Americans across the political spectrum are concerned about the high cost of health care, and some policymakers are turning to other countries for insights into how to reduce costs and expand coverage in the United States. One of those countries is Canada.
Some U.S. politicians, such as Senator Bernie Sanders (I–VT), laud Canada as a posterchild for universal health care.REF Critics decry Canada’s long wait times for medical services, and other drawbacks, as an expected outcome of “socialized medicine.”REF In fact, participants on both sides of the debate often misunderstand Canada’s health care system or fail to offer a complete description.
Comprehensive international comparisons of universal health care systems indicate that Canada is a relatively high spender that achieves only mediocre, and sometimes poor, performance, particularly with regard to the availability of medical resources and the timeliness of care. Canada’s health care system is also particularly restrictive in a number of ways with which Americans may be unfamiliar. It is important for U.S. policymakers and the public to understand the underlying policies, and practical reality, of the Canadian system as they seek to reform the U.S. system.
An Overview of the Canadian Health Care System
According to the Canadian constitution, the provision of health care is the responsibility of each province. However, the federal government exercises significant control over the policies that characterize provincial health care systems through its funding. The guiding principles of this financial relationship—and the basis of Canada’s universal health care framework—are enshrined in the Canada Health Act (CHA), enacted in 1984.
One of the key features of Canada’s system is the significant restriction on private-sector financing and delivery of core medical services. The CHA significantly restricts private activity on both fronts. Specifically, the CHA states that the insurance plan of a province must be administered on a not-for-profit basis by a public authority and must cover medically necessary services provided by hospitals and medical practitioners for every resident on uniform terms and conditions. Provincial plans must not directly or indirectly (through charges or otherwise) impede reasonable access to health services and must not impose any minimum residency requirement in excess of three months before providing coverage. In addition, the CHA also prohibits private insurance for medically necessary services that share the cost with the public system. As a result, Canada is a rare example of a country that effectively prohibits private insurers from providing coverage for services outside the government program. Meaning that, while private coverage exists, it is only available for those medical goods and services that do not require coverage by the CHA.
Another key feature of the Canadian system is that there are no cost-sharing requirements for patients under provincial plans—no deductibles, co-pays, or extra-billing.REF By contrast, co-payments and other cost-sharing requirements are the norm in most other developed countries (with the exception of Britain, which has the public National Health Service) as a way to make patients better understand the scarcity of health care resources so that they will use the health care system responsibly.REF
Perhaps as a direct consequence of Canada’s single-payer (government-funded) system, hospitals are funded using prospective “global budgets.” Under this method of remuneration, hospitals receive a set amount of funding to treat patients, thus incentivizing hospital managers to limit patient admissions and treatments.REF While perhaps useful for containing costs, global budgets may also disincentivize hospital administrators from treating patients who have conditions that are costly to treat.REF More generally, global budgeting typically leads to rationed care, as only a limited amount of activity can be paid for before hospitals exhaust their budgets.
The legal status of health care providers who work entirely outside the public system is ambiguous, and only 1 percent of hospitals were classified as for-profit institutions in 2016.REF Furthermore, and unlike most other countries, provinces in Canada heavily discourage (or outright prohibit) physicians from practicing in both the public and the (almost non-existent) private sector. As a practical matter, provincial governments also discourage private clinics from operating entirely independently of the public system, even if the suppliers do not bill the government for services provided. Canadians also have no legal right to buy private health care services that are covered by the government program, unless they go outside Canada for those services.REF
The resulting system is one in which Canadians are effectively prohibited from pursuing private treatment for medically necessary services in their own country. Although patients can, in principle, pay the full costs of their treatment out of pocket, government restrictions on physicians’ ability to receive out-of-pocket payments, as well as regulations surrounding shared costs or capital equipment with the public system, and the vague wording of the CHA (particularly section 12) have created an environment wherein provincial governments, fearing the loss of federal government funding, have implemented legislation to effectively prohibit private payment options.
While some individual legal cases have challenged prohibitions on private payment (notably the Chaoulli case in Quebec in 2005), Canadian patients effectively do not have the option of buying basic medical services privately. They have only the option of seeking treatment in a different country. A recent study estimated that approximately 217,500 Canadians traveled abroad to receive health care in 2017.REF There is no other developed country, to the authors’ knowledge, that places similar restrictions on patient choice.
With its restrictions as described above, the CHA severely constrains the ability of provinces to try different approaches to health care coverage and delivery, as well as the provinces’ freedom to adopt new technologies and improve efficiency.
