Obamacare’s seismic effects on insurance markets continue to be felt nearly eight years after its enactment. Enrollment in individual-market coverage is now declining, despite tens of billions of dollars in federal subsidies.[REF] The number of small firms offering health benefits to their workers dropped by 24 percent between 2012 and 2016.[REF] Premiums for individual coverage more than doubled between 2013 and 2017,[REF] and rates rose again in 2018.
This study examines how the Affordable Care Act’s (ACA’s) regulatory regime contributed to premium increases in the individual market. In some cases, estimates exist for the premium effects of particular provisions. The effects of several provisions, however, cannot be isolated from those of other closely related requirements. We present the estimated premium effects of these provisions in the aggregate, as they are presented in the studies on which we relied.[REF] The findings of those studies are discussed in this Backgrounder and summarized in the appendix.
Using data from those studies, this paper presents estimated effects of various ACA provisions on individual-market premiums. We group these provisions into four categories, ranging from those whose effects are readily isolated and qualified to those whose effects can be quantified only in combination with related provisions.
In general, we found that:
- Certain provisions of the ACA—including taxes and fees, essential health benefits, and actuarial value requirements—exerted discretely measurable and direct increases in premiums.
- Other provisions, particularly the new rules on adjusting premiums for age and sex, primarily had the effect of redistributing costs from some enrollees to others, but to some degree likely exerted a secondary effect on premiums by altering the composition of the resulting pool of enrollees. For example, the ACA’s requirement that people in their 60s be assessed premiums that are no greater than three times the premiums paid by those in their 20s redistributes costs from older individuals to younger ones. That requirement, however, could have exerted a secondary effect on premiums to the extent that it resulted in older adults being disproportionately represented in the insurance pools.
The largest effect on premiums consists of a cluster of ACA insurance-access requirements—specifically the guaranteed-issue requirement and the prohibitions on medical underwriting and applying coverage exclusions for pre-existing medical conditions under any circumstances. This cluster of regulations collectively accounts for the largest share of premium increases.
Other provisions of the law further magnified the premium effects of the ACA insurance-access requirements. For instance, to prevent adverse selection (and limit program cost) the law specified that anyone with access to affordable employer-sponsored coverage could not receive subsidized coverage through the individual-market exchanges. Yet the law did not apply that rule to those with employer-continuation coverage or early retiree coverage. Thus, the ACA permitted—and encouraged through generous subsidies for exchange coverage—the migration of a significant number of older people in poorer health from the employment-based market into the individual market.
Taxes and Fees
The ACA established a number of new taxes and fees on insurance companies, which these companies passed on to their customers in the form of higher premiums. Estimating the effect of these taxes and fees on premiums is fairly straightforward. Actuarial services firm Milliman projected that, in 2014, taxes and fees would increase premiums by around 4.4 percent.[REF] That increase would consist of:
- An increase of 2 percent due to the health insurance tax. The ACA required imposition of this tax, which was set at a level that was to raise $8 billion for the federal government in 2014.
- A market average increase of 1.4 percent attributable to health insurance exchange user fees. The Department of Health and Human Services (HHS) imposed a 3.5 percent of premium fee on products sold through the federal exchange. The state-run exchanges imposed similar fees. Given that the market would consist of both on and off exchange products, Milliman estimated that on a market-wide basis the average premium effect would be 1.4 percent.
- A further 1 percent increase in premiums for various other fees imposed on insurers by the ACA.
