Abstract: In 2006, the Dutch government implemented a universal insurance mandate. Many American policymakers are looking to the Dutch experiment as a model to fix America’s complex and costly health care system. But the Dutch reforms have not caused individual consumers to seek value, and the “managed competition” has led to a less competitive market. After just two years, the Dutch insurance market was a clear-cut oligopoly. Given the narrow, partisan enactment of President Obama’s health policy agenda, America appears to be on a similar path. Two health policy analysts, including one from Holland, explain why patients in the Netherlands do not have a significant choice among health insurance companies, nor can they access sufficient information about the health system and different options—and why this system would not benefit patients in America, either.
President Barack Obama recently signed two major pieces of legislation that will engineer a massive overhaul of the health care sector of the American economy: The Patient Protection and Affordable Care Act and the Health Care and Education Reconciliation Act of 2010.[1]
Management of Competition. Together, these acts authorize the federal government to impose unprecedented mandates on individuals and employers; expand eligibility for Medicaid, the joint federal–state health program for the poor and the indigent; create a new system of taxpayer subsidies for individuals and businesses to expand health coverage; and undertake major changes in Medicare payment policy.
In terms of health insurance, however, the most significant changes are embodied in provisions for the federal definition, control, and standardization of health care benefits and the transfer of regulatory authority over health insurance from the states to the federal government. Beginning on January 1, 2014, states will be required to establish and maintain congressionally designed health insurance exchanges under the supervision and regulatory control of the U.S. Department of Health and Human Services (HHS). Under federal regulatory control, the new health insurance exchanges will be the vehicle for individuals, families, and small employers to purchase federally approved health insurance plans. These exchanges will also provide an arena for two or more government-sponsored health plans, administered by the Office of Personnel Management (OPM) to compete against private health insurance, potentially in every state of the union.[2] These provisions could very well accelerate the already unhealthy consolidation of health insurance markets, rather than open them up to more robust competition.
The new regulatory regime is highly prescriptive. The Secretary of HHS will promulgate rules for the states’ “open season” for enrollment in these new health insurance exchanges, and the presentation of plan information and even state Web site operations will be carried out under federal guidance. The Secretary will also be charged with enforcing federal insurance rules (such as guaranteed issue or prohibition of pre-existing condition exclusions) in every state market. Meanwhile, states will be required to establish one or more health insurance rating areas, subject to review by the Secretary, who will decide what are, and what are not, “permissible age bands” for the purpose of health insurance rating.[3]
While the new health care law embodies, however imperfectly, the President’s health policy agenda and conventional liberal health policy prescriptions, it also represents the political progress of “managed competition” theory in health insurance market reform. According to this theory, the government will not only enforce a common set of market rules, including rating rules, but the government must also standardize health insurance benefits, limiting variation in health benefits or benefit offerings. Competition among health plans will thus be confined to competition based on quality and price. Theoretically, at least, universal coverage is to be secured through an individual mandate to purchase the government’s standardized coverage.
The Dutch Example. America’s existing health care system is complex and costly; patients cope with limited choice and an inequitable division of charges. American reformers of all political persuasions have been preoccupied with the problem of how to promote major expansions in coverage while containing rising health care costs and improving patient outcomes. American policymakers have been looking abroad for cues on how to improve American health care financing and delivery. The health insurance experiment in the Netherlands has often been described as a success story, and a model that can teach American reformers how to create a better system.
In 2006, the Dutch government implemented a universal insurance mandate with emphasis on controlling macro health care costs. The theory was that rather than regulate the supply of health care, the government would stimulate competition. In order to achieve this, the Dutch devised a system of “managed competition” that included a statutory general insurance provision. Dutch citizens are now obligated to buy a basic insurance package, as defined by the government, and insurers have a duty of acceptance.
Many American policymakers, such as Senators Ron Wyden (D–OR) and Robert Bennett (R–UT), see the Dutch experiment as a superior model compared to the single-payer system adopted in Canada and Great Britain. Ideally, a competitive market in the provision of health care will bring about greater efficiency and increased focus on demand; it will also stimulate entrepreneurship, flexibility, and innovation. Introduced to the United States, a reformed insurance system based on government-regulated competition could theoretically assure freedom of choice and equal access to a minimum quality of health care for all Americans.
