Over half of the Democrats in the House and 14 Democrats in the Senate are calling for enactment of a new government-run health coverage program to replace all existing private health insurance, including employer-sponsored health benefits, as well as the current publicly funded coverage for Americans enrolled in Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP). The proposed new program would be operated and funded solely by the federal government, and private insurers and employers would be prohibited from offering coverage that duplicated any of the program’s benefits.REF While the terminology (such as single-payer and Medicare for All) and the details may vary, any such proposal would significantly increase federal government spending and require major tax increases.
Advocates of this idea suggest that Americans currently covered by private health plans would be financially better off, even after their taxes are raised to fund the proposed new government program. For example, Senator Bernie Sanders (I–VT) has said: “Are people going to pay more in taxes? Yes. But at the end of the day, the overwhelming majority of people are going to end up paying less for health care because they aren’t paying premiums, co-payments or deductibles.”REF
That assertion is incorrect. Our analysis finds that in order to fund such a program, it would be necessary for the federal government to impose substantial, broad-based taxes equal to 21.2 percent of all wage and salary income. Those taxes would be in addition to the payroll taxes that most workers already pay for the existing Social Security and Medicare programs, bringing total payroll taxes to 36.5 percent for most workers.REF We also find that nearly two-thirds of American households (65.5 percent, comprising 73.5 percent of the population) would experience reductions in their disposable income, making them financially worse off. Those households would pay more in new taxes to fund the program than they would save as a result of the program eliminating their current spending on private health insurance and out-of-pocket medical expenses.
After accounting for both the tax increases and the reductions in private spending for health insurance and medical care, we find that average annual household disposable income would decline by $5,671 (or 11 percent) under a new government-run health care program.
Among households with employer-sponsored health benefits, 87.2 percent would be worse off financially under a new government-run health care program, and their annual disposable income would be $10,554 lower, on average. That would occur despite those households receiving wage increases, as employers responded to the new program by converting the value of current tax-free, employer-provided health benefits into additional taxable cash income.REF The reason: Workers would pay much higher taxes to fund the cost of the new program because workers would need to (1) replace their own private spending, (2) replace non-workers’ private spending, and (3) pay for the additional spending that would result from the program stimulating increased use of medical care.
Background
Over half of the Democrats in the House and 14 Democrats in the Senate have co-sponsored so-called Medicare for All bills, the key features of which are the establishment of a federal government-run health care program that would:
- Cover all U.S. residents;
- Provide comprehensive benefits, including coverage for items and services that are only covered to a limited extent today, such as dental, vision, hearing, and long-term care;
- Not charge patients any fees or co-payments for the care they receive;
- Replace existing private coverage and prohibit insurers and employers from offering plans that cover the same benefits as the new government program; and
- Replace the three major existing government coverage programs—Medicare, Medicaid, and CHIP.
As such, the proposal would fundamentally alter the structure and operations of the U.S. health system with numerous effects, not the least of which would be substantial increases in federal spending and taxation, as well as significant changes to the personal finances of American households.
Analysts from across the political spectrum have produced studies estimating the effects of such a program on total U.S. health spending and the federal budget. Those studies reached roughly similar conclusions.REF Namely, that a government-run health care program would increase federal spending by at least $30 trillion over the first 10 years of implementation, and that were such a program currently in effect, federal spending would be more than $2 trillion higher than it is now.
However, less attention has been devoted to calculating the taxation needed to fund what amounts to a 50 percent increase in federal spending.REF Yet, average Americans are less interested in how a government-run health care program would affect the federal budget or total U.S. health spending than in what its provisions, including the taxes to pay for it, would mean for their family’s finances.
The biggest changes would result from the legislation effectively “nationalizing” spending that is privately funded today—roughly half of total U.S. health care spending.
That means that Americans would no longer pay directly for any of their medical care or health insurance, and they would have to pay higher taxes to fund the new program. Furthermore, about half of American households are currently covered under employer-sponsored health plans. The cost of that coverage is part of the total compensation paid by employers to their workers, but it is excluded from the taxable incomes of those employees. Replacing those private plans with a new government program would also result in the value of those benefits being converted into taxable cash wages.
The financial effects of the legislation would differ for specific individuals and families depending on their employment status, their incomes, and the source and scope of their current health care coverage. For any particular household, the implementation of a government-run health program would produce one or more of the following effects: (1) reductions in the amount spent directly on health insurance and medical care, as a result of the new program providing comprehensive benefits with no premiums or co-payments for enrollees; (2) increases in the amount of taxable income, as a result of current non-taxable health benefits being converted into additional taxable compensation; and (3) changes to the amounts of federal and state taxes paid, as a result of the program eliminating current health care tax preferences and imposing additional taxes.
The analysis in this Special Report calculates the net effect on American families’ finances in four basic steps. First, we identify the additional costs to the federal government of a government-run health care program as envisioned in the proposed legislation. Second, we account for the increase to the tax base that would result from the legislation precipitating the conversion of current tax-free, employer-sponsored health benefits into additional taxable wages and salaries. Third, we calculate the increased taxation needed to fund the additional federal spending, relative to the revised larger tax base. Fourth, we calculate the effects on household finances of the changes to their spending on medical care and taxes.
The results are expressed as the net change to household disposable income after taxes and health expenses (that is, payments for premiums, co-payments, and unreimbursed medical care). Put another way, the net effect is the change in the amount of income a household has left for other purposes after paying taxes and health expenses under current arrangements versus under a universal federal health care program.
Limitations. These figures should be understood as a close approximation of how families and individuals will be affected by Medicare for All.
We limited our analysis to providing baseline estimates for how replacing private health spending with federal spending, and funding that additional spending with tax increases, would alter the federal budget and household finances. As such, our analysis is a static accounting of funding shifts and we did not attempt to estimate the effects of behavioral changes in response to higher tax rates. Further, we did not incorporate into our analysis assumptions about aspects of the legislation that are not specific enough to estimate their effects with confidence. Instead, we provide a separate discussion of those issues and their associated uncertainties in Appendix B.
We conducted sensitivity analysis and found little difference in the distributional results when assuming that some elements of the proposal design are more, or less, expensive than our baseline estimates.
Findings
Our analysis finds that if Medicare for All, as envisioned in the current House and Senate bills, were already in place, it would increase 2020 federal spending by $2.387 trillion, more than 50 percent.REF We also find that funding that increase in federal spending would require additional payroll taxes equal to 21.2 percent of all wage and salary income. Those taxes would be in addition to existing Social Security and Medicare payroll taxes, meaning that most working Americans would need to pay 36.5 percent of their wages in federal payroll taxes to fund both Social Security and a government-run health care program.
Among the population as a whole, household disposable income after tax and health spending would, on average, decline by $5,671 under a government-run health care program, with 65.5 percent of all households financially worse off than they are now. (See Table 1.)
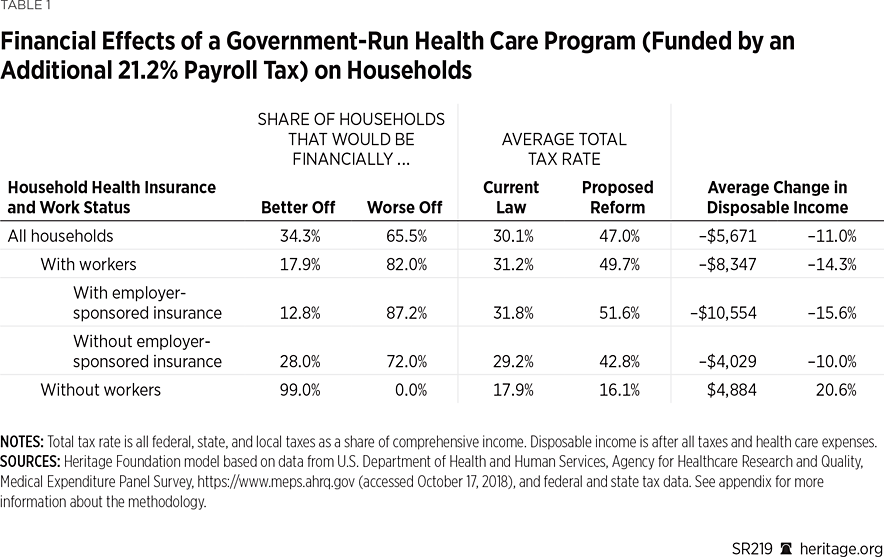
Specific effects and net results would differ for individual households based on the type and scope of their current health insurance coverage, the amount of their current out-of-pocket medical spending, the amount and sources of their income, the type of taxes imposed to fund the program, and whether a household has workers.REF
Effects on Working Households. Most households with workers (82.0 percent) would see their taxes increase by more than they would save from no longer paying privately for health insurance and medical care. That is mainly because they would need to pay new taxes to fund the new government spending that replaces both their own private spending and that of non-workers, as well as additional spending generated by the new program increasing demand for health care goods and services.