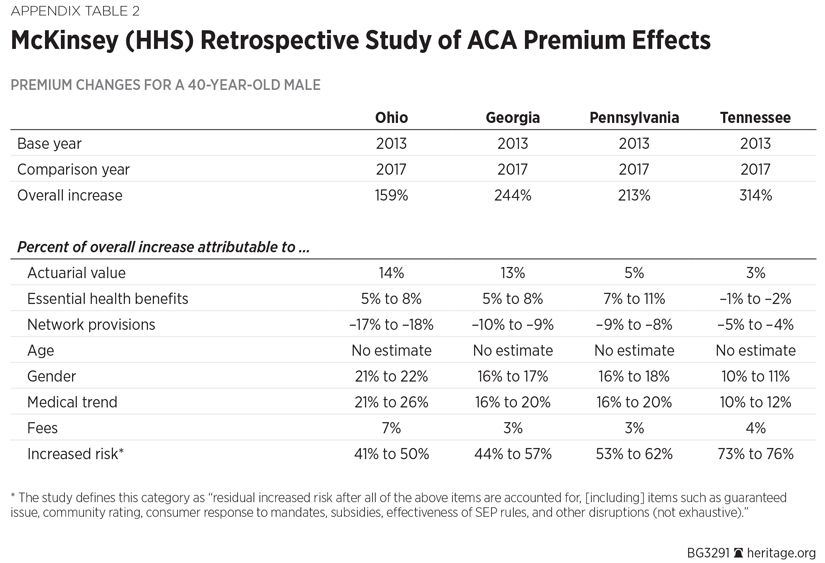
The retrospective study by McKinsey and Company implies that the actual effect of these taxes and fees may have been less than the Milliman projection. For example, premiums for a 40-year-old male in Ohio rose by 159 percent between 2013 and 2017, according to the McKinsey analysis. Taxes and fees accounted for 7 percent of that increase, which would suggest an average annual premium effect of 2.8 percent.[REF]
This lower estimate may be partly due to the fact that Congress placed a moratorium on the tax for 2017.[REF] It may also be partly attributable to the fact that Milliman underestimated how large premium increases associated with other ACA provisions would be. Taxes and fees (other than the exchange user fees) were fixed. Premiums were not. Since those premiums rose more than the Milliman analysis suggested, taxes and fees constituted a smaller-than-expected relative share of the premium increases.
Coverage Mandates that Increased Premiums
Essential Health Benefits. Obamacare requires health plans in the individual and small-group markets to cover a set of “essential health benefits.” The Milliman study estimated that the average premium increase attributable to expanding coverage to meet the law’s essential health benefits requirements could range from 3 percent to 17 percent, depending on the state.[REF] The variations are attributable to the extent to which prior state benefit requirements already matched the new federal requirements. If a state already required coverage of a particular benefit—for instance, prescription drugs—at a level meeting the new federal standard, there would be no resulting premium increase. In cases where there was no previous state requirement, or the previous state requirement was less stringent than the new federal standard, the need to expand coverage to comply with federal law would result in premium increases.
Most of the available actuarial studies commissioned by individual states prior to implementation of the law also arrived at estimates within the same range.
The McKinsey retrospective study for HHS found similar results—estimating that complying with the essential health benefits requirements accounted for an estimated 5 percent to 8 percent of premium increases in Ohio and Georgia and 7 percent to 11 percent in Pennsylvania. On an annualized basis, these increases are generally in line with the Milliman projections.
Preventive Services Requirement. The ACA’s prohibition on plans charging enrollees co-payments for certain preventive services was likely responsible for an additional 1 percent to 2 percent increase in premiums. In the impact analysis that accompanied its 2010 regulation implementing the preventive services mandate, the HHS estimated that imposition of the preventive services mandate would increase premiums by about 1.5 percent.[REF] Because most health plans already covered most or all of the specified preventive services, the increase in premiums was mainly the result of costs shifted from out-of-pocket payments to premiums, plus some additional utilization of covered services. The McKinsey study did not analyze the effect of this provision.
Minimum Actuarial Value. “Actuarial value” is a calculation for measuring the share of medical spending that a health plan can be expected to reimburse for in-network covered benefits for a standard population. The minimum actuarial value requirement in the ACA effectively establishes a floor for what plans must pay toward the cost of covered services.[REF] The law standardizes plans into four “metal” tiers (Bronze, Silver, Gold, and Platinum) according to actuarial value. It specifies that the actuarial values must be 60 percent for Bronze plans, 70 percent for Silver plans, 80 percent for Gold plans, and 90 percent for Platinum plans. Thus, plans may no longer have an actuarial value below 60 percent.[REF]
One study estimated that 51 percent of enrollees in pre-ACA individual-market plans were in plans with actuarial values of less than 60 percent.[REF] The study also found that most of the enrollees in plans with actuarial values of less than 60 percent were in plans with actuarial values of between 50 percent and 59 percent. Thus, the distribution of enrollment by plan actuarial value level reported in the study indicates that more than 85 percent of enrollees in pre-ACA individual-market coverage were in plans with actuarial values of 50 percent or greater.[REF] That is relevant given recent proposals in Congress to allow the sale of “Copper” plans with an actuarial value of 50 percent.
