command congressional attention and spur decisive action.
Traditional Medicare (Medicare Parts A and B), which covers roughly seven out of 10 enrollees, is an old fashioned, fee-for-service (FFS) program. Its structure is firmly grounded in the technocratic assumptions of 1960s liberalism.[11] Under this highly centralized structure, the government must define each benefit, medical treatment, and procedure and set their specific payment amounts. Adding a new medical benefit or changing or updating benefits can become a major political event. Congressional micromanagement of the program thus remains the perennial norm.
Politicized benefit setting has yielded very mixed results. In 1988, Congress enacted the Medicare Catastrophic Coverage Act, which would have provided protection against catastrophic illness and expanded benefits, including drug coverage. It failed.[12] In 2003, Congress enacted the Medicare Modernization Act, which added a prescription drug benefit and overhauled Medicare’s system of alternative private health plans. It succeeded.[13]
In 2010, on a purely partisan basis, Congress enacted the Affordable Care Act. This polarizing law contained 165 provisions affecting Medicare. It authorized various care delivery reforms; increased Medicare drug subsidies; added preventive services; devised rewards, penalties, and reporting requirements for doctors and hospitals; scheduled breathtaking Medicare payment reductions; and imposed an unprecedented hard cap on the growth of Medicare spending.[14]
With regard to the hard cap on spending growth, the Independent Payment Advisory Board (IPAB), the agency created by the law to enforce the caps and recommend the payment cuts, is not yet functioning. The board and its mission face stiff bipartisan opposition in Congress. Savings from the law’s various delivery reforms are also uncertain, and its draconian Medicare Part A payment cuts, scheduled for implementation over the next 10 years and beyond, already face mounting political opposition.
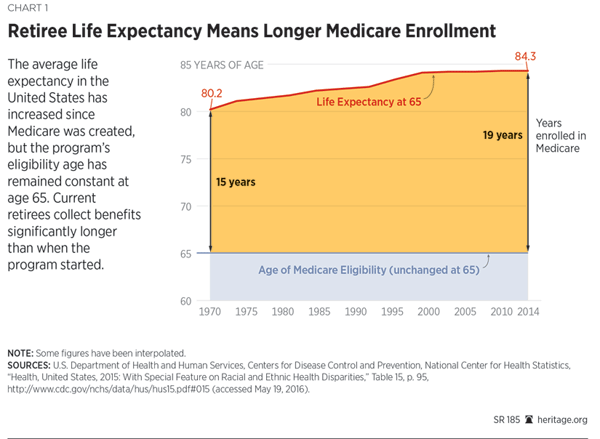
Medicare must also cope with an unprecedented demographic revolution. Americans are growing older and living a great deal longer in retirement. When Medicare was enacted 50 years ago, the law retained Social Security’s age of eligibility at 65 years, set in 1935. In 1965, the average American’s life expectancy was 70.2 years. In 2015, average life expectancy reached 79.4 years, and in 2030, it is projected to reach 80.7 years.[15] The Congressional Budget Office (CBO) confirms that aging of the population will be the decisive factor driving future federal health spending.[16]
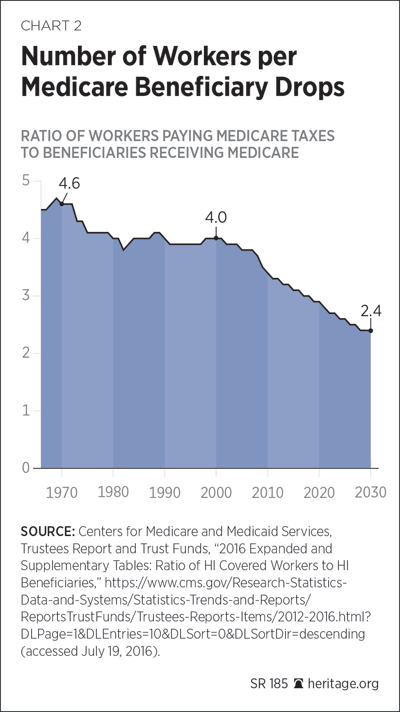
Contrary to a mistaken belief among many seniors that they have somehow “paid” for the benefits that they enjoy in retirement, the truth is that today’s working taxpayers pay for nearly all of Medicare’s current benefits. Moreover, the ratio of working Americans to Medicare recipients continues to shrink and is today slightly more than 3 to 1. By 2030, there will be just 2.4 workers for every person on Medicare.[17] Thus, while paying taxes for four major federal entitlements (including the Affordable Care Act’s insurance subsidies), America’s working families, with fewer children, are supporting a relatively larger and increasingly older retired population.[18]
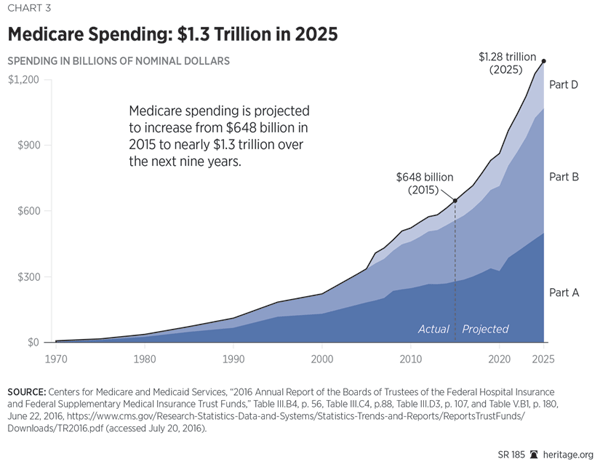
Aside from these structural and demographic problems, there are serious fiscal challenges. Medicare spending has routinely been underestimated (though making such projections is admittedly difficult because of the vagaries of patient behavior, changes in medical technology, or shifting medical practice patterns) and historically has outpaced inflation, the growth of the federal budget, and the growth of the economy. In the near term, the Medicare trustees report, Medicare’s total spending will increase from $683.2 billion in 2016 to $716.8 billion by 2017 and will surpass $1.2 trillion by 2025.[19] Over the period from 2017 to 2025, outlays will generally outpace the growth in the general economy (as measured by GDP), aggregate national health expenditures, and private health insurance.[20]
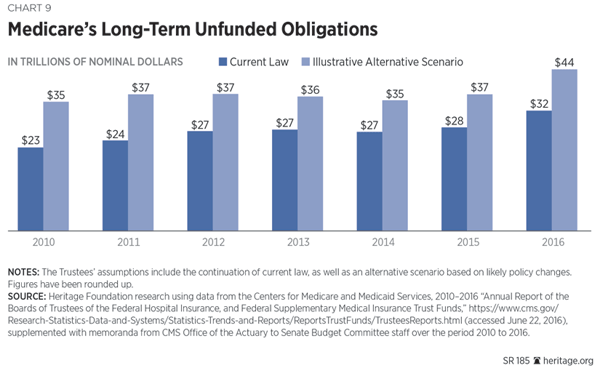
The program is also generating huge long-term debt in the form of trillions of dollars in unfunded obligations, meaning promised Medicare benefits that are not financed through dedicated revenues.[21] Its current fiscal trajectory can only have an unhappy ending: major tax increases, savage benefit cuts, or some undesirable combination of both.
Solving Medicare’s Challenges. For Congress, the policy goal should be not merely a reduction in the rate of Medicare spending, but rather a steady improvement in the quality of that spending and securing the highest value for Medicare dollars, which will benefit seniors and taxpayers alike.[22] New tax and spending policies are not enough to accomplish this major task; nor is a merely increasing the number of upper-income recipients who pay higher Medicare premium payments or increasing the normal age of Medicare eligibility. Free-market dynamics will make the greatest difference in securing quality and cost control. Intense market competition among health plans and doctors and other medical professionals, driven by patient choice through a defined-contribution (premium support) financing system with fully transparent premiums and pricing, can achieve these goals.[23]
Structure and Financing of a Complex Program
Medicare has evolved in fits and starts over the past 50 years. Today, it is organized into four parts that reflect four distinct sets of benefit offerings. Each part is designed differently, governed by a different set of rules, and funded by separate revenue streams and beneficiary financing. Payments on behalf of recipients, however, have a permanent, indefinite appropriation, meaning that they do not require annual congressional appropriations.
Politicians routinely promise to defend Medicare’s “guaranteed benefits.” That claim, however, is mostly rhetorical: There is, strictly speaking, no “guarantee” attached to Medicare benefits.[24]
Traditional Medicare. Medicare Part A, the Hospital Insurance (HI) program, and Part B, which covers physicians’ and outpatient services, are best described as “traditional” Medicare. This division of coverage mirrored the Blue Cross–Blue Shield model of the 1960s and is still the main vehicle for the fee-for-service financing of that period. Doctors, hospitals, and other medical professionals are reimbursed for their individual services rather than paid through salaries or reimbursed with capitated payments. Medicare fees are determined by congressionally authorized administrative payment formulas for thousands of coded medical services. All of these payments are subject to payment caps or price controls.
