In 2017, very little changed in net health insurance coverage, but below the surface, some significant shifts occurred in sources of coverage. In 2017, net enrollment in private and public coverage increased by only 191,000 people. The individual market, however, lost nearly 1.8 million enrollees in 2017—a decrease of 10.5 percent in a single year—dropping from 17 million people at the end of 2016 to 15.2 million at the end of 2017. That drop occurred almost entirely among people who did not qualify for Obamacare subsidies. While the number of individual-market enrollees who receive Obamacare subsidies declined by less than 2 percent, from 7.6 million enrollees to 7.5 million enrollees, unsubsidized non-group-market enrollment dropped by 17.6 percent, from 9.4 million to 7.7 million people.
An additional shift occurred within the employer-group-coverage segment. Enrollment in fully insured group plans decreased by 393,000 people, while enrollment in self-insured plans increased by 2.7 million.REF The net result was 2.3 million more individuals with employer-sponsored coverage in 2017.
Public coverage saw very little change. Overall enrollment in Medicaid and the Children’s Health Insurance Program (CHIP) was flat for 2017. States with the Affordable Care Act (ACA) Medicaid expansion in effect experienced Medicaid enrollment growth of 71,000 people (less than two-tenths of 1 percent); states without the expansion in effect experienced a decrease in Medicaid enrollment of 416,000 individuals (1.8 percent). On net, private health insurance enrollment increased by 536,000 individuals, or three-tenths of 1 percent, from 174.6 million at the end of 2016 to 175.2 million at the end of 2017, while enrollment in Medicaid and CHIP declined by 345,000 people, less than half of 1 percent, from 74.9 million to 74.6 million.REF
Enrollment Trends Since 2014
Table 1 shows the annual and cumulative changes in health insurance enrollment by sector since the implementation of Obamacare in 2014. Across all types of coverage, net enrollment growth from 2014 to 2017 was 15.8 million individuals—with 86 percent of that increase attributable to additional Medicaid and CHIP enrollment.
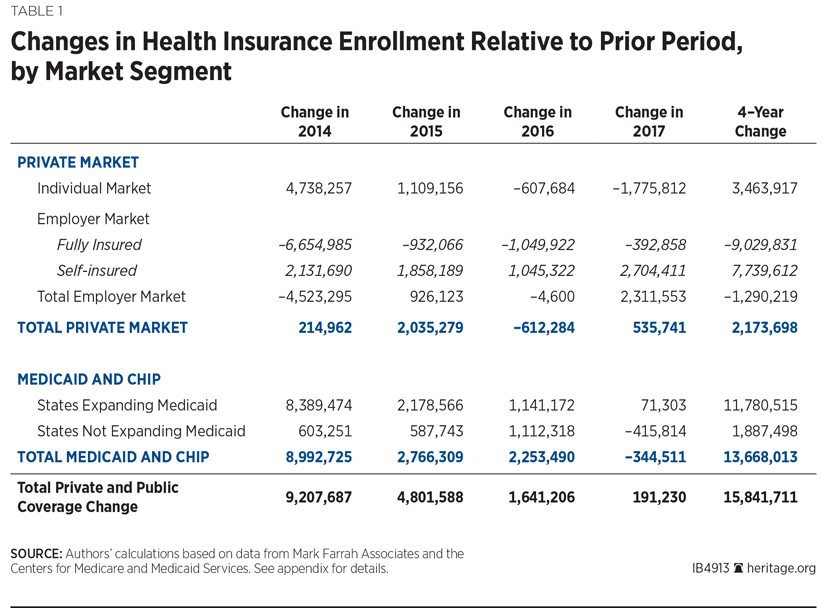
The number of people covered by individual-market policies expanded in 2014 and 2015 in response to the availability of Obamacare’s new exchange subsidies, but then shrank in 2016 and 2017. During the three years prior to the implementation of the ACA (2011 to 2013) enrollment in individual-market coverage was fairly stable between 11.8 million and 12 million people. The introduction of subsidies for exchange coverage produced a 40 percent enrollment surge in 2014, followed by an additional 7 percent increase in 2015. That trend reversed as the non-group market shrank by 4 percent in 2016, and then by a further 10.5 percent in 2017.
