With the ongoing congressional effort to reform health care falling short of repealing Obamacare, it is critical that Congress maximize every opportunity to undo Obamacare’s damage. The draft bill released by the Senate on Thursday misses important opportunities to move closer to that objective.
On net, the Senate bill is better than the status quo because it contains provisions to reduce insurance premiums and promote access to insurance in the short run, cut taxes, and provide major Medicaid reform that will help refocus the program on those most in need.
The question remains, however, whether the bill will repair enough of the damage caused by Obamacare to enable individuals, such as the middle-class self-employed, to find affordable health insurance in the longer run. To undo more of Obamacare’s damage, the Senate should go further by expanding states’ regulatory reform options to encourage continuous coverage and further roll back Obamacare mandates. The Senate should also provide additional Medicaid reforms to improve the program for beneficiaries and taxpayers alike.
Obamacare’s Damaging Federal Mandates
Obamacare’s federal control over state health insurance markets has proven to be a costly and painful experiment, resulting in soaring premiums and skyrocketing deductibles for enrollees. One factor driving up costs was Obamacare’s preemption of state authority for insurance markets and its imposition of costly new federal benefit mandates and regulations. This unnecessary move short-circuited the ability of states to adopt different approaches or to modify rules to accommodate changing circumstances.
Obamacare’s structure of new federal health insurance regulations and subsidies was designed to provide lower-income individuals in need of medical care with comprehensive coverage at little cost to the recipients. Obamacare also applied those same regulations, but not the subsidies, to the broader individual and small employer health insurance markets.
Americans with unsubsidized coverage through individual-market or small-employer policies have borne the brunt of the premium increases and coverage disruption caused by Obamacare’s insurance market regulations. They are the ones most in need of relief from Obamacare. Additionally, Obamacare’s mandates aggravate the cost problem by discouraging young persons from enrolling in coverage, leaving the insurance pools with older and less healthy enrollees and ignoring the needs and preferences of customers.
The Centers for Medicare and Medicaid Services (CMS) reported that in the federally supervised health insurance exchanges (39 states), between 2013 and 2017, average monthly premiums increased from $232 to $476—a 105 percent increase.[REF] CMS concluded that insurance plans’ high premiums and the lack of affordability in these markets is the main reason that individuals are cancelling or terminating their coverage. Between 2014 and 2017, about one million individuals per year dropped their coverage.[REF]
Soaring health insurance costs are hammering customers in non-group coverage, leaving those customers to navigate the wreckage of severely damaged individual markets. Health plan withdrawals are contributing to rapidly declining market competition and thus restricting consumer choice. In 2018, according to a recent New York Times report, about 45 percent of U.S. counties will have either one or no insurers offering coverage in the Obamacare exchanges.[REF] Meanwhile, customers are discovering that their coverage choices are increasingly limited to plans with high deductibles and narrow physician networks.
Obamacare’s excessive regulatory regime directly contributed to this state of affairs. Three particular culprits are the “3-to-1” age-rating mandate,[REF] the actuarial value mandate,[REF] and the essential health benefits mandate.[REF]
Addressing Obamacare’s Damaging Mandates
What the Senate Bill Gets Right. Like the House bill, the Senate bill eliminates Obamacare’s individual mandate and employer mandate penalties, repeals its age-rating mandate, and allows states to waive the “essential health benefits” mandate, the actuarial value mandate (which the House bill would repeal), as well as other insurance mandates.
The Senate bill expands the allowable age-rating variation for adults from a ratio of 3-to-1 to a ratio of 5-to-1, which enables insurers to set premiums to match the normal variations in average medical expenses by age. This change would allow insurers to once again charge young adults premiums commensurate with their lower expected medical costs, and thus price their plans to be more attractive to younger, healthier individuals. It reverses Obamacare’s “age-rating compression,” which significantly increased premiums for young adults—contributing to lower-than-expected enrollment by those individuals in Obamacare-compliant coverage.
The Senate bill also allows states to apply for waivers from other Obamacare insurance mandates, including the requirements that plans cover specified “essential health benefits” and provide minimum actuarial value.[REF]
Rather than creating a new waiver process (as the House bill would), the Senate bill simplifies and streamlines a waiver process in current law (referred to as Section 1332).[REF] That approach allows states to waive more insurance market provisions than the House bill. Section 1332 allows states to apply to the Secretary of Health and Human Services and get a waiver from 11 statutory provisions, including the individual and employer mandates, the actuarial value mandate that determines coverage levels, the federal rules governing the definition of individual and small group coverage, the federal essential health benefit requirements, and federal standards for qualified health plans.[REF]
Therefore, on net, the Senate bill does more to free states from Obamacare’s insurance mandates than the House bill (when considering the combined effects of the waivers options and the statutory changes).
