Americans are engaged in an intense national debate over the Patient Protection and Affordable Care Act of 2010 (ACA, popularly known as “Obamacare”). Despite President Barack Obama’s glowing account of his “signature” accomplishment, the ACA’s six-year record demonstrates that the legislative product he signed into law is deeply—and in many respects irreparably—flawed. Obamacare is bedeviled by poor performance in a number of vital areas:
- Increased costs for individuals, families, and businesses;
- Resumption of excessive health care spending and middle-class taxation; and
- A seemingly endless series of managerial failures or unanticipated consequences.
The ACA is a formidable engine of concentrated bureaucratic power and control, yet its future is clouded by persistent unpopularity.
Persistent Unpopularity
The ACA was the product of a narrowly partisan process.[1] Before final passage, during the months of February and March 2010, not one major survey recorded majority support for the legislation.[2] In the congressional elections of 2010 and 2014, during which the law was a major issue, opponents were overwhelmingly victorious at the polls.
After securing enactment of the law in the teeth of popular opposition, Administration officials and their allies in Congress and elsewhere repeatedly claimed that the American people would come to like the ACA over time.[3] Yet, according to a recent compilation of survey data from RealClear Politics, 49.3 percent of Americans oppose the law compared to 39 percent who favor it.[4]
This is not surprising. In 2011, Heritage Foundation analysts, in a series of 15 papers covering the ACA’s main provisions, outlined the law’s likely impact on the financing and delivery of care.[5] By 2014, many of those predictions had come true.[6] In fact, the prospect of rising costs, disruption of existing coverage, and metastasizing bureaucracy—dynamics that also doomed the Medicare Catastrophic Coverage Act of 1988 and undermined the Clinton health plan of 1993—have characterized the ACA’s rocky implementation.[7]
Practical Concerns
Americans’ health care worries are real, and their concerns are practical. For the overwhelming majority of Americans, the right policy goal is making health care more affordable.[8] Today, however, the “typical family” pays about 35 percent of their income for health care.[9] The temporary slowdown in health spending, which started in the early 2000s, is over, and businesses, individuals, and families are once again threatened with higher health care costs. Since 2013, premiums and deductibles in the non-group market have jumped dramatically, while millions have lost their previous coverage, notwithstanding high-profile presidential promises that they could keep it.
Bureaucracy, red tape, and paperwork still plague the financing and delivery of care, clogging pathways to innovation, increasing costs, and frustrating individuals and families, employers and employees, and doctors and patients alike. Indeed, the ACA’s administrative requirements are making these long-festering problems progressively worse.
The Administration cites the law’s five-year expansion of insurance coverage: 20 million additional enrollees.[10] Major Medicaid expansion is arguably the law’s biggest achievement,[11] though persons enrolled in Medicaid often have no alternatives and have only limited access to doctors and medical specialists. The professional literature shows that Medicaid’s performance in care delivery is substandard.[12]
Given the sheer magnitude of the ACA’s insurance subsidies, it is odd that exchange enrollment is falling well short of official expectations. In 2015, the Congressional Budget Office (CBO) reported that 9.5 million persons enrolled in the exchanges rather than the expected 11 million; for 2016, the CBO projects 13 million exchange enrollees, a big drop from the agency’s earlier projection of 21 million.[13] Moreover, 2014 data show that increased enrollment in exchanges has been accompanied by roughly equal decreases in job-based coverage.[14]
Poor Performance
The functionality of key ACA provisions is a recurrent issue. Timothy Jost of Washington and Lee University and Harold Pollack of the University of Chicago, prominent academic supporters of the ACA, nonetheless acknowledge: “The ACA undertook from the beginning an ambitious reform agenda, but some of its approaches have turned out to be ineffective, poorly targeted, or not ambitious enough to address deeply rooted problems.”[15]
The law’s most publicized operational problems surfaced with the disastrous October 2013 rollout of healthcare.gov, the federal government’s website for enrollment in the health insurance exchanges. It was a technical and managerial failure of mammoth proportions. The Department of Health and Human Services (HHS) Office of Inspector General found multiple managerial failures damaging the website launch: “Most critical were the absence of clear leadership, which caused delays in decision-making, lack of clarity in project tasks, and the inability of CMS [the Centers for Medicare and Medicaid Services] to recognize the magnitude of the problems as the project deteriorated.”[16]
Technical problems can be resolved by technical fixes, and managerial messes can be cleaned up with new management, but the ACA’s problems have multiplied well beyond the functionality of the federal website or poor management of an admittedly complex set of interlocking programs. Fundamentally, they are problems of legislative design, particularly in the regulation of health insurance:
- An overly complex system of excessive insurance subsidies,
- Health benefit mandates and rating rules that greatly increase health insurance costs, and
- A flawed arrangement for protecting persons from coverage exclusions for preexisting medical conditions.[17]
Grace-Marie Turner of the Galen Institute, a critic of the ACA, has identified 70 administrative, legislative, and judicial changes in the law, some quite large, that attempt to compensate for its design flaws or forestall unacceptable consequences.[18] “In short,” observes Christopher Conover, a professor of health policy at Duke University, “the law being implemented today is in many ways quite different than the law passed by a very temporary super-majority of Democrats back in 2010.”[19]
Consider, for example, the large long-term care program: the Community Living Assistance Services and Supports (CLASS) Act. Based on the Administration’s own initial assessment, it was not and could not be financially viable, and Congress, with the acquiescence of the Administration, ended it in 2012, thus precipitously erasing the anticipated collection of tens of billions of dollars in revenues within the initial 10 years of the ACA’s implementation—monies crucial to the Administration’s stated goal of deficit reduction.
Consider also the law’s government health insurance exchanges, heavily regulated and federally supervised health insurance mechanisms that are markedly different in goals and functions from market-based exchanges.[20] Six years after the law was enacted, only 13 states are running their own exchanges—a fairly poor showing for a taxpayer cost of over $5 billion—and a number of state efforts have failed in a spectacular fashion.[21]
There are other flawed ACA creations. More than half of the law’s nonprofit co-op health plans, heavily financed with taxpayer-backed loans and designed to enhance competition in the exchanges, have collapsed.[22] Similarly, the multi-state plan program, creating a special class of plans administered by the U.S. Office of Personnel Management (OPM), is also performing well short of expectations.[23]
The law’s health insurance subsidy program, encompassing both premium- and cost-sharing assistance, is mind-numbingly complex and excruciatingly difficult to administer. The amount of an enrollee’s subsidy depends not only on the person’s eligibility and income category, but also on changes in income over the course of the year, family size, the cost of the specific exchange benchmark plan in the person’s county of residence, and completion of the necessary paperwork to secure the assistance.