Effects on Working Households with and without Employer-Sponsored Coverage. The effect would be largest for working households with employer-sponsored insurance, whose disposable income would be $10,554 lower on average. In contrast, working households without employer coverage would see disposable income decline by an average of $4,029.
Most of that difference is explained by the fact that the average cash income of households with employer-sponsored insurance is nearly twice that of working households without employment-based coverage ($103,612 versus $58,963). That difference would further increase as employers responded to the legislation by converting tax-free health benefits into additional taxable compensation.
Effects on People Currently Enrolled in Medicare. Thirty-four percent of American households include at least one person who is covered by Medicare. Both the House and the Senate bills would replace Medicare with a new government-run health program that, unlike Medicare, would not charge premiums, deductibles, or coinsurance, and would cover additional benefits. On average, Medicare pays for only about 65 percent of an enrollee’s total health expenses, while the new program would cover nearly 100 percent of those costs.
Half (51 percent) of Medicare households include no workers (essentially, these are fully retired people). Those households would all be financially better off by an average of $5,368 if the new program was funded entirely through payroll taxes.REF This subset of households also accounts for 85 percent of all households without workers.
The other half (49 percent) of Medicare households—those with workers—would be financially worse off by an average of $2,768 under a government-run health plan because 53.8 percent of them would pay more in taxes than they would save as a result of the new program eliminating their current of out-of-pocket health spending.
Effects on Those Currently Covered by Medicaid and CHIP. Today, 18 percent of households have at least one person who is covered through Medicaid or CHIP (but not Medicare), and 90 percent of those households also have at least one worker. These households would be financially worse off by an average of $5,592, because 87 percent of them would pay more in taxes than they save from the elimination of their remaining out-of-pocket health spending. That is partly because individuals enrolled in Medicaid or CHIP would see little in the way of savings under the legislation since they already have comprehensive government-funded coverage. For the remaining 10 percent of households with Medicaid or CHIP enrollees that have no workers, those households would be financially better off by an average of $505.
Examples of Effects
To show how shifting to a government-run health care program would financially affect working households with different characteristics, we constructed the following five illustrative households, with the results summarized in Table 2. (See Appendix C for the full table for each illustrative household.)
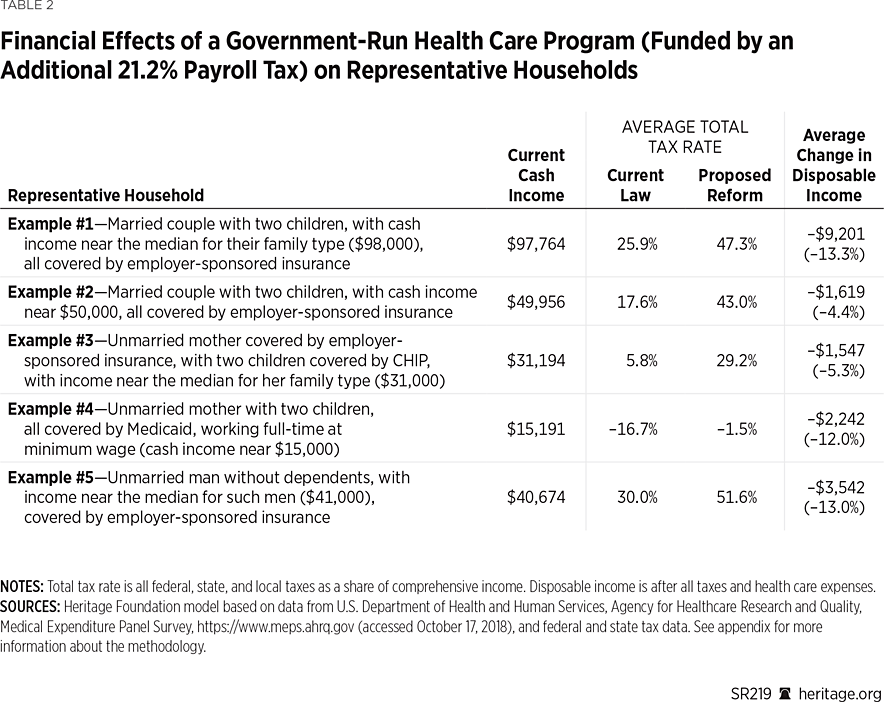
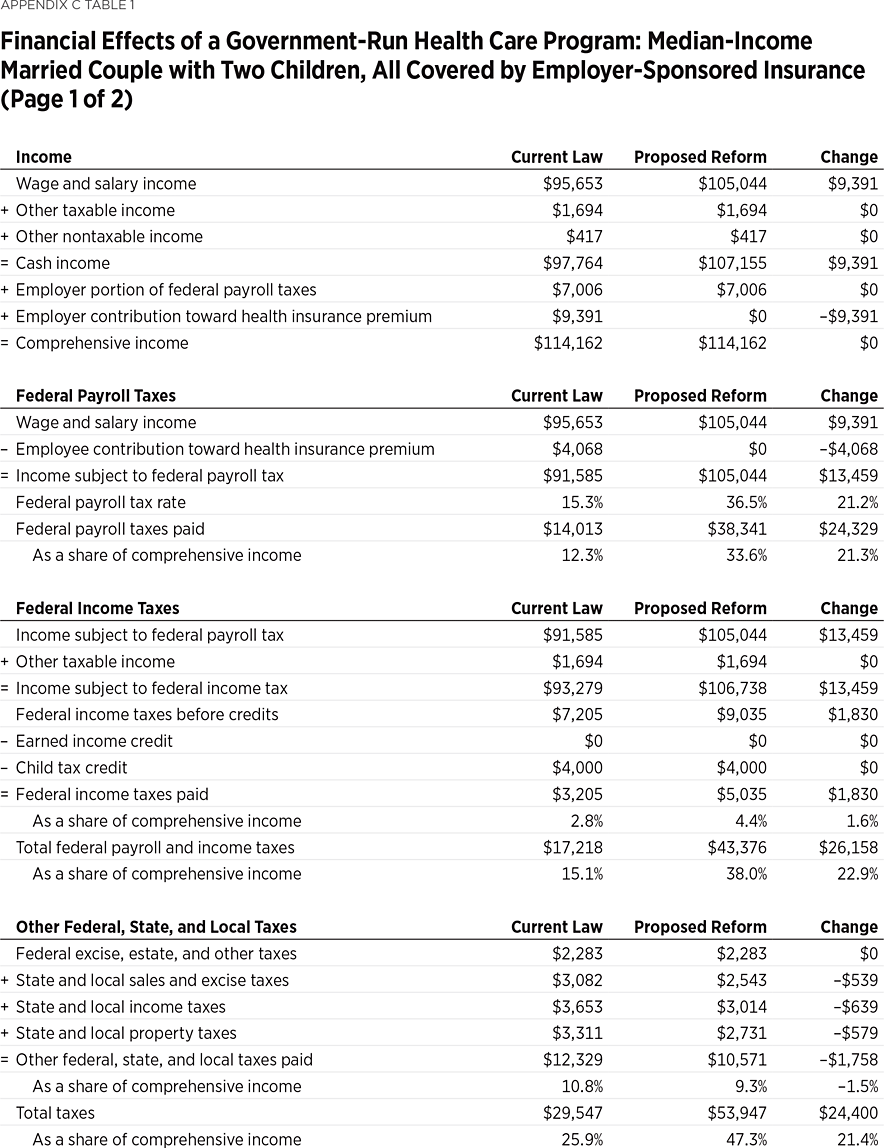
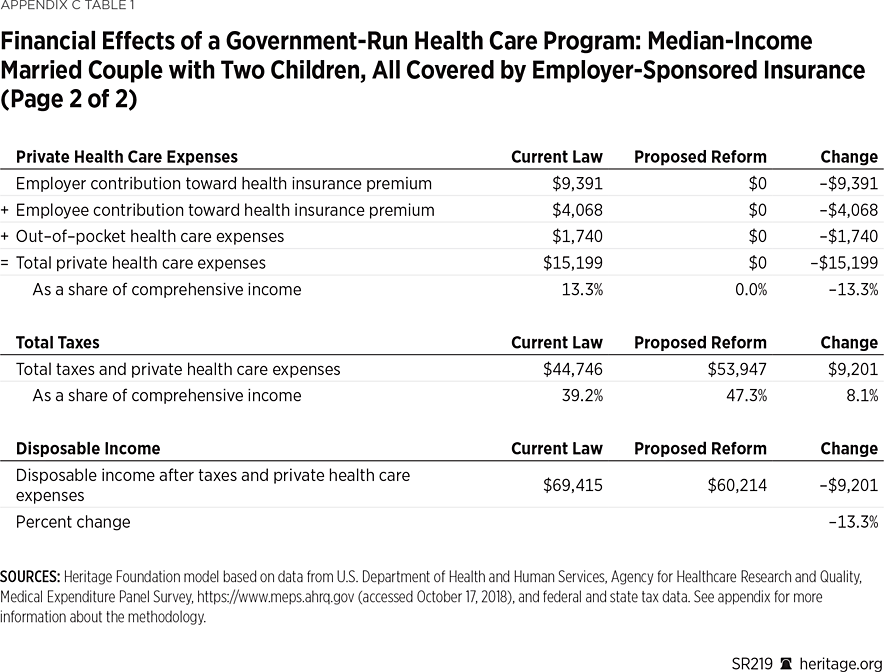
Example 1: A Median-Income Married Couple with Children and Employer Health Benefits Would be $9,201 Worse Off. A married couple with two children and cash income near the median for all such families (about $98,000), and covered by employer-sponsored insurance, would have $9,021 less in disposable income under a government-run health care program. While this family’s total income including employer-paid benefits would remain unchanged, the portion subject to taxation would increase by $13,459 (the sum of the $9,391 value of the employer contribution and $4,068 employee contribution toward the employer-sponsored insurance plan, which are currently untaxed).
