Plan year 2022 is the ninth year of operation for the health insurance exchanges created by the Affordable Care Act (ACA), known as Obamacare. It also marks the fourth consecutive year of increased insurer participation at both the state and county levels—a reversal of the prior trend of decreasing insurer participation during plan years 2016 through 2018, and a reflection of actions taken by the Trump Administration. Yet, new regulations by the Biden Administration could reverse these trends, driving up premiums and sparking renewed insurer exits.
State-Level Insurer Competition in the Exchanges
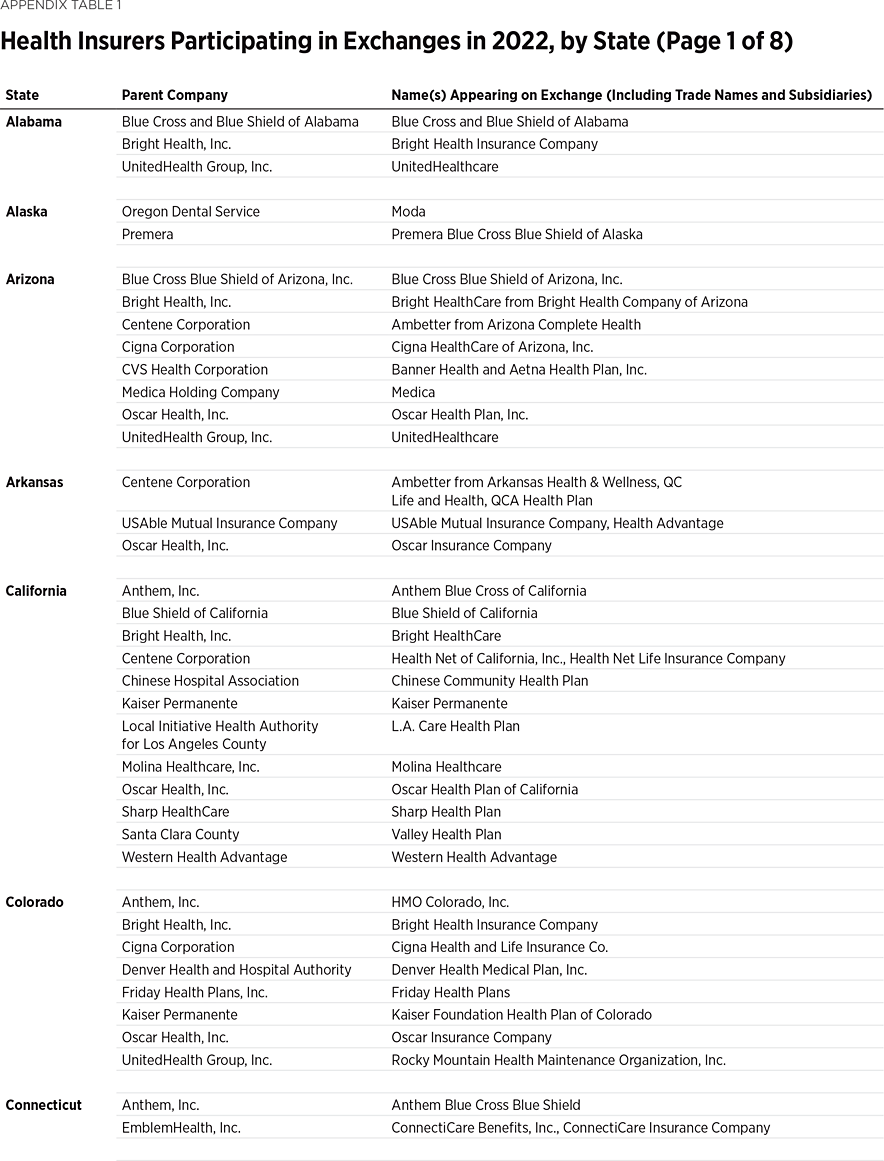
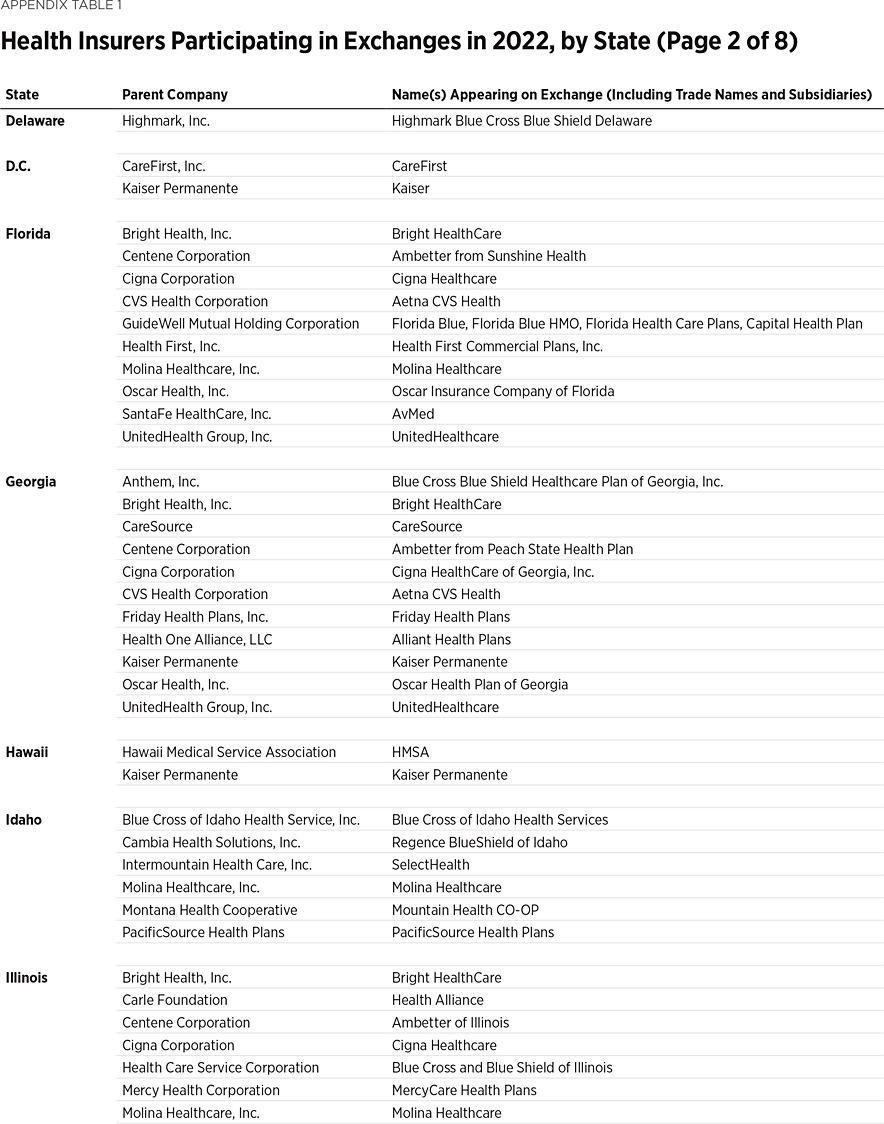
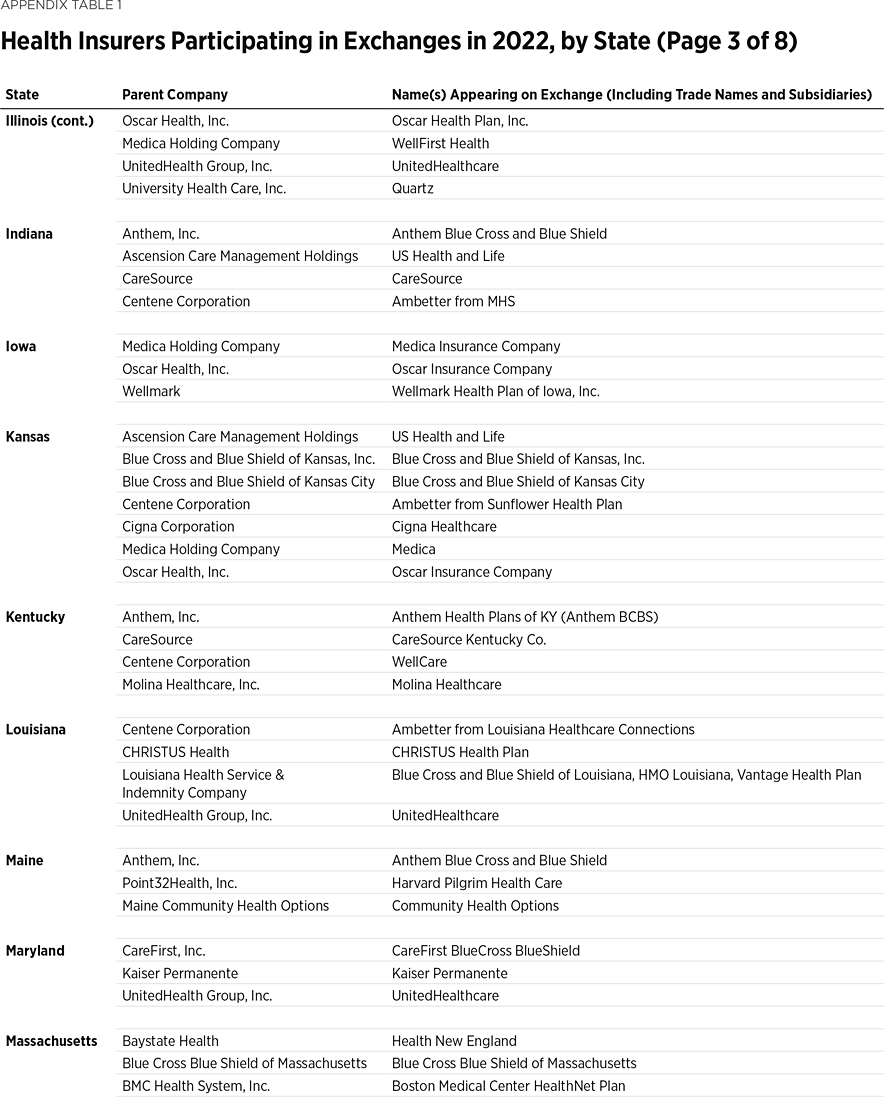
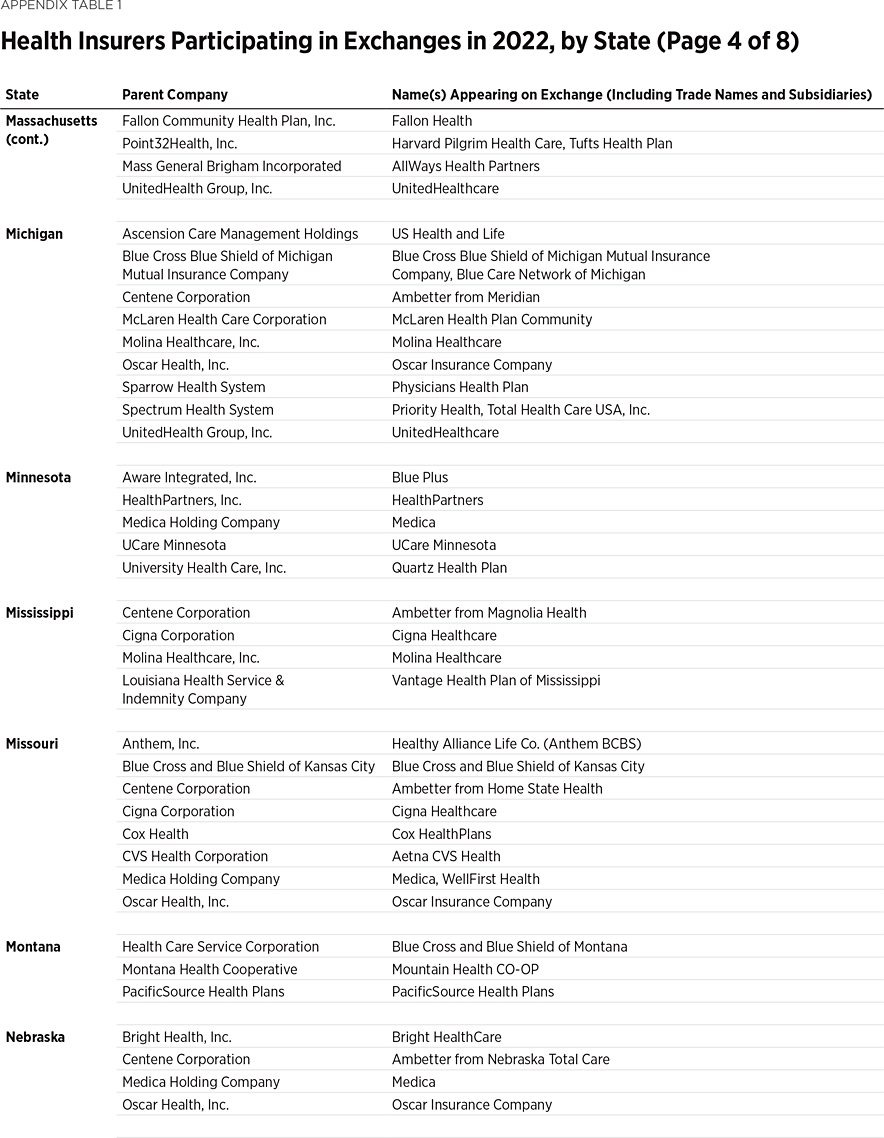
