Abstract: If implemented as enacted, Obamacare will impose significant new Medicaid costs on states and constitute a major federal usurpation of long-standing state authority in regulating private insurance. This will be expensive and disruptive for those Americans who rely on individual or employer-based insurance for their health insurance. While some of the most expensive and disruptive provisions of the massive legislation do not take effect until 2014, other provisions are already going into effect and state lawmakers need to act right away if they are to implement their own Medicaid and private insurance market reforms to mitigate the harmful effects of Obamacare. State lawmakers must recognize that states are not mere agents of the federal government. They are not powerless, and there is nothing that requires them to assist in implementing this new, misguided federal health care agenda. They should assert their rightful authority, and represent and protect their citizens by resisting the disruptions entailed in Obamacare—taking actions that pressure the next Congress to scrap or redesign this harmful federal legislation.
The recently enacted Patient Protection and Affordable Care Act, the federal government’s sweeping health care legislation, will impose significant new costs on state government budgets, while also constituting a significant usurpation by the federal government of long-standing state authority over health insurance regulation.
The immediate task for state lawmakers is to find ways to protect their constituents—including state taxpayers, health insurance policyholders, and individuals who depend on public health care programs—from the adverse effects of Obamacare.
The fact that some of the most expensive and disruptive provisions of Obamacare do not take effect until 2014 should not lull state lawmakers into thinking that they can wait for the results of the Obama Administration’s regulatory implementation or the outcome of the renewed health care legislative battle in the next Congress before acting. Some significant provisions took effect upon enactment and a number of others will go into effect later this year or next year.
Thus, governors and state legislators need to start planning their responses and start drafting any applicable legislation for consideration in their next legislative sessions—now. Failure to do so means surrendering control over a large share of their states’ current budgets to federal officials and becoming passive bystanders as—faced with an onslaught of new federal regulation—private insurers scramble to position themselves for an Obamacare market by taking steps that will likely result in less insurer competition, fewer plan choices, and higher coverage costs, all beginning next year.
The wisest approach for state lawmakers is to take steps that better position their states for either of two possibilities: a new Congress that repeals Obamacare, or a protracted, multi-year political and legal battle conducted against the backdrop of an Administration attempting to implement the legislation as enacted.
A Massive Expansion of Medicaid
The Medicaid coverage provisions of the new federal health care legislation will result in an enormous expansion of state Medicaid rolls. This Medicaid expansion will account for over half of the estimated reduction in the uninsured population under Obamacare.[1]
Starting in 2014, the legislation requires states to extend Medicaid eligibility to all non-elderly individuals with family incomes below 133 percent of the federal poverty level (FPL). This mandatory coverage expansion will principally consist of two groups. The first group consists of parents or caregivers of children, where the children are eligible for Medicaid. While almost all children in families with incomes below 133 percent of FPL are already eligible for either Medicaid or the Children’s Health Insurance Program (CHIP),[2] only five states and the District of Columbia extend Medicaid coverage to all parents or caregivers with incomes below 133 percent of FPL.[3] An additional 15 states now provide Medicaid, or similar coverage—or in some cases more limited coverage—to some, but not all, parents with incomes below 133 percent of FPL.[4]
The second, and much larger, group of new enrollees will consist of non-elderly, non-disabled adults without dependent children, who have incomes below 133 percent of FPL. Until now, Medicaid coverage could only be extended to able-bodied adults without dependent children as part of a demonstration waiver program. The new health care law not only permits states to extend Medicaid coverage to such individuals beginning immediately, but also requires states to cover them starting in 2014.
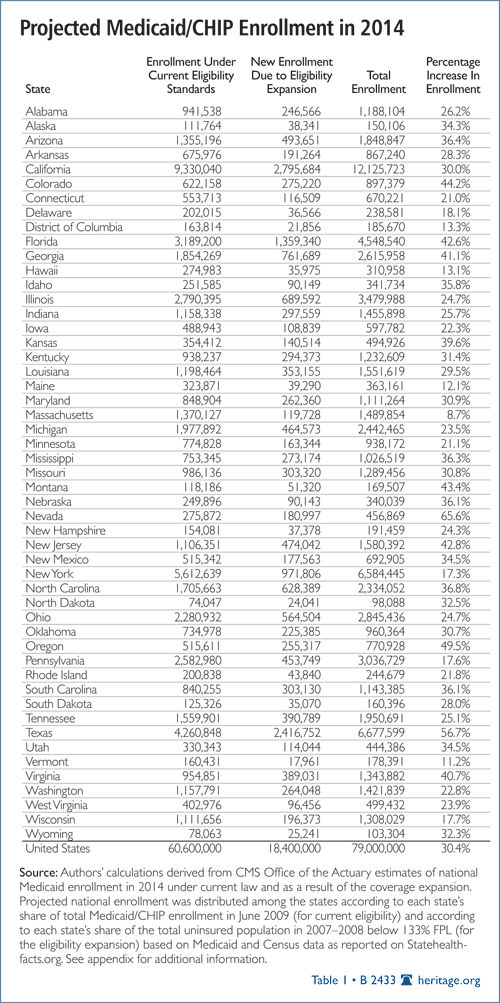
Table 1 provides Heritage Foundation state-level enrollment projections for 2014—the first year of the mandatory-coverage expansion— derived from national estimates from the Centers for Medicare and Medicaid Services (CMS) Office of the Actuary. The CMS Actuary projects that national Medicaid enrollment in 2014 will be 30.4 percent higher as a result of the required coverage expansion than it otherwise would be absent those provisions.
At the state level, Heritage estimates that the growth in Medicaid caseloads will range from an 8.7 percent increase in Massachusetts to a 65.6 percent increase in Nevada.
What Medicaid Expansion Will Cost States
Obamacare attempted to appease state lawmakers by committing federal taxpayers to paying for the entire benefit costs of the Medicaid expansion from 2014 to 2016. In 2017, state taxpayers will be on the hook for 5 percent of the benefit costs for the additional enrollees, with each state’s share then increasing to 6 percent in 2018, 7 percent in 2019, and 10 percent in 2020 and thereafter.[5]
Beyond the benefits costs of the expansion, there will be additional administrative costs to both the federal and state governments. The added costs are not included in the estimates prepared by the Congressional Budget Office (CBO) and the Centers for Medicare and Medicaid Services, but they will be a significant expense for states. Administrative costs are divided between state governments and the federal government at separate, uniform match rates. The standard administrative cost match rate is 50 percent, though the federal government provides higher match rates (in most cases 75 percent) for a few, discrete administrative expense items, such as certification of nursing facilities or operation of a state Medicaid fraud control unit.[6]
The most recent available data show that administrative expenses add an average of 5.5 percent in addition to total (federal and state) benefit costs, and that, on average, the federal government pays 55 percent of total administrative costs, with the other 45 percent paid by the states.[7] Thus, every $100 increase in benefit spending can be expected to generate another $5.50 in administrative costs, of which states would pay $2.48. Because the legislation does not change the match rates for administrative costs, states will still have to pay their share of administrative costs, even during the initial three years of the expansion when the federal government is funding all of the benefit costs.