Another analysis of pre-ACA individual-market coverage in a number of states estimated that imposing the ACA’s minimum actuarial value of 60 percent on all plans likely resulted in a market average premium increase of 8.5 percent.[REF] As with benefit mandates, the effects of the ACA’s minimum actuarial value requirement varied by state depending on the share of pre-ACA plans in the state with actuarial values lower than 60 percent. For instance, an analysis of the Colorado market found that a smaller share of plans in that state did not meet the new federal minimum. It determined that “about 39% of those in the individual market hold plans with an actuarial value below this level,” and estimated that “enforcing this new minimum standard will therefore raise premiums by 5.3% on average.”[REF]
The McKinsey study confirms this state variation.[REF] It attributed 14 percent of the 159 percent premium increase for coverage of a 40-year-old male Ohioan between 2013 and 2017 to the ACA’s actuarial value standards. That would compute to an average annual premium effect of 5.5 percent. In Tennessee, the actuarial value requirement accounted for only 3 percent of the 314 percent premium increase between 2013 and 2017, an annual premium effect of around 2.4 percent.
Rating Restrictions that Redistributed Premiums
The ACA prohibits insurers from varying premiums on the basis of sex and limits the allowable age-based variations in premiums for adults. Neither of those requirements directly increase total coverage costs for health plans. However, they do force insurers to adjust premiums for some enrollees either up or down. Those required adjustments to premiums might have some effect on enrollee decisions to purchase coverage—as marginally reducing the premium for some enrollees makes the coverage more attractive to them, while marginally increasing the premium for other enrollees makes the coverage less attractive to them.
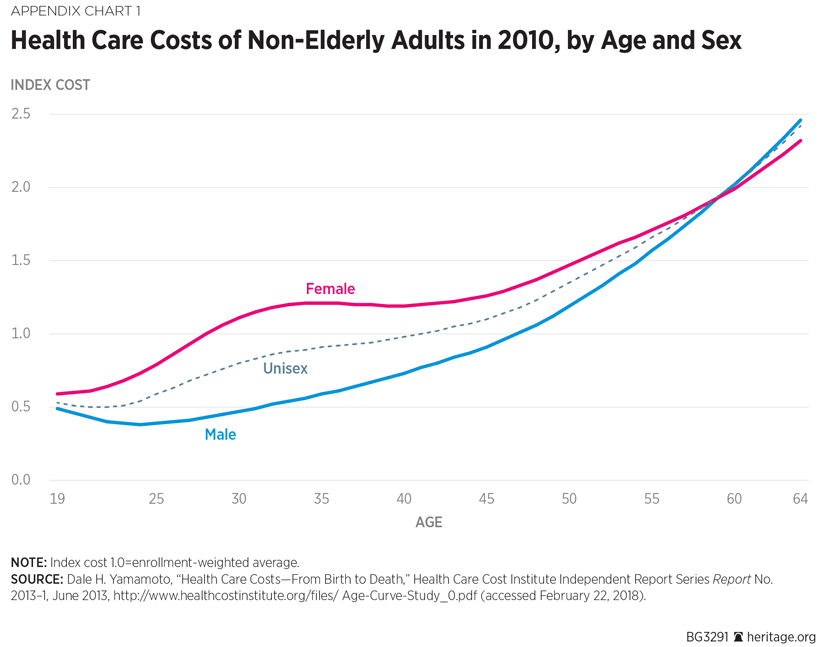
Prohibition on Rating by Sex. Analyses of claims data by sex and age show that, starting in the late teen years, women begin to incur higher health spending than men. That difference steadily widens until the mid-thirties. Then the pattern reverses, with the difference in health spending between women and men steadily narrowing until around age 60, when the lines cross and men begin to cost more than women. Thus, it could plausibly be inferred that the ACA’s prohibition on varying health insurance rates by sex might make the resulting premiums more attractive to middle-aged women and less attractive to middle-aged men.[REF]
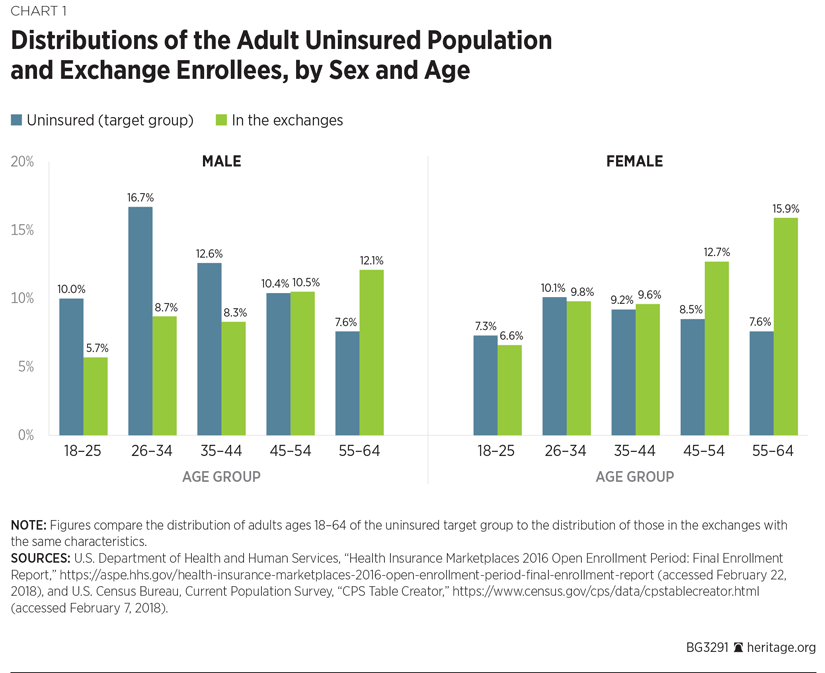
The data presented in Chart 1 compares the distribution of the target uninsured population by age and sex with the same distribution of exchange enrollees.[REF] Chart 1 shows that, regardless of age, women are less likely than men to be uninsured and more likely to be enrolled in exchange-based coverage.