Hospitalization. Medicare Part A is a mandatory program.[25] It covers inpatient hospitalization as well as limited nursing care, hospice care, and some home health care. While the vast majority of beneficiaries pay no Part A premiums, all pay a deductible for each hospital stay ($1,288 in 2016) and progressively higher levels of coinsurance after 91 days of hospitalization, up to $644 per day in 2016.[26] Part A serves an estimated 56.7 million Medicare recipients.[27]
Part A is funded almost entirely by the 2.9 percent federal payroll tax, the revenues from which are deposited in the HI trust fund. This is not a savings fund in any sense; it is a “pass through” vehicle to pay the program’s hospital bills. In other words, the HI program is a classic pay-as-you-go system, meaning that today’s workers pay the benefits of today’s Medicare recipients just as tomorrow’s workers will pay for the benefits of tomorrow’s recipients.
Under the Affordable Care Act of 2010, effective in 2013, upper-income workers—single persons with annual incomes of $200,000 and couples with annual incomes of $250,000—pay an additional 0.9 percent in payroll tax. Over time, because these income thresholds are not indexed to inflation, more and more individuals and couples will be subject to the higher tax until, as the Medicare trustees point out, an estimated 79 percent of all workers will be paying the higher 3.8 percent payroll tax.[28] High-income workers are also subject to a 3.8 percent “Medicare tax” on unearned income, but the revenues from this new tax are not earmarked for the HI trust fund;[29] instead, they are used to finance additional spending required by the Affordable Care Act.
Under current law, the government may pay for Part A medical services only to the extent that funds are available in the trust fund.[30] So far, despite the Medicare trustees’ periodic warnings of threatened insolvency, the HI trust fund has never been insolvent. This year, the trustees projected that the trust fund would have relatively small surpluses through 2020, followed by annual cash deficits, and then would fall into insolvency in 2028.[31] The CBO, using different assumptions, recently projected that the trust fund would become insolvent in 2026.[32] In any case, the HI trust fund does not meet the trustees’ short-term or long-term standards of “financial adequacy.”[33]
Physicians’ Services. Medicare Part B is voluntary and enrolls about 52 million recipients.[34] It covers physician services, outpatient hospital services, preventive care, and some home health services. Part B is financed by a combination of beneficiary premiums (the monthly standard for most enrollees is $104.90 in 2016) and general taxation, and its benefits come with a modest annual deductible ($166 in 2016), with 20 percent coinsurance for most services.
From 1966 until 1975, seniors paid 50 percent of their total Part B premium. Today, for the standard Part B premium, beneficiaries fund just 25 percent of premium costs; the taxpayers pay the remaining 75 percent out of general revenues. Unlike Part A, general fund transfers keep the Part B “trust fund” permanently in balance. The portion of total federal income taxes required to fund the general revenue portion of Part B services will grow from roughly 16 percent today to 21.4 percent by 2030.[35]
Upper-income beneficiaries—between 5 percent and 6 percent of the total Medicare population—pay progressively more through an income-based payment schedule above the standard Part B premium. There are four levels of higher Part B premium payments, ranging from $170.50 per month to $389.80 per month in 2016. The highest premiums are paid by enrollees with annual incomes in excess of $214,000 for individuals and more than $428,000 for couples.[36]
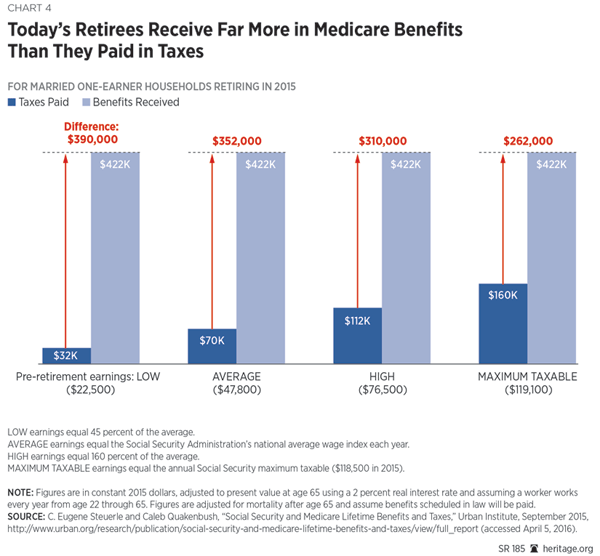
As noted, many seniors mistakenly believe that they have “paid” for their Medicare benefits. This is an illusion.[37] Medicare recipients typically get back two to three times more in benefits than they have paid in taxes during their working lifetimes, and recipients’ relatively small share (25 percent) of the Part B and Part D premiums accounts for no more than 13 percent of Medicare’s annual total financing.[38]
Competitive Medicare. In 2003, Congress established new defined-contribution financing, the allocation of fixed amounts of Medicare funds per beneficiary through market- based competitive bidding. Congress applied this financing for enrollees choosing comprehensive private health plans and for their prescription drug benefits.[39] In both instances, private health plans compete in providing medical and pharmaceutical services to Medicare recipients. Both programs have a good record of offering a broad array of health benefits and services, ensuring better-quality care, and generating higher levels of patient satisfaction.[40]
Private Health Plan Options. Before Medicare’s enactment in 1965, roughly half of all seniors had private health insurance.[41] Given the dynamics of crowd-out, private plan alternatives soon all but disappeared. Beginning in the 1970s, however, Congress experimented with private plans in Medicare, mostly managed care plans, with uneven success. In the Balanced Budget Act of 1997, Congress created the Medicare+Choice program, Medicare Part C, an updated effort to offer seniors private health plan alternatives. Hit with a deadly combination of payment caps and regulatory overkill, however, health plan participation plummeted, and the effort failed.[42]
With the Medicare Modernization Act of 2003, Congress created the Medicare Advantage (MA) program, a new version of Part C. The program is funded by recipients’ Part B premiums and government subsidies. Health plans at the county level are paid on the basis of competitive bidding for the provision of traditional Medicare benefits, including prescription drug benefits, and the cost of traditional Medicare in the county. If plans price their offerings above the traditional Medicare benchmark, enrollees must pay an additional premium amount if they wish to enroll in those plans. If plans price their offerings below the traditional benchmark, they must offer enrollees rebates in the form of reduced premiums or richer benefits.
In 2015, 99 percent of Medicare beneficiaries had access to MA plans.[43] Enrollees nationwide could typically choose from among 18 health plans, and roughly 17 million were enrolled in Medicare Part C.[44] Medicare Advantage enrollment, estimated at 32 percent of total Medicare enrollment in 2016, is on track to reach 35 percent by 2022.[45]
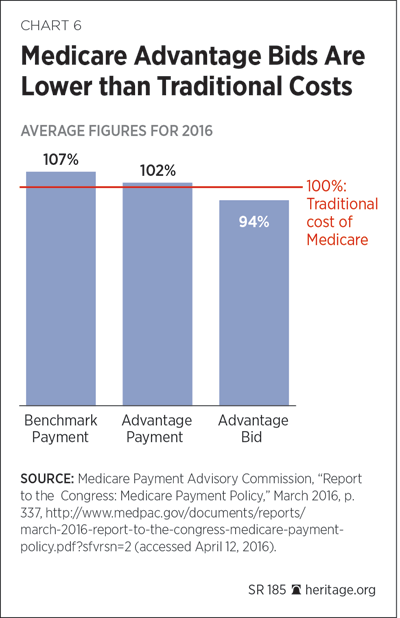
These private plans have been routinely bidding below the traditional Medicare benchmark level in providing Part A and Part B benefits. According to Alice Rivlin and Willem Daniel of the Brookings Institution, “Evidence shows that MA plans, especially if they are Health Maintenance Organizations (HMOs) can deliver Medicare benefits more cost effectively than traditional FFS Medicare, especially in higher cost urban areas where a large fraction of Medicare beneficiaries live.”[46] Medicare Advantage has also registered higher levels of enrollee satisfaction than traditional Medicare has registered[47] and has served the poorest and sickest Medicare recipients particularly well.[48]
Under the Affordable Care Act of 2010, payments to MA plans are scheduled to be reduced by an estimated $156 billion over 10 years, and the payment formula incorporates a new bonus system. The link to traditional Medicare spending, however, is retained.