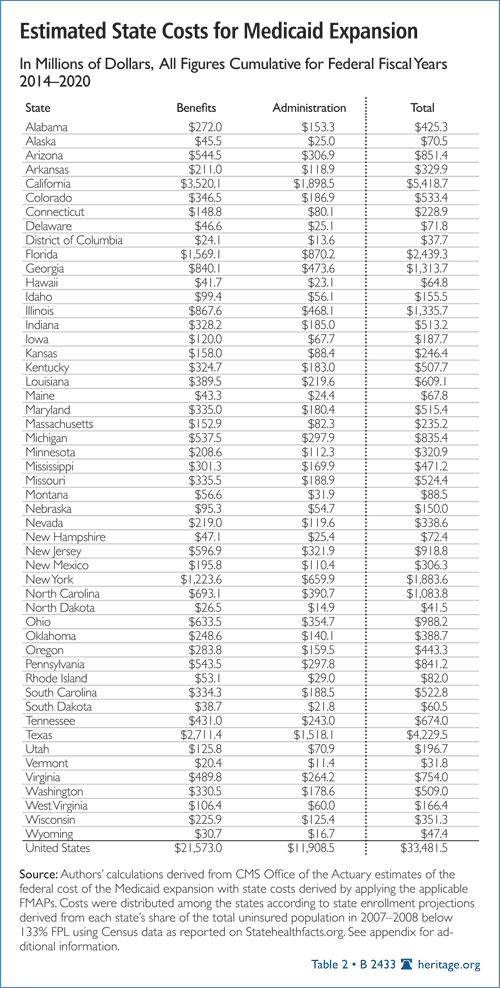
As shown in Table 2, The Heritage Foundation’s initial estimates are that the Medicaid expansion will increase state tax obligations by just under $33.5 billion for federal fiscal years (FY) 2014 through 2020. Of that amount, $21.5 billion will be the states’ share of the benefit costs, and just under $12 billion will be the states’ share of the added administrative costs. Indeed, the state share of administrative costs for the expansions will exceed $100 million a year in each of the four biggest states—California, Florida, New York, and Texas. In fact, the complexity of the system with separate rules for three classes of individuals— those who qualify for Medicaid under prior rules, those who qualify under the new expanded Medicaid eligibility rules, and those who instead qualify for the new subsidized coverage administered by the exchanges—will likely produce actual administrative costs that are higher than these estimates.
It is also important to emphasize that the total cost (federal and state) of the Medicaid expansion— which, based on CBO and CMS estimates, will likely be between $400 billion and $500 billion over the first seven years—will be shouldered by taxpayers. Although some state policymakers may think that the Medicaid expansion is a relatively good fiscal deal for their states because the federal government will pick up at least 90 percent of the cost for newly eligible individuals, taxpayers in their states will face higher tax bills as a result, not just for the state costs but for the federal costs as well. Furthermore, the additional federal taxes or borrowing needed to fund this expansion will inevitably dampen economic activity in the states.
“Crowd Out” Effects. Under the new law, Medicaid coverage will extend not only to those who are currently uninsured and whose income is below 133 percent of the FPL, but will also sweep into the program several million individuals below that income threshold who are currently covered by private employer-sponsored coverage or individual coverage. This “crowding out,” or displacement, of private coverage will most likely occur among individuals who work for businesses with fewer than 50 employees. The reason for this is that the law exempts the vast majority of such firms from the new mandate on employers to provide coverage— which will apply to larger firms starting in 2014.[8] Given that their workers will qualify either for Medicaid or for heavily subsidized coverage through the new health insurance exchanges, many small businesses that currently offer coverage will likely terminate their health insurance plans in 2014.
While the employer mandate penalties may discourage larger employers from dropping their plans, it is likely that many of the large firms that are still providing coverage after 2014 will offer only the minimum level of required coverage. Thus, states can expect that even those low-income workers who still have access to a large employer plan will likely enroll in Medicaid as “wrap-around” coverage.
“Woodwork” Effect. States can expect their Medicaid program costs to further increase in 2014, as a result of what Medicaid officials refer to as the “woodwork” effect—meaning, that individuals who qualify under current law for Medicaid, but who have not yet enrolled, will “come out of the woodwork” to do so.
This effect will result from the interaction of other provisions in the legislation with the Medicaid expansion. Specifically, the legislation establishes a new set of generous health insurance subsidies for individuals with incomes below 400 percent of the FPL, administered through new health insurance exchanges. The health insurance exchanges also have the task of determining eligibility for those new subsidies. In cases where an exchange determines that an individual qualifies for Medicaid, instead of for the new subsidy system, the law requires the exchange to enroll that individual in the applicable state Medicaid program. State Medicaid officials are required to accept such individuals into their programs and are prohibited from conducting their own separate eligibility determination.[9] If the individual in question is eligible for Medicaid coverage under the eligibility criteria for the state’s Medicaid program that is in effect immediately before the passage of the new federal legislation, then the state’s Medicaid costs for that individual will be matched by the federal government according to the state’s standard match rate. (The higher match rates will apply only to spending for individuals considered part of the “expansion” population under the new federal law.) Thus, states will experience yet higher costs associated with the enrollment of individuals who had qualified for Medicaid under prior eligibility standards, but who had not previously enrolled in the program.
Exporting “Doc Fix” to the States
Another provision in the new federal legislation requires states to increase Medicaid reimbursement rates for primary care physicians (PCPs) to the same level as the applicable Medicare payment rates for the 24-month period of January 1, 2013, to December 31, 2014.[10] The legislation specifies that the federal government will pay all of the added costs. However, this provision will trigger a Medicaid “doc fix” issue for some states starting January 1, 2015— when both the mandate, and the federal funding to compensate for its costs, will expire.