The Canada Health Act. It is important to understand the relationship between Canada’s federal and provincial governments. A constitutional monarchy, Canada is a federation with 10 provinces and three territories. The division of powers between the federal government and provincial governments is described in the Constitution Act of 1867.
Specifically, section 92(7) states that “[i]n each Province the Legislature may exclusively make Laws in relation to…[t]he Establishment, Maintenance, and Management of Hospitals, Asylums, Charities, and Eleemosynary Institutions in and for the Province, other than Marine Hospitals.”REF In other words, the provision of medical services is a provincial responsibility. As a result, Canada is often described as a pastiche of 10 health care systems—one for each province.
However, while matters related to the provision of health care services is clearly a provincial responsibility, this is not necessarily the case for the financing of (or payment for) those services. In fact, the federal government exercises a significant amount of control over provincial health care systems through its funding. While the nature and magnitude of federal government influence has evolved over time,REF the guiding principles for the current federal–provincial government relationship are determined by the CHA.REF
The CHA states that the primary objective of Canadian health care policy is “to protect, promote and restore the physical and mental well-being of residents of Canada and to facilitate reasonable access to health services without financial or other barriers.”REF
However, the CHA does not directly set health care policy. Rather, it is a financial act that establishes the “criteria and conditions in respect of insured health services and extended health care services provided under provincial law that must be met before a full cash contribution may be made” by the federal government.REF Specifically, the CHA outlines the conditions that provinces must meet in order to receive a full cash contribution from the federal government through the Canada Health Transfer program, which amounted to C$38.6 billion (U.S. $29.2 billion) from April 2018 to 2019 (the Canadian fiscal year).REF
The aspects of the CHA most relevant for setting out the framework within which provincial health care systems must function are outlined in sections 8 to 12. Commonly referred to as the five principles of the CHA, the salient points of these sections are:
- Section 8 (Public Administration): “[T]the health care insurance plan of a province must be administered and operated on a non-profit basis by a public authority appointed or designated by the government of the province.”
- Section 9 (Comprehensiveness): “[T]he health care insurance plan of a province must insure all insured health services provided by hospitals, medical practitioners or dentists, and where the law of the province so permits, similar or additional services rendered by other health care practitioners.”
- Section 10 (Universality): “[T]he health care insurance plan of a province must entitle one hundred per cent of the insured persons of the province to the insured health services provided for by the plan on uniform terms and conditions.”
- Section 11 (Portability): The health care insurance plan of a province may not “impose any minimum period of residence in the province, or waiting period, in excess of three months before residents of the province are eligible for or entitled to insured health services”; must pay “the cost of insured health services provided to insured persons while temporarily absent from the province”; and “provide for the payment, during any minimum period of residence, or any waiting period, imposed by the health care insurance plan of another province.”
- Section 12 (Accessibility): The health care insurance plan of a province “must provide for insured health services on uniform terms and conditions and on a basis that does not impede or preclude, either directly or indirectly whether by charges made to insured persons or otherwise, reasonable access to those services by insured persons,” and must provide reasonable compensation to health care providers.
The compliance of these five principles, or lack thereof, is completely at the discretion of the sitting federal government, which can withhold partial (or complete) cash transfers for perceived violations by provincial governments. Further, sections 18 to 21 state that the federal government is required to make non-discretionary deductions to the cash transfers equal in amount to any extra-billing and user charges.
When it was enacted in 1984, the CHA represented the natural evolution and amalgamation of decades of provincial and federal initiatives toward universal health care—not a top-down dictate imposed by the federal government. In fact, every province already had some form of a universal health care system prior to the enactment of the CHA, in addition to existing funding relationships with the federal government.REF
That said, two Fraser Institute analysts argue that the CHA presents a significant obstacle to provincial experimentation with successful health care policies practiced elsewhere.REF For example, the CHA does not provide a clear definition of medically necessary services that are required to be insured by the provinces’ plans. Nor does it define the term “reasonable access” or provide clear guidelines for the magnitude of penalties the federal government can impose on provinces for deemed violations of the five principles.