Applying the higher federal payroll tax rate to the higher taxable wage base would increase their federal payroll tax bill by $24,329. Because more of their income is subject to tax, the couple would also pay an additional $1,830 in federal income taxes. While their state and local taxes would be reduced by $1,758, their total tax bill would increase by $24,400, to $53,947—47.3 percent of their total income. Eliminating their insurance premiums as well as their out-of-pocket medical expenses of $1,740 would save them $15,199 of private health care expenses, but it would not fully offset the increase in their tax bill. This middle-income family would see its net income (after taxes and private health expenses) decline by $9,201 (13.3 percent), from $69,415 to $60,214.
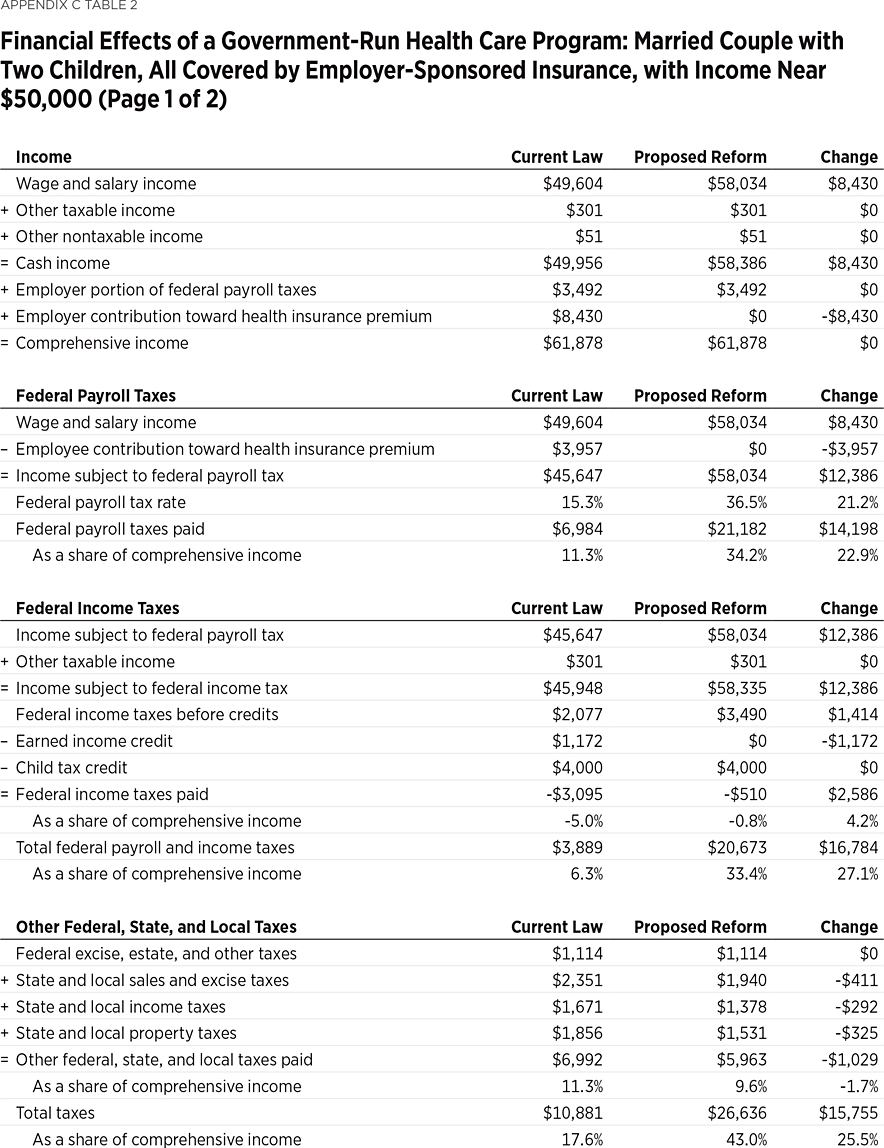
Example 2: A Lower-Middle-Income Married Couple with Children and Employer Health Benefits Would be $1,619 Worse Off. A married couple with two children, cash income near $50,000, and covered by employer-sponsored insurance would have $1,619 less in disposable income under a government-run health care program. While this family’s total income including employer-paid benefits would remain unchanged, the portion subject to tax would increase by $12,386 (the sum of the $8,430 value of the employer contribution and $3,957 employee contribution toward the employer-sponsored insurance plan, which are currently untaxed).
Applying the higher federal payroll tax rate to the higher taxable wage base would increase their federal payroll tax bill by $14,198. Because more of their income is subject to tax, they would also pay an additional $1,414 in federal income taxes and lose all $1,172 of their earned income credit. While their state and local taxes would be reduced by $1,029, their total tax bill would increase by $15,755 to $26,636 (43.0 percent of their total income). Eliminating their insurance premiums as well as their out-of-pocket medical expenses of $1,750 would save them $14,137 of private health care expenses, but it would not fully offset the increase in their tax bill. This lower-middle-income family would see its net income (after taxes and private health expenses) decline by $1,619 (4.4 percent), from $36,860 to $35,241.