Doc fix has become congressional slang for legislation to cancel automatic reductions in Medicare physician payment rates. Absent legislative overrides, the fees that Medicare pays doctors would automatically decline based on a formula included in 1997 legislation that was supposed to limit Medicare spending growth. However, since then, Congress has repeatedly bowed to political pressure and concerns that enrollees will lose access to care by passing legislation to cancel the physician payment cuts.
The new legislation sets up a similar political dynamic for the Medicaid program and state lawmakers. When the mandated increase in Medicaid primary care physician rates (and the associated federal funding) ends, states could theoretically reduce Medicaid PCP payment rates to their previous levels, but both physicians and their Medicaid patients are likely to lobby against such a move. The alternative, of course, is for states to continue to reimburse PCPs at the higher rates, but with state taxpayers covering the state’s share (based on normal match rates) of the extra costs.
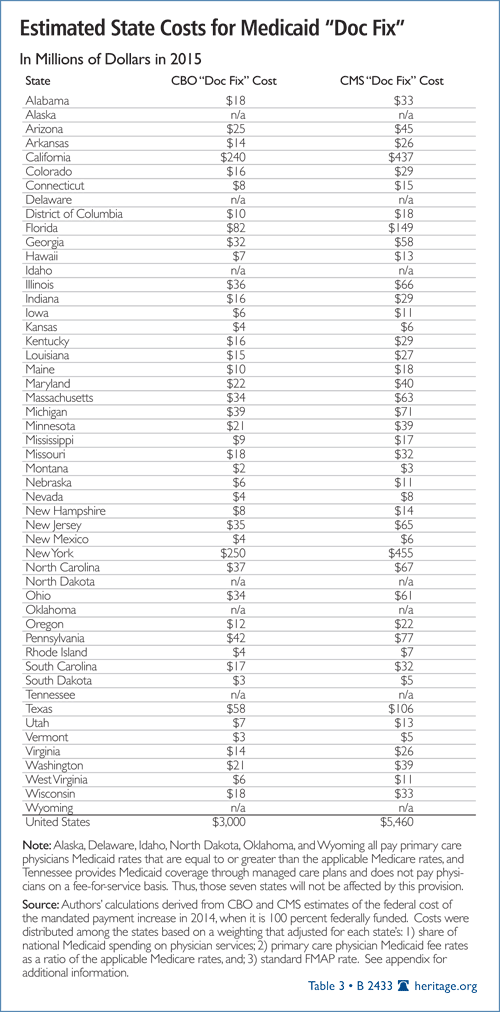
As Table 3 shows, increasing primary care physician payment rates will not be an issue for the six states that already pay Medicaid rates to PCPs equal to or in excess of the applicable Medicare rates. Furthermore, for the 18 additional states that pay Medicaid rates between 80 and 98 percent of Medicare rates, the state cost impact will be minimal. However, a number of states, most notably New York and California, would incur significant state costs if they continued to reimburse PCPs at the higher rates after 2014.
The states that will be most affected are those that have both low Medicaid payment rates for primary care physicians and low federal match rates for their Medicaid programs. For example, New York’s Medicaid rates for PCPs are only 36 percent of Medicare rates; New Jersey’s are 41 percent; and California’s are 47 percent—while all three states have a 50 percent federal match rate for their Medicaid programs. Thus, Medicaid rates paid to PCPs in California and New Jersey will more than double from their current levels, and rates in New York will nearly triple, between 2013 and 2014. Continuing those payment levels after 2014 will require taxpayers in all three states to fund half the extra costs.
This also explains why states’ costs will increase even when the federal government picks up the costs associated with the expansion. Because provider reimbursement rates are uniform across the eligibility groups, any rate increase will apply to current enrollees as well as to the newly eligible.
In some states providers have obtained federal court injunctions preventing the state from reducing Medicaid reimbursement rates. For example, in March, a federal appeals court affirmed the district court’s order of a preliminary injunction preventing implementation of Medicaid provider payment reductions enacted by the California General Assembly last year.[11]
Other Medicaid Costs for the States
Beyond the extra Medicaid costs that states are certain to incur, there are some other state Medicaid cost increases that are probable, but not definite. The two most significant items in this category are payments to so-called Disproportionate Share Hospitals (DSH) and payments to specialist physicians.
DSH Payment Reduction. DSH funding consists of extra, lump-sum Medicaid payments to hospitals that treat a “disproportionate share” of Medicaid patients. Theoretically, DSH payments help defray those hospitals’ costs of providing uncompensated care to the low-income uninsured, though most states have little real accounting control over how hospitals actually use the funds.
Under the new law, beginning with FY 2014 (October 1, 2013), federal DSH funding will be reduced each year. The theory is that as more of the uninsured gain coverage, hospital uncompensated care costs will decline, with the rationale for offsetting DSH payments diminishing as well. While this theory is logical, in practice, state lawmakers are likely to confront political pressure from DSH payment–dependent hospitals seeking to maintain their revenues.
That is exactly what has happened in Massachusetts, which under its 2006 Medicaid waiver reallocated hospital DSH funding to pay for health insurance coverage subsidies for the low-income uninsured through the state’s new Commonwealth Care program. While about 175,000 uninsured Massachusetts residents gained coverage as a result, and while the cost of their coverage has not exceeded the total amount of the reallocated funding, the DSH funding–dependent hospitals in that state have successfully lobbied to preserve some of their funding stream at an added cost to state taxpayers. The hospitals’ justifications are that they still incur significant uncompensated costs—though they are obviously reticent about admitting how much of those costs are attributable to treating illegal aliens who do not qualify for Medicaid or other subsidized coverage—and that the extra funding helps offset the lower payment rates they receive from Medicaid.
Thus, under the new legislation, while states will theoretically spend less on their share of Medicaid DSH funding, political pressures may effectively negate any potential savings and, if state lawmakers are pressured into replacing reduced federal DSH funding with state funds, state costs may actually increase.
Payments to Specialty Physicians. While the provision in the new law that requires temporary Medicaid payment rate increases for primary care doctors will not apply to the rates paid for procedures performed by specialty physicians, the reality is that state lawmakers will likely find it politically difficult to limit Medicaid payment rate increases to primary care physicians. As with the increase in primary care payment rates, the political and financial significance of the issue of specialty physician payment rates will vary among the states according to their current Medicaid physician payment levels. The states that pay the lowest rates (relative to Medicare and private insurance) will face the greatest political pressure to also increase specialty physician rates and shoulder the largest added costs for such a move. Furthermore, this issue is likely to come to the forefront in the states’ 2012 legislative sessions, in anticipation of the scheduled January 1, 2013, federally mandated payment rate increase for primary care physicians.