Particularly notable is that women in the age cohorts of 18 to 24, 26 to 34, and 35 to 44 account for about the same share of the uninsured and exchange enrollee populations. Thus, while the ACA’s prohibition on varying rates based on sex reduced the premiums for middle-aged women, it does not appear to have resulted in meaningfully higher female exchange enrollment. However, Chart 1 also shows that for men in those same three age cohorts their shares of the exchange enrollee population are between one-half and two-thirds of their respective shares of the target uninsured population. Thus, the fact that premiums increased for middle-aged men because the ACA prohibited insurers from varying premiums based on sex may have contributed to lower enrollment by men in exchange coverage, relative to what could otherwise have been expected given their shares of the uninsured population.
Age-Rating Compression. Obamacare limits age variation of premiums for adults to a maximum ratio of three to one.[REF] In other words, for the same plan, an insurer is not permitted to charge a 64-year-old a rate that is more than three times the rate it charges a 19-year-old. Yet the natural age variation in medical costs among adults is about five to one.[REF] Thus, the effect of this mandated “rate compression” is to force insurers to artificially underprice coverage for older adults and artificially overprice coverage for younger adults. Analyses of this provision find that the ACA’s three-to-one limitation increased premiums for younger adults by around one-third, while reducing premiums for pre-retirement-aged adults (50 to 64 years) by about 10 percent to 15 percent.[REF]
While younger adults tend to be in better health, they also tend to earn less than older workers with more experience. That combination makes young adults more sensitive to changes in the price of health insurance and more likely to decline coverage if it becomes more expensive. Thus, imposing rating rules that artificially increase health insurance premiums for young adults marginally increases the cost of coverage for those who are already most likely to be uninsured.
To the extent that the ACA’s rate compression makes premiums more attractive for older adults and less attractive for younger adults, it can contribute to unfavorably skewing the risk mix of the market—in turn, forcing insurers to raise premiums further across the board.
The data presented in Chart 1 indicate that the ACA’s age-rating provision was likely a contributing factor in skewing exchange enrollment toward older, more expensive adults. Chart 1 shows that, relative to their shares of the uninsured population, women aged 18 to 25 are slightly underrepresented among exchange enrollees, while men aged 18 to 25 are significantly underrepresented. At the same time, both women and men aged 55 to 64 account for significantly larger shares of exchange enrollment than of the target uninsured population.
Insurance Rules that Increased Selection Effects
The insurance regulations that appear to have had the greatest effect on premiums are those requiring access to coverage for individuals with medical conditions—specifically the guaranteed-issue requirement, and the prohibitions on medical underwriting and applying coverage exclusions for pre-existing medical conditions.
Considered as a whole, this regulatory regime requires people in reasonably good health to pay higher premiums in order to finance the cost of adding more individuals in poorer health to the pool. While the effect is to make coverage more expensive and (and thus, less attractive) to healthy people, the architects of Obamacare believed that imposing a tax penalty for not buying coverage would compel healthy people to buy coverage anyway, despite the increased price.