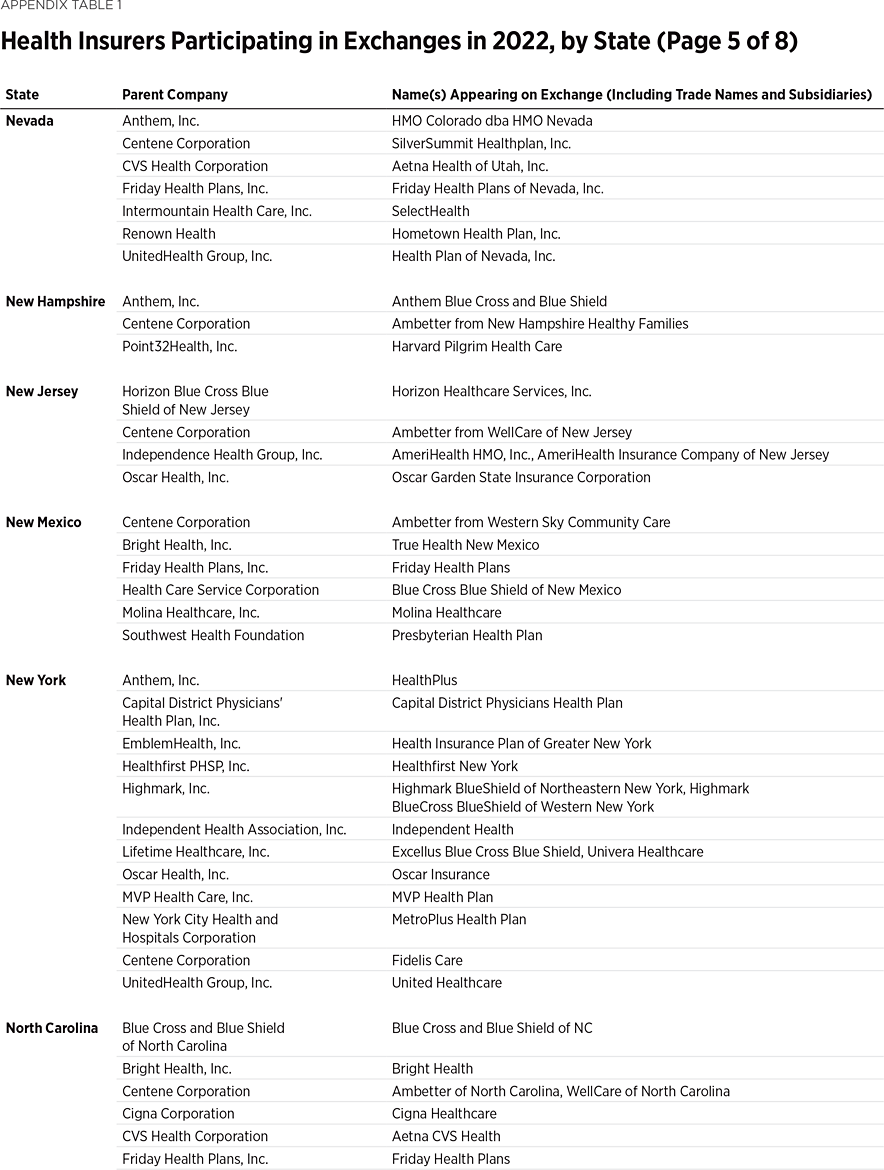
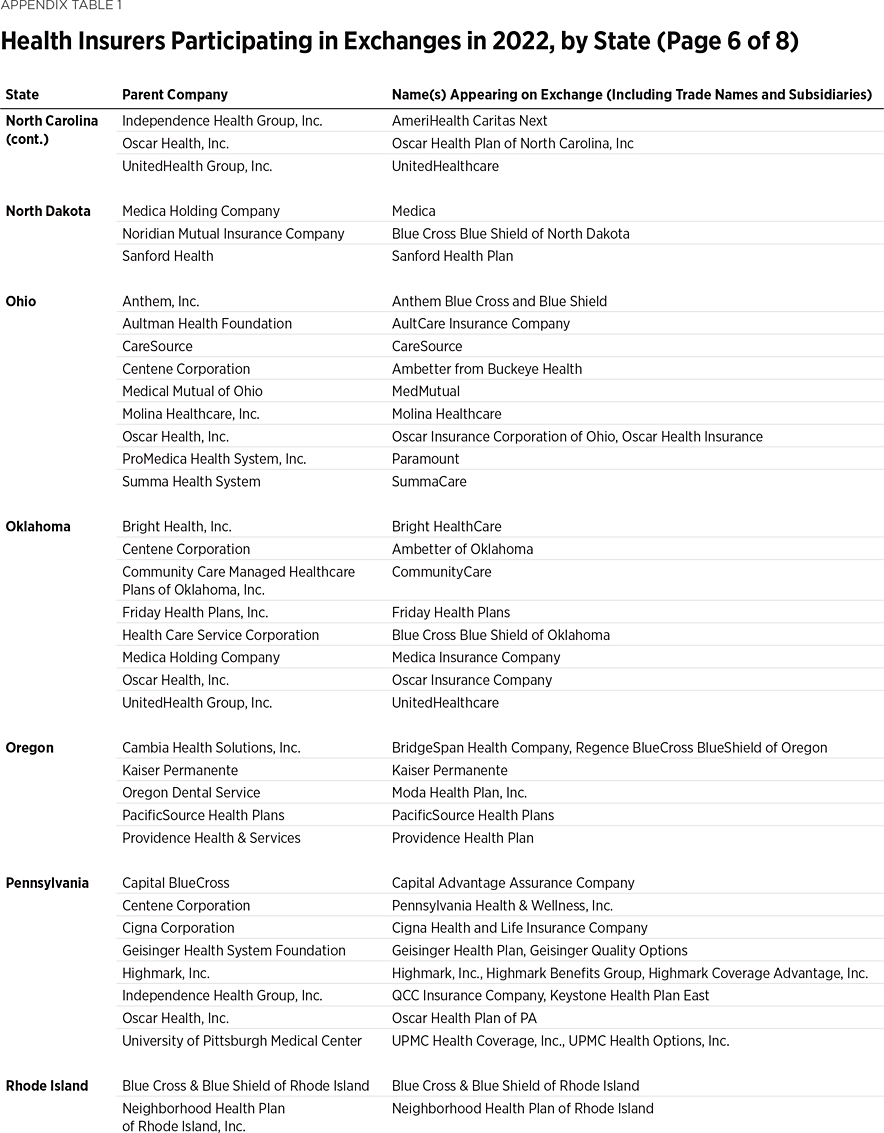
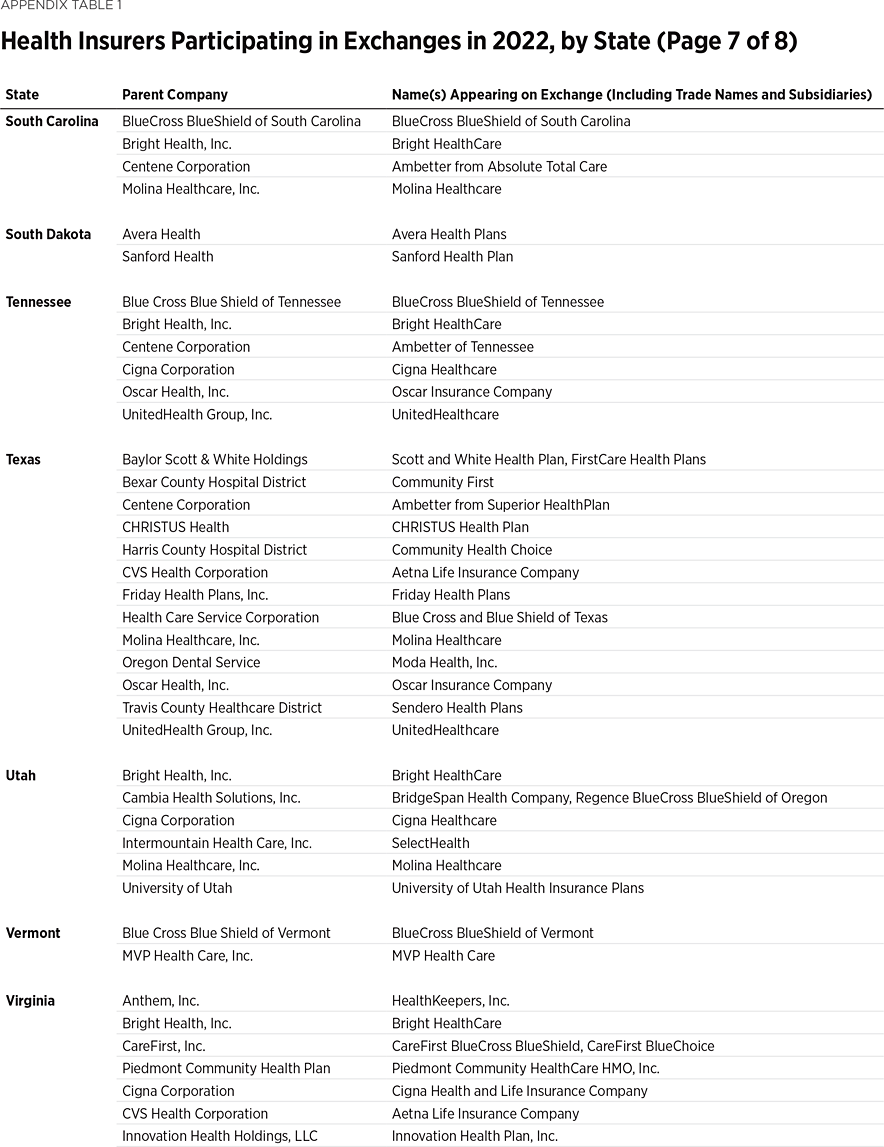
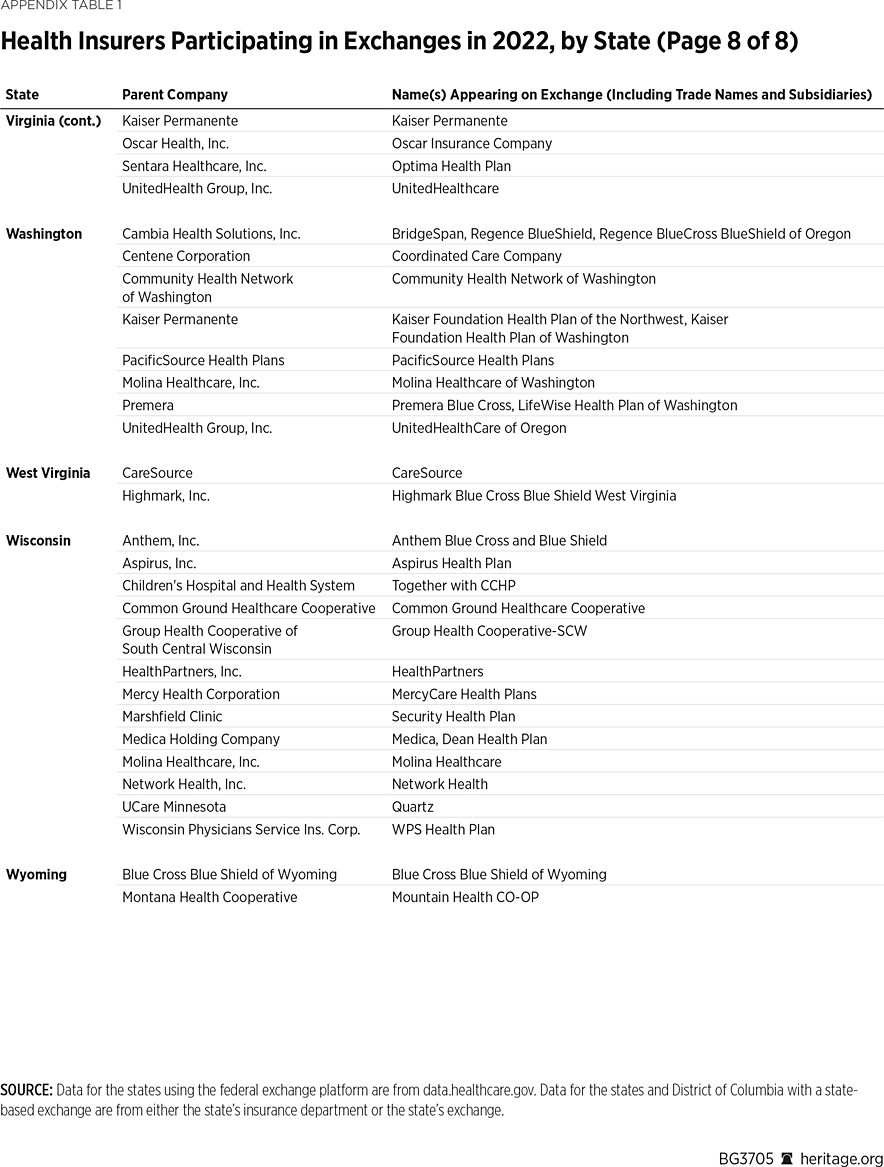
One way to measure insurer competition is to assess insurer participation on a state-by-state basis. That analysis, summarized in Table 1, shows the number of carriers in each state and the District of Columbia in the individual market in 2013, as well as in the exchanges each year since they began in 2014. Insurers that offer exchange coverage through more than one subsidiary in a state are counted as one carrier (the parent company), while insurers that offer coverage in more than one state are counted for each state (as exchange participation is a state-level decision).