While enrollment in fully insured employer plans experienced an 11 percent drop in 2014 (from 60.6 million to 54.0 million), that drop appears to have been largely a one-time event. Prior to the implementation of the ACA, enrollment in fully insured employer plans had been gradually declining by about 2 percent per year, and that trend resumed after 2014. The fully insured employer market shrank by 1.8 percent in 2015, 2.0 percent in 2016, and 0.8 percent in 2017.
At the same time, enrollment in self-insured employer-group plans has grown at an average annual rate of about 2 percent per year since the implementation of the ACA, expanding from 100.5 million individuals in 2013 to 108.3 million in 2017, though in 2017 that segment of the market experienced its largest annual enrollment growth (2.7 million individuals, or 2.56 percent) since 2013.
The combined effect of the changes in individual-market and employer-group coverage produced a net increase in private-sector coverage of 2.2 million individuals over the four-year period of 2014 to 2017.
Since the implementation of Obamacare, enrollment in Medicaid and CHIP has grown by 13.7 million individuals (22 percent), from 60.9 million at the end of 2013 to 74.6 million at the end of 2017. In states that adopted the ACA Medicaid expansion, enrollment increased by 11.8 million (29 percent); in states that did not adopt the expansion, enrollment increased by 1.9 million individuals (9 percent).
A Shrinking Individual Health Insurance Market
The most significant change in 2017 was the sharp drop in the number of people with individual-market coverage, particularly the number of unsubsidized customers. Table 2 breaks out enrollment data for the individual market by subsidy status.REF It shows that while the number of enrollees with subsidized exchange coverage declined slightly (by 1.7 percent) in 2017, the number of unsubsidized enrollees dropped by 17.6 percent. Unsubsidized individual-market enrollment has declined every year since the implementation of Obamacare at an accelerating pace.

Since the implementation of Obamacare, the number of unsubsidized individual-market customers has shrunk by 4.1 million—more than a third (34.7 percent)—from 11.8 million in 2013 to 7.7 million in 2017. During the same period, Obamacare added 7.5 million subsidized customers to the market.
Individual-market enrollment peaked in 2015. While enrollment expanded in 2014 and 2015 in response to the availability of Obamacare’s new exchange subsidies, it then shrank in 2016 and 2017. As Table 2 shows, individual-market enrollment reached almost 17.7 million people in 2015, but declined to 15.2 million in 2017, the lowest level since before the implementation of Obamacare.
Both the number of buyers and sellers peaked that year; 2015 was the high-water mark for insurer participation in the Obamacare exchanges at both the state and county levels.REF
These enrollment trends reflect the reality that the ACA altered the basic composition of the individual health insurance market.
Before the implementation of Obamacare, the primary customers for individual-market insurance were Americans who were either self-employed or buying coverage between jobs. They were mainly seeking financial protection against potential future medical expenses.
The changes made by the ACA attracted a new set of customers responding to the law’s offer of subsidized insurance to pay for their current medical expenses. That skewed the post-ACA individual market toward a risk pool disproportionately consisting of older, less healthy, and costlier-to-insure individuals. In the first two years, hundreds of thousands of costlier customers migrated into the individual market from other coverage.REF The results were sharp premium increases that, in turn, prompted a growing exodus of unsubsidized customers.
Table 2 shows how Obamacare resulted in the displacement of the market’s traditional customers over the four-year period. In 2014, the first year of implementation, unsubsidized enrollment declined by 692,000 individuals. That figure includes any pre-Obamacare customers who qualified for the newly available subsidies (in other words, anyone already enrolled in non-group coverage who shifted from unsubsidized to subsidized). In the subsequent three years (2015 to 2017) unsubsidized enrollment declined by a further 3.4 million individuals, all of which can be attributed to those customers exiting the market.