When examined in more detail, however, it becomes clear that facts and theory have not coincided in the Dutch system. Specifically, the reforms have not caused individual consumers to seek value—the market rate at which price aligns with quality. Perversely, quite the opposite has occurred, as the attempt to manage market conditions has reduced competition. Cost-consciousness remains elusive, and managed competition has led to an oligopolistic insurance market bereft of meaningful choice.
The Dutch System: The Rationale
Prior to reform, the Dutch health care system was characterized by strong government regulation and an inefficient dual insurance system of public and private insurance.
The provision and funding of long-term care and uninsurable risks—such as care for the elderly or for people with chronic physical or mental disabilities—was largely regulated by the Algemene Wet Bijzondere Ziektekosten (AWBZ), or “Exceptional Medical Expenses Act.” The AWBZ was and continues to be applicable to all Dutch citizens. This “first compartment care” emphasizes support in the case of and compensation for irreversible limitations; “second compartment care” focuses on recovery and includes hospital care and visits to a primary care physician. The Dutch also identify “third compartment care,” which is defined as “luxury care,” such as dental procedures and optional physiotherapy.
Before 2006, the provision and funding of insurance for second and third compartment care were determined by an individual’s total income. In 2005, the wage ceiling was set at a gross annual income of €33,000 ($40,600) for employees and €21,050 ($25,900) for the self-employed.[4] Those people earning less were determined eligible for the public system. Those who did not qualify for the public system could purchase private insurance to cover potential short-term medical needs in the second compartment and—in some cases—also for “luxury care” in the third compartment. By 2005, roughly two-thirds of the Dutch population had entered the public program, known as the “sickness funds,” so there was a need for strong cost control.
This dual system led to many problems and did not adequately respond to patients’ needs, in large part because it did not focus on demand.
First, there were long waiting lists, since health care providers were forced to implement strict budget control and had only limited means by which to provide care. Government budget and price controls caused enormous inefficiencies in the provision of health care. Health care providers simply filled their budgets; they were not stimulated to develop flexibility, innovation, and entrepreneurship.
Second, there was little or no freedom of choice for patients. Patients in the sickness funds had no choice of health care providers. In the private scheme, insurers had no duty of acceptance, so patients in high-risk groups—such as those suffering from chronic diseases—had limited choices among insurers.
Third, there was little or no information available on the quality of health care delivery. This last problem continues to plague the Dutch system.
During the 1980s, a period of rising unemployment and limited economic growth in the Netherlands, it became clear that strong regulation of the health care sector had gradually thwarted the relationships among care providers, insurers, and patients. A general consensus emerged that government steering of health care supply should make room for a competitive and transparent market driven by demand. The discussion led to two main proposals of reform: reorganization of health care provision and adjustment of the outdated insurance system.
The Dutch System: How it Works
According to the Dutch government, a new division of tasks and responsibilities in the health care sector was essential “to guarantee good and affordable care for everyone in the future.”[5] In theory, this new separation amounts to fewer rules imposed by national government, stronger purchasing power by consumers, and greater room for insurers and health providers to negotiate.[6]
In order to achieve all this, the Dutch government implemented a general insurance provision for second-compartment care. This compulsory insurance now covers all but approximately 1 percent of the Dutch population.[7] In addition, 92 percent of the Dutch[8] purchased additional insurance in 2008 for third-compartment or supplemental care: all health care that is not covered by the basic package, such as dental care, eye care, “alternative” doctors, and additional physiotherapy.
The Individual Mandate. One major feature of the Dutch reform is that every person living or working legally in the Netherlands must purchase health insurance. Exceptions are made for children under the age of 18, who are automatically covered, and new residents, who are granted a four-month grace period to obtain insurance.[9]
Premium payments must be kept current in order for a Dutch resident to switch insurance plans during the annual open season. Residents with accounts more than six months in arrears are taxed by the government, which uses the money to compensate the insurer for the lapsed payments.[10]
The 1 percent uninsured presently face fines equivalent to outstanding premiums of up to five years plus a 30 percent penalty, though enforcement has been lax.[11] New methods designed to root out the remaining pockets of noncompliance are scheduled to go into effect this year.[12]
The General Insurance Provision. According to the Dutch government, “a general health care insurance provision founded in public law but implemented by private players—including players with a profit motive—is the most appropriate way to ensure that the various public interests involved in the health care sector are safeguarded.”[13]
In the Dutch system, the government mandates the basic benefit package that all residents must receive. The fundamental principle in determining the scope and the quality of the package that the general insurance provision covers is “essential health care”: care of so-called “proven effectiveness.” This includes visits to the primary care physician, hospital stays, pharmaceuticals, and psychiatric care. Holland’s National Health Insurance Board determines the basic level of coverage required by all insurance companies, but it does not prescribe the precise methods of health care delivery, particularly in terms of primary care. In the Dutch system, primary care providers include not only physicians and nurses, but also dentists and midwives.[14]
Insured people are free to choose their preferred health care provider among those contracted by an insurance company. Insurance companies can force health providers to provide better quality for lower costs by threatening not to contract them. For most health providers it is essential to contract with health insurance companies because they represent large groups of patients. The more insurance companies merge, the more difficult it becomes for providers to operate without contracts.