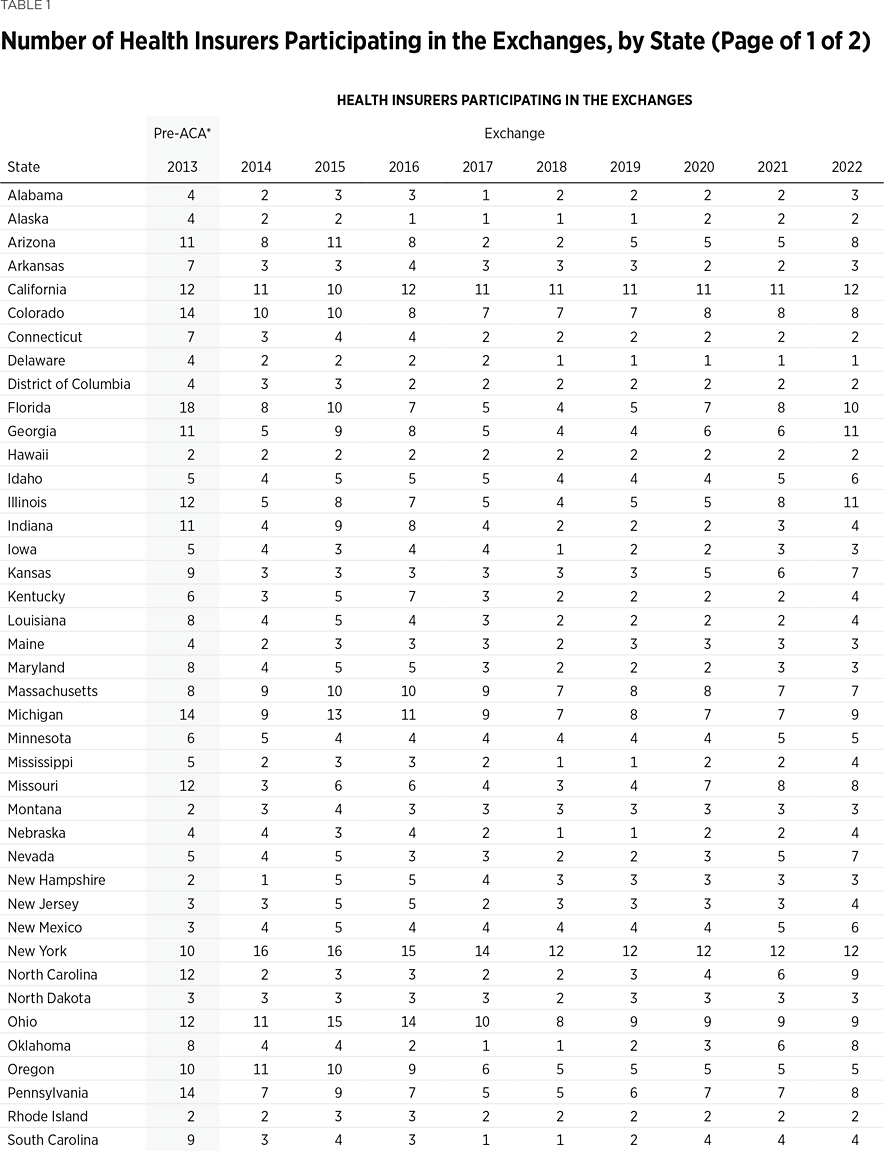
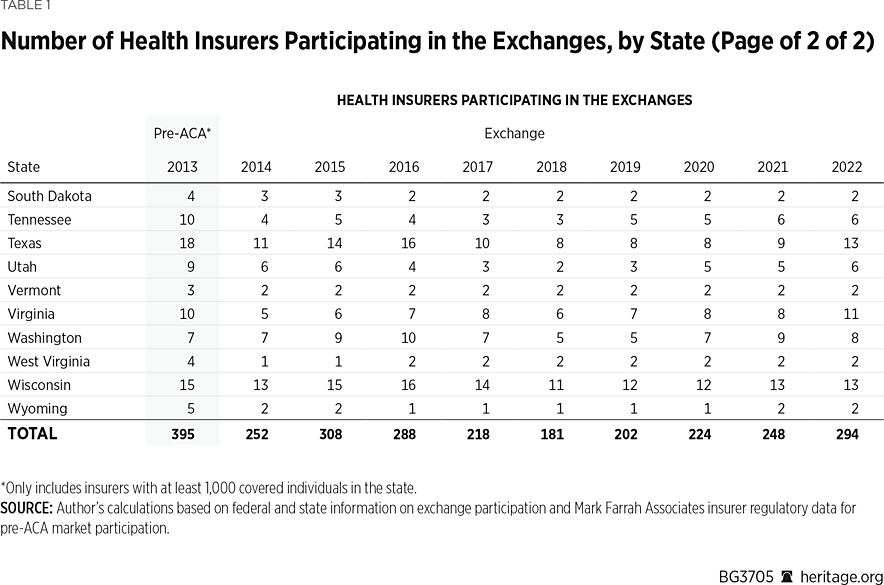
In 2013, the last year before Obamacare’s implementation, 395 insurers sold coverage in the individual market across all states and the District of Columbia. In 2022, 294 insurers are offering coverage through the Obamacare exchanges. That is an increase of 113 insurers over the low of 181 in 2018, but it still leaves the 2022 exchanges 25 percent less competitive than the individual market was before the implementation of Obamacare.