Prescription Drugs. When the Medicare Modernization Act of 2003 (MMA) was being debated, three-quarters of all seniors already had prescription drug coverage, and congressional conservatives worried that a universal entitlement for drugs would displace existing private coverage. The creation of another universal entitlement also threatened to increase greatly the unfunded obligations of the already financially troubled program. In both cases, those concerns turned out to be justified.[49]
In the final version of the legislation, Congress created a universal entitlement to prescription drugs in Medicare Part D as a voluntary program. Prescription drugs were to be delivered through private health plans, including employer plans.[50] For financing, Congress authorized a defined contribution to these private plans on behalf of Medicare recipients, with payment to be based on competitive bidding among plans for the provision of the standard Medicare drug benefit. Upper-income Medicare recipients were required to pay higher Part D premiums, and lower-income recipients got additional subsidies to offset their drug benefit costs.[51]
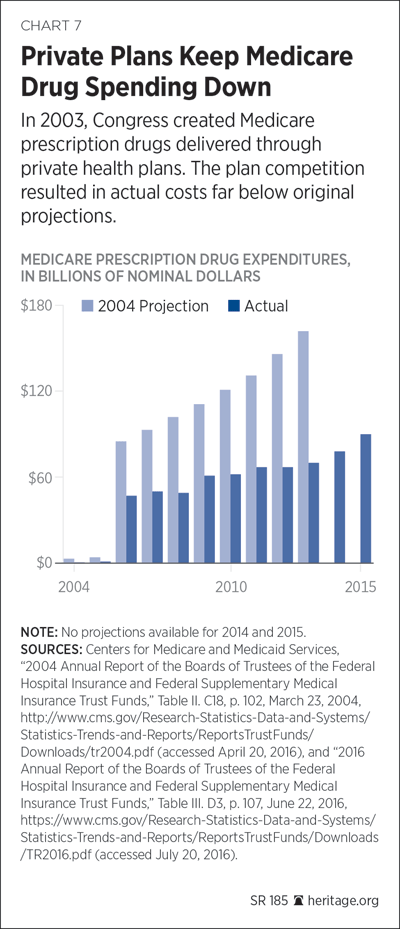
As with Medicare Part B, three-quarters of Part D’s funding comes from general revenues and other government financing, and about one-quarter comes from Medicare recipients’ premiums. In terms of the effectiveness of its financing and competitive structure, the program has been a success. Part D’s aggregate costs have been 50 percent below original projections, and its premiums have been remarkably stable.[52]
Today, all Medicare enrollees have access to drug coverage, and 72 percent are enrolled in Part D.[53] Most are enrolled in special prescription drug plans (PDPs); 886 of such plans are offered in 34 regions around the United States, and all Medicare enrollees have a multiple choice from among these plans.[54] Among seniors, the program is immensely popular. An impressive 90 percent of Medicare enrollees are satisfied with Part D, and of that number, 59 percent are “very” satisfied.[55]
Chronic Medicare Conditions
While Medicare has indeed provided seniors access to continuous coverage and secured them some measure of financial security, the program has been burdened by persistent problems. Some became evident shortly after Medicare’s enactment; others emerged over time; virtually all have since become recurrent weaknesses of the program. Among these chronic problems are:
- Rising costs;
- Future debt;
- Metastasizing bureaucracy;
- Continuing gaps in coverage;
- The quest for quality;
- Inefficient pricing;
- Subversion of professional independence and restriction of patient freedom;
- Generation of waste, fraud, and abuse; and
- Threatened access to care.
Rising Costs. Over the past 50 years, big Medicare cost increases have been a recurrent problem. In 1966, the first year of Medicare’s operation, hospital expenditures jumped 20 percent, and the growth in physician fees jumped from 3.8 percent in 1965 to 7.8 percent in 1966.[56] As Theodore R. Marmor, professor of political science at Yale University, has remarked:
Medicare was unable…to escape from the growing problems of American medicine generally, especially medical inflation. Indeed the problem of cost control emerged as a largely unforeseen, recurring and central influence on Medicare’s development in the decades following its enactment.[57]
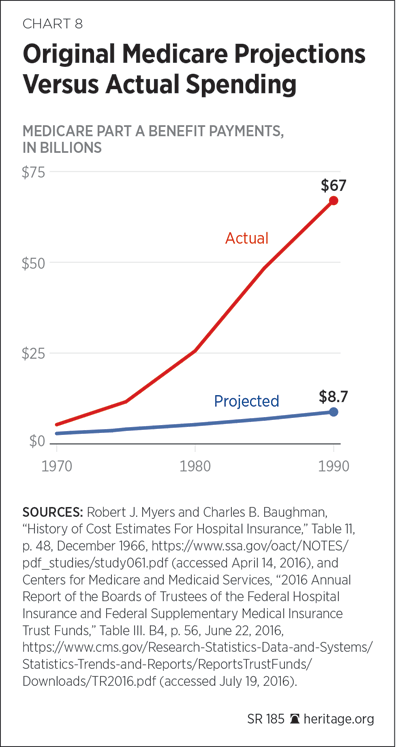
In 1966, as they were plotting out Medicare’s fiscal future, government actuaries made HI cost projections that were wildly inaccurate, projecting Medicare hospitalization costs at slightly more than $9 billion in 1990, when the actual cost turned out to be nearly $67 billion.[58] Although unanticipated high levels of spending became routine, certain Medicare services displayed stunning growth. From 1991 to 1995, for example, Medicare spending for home health services skyrocketed by 35.2 percent.[59] As spending increases were jumping well beyond official expectations, the government’s regulatory responses secured only temporary respites in this growth—respites invariably accompanied by billions of dollars of cost shifting from one part of the program to another, or onto employers and employees with private health insurance.
In a reversal of historical patterns, Medicare spending has slowed during the past few years. Total Medicare spending climbed at an average annual rate of 7.6 percent from 1985 to 2015, and government actuaries project that growth will be 7.1 percent from 2015 to 2025.[60] While independent analysts generally cite the economic slowdown as the reason for the decline in aggregate health spending over the past few years, the CBO finds no correlation between Medicare spending and economic growth.[61] The U.S. Government Accountability Office (GAO) similarly reports that:
The reasons for this slowdown are not entirely clear and it is uncertain whether the effect will be transitory or longer lasting. Nonetheless, Medicare’s historical trends, the aging of the population, the uncertainties associated with recent reforms and the effects of advances in medical technology, all underscore the continued efforts to moderate spending growth while ensuring that beneficiaries have appropriate access to high quality health care.[62]
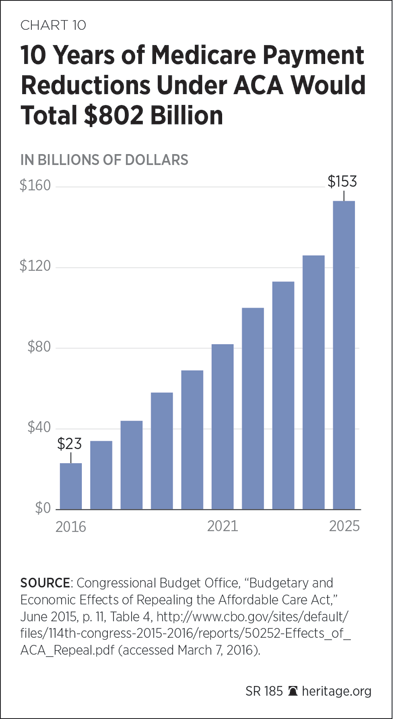
The ACA’s scheduled Medicare payment cuts and program changes amount to $802 billion over the next 10 years, and Administration officials are hoping that these efforts, combined with the ACA’s implementation of new delivery and Medicare payment reforms, will ensure a continued slowdown in Medicare spending. However, the CBO initially scored most of the law’s much-anticipated delivery reforms as having no effect or a negligible effect on health care spending.[63] As for the big Medicare payment reductions, if they were actually enforced, they would indeed yield big savings over time, but they would also severely underprice Medicare services below comparable payment levels in the private sector, and the resulting political pressure to halt or reverse them would be enormous. That is why both the Medicare Actuary and the CBO have stated plainly that the ACA’s Medicare payment reductions are either unrealistic or politically unsustainable.[64]
As noted, the pace of Medicare spending is already accelerating. The program will be, far and away, the biggest driver of federal health care spending over the next three decades. Estimates of the upward trajectory vary:
- Government actuaries estimate that Medicare spending will grow by 6.7 percent in 2019 and reach 7.6 percent by 2025;[65]
- The CBO also projects that the size of Medicare will grow from 3.6 percent of GDP in 2015 to 4.7 percent of GDP by 2026;[66] and
- The Medicare trustees further project that Medicare will grow to 5.6 percent to 6.2 percent of GDP by 2040, depending on assumptions.[67]
Congress is also taking discrete steps to increase Medicare spending. For example, the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) repealed and replaced the unworkable Medicare physician payment update formula, but it also added $175 billion to Medicare Part B spending over the next 10 years and offset that additional spending with a mere $35 billion in Medicare savings. Beyond increasing taxpayer obligations, the new law added an estimated $141 billion to the nation’s deficits.[68]
Looking further ahead, the Medicare trustees are required to issue a “fiscal warning” whenever general revenues exceed 45 percent of total Medicare outlays within a period of seven years.[69] Increasingly, and well into the foreseeable future, Medicare costs will be funded out of general revenues. General revenues will once again exceed 45 percent of total Medicare outlays by 2023.[70]
Future Debt. From 2008 to 2012, according to the Congressional Research Service (CRS), federal deficits totaled $5.6 trillion, and the public debt has doubled so that it now amounts to 76 percent of America’s gross domestic product (GDP).[71] For its part, the CBO has issued its own stern warnings about America’s fiscal future.