While low-income enrollees in the exchanges are supposed to be insulated from rising premium costs (and many are), incorrect income reporting or flawed data collection has resulted in 50 percent of recipients owing money back to the government.[24] Investigating the program, the U.S. Government Accountability Office (GAO) found data inconsistencies among 431,000 enrollees, accounting for $1.7 billion in 2014 subsidies, as well as inadequate protections against fraud.[25] The program is also under congressional scrutiny for the wrongful transmission of an estimated $750 million in taxpayer subsidies to illegal aliens.[26]
Finally, there are the law’s unprecedented mandates. In 2014, the individual mandate forcing Americans to buy federally approved health coverage became effective, but the seeming reluctance of the Obama Administration to enforce it vigorously was soon evident in various exemptions and delays.[27] In 2016, based on official estimates, approximately 90 percent of an estimated 30 million uninsured would not be forced to pay the penalty because of multiplying exemptions.[28]
Likewise, in 2014, the Administration delayed the reporting and penalty provisions of the employer mandate as well as the politically unattractive Medicare Advantage (MA) payment cuts. Even prominent congressional “progressives” have reversed course on the wisdom of MA payment reductions. Sixty-one Senators and more than 300 House Members are on record against cuts in the popular program.[29]
Detailed Control
The Patient Protection and Affordable Care Act of 2010 is arguably the largest and most comprehensive social legislation in American history. In 908 pages of statutory text, organized in 10 titles, its prescriptions cover a broad range of big topics:
- The structure and operations of the health insurance market;
- The administration of public programs (with 165 sections affecting Medicare alone);
- Health care delivery reforms; and
- The training and recruitment of the health care workforce.
The result: Virtually every major decision in the health care sector of the American economy is either made or constrained, directly or indirectly, by federal officials.
Under Title I, federal officials define the content of health insurance coverage, including required medical treatments, procedures, and preventive health care services. Federal officials enforce permitted levels of coverage as well as the officially acceptable level of premiums. With certain statutory or administrative exceptions, all Americans are legally required to provide or enroll in federally approved insurance coverage or pay a tax penalty for refusing to provide such coverage as an employer or to enroll in such coverage as an individual. Federal officials enforce rules governing insurance rating, co-payments and deductible levels, and allowable profit and administrative expenses. Private health insurance is “private” in name only.[30]
The ACA has also effected a massive erosion of the states’ traditional authority over health insurance regulation. Federal officials establish or supervise health insurance exchanges for the purchase of health plans.[31] In 2017, the law provides for a waiver from federal rules for state experimentation if, and only if, the Secretary of Health and Human Services should grant such a waiver. Even so, the scope of the ACA waiver is limited.[32]
Top 10 Reasons Why the ACA’s Future Is Uncertain
The ACA secures a massive centralization of power in Washington, yet this compromises the federal government’s own efficiency and effectiveness. As Dr. Joseph Antos of the American Enterprise Institute and his colleagues have observed:
The fundamental problem with reliance on centralized control over a sector of the economy as complex and vast as health care is that no person or bureaucracy could possess the requisite knowledge to properly set the dials of control to achieve the best balance of cost and quality. Moreover, what is understood about effective medical care is changing far too rapidly for a government bureaucracy to keep up.[33]
Not surprisingly, for sound philosophical reasons that are deeply rooted in America’s rich political culture of personal liberty, those Americans who opposed enactment of the ACA have expressed profound aversion to government control of their health care decisions.[34] Beyond these practical and philosophical reasons, there is no mystery why Americans, on everyday matters that directly concern them, continue to oppose the law. For example:
Reason #1: Despite the President’s repeated promises, rising insurance costs continue to burden businesses and families.
At the very inception of the debate, President Obama repeatedly insisted that American families would experience an annual reduction of $2,500 in their health costs.[35] During the 2009 debate, Jonathan Gruber, MIT professor of economics and an Administration adviser, also predicted, “What we know for sure is the bill will lower the cost of buying non-group health insurance.”[36]
From the beginning, the President’s claim of a premium decline was unsupported by the data. During the 2009 debate on the law, the CBO initially estimated that premiums in the individual market would increase between 10 percent and 13 percent.[37] For the vast majority of Americans still enrolled in the huge employment-based health insurance markets, the Office of the Actuary at the Centers for Medicare and Medicaid Services reported in April 2010 that the health law’s new taxes on health insurance, drugs, and medical devices would also translate into higher group insurance premiums.[38]
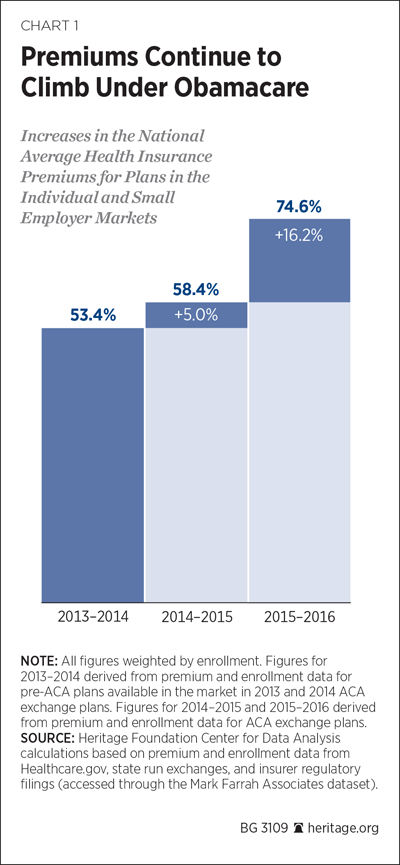
Rate Shock. In 2014, the first year of full implementation of the Title I provisions governing health insurance, Americans enrolled in the exchanges experienced premium rate shocks. Based on the data in the individual market over the 2013 to 2014 period, enrollees’ 2014 premiums, reflecting the new mandates and regulations, generally increased in most states of the Union, though increases varied:
- For 27-year-olds, premiums in 11 states more than doubled;
- For 50-year-olds, there was a premium increase of 50 percent or more in 13 states; and
- In 14 states, premium increases were more modest: between none and 25 percent.[39]
Within the ACA exchanges, narrow network plans also flourished—an unpleasant surprise for patients who wanted broader access to doctors and other medical professionals.[40]
In 2015, the rate of growth in premiums declined. While the average national premium increase in the exchanges was 5.3 percent, there was wide variation among the states.[41] In New York and Ohio, for example, the average premium increases were 2 percent and 11 percent, respectively.