Offsets to Costs. Other provisions of the federal legislation will generate some offsetting Medicaid savings for states, though for most states those savings are likely to be minimal. Only one change is likely to produce state savings of any significance, and only a few states stand to benefit from the applicable provision. One provision of the federal legislation is likely to generate savings between now and 2014 for taxpayers in some states by enabling their state governments to shift some of their current costs to taxpayers in other states. The new law allows states that have health insurance programs that are funded by state tax dollars and that already cover individuals who will qualify for Medicaid in 2014, to enroll those individuals in Medicaid immediately. The costs will be shared by the federal government at normal match rates until 2014 and at the expansion match rates thereafter.[12] Connecticut has become the first state to take advantage of this provision, shifting an estimated $53 million in state costs for Connecticut’s next fiscal year onto federal taxpayers in other states.[13]
Maintenance of Effort Requirement. The provisions of Obamacare that will have the most immediate effect on state budgets are the “maintenance of effort” (MOE) requirements in the law that are applied to Medicaid and CHIP. Under those provisions a state would lose all federal funding if it takes actions that make eligibility more restrictive than the standards in effect for the state’s program at the time the new federal legislation was enacted. In fact, states are already subject to a similar MOE requirement imposed as a condition of receiving a two-year temporary increase in federal Medicaid funding (through the end of 2010) as part of the 2009 stimulus legislation.
The bad news for states is that this federal mandate comes in the midst of their worst fiscal situation in decades. Because Medicaid is one of the largest items in any state budget, it is also one of the first places where governors and legislators look for savings when they need to trim spending to bring state budgets back into balance. In 2008, aggregate state Medicaid spending accounted for 20.7 percent of all state government expenditures, while spending on elementary and secondary education represented 21.6 percent, and the share of aggregate state spending devoted to transportation was 7.9 percent.[14]
Traditionally, states have three main tools for reducing Medicaid expenditures: restrict eligibility, cut provider reimbursements, or reduce benefits. The MOE requirements effectively mean that states no longer have the first option of limiting eligibility. However, they can still cut provider payments or scale back program benefits.
Partly as a result of the MOE requirement in the 2009 stimulus legislation, 41 states and the District of Columbia cut provider reimbursements rates in 2009 or 2010, and 29 states and the District did so in both years. Additionally, 39 states and the District cut Medicaid pharmacy benefits, and 22 states cut Medicaid medical benefits over the past two years.[15] All of these cuts are likely to continue if state budget projections do not significantly improve.
The problem is that in many states Medicaid reimbursement rates are already quite low. That makes Medicaid beneficiaries’ access to health care providers problematic, particularly in states such as New York, New Jersey, and California that pay providers exceptionally low rates. In addition, setting physician payment rates even lower will not necessarily reduce the aggregate costs of state Medicaid programs if the result is that more enrollees are forced to seek care in hospital emergency rooms because they cannot find doctors willing to accept Medicaid patients.
Even though the CHIP MOE prevents states from changing eligibility, CHIP enrollment will decline somewhat after 2014, resulting in some state savings. To qualify for CHIP, a child must be uninsured. However, many children will likely become insured through family coverage in subsidized plans offered by the new exchanges starting in 2014, for which a state contribution will no longer be required.
Washington’s New Insurance Market Rules
In addition to the Medicaid changes that will directly affect state budgets, state lawmakers will also need to contend with a variety of new federal health insurance market regulations. This federal usurpation of long-standing state authority in regulating private insurance will be expensive and disruptive for those who rely on individual or employer-based commercial insurance for their health care coverage. While the new law’s Medicaid provisions will present governors and state legislators with fiscal challenges, the insurance provisions will present them with policy challenges. The task for state lawmakers will be to find ways to protect their constituents from the adverse effects of the new federal health insurance regulations.
The new federal health insurance regulations will affect coverage in four major areas:
1) Benefit Requirements. The legislation gives the Department of Health and Human Services (HHS) new authority to establish minimum benefit requirements for all health insurance plans. The law requires that, effective for plan years starting this fall, health insurers and employer self-insured plans must cover preventive services with no enrollee cost-sharing. New prohibitions that prevent health insurance carriers and employers from setting annual or lifetime coverage limits will also be phased in starting this year and take full effect in 2014. Beginning in 2014, HHS is granted additional, sweeping, and discretionary authority to set, and periodically revise, minimum health insurance coverage requirements for virtually all medical services and health care providers. Furthermore, the Secretary of Health and Human Services is even given authority to regulate the amount and form of enrollee cost-sharing. The result will be a uniform, comprehensive health insurance minimum benefit package dictated by HHS.
For individuals and employers, the result of these new federal regulations will be across-the-board increases in health insurance costs and premiums. Those resulting premium increases will be the product of three factors. First, reductions in enrollee cost-sharing will mean that plans must pay more of the cost for certain services that they already cover, thus shifting those costs from patients to plan premiums. Second, the elimination of enrollee cost-sharing for specific services will stimulate greater use of those services, further increasing premiums. Third, premiums will also increase to the extent that new federal regulations require plans to cover benefits or services that were previously excluded from coverage or subject to plan limitations on the scope or duration of the services eligible for reimbursement. These additional costs will likely exceed any possible savings from lower administrative costs for insurers.
As state lawmakers are well aware from their own experience with insurance benefit mandates at the state level, providers and patient groups can be expected to exert special interest pressure on HHS and Congress to constantly expand the scope of the federal minimum coverage requirements. To the extent that HHS or Congress bows to that political pressure, the cost of health insurance will escalate still further after 2014.
2) Coverage Rules. The federal legislation also establishes some new coverage rules. Effective this fall, insurers and employers must allow young adults to retain dependent coverage on a parent’s policy until age 26, and plans are prohibited from imposing pre-existing condition exclusions on dependent children. However, the effects of those two changes are expected to be modest, as they will apply to relatively few individuals.[16]
Much more significant is that, starting in 2014, Obamacare will prohibit the application of pre-existing condition exclusions under any circumstances.
Current law specifies that individuals who already have employer-sponsored insurance cannot be denied new coverage, be subjected to pre-existing condition exclusions, or be charged higher premiums because of their health status when switching to different coverage.[17] Thus, in the employment-based health insurance market, pre-existing condition exclusions may only be applied to those without prior coverage, or to those who wait until they need medical care to enroll in their employer’s plan. These existing rules represent a fair and balanced approach: Those who do the right thing (getting and keeping coverage) are rewarded; those who do the wrong thing (waiting until they are sick to buy coverage) are penalized. A modest and sensible reform would be to simply apply the same set of rules to the individual health insurance market.
