The Biden Administration’s health care policies are failing Americans. Sixteen months into the Administration, the three major government health programs—Obamacare, Medicaid, and Medicare—are all worse off today than they were before. The Administration’s policy solutions do little to address the root causes and in many ways make matters worse.
The only effective way to resolve persistent problems in health care is to leverage the power of personal choice and market competition. Congress should take the steps needed to transform the health care system away from a government micromanaged public utility model, as advocated by the left, and instead embrace a patient-centered health care agenda that puts individuals and families, not the government, in control of health care decisions and subjects the health care sector to the discipline of market competition.
Biden Administration’s Failing Record on Health Care
Health care costs and spending are escalating, dependence on government programs is at an all-time high, and individuals and families have less control of their health care decisions. The Biden Administration has offered little to address the underlying causes of what ails the health care system—especially rapidly rising health costs. In fact, the policies being advanced by the Administration will likely worsen the situation, not improve it.
Obamacare. Enacted in 2010, the Affordable Care Act (also known as Obamacare) created two new entitlements: a taxpayer-subsidy scheme for insurance coverage purchased through government-run exchanges and a major Medicaid expansion, opening eligibility to a new class of able-bodied, childless adults. It also put in place a massive federal regulatory framework that preempted state authority to regulate health insurance and used a set of tax hikes and provider cuts to ostensibly offset new spending.
The Obama Administration promised to “lower costs for families and for businesses and for the federal government, reducing our deficit by over $1 trillion in the next two decades.”REF Yet after 12 years, Americans face even higher costs, fewer choices, and more government interference in their health care decisions.
The Biden Record: Since Obamacare’s enactment, average monthly premiums have more than doubled—a 129 percent increase from 2013–2019. (See Chart 1.) Deductibles are also higher, having risen from $5,100 (self-only policy) and $10,300 (family policy) in 2013 to $6,894 (self-only) and $13,949 (family) in 2021.REF Furthermore, the number of insurers offering coverage in the Obamacare exchanges is 25 percent less than the number that offered coverage in the individual market before Obamacare.REF
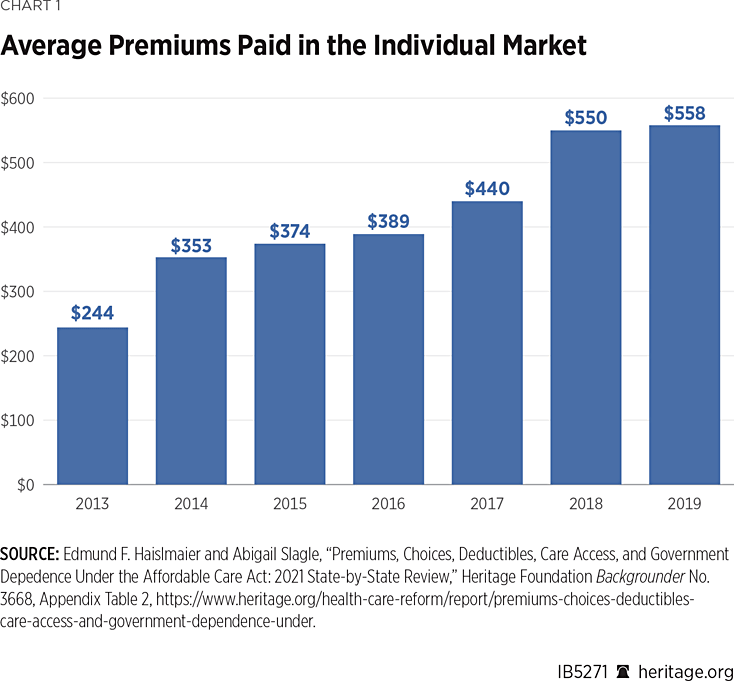
Instead of addressing the root causes of these problems, the Biden Administration has focused on rolling back positive changes that the Trump Administration initiated to stabilize the health care market, bring down costs, and increase coverage options.REF For example, the current Administration has issued regulatory changes to enable enrollees to skip premium payments, allow for year-round enrollment, eliminate verification requirements for special enrollment periods, and further prescribe plan options and thereby limit choice in plan design—all of which can be expected to result in higher premiums and fewer options.REF
Medicaid. Established in 1965, the Medicaid program created a government welfare program to provide health care services to certain low-income groups. Under this joint federal–state program, the federal government sets broad rules, the state administers the program within those basic parameters, and the federal and state governments share the costs.
Originally designed to assist low-income pregnant women, children, persons with disabilities, and the elderly, Obamacare permitted states to expand Medicaid eligibility to a new category—able-bodied, childless adults—and gave those states additional federal assistance for doing so.