The Senate bill also eases state efforts to retake control of their health insurance markets by liberalizing the conditions for states to secure a waiver from existing rules. Under current law, states can get a waiver from Obamacare provisions under Section 1332 only if they can demonstrate to the Secretary of the Department of Health and Human Services (HHS) that their state insurance alternatives will provide coverage that is as “comprehensive” as Obamacare’s federal requirements. They also must be able to show that they can provide cost-sharing protections that meet Obamacare’s standards. Furthermore, their alternative design must enroll as many persons in coverage as Obamacare and not increase the federal deficit.[REF]
This approach is problematic because the language of Section 1332 is biased toward particular policy outcomes. Under Obamacare, liberal states could more easily secure a waiver to set up a “single payer” (government monopoly) insurance program, as California is exploring,[REF] than conservative states pursuing innovative market-based reforms, a robust expansion of consumer choice, or more intense market competition among more diverse and less costly health insurance options.
The Senate bill rightly addresses this problem by eliminating the requirements that under a waiver the coverage must be comparable in scope to that specified in Obamacare, as well as the requirement that a state’s alternative must cover as many persons as would Obamacare. By getting rid of these obstacles, while retaining the deficit neutrality requirement, Congress could give states the opportunity to pursue more aggressive reforms of insurance markets, allowing reforms to emerge in the “bottom-up” policy experimentation central to federalism.[REF]
Additional Steps the Senate Should Pursue. A major weakness of the Senate bill is that, unlike the House bill,[REF] it does not create enough incentives for continuous coverage—either directly or by permitting states to use the waiver process to adopt such provisions on their own. Such provisions are important to limiting the adverse selection and gaming effects that have driven up premiums under Obamacare.
The Senate bill should be strengthened by permitting states to experiment with different approaches for incentivizing continuous coverage. The House bill authorized insurers to impose a one-year premium surcharge on individual market applicants who lack continuous coverage at the time of enrollment or to charge those without continuous coverage risk-rated premiums for a year.[REF] The Senate should provide additional options, such as allowing states to authorize insurers to prohibit preexisting condition exclusions only for those individuals who can demonstrate continuous coverage during the prior year. The Senate also should provide flexibility for insurers to impose on those who do not maintain continuous coverage additional cost-sharing requirements (e.g., higher deductibles) for a limited period of time.
Additionally, the Senate should roll back Obamacare’s requirement to cover specified preventive services with no cost sharing charged to enrollees. Prior to Obamacare, plans typically covered most of those services already, obviating the need to mandate coverage. Also, a number of those so-called preventive services are actually diagnostic tests or procedures, and allowing insurers to set patient co-pays is an appropriate way to manage utilization.
Ensuring Medicaid Helps Those Most in Need
Medicaid is a means-tested health care and social services program for low-income children, pregnant women, and aged or disabled individuals. Obamacare expanded Medicaid eligibility to include able-bodied adults without children. Indeed, the Medicaid expansion has accounted for over 80 percent of the net increase in total (both public and private) health insurance enrollment since Obamacare’s coverage provisions went into effect at the beginning of 2014.[REF] The Senate bill rightly takes steps to better target Medicaid’s safety net to those who most need it to ensure that Medicaid reforms work for the long haul and provide access to better care.
What the Senate Bill Gets Right. The Senate bill (like the House bill) would end the open-ended entitlement of states to federal Medicaid funding. It would cap federal contributions to Medicaid spending, with the federal government instead allocating federal monies to state Medicaid programs on a set, per capita basis[REF] for the different covered Medicaid populations: children, the elderly, the disabled, and able-bodied adults, including those made newly eligible for Medicaid under Obamacare. The per capita funding amounts for a state would be determined based on average spending by the state for each category of enrollees, with total funding reflecting the number of enrollees in each category in the state.
The Senate’s per capita cap funding approach is a major reform, consistent with policies recommended over the years by conservative health policy experts.[REF] It represents a major improvement over existing federal payment arrangements and allows states greater flexibility in the administration of the Medicaid program. The per capita approach also offers the benefits of giving states stronger incentives to eliminate waste and fraud in the program; preventing states from gaming federal reimbursement formulas; and better targeting resources to the needy and most vulnerable to improve results.