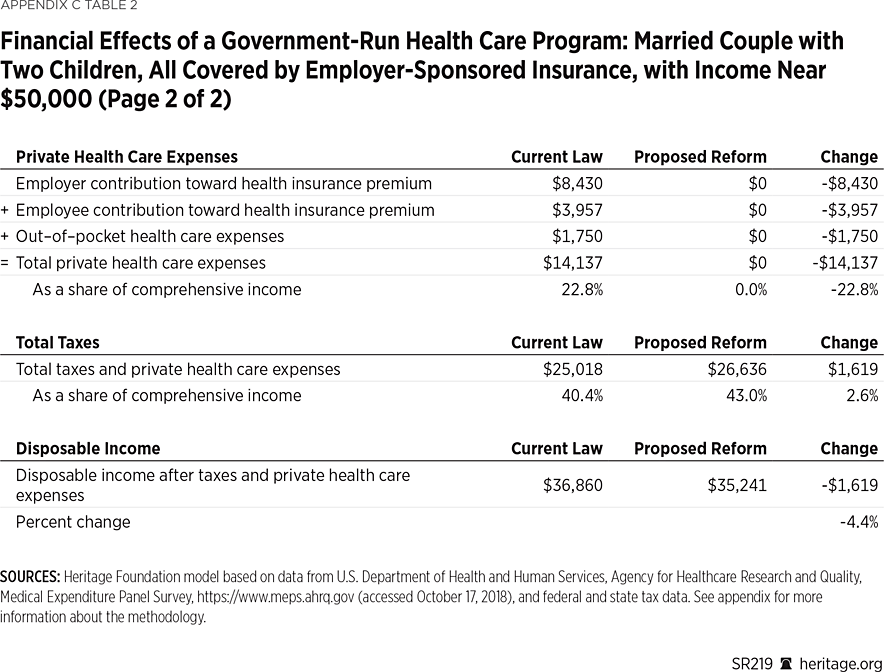
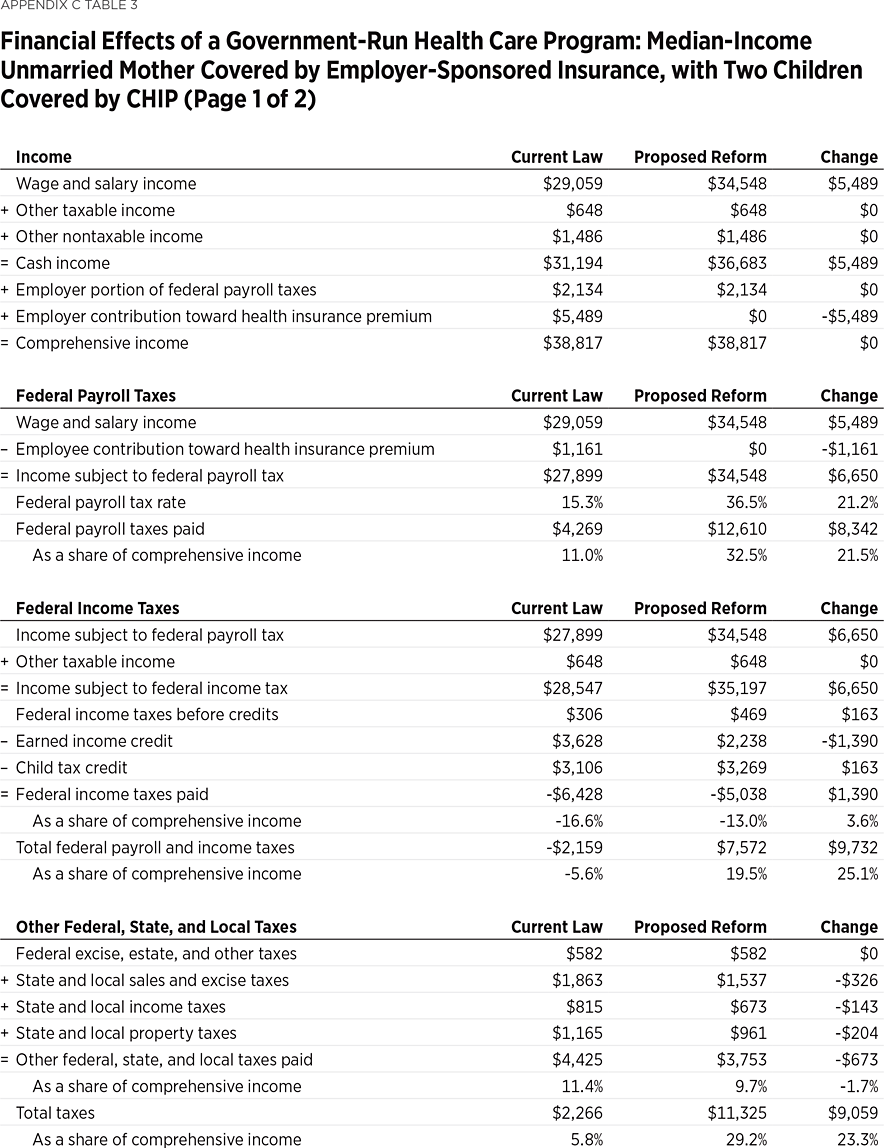
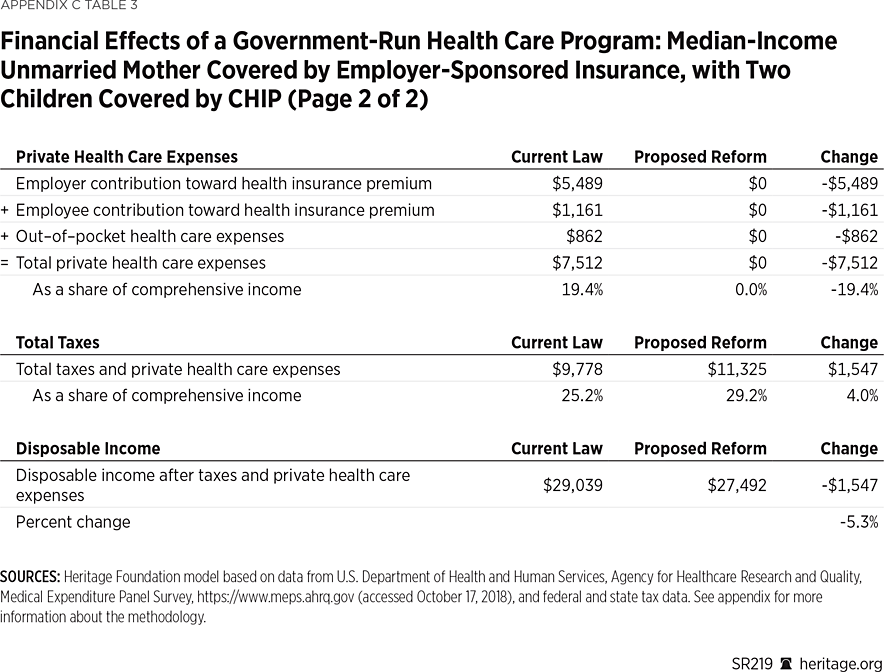
Example 3: A Median-Income Working Single Mother Would Be $1,547 Worse Off. An unmarried mother covered by employer-sponsored insurance, with two children covered by CHIP, and with cash income near the median for all such families (about $31,000), would have $1,547 less in disposable income under a government-run health care program. While her total income, including employer-paid benefits, would remain unchanged, the portion subject to tax would increase by $6,650 (the sum of the $5,489 value of the employer contribution and $1,161 employee contribution toward the employer-sponsored insurance plan, which are currently untaxed).
Applying the higher federal payroll tax rate to the higher taxable wage base would increase her federal payroll tax bill by $8,342. Because more of her income is subject to tax, she would also pay an additional $163 in federal income tax, which would be offset by an increase in the child tax credit, and she would lose $1,390 in earned income credit. While her state and local taxes would be reduced by $673, her total tax bill would increase by $9,059 to $11,325—29.2 percent of her total income. Eliminating her insurance premiums as well as the family’s out-of-pocket medical expenses of $862 would save her $7,512 of private health care expenses, but it would not fully offset the increase in her tax bill. This family would see its net income (after taxes and private health expenses) decline by $1,547 (5.3 percent), from $29,039 to $27,492.