While the size of annual deficits (reaching $1.4 trillion in 2009) has recently declined, for example, the CBO projects that they are poised to rise again and to accumulate a total of $9.4 trillion from 2017 to 2026.[72] Assuming an extension of current baseline spending, the CBO projects that the debt will amount to 86 percent of GDP by 2026. The deadly combination of dramatic federal spending increases and dangerous deficits over the next three decades will lead to a public debt that amounts to 141 percent of GDP, “exceeding the historical peak of 106 percent that occurred just after World War II.”[73] As the CBO has repeatedly declared, the aging of the population and rising federal entitlement costs, particularly Medicare costs, will aggravate the nation’s fiscal problems.[74]
Congress and successive Administrations have made benefit promises to Medicare recipients that current and future generations of taxpayers—assuming that those promises are honored—must finance with new taxes. In other words, taxpayers are inheriting an enormous “off-budget” debt. Excluded from the conventional accounting of the national debt, this mounting burden is often referred to as Medicare’s unfunded obligation. This 75-year unfunded obligation is staggering, ranging from $32.4 trillion to $43.5 trillion, depending on the assumptions used.[75] Over the past five years, despite many administrative and legislative changes, the program’s long-term fiscal condition has not improved. Maintaining Medicare’s status quo means huge taxes for young working families.[76]
Metastasizing Bureaucracy. Medicare’s governance has been a perennial problem. In 1966, Medicare was administered by the Social Security Administration, but for a variety of reasons, the SSA was found unsuitable for the task.[77] In 1977, Medicare’s administrative apparatus was housed in the newly created Health Care Financing Administration (HCFA), a division within the giant U.S. Department of Health and Human Services (HHS), but throughout the 1980s and 1990s, this increasingly dictatorial and distant Medicare bureaucracy incurred a deep and abiding hostility among doctors, hospitals, and other medical professionals.
By the late 1990s, Medicare’s governance problems had reached a crisis point, and in 1999, in an open letter in Health Affairs, the nation’s most prominent health policy journal, a diverse group of health policy experts declared that congressional authorization of more administrative duties should be matched with a bigger budget and more staff.[78] When the Bush Administration took office in 2001, it retained the agency’s regulatory mission but gave the Medicare bureaucracy a more attractive and more customer-friendly name: Centers for Medicare and Medicaid Services (CMS).
Today, the CMS employs 5,400 people in its Baltimore, Maryland, and Washington, D.C., offices and in 10 regional offices around the nation. Besides Medicare, the CMS is responsible for Medicaid, the huge and growing health program for the poor and indigent, and the Children’s’ Health Insurance Program (CHIP). It also oversees the ACA’s programs, such as early retirement reinsurance, state high-risk pools, and oversight and regulation of health plans offered through the law’s health insurance exchanges.[79] In its administration of the ACA, the CMS must cooperate with several other key federal agencies, including the U.S. Department of Labor; the Internal Revenue Service (IRS); and the U.S. Office of Personnel Management (OPM).
With such a daunting range of responsibilities, the CMS’s impact on America is greater than that of most Cabinet departments. Because Medicare is almost always a key issue in annual budget debates, in addition to being the nation’s largest “insurer,” the Medicare bureaucracy is subject to intense oversight.[80]
But the CMS’s top job is Medicare. The agency contracts with large private insurance carriers, such as Blue Cross and Blue Shield, to process Medicare claims and implement the program’s reams of rules and regulations. Not only does the agency play the role of insurer for the nation’s senior and disabled citizens; it also enforces a complex array of administrative pricing systems, administers the contracts for fiscal intermediaries and carriers, oversees the process for paying FFS claims, runs Medicare’s private plan and prescription drug programs, combats fraud and abuse, issues directives and guidance to plans and providers, and provides information to Medicare recipients.
Actually, the tens of millions of Medicare patients have little if any direct interaction with the Medicare bureaucracy.[81] Structurally, Medicare is a provider-centric rather than patient-centric program, and the Medicare bureaucracy’s routine agenda—administering payments and issuing regulations—is largely provider-driven. Regulatory solutions to the program’s innumerable problems often generate problems of their own and result in even more regulation, a cascade of provider complaints, and subsequent congressional interventions.
Over the past 50 years, the Medicare bureaucracy has issued tens of thousands of rules, regulations, and guidelines governing every aspect of health care financing and delivery. Aside from formal rules, the CMS has 37,000 “guidance documents” on its website.[82] The agency is thus a powerful engine of bureaucratic control. When Congress, or CMS pursuant to congressional authority, defines a benefit or authorizes a medical procedure, CMS officials must try to price these benefits and procedures in a rational way to avoid overpaying or underpaying providers. Congress also delegates regulatory authority to the agency to determine the conditions under which these thousands of medical procedures are delivered and reimbursed and to decide whether or not they are medically “necessary or appropriate.” Delivery of hospital and physician care is thus subject to regular government intrusions that compound similar intrusions by state regulatory bodies as well as private managed care plans.
Today, Medicare officials routinely report low administrative costs of between 1 percent and 3 percent,[83] but these reports do not include the total costs of public provision, such as the costs of tax collection or the time, energy, and effort expended by federal officials through legislative and regulatory processes. Nor do these reports account for the notorious costs incurred by continuing administrative failures to curb or eliminate wasteful and unnecessary spending, such as “improper payments” to providers, or the consequent heavy losses resulting from fraud and abuse. A related problem is that Medicare shifts administrative costs to doctors, hospitals, and other medical professionals. These additional costs take the form of transactional costs that are generated by compliance with mandatory coding and reporting requirements—a serious administrative burden on medical professionals.
Complying with Medicare rules and paperwork takes precious time, energy, and effort away from patient care. According to a recent Rand Corporation study:
Physicians of all specialties reported feeling overwhelmed by the cumulative effect of rules and regulations on their ability to deliver patient care or run a practice. These frustrations were present in all practice models, but physicians in small and medium-sized practices expressed these frustrations most strongly.[84]
Once again, this is an old problem, yet quantitative analysis has been sparse. In 2001, a PricewatershouseCoopers study found that for every hour of Medicare patient care in a hospital, hospital officials spent at least one half-hour complying with Medicare rules and paperwork.[85] In 1995, the American Medical Association (AMA) reported that doctors were spending about 25 percent of their time complying with Medicare paperwork.[86] In 1992, the Medicare Physician Payment Review Commission reported that the bureaucratic “hassle factor” was a top complaint of seven out of 10 doctors, and physicians judged Medicare to be worse than Medicaid or even the roundly despised private HMOs.[87]
Over the past 50 years, the range and scope of Medicare’s regulatory activities have become mind-numbingly detailed. The massive ACA, of course, adds to these regulatory burdens and costs. So, too, does the Medicare Access and CHIP Reauthorization Act of 2015. Implementation of the law’s new payment system is projected to hit smaller medical practices particularly hard, with an estimated 87 percent of solo practices facing payment penalties.[88] Writing in Health Affairs, researchers report that doctors and their staffs spend, on average, an estimated 785.2 hours per physician tracking and reporting “quality” measures for Medicare, Medicaid, and private health plans. The annual average cost of these exercises is $40,069 per physician—an estimated $15.4 billion annually systemwide.[89] Not surprisingly, Medicare’s bureaucratic requirements are contributing to the demoralization of doctors and other medical professionals.
Continuing Gaps in Coverage. Traditional Medicare is characterized by crucial gaps in coverage.[90] After 50 years, the traditional program still offers no protection against catastrophic illness, a common feature of all private insurance plans and a requirement in “competitive” Medicare for private health plans and prescription drug coverage. Today, 86 percent of Medicare recipients buy private Medigap plans or enroll in some other form of supplemental coverage. Of these, about 18 percent of those in the Medicare fee-for-service population are “dual eligible” and rely on Medicaid.[91]
The relationship between traditional Medicare and supplemental insurance generates additional and unnecessary spending by seniors and taxpayers. Seniors pay an extra premium for the supplemental coverage, which covers not only catastrophic events, but also traditional Medicare’s complex system of co-insurance and deductibles. As The Washington Post noted in 2013, “The current Medicare program includes a hodgepodge of cost-sharing requirements that neither give participants clear incentives to limit consumption of services nor shield them from catastrophic expenses.”[92] Higher utilization generates higher Part B premiums for seniors as well as heavier Part B costs for taxpayers. This “double-coverage” arrangement thus results in enormous additional costs for seniors and taxpayers alike.[93]
Although independent analysts have cited the financial drag of this defective arrangement for many years, Congress did not address it until 2015—and then it merely restricted Medigap coverage of the Part B deductible and delayed that limited restriction until 2020 for newly enrolled Medicare beneficiaries. The CBO scored the savings from this timid tweak at a mere $400 million over the 10-year period from 2015–2025.[94]
Medicare’s coverage gaps are a product of its centralized structure in which benefits, treatments, and procedures are set by law, regulation, and politics. While the FFS program allows a senior a “choice of doctor,” there is no guarantee of a specific medical treatment or procedure: Medicare may not cover it. If Medicare does cover a medical treatment, it may be “covered” only under the specified conditions that the Medicare bureaucracy allows or determines to be “necessary and appropriate.” Doctors and patients can appeal a claims denial, but the backlog of these cases is approximately 500,000, and the waiting time for an appeals hearing can be 90 days for a Medicare patient and up to three years for a Medicare doctor.[95]
Moreover, Medicare has generally rejected medical claims, particularly in Part B, at a higher rate than that of most private health insurers. In a series of recent reports on Medicare and nine prominent private insurers, the AMA found that Medicare topped the list for claims denials in 2008 and 2013; ranked second in 2009, 2010, and 2011; and fell into third place in 2012.[96] Under Medicare’s claims appeals process, in fiscal year (FY) 2014, 39.5 percent of appeals resulted in fully or partially favorable decisions; 60.5 percent of appeals resulted in unfavorable rulings or were dismissed.[97]
Medicare claims have been denied for a variety of reasons: The medical services were not statutorily authorized, were impermissibly delivered outside of Medicare’s complex regulatory requirements, or were deemed medically “unnecessary or inappropriate.” For medical professionals, deviation from Medicare’s administrative directives has long posed risks of fines or penalties.[98] It still does.