But by prohibiting the application of pre-existing condition exclusions under any circumstances, the new law mindlessly wrecks this careful balance and creates a recipe for disaster.
Since heath plans will also be required to extend coverage to any qualified applicant, and will not be allowed to vary premiums based on individual health status, the effect will be to encourage healthier individuals to wait until they are sick before they buy health insurance. With fewer healthy individuals buying coverage, premiums will need to rise to cover the costs of the sick, which in turn will drive even more individuals in good, or even fair, health to drop coverage—knowing that if they become sick they can buy insurance later—thus driving premiums yet higher. The result could be a classic insurance plan “death spiral.”
Rather than ditching this bad idea in favor of a more sensible and balanced approach, congressional leaders tried to limit its inevitable disastrous effects by adding an individual mandate to buy health insurance or pay an income tax fine. A large part of the rationale offered for the mandate was the need to prevent healthier individuals from dropping their coverage.
Setting aside the merits of challenges to the individual mandate’s constitutionality, the practical reality is that the mandate will be ineffective and unenforceable due to the way Congress wrote the specific provisions. For most individuals, the tax penalty for not buying coverage will be modest. More important, in response to strong and widespread public opposition to the mandate, Congress added provisions that explicitly bar the IRS from using its normal tax enforcement powers of property liens and criminal penalties to collect the fines imposed on individuals who do not comply. Thus, when faced with escalating health insurance premiums, individuals who do not want to pay for coverage not only can ignore the mandate, but, by making minor changes in their federal income tax withholding payments, can also avoid paying most, or even all, of the penalties for noncompliance.
Because the blanket prohibition of pre-existing condition exclusions and the individual mandate provisions do not take effect until 2014, there is still time for a future Congress to prevent a health insurance market destabilization by repealing this disastrous legislation. At that point Congress can then consider making more sensible changes. However, until Congress acts, state policymakers face the looming threat of a health insurance market meltdown.
3) Rate Regulations. In addition to the indirect effects on insurance premiums of new federal benefit mandates and coverage rules, health insurance premiums will also be directly affected by new federal rate regulation provisions. The largest effect will come from a provision that limits age-rating of premiums to a ratio of no more than three to one. This provision will take effect in 2014 and means that plans will not be allowed to charge a 64-year-old more than three times the premium charged an 18-year-old for the same coverage. In contrast, the natural variation in coverage cost is about five to one— meaning that the oldest group of (non-Medicare) individuals normally consumes about five times as much medical care as the youngest group.
This mandated “compression” in the age-rating of coverage means that insurers must charge older individuals premiums that are less than the actuarial value of their coverage, with the result that insurers will need to compensate by charging younger individuals premiums that are higher than the actuarial value of their coverage. Thus, this federally mandated under-pricing of coverage for older individuals will further increase premiums for the young— who, because of their generally good health status and lower earnings, are the group that is most sensitive to changes in the price of coverage and most likely to decline coverage.
Obamacare also creates new federal rules— “minimum loss ratio” regulations—for how insurers spend premium dollars. Starting in 2011, plans must spend a minimum amount of premium income on medical care and “activities that improve health care quality,” or refund the difference to policyholders. The minimum levels will be 85 percent for large group plans and 80 percent for small group and individual plans. In addition, HHS is given new power to conduct annual reviews “of unreasonable increases in premiums for health insurance coverage.”[18]
4) Imposing New Federal Schemes. Moreover, Congress included four new health care coverage schemes that further compound the problems of the legislation:
a) Temporary Federal High-Risk Pools. The law instructs HHS to establish temporary federal high-risk pools starting in 2010 to cover uninsured individuals between now and 2014, with $5 billion authorized for the program.[19] State governments are invited to contract with HHS as vendors to administer the new federal high-risk pools in their states, but are prevented from shifting into them individuals currently enrolled in other coverage, including those covered by existing state high-risk pools. The CMS Office of the Actuary projects that the available funding for the program will be exhausted by 2012.[20] That will force HHS either to set enrollment limits for the program at the outset or to subsequently terminate coverage for enrollees, unless the next Congress authorizes additional funding.
b) Health Insurance Exchanges. The legislation requires HHS to establish operational health insurance exchanges in every state by 2014. Again, states are invited to act as vendors to administer a federal program according to a detailed set of federal rules and regulations, but are not allowed to exercise any meaningful discretion in administering the exchanges. The main purpose of the exchanges will not be to give consumers greater choice of coverage, since the coverage offered through them will be a limited number of standardized plans. Rather, their principal purpose will be to administer a new set of federal health insurance subsidies for those with incomes up to four times the federal poverty level, and to regulate the coverage purchased with those subsidies. The exchanges are also empowered to enroll anyone in Medicaid they determine eligible for the program, with states forced to share the resulting costs but prohibited from conducting their own eligibility determinations or verifying the accuracy of the eligibility determinations made by the exchanges.
Large employers will be fined if their workers receive subsidized coverage through an exchange, but firms with 50 or fewer employees are exempted from those fines. The likely result is that many small employers who currently offer coverage will dump their plans beginning in 2014, since their workers will then qualify for either Medicaid or the new subsidies. Even large employers are likely to dump their plans if most of their workers qualify for subsidized alternative coverage and the savings to the employer are greater than the fines for not offering coverage.
c) New National Health Insurance Plans. The new law instructs the federal government’s Office of Personnel Management (OPM), which administers the Federal Employees Health Benefits Program (FEHBP), to contract with health insurers “to offer at least 2 multi-State qualified health plans through each Exchange in each State,” and further stipulates that at least one of the contracts is to be with a non-profit insurer.[21] Of particular concern to state officials is that from the way Congress wrote these provisions the extent to which state insurance regulators will be able to require the OPM-sponsored plans to meet state insurer financial regulations, and thus ensure that the plans remain solvent, is unclear.
d) New CO-OP Plans. The legislation also instructs HHS to promote the creation in each state of at least one non-profit, member-controlled, “consumer-operated and oriented plan” (CO-OP) health insurer. Both the CO-OP provisions and the provisions instructing OPM to sponsor “multi-state” plans were added as part of efforts by Senate Democratic leaders to bridge the sharp division within their caucus over whether the legislation should include a new government-run health insurer—the so-called public option. Thus, both sets of provisions are primarily political in nature and, from a policy perspective, poorly designed and drafted.