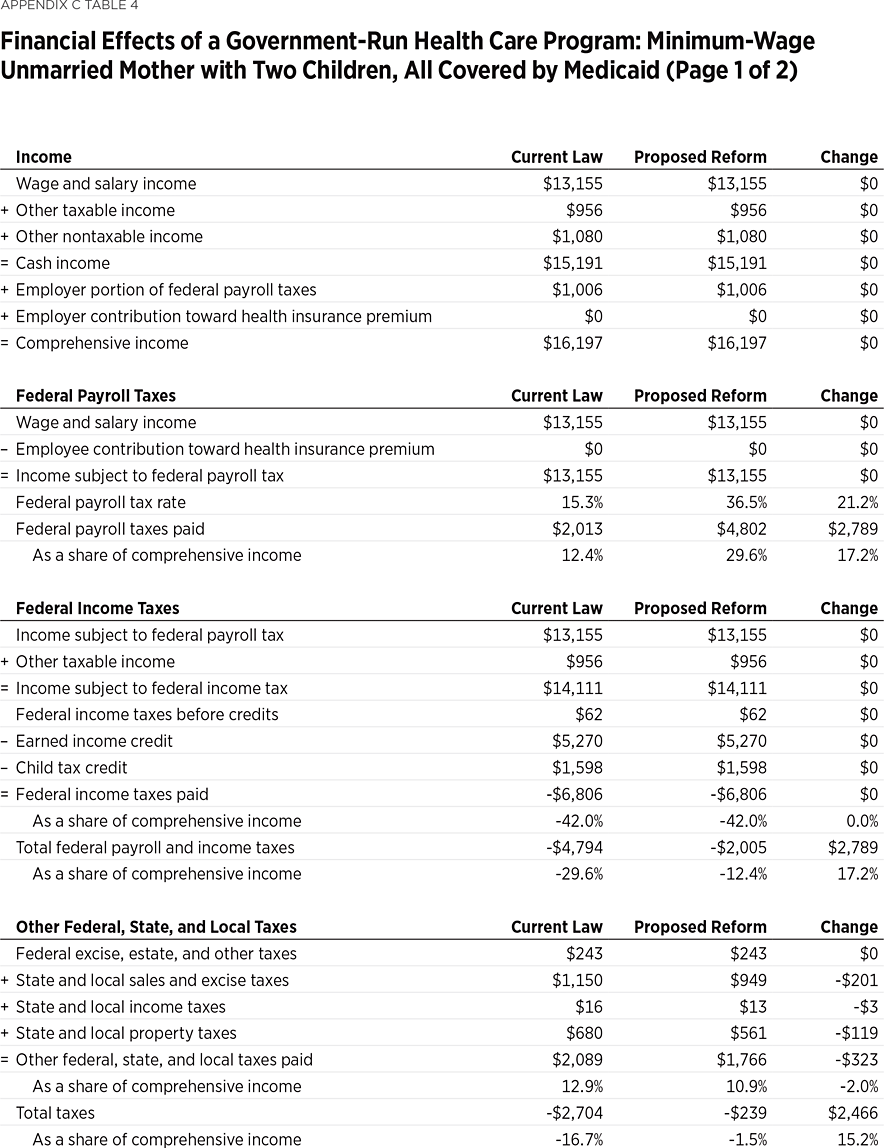
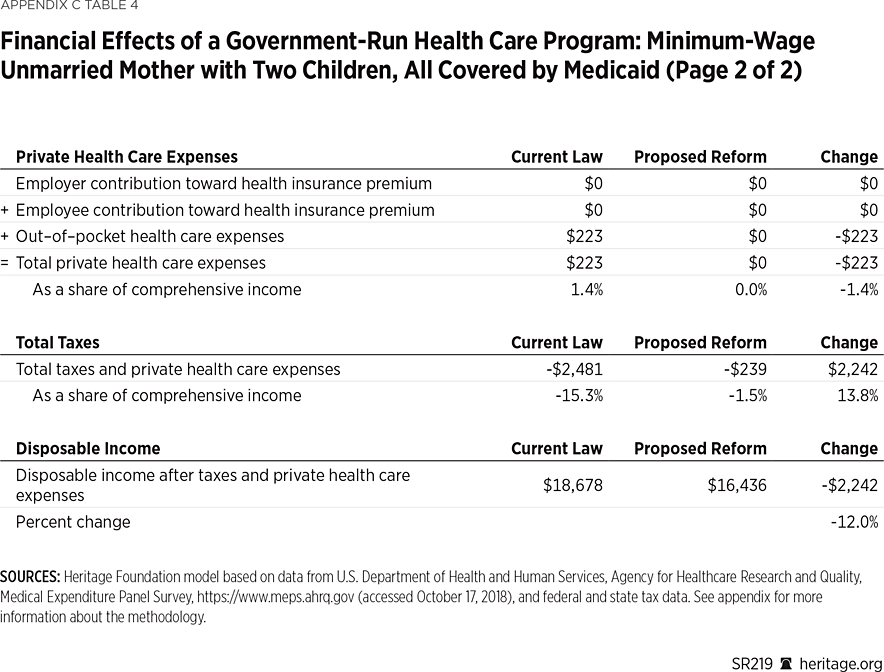
Example 4: A Single Mother Earning Minimum Wage Would Be $2,242 Worse Off. An unmarried mother with two children, all covered by Medicaid and with income near that of a full-time, year-round minimum wage worker (about $14,200) would have $2,242 less in disposable income under a government-run health care program. Applying the higher federal payroll tax rate to her taxable wages would increase her federal payroll tax bill by $2,789. Her federal income taxes would be unaffected, as she would continue to receive $6,806 in refundable tax credits (earned income credit and child tax credit).
Her state and local taxes would be reduced by $323. Because she receives more in refundable tax credits than she pays in total federal, state and local taxes, her current net benefit through the tax code is $2,704. Because she would be paying more in taxes under the proposed reform, her net benefits through the tax code would be reduced to $239, or 1.5 percent of her total income. This entire family is on Medicaid, so out-of-pocket medical expenses are low, at only $223, making the elimination of private health care expenses of little benefit to this household. This working-poor family would see its net income (after taxes and private health expenses) decline by $2,242 (12 percent), from $18,678 to $16,436.
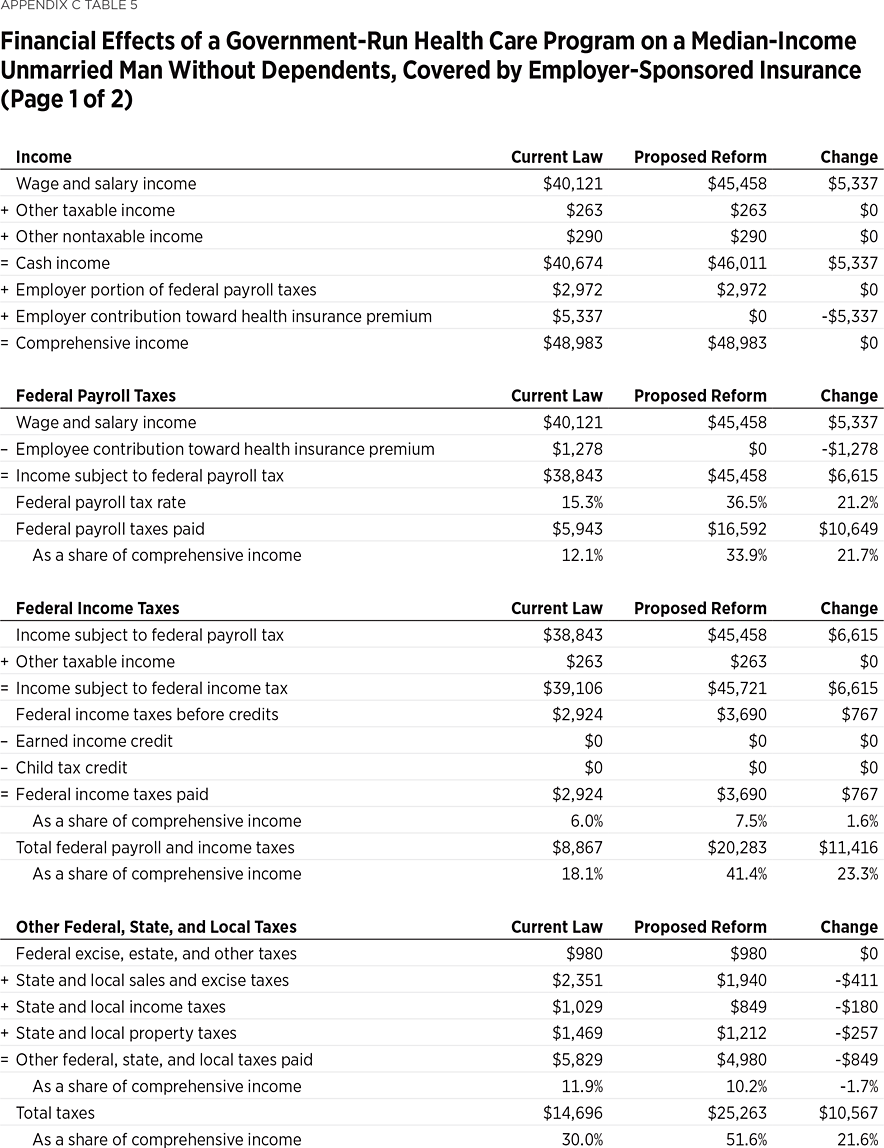
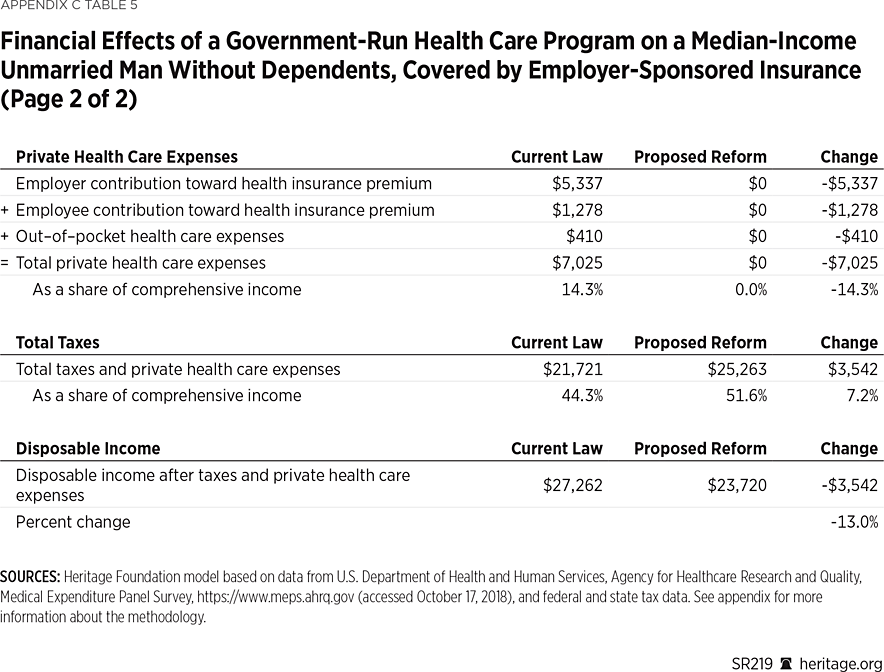
Example 5: A Median-Income Single Man Without Dependents Would Be $3,542 Worse Off. An unmarried man with no dependents, income near the median for all such individuals (about $41,000), and covered by employer-sponsored insurance, would have $3,542 less in disposable income under a government-run health care program. While his total income including employer-paid benefits would remain unchanged, the portion subject to tax would increase by $6,615 (the sum of the $5,337 value of the employer contribution and $1,278 employee contribution toward the employer-sponsored insurance plan, which are currently untaxed).