Over the past 50 years, Medicare’s reimbursement process for new treatments, including medical technologies, has often been painfully slow, cumbersome, and mysterious.
- In July 1994, the U.S. General Accounting Office (now Government Accountability Office) reported that a decision to extend existing coverage for such a treatment could take anywhere from two months to a year. If the treatment or procedure was more complicated, such as a liver transplant, it could take several years. After the Medicare bureaucracy made an internal coverage decision, that decision had to be published in the Federal Register for “notice and comment,” normally a 60-day period. Assuming no serious objections from powerful stakeholders (special interests), the Secretary of HHS would publish a “final” rule. Depending on the circumstances, the GAO found that the rule-making requirements alone could add another nine to 12 months to the process.[99]
- In August 2000, the Lewin Group, an econometrics firm modeling health initiatives, similarly found that the adoption of advanced medical technologies in Medicare could take anywhere from 15 months to five years.[100]
With the emergence of Medicare Advantage plans and private Medicare prescription drug plans, including their provision of catastrophic coverage, seniors have better options than enrollment in traditional Medicare. For seniors today, a broad range of medical services, including preventive medicine, care coordination, and case management, is available in Medicare Advantage. Seniors also they have access to a broad array of drug therapies through private plans participating in Medicare Part D.
The Quest for Quality. Quality, as currently measured in traditional Medicare, is mixed. From 2010 to 2013, hospital mortality and (to a lesser extent) hospital inpatient safety improved.[101] Recent years also have seen slight improvement in home health care but mixed results in the administration of renal dialysis.[102]
President Barack Obama and congressional sponsors of the recently enacted Medicare physician payment reform insist that their legislative measures will improve the quality of Medicare services. With respect to the ACA, for example, hospital Medicare payment is to be tied to compliance with government-established quality standards. Under the new Hospital Value-Based Purchasing Program,[103] hospitals are to be paid or penalized on the basis of their performance in handling, among other things, certain medical conditions such as heart attacks and pneumonia. The HHS Secretary determines the standards for quality care and selects the measures that are used to grade and pay hospitals.
The ACA also creates the Hospital Readmission Reduction Program.[104] When Medicare patients seek readmission for a previously treated condition, the law will penalize hospitals with high readmission rates, and thus excessive costs, by reducing the Medicare payment for those hospital patients.
For doctors, the ACA adds a “quality of care” modifier to the Medicare fee schedule while giving the HHS Secretary broad authority to adjust the formula.[105] The law also would have extended and toughened the Physician Quality Reporting Initiative (PQRI) in Medicare, but that provision and its penalties were repealed by the Medicare Access and CHIP Reauthorization Act of 2015.[106]
Under MACRA, Congress consolidated three existing Medicare “value-based” performance programs into one program and created a new merit-based incentive payment system. Physicians will be able to participate in new “alternative payment models” (APMs), including private-sector payment models, to improve quality, and Medicare patients will have access to information on physician performance. The new law also authorizes the HHS Secretary to develop “quality measures” in collaboration with physicians and provides for “physician-developed clinical guidelines.” HHS Secretary Sylvia Burwell recently announced a CMS administrative initiative to ensure that 30 percent of all Medicare payments will be “value-based” by 2016, rising to 50 percent by 2018.[107]
The future of MACRA will depend on whether Washington policymakers can make the tough transition from appealing rhetoric to clinical reality. As Dr. John O’Shea, a practicing surgeon and senior fellow at The Heritage Foundation, has observed:
Value-based health care should be the goal of any health reform initiative. However, even with [the Sustainable Growth Rate] out of the way, there are major challenges to achieving that goal, including the lack of an agreed-upon, patient-centered definition of value; a shortage of meaningful performance metrics; and a deficiency of accounting systems capable of reflecting the true cost of delivering care.[108]
For many years, Medicare’s quality of care and the Medicare bureaucracy’s ability to ensure it have been recurrent issues.[109] The Medicare Payment Advisory Commission (MedPAC), the panel that advises Congress on Medicare reimbursement issues, has criticized traditional Medicare’s approach to quality measurement as too administratively burdensome for medical professionals and too heavily focused on process rather than outcomes. MedPAC also has concluded that Medicare’s approach too often distracts medical professionals from deploying their resources to address their own clinical assessment of quality problems.[110]
More recently, MedPAC’s concerns have been re-echoed by none other than Dr. Donald Berwick, formerly President Obama’s CMS Administrator and arguably the nation’s leading advocate for value-based care initiatives. Dr. Berwick warned policymakers to “stop excessive measurement” and abandon complex incentives:
We need a moratorium, I think, on complex incentive programs for individual health care workers, especially for doctors, nurses and therapists. If a program is too complicated to understand, too complicated to act upon by getting better, then it isn’t an incentive program. It’s a confusion program. It’s a full employment program for consultants.”[111]
The CBO’s evaluation of previous value-based payment efforts has shown them to be spotty and largely unimpressive.[112] It is still far too early to tell whether the combination of the ACA and congressional payment reforms will make a significant difference by improving patients’ medical outcomes and saving Medicare dollars.
The Obama Administration envisions Accountable Care Organizations (ACOs)—groups of medical professionals organized to deliver high-quality coordinated care and share in the savings—as a powerful driver of positive clinical change. For 2014, ACO performance is mixed: Eleven out of 20 “Pioneer” ACOs secured savings and Medicare bonus payments, and about half of the ACOs in the Medicare Shared Savings Program generated Medicare savings.[113] With respect to “hospital value-based purchasing,” the GAO recently found that implementation of this ACA provision has had no significant impact on Medicare savings or the provision of quality of care.[114] The Medicare trustees have concluded that “[t]he ability of new delivery and payment methods to lower cost growth rates is uncertain at this time.”[115]
The government’s task is inherently difficult. Part of the problem, as Dr. O’Shea argues, has been the lack of consensus on what exactly constitutes “quality” in medical care. There has also been a tension between academic medicine and government officials on quality issues, and these differences deepen in the concrete circumstances of clinical practice when individual physicians, with a sound knowledge of the medical history of their individual patients, deviate from what is officially prescribed, recommended, or sanctioned.
A related issue has been the speed and flexibility with which the Medicare bureaucracy can respond to quality problems. For Medicare patients, the problem is not that the bureaucracy will fail to produce a sufficient number of rules and regulations governing quality. The problem is that its clunky administrative processes may produce edicts that reflect the undue influence of special-interest politics or standards that are either irrelevant or out of date in a dynamic environment characterized by rapidly advancing medical technology and steadily improving clinical techniques.
The danger, in other words, is that the lowest-common-denominator definition of health care “quality”—the product of politically negotiated agreements among competing provider groups—could triumph over what is clinically or scientifically most appropriate, largely because that negotiated definition secures politically achievable levels of administrative payment.
Inefficient Pricing. Traditional Medicare remains a showcase of 1980s administrative pricing and price controls. “The reform of Medicare’s methods of paying hospitals and doctors,” says Professor Marmor, “reshaped the program’s politics, introducing what amounted to a new regulatory regime.”[116]
In 1983, Congress enacted the Reagan Administration’s proposal to create a prospective payment system (PPS) for Medicare hospitals. Under the PPS, Medicare paid hospitals a fixed fee for treatment of a patient based on the patient’s condition within a diagnostic related group (DRG), regardless of the actual cost of the care delivered. In the words of Professor Marmor, “it is a deep irony that the most consequential health policy innovation of the Reagan period—Medicare’s prospective payment method of DRGs—was an exceedingly sophisticated, highly regulatory form of administered prices.”[117]
The results were predictable. There was a cost shift from Medicare inpatient to outpatient care, patients were discharged prematurely, and payment standardization ignored crucial differences in case severity. As a result, readmission and remedial costs increased.[118]
In 1989, with the backing of the Bush Administration, Congress enacted a comprehensive reform of the Medicare physician payment system.[119] It had three major components:
- The Resource-Based Relative Value Scale (RBRVS), a new way to calculate the “value” of a physician’s labor based on a social science measurement of the inputs or “resources” (time, energy, effort, and practice costs) that go into providing any one of the approximately 8,000 services reimbursed under Medicare. Today, the RBRVS remains the foundation of the complex Medicare physician payment.