Table 1 shows that state-level exchange competition dropped significantly over the three plan years of 2016 to 2018 but rebounded in subsequent years (2019 to 2022). For plan year 2022, 24 states saw a net increase in the number of insurers offering exchange coverage, while one state (Washington) had a net decrease.
Over the past four plan years, the net number of insurers offering exchange coverage increased in 37 states and remained unchanged in 13 states and the District of Columbia. The year-to-year pattern of insurers entering and exiting the exchanges is shown in Chart 1.
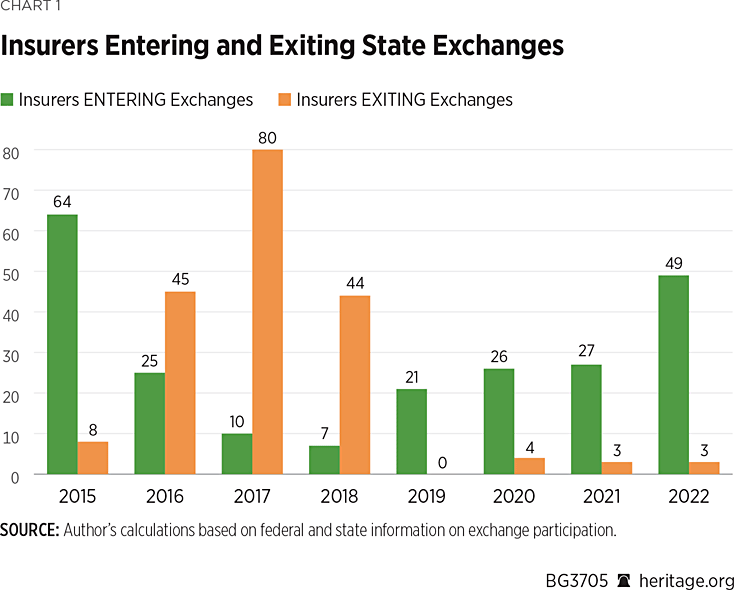
Yet, even with the increase in insurer participation over the past four years, only nine states have more insurers offering Obamacare exchange coverage in 2022 than were offering individual market coverage before the ACA, while seven states have the same number and 34 states and the District of Columbia have fewer.
2022 County-Level Insurer Competition in the Exchanges
Though state-level data are informative, the most tangible measure of competition for consumers is data at the county level. That is because health plans are offered, and priced, locally. Also, because many insurers only offer Obamacare exchange coverage in certain parts of a state, county-level data provide a more precise picture of the choices available to consumers.
The state-level pattern of decreasing insurer participation in the years 2016 through 2018, followed by increasing participation in the years since then, was echoed at the county level.
As Chart 2 shows, while the share of counties with only one exchange insurer grew to more than half (51.3 percent) of all counties in 2018, it has since fallen to 6.6 percent of counties in 2022—or about where it was in 2015 at the peak of insurer participation. Chart 2 also shows that the return of insurers to the exchanges has brought the share of counties with an insurer monopoly or duopoly back down from 81.8 percent in 2018 to 40.4 percent in 2022.
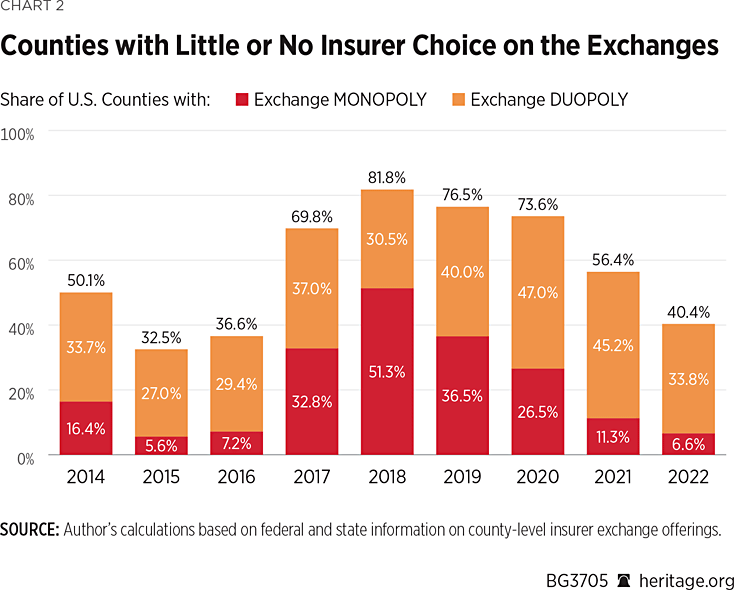
That improvement was mainly driven by changes in the share of counties with only one insurer. In 2018, there were 1,613 counties that had only one insurer. By this year, 556 of those counties had gained a second insurer, and another 870 counties had gained two or more insurers. During the same period, 20 counties went from two insurers to one. The net result is that this year only 207 counties have a single insurer offering exchange coverage.
Patterns of Insurer Exchange Participation
The increase in insurer exchange participation resulted from a combination of insurers expanding into additional states and insurers returning to states they had previously exited.
Two newer insurers—Oscar Health and Bright Health—are notable for their business strategy of offering coverage only within selected local markets.