Applying the higher federal payroll tax rate to the higher taxable wage base would increase his federal payroll tax bill by $10,649. Because more of his income is subject to tax, he would also pay an additional $767 in federal income tax. While his state and local taxes would be reduced by $849, his total tax bill would increase by $10,567, to $25,263—51.6 percent of his total income. Eliminating his insurance premiums as well as his out-of-pocket medical expenses of $410 would save him $7,025 of private health expenses, but it would not fully offset the increase in his tax bill. This middle-income man would see his net income (after taxes and private health expenses) decline by $3,542 (13 percent), from $27,262 to $23,720.
Conclusion
Under a government-run health care program, most American workers would have to hand over 36.5 percent of their wages to the federal government. Those taxes would consist of: a new tax to fund Medicare for All—another 21.2 cents on every dollar earned—in addition to the payroll taxes of 15.3 percent that most workers already pay to fund the existing Social Security and Medicare programs. Furthermore, the new payroll tax would need to be imposed on every dollar of wages—from the first one earned by the lowest-paid worker to the last one earned by the highest-paid worker.
Overall, an estimated 65.5 percent of households comprising 73.5 percent of the population would be worse off financially under a new government-run health care program. The results would be even more skewed for households with employer-sponsored insurance, as 87.2 percent of them would be worse off financially under a government-run health care program.
Appendix A: Data and Methodologies
For reasons of both clear presentation and confidence in projections, our analysis assumes that the program is fully implemented in 2020.REF
I. Estimates of Additional Federal Spending

Appendix A Table 1 summarizes our baseline estimates for the effects on the federal budget of adopting a program with the same key features as those in the “Medicare for All” bills currently pending in the House and Senate.REF It shows that a government-run health care program would increase 2020 federal spending by almost $2.4 trillion.REF Our sources and calculations for each item in Appendix A Table 1 are as follows:
Replacing Private Spending. The program would replace current private-sector spending on health insurance and medical care with new federal spending for the same goods and services for the same population.
We used the most recent National Health Expenditure (NHE) estimates for private insurance and out-of-pocket spending. Because the program benefits do not include coverage for non-prescription drugs and non-durable medical supplies, we subtracted the NHE estimates for spending on those items from the NHE estimates for total out-of-pocket spending.REF
Replacing State Spending. The new program would replace Medicaid and CHIP. Currently, states pay a share of the costs for Medicaid and CHIP and also make payments to Medicare for drug coverage for dual-eligible beneficiaries. However, under the program, the federal government would become responsible for all of the cost of covering those same individuals. We calculated that additional cost to the federal government using the most recent Congressional Budget Office (CBO) projections.REF
One study assumed that the federal government would be able to capture much of the states’ savings, while another study reported alternative figures for spending by payer with, and without, that assumption applied.REF However, the pending bills do not include provisions to capture state savings, and any design for doing so would face significant practical and political obstacles.REF
For instance, Senator Elizabeth Warren (D–MA) proposes a “maintenance-of-effort requirement” on state and local governments under which current spending by those governments on Medicaid and CHIP and employee health benefits would be redirected to funding for the new federal program. She states, “This is similar to the mechanism that the George W. Bush Administration used to redirect Medicaid spending to the federal government under the Medicare prescription drug program.”REF
It is true that when Congress created the Medicare Part D prescription drug program, it included a provision to “claw-back” state Medicaid savings, stipulating that federal funding for the rest of a state’s Medicaid program would be reduced by an equivalent amount if the state did not pay its savings into Medicare.REF
Yet, under a new federal health program that replaces Medicaid, Congress would no longer have that leverage over states, since states would no longer need federal Medicaid funding. Furthermore, even if Congress chose to retain the existing Medicaid program just for institutional long-term care, as the Senate bill would, state savings from federalizing the rest of Medicaid would still exceed the loss to states of all federal funding for long-term care.
Increased Utilization. Because the program would be universal and would provide comprehensive benefits with first-dollar coverage, it would increase demand for health care goods and services. In the case of acute care services, the program would stimulate increased utilization in three ways: (1) by expanding coverage to U.S. residents who are not currently insured; (2) by providing comprehensive coverage of benefits that are currently covered to only a limited extent (such as dental and vision care); and (3) by eliminating all, or nearly all, patient cost sharing. In the case of long-term-care services, the primary effect would be the replacement of “informal care” provided by relatives, with “formal care” provided by home health workers and nursing facilities.
Appendix A Table 1 lists the estimated costs of increased utilization separately for acute-care services and for long-term care services. In each case, the estimates reported are the more conservative (that is, lower) of the projections in other studies.REF
Loss of Medicare Premium Revenues. Medicare enrollees pay premiums to the federal government for coverage under Part B (physician services) and Part D (prescription drugs). The legislation would subsume Medicare into the new program, which would provide those benefits—but without charging premiums to enrollees. While the bills do not explicitly repeal the relevant provisions of the Medicare statute, we assume that Medicare premiums would no longer be collected and that the federal government would need to replace those lost revenues.REF
Loss of Affordable Care Act (ACA) Tax and Penalty Revenues. Federal spending on ACA subsidies would also be transferred to the new program, but federal revenues generated by some other ACA provisions would disappear. Specifically, because both private health insurance policies and employer-sponsored health benefit plans would be eliminated, revenues collected from the ACA’s excise taxes on health insurance policies and on high-cost employer health plans, and from fines imposed on large employers that do not provide their workers with minimum coverage, would all fall to zero.REF
Elimination of Tax Preferences for Private Health Insurance. The House and Senate bills do not explicitly repeal the current tax preferences for private health care coverage. However, the bills functionally eliminate those tax preferences by prohibiting insurers and employers from offering coverage that duplicate benefits offered under the new government program.REF
The largest such tax preference, by far, is the tax exclusion for employer-sponsored health benefits. Under that provision of the tax code, amounts spent by employers and employees on employer-sponsored health benefits are excluded from the employee’s taxable income for purposes of both the federal income tax and the Social Security and Medicare payroll taxes. Replacing those private tax-free health benefits with coverage through a government health program would not only make that tax preference irrelevant but, as discussed in section II. Estimated Changes to the Tax Base, would also result in employers converting the value of those benefits into additional taxable wages paid to their workers.
Appendix A Table 1 reports our estimate of the additional tax revenues that the federal government would receive from the conversion of currently tax-free health benefits into additional taxable income. We constructed our estimate as follows:
- We used data from the Census Bureau’s Current Population Survey to calculate the average marginal tax rates for the income tax, Social Security tax, and Medicare tax for workers with employer-sponsored health benefits.
- We applied the resulting average marginal tax rates to the aggregate amount of newly taxable income (see section II. Estimated Changes to the Tax Base) to derive the increases in federal revenues from the three taxes.
- We subtracted from our estimate of increased Social Security tax revenues, the CBO’s estimate for the unfunded (deficit) portion of Social Security benefits for the year, as Social Security revenues are first applied to paying current benefits and annual benefit spending now exceeds annual revenues.REF
Similarly, the legislation would also functionally eliminate the income tax deduction for health insurance premiums paid by the self-employed and the non-refundable portion of the ACA income tax credits for individual-market coverage purchased through the exchanges. We include the CBO’s estimates for those provisions as additional revenues in Appendix A Table 1.
II. Estimated Change to the Tax Base
The largest effect of adopting the proposed program would be the replacement of almost all private spending on medical care with new federal spending. Because most current private health spending is through tax-free employer plans, that change would also significantly increase the tax base. Consequently, it is necessary to account for that effect before calculating the additional taxes needed to fund a government-run health care program.