- A limit on “balance billing,” the amount a doctor could charge a patient over and above the Medicare approved charge, regardless of whether or not the patient would be willing to pay an extra amount for the physician’s service, clinical expertise, or professional experience: in other words, a direct price control on physicians’ services.
- A Volume Performance Standard (VPS) to cope with the expected fallout from the new price control regime. With controls on physicians’ service charges, Congress created powerful incentives for doctors to make up revenue losses by increasing the volume of their services. To prevent such volume increases, under the VPS, Medicare would establish a target for the annual rate of growth in the volume of services. If physicians exceeded the target, then the aggregate Medicare reimbursement would be reduced proportionately: the bigger the annual volume, the larger the annual payment reduction.
This congressional scheme suffered from a fatal contradiction: Any future reduction in general Medicare payment did nothing to prevent an individual doctor from increasing the volume of his particular services. The very prospect of future revenue losses, in fact, created even more powerful incentives for physicians to increase volume, and thus Medicare spending, to compensate for those expected losses.
In the Balanced Budget Act of 1997, Congress replaced its unworkable Volume Performance Standard with the Sustainable Growth Rate (SGR), a formula tying physician payment growth to economic growth. If Medicare physician spending exceeded an annual growth target, physician payment would be reduced proportionately. The SGR, mandating draconian annual payment cuts, also proved to be unworkable—an epic public policy failure. In 2015, Congress finally repealed it.
Looking back, the 1989 Medicare payment reform, particularly the RBRVS, was intended to establish a “fair and rational” pricing system that, among other things, would rectify the perceived imbalance between primary care physicians and specialists. In other words, the law was designed to be an instrument of taxpayer-financed income redistribution among medical professionals—an objective that it failed to achieve.[120]
The advocates of the 1989 reform also claimed that the Medicare RBRVS was a “scientific” method by which to determine the “objective value” of a physician’s service.[121] It also failed to achieve this quixotic objective. The RBRVS’s utility as a “scientific” basis of physician payment was soon undercut by its inherent methodological limitations and the powerful pressures of special-interest politics.[122] For example, in assigning “value” for the physician’s work elements of the RBRVS formula, the CMS relies on the AMA’s Relative Value Scale Update Committee (RUC). As the GAO recently reported, this panel’s largely opaque process is profoundly flawed because it “relies on the input of physicians who may have potential conflicts of interest with respect to the outcomes of CMS’s process.”[123] The GAO also concluded that the survey data used by the RUC are weak, subverting the accuracy of its Medicare recommendations.[124]
This is not surprising. Objective value cannot logically be derived from subjective determinations. According to Dr. Robert Berenson of the Urban Institute:
Now, with the benefit of 20-year hindsight, the Medicare Fee Schedule (MFS) is no longer viewed as rosily as when it debuted. While most concern has focused on the FFS incentive to increase service volume, close observers of the MFS are also concerned that the periodic updates have resulted in payments for some services that no longer reflect the underlying resource costs.[125]
For 50 years, Medicare’s administrative payment systems generated a flood of critiques, ranging from the GAO to health policy specialists and independent economists, reflecting a broad range of diverse political perspectives. They became tiresomely familiar. Medicare often paid too much or too little, or Medicare’s administrators did not have enough data, did not take into account the right factors, or failed to make the right calculations to set a “fair and rational” price for medical services. Adjustment, readjustment, or modification of complex formulas governing Medicare payment invariably overshot or undershot the mystical mark, with officials embarked upon a seemingly endless, dreamy quest for the “right price” somewhere far beyond the frontiers of the free market.
To this day, Medicare’s pricing problems continue to plague payment for high-profile services like hospitalization and inpatient prescription drugs. Between 2010 and 2013, for example, Medicare overpaid hospitals by $2.6 billion for drugs because of a flaw in the program’s payment formula.[126] In 2015, the HHS Inspector General found that Medicare payments for infusion drugs were double what they should have been, costing taxpayers an estimated $251 million, largely because of Medicare’s flawed methodology and outdated data.[127] Yet administrative “fixes” often create new administrative problems. The Obama Administration’s proposed 2016 rule for Medicare Part B drug pricing, for example, would threaten provision of drugs at smaller medical practices, inconvenience patients, and shift costs to more expensive hospital settings.[128]
Given Medicare’s long experience, Congress would do well to heed the advice of Professors Michael Porter of Harvard University and Elizabeth Teisberg of the University of Virginia: “The methodology for top-down price setting can be improved, but never perfected. Administered prices will never really work.”[129]
Subversion of Professional Independence and Restriction of Patient Freedom. Enacting Medicare 50 years ago, Congress stipulated that:
Nothing in this Title shall be construed to authorize any federal officer or employee to exercise any supervision or control over the practice of medicine or the manner in which medical services are provided, or over the selection, tenure or compensation of any officer or employee of any institution, agency, or person, providing health services; or to exercise any supervision or control over the administration or operation of any such institution, agency, or person.[130]
This original Medicare provision—still on the books—is crystal clear. Nonetheless, Congress has enacted changes over the past 50 years that have circumvented the professional autonomy of physicians and involved federal officials ever more deeply in medical practice.
Members of Congress often say that they regard the traditional doctor–patient relationship as primary and sacred. In fact, Congress has undermined it.
Section 4507 of the Balanced Budget Act of 1997, for example, imposed an unprecedented statutory restriction on the right of doctors and patients to enter into private agreements outside of Medicare to deliver services covered by program.[131] Congress permitted Medicare patients to enter into private agreements with doctors and pay them directly for any medical services covered under Medicare—but only if the doctor signed an affidavit of the contract, submitted that affidavit to the Department of Health and Human Services within 10 days of the agreement, and refrained from billing Medicare for the treatment of any other Medicare beneficiary for a period of two years. The Clinton Administration insisted on this provision, which mirrored a similar provision of the failed Clinton health plan of 1993.
Not only was Section 4507 insulting to doctors and patients, spurring litigation by conservatives and privacy advocates, but it also contributed to a great deal of confusion.[132] Though the Medicare bureaucracy has issued subsequent regulations softening the implementation of this bizarre provision, it remains on the books.
For Congress and the Clinton Administration, the 1997 restriction had its desired effect. Realistically, very few physicians could give up Medicare practice for two full years, particularly if they practiced in a state like Florida that has a large number of Medicare patients. With demographic and fiscal pressures on the program mounting, and with physician and patient frustration in navigating traditional Medicare’s bureaucratic obstacle course growing, renewed efforts to repeal the 1997 restrictions could generate broader popular support.
In the meantime, the Affordable Care Act of 2010 will have profound effects on physicians’ practices, amounting to a significant deviation from Medicare’s original statutory restrictions on federal interference. CRS analysts have concluded that:
[The law] makes several changes to the Medicare program that have the potential to affect physicians and how they practice in ways both small and large, immediately and over time. While some of the provisions have clear and direct consequences, for instance altering physician reimbursement right away, others have the potential to influence how physicians might practice in the future by changing the incentives to encourage improvements in the organization and delivery of care.[133]
Generation of Waste, Fraud, and Abuse. Medicare’s very size and complexity—as the GAO has repeatedly insisted—render it vulnerable to waste, fraud, and abuse.[134] Because of the bureaucracy’s seeming inability to monitor payments effectively, the program routinely incurs this financial damage. In 2014, for example, The New York Times reported that Medicare fraud amounted to $60 billion yearly, or roughly 10 percent of Medicare’s annual costs.[135] Two years earlier, former Attorney General Eric Holder estimated Medicare fraud at between $60 billion and $90 billion a year.[136]
The persistence of Medicare fraud is not attributable to a lack of effort by federal law enforcement. In FY 2014 alone, the Department of Justice opened 924 criminal and 782 new civil health care fraud investigations, the FBI disrupted 605 fraudulent operations, and the HHS Inspector General’s investigations resulted in 867 criminal and 529 civil actions.[137]
Over the past 50 years, Washington’s standard response has been to spend hundreds of millions of dollars, beef up the HHS Office of Inspector General and the Department of Justice, hire more personnel, get better software, conduct more audits and investigations, and impose tougher fines, penalties, and jail terms. In 1998, Congress even created a bounty program for seniors to check out doctors and other medical professionals to find and report fraud, with rewards ranging from $100 to $1,000 for recovery of funds.