In practice, that was not the case. Faced with a widespread negative response to the mandate among their constituents, Members of Congress reduced the penalties for most people to below the cost of coverage, created an automatic “affordability” exemption from the penalty that millions of healthy low-income uninsured could qualify for, and explicitly barred the IRS from enforcing the mandate.
The net result was a constellation of rules that repelled relatively healthy people and attracted those who could reasonably expect their medical bills to exceed their premiums—which Obamacare’s individual mandate simply failed to counteract.
None of the available studies identifies how much each provision in this category may have affected premiums. Instead, both the Milliman and McKinsey studies report large catchall categories that combine this cluster of regulations with other regulations, or with the effects of other provisions of the law.
Milliman designates this category as “Changes in Risk Pool Composition/Adverse Selection” and predicted that 2014 individual policy premiums would be 20 percent to 45 percent higher as a result of requirements in this category. The Milliman analysis attributed the change in risk pool composition to two overarching factors: (1) new market entrants—meaning new individual-market enrollees who previously had other coverage or were uninsured; and (2) adverse selection related to plan choice, single risk pool, and renewal timing.
New market entrants, which Milliman assesses would increase premiums by up to 23 percent, are discussed in the following section, “Other ACA Provisions that Increased Selection Effects,” which will examine other sources of adverse selection.
Milliman notes that new market entrants and existing enrollees can select coverage that best fits their expected use. People in good health can upgrade their coverage when their health deteriorates. Parents can put a child in good (or poor) health on a policy that is separate from the plan in which one or both parents are enrolled. Adverse selection results from this knowledge asymmetry—people are in a better position than insurance companies to predict their medical use, and insurers are in any event forbidden to price their product to match expected use. Adverse selection, in turn, requires insurers to increase their rates.
“The adverse selection,” the Milliman report states, “will increase the overall cost of the single experience risk pool because such adverse selection cannot be reflected in premium rates by benefit plan level.”
Similarly, the elimination of underwriting premium rate-ups and pre-existing condition exclusions required insurers to “adjust their 2014 premium rates to recoup the lost revenue collected [in 2013] because [2013] premiums were allowed to vary by health status.”
The McKinsey study suggests that the changes in risk pool composition may have been larger than Milliman had projected. However, it is difficult to make direct comparisons between what Milliman termed “Changes in Risk Pool Composition” and what McKinsey calls “Increased Risk.”
McKinsey includes in that category “guaranteed issue, community rating, consumer response to mandates, subsidies, effectiveness of [special enrollment period] rules, and other disruptions (not exhaustive).” As with the Milliman study, McKinsey defines this category broadly and estimates that it had a rather substantial premium effect.
The effect—again based on a comparison of premiums for a 40-year-old male in 2013 and 2017—varies by state. In Ohio, Milliman estimated that it accounted for 41 percent to 50 percent of the 159 percent increase in premiums over that period (an implied average annual increase of 18.1 percent). In Tennessee, it accounted for 73 percent to 76 percent of the 319 percent increase in premiums (an implied average annual increase of 59.4 percent).
In sum, it appears that as much as half the costs reported in these catchall categories may more appropriately be attributed to other ACA provisions that could have been crafted differently. In other words, a portion of the identified cost increases were an inevitable result of imposing these new regulations on the individual market, but the remaining portion was not inevitable. Rather, it was the result of other policy changes in the law (discussed in the next section) compounding the effect of the regulatory changes that exacerbated adverse selection against the individual market.
Other ACA Provisions that Increased Selection Effects
The effect of the foregoing regulatory requirements was to make health insurance more attractive to those in poor health and less attractive to those in good health, making the risk pool more costly to insure than if it more closely reflected the overall risk profile of previously uninsured people. Those selection effects were further exacerbated as older and less healthy individuals shifted onto subsidized exchange coverage from employment-based plans or state and federal high-risk pools.[REF]
Shift of High-Risk Pool Enrollees into Individual Market. Prior to implementation of the ACA, most states operated subsidized high-risk pools for people denied coverage in the individual health insurance market. With the implementation of the ACA exchanges and subsidies, almost all of those high-risk pool enrollees transitioned into the individual market. Pre-ACA, there were about 225,000 state high-risk pool enrollees. The number of enrollees and their cost varied by state, with annual average per capita claims ranging from $6,200 in West Virginia to $26,100 in Alaska.[REF]
The ACA also created a temporary national high-risk pool program—called the Pre-Existing Condition Insurance Program (PCIP)—that operated between 2010 and 2014. Enrollment in the PCIP peaked at 114,000 individuals. One analysis noted: “In 2012, average per enrollee claims costs for PCIP were $32,108, or more than 2.5 times higher than average per enrollee claims costs ($12,471) under traditional state high-risk pools, all of which continued to operate that year.”[REF]
Thus, about 340,000 state and federal high-risk pool enrollees were added to the individual market in the first years of ACA implementation. Furthermore, the costs that they imposed on the market were actually higher than the cost of their previous coverage as the law’s standards for comprehensive exchange coverage meant that they were able to enroll in exchange plans with more benefits and lower deductibles and co-pays than their previous coverage.