Standard economic analysis expects that under the envisioned scenario (replacing employer-sponsored health insurance with a public program providing at least the same level of coverage) employers would convert spending on health benefits into additional taxable wages.REF That is because what matters to employers is the total amount of compensation paid for a worker’s labor, not the form in which the compensation is paid. Also, the sponsor of the Senate bill has recently proposed that, as part of the transition to the new program, employers would be required by law to convert the value of employee health plans into additional cash wages or other benefits.REF However, because other fringe benefits either have statutory maximums, or are subject to payroll taxes, or both, there is little scope for employers and workers to shift current spending on health benefits into other forms of tax-free compensation. Consequently, we assume that the entire value of employer-sponsored health benefits becomes additional taxable compensation.
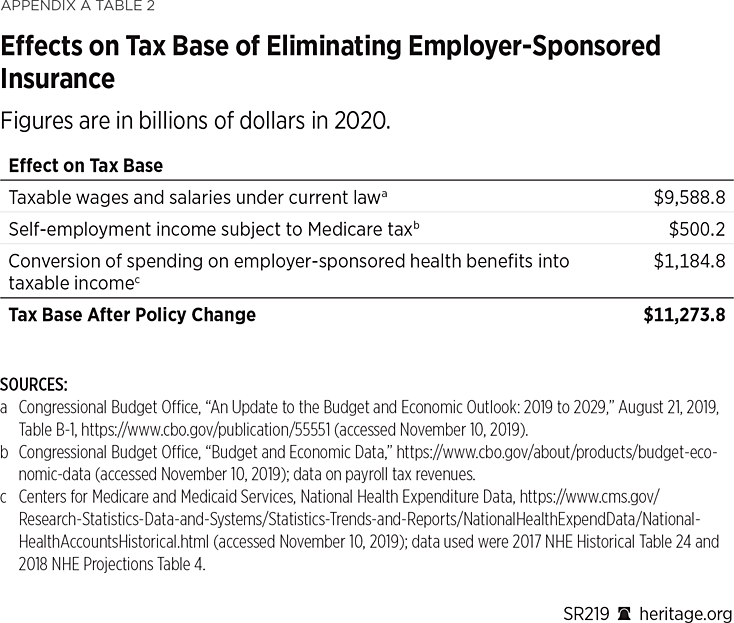
Appendix A Table 2 reports the components of the revised tax base. First is the CBO’s estimate of total wages and salaries. Second is an estimate of self-employment labor-income subject to the Medicare payroll tax.REF Third is the estimate of the additional cash income that would accrue to workers from converting pre-tax employer health benefit spending into taxable compensation.REF Summed, they show the revised tax base on labor income. The aggregate effects are that about 12 percent of total employee compensation would be shifted from non-taxed health benefits into taxable wages, increasing the total labor-income tax base by about 9.5 percent.
III. Estimating the Additional Tax Burden
Appendix A Table 1 shows that the net increase in federal spending under the program would be $2,387 billion in 2020, and Appendix A Table 2 shows that, after accounting for the conversion of employer-sponsored health benefits into additional taxable income, the 2020 labor-income tax base would be $11,274 billion. Consequently, the new federal taxes needed to fund the additional federal spending under the program would equal 21.2 percent of taxable payroll in 2020. That result is consistent with the findings of two other studies that provided tax-burden estimates.REF
The House and the Senate bills do not specify how the additional federal spending under the program would be funded. In order to estimate the tax effects of the proposal we applied the following assumptions:
- We assumed that the additional federal spending under the program would need to be funded through increased taxation. The current federal health programs that the legislation would fold into the new program are partially funded by federal borrowing, so we assume that level of deficit financing would continue under the new program. However, it does not seem plausible that additional borrowing could be used to finance the program’s new spending, given the federal government’s large, and growing, long-term fiscal imbalance.REF
- We calculated the additional federal tax burden as a percentage of taxable payroll, expressed as a uniform (uncapped) increase in the payroll tax rate. Not only is percentage of payroll a standard measure for quantifying the tax burden of social insurance programs, but a uniform payroll tax increase would generate fewer and smaller behavioral response effects than other possible tax increases.
- We assume that all of the increase in payroll taxes would be imposed on workers, and consequently, that the employer’s total employee compensation costs are the same after implementation as they were before implementation. Were all or part of the tax increase instead imposed on employers, it would produce additional adverse effects on cash compensation, employment, and business profitability—which, in turn, would necessitate even higher tax rates to collect sufficient revenues.REF
- Under the program, the federal government would need to replace current state and local government spending on Medicaid and CHIP. However, for purposes of calculating the effects on household finances we assume that states would pass their resulting savings on to their residents in the form of reduced state taxes. Thus, we account for that funding shift as a cost to the federal budget and as an offsetting saving to household budgets.REF
Currently, most American workers pay federal payroll taxes of 15.3 percent, of which 2.9 percent funds Medicare and 12.4 percent funds Social Security. Increasing payroll taxes by 21.2 percentage points to fund a government-run health program would mean that the payroll tax rate for most workers would be 36.5 percent.REF That result would be consistent with the payroll tax levels in a number of European nations, such as France, Germany, and Sweden, which operate comprehensive social insurance programs for both medical care and pensions.
Results Under Income Tax Financing Scenarios. As noted, we assumed that the program would be funded by a uniform increase in the (uncapped) payroll tax rate imposed entirely on workers because it is the scenario that would generate the least behavioral responses. The alternative of funding part, or all, of the program’s additional costs through increased income taxes would involve many more complexities, uncertainties, and behavioral responses. However, for comparison purposes, we also ran static analyses of the effects on household finances of partial and full funding through increased income tax rates.
Partial Income Tax Funding Scenario. Senator Sanders has suggested that part of the funding for his proposal could come from an “income-based premium” that appears to function as an increase of four percentage points in all federal ordinary income tax rates, and states that those whose income is less than their standard deduction would not be affected.REF Multiplying this tax rate by the $9,813 billion of income that would be subject to non-zero ordinary income tax rates at the federal level, we estimate that this tax would raise $393 billion in revenue in calendar year 2020.REF Under this scenario, the payroll tax would still need to be increased by 17.7 percentage points, making the total payroll tax 33.0 percent for most workers, to fund the remaining additional cost of the program.
We found that the distributional effects under this scenario would differ only marginally from those under our baseline assumption of financing the added spending entirely through a payroll tax increase. Overall, 64.4 percent of households—containing 71.8 percent of the total population—would see their disposable income after taxes and health expenses decline, down slightly from 65.5 percent and 73.5 percent, respectively, in the base scenario. Among households with workers, 84.7 percent of those with employer-sponsored insurance and 71.0 percent of those without employer-sponsored insurance would have lower disposable incomes, nearly the same as the 87.2 percent and 72.0 percent figures, respectively, in the base scenario. Only 2.7 percent of households without workers have high enough income from other sources that this partial financing through an income tax would cause their disposable income to decline under a government-run health program.
Income-Tax-Only Funding Scenario. For further comparison, we also ran our analysis using the assumption that all of the additional costs were funded by uniformly increasing all current income tax rates. Under static calculations, which do not account for behavioral response or macroeconomic effects, all ordinary income tax rates would need to be increased by 24.3 percentage points in order to fund the program. This would mean, for example, that the current 10 percent income tax bracket would be increased to 34.3 percent, while the current 37.0 percent income tax bracket would be increased to 61.3 percent, higher than at any point since the early 1980s. For this scenario, our result (an increase in income tax rates of 24.3 percentage points) is consistent with the result of the Committee for a Responsible Federal Budget (CRFB) study (a 25 percent income surtax).REF
Even under this scenario, we found that a slight majority of households would see their disposable income decline. The 52.2 percent of all households with lower disposable income after taxes and health expenses would include 67.0 percent of households with workers with employer-sponsored insurance, 44.6 percent of households with workers without employer-sponsored insurance, and 23.6 percent of households without workers. The households without workers who experience a decline in disposable income are generally retirees with substantial income beyond Social Security.
In addition to triggering numerous behavioral and macroeconomic effects, this scenario would also likely result in Congress making other changes to the income tax code, some of which, such as increasing tax rates on capital gains or subjecting a larger share of Social Security benefits to taxation, might further reduce the disposable incomes of retirees.
IV. Estimating the Effects on Household Finances
Our analysis is limited to the direct effects on household finances. We did not attempt to calculate welfare gains or losses to individuals resulting from the program altering the quantity of medical goods and services consumed.
We used the latest available (2016) data from the Medical Expenditure Panel Survey (MEPS) to estimate the net effects of the program on household finances. The MEPS Household Component (MEPS HC) of the survey includes basic demographic and health coverage information as well as specific questions about each person’s medical conditions, expenditures, attitudes, and experiences. Much of the reported data are verified and supplemented with information from health care providers to ensure quality. The data are weighted to ensure that they are representative of the U.S. civilian non-institutionalized population.
We assume that household members generally share resources, so aggregate changes in income and expenditures at the household level best reflect the change in well-being of individual members of the household.