The two analysts conclude that “the CHA’s vagueness leaves determinations of permissibility for a range of policies up to the federal government of the day, creating not only a lack of clarity for provincial policy makers, but also questions about what policies might be disallowed in future by governments with different views of a particular policy.”REF As a result, Canada’s health care system has been characterized by policy inertia—with provinces afraid to experiment with private provision (either contracted or parallel to the public system),REF dual-practice for physicians, or more narrowly defining the services that are considered medically necessary. In many cases, provinces impose restrictions on private delivery well beyond what is required by the CHA.REF
The Cost of Canadian Health Care
Notwithstanding the popular perception that it provides “free” health care, Canada spent approximately C$253 billion (U.S. $196 billion)REF on health care in 2018.REF Of this amount, approximately C$175 billion (U.S. $135 billion) is spent by various levels of government through the country’s public health care system, the majority of which—C$163 billion (U.S. $126 billion)—was spent by provincial and territorial governments. The public sector accounts for 68.9 percent of total health care spending.REF (See Chart 1). Approximately 37 percent of public-sector spending is directed toward hospitals, 22 percent toward physicians, and 8 percent toward pharmaceuticals.REF.
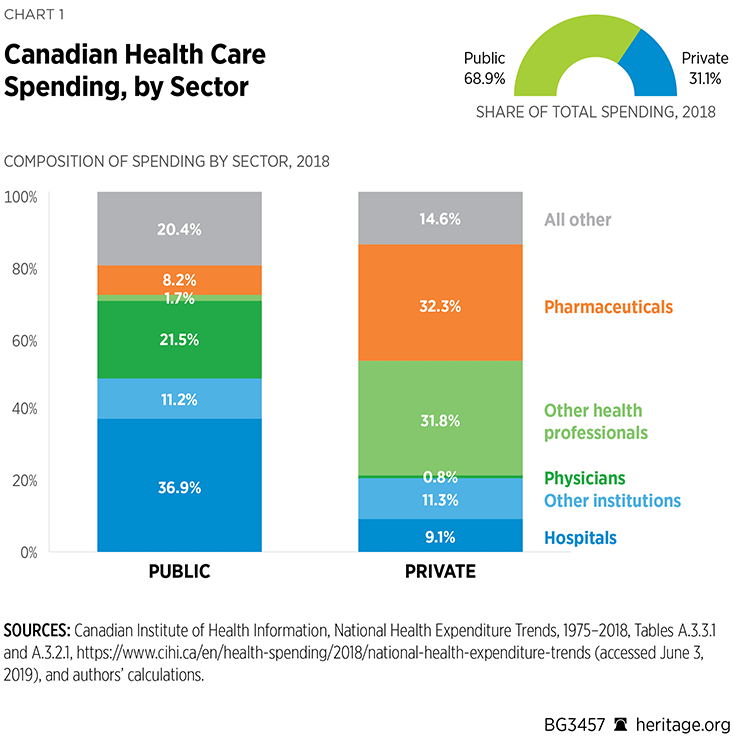
Health care is the single largest budget item for every provincial government in Canada. In 2018, health care accounted for between 37.5 percent (Quebec) to 45.1 percent (Nova Scotia) of provincial program spending.REF As a result, any change in health care spending has huge implications for other provincial government program spending, as well as for taxes and the overall fiscal sustainability of the provincial economy.
Although often referred to as a government or single-payer system, private-sector health care spending for services that are not covered by the government accounts for roughly 31 percent of the C$253 billion total. As can be seen in Chart 1, pharmaceuticals account for the largest share of private spending (32.3 percent), followed closely by spending on “other professionals” (31.8 percent).REF By contrast, hospitals account for 9 percent and physicians only 1 percent of private-sector spending.REF
The primary reason for the different distribution of spending between the public and private sectors is the CHA. As noted, the CHA requires the insurance plan of a province to be publicly administered and to cover medically necessary services provided in hospitals and by physicians on uniform terms and conditions. It also severely restricts the ability of the private sector to provide these services if it shares any costs with the public sector. Furthermore, the vague wording of the CHA has led several provinces either to outright prohibit or to severely discourage physicians from practicing in both the public and private sectors.REF
However, the CHA only requires the insurance plan of a province to cover pharmaceuticals (without extra-billing or user fees) when administered in a hospital. As a result, approximately 70.5 percent of Canadians have private drug insurance coverage,REF and “approximately 21 percent of Canadians obtain public drug coverage through provincial and territorial plans.”REF
It is therefore no surprise that public-sector funding accounts for 90 percent of hospital spending (Chart 2) and 98.4 percent of physician payments. Conversely, private spending accounts for about 57 percent of expenditures on prescription pharmaceuticals and 100 percent of non-prescription drugs.