The Senate bill also does more to maximize flexibility for state officials who wish to pursue new, innovative, and imaginative solutions for the care of the poorest and most vulnerable members of society. In Medicaid, it facilitates the approval of Medicaid waivers. For example, any state with a “grandfathered” managed-care waiver can continue that waiver as long as it is budget neutral and any modified managed-care waiver would be deemed approved unless the Secretary of HHS not later than 90 days [after the date of application] denies the waiver application or requests more information.[REF] Likewise, the Senate bill encourages fast-track approval of home and community-based waivers if a state determines the waiver would “improve patient access to services.”[REF] The Senate bill also encourages cooperation and coordination with state officials by requiring the Secretary to establish a “process for soliciting advice from state officials that administer a state Medicaid plan.”[REF]
Additional Steps the Senate Should Pursue. There are several ways the Senate should improve the Medicaid provisions to ensure the program helps those most in need.
First, Medicaid tends to provide less access to providers and poorer quality of care than private insurance. Many Medicaid enrollees cannot find a doctor to take care of them because the reimbursement rates and the regulatory system discourage physician participation in the program. Low-income able-bodied adults cycling on and off of Medicaid as their employment and incomes fluctuate experience disruption in their health care coverage. Enabling those individuals to instead access mainstream private insurance coverage would improve continuity of coverage and access to higher quality care.
Therefore, the Senate should convert existing Medicaid and Children’s Health Insurance Program (CHIP) funding for able-bodied adults and children into a premium-support program so those beneficiaries can enroll in private health insurance plans—and thus be able to secure access to the same doctors and medical professionals as their fellow citizens. This would help them obtain the same basic coverage and care as more affluent individuals, while also augmenting efforts to create more stable insurance markets. Such a reform would increase their access to the quality care that they need, and would increase the number of younger and healthier persons enrolled in the nation’s private health insurance pools.
Second, an effective per capita approach requires that federal contributions grow over time at rates that are realistic and consistent with achievable expectations for the ability of states to moderate future spending. If the indexing formula is too generous, the incentives for states to better manage their programs will weaken over time.
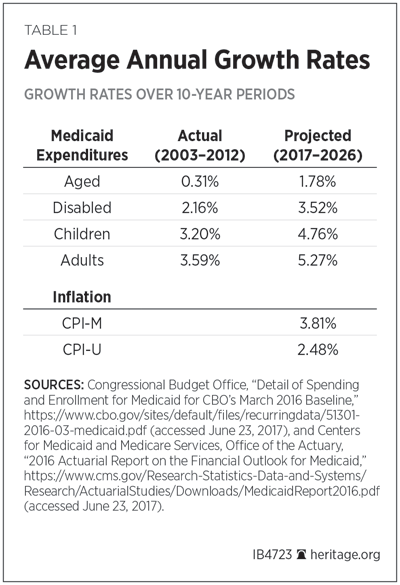
From the years 2020–2024, the Senate bill would index federal Medicaid payments under the per capita cap system by medical inflation for different groups. From 2025 onward, it would be based on Consumer Price Index for All Urban Consumers (CPI-U), a conventional measure of inflation. This is a blunt instrument on both counts, possibly resulting in overpayments or underpayments for very different categories of Medicaid beneficiaries based on the timeframes.
A better policy is to calibrate spending increases for different categories of beneficiaries based on projected spending for their services, and the use of inflation indexes should reflect those differences. Therefore, the Senate should revise the indexing provisions in the bill to better match them to the historic and projected growth rates of the different beneficiary groups, as reported in the accompanying table.[REF]
Third, the Senate should go further to ensure states have the flexibility they need to manage their Medicaid programs. The Senate should take such steps as giving them explicit authority to set and manage eligibility for their Medicaid programs through a range of means such as asset tests.
Moreover, the Senate should ensure that Medicaid focuses—as soon as possible—on the most vulnerable by removing Obamacare’s excess federal funding for newly eligible able-bodied adult recipients. Under the Senate bill, on January 1, 2021, the enhanced federal match rate goes to 85 percent for all enrollees immediately. The House bill, in contrast, takes the better approach of grandfathering the extra federal funding for expansion enrollees until January 1, 2020, as long as they remain continuously enrolled—and only in states that had expanded Medicaid by March 1, 2017, with federal funding for any new expansion enrollees set at the applicable per capita amount.[REF]
Importantly, the Senate should recognize that the current bill’s proposal to give states an option for setting work requirements on able-bodied Medicaid recipients will not be particularly effective.[REF] Most states will simply ignore the option. Its enforcement is very difficult in a society that provides emergency medical care to all. Medicaid work requirements could be circumvented easily by simply dropping out of the program and seeking emergency medical care when needed, at which point the individual would be re-enrolled in Medicaid, with the potential to repeat the cycle again. There are far better options for pursuing work requirements in other welfare programs that have been consistently ignored by Congress.[REF]
Other Ways to Undo Obamacare’s Damage
Repeal the Cadillac Tax. Obamacare imposed a 40 percent excise tax—often referred to as the Cadillac tax—on “high-cost employer-sponsored health coverage.” The provision set per-enrollee maximum allowable amounts for employer health plan costs and then applied the excise tax to any health plan spending above those amounts. This provision is scheduled to take effect in 2020. Its retention would have a major negative impact on the health care sector of the economy. Additionally, the tax is a blunt and punitive remedy that effectively forces employers to avoid the tax by reducing plan benefits.