The Biden Record: Despite a history of access and quality issues,REF since President Biden took office, enrollment and spending in Medicaid have ballooned, adding more pressure on a program struggling to deliver high-quality care to its traditional enrollees: pregnant women, poor families and children, the elderly, and persons with disabilities. Of the nearly 79 million people enrolled in Medicaid, enrollment among adults has surged. From February 2020 to November 2021, enrollment among adults increased 29 percent, from 34 million to 44 million,REF and spending increased 11.4 percent in 2021.REF Although COVID disruptions doubtless influenced enrollment, the Biden Administration is touting the substantial rise in this welfare program as a success.REF
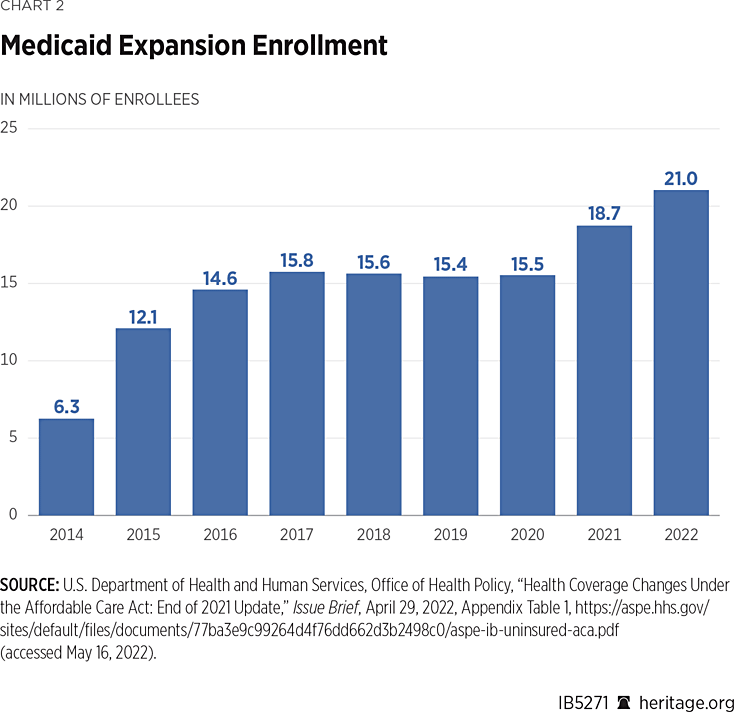
Instead of tackling the demographic, structural, and fiscal challenges facing the Medicaid program, the Biden Administration’s policies further exacerbate these problems. To start, the Administration laid out a protracted process for states to remove ineligible individuals from the Medicaid program post-COVID—a tactic that appears to be aimed at prolonging enrollment in Medicaid regardless of eligibility. In addition, the Biden Administration took the unprecedented step of stripping states’ ability to promote independence among able-bodied adults by requiring work or training as a condition of receiving benefits, thus discouraging state innovation and flexibility. These actions expand federal control and create a chilling effect on state innovations that reduce dependence on government and improve health care options for low-income families.
Medicare. Medicare is the federal health program that provides health care services to seniors over the age of 65 and certain disabled individuals. Seniors in the Medicare program can choose between stand-alone physician and hospitalization services in the traditional fee-for-service benefit package or a more comprehensive benefit package offered by private insurers through a defined-contribution payment model. In addition, seniors under Medicare have access to prescription drug benefits either through a stand-alone benefit plan or through prescription drug coverage fully integrated into competing private plans.
Each year, the Medicare Trustees are required to issue a report on the program’s operations and financial solvency. For the past three years, the Medicare Trustees have warned that the program’s financial outlook is unstable. Specifically, the program’s funding for hospital care is expected to be depleted by 2026, and the program’s long-term solvency would require a 27 percent increase in the payroll tax or a 16 percent cut in spending.REF
The Biden Record: By law, the Medicare Trustees must report a “funding warning” whenever there is an excessive reliance on general tax revenues drawn down from the Treasury. Though it is required to take action and present to Congress a plan to address these financial problems, the Biden Administration, like others before it, has ignored these warnings and requirements.REF
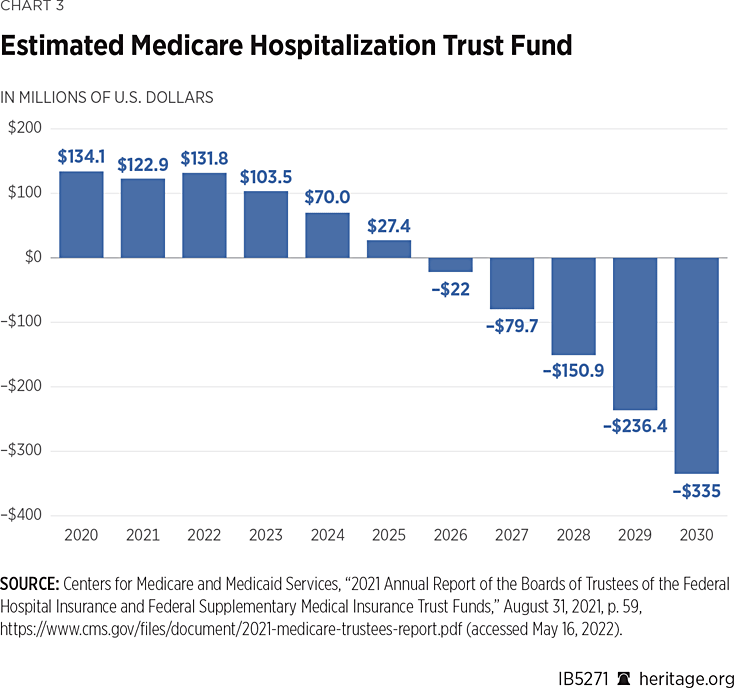
Instead of addressing Medicare’s short-term solvency and long-term financial challenges, the Biden Administration has offered no plans to shore up the program. The President’s FY 2023 budget, for example, is devoid of any meaningful changes to address these imminent dangers.