While prosecuting and punishing the taxpayers’ enemies, Congress should not ignore root causes. Medicare contractors process millions of claims each business day for tens of billions of dollars, governed by complex payment formulas, to pay hundreds of thousands of medical providers. Medicare’s weakness in controlling wrongful payment is exacerbated by an outdated third-party structure, a bureaucratic process that dispenses a seemingly unlimited flow of taxpayers’ dollars and is ungoverned by powerful market incentives that otherwise would encourage plans and providers to combat waste, fraud, and abuse to protect their competitive positions. Medicare’s structural defects virtually invite and nourish these costly pathologies.
Beyond outright fraud, Medicare routinely reports problems of “improper payment.” For 2015, the HHS Office of Inspector General estimated $43.3 billion in such payments.[138] Medicare codes for physician reimbursement cover over 8,000 medical procedures, and each is subject to regulatory conditions governing reimbursement. In that regulatory environment, clerical errors are common, and doctors can be fined for clerical errors. The worst of it is that, once again, the system’s very complexity enables clever fraud artists to hide in the lush bureaucratic overgrowth of these paperwork jungles, while honest doctors can get caught up in an investigation simply because of their own or their staffs’ clerical errors.
The intersection between medical arts and science and medical payment is difficult for government officials to navigate. When is a Medicare payment for a treatment or procedure improper? Is it improper merely because it falls through a slim crack in Medicare’s regulatory concrete, thus forcing a doctor to choose between adhering to a fixed rule and adhering to the physician’s ethical obligation to his or her patient? In a clinical setting, as noted, there are and can be honest disagreements, even among highly trained and experienced medical professionals, as to whether or not a particular medical treatment or procedure for a patient is or is not “medically necessary.” Policymakers should also keep in mind that there is a vast difference between fraud and an “improper” payment based on a clerical or coding error.
Threatened Access to Care. Over the next 50 years, Medicare enrollment is projected to increase from more than 57 million to more than 102 million.[139] Moreover, as enrollment surges to almost 82 million over just the next 15 years, the United States will also be facing a doctor shortage. In a 2015 report released by the Association of American Medical Colleges, researchers estimate that by 2025, the shortage of physicians will range from more than 46,000 to more than 90,000.[140]
Today, nearly all of America’s physicians care for Medicare patients, but newly retiring seniors still have reason to be concerned.
- The National Center for Health Statistics, an HHS agency, recently reported that 83.7 percent of office-based physicians accept new Medicare patients;[141]
- According to a report published in Health Affairs in 2012, an estimated 17 percent of Medicare doctors no longer take new Medicare patients;[142]and
- A major survey conducted on behalf of the Physicians Foundation in 2014 found that 24 percent of physicians limit their Medicare practices.[143]
America’s doctors are also being asked to do more for less. According to the Physicians Foundation survey, 81 percent of doctors say that they are overextended or working at full capacity.[144] Analysts at the Center for Studying Health System Change examined physician income patterns between 1995 and 2003 and found that average physician income appeared to be on the rise but, once adjusted for inflation, actually showed a real decline. For all physicians, the decline was 7.1 percent; for surgical specialists, it was 8.2 percent; and for primary care doctors, it was 10.2 percent.[145]
In this context, Congress should realize that the huge Medicare program has a direct impact on private-sector medical pricing. According to economists Jeffrey Clemens of the University of California at San Diego and Joshua Gottlieb of the University of British Columbia, “Over the medium to long run, we estimate that a $1 decrease in Medicare’s fees led to a $1 decrease in private payments. Private sector responses to these broad-based rate changes appear to unfold over several years.”[146]
Congressional sponsors of MACRA believed that their 2015 legislation boosting Medicare spending until 2025 would improve Medicare for both doctors and patients. The Medicare trustees, however, have already dampened that expectation:
The Trustees anticipate that physician payment rates reimbursed via the PFS under current law will be lower than they would have been under the SGR by 2048 and will continue to worsen thereafter. Absent a change in the delivery system or level of update by subsequent legislation, the Trustees expect access to Medicare-participating physicians to become a significant issue in the long term under current law.[147]
The American medical profession is subjected to an aggressive and intrusive set of regulatory initiatives, reporting requirements, and payment penalties, as well as the imposition of a complex new coding system, the ICD-10.[148] In addition, physicians and other medical professionals labor under the threat of significant Medicare reimbursement reductions, to be enforced (eventually) by the ACA’s Independent Payment Advisory Board. In an October 2014 letter to former CMS Administrator Marilyn Tavenner, Dr. James L. Madara, Executive Vice President of the AMA, observed that:
No other segment of the health care industry faces penalties as steep as these and no other segment faces such challenging implementation logistics. The tsunami of rules and policies surrounding the penalties are in a constant state of flux due to scheduled phase-ins and annual changes in regulatory requirements. In fact, the rules have become so complex that no one, often including the staff in charge of implementing them, can fully understand and interpret them. In many instances, physicians will be held accountable for expenses that are completely outside their control, and those treating Medicare’s frailest patients are most at risk for incurring penalties.[149]
For decades, Congress and successive presidential Administrations attempted to control Medicare spending through payment reductions and, later, through price fixing. The ACA reinforced this payment reduction policy with a vengeance; based on the latest CBO estimate, the law’s scheduled Medicare payment reductions will yield “savings” amounting to $802 billion over the next 10 years. This will include cuts in payments to Medicare Advantage plans, hospitals, nursing homes, home health agencies, and even hospice care facilities.
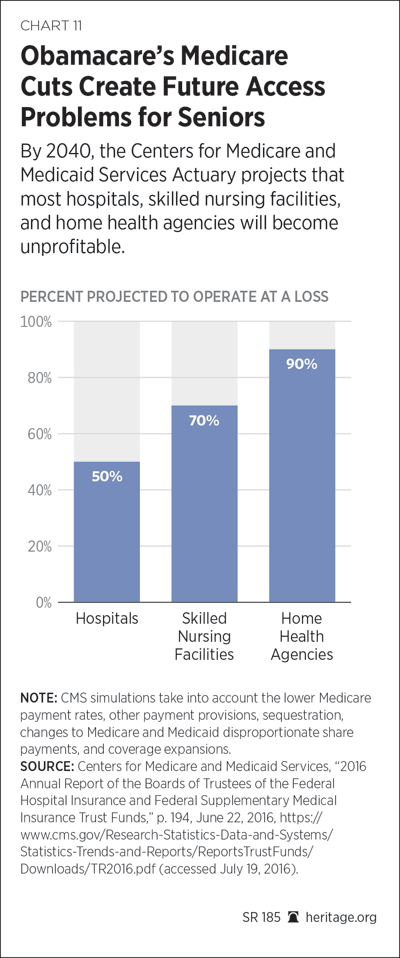
Today, Medicare payment for inpatient hospital services is well below private market rates. “By 2040,” according to the Medicare trustees in their 2016 report, “simulations suggest that approximately half of hospitals, 70 percent of skilled nursing facilities, and 90 percent of home health agencies would have negative total facility margins, raising the possibility of access and quality of care issues for Medicare beneficiaries.”[150]
Faced with these Medicare Part A payment reductions, it is likely that affected medical professionals and institutions would cut back on their Medicare practice, withdraw from the program, or shift their business elsewhere. Cuts in payments for medical services that patients depend on will affect patients themselves, not just providers. Since 2010, the Office of the Actuary at HHS has regularly warned that the ACA payment reductions would “jeopardize” patient access to care.
Elements of Medicare Reform
Medicare cannot and will not continue as it is today. The good news is that there is no shortage of good policies that can improve the traditional program and pave the way for a better Medicare future based on the free-market principles of patient choice and market competition.[151]
In pursuing Medicare reform, Congress should set clear goals. At the very least, a Medicare reform agenda should accomplish four overriding objectives:
- Simplify the program. Congress can start to reduce Medicare’s complexity by combining Medicare Parts A and B into a single plan, complete with a single deductible and uniform coinsurance. This simplification should accompany serious Medigap reform and the addition of catastrophic protection. Such a proposal might even win strong bipartisan support. According to Karen Davis and colleagues at the Commonwealth Fund, a prominent liberal think tank, for example, “The fragmentation of coverage into separate parts for hospital (Part A) and physician (Part B) and prescription drugs (Part D) adds to the administrative cost, complexity, and confusion for beneficiaries, and hinders coordination of care.”[152]
-
Restore patient freedom and government noninterference with medical practice. Congress should take steps to restore Medicare’s original statutory guarantee of physicians’ professional independence from government control. It can begin with implementation of the recently enacted Medicare physician payment reform law by making sure, through keen and intense congressional oversight, that medical and not government professionals determine standards for clinical improvements, medical protocols, or quality and that any performance standards are compatible with that principle. In short, lawmakers should work to reverse recent trends, including the regulatory excesses of the Affordable Care Act, that accelerate greater government control or supervision of the practice of medicine.