We used the latest available data, collected from 12,704 households for the year 2016, to estimate the financial effects of a government-run health care program. We did so as follows:
- Convert existing employer-sponsored insurance into taxable wages and salaries;
- Impose existing federal tax law plus an additional 21.2 percent payroll tax, bringing the total federal payroll tax to 36.5 percent for most wage and salary income;
- Assume that all state and local taxes are reduced by 17.5 percent, to account for lower state revenue requirements due to the elimination of state payments for Medicaid, CHIP, and Medicare; and
- Eliminate private health care expenditures, including premiums and out-of-pocket expenses.
With respect to the conversion of employer-sponsored insurance:
- Employee contributions may currently be deducted from gross income prior to the computation of both payroll and income taxes. Thus, we assume that all employee contributions are currently not taxed, and under the program become part of the worker’s taxable income for purposes of both types of taxes.
- Employer contributions are estimated based on data from the MEPS Insurance Component (MEPS IC), which surveys employers on the characteristics of their insurance plans. An employer’s contribution toward health insurance premiums will currently vary across eligible employees within any given firm based on whether the employee elects self-only or family coverage or declines coverage altogether. Converting those contributions into additional taxable wages or salaries for each employee on an individual basis would create both practical and legal issues for employers as it could produce significantly different new base pay rates for employees that previously received identical base pay. Consequently, we assume that under the reform each employer would convert the aggregate amount of its health plan contribution into base pay increases for all employees that were eligible to participate in the plan at the time of its dissolution. We further assume that the amount of increased pay would be equal to the average amount per eligible employee that the employer had been contributing. That additional wage and salary income is then taxed at the employee’s ordinary rates.
- We assume that the employer’s total employee compensation costs are the same after implementation as they were before implementation.REF
With respect to federal, state, and local taxes:
- We assume that the additional federal payroll tax is paid by the employee, which is consistent with its primary economic incidence.
- For federal taxes other than income and payroll taxes, we applied average tax rates as a share of income, by income level and family structure of the tax-filing unit, for the year 2017 from the Tax Policy Center’s microsimulation tax model.REF
- For state and local taxes, we applied average tax rates as a share of income, by income level of the tax-filing unit, for the year 2018 from the Institute on Taxation and Economic Policy’s microsimulation tax model.REF
- We took the figure for total state Medicaid and CHIP spending of $262 billion in 2019 and divided it by total state and local tax revenues of $1,497 billion for the most recent 12 months to derive a ratio of 17.5 percent.REF We then assumed that household state and local taxes would be reduced by that percentage. Because it is highly unlikely that all states would cut taxes to offset their reduced Medicaid spending, and also highly unlikely that states would cut taxes dollar for dollar to exactly match spending reductions, these estimates are biased toward showing households being better off than they actually are likely to be under a government-run health care program.
With respect to creating the composite household for each illustrative example, we:
- Selected all MEPS households that fit the criteria for household structure.
- Identified a target income value, generally the median reported total income for the household type.
- Retained all households with reported total income within 10 percent of the target value, in order to obtain a sufficiently large sample so that later calculations would be less sensitive to households that were outliers in terms of the composition of income or the level or composition of medical expenses.
- Averaged the reported values across these households to create values for the composite household for each category of income or medical expense. Each composite illustrative household therefore has the average characteristics of all households with the stated household structure and total reported income within 10 percent of the stated target value.
Appendix B: Uncertainties
There are two types of assumptions that we did not incorporate into our baseline analysis: (1) behavioral effects related to economic decision making, and (2) aspects of the proposed legislation that are not specific enough to estimate with confidence.
Work Disincentives and Economic Growth. The creation of a government-run health program that replaces privately funded employer-sponsored health benefits would likely induce some workers to reduce their hours worked or to cease working. The workers most likely to do so are the ones for whom maintaining their current private coverage is a primary factor motivating them to continue working today. We expect that this work-disincentive effect would be greatest for workers above the age at which they can qualify for retirement benefits and for secondary workers in households with more than one worker. We did not attempt to estimate the magnitude of this effect. To the extent that it occurs, it would reduce the tax base for funding the program and require higher taxes on remaining workers.
We also did not attempt to estimate overall macroeconomic effects of this potential reduction in work hours or other aspects of the proposal that could slow economic growth and reduce the tax base relative to the baseline. Therefore, our estimated tax rates are likely to be somewhat lower than those that would be required to fund the program.
Provider Payments. The House and Senate bills offer only broad guidelines for how federal officials are to set payments. Consequently, our analysis did not include any assumptions about changes to provider payment rates under the program. We instead assume that the program will reimburse providers at rates equivalent to the payer-weighted average rates that they currently receive.
The House bill would pay institutional providers on the basis of negotiated global budgets, encourage salaried employment of physicians, and create a new fee schedule for providers that continue to be reimbursed on a fee-for-service basis.REF Given that the House bill does not further specify how those new budgets and rates would be set, it is impossible to project eventual payments under the House bill and compare them with current reimbursement levels.
Under the Senate bill, providers would be paid according to “fee schedules” that are “consistent with” Medicare’s current processes for setting payment rates.REF Medicare physician payment rates are currently estimated to be about 75 percent of those for private preferred provider organization (PPO) plans, while Medicare hospital payment rates are about 60 percent of those for private insurance.REF Hospital payment rates for Medicaid are about the same as those for Medicare, while physician Medicaid rates are generally lower than Medicare. Given that there are currently about 58 million Medicare beneficiaries, 74 million Medicaid and CHIP enrollees, and about 175 million Americans covered by private insurance, uniform reimbursement at Medicare rates would result in significant net income reductions for hospitals and doctors.
While the cost of the program could be reduced by paying providers less, analysts differ in their assessments of how far payments could be reduced before patient access to care becomes restricted due to an insufficient supply of providers to meet demand.REF However, we find that even significant provider payment reductions would have only a modest effect on the required new federal spending and taxes.REF
Administrative Costs. Analysts differ over whether administrative costs would be lower under a government-run health program. Given that the changes will have only marginal effects on the overall cost of the program, we did not attempt to estimate them.
One recent study compared the health spending of Medicare enrollees covered by traditional Medicare (public plan) with those in Medicare Advantage (private plans) and found that, after adjusting for possible differences between the two groups, total spending for the Medicare Advantage group was 9 percent to 25 percent lower than that for the traditional Medicare group. The study found that the difference “primarily reflects lower utilization of services rather than lower payments for the same services.”REF That suggests that eliminating the administrative costs associated with private plans managing utilization and encouraging the substitution of less expensive care could actually result in a net increase in total costs under the envisioned government-run health program.
In contrast, three studies that estimated the cost of Medicare for All concluded that administrative costs could be as low as 6 percent of total program costs.REF One of those studies quantified that, under the assumption that the new program operated with administrative costs at the 6 percent level, the projection of $4,091 billion in total national health spending in 2020 would be reduced by $74 billion.REF Similarly, a 2013 analysis of the Vermont single-payer proposal projected that administrative costs would account for 7 percent of total costs for that program.REF Also, a 2018 analysis of a proposed single-payer program for New York projected that administrative costs would be 6 percent of total cost, in part based on that study’s finding that administrative costs currently account for 7 percent of New York Medicaid program expenditures.REF
Reduced Pharmaceutical Spending. Both the House and Senate bills would have the government negotiate the prices it pays for prescription drugs, “promote the use of generic medications,” and establish a drug formulary. Given that generics now account for about 90 percent of prescriptions, but just 23 percent of total drug spending, any savings would have to come predominantly from reduced spending on newer medicines that still have market exclusivity.REF Even so, total spending on pharmaceuticals accounts for only about 10 percent of total personal health spending, meaning that there is limited scope for savings in this area. One study estimated $54 billion in savings in 2020 from system-wide reductions in prescription drug payments, but the author of the study noted that his estimate is based on an “aggressive assumption” that almost all current brand-name prescriptions would be filled with generics at an average price reduction of 80 percent.REF Thus, such estimates are highly uncertain and it is hard to envision how payment reductions at, or even near, that level could be achieved without effectively eliminating incentives for the development of new drugs in the process.
Increased Social Security Payments. The conversion of tax-free employer coverage into taxable wages would increase the “average indexed monthly earnings” (used to calculate a worker’s Social Security benefits) of most of the workers receiving wage increases. That would make many of those workers eligible for higher-benefit payments when they retire, which would have a secondary effect on the federal budget of increasing Social Security’s future obligations.
Appendix C
Edmund F. Haislmaier is Preston A. Wells Jr. Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Jamie Bryan Hall is Research Fellow in Quantitative Analysis in Domestic Policy Studies.