Most of the customers who exited the market likely are middle-income, since they did not qualify for Obamacare’s low-income premium subsidies, and self-employed, since they had been buying their own health insurance. What is less clear is where those customers have gone. Some may have obtained jobs with employer-sponsored health insurance. Others may have instead given up on health insurance—in which case, Obamacare is now un-insuring the previously insured.REF
Implications of Recent Regulatory Changes
Some assert that the Trump Administration has taken regulatory actions that will “destabilize” health insurance markets.REF Such actions include expanding the availability of association health plans to the self-employed and reversing the Obama Administration’s restrictions on short-term health insurance plans (which do not have to comply with Obamacare’s mandates).REF
Yet, enrollment data indicate that the market was already significantly destabilized prior to the Trump Administration taking office. In that regard, it is important to note that 2017 health plans and premiums were set in October of 2016, and that the 2017 open-enrollment period ran from the week before the election through the week after the Inauguration. Thus, the sharp drop off in unsubsidized individual-market enrollment during 2017 occurred in response to factors that pre-date the Trump Administration.
Consequently, any take-up of alternative coverage under the Trump Administration’s regulatory changes is more likely to be by those who have already abandoned costly Obamacare-compliant plans than by those still buying them. Given the significant, and growing, decline in the number of unsubsidized individual-market customers since the implementation of Obamacare, it would be more accurate to view the Administration’s policy changes as responses to existing market destabilization than as catalysts for further destabilization.
Changes in Employment-Based Coverage
Obamacare imposed new benefit requirements on individual-market coverage and group policies sold by insurers in the small-group market (defined as firms with fewer than 50 employees). These mandates increased the cost of those policies. While the law did not extend those benefit requirements to either self-insured plans or policies sold in the large-group market (defined as firms with 50 or more employees), it did impose a new mandate that employers with more than 50 workers offer health insurance to their employees.
Enrollment in fully insured employer plans dropped by about 11 percent in 2014. Furthermore, enrollment dropped among both small and large firms.REF That suggests that a number of smaller firms responded to Obamacare by discontinuing coverage, while some larger firms shifted from fully insuring to self-insuring their employee health plans. After 2014, the fully insured group market returned to its pre-Obamacare pattern of contracting by about 2 percent per year, which suggests that the events of 2014 were largely a one-time response to implementation of the ACA.
Effect of Obamacare’s Medicaid Expansion
Since the implementation of Obamacare in 2014, the vast majority of coverage gains have occurred in Medicaid, particularly in those states that adopted the law’s expansion of Medicaid eligibility to low-income able-bodied adults.
Table 1 shows that over the four years 2014 through 2017, combined enrollment growth for both private and public coverage was 15.8 million individuals—with 86.3 percent of that increase attributable to additional Medicaid enrollment. Higher Medicaid enrollment in states that adopted the ACA Medicaid expansion accounted for almost three-quarters (74.4 percent) of total (public and private) enrollment gains.
The vast majority of enrollment gains occur within the first year following a state’s implementation of the expansion.REF Given that no additional states implemented the Medicaid expansion in 2017, it explains why enrollment in the program was essentially flat for the year.
Conclusion
The vast majority of enrollment gains under Obamacare have come through the law’s expansion of Medicaid coverage to include able-bodied adults without dependent children.
Obamacare has also provided subsidized individual-market coverage to another 7.5 million people. However, in the process, the law significantly skewed the individual-market risk pool, producing sharp premium increases that, in turn, prompted a growing exodus of unsubsidized customers.
Policymakers need to recognize that the individual health insurance market was never big enough to support the burdens placed on it by Obamacare, particularly the influx of high-cost enrollees. The accumulating data on enrollment, claims, and premiums all indicate that Obamacare has been transforming the individual market into a federally subsidized, low-income, high-risk pool. As a result, that market is no longer providing affordable coverage for its traditional customer base of middle-income workers and families without access to traditional employer plans.