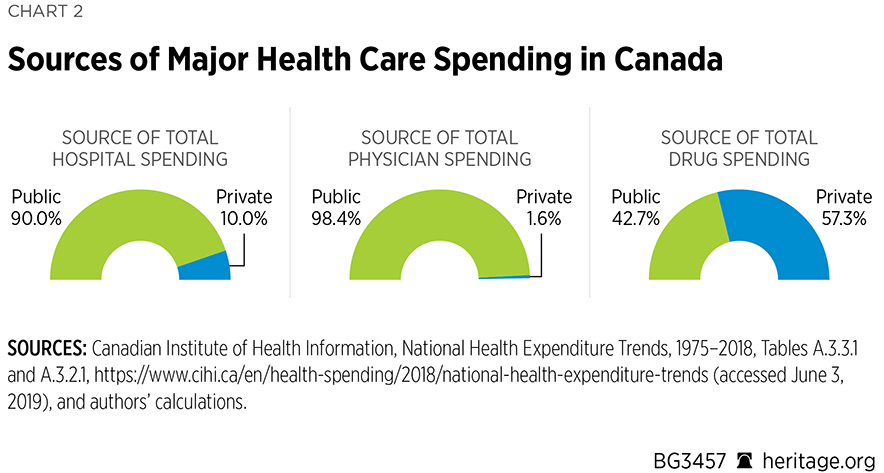
While Canadians are acutely aware of the private costs they bear for pharmaceutical insurance (a current topic of national debate) and medical services that do not require coverage by the CHA (such as vision and dental services provided outside the hospital setting), there is a general lack of public understanding about their full financial contributions to the public health care system. The public system is financed by general government revenues collected through a variety of taxes—including on income, sales, employment insurance, and “sin.” As a result, it is difficult for Canadian families to estimate how much they pay for public health care.
Annual estimates by the Fraser Institute provide some insight into the average family’s tax contribution to the public health care system. For example, in 2018, the Fraser Institute analysts estimated that the average family of four (two parents, two children), with a household income of C$138,008 (U.S. $106,512) paid approximately C$12,935 (U.S. $9,983) for public health care through the country’s tax system. The same study also estimated that the 10 percent of families with the lowest incomes paid approximately C$496 (U.S. $383) for public health care in the same year, while the top 10 percent paid C$38,903 (U.S. $30,025).REF Whether one considers these figures astronomically high or a great bargain, one thing is clear: Canadian health care is not free.
The Performance of Canada’s Health Care System: An International Perspective
A recent study by the Fraser Institute compared the performance of 28 countries,REF categorized by the Organization for Economic Co-operation and Development (OECD) as having “universal” or near-universal health coverage.REF Using a “value for money” approach, the Fraser Institute analysts examined 47 indicators in the areas of spending, availability of resources, utilization of services, timely access to care, clinical quality, and health status. The analysts concluded that despite ranking amongst the most expensive “universal” health care systems, Canada’s performance was only mediocre, and in some cases notably poor. In particular, Canada had substantially fewer medical resources than the average OECD country, with a mixed record in terms of use of resources and clinical performance. It also consistently ranked at the bottom of the pack in terms of patient wait times.REF The results of the Fraser Institute study are summarized as follows:
Health Care Spending. In 2016, Canada ranked sixth-highest for health care expenditure as a percentage of gross domestic product (GDP), and 11th-highest for health care expenditure per capita, out of the 28 countries included for comparison.REF After adjustment for age, Canada ranked fourth-highest for health care expenditure as a percentage of GDP and 10th-highest for health care expenditure per capita.REF
Of course, high spending by itself is not necessarily a bad thing, if it is accompanied by commensurate high performance that is, in turn, demanded by the citizenry. Hence, while comparisons often highlight the higher level of spending, a singular focus on relative spending is, at best, inadequate and, at worst, misleading.