For 2016, insurance companies expect “higher-than-expected” premium costs in the exchanges.[42] HealthPocket, a national firm comparing rates and benefits, reports that insurers in 45 states have requested an average premium rate increase of 12 percent.[43] The CBO recently confirmed this general upward trend: “Insurance premiums—the payments made to buy that coverage by enrollees or by other parties on their behalf—are high and rising.”[44]
Premium growth rates vary between group and non-group coverage, and the CBO is generally conservative in its estimates. For group coverage, the CBO projects that premium growth will accelerate over the period from 2016 to 2025, increasing by “nearly” 60 percent.[45] For non-group coverage in the exchanges, between 2016 and 2018, the CBO estimates that premiums for the basic “silver” plans (the benchmark plans in the ACA exchanges) will grow about 8 percent annually on average; after 2018, they are projected to rise in line with employment-based plans: roughly between 5 percent and 6 percent per annum on average.[46]
Reason #2: The ACA generates big and surprising out-of-pocket costs.
Beyond premium increases, there are deductible costs. There is generally an inverse relationship between premiums and deductibles. Choosing a low-cost premium plan in the health insurance exchanges usually means paying much higher deductibles. For many persons, the trade-off is perfectly reasonable, but the law imposes costly comprehensive benefit requirements and insurance rules, so for many middle-income persons, given that there is no legal alternative, the choice of insurance is constrained. Urban Institute analysts, though strongly supportive of the ACA, note the problem:
Although coverage has increased significantly thus far, fewer people than expected may sign up in the future if they determine that they are paying premiums for plans that require substantial amounts of cost-sharing. For many moderate-income people, particularly those in good health, the high cost-sharing requirements may not seem worth the premiums paid to get them.[47]
Families USA, a prominent liberal advocacy group and also a strong supporter of the law, has likewise reported that as a general matter, too many lower- and middle-income persons purchasing exchange plans found the deductibles and other out-of-pocket costs discouraging and went without care.[48]
It is a curious paradox that the ACA has generated monumental growth in high-deductible health plans, the very type of coverage that progressives have long found unpalatable and that are sometimes denounced as “junk” insurance. In the exchanges, as of March 2015, almost 90 percent of persons were enrolled in lower-cost silver or bronze health plans. Silver plans had an average deductible of $2,500, and bronze plans had deductibles exceeding $5,300 for single coverage.[49] About half of all workers in employment-sponsored coverage, by contrast, have an annual deductible of roughly $1,000 or more.[50] The high-deductible sticker shock has doubtless most affected those persons who have lost employer-based coverage.
As with ACA plan premiums, as noted, there is a taxpayer subsidy for plan deductibles and other out-of-pocket costs for income-eligible persons enrolled in the exchanges. These special subsidies are available only to enrollees who choose a silver-level health plan, which means that the plan must pay 70 percent of the average enrollee’s total medical expenses for covered benefits, with the enrollee paying the rest through deductibles and co-payments. In comparison, the actuarial value level for a bronze plan is set at 60 percent, and the more expensive gold and platinum plans are set at 80 percent and 90 percent, respectively.
Under the law, a premium subsidy is available for a person with an annual income of between 100 percent ($11,770) and 400 percent ($47,080) of the federal poverty level (FPL). The cost-sharing subsidies covering deductibles and other out-of-pocket costs are limited to a person with an annual income of between 100 percent and 250 percent ($29,425) of the FPL.[51] These subsidies reduce the deductibles and co-pays only for persons picking the silver plans, and depending on their income, the amount is progressively increased down the income scale. The effect of the cost-sharing subsidy for the lowest-income persons (between 100 percent and 150 percent of the FPL) is generous and secures for them an actuarial value of 94 percent, which means that the choice of a silver plan would cover 94 percent of their total medical expenses.
Apart from those who qualify for heavily subsidized premiums and co-payments, the rest of those who purchase individual and small-group insurance have experienced much higher premiums and much higher than expected deductibles, which in turn reflect the built-in costs of ACA’s coverage mandates and insurance regulations. The recognition that this is a serious problem is not confined to either conservative analysts or the Administration’s congressional critics. Ordinary Americans also grasp the trends.
Reason #3: The ACA has reduced insurance competition.
In 2009, making his case to Congress for reform, President Obama said:
My guiding principle is, and always has been, that consumers do better when there is choice and competition. That’s how the market works. Unfortunately, in 34 states, 75 percent of the insurance market is controlled by five or fewer companies. In Alabama, almost 90 percent is controlled by just one company. And without competition, the price of insurance goes up and the quality goes down. And it makes it easier for insurance companies to treat their customers badly—by cherry-picking the healthiest individuals and trying to drop the sickest, by overcharging small businesses that have no leverage, and by jacking up rates.[52]
The President is right: There is a positive correlation between increased competition and decreased premium growth,[53] but there is more to it than that. As the CBO has noted, “Operating in a more competitive market gives insurers a stronger incentive to limit the premiums that they charge and to constrain their administrative costs and profits—but in many parts of the United States, insurance markets are not very competitive.”[54]
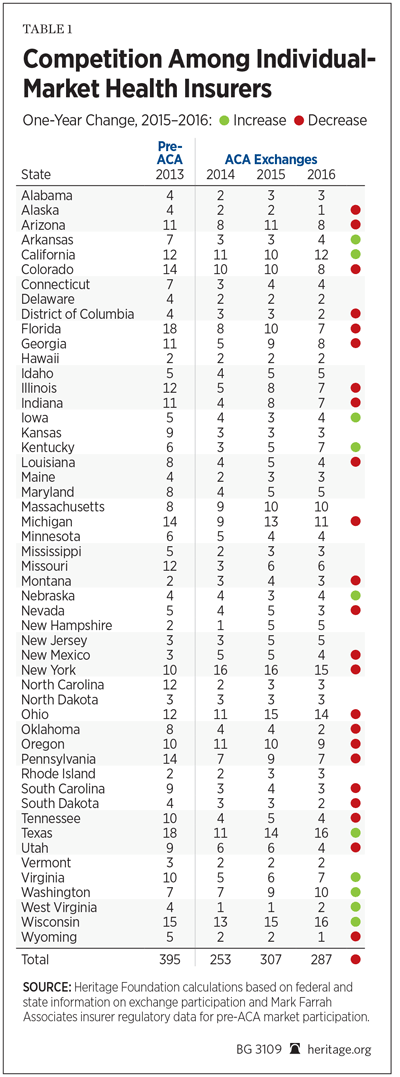
In fact, Heritage Foundation research has confirmed that the ACA has not increased health plan competition. To the contrary, the country has experienced a further concentration of the health insurance markets. In 2013, there were 395 insurers operating in the non-group market; in 2015, there were 307; but in 2016, there are only 287.[55]
In 2015, at the county level where health insurance reflects local pricing, consumers in one-third of the nation’s 3,134 counties bought coverage in exchange markets that were dominated by a monopoly (only one insurer) or duopoly (only two insurers). In fact, 58 percent of the nation’s counties in 2015 had only three or fewer insurers participating in the exchanges.[56] Equally troubling, the ACA has apparently accelerated the further concentration of market power in health care delivery, increasing corporate control over private medical practice.[57]
Reason #4: The ACA has a negative impact on job growth.