Nonetheless, some providers have spurned the arrangement by practicing without contracts. Patients who insist on seeing out-of-network providers must pay for the costs themselves, though most insurance companies will reduce these costs as part of an additional insurance package. This way, patients pay a higher premium in exchange for broader options among care providers. At the same time, patients may choose to decrease their premium price and increase personal responsibility by allowing for more out-of-pocket expenses.
All insurance companies have a duty of acceptance so there can be no risk selection. To ensure equal access there is a system of risk equalization between insurers. All of the insured pay a nominal premium for the “basic” package, which is in fact substantial by American standards. Insurers compete on price, delivery quality, and benefits included in additional packages. In fact, coverage of additional insurance appears to be the primary reason that patients switch insurers.[15] It is during the annual six-week open season that people can choose the health care insurer with which they want to register.[16]
Drawbacks to the insurance provisions and other aspects of the Dutch system are discussed later in this paper.
Group Insurance. In the Netherlands, there is no employer mandate to provide health insurance, nor must an employee choose among the health insurance plans made available by the employer. Though many employers do sponsor insurance, individuals can and do obtain group coverage outside of work. Any type of group can form in order to purchase insurance at the discounted group rate of up to 10 percent, and it is not uncommon for social organizations to offer health insurance. In fact, 59.2 percent of the Dutch population was part of a group insurance in 2008.[17] This means that affordable group insurance coverage is not confined to employer-sponsored health plans, which are the exclusive beneficiaries of favorable tax and regulatory policy in the United States.
Financing. Because the first insurance compartment is still uniformly covered under the terms of the AWBZ, the differences in the current system arise from the fragmented financing structure in the second compartment.
The Dutch government tries to permanently compensate for negative income consequences by means of the tax system. If an individual is 18 or older, single, and earns less than €32,502 ($40,000) per year, he receives an annual allowance of up to €692 ($850). People with a domestic partner receive allowances if they earn less than €47,880 ($58,900) a year.[18] The rest of the premium is paid by the individual. For 2009, the annual price for the basic package varies from €963 ($1,200) to €1,149.96 ($1,400).[19]
Apart from allowances, there are also tax deductions in the Netherlands. All working individuals in the Netherlands can deduct health care costs from their income tax. They can deduct the costs for premiums paid, nursing care, expenses for clothing and bed linen tied to long-term illness, travel expenses when disabled, and similar extraordinary costs.
The Dutch government also introduced a rebate for individuals who did not use any health care services. The idea behind this no-claim rebate was to reduce moral hazard by making people more aware of their health expenditures. However, the policy did not achieve its desired purpose. First, the policy was considered unfair, as in the case of people who needed the same medication for their whole lives and thus could never receive a no-claim rebate. Second, the policy was ineffective given its broad exemptions for primary and nursing care.
As of January 2009 the no-claim rebate was transformed into an annual payment of €150 ($185), which all citizens have to pay out of pocket before the insurance kicks in. Only the chronically ill and the disabled receive financial compensation from the government for this out-of-pocket contribution.
Risk Adjustment. Insurance companies are subject to guaranteed issue and community rating rules. Under guaranteed issue, an insurance plan cannot refuse coverage regardless of health status of the enrollee, thus guaranteeing insurance protection to the very sick and those with so-called pre-existing medical conditions. Under community rating, health plans must charge the same price to everyone within (but not across) each of the 12 provinces regardless of his level of risk or health status. Together, these rules—allowing for universal enrollment of the healthy and sick, and charging the healthy and sick the same regardless of their costs—guarantee adverse selection, where some health plans find themselves with a disproportionate share of sick or high-risk enrollees, and thus with higher costs.