The Senate bill further delays the effective date of the Cadillac tax until 2026, forgoing the opportunity to permanently repeal it. The Senate should couple repeal of the Cadillac tax with a critical reform of the tax treatment of employer-based health care in the form of setting a limit on the amount of pre-tax contributions to employer-sponsored health insurance.
Move Toward Equity in Health Care Tax Policy. Economists across the political spectrum have long argued that the current policy of providing an unlimited exclusion from taxation for income received in the form of employer-sponsored health benefits is a major systemic driver of health care costs. By its special treatment of employer-based coverage, the policy also undermines portability of coverage, contributes to the opacity of health care costs, distorts health care markets, and limits consumer choice and competition, and is regressive in its application to American workers and their families.
A cap is an appropriate correction for these economic distortions. Capping pre-tax contributions would encourage employers and workers to seek better value for money spent on health care without the rigidity of the Obamacare excise tax, which effectively forces employers to limit the scope of health benefits plans. Such a policy would be consistent with the pre-tax funding limits set in law for other employee benefits, such as contributions to retirement savings, group term-life insurance, and dependent care expenses.
Moreover, capping the exclusion can be coupled with a reform to let individuals with employer-sponsored benefits choose whether they want to use the existing tax exclusion or the new tax credit. This option would especially benefit lower-wage workers, who likely would benefit more by opting for the tax credit and may be more likely to accept offers of employer-sponsored coverage. Moreover, employers in lower-wage industries may be induced to offer coverage.[REF]
Improve Health Savings Accounts. Finally, the Senate should go further in helping Americans save for health care through Health Savings Accounts (HSAs), which allow individuals to save money for their health expenses in an account they own and control, without losing the money at the end of the year. These accounts are a marked improvement over other tax-privileged choices like Flexible Savings Accounts, in which the user has to “use or lose” the money annually. HSA adoption in both the individual and the employer-sponsored health insurance markets has increased significantly in recent years.
HSAs offer two significant advantages. First, account holders are able to exercise more direct control over how their health care dollars are spent and have the ability to pocket the savings from obtaining better value care (as opposed to savings accruing to their insurer). Second, they give Americans both an incentive and a mechanism to save for future health expenses.
Two key problems with HSAs limit their usefulness. Individuals must buy a high-deductible insurance policy to contribute to the accounts, and they are limited in their ability to save in these accounts. The Senate bill, like the House version, addresses the latter issue by increasing allowable contribution amounts for HSAs.[REF]
The Senate should go further and permit HSAs to be used with any type of insurance plan, not just high-deductible policies. They also should ensure HSAs can be used as repositories for contributions from public or private sources in order to assist lower income individuals to finance health insurance and medical care. These changes also would ensure neutrality with respect to any incentives for spending on health insurance versus spending on medical care directly.
Conclusion
Obamacare produced escalating premiums and higher deductibles—and reduced access to insurers and providers. Congress must act with urgency to begin reversing Obamacare’s damage and putting health insurance markets back on a more stable footing. Starting with this current legislative effort, the Senate should maximize its opportunity to provide individual Americans with better and more affordable health care options by making further changes to free states from Obamacare’s centralized insurance mandates, improve Medicaid reform, and provide individual Americans with better health care options.
Even with these changes, significant work remains to undo the damage of Obamacare and resolve the problems in the American health care system that preceded it. Future reforms will need to be part of an ongoing process at both the state and federal levels. Congress will have to address issues left out of this bill, such as the Medicare program, which remains in need of fundamental reform. Similarly, the cost of health insurance is a product of the cost of medical care. Ultimately, those costs will be controlled only by additional reforms—at both the state and federal levels—that create more consumer-driven market incentives for medical providers to offer better value care and empower consumers with options to seek better value.
The list of reforms needed for an ailing health care system is long. Congress must maximize every opportunity to bring Americans relief.
—Edmund F. Haislmaier is a Senior Research Fellow in the Center for Health Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Robert E. Moffit, PhD, is a Senior Fellow in the Center for Health Policy Studies. Robert Rector is a Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity. Marie Fishpaw is Director of Domestic Policy Studies.