Arguably, the employer mandate, which requires firms with 50 or more full-time workers to offer federally approved levels of insurance coverage or pay a tax penalty, is the most significant provision affecting business and employment.[58] For 2016, the employer tax penalty for each uncovered worker is from $2,160 to $3,240. [59]
The Galen Institute has detailed various ways in which the Obama Administration has tried to soften enforcement:
- On July 2, 2013, the Administration announced that it was delaying the requirement that employers offer approved coverage and report the offering until 2015;
- In 2014, the Administration announced that it would not enforce the mandate requiring employers to offer equal coverage to all employees; and
- In 2014, the Administration postponed enforcement of the employer mandate for mid-sized employers to provide coverage until 2016.[60]
Curiously, though the employer mandate has been a staple of the progressive health policy agenda for decades, prominent health policy analysts, such as those at the Urban Institute, have recently expressed reservations about it and have called for its repeal.[61]
One widely anticipated impact of the employer mandate was company substitution of part-time for full-time employment. Beyond anecdotal reports, recent analytical work indicates that the aggregate impact on the workforce has been limited. Paul Van de Water, a senior fellow with the Center on Budget and Policy Priorities, a prominent progressive think tank, reported in 2015 that the ACA was not stimulating a significant shift of workers from full-time to part-time work.[62]
Joseph Antos of the American Enterprise Institute and James Capretta of the Ethics and Public Policy Center note, however, that on the basis of CBO data, the largest negative impacts on labor participation will take place in 2017 and beyond.[63] Researchers writing in Applied Economic Letters also found little evidence of such a shift but warned that the ACA could create a future increase in part-time work with the full rollout of the employer mandate.[64]
Workforce Participation. Labor force participation has been declining for many years, reaching a low of 62.5 percent in 2015. The CBO projects that it will remain at that level in 2016 and fall again to 62.1 percent in 2019. While many factors contribute to this decline, the CBO has identified federal policies as contributing to the problem—most notably the ACA.[65]
The CBO has routinely reaffirmed its position that the ACA will have a negative impact on America’s workforce. For example:
- In June 2015, the CBO said that the law’s combination of subsidies, taxes, and Medicaid expansions would “discourage” work.[66]
- In February 2015, the CBO again told the Senate Budget Committee that the law would reduce labor, cut aggregate compensation, and reduce federal revenues proportionately.[67]
- In December 2015, the CBO estimated that the ACA will decrease the total labor supply by the equivalent of 2 million full-time workers by the year 2025.[68]
In January 2016, the CBO again projected a decline in labor force participation and a negative impact on economic growth:
CBO anticipates that several developments in federal fiscal policy under current law will affect the economy through their impact on the labor market. The most sizable effects stem from provisions of the Affordable Care Act (ACA). The ACA’s largest effect on the labor market—especially as overall employment conditions improve—will come from provisions of the act that raise effective marginal tax rates on earnings, thereby reducing how much some people choose to work. The health insurance subsidies that the Act provides through the expansion of Medicaid and the exchanges are phased out for people with higher income, creating an implicit tax on some people’s additional earnings. The act also directly imposes higher taxes on some people’s labor income. Because both effects on labor supply will grow over the next few years, CBO projects, they will subtract from economic growth over that period.[69]
Reason #5: The overall health care cost curve is “bending” upward.
In another policy paradox, progressive health reformers have routinely complained that Americans spend too much on health care but have embraced a legislative remedy that substantially guarantees ever greater health care spending. Proposed remedies to “fix” the ACA’s deficiencies would obviously entail additional spending.[70] For his part, in 2010, President Obama said, “Every single good idea to bend the cost curve and start actually reducing health care costs [is] in this bill.”[71]
The President’s assertions that his policy would redirect the health cost trajectory downward were rooted in his presidential campaign advice. In May 2007, David Blumenthal, David Cutler, and Jeffrey Liebman, top analysts then advising the Obama campaign, circulated a pivotal memorandum to “Interested Parties.”[72] They claimed that, among other things, the embryonic Obama health plan could achieve extraordinary savings, amounting to hundreds of billions of dollars annually, from federal “investments” in information technology and reduced overhead in health insurance, improved disease management, care coordination, clinical effectiveness, and “pay for performance” and related “delivery reforms.” They also envisioned big reductions in employer and employee insurance costs that would have a direct, positive impact on ordinary Americans: “The typical family will save $2500 per year.”[73] President Obama, as noted, fully embraced that attractive metric—a campaign “talking point” that has since become a toxic reminder of false expectations.
Following enactment of the ACA, some overly exuberant Administration allies quickly credited the newly minted law with a decline in the growth of health care spending. In fact, trend lines showed a steady decline in overall health spending growth that long predated the law’s enactment in 2010, and that pre-ACA downturn did have a positive impact on consumer spending. For example, for private insurance premiums in all markets, premium growth averaged 4.5 percent annually between 2005 and 2013.[74]