Shift from Continuation Coverage. Since 1986, federal law has required most employers to allow workers and dependents who are losing access to their employer-sponsored health insurance to pay a premium to continue coverage under the employer’s plan for a period of time.[REF] While payments for employer-sponsored health insurance are tax-free to workers, individuals with such “continuation coverage” typically have to pay the premiums for that coverage with after-tax dollars. One notable exception is the health care tax credit available to workers who are eligible for “trade adjustment assistance,” who may use that tax credit to offset premiums for continuation coverage.[REF]
The experience over the years with the continuation coverage requirement is that it resulted in significant selection effects, as those needing medical care were more likely to opt to pay for continuation coverage.
The ACA specifies that individuals with access to employment-based coverage are not eligible for subsidized exchange coverage. However, the ACA does not treat continuation coverage as employment-based coverage. Thus, individuals needing medical care who qualify for continuation coverage can turn down the offer of such coverage and instead purchase subsidized exchange coverage. In addition, the ACA treats the loss of employer coverage as an event qualifying for a “special enrollment period,” meaning that such individuals can enroll in subsidized exchange coverage right away without having to wait until the next open enrollment period. Furthermore, unlike the Trade Adjustment Assistance tax credit, the Obamacare tax credits can only be applied to exchange coverage, not to continuation coverage. While the take-up of continuation coverage is not tracked, it is reasonable to expect that, since implementation in 2014, a significant number of individuals qualifying for continuation coverage have opted for subsidized exchange coverage instead.
Migration from Early Retiree Coverage. Some employers offer health insurance coverage to early retirees until they are old enough to qualify for Medicare. As with continuation coverage, the ACA does not preclude those early retirees from turning down that coverage and opting for more generously subsidized ACA exchange coverage.
In fact, Obamacare included $5 billion for an “Early Retiree Reinsurance Program (ERRP).”[REF] The HHS states that the “ERRP was designed to help employers and other sponsors of employment-based health plans continue to provide coverage for early retirees until 2014, the initial year under the ACA in which insurance companies may no longer deny coverage based on pre-existing conditions, or charge more based on an individual’s health status.”[REF] Thus, the architects of Obamacare expected that some portion of early retirees would migrate into the new subsidized exchange coverage.
The HHS states that the employer plans participating in ERRP had over 2.6 million early retirees and that, “[b]ased on analysis of claims ERRP received, plan sponsors collectively requested reimbursement for more than 275,000 early retirees, spouses, surviving spouses, and dependents with significant health care costs (i.e., costs exceeding $15,000 in ERRP-eligible health care claims per plan year).”[REF]
There is no data on how many individuals with early retiree employer coverage have migrated into the exchanges since 2014. However, as Chart 1 shows, individuals in the early retiree age group (ages 55 to 64) are significantly over-represented in the exchanges relative to their share of the uninsured population. That indicates a shift into subsidized exchange coverage of already insured, higher-cost enrollees.
Enrollment Gaming. The regulations governing enrollment in subsidized exchange coverage have been “gamed” by some customers and medical providers in ways that increase costs for insurers, and thus, further drive up premiums. Another McKinsey analysis estimated that adopting changes to ensure more appropriate enrollment could reduce insurer claims cost for exchange coverage by as much as 10 percent.[REF]
One problem is that consumers have been able to wait until they need medical care before buying coverage and then enroll through a special enrollment period (SEP) outside of the annual open season. That was partly the result of the Obama Administration allowing SEPs for inappropriate events (such as a change in income that makes a person newly eligible for subsidies) and partly the result of failing to verify events that appropriately would trigger a SEP (such as a person claiming to have permanently moved to a different state). The McKinsey analysis estimates that about 4 percent of enrollees are enrolling inappropriately through SEPs and notes that those enrollees have claim costs that are three times higher than average.