Availability of Resources. Good performance is unlikely without having adequate resources to provide care. Out of 28 countries, on a per-thousand-population basis, Canada ranks 26th for physicians, 16th for nurses, 26th for curative (acute) care beds (of 26),REF and 25th for psychiatric care beds per thousand population.REF As shown in Table 1, after adjustment for age, Canada ranks 26th for physicians. Canada ranks 14th for nurses, 25th for curative (acute) care beds (of 26), and 25th for psychiatric care beds per one thousand people.REF
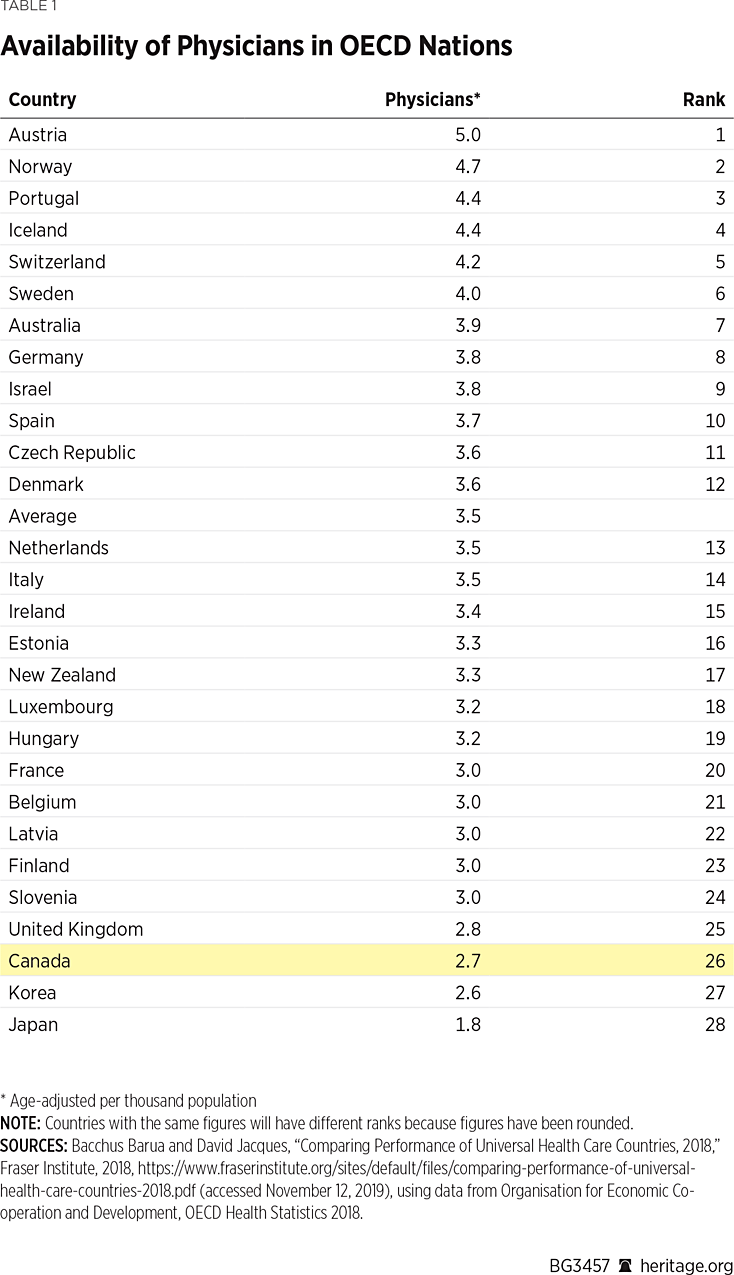
Similarly, Canada has fewer diagnostic technologies than the average OECD country. Per million population, Canada ranks 22nd (of 27) for magnetic resonance imaging (MRI) units, 22nd (of 27) for computed tomography (CT) scanners, 17th (of 24) for positron emission tomography (PET) scanners, and 11th (of 22) for mammography machines.REF After adjustment for age, Canada ranks 22nd (of 27) for MRI units (Table 2), 21st (of 27) for CT scanners, 19th (of 24) for PET scanners, and 12th (of 22) for mammography machines.REF
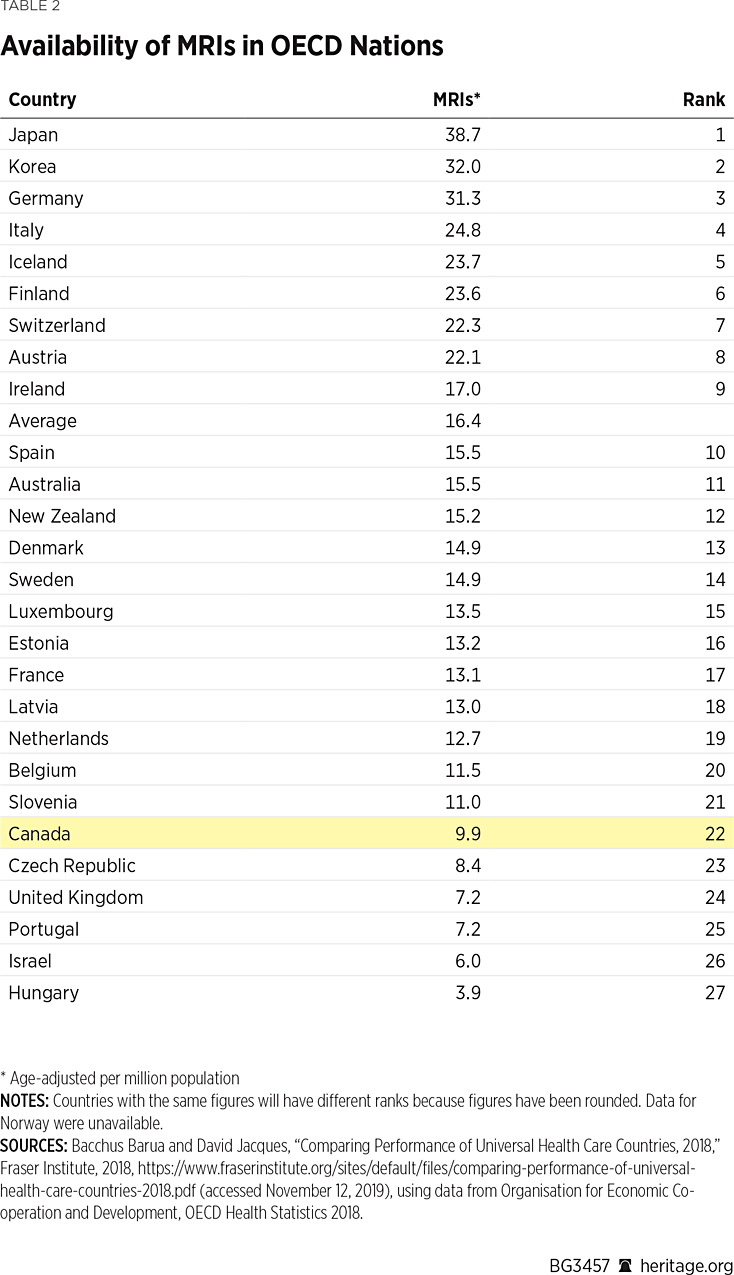
Use of Resources. Medical resources are of little value if they are not used. Furthermore, the number of services provided can help explain the relative costs of different health care systems. The study examined four key indicators: the number of (1) consultations with physicians, (2) hospital activity, (3) MRI scans, and (4) CT scans.
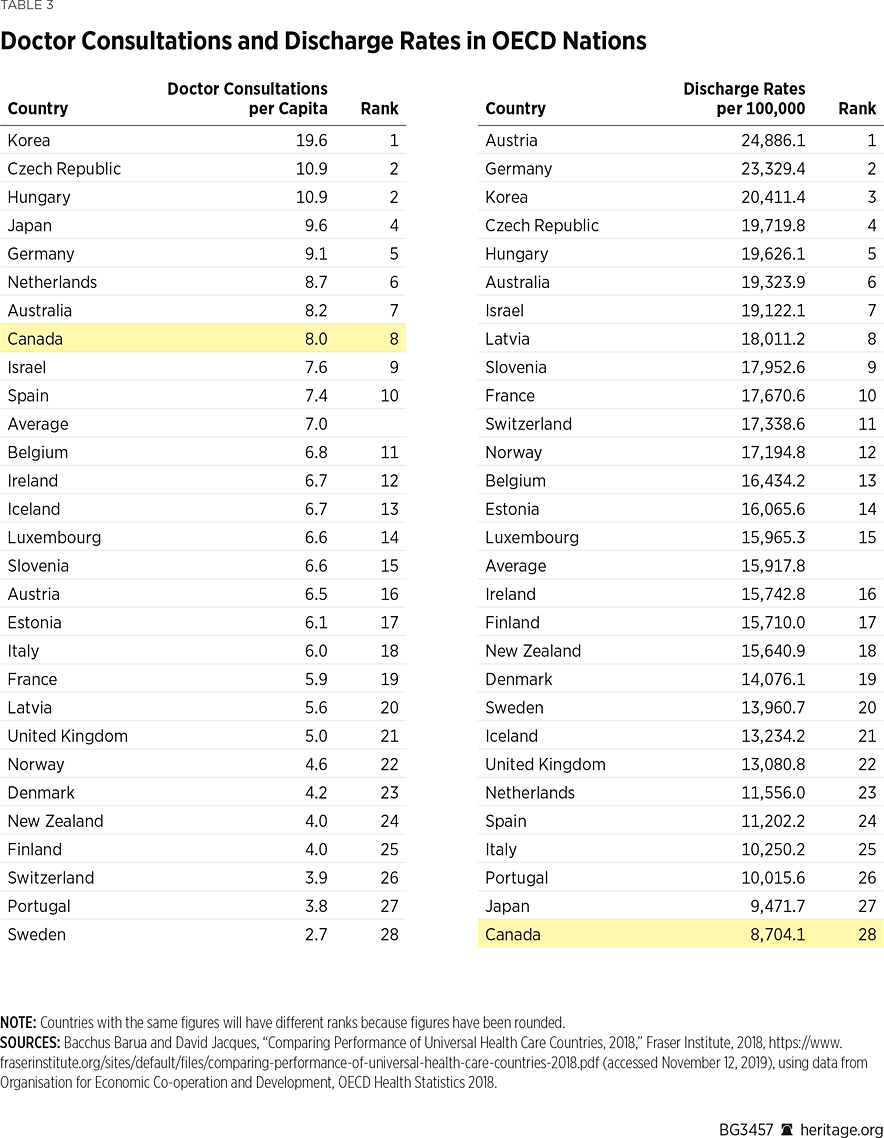
Canada ranks seventh (of 28) for doctor consultations per capita, last (of 28) for hospital discharge rates per 100,000 population, 13th (of 25) for MRI exams per thousand population, and 12th (of 25) for CT scans per thousand population.REF After adjustment for age, Canada ranks eighth (of 28) for doctor consultations per capita and last (of 28) for hospital discharge rates per 100,000 population. (See Table 3). For MRI examinations, Canada ranks 11th (of 25) per thousand population and 12th (of 25) for CT scans per thousand population.REF
Timeliness of Care. The availability of resources is an important factor conditioning the performance of a national health care system. Since resources can be used more or less efficiently, it is also important to compare measures of service delivery and treatment outcomes when creating “league tables” of health care systems.