The bad news for state officials is that Congress appropriated $6 billion for loans and grants to establish CO-OPs and instructed the Secretary of Health and Human Services to keep promoting the program until every state has one. The good news is that CO-OPs—unlike OPM-sponsored multi-state plans—are explicitly required by the legislation to comply with state insurance laws and regulations. As a practical matter, it is uncertain whether any CO-OP insurers will actually be created, as there is no obvious market demand. The statute imposes several restrictions that make it difficult to establish and operate one, and the legislation expressly prohibits the most likely and sensible path to setting one up, namely, a divestiture or conversion by an existing health insurer.
How State Officials Should Respond
Obamacare creates significant fiscal and policy challenges for states. The broad effects of the legislation, if implemented as enacted, will be to impose significant new Medicaid costs on state taxpayers, disrupt state health insurance markets and the current coverage of tens of millions of Americans, and usurp state authority. The new federal insurance regulations, particularly the provisions setting new, uniform federal benefit requirements, will reduce coverage options for individuals and employers and will likely drive up health insurance premiums. They are also likely to result in greater concentration in health insurance markets, leaving only a few large insurers operating as public utilities with a regulated low rate of return selling undifferentiated products to customers with no other options.
Maryland’s experience is instructive in this regard. In 1993, the state of Maryland imposed on its small-group health insurance market a minimum package of standardized benefits, annually updated by a state commission—a design similar to that in the new federal law. One result was that competition has declined to the point where the same two carriers have now covered more than 90 percent of all individuals in Maryland’s small-group market for years.
State lawmakers now face the task of finding ways to protect their constituents—including state taxpayers, health insurance policyholders, and individuals who depend on public health care programs—from the adverse effects of Obamacare. Governors and state legislators need to start planning their responses now and begin drafting any applicable legislation for consideration in their next legislative session. The wisest approach is to move reform measures that better position their states under either of two possible scenarios: a new Congress that repeals Obamacare, or a protracted, multi-year political and legal battle conducted against the backdrop of an Administration attempting to implement the legislation as enacted. Specifically, state lawmakers should immediately and aggressively pursue the following strategies:
- Shift non-elderly Medicaid and CHIP enrollees into premium support.
The combination of recession-induced lower state tax revenues and the new law’s Medicaid MOE requirements puts state lawmakers in a fiscal bind. Because the MOE requirements prevent them from controlling Medicaid spending by reducing eligibility, many state lawmakers assume that their only options are to cut provider reimbursements or further limit program benefits.
However, there is another—and better—option that states should pursue. The most effective tool for states to control their Medicaid and CHIP spending is to shift their programs from directly paying providers to subsidizing private coverage for enrollees. Not only will this “premium support” approach help states control spending; in many states it will also increase beneficiary access to physicians.[22]
States should immediately begin designing and implementing Medicaid and CHIP premium support initiatives for non-institutionalized beneficiaries. In doing so they should take advantage of the flexibility remaining in federal law by adopting all “benchmark plan” designs, providing for maximum allowable enrollee cost-sharing, and replacing the individual cost-effectiveness test with an average cost-effectiveness test. States should also pursue contracting with one or more private insurers to create supplemental policies that cover required “wrap-around” benefits for Medicaid beneficiaries enrolled thorough premium support in less comprehensive private plans. Then the state can simply pay the premiums for those supplemental policies as well.
The advantages of premium support for enrollees are that they will likely get better access to physicians and more appropriate medical care. In addition, subsidized private coverage is free of the “welfare stigma” associated with traditional Medicaid, or even Medicaid managed-care plans, since providers will only see the private coverage—not the subsidies behind it.
Premium support will also help expand and strengthen a state’s private insurance market—particularly its small-employer coverage market—by adding a large number of mainly healthy and younger individuals to the market.
From a state budget perspective, cost savings from premium support are likely to come in four forms: (1) savings from increased enrollee cost-sharing, (2) efficiency savings from covering under a single policy all members of a family currently covered separately by different combinations of public or private plans, (3) administrative savings achieved by significantly reducing the need for the state’s Medicaid and CHIP programs to operate systems that directly reimburse providers and verify claims, and (4) likely the biggest source of savings will come from more appropriate use of medical care. While private plans pay doctors higher rates, if Medicare and CHIP beneficiaries with premium support get earlier and more coordinated physician care, their historic practice of over-using expensive hospital emergency room services should decline—thus, offsetting the increased spending on physician care while also addressing the problem of emergency room over-crowding.
Finally, states should craft their “premium support” initiatives as state-plan amendments to their programs, rather than submitting waiver requests to HHS. Unlike the waiver process, over which the Secretary of Health and Human Services is granted broad discretionary authority, Medicaid and CHIP state plan amendments can only be disallowed if the Secretary finds that they would violate statutory federal requirements for how states operate their programs.
Furthermore, unlike with waiver determinations, a state has legal recourse to appeal an adverse determination by HHS about a state plan amendment in federal court. Although states have lost some flexibility in using premium assistance under both the CHIP reauthorization legislation and the Obama Administration’s newly issued regulations on benchmark plans and cost sharing, premium support is still a worthwhile strategy for states to pursue.
- Refuse to administer the new federal high-risk pools.
To date, 18 governors have wisely refused to let their state governments administer the new federal high-risk pool.[23] There are sound reasons for their decisions, as the new high-risk pools are poorly designed.
Any U.S. citizen or lawful resident with a pre-existing medical condition who has been uninsured for at least six months will be eligible for coverage. Congress gave the Secretary of Health and Human Services complete discretion in determining which pre-existing medical conditions will qualify—no matter how minor. Thus, unless the Secretary decides to limit eligibility only to those individuals with expensive conditions, it is certain that demand will quickly outstrip the available funding.
Furthermore, the law stipulates that an enrollee in a new high-risk pool cannot be charged a premium higher than the applicable standard rate for the same coverage in the general market. In contrast, all of the 34 states with existing state high-risk pools follow the long-standing guidance of the National Association of Insurance Commissioners (NAIC) to charge high-risk pool enrollees premiums that are at least 125 percent of standard rates.[24] Specifying that premiums charged to enrollees in the new pools not exceed standard rates means that, relative to existing state high-risk pools, the new pools will provide more generous subsidies (at a higher cost) and will likely attract many more applicants, particularly individuals with relatively minor pre-existing medical conditions.
Finally, another major concern with state governments administering the program is that when the federal funding runs out, state lawmakers will be faced with either terminating the coverage of enrollees or continuing to fund the program with state tax dollars. From the perspective of state officials, they are better off letting the Department of Health and Human Services administer the program, either directly or through private-sector contractors. That way, federal officials will be the ones who are unambiguously responsible for any adverse funding or enrollment decisions.