Congress should also restore the personal freedom of Medicare patients to enter into private agreements, or contracts, with physicians of their choice for the provision of any legal medical service outside of the Medicare program without those physicians having to risk financial punishment. The statutory requirement that doctors drop out of Medicare entirely for two years when engaging patients in such a contract is clearly intended to undermine private contracting as a patient option. Three former AMA presidents, Drs. Donald Palmisano, Daniel S. Johnson, and William Plested, prescribe exactly the right remedy: “The right of patients to privately contract with physicians to ensure they have the medical care they want, without penalty—regardless of what the government pays—must be recognized and protected.”[153]
- Reduce taxpayers’ costs. Congress can make several structural changes that would reduce current and future taxpayers’ costs while enhancing the financial status of the traditional Medicare program. Many of these changes have attracted serious bipartisan support. Specifically, Congress should:
- Increase the normal age of eligibility. With seniors living longer, lawmakers should raise the age of eligibility from 65 to at least 68 over a period of 10 years and index it to life expectancy. Although there have been disagreements about the appropriate age of Medicare eligibility, there has been a strong bipartisan consensus that it should be increased.
-
Further reduce premium subsidies based on income. As noted, seniors normally pay standard premiums amounting to roughly 25 percent of total Medicare premium costs, with the remainder financed by tax-free subsidies from general revenues. Those with an annual income in excess of $85,000 (couples with an annual income in excess of $170,000) pay higher Part B and Part D premiums, ranging from 35 percent up to 80 percent of total Medicare premium costs. Today, these recipients account for just 6 percent of the total Medicare population. Congress should reset these income thresholds and require seniors with an annual income in excess of $55,000 (couples with an annual income in excess of $110,000) to start paying higher premiums.[154] By adopting this initial income threshold, Congress would increase the number of Medicare recipients paying higher premiums to roughly 10 percent of the total Medicare population, and the wealthiest among them (about 3 percent) would pay their own way entirely.[155]
The premium payment structure for upper-income Medicare recipients should also be reformed. In designing a new income-based Medicare subsidy program, Congress should junk the cliff-like premium jumps—ranging from 35 percent to 80 percent of the total Medicare premium—and substitute small and incremental payment increases in line with increases in annual income, resulting in a gradual slope of increased premium payment.
There has also been strong bipartisan support for reducing taxpayer subsidies for the wealthiest Medicare recipients. President Obama, for example, proposed that 25 percent of the Medicare population pay higher Part B and Part D premiums above the standard rate.[156]
- Gradually increase the standard Medicare beneficiary share of the total payment of Part B and Part D premiums. Medicare recipients, as noted, originally paid 50 percent of the total premium, and taxpayers paid 50 percent. Over the years, Congress shifted those premium costs to the taxpayers, who today fund approximately 87 percent of Medicare’s total annual costs. To reduce the taxpayers’ burden, Congress should gradually increase Medicare recipients’ share of total premium costs from 25 percent to 35 percent while retaining Medicare’s existing “hold harmless” rules designed to protect low-income seniors.[157] This could be done at the rate of 2 percent per year over a five-year period or 1 percent a year over a 10-year period.
- Establish a temporary Part A premium. The Part A premium would be operable only for any year in which the Hospital Insurance (HI) trust fund is facing a cash deficit, and the premium amount would be calibrated annually to cover the cost of that projected deficit. By 2021, the Medicare trustees are once again projecting a return to annual cash deficits in the HI program. Enactment of a modest premium to cover the shortfall for that year would be a prudent response.
- Replace Medicare Advantage payment cuts with market-based bidding. Specifically, Congress should change Medicare Advantage’s payment system to one that is based exclusively on regional market-based bidding, separate and apart from existing Medicare’s fee-for service benchmarks.[158] In broad outline, this general policy has been endorsed by President Bill Clinton in 1999, President Obama in 2009, and more recently by analysts at the Brookings Institution.[159]
-
Integrate traditional and competitive Medicare into a single program. Congress should require a simplified traditional Medicare plan that competes head-to-head with Medicare Advantage plans and other private options, as well as employment-based plans.[160] As noted, the majority of seniors already are enrolled in a Medicare defined-contribution program, whether through Medicare Advantage or through Part D. While this funding is not normally referred to as a form of premium support, for all practical purposes, that is what it is. Congress should expand this financing system, establish a level playing field, and intensify competition for all plans and providers. Aside from being a powerful engine of economic efficiency, a genuine market based on personal choice and provider competition would deliver superior value, produce better quality, and engender higher levels of patient satisfaction.
Under such a reform, the government contribution to an enrollee’s premium could be based on regional competitive bidding among all health plans, including traditional Medicare, to offer a basic package of health benefits consisting of the standard benefits of Parts A, B, and D or their actuarial equivalent. All plans would be required to offer catastrophic coverage, just as all Medicare Advantage plans do today. A Medicare recipient who purchased a plan that was less than the amount of the government contribution could keep that money as a cash rebate or roll the funds over into a tax-free health savings account. A recipient who purchased a plan that exceeded the government contribution would pay the additional amount in premium.
Congress could further refine the formula for the government contribution and adjust it for income, just as it adjusts Medicare Parts B and D premiums today, and continue to improve on the Medicare Advantage risk-adjustment mechanisms.[161] Because of the pre-existing infrastructure of such a market embodied in Medicare Parts C and D, including the process for dissemination of comparative plan information and application of risk-adjustment mechanisms, this transformation could easily be phased in over three to five years or even less. The CBO found that in such a competitive system, compared to traditional Medicare, private plans could deliver the same level of benefits at a lower price and estimated that savings over just six years could range from $69 billion to $275 billion, depending on the assumptions used.[162]
Given its sheer size, such a market-driven change in Medicare would have a huge impact on other sectors of America’s vast health care economy. Moving to Medicare premium support, thereby compelling health plans and providers to compete for customers on a single level playing field, would have enormous positive consequences. Patient choice, clarity in pricing, and transparency in performance, combined with intense competition among plans and providers, would ensure more direct accountability to patients. Such a new market would not only control cost, but also stimulate innovation in health plan benefit designs. From a financial standpoint, it would generate serious savings for seniors and other taxpayers alike.[163] Premium support would also:
- Result in less government bureaucracy and regulation.[164] In such a system, competing health plans, not the Medicare bureaucracy or its agents, would contract with doctors and hospitals, determine their employment or conditions of participation, establish provider rates and conditions of reimbursement, collect premiums and pay claims, easily incorporate new benefits, and oversee the quality of medical services.
- Stimulate greater clinical innovation and progressive improvements in care delivery. As traditional Medicare struggles to promote innovation through administrative payment manipulations, the Medicare Advantage program has already pioneered case management, care coordination, and the expansion of preventive care, and Medicare Part D has provided Medicare patients with a broad array of drug therapies that rivals that available to federal workers and retirees in the Federal Employees Health Benefits Program (FEHBP).[165]
- Discourage the routine congressional micromanagement and sharply reduce or eliminate the special-interest politicization of pricing and procedures that plague Medicare today. Decision-making would be radically decentralized—diffused among millions of enrollees seeking the best value for their Medicare dollars—and market pricing would reward the most efficient medical plans and providers. This would be a refreshing break from the routine machinations of powerful special-interest lobbyists who use the program as a mechanism of income redistribution among providers at the expense of seniors and taxpayers alike. Competing plans would be directly accountable to patients and would have powerful incentives to make fair and rational payments to doctors and other medical professionals while avoiding wasteful spending. They also would have powerful new market incentives to combat fraud and abuse simply because any failure to do so would directly detract from their bottom line and undercut their market share.
Conclusion
Over the past 50 years, Medicare has achieved indisputable successes in providing seniors with continuous coverage and a strong measure of financial security. Now, in the 21st century, Congress and successive presidential Administrations need to undertake reforms that will not only improve Medicare to secure value for patients, but also enhance the program’s solvency and reduce its growing burden on current and future taxpayers.
Left unreformed, Medicare will continue to put intense pressure on the federal budget, contribute to coming deficits, and generate massive future debt. As American Enterprise Institute Senior Fellow Robert Helms has observed, “If there is a lesson to be learned from the history of Medicare, it is that although government-financed health care has enormous appeal to most politicians, the popularity of a program does not repeal the laws of economics.”[166]
There are strong grounds for optimism. Medicare has successfully used new systems of defined contribution for payment of comprehensive private health plans (Medicare Part C) and prescription drug coverage (Medicare Part D). Both programs have demonstrated the bounteous benefits of consumer choice and genuine competition.
Congress can take the final step and subject hospital and physician benefits to the same intense market forces of personal choice and provider competition that today govern private plans and prescription drugs. Reform would reduce bureaucracy and red tape and further stimulate innovation in benefit design and care delivery. Such a reform would not only apply a potent remedy for Medicare’s chronic conditions, but also help to secure fiscal wellness for the program and the nation.
—Robert E. Moffit, PhD, is Senior Fellow in the Center for Health Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.