But the most compelling reason for the slowdown in the growth of health care spending had little or nothing to do with the ACA. It was largely the result of the downturn in the economy, particularly during the period of the Great Recession (2007–2009). Of all of the variables contributing to the slowdown, claim Bradley Herring of Johns Hopkins University and Erin Trish of the University of Southern California, “The most important…appears to be the Great Recession’s effect on reduced real per capita income and the subsequent effect on reduced health care spending, as about 41% of the recent slowdown can be explained by these reductions in income.”[75]
In another analysis, researchers at the Kaiser Family Foundation reported that the average annual growth in health care spending was 8.8 percent—a high rate of spending—over the period from 2001 to 2003, after which it declined steadily: From 2008 to 2012, it was just 4.2 percent. Kaiser researchers estimated that the economic decline was responsible for 77 percent of the decrease in health spending growth during that period.[76]
With regard to traditional Medicare in particular, CBO analysts examined Medicare spending over the period from 2007 to 2012 and reported that the growth rate averaged 3 percent. They determined that the slowdown largely reflected changes in Medicare patient and provider behavior and a variety of other factors unconnected with the sluggish economy.[77] Concerning Medicare and the ACA, CBO analysts later observed that “very few of the ACA’s provisions had been implemented in any substantial way, making it difficult to attribute much of the slowdown to the effects of specific provisions of that law.”[78]
Upward Bound. As for the longer-term impact of the ACA, the notion that the law would result in a downward “bending of the cost curve” was always fanciful. Simultaneously “bending the cost curve” downward and increasing insurance enrollment and government subsidies would have been a neat trick[79] for a law that created new federal entitlements and thus became a powerful engine of massive future federal spending. In their very first report on the impact of the law in 2010, analysts with the CMS Office of the Actuary estimated that in 10 years, national health spending would increase by an estimated $311 billion more than it would have increased if the law had not been enacted.[80]
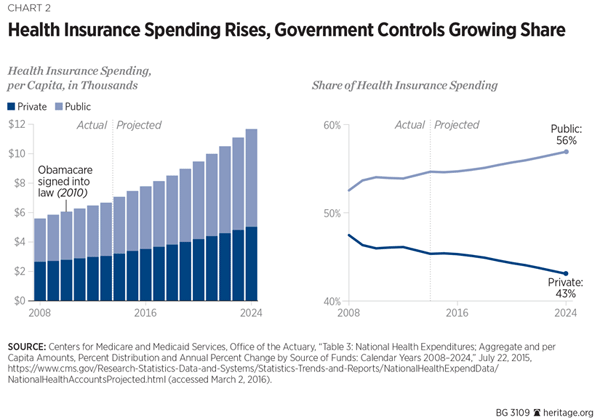
Under the ACA, the trends indicate that public spending will account for a progressively larger share of the health care economy than will private spending. In either case, a sharp growth in health care spending, both public and private, is once again well underway. “Although health care spending grew more slowly in the past several years than it has historically,” the CBO reports, “over the coming decade, per-enrollee spending in federal health programs will grow more rapidly than it has in recent years.”[81]
The latest projections are sobering. In 2014, private health insurance spending increased 5.09 percent, the largest jump since 2007, and public spending increased 6.7 percent.[82] On a per capita basis, based on CMS data, total spending on health insurance will rise from $7,786 in 2016 to $11,681 in 2024.[83]
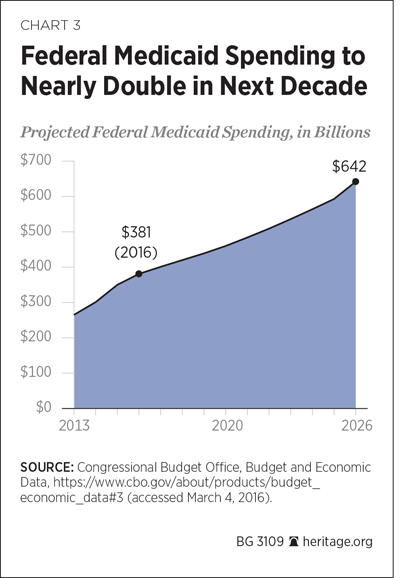
The constituent elements of health spending are showing an upward surge. Over the period from 2013 to 2015, Medicaid spending increased by 32 percent, according to the CBO; it will increase by 9 percent in 2016, and only then will Medicaid spending growth begin to taper off.[84] The ACA’s health insurance subsidies will register an average annual growth rate of 9.1 percent over the period from 2017 to 2026, the fastest rate of 10-year growth among all of the federal government’s means-tested programs.[85]
For 2015, the CBO reported that Medicare spending, which has an enormous influence on America’s health care economy, increased about 7 percent, the fastest rate of growth since 2009.[86] Overall, the CBO also reported that in 2015, the federal government spent a total of $936 billion on health programs (for example, Medicaid, Medicare, and the ACA), a 13 percent increase over the 2014 level, outpacing Social Security spending, which totaled $882 billion.[87]
Compounding population aging and increased per capita spending are ACA exchange subsidies and rising Medicaid enrollment. Medicaid enrollment, based on CBO projections, is expected to rise from 76 million in 2015 to 85 million by 2026.[88] The Administration’s allies in Congress and elsewhere may judge this a laudable expansion of government’s role in health care, but it does nothing to bend the notorious “cost curve” downward.
Reason #6: The ACA is imposing major tax increases on America’s middle class.
On August 11, 2009, during the initial stages of the congressional debate, President Obama said, “My belief is…that [health reform] should not burden people who make $250,000 a year or less.”[89]
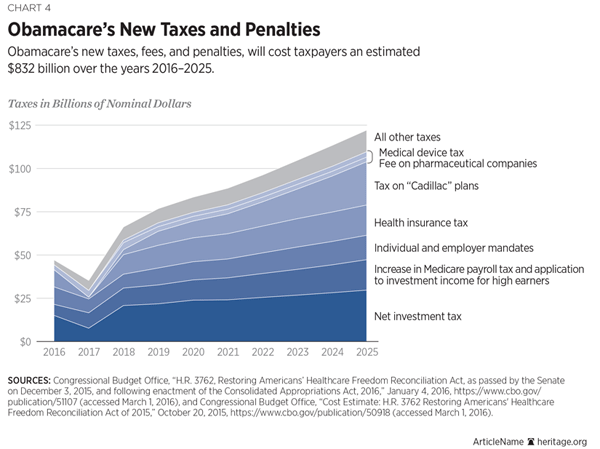
The President’s claim was always at best disingenuous. With a gaggle of tax increases, fees, and tax penalties, the ACA is, among other things, a huge tax bill. Over the period from 2016 to 2025, Americans will pay an estimated $832 billion in taxes, including taxes on health insurance plans, drugs, and medical devices that will be passed on to the middle class.[90] Not surprisingly, Congress recently enacted delays in both the health insurance tax and the 2.3 percent excise tax on medical devices.[91]
The so-called Cadillac tax—the 40 percent excise tax on “high value” health plans (in excess of $10,200 for single coverage and $27,500 for family coverage)—is also in effect a tax on the middle class. The vast majority of Americans affected by the tax, mostly those working for large companies, have annual incomes of less than $200,000. Reacting to its unpopularity, Congress recently enacted a two-year delay in the implementation of the Cadillac tax, which is now scheduled to take effect in 2020 rather than 2018.[92] In 2020, when the provision takes effect, CBO projects that unless employers change their plans, the tax will affect between 5 percent and 10 percent of employer group enrollees, rising to between 15 percent and 20 percent by 2025.[93] Many employers will doubtless scale back their health benefit offerings to avoid the tax.[94]
Independent analysts confirm the tax’s widespread impact on American workers.