Oscar Health first offered exchange coverage in 2014 in New York City, while Bright Health started in 2017 by offering exchange coverage in seven Colorado counties encompassing the cities of Boulder, Colorado Springs, and Denver. In subsequent years, both insurers expanded into more metropolitan areas in more states. For plan year 2022, Oscar offers coverage in 21 states while Bright offers coverage in 15 states. Yet, Oscar and Bright only offer coverage in select counties within those states—except for Nebraska, where both companies offer coverage statewide, and New Mexico, where True Health New Mexico (which Bright acquired last year) operates statewide. However, Bright just announced that it will discontinue coverage in New Mexico and five other states next year.REF
The behavior of larger, more established insurers is illustrated by how two of them—Aetna (now a subsidiary of CVS Health) and United Healthcare—have responded over time. Aetna offered exchange coverage in 17 states in 2014 and 2015, but by 2018 had exited all of them. After a four-year absence, the company resumed coverage in eight of those states for plan year 2022. Similarly, United Healthcare offered exchange coverage in 34 states in 2015, but by 2018 had exited all but three of them and offered coverage in only four states in 2019 and 2020. Since then, United has returned to more states—a total of 10 in 2021 and 18 in 2022.
Market Stabilization
The rebound in insurer competition reflects actions by Trump Administration officials to stabilize the exchange market.
Specifically, the Trump Administration closed regulatory loopholes that some medical providers and enrollees had used to “game” the system and saddle insurers with significant losses. In turn, those losses were factors that contributed to escalating premiums and insurers exiting the market. The Administration also revised other regulations to provide states and insurers with more flexibility to accommodate local circumstances.
Another move by the Trump Administration was to eliminate the payment to insurers of separate “cost-sharing reduction” subsidies. Congress never appropriated funding for those separate payments and their elimination forced insurers to include those costs in their base premiums for silver plans.REF That made the true cost of silver plans transparent, but also increased the ACA’s “premium tax credits,” which are pegged to the second-lowest-cost silver plan available to the subsidy-eligible enrollee. Thus, for subsidized enrollees—who overwhelmingly choose silver plans—the increase in premiums was offset by an increase in subsidies, while premiums for other plans were unaffected by the change.
In addition, the Trump Administration approved “Section 1332” waivers in 15 states, which gave those states regulatory relief from some of Obamacare’s mandates in order to better align existing federal subsidy dollars with enrollee need using state-based “reinsurance” programs. As a result, insurers in those states were able to maintain, or even reduce, premiums. That particularly benefited unsubsidized exchange customers.REF
New Regulations Could Reduce Choice and Competition
On May 6, the Department of Health and Human Services (HHS) published the finalized version of its “HHS Notice of Benefit and Payment Parameters for 2023” rule.REF Each year, HHS issues this omnibus rule, consisting mainly of technical changes and updates to various Obamacare requirements that insurers need to account for when designing their product offerings for the next plan year.
In its proposed version of the rule for plan year 2023, the Biden Administration also included several provisions that either reverse regulatory improvements made by the Trump Administration or impose additional requirements on insurers.REF Most of those changes remain in the final version of the rule. Consequently, the Biden Administration now risks replicating the premium escalation and insurer exits that characterized the exchanges from 2016 to 2018.
Specifically, the following four Biden Administration regulatory changes have the greatest potential to increase premiums and reduce insurer competition:
1) Reinstating a Loophole that Enables Enrollees to Skip Paying Premiums. The ACA requires insurers to issue coverage to all qualified applicants. It also provides a three-month grace period for non-payment of premiums by subsidized purchasers in the exchanges. In contrast, unsubsidized buyers (both on and off the exchanges) are subject to state laws—which in most states provide a standard one-month grace period. The interaction of those two ACA provisions creates a perverse incentive for some enrollees to avoid paying past-due premiums when re-enrolling—even in the same plan with the same insurer.
The Trump Administration addressed that problem by issuing regulations clarifying that insurers could delay the effective date of new coverage until any past-due premiums the applicant owed the insurer for the previous plan year were paid up.REF The Biden Administration’s new rule reverses that policy, on the grounds that it creates “barriers to health coverage,” and argues that insurers can instead “pursue other mechanisms to collect past-due premiums.”REF
The problem with that argument is that the “other mechanisms”—such as hiring debt collectors or obtaining court orders—are cumbersome, time consuming, less effective, and could cost more than the amount owed.
In commenting on this provision in the proposed rule, the American Academy of Actuaries expressed “strong concerns about the potential impact to health plans and rates for other plan participants that could arise from members gaming the system if CMS [Centers for Medicare and Medicaid Services] finalizes the proposal to allow past-due premiums to be forgiven for re-enrolling members.” The Academy went on to note that “this proposal may adversely affect premiums, as premiums for all members would have to increase to offset the increased bad debt assumed by issuers.” (Emphasis in original.) The Academy further stated that premium increases “could be in the range of 0.3% to more than 3%,” that the “expected rate of disenrollment would increase,” that the “required premium load would increase at an even higher rate as the amount of unpaid premiums increases are compounded by decreases in paid premiums,” and that it could also “reduce access if issuers exit the market.”REF
The same concerns and objections were echoed in comments submitted by the Accreditation Association for Ambulatory Health Care as well as those from several insurers.REF Molina Healthcare estimated that the effect “could equate to 4%–7% of annual premium on average, which will encourage even more nonpayment of premiums.” Molina went on to point out:
The policy could also increase adverse selection as typically the healthiest members would most likely stop paying premiums thus reducing the funds available to issuers to cover costs for sicker members. The financial exposure associated with this proposal could also extend to providers, who would be left without proper payment as the grace period claims payment provisions would activate due to a member’s nonpayment of premiums in the last quarter of the benefit year. CMS should encourage year-round insurance coverage and not introduce a large loophole which will degrade program integrity, incentivize fraud, waste, and abuse, and increase costs, adversely impacting coverage affordability especially, and unfairly, for those consumers who play by the rules and make their premium payments.REF
The response of the Biden HHS was to downplay and dismiss these concerns and simply adopt its proposed changes in the final rule.REF Thus, under the amended regulations, an insurer will now be deemed to be in violation of Obamacare’s guaranteed issue of coverage requirement (and consequently subject to fines and other enforcement actions) if the insurer refuses to issue coverage to an applicant due to the applicant’s “failure to pay premium owed under a prior policy, certificate, or contract of insurance, including by attributing payment of premium for a new policy, certificate, or contract of insurance to the prior policy, certificate, or contract of insurance.”REF
2) Eliminating Verification Requirements for many Special Enrollment Periods (SEPs)—Encouraging More People to Forego Buying Coverage Until They Need Medical Care. The ACA requires insurers to issue coverage to all qualified applicants during an annual open enrollment period, and during SEPs outside open season for individuals experiencing a “qualifying life event”—such as getting married, losing employer coverage, or moving to another state. Those provisions were designed to balance enabling sick individuals to get coverage with the necessity of discouraging healthy individuals from waiting until they expect to require medical care before buying coverage—behavior which could cause the market to collapse. While the basic regulatory design was the same as that applied to the employer-group-coverage market, which has long had guaranteed issue of coverage, for plans sold through the Obamacare exchanges Congress expanded the number and type of qualifying events that trigger an SEP.REF
Initially, the Obama Administration relied mainly on applicants self-attesting that they qualified for an SEP and required little or no documentation to support assertions of eligibility. As insurers reported disproportionately high claims costs for SEP enrollees, the Obama Administration began to require more verification, and the Trump Administration expanded those requirements.REF The Biden Administration is now eliminating pre-enrollment verification for most SEPs in the 30 states whose exchanges are federally run and will allow state-run exchanges to determine for themselves the extent to which they will verify SEP applications.