To cope with this problem, the Dutch have created a Risk Equalization Fund. The fund offsets disproportionately high-risk insurance pools with subsidies to cover the additional costs of high-risk enrollees. An insurer with many high-risk patients, such as the elderly and chronically ill, receives larger contributions than insurers with relatively little risk. The fund is financed by two sources: a 7.2 percent tax on the first €31,200 ($38,400) earned by employees, and payments from insurers with below-average predicted costs.
The government first determines the total health care payments and then uses risk equalization to divide those payments over health insurers on the basis of predictable cost differences. Risk equalization is currently done before any patient costs are incurred for the year (ex ante) and then again at the end of the year (ex post).
The ex ante risk equalization is a prospective system of government-run risk adjustment that requires government planning for the correct allocation of the tax funds. The National Health Insurance Board, which also sets the basic benefit package for the health plans, is assigned this task. The board uses statistics, such as age, gender, urbanization, income, pharmaceutical cost groups (PCGs), and diagnostic cost groups (DCGs), in order to calculate equalization payments.[20] In 2006, 12 percent of the Dutch were members of PCGs: people with chronic diseases (at least one year of health problems), people who had drug prescriptions for at least 181 days of the previous year, or people with high future predictable costs. DCGs consist of people who were admitted to a hospital for three or more days in the previous year.[21]
These adjustment mechanisms are reviewed every two years to verify that insurance companies do not have an incentive to engage in risk selection. The ex post or retrospective equalization defrays actual costs above the insurer’s projected spending. For this calculation, the Ministry of Health uses information and statistics from official authorities and government organizations.[22]
Demand-Driven Health Care
In addition to the new insurance system, the Dutch government aimed to stimulate competition by increasing the buying power of insurers. The government therefore relaxed certain budget and price controls, enabling care providers and insurers to negotiate the prices of some treatments. The rationale was that:
Care providers will compete with one another to attract as many patients as possible. The government will lay down requirements for the minimum quality of healthcare provision but there will be freedom of movement, which will stimulate care providers to innovate and to provide a better quality of care than their competitors. Insurers will compete with one another on premiums to attract as many clients as possible. Those who offer the most advantageous alternative premiums will appeal the most to patients. Ultimately, this new system will bring about greater efficiency in the allocation of resources.[23]
But a “more competitive market” did not mean a “free market.” The role of the government remained to “set the parameters that are needed from the viewpoint of the public interest.” The government retained responsibility “in some subsidiary areas, for example training courses, top clinical care and (collective) prevention.”[24] The government still controls the (revised) pricing and funding system and the overall supply of health care. Moreover, the responsibility of providing health quality information to patients remains with the government.
Managed Competition. In some respects, there is little that is genuinely new or original in the Dutch reforms. The reforms, as noted, are based on the influential theory of managed competition, meaning that private health insurance companies compete within a regulated market organized by government officials. Of course, competition for goods and services is nearly always “managed” in the narrow sense that markets typically do not exist outside of the rule of law. For instance, contract law helps protect consumers in the buying and selling of goods and services.
In the case of managed competition for health insurance, however, there is a fairly well developed theory as to what it means, what it is designed to achieve, and how it should be implemented. The key characteristics of the system include an individual mandate to buy health insurance, combined with a program of government subsidies for low-income persons; a government standardization of the health benefits package offered by private health plans; the provision of community-rated insurance plans; and a system of risk adjustment achieved through advanced risk equalization mechanisms. When managed competition theorists speak of health insurance plans, they usually mean managed care plans, characterized by systems of capitated payment (based on the volume of patients under a provider’s care, rather than services rendered) and care coordination.
The Marriage of Theory and Practice
Thus far, the only clear success of the Dutch reforms is that the individual mandate has achieved nearly universal coverage. The impact on health expenditures remains undefined as the Organisation for Economic Co-operation and Development (OECD) reports that the Dutch spent 9.8 percent of GDP on health care in 2007, the same percentage as in 2005. Whether this reflects cost savings is unclear, as the other countries providing data for 2005 and 2007 have a record that is almost exactly balanced: 13 countries reported a spending increase relative to GDP, and 12 countries reported a decrease.[25]
Time will tell whether managed competition can help rein in Dutch health care spending, but two major shortcomings in the reform efforts suggest that any optimism of cost savings should be carefully guarded. First, consumer choice is so constrained that a negligible percentage of the population now switches insurance plans during the annual open season. Second, a market designed to be competitive has quickly turned into an oligopoly replete with allegations of price-setting and other collusive behavior. These troubling developments have been enabled, if not compounded, by a lack of information about health care delivery and quality of care.