- Decline federal “premium review” grants.
The provisions instructing the Department of Health and Human Services to conduct health insurance premium reviews also authorizes HHS to distribute up to $250 million in grants to states to assist HHS in implementing those provisions. In exchange, however, state insurance departments must provide HHS with insurer data and collaborate with HHS in administering rate regulations. To preserve the integrity and independence of their own insurance departments and insurance laws, state officials would be well advised to decline this offer of federal funding. The rate review provisions are not only poorly drafted, but were politically motivated additions to the legislation. Statements by Administration officials since the enactment indicate that implementation of the provisions by the Obama Administration is likely to also be driven more by political considerations than by sound policy or genuine consumer protection.
For example, both the statute and subsequent comments by Administration officials refer to “unreasonable premium increases.” What is missing is any recognition that another key aspect of proper insurance regulation is to prevent the problems that occur if insurers under-price their products. If an insurer fails to charge enough in premiums to cover its expected claims costs, then it is at risk of being unable to make good on the promises made to its customers. As any state insurance regulator understands, ensuring that carriers have sufficient premium income to cover future claims costs is an important consumer protection.
Also missing from the new federal law is any recognition of the equity issues involved in setting rules for insurers that cross-subsidize different lines of coverage. For example, is it “fair” if regulators require an insurer to limit premium increases on its individual market policies, but as a result the carrier then has to further increase rates for group policies to make up the difference, or vice-versa? Of course, there is no single “correct” set of answers to these kinds of questions, but state lawmakers and state insurance regulators at least have the benefit of decades of experience addressing such issues, while the federal government has none whatsoever.
To be sure, insurance companies (including non-profit ones) are not altruistic enterprises, and state insurance regulation is no more immune to political considerations than is federal regulation. However, given the demonstrated propensity of congressional leaders and Obama Administration officials to blame insurers for the adverse consequences of their own legislation, the vast disparity between the state and federal governments in experience and expertise in insurance regulation, and the inherent conflicts that will arise between the new federal rate regulations and existing state insurer solvency regulations, it is important that state lawmakers preserve the independence of their own insurance laws and state insurance departments. That means states should not accept federal funding with strings attached that compromise their independence or make their insurance departments mere branch offices of HHS.
- Implement state health insurance market reforms and exchanges based on state, not federal, designs.
Obamacare will drive up health insurance costs with new coverage mandates while simultaneously trying to hold down premiums with politicized rate regulation. The federal standardization of coverage will also limit the ability of insurers to differentiate themselves in the market or offer their customers lower-cost benefit designs, while the minimum loss ratio regulations will reduce incentives for insurers to be more efficient in managing or paying for care—as insurers will be able to retain little, if any, of the savings that might result.
Faced with this impending regulatory “squeeze play,” insurers are already evaluating their options and can be expected to act in some predictable ways: Insurers with other lines of business (such as property or life insurance) will likely discontinue or sell their health insurance book of business to a competitor and exit the market. Carriers that offer only health coverage will look to mergers and acquisitions as the path to becoming “too big to fail.” Their logic will be that if the federal government is going to turn private health insurance into a regulated utility with a low rate of return, then the way to survive is to be one of the remaining few large insurers that the federal government needs to keep in business in order to administer the system.
Thus, absent initiatives by state governments to counter these effects by expanding choice and competition, state health insurance markets will begin to see fewer carriers and plan options—most likely starting next year.
The best response for state lawmakers is to immediately move in the opposite direction of the new federal legislation by first determining their state’s needs and priorities, and then enacting their own reforms that increase health insurance choice, competition, and coverage while also reducing costs. Lawmakers in each state can select from the following broad strategies the elements that offer the best approach for addressing their state’s particular needs and circumstances: (1) increase consumer choice by creating a “defined contribution” option for employer-sponsored health insurance coverage, (2) reduce coverage costs and allow more variety in plan design by repealing unnecessary state-mandated health insurance benefit requirements, (3) encourage insurer participation by lowering barriers to market entry through statewide risk adjustment mechanisms collectively designed and administered by the carriers selling health insurance in the state, (4) expand coverage options by creating a “premium aggregation” mechanism that enables individuals to buy coverage using contributions from multiple employers (such as when a family has two earners or an individual has two part-time jobs), and, in the case of low-income families, Medicaid or CHIP premium support payments from the state, and (5) provide consumers with greater price and quality transparency with respect to insurance coverage and physician and hospital services.[25]
The fact that the federal legislation perverts the intent of a health insurance exchange—replacing its original purpose as a state tool for increasing consumer choice and encouraging greater variety and competition in health insurance with the new purpose of administering federal coverage uniformity, and supplanting state insurance regulators—should not dissuade state lawmakers from pursuing their own designs for exchanges (consistent with the original intent of the concept) or other administrative mechanisms as tools for implementing their own reforms to promote consumer choice and enhanced health plan competition.
For example, Utah officials and stakeholders determined in their assessment process that their state’s small businesses coverage offer rate was well below the national average and that Utah has a significant number of workers with two or more part-time jobs who do not qualify for employer group coverage offered to full-time employees. Thus, they decided to make defined contribution and premium aggregation using a state health insurance exchange key elements of Utah’s reform strategy. They also devised an implementation strategy that relies on existing private vendors to provide the necessary administrative services at a negligible cost to the state’s budget.[26] Other states can also use private vendors to quickly design and implement similar solutions customized to their own particular needs and circumstances.
By enacting their own insurance market reforms and creating their own exchanges, or similar administrative mechanisms, based on their own designs now, states can make it politically more difficult for federal officials to implement provisions of the new federal legislation (such as minimum federal benefit standards) that will drive up premiums and reduce coverage choices. State-designed exchanges can also serve as the administrative platform for implementing Medicaid and CHIP premium support initiatives and, if the legislation is not repealed by then, for organizing alternative coverage arrangements for individuals and employers who refuse to comply with the new federal mandates that also take effect in 2014.
- Insist that federal officials explain publicly how they will administer Obamacare.
State legislators should convene public hearings and summon the federal Secretary of Health and Human Services, members of their state’s congressional delegation, and other federal officials to explain how they intend to implement the numerous provisions of the legislation that will affect their state’s Medicaid and CHIP programs and the private health insurance plans of individuals and employers. Obviously, state lawmakers cannot override the federal regulatory process, but they can force more of it out into the open and subject it to heightened public scrutiny. They can put federal officials on notice that if they assert their new authority, then states will force them to accept responsibility for the results—and that state lawmakers will ensure that their constituents know who is to blame when state revenues have to be diverted from other priorities to fund expanded health care coverage, or individuals see their health insurance premiums increase or their employer drop their coverage. If federal officials refuse to testify before state legislatures, their refusals will themselves be public testimony.