A related problem that insurers have repeatedly noted is that of customers who, once they have received care, stop paying their premiums, even though they could afford to do so and keep their insurance. That means that less of their claims costs are covered by their own premium payments, and must instead be paid by other policyholders. McKinsey estimates that about 5 percent of enrollees stop paying for coverage prematurely.
Another significant issue is those enrollees with costly medical conditions who should be in other coverage such as Medicare or Medicaid. Those enrollees may prefer exchange coverage because plans above the Bronze level are likely to have lower out-of-pocket costs than traditional Medicare. At the same time, providers would rather have more of their patients in private plans paying better rates than in government programs. Consequently, patients with expensive conditions (such a kidney failure or HIV) have been enrolled in exchanges rather than in Medicare or Medicaid, and providers have even paid the enrollees’ shares of the premium for the exchange coverage. According to McKinsey, this type of inappropriate enrollment in exchange coverage involves less than 1 percent of enrollees, but the claims costs of those enrollees are a staggering ten times the average.
The Trump Administration attempted to address a number of these issues in its market stabilization rule, but the extent of those revisions was limited in some places by statutory requirements. More important, those changes have only been in effect since the middle of 2017—meaning that even if they help reduce costs, any savings will not be reflected in insurance premiums before next year.
Insurance Regulations with Uncertain Costs. The ACA also contains a number of other insurance regulations that were not included in various regulatory cost analyses.
Four of them—(1) summary plan description requirements; (2) uniform explanation of coverage requirements; (3) the requirements for insurers to have internal and external review processes for handling appeals of coverage determinations and claim denials; and (4) the requirements that insurers report to the Secretary on “quality of care”—impose additional administrative costs on insurers that are likely no more than marginal.
The requirement to cover individuals enrolled in clinical trials also likely imposes little cost on insurers, as it requires them to cover routine medical costs for such patients the same as for enrollees not participating in a clinical trial. It does not require plans to cover costs associated with the clinical trial itself, as those are the responsibility of the trial’s sponsor.
The requirement to extend dependent coverage to age 26 also likely added very little to plan costs, as prior to the ACA 37 states already imposed the same, or a similar, requirement.[REF] Thus, this provision primarily affected self-insured employer plans, which are not subject to state insurance laws.
Finally, the ACA’s prohibition on annual and lifetime coverage limits may have increased insurer costs somewhat, to the extent that the new federal rules exceeded prior state law. However, the plans most affected by these requirements were “limited benefit” or “mini-med” plans, which were already regulated as separate products (not as “major medical” coverage) under state laws and were almost entirely offered as employment-based plans for firms with predominantly low-wage workers.
Policy Reaction
Most of the ACA’s numerous regulatory changes disrupted markets and substantially increased premiums for individual insurance policies. The result is that the post-ACA individual-market risk pools skew older, less healthy, and more costly to insure.
Some states have sought to address this problem by obtaining waivers from the ACA’s single-risk-pool requirement. Section 1332 of the ACA permits states to apply for waivers from this requirement. Alaska sought and obtained such a waiver for the 2018 plan year.[REF] The state identified 33 medical conditions that were associated with high medical claims. It then segmented individuals with these conditions into an “invisible high risk pool,” effectively segregating their medical claims from the rest of the pool. They financed these medical claims through a combination of state assessments and federal funds that would otherwise have been paid directly to insurance companies as premium subsidies. The state presented actuarial evidence that this would be budget neutral for the federal government, because the risk mitigation would reduce premiums and, therefore, the total amount the federal government would pay in premium subsidies.
While Alaska’s results are promising, they are hardly conclusive. One study found that premiums for the lowest-cost Bronze plan in the state fell by 25 percent for 2018, the first year in which the waiver was implemented.[REF] However, Alaska is a unique state in some respects. Premiums for insurance are much higher in Alaska than in other states. Also, given the state’s relatively small population, the shift of high-risk pool enrollees into the individual market may have created a disproportionately larger adverse effect on Alaska’s individual market than it did in other states.
Moreover, the waiver process is not especially predictable. In 2017, for example, several states withdrew their waiver applications because the Centers for Medicare and Medicaid Services did not complete action on the applications in time to affect premiums for the 2018 plan year.[REF] Given their ad hoc nature and unpredictability, waivers are not the most effective way to address problems that are as severe and pervasive as rising premiums for individual coverage.