The American Academy of Actuaries noted that “[l]ess restrictive SEP enforcement mechanisms have the potential to worsen the risk profile.”REF The trade association America’s Health Insurance Plans (AHIP) also opposed this change, stating that:
SEP pre-enrollment verification promotes a stable risk pool and reduces the negative impact of the abuse of SEPs. We are concerned that removing SEP pre-enrollment verification, together with recent policy changes including a longer open enrollment period and continuous enrollment for individuals with incomes under 150 percent of the federal poverty level, will have the cumulative impact of destabilizing the individual market risk pool and raise premiums. Instead, HHS should prioritize policies that encourage 12 months of continuous coverage.REF
United Healthcare, Cigna, and the Blue Cross Blue Shield Association cited similar concerns in their comments opposing this change.REF
Notwithstanding those concerns, the Biden Administration adopted this proposed change in the final rule. Consequently, starting next year, the federally run exchanges will conduct verifications only for applicants who claim loss of other “minimum essential coverage” as the reason for their SEP eligibility.
3) Imposing More Detailed Federal “Network Adequacy” Regulations that Could Make It Harder for Insurers to Offer Plans in Rural Counties. Obamacare’s statutory language is vague and aspirational with respect to the provider networks of plans sold on the exchanges. The law simply instructs the Secretary of HHS to “establish criteria” for certifying plans to be offered on the exchanges and enumerates eight parameters—the second of which reads, “ensure a sufficient choice of providers.”REF
Given that state health insurance laws typically include “network adequacy” standards for managed care plans, the Obama and Trump Administrations mainly relied on those state laws when approving plans to be offered on the federally run exchanges. The Biden Administration has now amended the regulations to impose new federal “time and distance standards” (starting in 2023) on providers in 34 different medical specialties and “appointment wait time standards” (starting in 2024) on facilities offering any of 11 different specialty services.REF Furthermore, the new regulations stipulate that any insurer seeking to offer a plan that does not meet the new standards will be required to include with its application a “written justification” for “how the plan’s provider network provides an adequate level of service for enrollees and how the plan’s provider network will be strengthened and brought closer to compliance with the network adequacy standards prior to the start of the plan year.”
These new regulations could adversely affect insurer choice and competition, particularly in rural areas with fewer providers. If insurers are unable to meet the requirements, or obtain exemptions, rural counties would likely have fewer insurers offering coverage and only more expensive non-network plan options.
AHIP and several insurers, as well as the Kansas Insurance Department—which predicts that between 54 and 60 of that state’s 105 counties could be adversely affected—submitted comments objecting to these additional requirements.REF
Those commentors all asserted that existing state regulations are the best way to ensure that network adequacy standards appropriately account for local circumstances. As CVS Health put it, “There is no consumer benefit by adding a federal layer of regulation to an already functioning state regulatory environment.”REF
4) Requiring Insurers to Offer Government-Designed “Standard” Plans. Under the Biden Administration’s new regulations, starting in 2023, if an insurer participating in a federally run exchange offers a “non-standardized” plan, it will be required to also offer a “standardized plan” in the same service area, at the same metal level and with the same network type as the non-standard plan.
The final rule sets forth the specifications for those standardized plans in two tables.REF
The rationale offered by the Biden Administration is that “the significant increase of plan offerings available on the Exchanges over the last several plan years” could result in consumers experiencing “choice paralysis.”REF
However, as one insurer pointed out: “The proposed rule would have the unintended effect of producing more, not fewer, products to the market and thus would exacerbate the issue identified by CMS.”REF Other commentors echoed that observation.REF
The American Academy of Actuaries cautioned that “adding more plans to a crowded marketplace will not make purchasing easier, even if these plans are standardized. Instead, the additional offerings may add to the confusion, particularly as it is likely the standardized plan options may not meet the needs of some consumers.”REF
Even a provider group, the Federation of American Hospitals, weighed in against the idea, stating:
We do not agree with CMS’s concern that the number of plan options has risen along with rising Exchange enrollment. On the contrary, we believe that the increasing number of plan choices indicate an increasingly robust market where issuers and providers have the flexibility to innovate, and consumers are able to enjoy a wide range of options.REF
Another telling indicator was this observation by the Blue Cross Blue Shield Association: “We also would note that the proposed standardized plans represent benefit designs that are not commonly seen in the market.”REF That is an understated way of pointing out that the government-designed plans are likely to be unappealing to many consumers.
In responding to these comments, HHS admitted that “standardized plan option requirements could potentially increase the total number of plan offerings,” but encouraged insurers “to modify their existing non-standardized plan offerings…to conform with the cost-sharing parameters of the standardized plan options” as a way to “reduce the risk of choice overload.”
In sum, the Biden Administration thinks that the problem with Obamacare is that it offers too many different insurance plans, and that the solution is for insurance companies to offer plans designed by the government—and preferably only such plans. Implementing these new requirements will likely further disincentivize insurer participation in the Obamacare exchanges.
Conclusion
As the Obamacare exchange market has stabilized over the past four years, more insurers have resumed, or expanded, their offering of exchange coverage. While insurer competition is still far below pre-ACA levels at both the state and county levels, insurer choice and competition in the Obamacare exchanges for 2022 is roughly back to where it stood in 2015—before large and escalating losses prompted numerous insurers to exit the exchanges.
The Biden Administration’s new regulations now threaten to reverse much of that progress. They could significantly reduce insurer choice and competition in the exchanges and increase premiums for individuals and taxpayers who subsidize these costs.
Edmund F. Haislmaier is the Preston A. Wells, Jr., Senior Research Fellow in the Center for Health and Welfare Policy at The Heritage Foundation.