To its credit, the Trump Administration is trying to do what it can to offer more affordable alternatives for those displaced Americans. Now Congress needs to get back to work on undoing the damage done by Obamacare to the individual health insurance market.REF
—Edmund F. Haislmaier is the Preston A. Wells Jr., Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.
Appendix: Data Sources and Adjustments
Data for private-market enrollment by market segment is derived from insurer regulatory filings compiled by the National Association of Insurance Commissioners (NAIC) and accessed through Mark Farrah Associates. Enrollment in self-insured employer plans is as reported by Mark Farrah Associates for plans administered by an insurance carrier. The firm compiles that data from insurer regulatory filings, supplemented by other public and private sources, such as Securities and Exchange Commission filings.
Medicaid and CHIP enrollment figures are from Centers for Medicare and Medicaid Services (CMS) state-level monthly enrollment reports. Those reports include enrollment in both fee-for-service Medicaid and Medicaid managed-care plans and are point-in-time counts, which make them consistent with the counts of private-market coverage reported in insurer regulatory filings.REF Medicaid/CHIP enrollment data for December 2013 was obtained from a report by the Kaiser Commission on Medicaid and the Uninsured and used as the basis for calculating enrollment growth during 2014.REF
Several adjustments were made to the Mark Farrah Associates private-market data to make it as complete and accurate as possible. Specifically:
Arkansas implemented the Medicaid expansion through a so-called private-option design. Under that approach, qualified individuals are enrolled in the state’s Medicaid program, and then, at the beginning of the month following enrollment, select (or are assigned) coverage through a Silver-level plan offered in the exchange, with Medicaid paying almost all of the premiums. This arrangement could result in double counting those individuals. The CMS reports include private-option enrollees in Arkansas’s Medicaid enrollment figures and exclude them from the state’s exchange enrollment figures. However, the regulatory filings by carriers offering exchange coverage in Arkansas include private-option enrollees in their enrollment counts for individual-market coverage—which, from the carrier perspective, would be appropriate. Separately, the Arkansas Department of Human Services (DHS) reported that the number of individuals with completed private-option enrollment at the end of 2017 was 249,977.REF
Consequently, to avoid counting private-option enrollees twice, the Arkansas DHS figure was subtracted from the figure for total individual-market enrollment for Arkansas derived from the insurer regulatory filings. Thus, this analysis counts Arkansas private-option enrollees as Medicaid enrollees.
New Hampshire has implemented a “premium support” waiver as part of its Medicaid expansion. As with Arkansas, CMS reports include those premium support beneficiaries in the state’s Medicaid enrollment figures, and exclude them from the state’s exchange enrollment figures, while private insurers report them as enrolled in individual-market coverage. The New Hampshire Department of Health and Human Services (HHS) reported that the number of individuals enrolled through premium support in exchange plans at the end of 2017 was 39,026.REF To avoid counting Medicaid premium support enrollees twice, the New Hampshire HHS figure was subtracted from the figure for total individual-market enrollment for New Hampshire derived from the insurer regulatory filings. Thus, this analysis counts New Hampshire Medicaid premium support enrollees as Medicaid enrollees.
Four New York carriers that offer coverage through that state’s exchange are Medicaid managed-care insurers that did not offer coverage in the individual or group markets prior to 2014, and do not file NAIC reports, as they are regulated by the New York State Department of Health. Figures for those carriers are taken from the 2017 enrollment report published by the state exchange.REF However, end-of-year enrollment figures for those carriers for prior years are available from their federal medical loss ratio report filings, so their enrollment figures for 2014, 2015, and 2016 were updated accordingly.
Fourth-quarter reports were missing for two insurers. Enrollment figures reported in their most recent (3Q 2017) NAIC filings were used on the presumption that most, if not all, of those enrollees still had their coverage in force through the end of 2017.
The net effects of these adjustments to the enrollment figures derived from the Mark Farrah Associates dataset were a decrease of 111,006 for the individual market and an increase of 1,007 for the fully insured group market.