- Conduct and publicize “benchmark” analyses.
States should immediately conduct “benchmark” analyses to provide “baseline” projections for at least the next five years for key metrics, and then use the results to measure the effects of various provisions of Obamacare. The results can also serve as a baseline for estimating the effects of any alternative state reform proposals. Key metrics include:
- Projected annual enrollment and per capita spending for Medicaid and CHIP, by eligibility category under current law;
- Projected growth in average premiums in the state’s individual, small, and large group health insurance markets under current law;
- Projected average premiums by age in the state’s individual and small group markets under current law; and
- Current and projected health insurance coverage status of the state’s residents by source of coverage under current law.
The utility and integrity of the results will be greatly enhanced if state lawmakers ensure that the process for conducting these benchmark analyses is open and nonpolitical, and that the resulting reports clearly explain the methodologies and assumptions used. Where appropriate, the analyses should also provide upper-bound and lower-bound estimates to account for the inherent uncertainty of key assumptions, such as underlying medical cost growth rates or changes in the states’ resident populations. States can contract with recognized actuarial and econometric consulting firms to conduct these studies.
Developing a state-specific baseline is the essential precursor to constructing state-specific estimates of the effects of the new federal law. State officials will want to construct their own estimates because, if for no other reason, national level estimates will not be sufficiently precise for state planning purposes. Variations among the states in the composition of their populations, economies, health systems, public programs and insurance rules mean that, in any given state, the actual effects of a particular provision of the new law may differ significantly from the projected national effects estimated by federal officials. Indeed, significant disparities in the effects among states are likely to arise with respect to even minor provisions of the new law.
Case in point: The requirement to extend dependent coverage to age 26 is a minor provision that is projected to have modest effects on cost and coverage at the national level. However, the most recent Census data show that while 18- to 24-year-olds (the Census age breakout that most closely aligns with the group affected by the provision) account for 9.79 percent of the U.S. population, that age group as a share of resident population in the states varies from a low of 8.17 percent in Nevada to a high of 12.88 percent in North Dakota. Thus, among the states there is a 57 percent variation between the two with the lowest and highest shares of young adults in their populations. That demographic difference alone will be a key variable in explaining any variation between those two states in the cost and coverage effects of just this one, relatively minor, provision.
With their own, state-specific benchmark analyses in place, states will be able to more precisely estimate the effects of the new federal law and state lawmakers will be able to demonstrate to their constituents what portion of a particular result—such as an increase in insurance premiums—is attributable to the federal health care legislation and what portion is attributable to other factors.
Conclusion
The enactment of the massive Patient Protection and Affordable Care Act will not only alter the relationship between individuals and the federal government, it will also alter the relationship between the federal government and the states. Under the terms and conditions of the act, the states would be reduced to mere agencies of federal authority, carrying out the policy agenda of the Secretary of the U.S. Department of Health and Human Services.
Some of the relevant provisions of this law that directly affect the states will not go into effect for four years, and by that time, the law may be substantially, changed, amended, or repealed.
In the meantime, state officials should recognize one simple fact: States are not mere agents of federal authority. They are not powerless. There is absolutely nothing that requires them to assist in implementing this misguided legislation. Rather, they should take every opportunity to assert their rightful authority, resist, within the confines of the law and the Constitution, any inappropriate or unconstitutional exercise of Washington’s power and aggressively advance their own, better solutions. In other words, they have a duty to represent their citizens.
—Edmund F. Haislmaier is Senior Research Fellow and Brian C. Blase is Policy Analyst in the Center for Health Policy Studies at The Heritage Foundation.
Appendix Methodology
Table 1. Projected Medicaid/CHIP Enrollment, by State in 2014. National enrollment estimates by the CMS Office of the Actuary were distributed among the states according to each state’s share of total Medicaid/CHIP enrollment in June 2009 (for current eligibility) and according to each state’s share of the total uninsured population in 2007–2008 below 133 percent of FPL (for the eligibility expansion) based on Medicaid/CHIP enrollment data and census data as reported on http://www.Statehealthfacts.org.
Table 2. Estimated State Costs for Medicaid Expansion, by State, Cumulative for FY 2014– 2020. National enrollment and federal spending estimates by the CMS Office of the Actuary were used to derive the average federal cost per enrollee, per year, which were then distributed among the states according to each state’s share of the total uninsured population in 2007–2008 below 133 percent of FPL. State costs were then calculated off the federal cost estimates using the applicable match rates for each state as adjusted by the provisions of the legislation. The added administrative cost load was calculated by applying current ratios for total administrative costs as a percent of total benefit spending and then apportioning those costs between the federal and state governments based on historical data that indicate an average effective Federal Medical Assistance Percentage (FMAP) of 55 percent for all administrative costs.
Table 3. Estimated State Costs for Medicaid “Doc Fix,” by State. The federal cost of the mandated increase in primary care physician (PCP) rates in FY 2014 (when it is entirely paid for by the federal government) are estimated at $3 billion (CBO) to $5.5 billion (CMS). Continuing that policy in 2015 and thereafter would require states to assume their shares of the total cost of the payment rate increase. The cost to an individual state will vary based on three factors: the state’s aggregate spending on PCP services; the ratio of the state’s current Medicaid PCP payment rates relative to Medicare rates; and the state’s FMAP.
Projected state costs were constructed as follows: (1) A weighting for each state’s share of total (federal and state) national Medicaid spending on all physician services was calculated. (2) Each state’s share of physician spending was then divided by the state’s Medicaid-to-Medicare reimbursement ratio to obtain a state burden index, after first removing from the equation states that already have Medicaid PCP reimbursement rates that are equal to or greater than Medicare rates. (3) The initial state burden index was then re-weighted so that all the weights of the affected states summed to one. (4) The re-weighted state burden index was then applied to the CBO and CMS federal cost estimates to distribute the total federal costs among the affected states. (5) Finally, state costs were estimated by multiplying each state’s share of the federal funding by one minus the state’s applicable FMAP.
When summed, the projected aggregate state costs are about $1.3 billion (using CBO estimates) and $2.3 billion (using CMS estimates), or approximately 43 percent of the total cost. That ratio is consistent with the national distribution between federal and state governments of total Medicaid spending.