Worse Plans Looming
With support from its allies in Congress, the Biden Administration’s short-term plans are only a placeholder to clear the way for more dramatic changes—plans that would turn America’s health care system into a single, government-run monopoly.
The so-called Build Back Better plan sought to increase and expand federal subsidies for Obamacare, push more states to expand Medicaid, and reintroduce the “public option,” a government-run plan that would rig the insurance markets to crowd out private coverage.REF Since efforts to advance Build Back Better have stalled, the Administration is now attempting to use the regulatory process to advance its agenda on a piecemeal basis.REF
Further, Congress is now changing its focus to injecting government price controls into the health care sector, starting with the pharmaceutical industry—a policy that not only will limit access and stifle innovation, but also is a bridge for extending government price controls across all health care sectors.
Altogether, these Build Back Better provisions lay the groundwork for a full single-payer plan. Such a plan would eliminate Medicare and Medicaid, end private coverage, including employer-based coverage, and replace it with a single, government-run plan—a solution that would result in less access, fewer choices, and higher taxes.REF
A Better Way: Empower Patients and Fuel Competition
Stopping the Biden Administration and Congress from expanding the Administration’s government-centered legislative and regulatory health agenda is critically important, but advancing a positive and constructive set of alternatives is equally important. Policymakers must take action to transform the health care system so that patients can be secure in knowing that their health care is controlled by them and not government officials.
Congress plays a critical role in clearing the path to a more patient-centered, market-based health system. It can start the process by taking the following actions:
- Expand access to alternative coverage options. Instead of more federal subsidies to cover up the failures of Obamacare, individuals and families need more affordable coverage options. The Trump Administration took several steps to make non-government arrangements more available. Congress should codify these new types of arrangements, including Association Health Plans, Short Term Limited Duration Plans, and Individual Reimbursement Accounts. Congress should also update and adopt changes in Health Savings Accounts to make these patient-centered arrangements more accessible and flexible.
- Strengthen state flexibility to bring down premiums. States play a critical role in health reform. But while states have taken important actions,REF more should be done to remove federal impediments to state innovation. The Trump Administration expanded the scope of state flexibilities and included additional, innovative models for the states to bring down premiums and expand coverage options.REF Congress should make those options permanent to help states bring down premiums, expand choice, and thereby make coverage more affordable, and reduce the need for taxpayer subsidies.
- Give low-income Americans a choice in their health care. Low-income individuals and families should not be locked into a lifetime of dependence on poor-performing, government-run health care programs. Americans, regardless of income status, should benefit from the innovations of the private sector. To that end, similar to the school choice model, Congress should allow low-income individuals and families that are eligible for Medicaid to apply that financial assistance to the private plan of their choice.REF
- Modernize Medicare for a new generation of seniors. Medicare Advantage, the private insurance option for seniors, is growing in popularity. Congress should build on the success of Medicare Advantage by improving the payment model and allowing more innovative and flexible benefits—for example, by permitting insurers to offer plans that use a Direct Primary Care payment designREF and by allowing Medical Savings Account plans to offer the same integrated prescription drug benefits that other Medicare Advantage plans offer.
- Provide consumers with price transparency and stronger consumer protections. Advancing more patient-centered health care models will require additional tools and resources to support patients. For example, individuals need better information on prices, quality, and choices. Furthermore, patients should be able to reap the benefits of cost-saving decisions and be protected from contract decisions outside of their control. Congress and the states should facilitate meaningful price transparency initiatives, permit patients to share in premium savings with insurance plans, and revisit flawed surprise-billing legislation.
Conclusion
The Biden Administration’s policies have done little to address the underlying challenges facing the health care system. Whether Obamacare, Medicaid, or Medicare, the Biden Administration’s policies paper over the policy failures.
The health care system needs meaningful change. Congress should begin to lay the groundwork for a more patient-centered, market-based health care system that gives individuals and families greater control of their health care dollars and decisions while also reducing costs and improving quality through increased competition and transparency in the health care sector.
Nina Owcharenko Schaefer is Director of the Center for Health and Welfare Policy at The Heritage Foundation.