In this regard, timeliness of health care delivery is an important characteristic of the performance of health care systems. Canada is tied for last place (of 10) for the percentage of patients able to make a same-day appointment when sick (43 percent), and ranks fourth (of 10) for the percentage of patients who report that it is very easy, or somewhat easy, to find care after hours (63 percent).
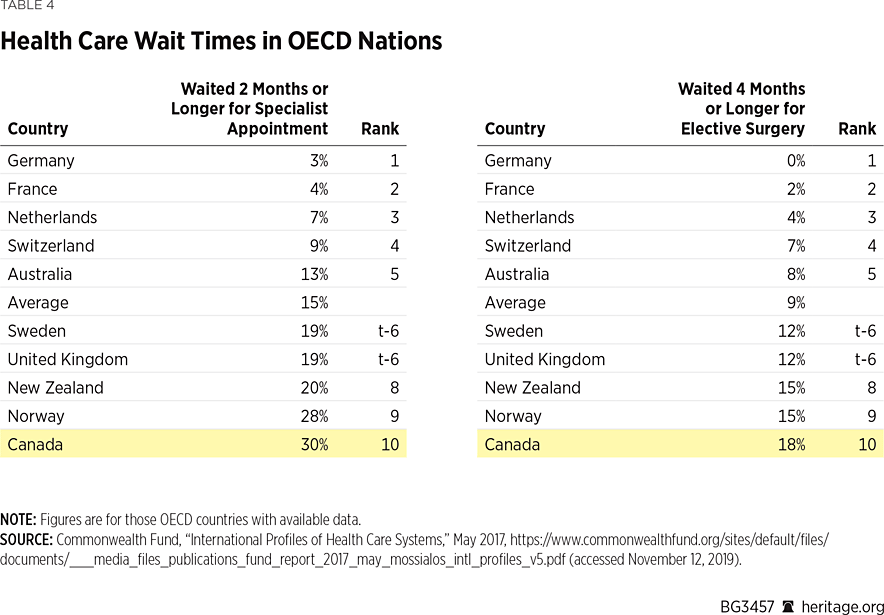
Canada placed last among the 18 countries for which data was available on the percentage of patients (56.3 percent) who reported waiting more than four weeks for an appointment with a specialist. As shown in Table 4, Canada also ranked worst (10th of 10) for the percentage of patients who reported waiting two months or more for a specialist appointment (30 percent), and worst (10th out of 10) for the percentage of patients who reported waiting four months or more for elective surgery (18 percent).REF
Long wait times for medically necessary care are, perhaps, a defining feature of Canada’s health care system. But wait times have been getting worse. In 1993, the Fraser Institute estimated that the median wait time for elective surgery across 12 specialties was 9.3 weeks. In 2018, the most recent estimate, that wait time had jumped to 19.8 weeks.REF
It is important to remember that wait times are not benign inconveniences. They can, and do, have real health consequences for patients—who may be in pain, whose conditions may worsen over time, and in the worst cases, may die—while they wait for treatment.REF
There is also an economic cost—the value of time lost while waiting for treatment, either directly through lost wages, or indirectly through lower productivity. Conservative estimates based on only the wait between specialist to treatment (not including the prior wait to see a specialist) put the cost (based on estimated lost wages) during the work week at C$2.1 billion (U.S.$1.6 billion)—C$1,924 (U.S. $1,485) per patient. The costs climb to C$6.3 billion (U.S. $4.9 billion)—C$5,860 (U.S. $4,523) per patient—when valuing (at the same hourly rate) evenings and weekends for the 1,082,541 patients who waited for treatment in 2018.REF