- Kaiser Family Foundation researchers, for example, estimate that one in four employers offering health benefits would be affected.[95]
- Analysts at Johns Hopkins University estimate that with full implementation of the Cadillac Tax, the increasingly larger number of affected employees will experience significant benefit reductions.[96]
- American Enterprise Institute analysts say, “Given that there is an economic trade-off between wages and benefits, the Cadillac tax disproportionately harms lower-income workers with generous health benefit plans.”[97]
Even ACA taxes targeted to those who are officially designated by the government as “rich” are designed to reach eventually deep into the ranks of the middle class. For example, the 3.8 percent Medicare payroll tax on a high-income person making $200,000 annually is not indexed for inflation, so the tax will apply progressively to more and more persons as time passes. The Medicare Trustees estimate that this “high income” tax would eventually reach 80 percent of all taxpayers.[98]
The Individual Mandate Penalty. The tax penalty accompanying the individual mandate also falls disproportionately on lower-income and lower-middle-income citizens. In 2014, the CBO projected that approximately 4 million individuals would face the mandate penalty in 2016 and generate an estimated $4 billion in revenues.[99] The CBO also estimated that 69 percent of those persons would have incomes below 400 percent of the FPL, or below $47,080 in today’s dollars.[100]
For 2016, the individual mandate tax penalty for a single adult has increased to $695. The law requires that the tax penalty is to be the greater of either a flat dollar amount equal to $695 per adult plus $347.50 per child, up to a maximum of $2,085 for the family, or 2.5 percent of family income in excess of the 2015 income tax filing thresholds ($10,300 for a single person and $20,600 for a family).[101]
A key question is whether persons subject to this higher tax penalty would have an incentive to pay it and forgo coverage or whether it would encourage persons to enroll in the coverage in the government’s health insurance exchanges. In 2015, the Kaiser Family Foundation estimated that “out of almost 11 million uninsured people who are eligible to enroll in marketplace coverage either with or without financial assistance, 7.1 million would pay less for any penalty than they would to buy the least expensive insurance available to them.”[102]
Of particular interest is the response of young adults, who are disproportionately represented among the ranks of the uninsured. For many years, there has been a downward trend in young Americans enrolling in health insurance coverage. The number of persons under the age of 65 with private insurance has shrunk from 77 percent in 1984 to 62 percent in 2013, and this decline, particularly in the 1990s, was attributable to premium increases.[103]
A related problem is the stability of the exchanges. As noted, in 2015, 9.5 million (as opposed to an original CBO projection of 13 million) persons enrolled in the exchanges. For 2016, exchange enrollments have already fallen below the CBO’s initial projections, as well as the projections of the Administration, the Urban Institute, and the Rand Corporation.[104] For 2016, the CBO initially estimated that 21 million persons were to be enrolled in the ACA exchanges; the CBO has revised that number downward to just 13 million.[105] The Obama Administration reported that 2016 enrollments reached 12.7 million, but that number surely will follow previous patterns of attrition, such as persons signing up but failing to pay their premiums.
Reason #7: Medicare payment cuts will threaten seniors’ future access to care.
The law authorizes $715 billion in the form of Medicare payment reductions over the next 10 years.[106] It is logically impossible to cut payments for Medicare services without affecting seniors who depend on those services.
On April 22, 2010, in his very first assessment of the impact of the law, CMS Chief Actuary Richard S. Foster reported that the law’s Medicare provider payment cuts would make 15 percent of hospitals and other Medicare Part A health care providers unprofitable and “jeopardize” seniors’ access to care.[107] On August 10, 2010, Office of the Actuary analysts revised these initial estimates, claiming that 25 percent of Medicare providers could face “negative” profit margins by 2030 and 40 percent could face negative profit margins by 2050. The analysts said that many Medicare providers would not be able to sustain such losses and would have to withdraw from the program.[108]
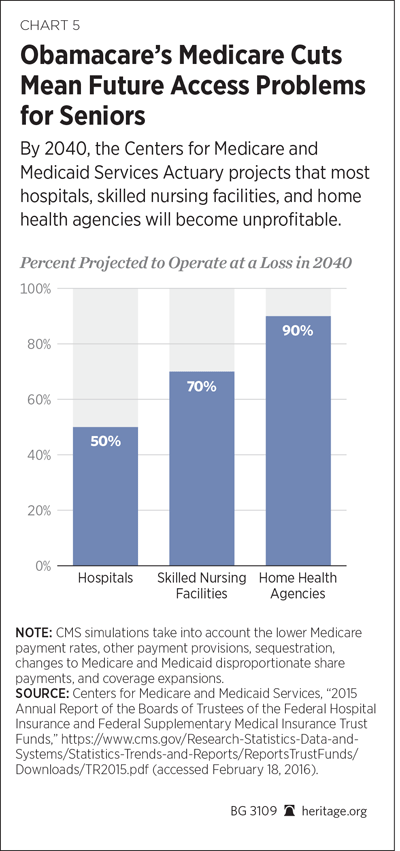
For the past five years, the CMS Actuary, with few modifications, has reconfirmed this negative outlook for the ACA’s impact on Medicare access. In their 2015 report, the Medicare Trustees largely echoed the Actuary’s concerns about the impact of the payment reductions and seniors’ access to care: “By 2040, simulations suggest that approximately half of hospitals, 70 percent of skilled nursing facilities, and 90 percent of home health agencies would have negative total facility margins, raising the possibility of access and quality of care issues for Medicare beneficiaries.”[109]
Reason #8: The ACA threatens increased deficits and debt.
President Obama said that his health reform proposal would not add “a dime” to the federal deficit and insisted from the inception of the debate that the final product would drive down the deficits and be a triumph of fiscal responsibility.[110]
The CBO has continued to validate the ACA as a vehicle for deficit reduction.
- In 2010, the CBO scored the bill as reducing the deficit by an estimated $124 billion in its first 10 years.
- In 2012, the CBO estimated that over the period from 2013 to 2022, the law would reduce the deficit by $109 billion.
- In 2014, the CBO declared that, for a variety of reasons, it could not then determine the budgetary impact of the law.[111]
- In 2015, the CBO again assumed that the ACA would reduce the federal deficit and estimated that repealing major provisions of the law would increase federal budget deficits by $137 billion over the period from 2016–2025.[112]
Given the ACA’s complexity, the CBO’s task is inherently difficult. CBO analysts must try to account for a variety of unpredictable market shifts in insurance coverage that could go in any direction. The CBO also says, for example, that per capita spending for Medicare and Medicaid is “very difficult” to predict, noting that if per capita costs rise 1 percent faster or slower annually than the CBOs 10-year projection, total federal outlays for both programs would be $1 trillion higher or lower for the projected period.[113]
In 2014, narrower than anticipated networks in health insurance exchange plans and higher than expected deductibles resulted in lower plan premiums, which in turn reduced the cost of the federal insurance subsidies and thus overall projected ACA spending. Lower than anticipated Medicaid enrollment following the Supreme Court’s 2012 ruling striking down of the Medicaid mandate on the states guaranteed a reduction in Medicaid spending projections.[114] Lower than anticipated enrollment, premium payments and subsidies, and lower Medicaid enrollment and spending resulted in a general lowering of the law’s total costs and thus contributed to the CBO’s continued projections for deficit reduction.
CBO analysts have been forthright about the uncertainty of their scoring. For example, in 2015, the CBO told the Senate Budget Committee, “If macro-economic effects had been included in the cost estimate for the ACA that CBO provided in March 2010, the estimated net effect of that legislation on the deficit would probably have been less favorable than that which was shown.”[115] More recently, addressing the potential repeal of the law, the CBO flatly acknowledged that the impact on the deficit could go either way: “The uncertainty is sufficiently great that repealing the ACA could in fact reduce deficits over the 2016–2025 period—or could increase deficits by a substantially larger margin than the agencies have estimated.”[116]
The CBO’s assessments are based on a required and conventional assumption: the continuity of current law, in this case one that authorizes simultaneously massive increases in revenue and unprecedented cuts in provider payments.