A more systematic approach to addressing the causes of rising premiums under Obamacare was advanced in September 2017 by Senators Lindsey Graham (R–SC) and Bill Cassidy (R–LA). Although needing policy refinement to achieve its underlying goals,[REF] the Graham–Cassidy measure would have consolidated several ACA funding streams into a program of grants to states. In conjunction with the funding, the legislation would also have given states more autonomy over the regulation of their insurance markets, allowing innovative regulatory approaches under which such markets could better function. For instance, states receiving such funds would not be bound by federal requirements on essential health benefits, actuarial value, or age rating.
Most important, the measure would release states from the single-risk-pool requirement, without having to pursue the waiver process. Graham–Cassidy also would permit states to use block grant funds to subsidize coverage for pools of individuals that present sub-standard risk. Under current law, a state must request a waiver from the single-risk-pool requirement. States that receive a grant under Graham–Cassidy are not subject to this requirement. The proposal was flexible in how a state might structure such a risk-mitigation program, listing reinsurance, high-risk pools, and risk adjustment among an array of acceptable approaches.
Looking Ahead
Some regulations—such as for taxes and fees, actuarial value, and essential health benefits—had discrete, measurable, and direct effects on premiums. For other regulations, such as those related to age and sex rating, the effect was indirect. Those rating rules generally redistributed premiums between cohorts, such as by requiring younger enrollees to finance premium discounts for older enrollees.
A cluster of regulations prohibiting medical underwriting and requiring coverage of pre-existing medical conditions exerted the most powerful effect on premiums. Those effects were exacerbated by other provisions in the ACA that altered pooling arrangements, such as allowing early retirees to migrate from employer-sponsored coverage and the termination of high-risk pools that forced those with chronic medical conditions to obtain coverage through the exchanges. The net result was a pool in which enrollment skewed older and sicker, forcing insurers to raise premiums.
The Administration has taken some steps to help mitigate these challenges but, as noted, these efforts alone can only go so far. Legislative action is the most effective approach. The Graham–Cassidy proposal offers a conceptual framework for empowering states to repair or ameliorate much of the market dislocation resulting from Obamacare.
Yet, the Graham–Cassidy framework is only the start. It should be further refined[REF] to ensure that the next phase of health reform focuses on constructing a more patient-centered health care system that gives Americans choices and control over their personal health care decisions.
—Edmund F. Haislmaier is Preston A. Wells, Jr. Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Doug Badger is a Visiting Fellow at The Heritage Foundation and Senior Fellow at the Galen Institute.
Appendix: Summaries of Major Studies Analyzed in this Report
Milliman Study (2013) for America’s Health Insurance Plans (AHIP)
This prospective study was prepared by Milliman, a large actuarial firm, for AHIP, an association of major health insurers. It estimated the effects of ACA regulations—sometimes individually and sometimes in a group—on individual-market premiums between 2013 and 2014. Because state regulatory schemes varied, it generally includes a range of estimates for each regulation or category of regulations, rather than point estimates.
The study’s major findings are summarized in Appendix Table 1.

McKinsey Retrospective Study of ACA Premium Effects (2017) for HHS
This retrospective study was prepared by McKinsey and Company, a global management consultant firm, for the Department of Health and Human Services. It was released in a July 2017 “Dear Colleague” letter by Senators Ron Johnson (R–WI) and Mike Lee (R–UT).
The study compared average premiums for a 40-year-old male in four states (Ohio, Georgia, Pennsylvania, and Tennessee) in 2013 with premiums for Silver plan coverage for a 40-year-old male in 2017 in those same four states.
The study’s major findings are summarized in Appendix Table 2.
Society of Actuaries Study of Lifetime Health Care Costs (2013)
This study used commercial data held by the Health Care Cost Institute and Medicare fee-for-service data to analyze health care cost differences by age and their contribution to overall health care cost change. The study also found that health care costs vary significantly by sex along the age curve. Women tend to incur higher medical costs until around age 60, at which point men’s costs eclipse those that women incur.
Appendix Chart 1 depicts the study’s finding on medical cost variation by age and sex. It also displays a “unisex” line showing the cost curve by age that would result from a legal prohibition (as in the ACA) on rating men and women separately. As the chart shows, the naturally occurring variation in costs between young adults and older adults is about 5:1. However, the ACA limits age variation of premiums to 3:1—that is, insurers cannot charge a 64-year-old a premium that is more than three times the premium charged to a young adult.