Outcomes and Quality. An often-cited indicator of outcomes is life expectancy. Perhaps the most commonly used measure of health status is life expectancy at birth, that is, the average number of years a person can be expected to live assuming age-specific mortality levels remain constant. Canada ranks 13th (of 28) for its performance on the indicator measuring life expectancy at birth (calculated by the OECD).REF
Because this (and other such indicators) can be problematic for a number of reasons, it is often more informative to examine indicators of clinical performance and quality. Canada ranks 17th (of 24) for performance on the indicator measuring the rate of diabetes-related lower extremity amputation, which is statistically worse than the average range for the OECD countries included for comparison, but ranks well—fourth of 22—for the rate of hip-fracture surgery initiated within 48 hours after admission to the hospital.REF
Canada ranks sixth (of 28) for performance on the indicator measuring 30-day mortality after admission to the hospital for acute myocardial infarction, statistically better than average, 18th (of 28) for performance on the indicator measuring 30-day mortality after admission to the hospital for a hemorrhagic stroke (not statistically different from the average), and 18th (of 28) for performance on the indicator measuring 30-day mortality after admission to the hospital for an ischemic stroke (not statistically different from the average).REF
Canada ranks sixth (of 26) on the indicator measuring the rate of five-year survival after treatment for breast cancer (statistically better than average), 12th (of 26) for five-year survival after treatment for cervical cancer (not statistically different from the average), sixth (of 26) for five-year survival after treatment for colon cancer (statistically better than average), and sixth (of 26) for the rate of five-year survival after treatment for rectal cancer (statistically better than average).REF
While the indicators presented in this section are only a sample of indicators examined by Fraser Institute analysts, they confirm the analysts’ overall conclusion—that, compared to other health care systems, Canada is a high spender, with a mixed record on usage and clinical performance, and a poor record in terms of the availability of medical resources and timely access to care.