Fragile Assumptions. These are fragile assumptions, though they polish the shiny façade of the ACA’s fiscal rectitude. In 2010, the CBO scored a legislative product that was marked by some impressive budgetary gamesmanship:[117] the front-loading of revenues and back-loading of benefit payments over the first 10 years to guarantee a positive deficit-reducing score.
Since 2010, however, a deadly combination of budgetary pressures has threatened the ACA’s deficit-reduction potential. The law locks in massive federal spending with unpopular taxes and unreliable savings. For example, the substantial revenues from the long-term care program ($86 billion from 2012–2021) disappeared with its total collapse.[118] Other revenues crucial to the ACA’s deficit-reduction potential are its increasingly unpopular taxes such as the Cadillac tax, medical device tax, and health insurance tax. The survivability of these provisions is questionable, since they generate intense bipartisan congressional opposition. Congress delayed all three of these taxes in 2015.
Savings are also unreliable.
- Congress enacted the ACA in 2010 on the assumption that the Medicare physician payment system, the Sustainable Growth Rate formula (SGR), would continue to restrain Medicare spending. In 2014, when Congress, with the support of the Obama Administration, eliminated the SGR, the lawmakers also added an estimated $141 billion in federal deficits over 10 years.[119]
- In 2015, Congress defunded the Independent Payment Advisory Board (IPAB), a key ACA mechanism designed to make recommendations for further Medicare payment reductions to meet Medicare’s unprecedented budgetary caps.[120] The board is still not operational.
- The hundreds of billions of dollars in additional savings from the ACA’s huge Medicare payment changes and reductions are also unlikely to materialize. As early as 2010, the CBO expressed skepticism that Medicare cuts of that magnitude were politically sustainable, and the Medicare Actuary repeatedly declared them unrealistic.
- Certain ACA “savings” assumptions were simply unfounded.[121]
Centralized and putatively efficient administrative payment for high-quality medical outcomes is at the heart of the ACA’s “delivery reforms.” Although Administration officials believed that their delivery reforms—such as “value based purchasing” for hospitals and “pay for performance” for physicians—would be both cost-effective and productive, in 2010, the CBO declined to score them as having any effect on health care spending. In 2012, the CBO conducted an evaluation of various “value-based” payment initiatives and found them largely ineffective in generating savings.[122] In 2014, only about half of the Medicare “accountable care organizations” (ACOs), the flagship of the delivery reform project, demonstrated savings.[123] Whether such initiatives, whatever their intrinsic value, can eventually generate significant and sustained savings is as yet unclear.
Taking the totality of these and a variety of other factors, independent analysts doubt that the ACA will reduce the deficit. Medicare Trustee Charles Blahous, for example, concluded that the ACA’s budgetary condition would continually worsen and projected a 10-year deficit that could range “somewhere between $340 [billion] and $530 billion.”[124]
The Broader Context. Meanwhile, on the broader issue of deficits, it is worth noting that in 2008, the last year of the Bush Administration, the annual deficit reached $458.6 billion. The deficit leaped to a breathtaking $1.4 trillion in 2009, the first year of the Obama Administration, and exceeded well over $1 trillion in 2010, 2011, and 2012.
The President is correct that annual deficits have declined steadily since 2009. In 2015, it reached its lowest point at $438.7 billion. For 2016, however, the CBO projects an increased deficit of $544 billion and a return to a fiscally ruinous status quo ante, with annual deficits piling up year after year to reach an accumulated total of $9.4 trillion over the period from 2017 to 2026.[125] Meanwhile, federal debt as a percentage of gross domestic product (GDP) jumped from 39.3 percent in 2008 to 73.6 percent in 2015.[126] The Obama Administration, however one judges its other accomplishments, leaves behind an indelible legacy of red ink.
Reason #9: The ACA forces Americans, in direct violation of their rights of conscience, to fund abortion through their tax dollars.
On August 20, 2009, President Obama said, “There are no plans under health reform to revoke the existing prohibition on using federal taxpayer dollars for abortions.”[127]
In fact, the ACA authorizes federal funding of abortion in its “qualified” health plans, a sharp break from previous law.[128] In the case of the special “multi-state health plans” administered by the OPM, the law requires the federal government, beginning in 2014, to contract with at least two national health plans, one of which must offer abortion coverage in the ACA exchanges.[129]
The ACA also violates personal rights of conscience. For example, in 2011, acting on her broad discretionary authority, HHS Secretary Kathleen Sebelius mandated employers and employees to pay for, among other things, federally certified abortion-inducing drugs. This unprecedented mandate, only partially nullified by the United States Supreme Court, is still operational for many employers and a subject of continuing federal litigation.
Reason #10: The ACA imposes arbitrary rules and costly mandates.
Under the ACA, federal officials are developing and enforcing an enormous body of regulation of the health care sector of the American economy. Thus far, the Obama Administration has published 19,368 pages of ACA “rules” in the Federal Register.[130]
Three federal departments are mostly responsible for the issuance of ACA regulations: the Department of Health and Human Services, the Department of Labor, and the Department of the Treasury, particularly the Internal Revenue Service (IRS). Beyond these large federal departments, the ACA creates scores of smaller boards, commissions, panels, and programs. The Congressional Research Service has concluded that the exact number of these entities is “unknowable” because a number of them can be created administratively.[131]
The clarity of ACA provisions is uneven. Certain sections are crystal clear, but many others are vague and even mysterious, making the precise application of a particular provision dependent on interpretation and enforcement by federal regulators. The law specifies, for example, that reimbursement for doctors and hospitals is to secure “quality” care or “value” in their transactions with patients, even though there is often profound disagreement among medical professionals on what, in any given case, quality or value may mean in a clinical context in the treatment of specific diseases or medical conditions.
Recently, interpreting Section 1557 of the ACA, the Administration issued a sweeping proposed rule requiring that all health plans must provide medical benefits or procedures in accordance with the new “gender” anti-discrimination standards of the HHS Office of Civil Rights. Procedures potentially ranging from abortion to “sex-reassignment” surgery would be covered by the new rule.[132]
Arbitrary Rules. The ACA’s transmission of broad discretionary authority to federal departments and agencies not only authorizes federal officials to issue rules, but also enables them to make exceptions to the rules they issue, grant waivers, or apply them differently to different segments of the population. There are many examples. Consider just two of the most egregious:
-
Effective in 2010, the ACA prohibited insurers from offering limited-benefit “mini-med” plans. Because these plans did not meet the 2010 federal standards for coverage caps, the plans’ officials either had to raise their rates to comply, making them less affordable for low-income persons who enrolled in them, or go out of business and thus deny those persons access to that coverage.
