Health care premiums are continuing to rise in 2015. While the pace of change has slowed since the dramatic increases of 2014, the savings promised under the Affordable Care Act (ACA) have still not materialized.
Measuring changes in premiums is an important element in understanding the impact of the ACA. In previous analysis, The Heritage Foundation determined that the new regulations and benefit mandates put in place through the ACA caused premiums to increase drastically in 2014, with average premiums increasing more than 50 percent in some states.[1] This Issue Brief examines premium changes in 2015 and finds continued but slower premium growth, indicative of a market going through a sorting process.
Results from 2015 Premium Analysis
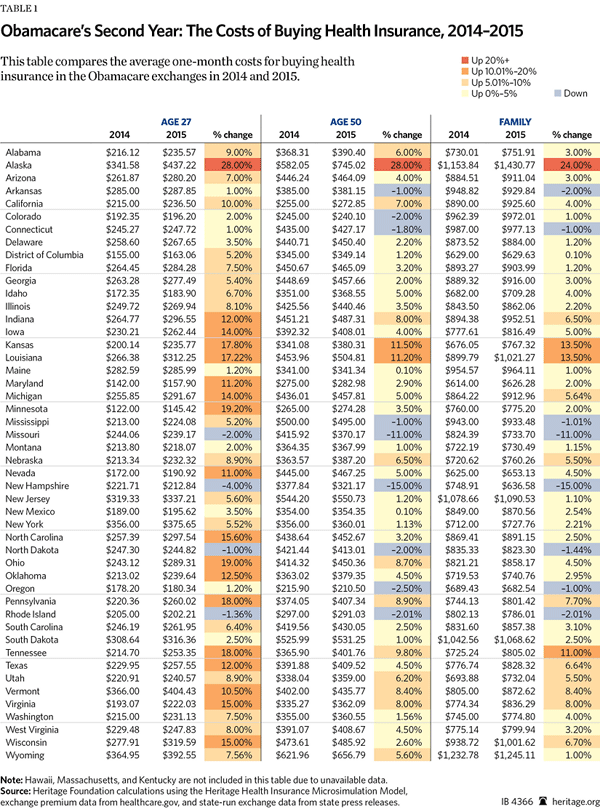
For the United States as a whole, average health care premiums will increase by 5.3 percent in 2015.[2] The estimate is derived using the Heritage Health Insurance Microsimulation Model, which uses enrollment data and plan-selection data from the Department of Health and Human Services (HHS) to analyze premiums within the ACA exchanges. This average increase, while indicative of the entire market, masks a wide disparity of experiences across the country and thus the experience of individuals will vary drastically based on location, as shown in Table 1.
For example, while average premiums in New York increased by about 2 percent, premiums in Ohio went up by approximately 11 percent. When looking at various plan offerings, the variation within a state can be substantial, too. In Michigan, rate changes for various plans range from a 22 percent decrease to an 18 percent increase. Additionally, Heritage analysis finds that premium increases, in general, are larger for younger, lower-cost individuals, continuing a trend set with the pricing in the 2014 exchanges.
Conor Ryan of the American Action Forum discusses the variations in his “Averages Won’t Tell the Story” analysis.[3] Similarly, health care consulting group McKinsey finds significant variation in premiums within the same tier even at the state level.
Understanding Other Premium Analyses for 2015
There have been several other studies that attempt to analyze the data from HHS regarding premiums within the exchanges. While there are differences among the studies, all show significant premium increases in at least some states, with premiums typically growing faster for the lower-priced plans.[4] Studies from Price Waterhouse Coopers and McKinsey found increases in average premiums between 6 percent and 10 percent across the country.[5] The Commonwealth Fund found something different: It claimed in its blog “Analysis Finds No Nationwide Increase in Premiums” that premium growth had slowed down.[6] However, the appendix to the study revealed that “the general pattern of premium increases observed was a regression toward the mean, with the lowest cost plans in 2014 raising their premiums significantly, while higher price plans in 2014 reduced their premiums.”
It is important to understand how these analyses can have such different results. While Commonwealth’s research appears to use population weighting and McKinsey’s eschews weighting in order to provide a look at lower cost plans within each tier, neither fully makes use of actual enrollment estimates. Commonwealth’s analysis in particular misses the point that population weighting does not capture the distribution of individual plan selection. Simply, more people pick the lowest-cost plans in each “metal” tier, which is different than a simple population weighting. Thus the claim that premiums have not changed is likely an understatement simply based on the methodology, because all evidence suggested by other analysis, including Commonwealth’s, points to larger increases in premiums of lower-cost plans.
In the case of McKinsey and others, the estimates are based on a comparison of lower-cost plans in each tier. This seems more justifiable, but could lead to an overstatement because not everyone selects the lowest-cost plans (even though the majority will). Still, it is likely not a great overstatement considering that around two-thirds of enrollees selected the lowest-cost plans in each tier.[7]
Conclusion
Given the new benefit mandates and other costly requirements imposed by the ACA, it is not surprising that 2014 exchange-plan premiums were, in general, significantly higher than pre-ACA premiums. It is also not surprising, given the substantial uncertainty that insurers faced when trying to set 2014 premiums, that there would be wide variations in 2014 rates and, after a year of actual claims experience, that 2015 rates would start to coalesce around a mean. That is a normal pattern for a market responding to the imposition of disruptive changes.
However, it is important to note that the resulting effects on individuals are far from evenly distributed. In a regression to the mean, the previously higher premiums fall while the previously lower ones rise. Yet because a majority of enrollees opted for lower-price plans last year, the effect this year is that more enrollees experienced an increase in premiums than experienced a decrease in premiums.
Put simply, reducing prices for more expensive products that few customers purchase has little real-world impact on the prices actually paid by most consumers. Conversely, if most consumers purchase the lower-cost products—as seems to be the case with exchange plans—many of them will be directly affected when a regression to the mean produces price increases for those products.
In sum, exchange-plan pricing in 2015 generally shows reductions in premiums for the expensive plans that few people purchased accompanied by increases in premiums for the lower-cost plans favored by the majority of enrollees. Thus, the real-world effect for most exchange consumers is that the prices they pay further increased in 2015, though not as dramatically as they did in 2014.
—Drew Gonshorowski is a Senior Policy Analyst in the Center for Data Analysis, of the Institute for Economic Freedom and Opportunity, at The Heritage Foundation.