Conclusion
Much of the debate in the U.S. surrounding the advantages and disadvantages of the Canadian health care system often oversimplifies the Canadian system. The Canadian system’s approach to universal health care is unique in many key respects, and particularly restrictive in a number of ways with which Americans may be unfamiliar.
Canada significantly limits private-sector financing and delivery of core medical services. Canadians can only purchase private insurance for services that are not considered medically necessary and do not share costs with the public system. Patient cost sharing (such as co-pays and deductibles) and extra-billing are prohibited in Canada’s public system, leaving patients insulated from the cost of care or understanding of the scarcity of resources, and care is often rationed as a result of the global budgeting for hospitals.
Finally, Canada is perhaps the only developed country that effectively prohibits patients from pursuing private treatment in their own country. While some individual legal cases have challenged restrictions on private payment, patients effectively have no options for buying basic medical services through the private sector within Canada’s borders.
Canada is also a relatively high spender, achieving only mediocre, and sometimes poor, performance compared to many other developed countries.
One notable outcome measure on which Canada is distinctly inferior is timeliness of treatment. Canadians suffer long wait times for accessing services of physicians. The long wait times arguably reflect particular features of Canada’s health care system, including first-dollar coverage for medically necessary services, the lack of a private alternative (for the financing and delivery of care), and the use of prospective global budgets for hospitals. Moreover, wait times impose costs on Canadians that are not reflected in traditional measures of health care costs.
These caveats reinforce the point that policymakers in the U.S. should exercise caution in proposing and implementing any major reforms to the country’s health care system that are based on the type of policies that characterize Canada’s health care system.
Bacchus Barua is Associate Director of Health Policy Studies, and Steven Globerman is a Senior Fellow, at the Fraser Institute in Canada.