The problem was that thousands of retail and service industry companies, various organizations, and even unions offered these plans, and an estimated 4 million Americans were enrolled in them. The Obama Administration’s political solution was to grant waivers to certain companies but not to others. McDonald’s, the giant fast-food restaurant chain that employed over 30,000 mostly low-income persons, got a temporary HHS waiver to retain its “mini-med” coverage.[133] It was not long before HHS granted exemptions to various firms, union organizations, and even certain gourmet restaurants in San Francisco.
- In 2013, the Obama Administration provided special taxpayer subsidies for Members of Congress and staff to offset their higher insurance costs in the ACA health insurance exchange.[134] The OPM, which administers the federal civil service, ruled that Members of Congress and staff, even though they are no longer enrolled in the Federal Employees Health Benefits Program (FEHBP), would nonetheless get FEHBP subsidies for insurance coverage outside of the FEHBP. Members were henceforth to enroll in the District of Columbia small-business exchange. In qualifying for enrollment, the House and Senate were officially designated “small businesses.” Beyond this absurdity, there was no statutory authority under the ACA or Title V, the law that governs the FEHBP, to authorize any such subsidies.[135]
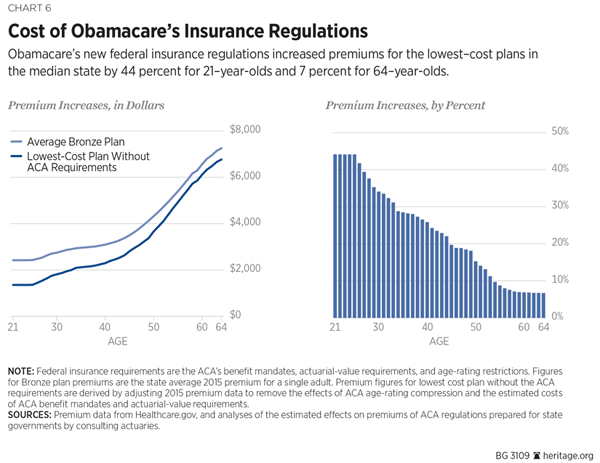
Costly Insurance Mandates. For millions of Americans, the most costly insurance mandates and regulations affect their coverage. For example, the ACA specifies that insurers cannot charge a 64-year-old more than three times the premium that would apply to a 21-year-old. The normal age variation in health costs between older and younger persons is about five or six to one, not three to one. The mandate thus artificially overprices insurance for young people while artificially underpricing insurance for older enrollees. For young adults enrolled in a bronze plan, the net effect is to increase their premium costs by an estimated 33 percent.[136]
The ACA also requires health plans to meet federal “essential health benefits” requirements, including 10 categories of health benefits as well as all officially recommended preventive services. For these services, health plans cannot charge any co-payments. This guarantees that their premium costs will be proportionately higher. Based on a review of the literature, it appears that the additional insurance premium costs are, on average, about 9 percent.[137]
Health plans’ “actuarial value” refers to the amount that a plan must pay toward the cost of covered services. Under the ACA, no qualified health plan can have an actuarial value of less than 60 percent, the so-called bronze-level coverage. Whatever the wisdom of the requirement, it raises the cost of the least expensive exchange plans by about 8 percent.[138]
ACA insurance rules standardize offerings and eliminate variation of coverage policies among the states, but the price is higher premium costs and an impediment both to innovation in benefit design and to opening up opportunities for individuals, particularly young persons who resist buying insurance, to secure more affordable coverage.
The Emerging Post-Obamacare Future
In January 2016, for the first time in six years and overcoming political and parliamentary obstacles, Congress enacted a repeal of the ACA’s major provisions. President Obama, as expected, quickly vetoed the bill, and his veto was sustained. Nonetheless, the large majority of Members who campaigned on a promise to their voters to repeal the law fulfilled that promise and demonstrated the parliamentary capacity, using congressional budget rules and a Senate majority, to repeal the law and lay the groundwork for replacing it with a superior alternative.
In preparation for 2017, House Speaker Paul Ryan (R–WI) assembled a special task force of House committee chairmen to craft a replacement for the law. Beyond the ACA, federal health policies governing the pre-Obamacare health care arrangements, particularly the insurance markets, were profoundly flawed. The formidable task for Congress, therefore, is to present and promote a new vision and meticulously craft the legislative details necessary to fulfill it.
There is an emerging consensus on the key areas to be addressed.[139] The top goal should be to empower individuals and families as the key decision-makers in the health care economy. Individuals and families would control the flow of health care dollars in the system, directly exercise economic power, and determine the kind of health plans and benefits, medical procedures, and treatments that they want in accordance not only with their medical and economic needs, but also with their ethical, moral, and religious convictions.
With health insurance, Congress should take specific steps to allow personal, portable, and affordable health coverage to flourish. This can be done by leveling the playing field for all Americans, opening up the markets, and ending official tax policy discrimination against persons based on their employment status. The key change would entail giving all persons a direct and simpler system of individual tax relief for the purchase of the health insurance of their choice, whether group or non-group coverage. Congress can also build on the broad consensus that has long existed both in the House and Senate and among the public at large to adopt procedures that ensure ease of access to coverage for persons with preexisting conditions.
In any new health reform agenda, Congress cannot ignore the major federal health entitlements. With Medicare, a reform agenda would build on the already existing—and highly popular—defined-contribution financing systems for comprehensive health plans in Medicare Advantage and the broad range of drug coverage in Medicare Part D. With Medicaid, Congress could likewise create a strong “premium support” or defined-contribution system that would mainstream low-income persons into the private health insurance markets. Intense market competition driven by consumer choice in an environment characterized by transparency on price and performance would not only control costs, but also ensure value.
Meanwhile, the ACA is ripe for repeal. For the American public, there are ample reasons for dissatisfaction. Specifically, there are the ACA’s:
- Higher costs;
- Arbitrary and sometimes absurd rulemaking;
- Bureaucratization of an already overly bureaucratized sector of the economy;
- Incompatibility with personal freedom and religious liberty; and
- Enormous spending and heavy taxation.
There are also widely acknowledged design flaws, evident in its hopelessly complex and unworkable subsidy schemes, boondoggle bailouts, and collapsing co-ops.
For many Americans, opposition to the ACA is rightly rooted in their rejection of the tacit assumption underlying its centralized architecture: that Washington’s political class possesses the wit and wisdom to restrain, guide, and direct this enormously complex and dynamic sector of the American economy and, in pursuit of that project, must exert greater control over their personal lives.
Americans know that their elected representatives can indeed craft a much better alternative than periodically patching the flawed Affordable Care Act. And Americans deserve better.
—Robert E. Moffit, PhD, is a Senior Fellow in the Center for Health Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.