Consumer Choice. Prior to reform, politicians explained to the Dutch people that the new system would be “free market healthcare.” Of course, if the health insurance market were truly a free market, individuals would not be obligated to buy insurance. Even with this caveat, an insurance mandate by definition is not mutually exclusive of free choice among health insurance plans; nor does it entitle the government to determine standard benefit packages independent of individual needs. In a market that tolerates meaningful competition, a broad scope of health insurance options will arise to meet the vastly different coverage needs of individual consumers.
In the system of managed competition that was actually implemented, by contrast, there is no real consumer choice. The high nominal premiums and the broad package, determined by the government, do not provide substantive differentiation. Insurers essentially offer the same services under different names.
Two statistics are often used to insinuate consumer choice in the Dutch market: (1) the number of insurers, and (2) the percentage of people switching plans each year.
The number of health insurance companies in Holland is often placed somewhere between 15 and 30, a relatively high number that might suggest robust competition. The truth is that there are four companies—Achmea, UVIT, CZ Group, and Menzis—that share 87.9 percent of the market. (See Chart 1) The eight largest insurers effectively control 100 percent of the market. This market dominance means that smaller insurers, if they are financially successful, will likely be acquired by one of the large companies.
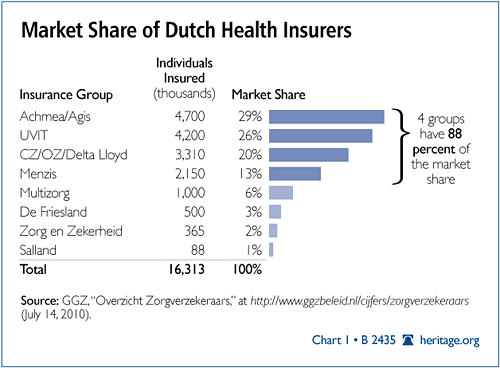
Additionally, the percentage of people changing plans has greatly decreased since the first year post reform. In 2006, almost one-fourth of the Dutch switched insurers. In 2007, one year after the introduction of the new system, the number fell to 6 percent. That figure fell even further to 4 percent in 2008 and to a paltry 3 percent in 2009.[26]
Though the Dutch are technically free to change plans each year, the lack of consumer switching is due to an unwillingness that borders on inability. First, the ability of consumers to find the best plan depends on their ability to obtain information. In 2006, the Dutch government took on the responsibility of informing its citizens about changes in the health insurance system, and it still provides Web sites comparing different insurance companies and insurance packages. The insurance companies, however, do not provide sufficient information about differences, prices, and changes in coverage. As the Netherlands Competition Authority recently reported, information is lacking not only about the quality of providers, but also about the insurance companies themselves (e.g., difference in premium prices, insurance packages, and services).[27]
Second, there must be meaningful price differentiation among plans in order to compensate consumers for switching costs. Many people will be unwilling to change health plans without an appreciable cost savings. Of course, state imposition of a more or less standard plan results in premiums that cost more or less the same: In 2009, the Dutch nominal premium prices ranged from €963 ($1,200) to €1,128 ($1,400) per year.[28]
To those not familiar with health insurance premiums, a 17 percent difference in premiums may seem to indicate substantial competition. Upon comparison to the United States, however, it quickly becomes clear why so few Dutch residents change plans each year.
The authors of this paper used eHealthInsurance, an online U.S. health insurance broker, to obtain quotes for a 25-year-old male nonsmoker living in a suburb of St. Louis, Missouri, purchasing individual insurance. For a preferred-provider plan (PPO) with a $10,000 deductible, the hypothetical 25-year-old should expect to pay about $375 a year. Should he prefer a health maintenance organization (HMO) with no deductible, he should expect to pay about $2,400 a year. In other words, an average nonsmoking, young American male can choose among premiums that differ by 540 percent, a premium range more than 31 times greater than that in the Netherlands.
For a 60-year-old woman who smokes and lives in Sarasota, Florida, the percentage range is smaller: Her individual plan options range between about $3,300 and $9,200 a year, a 175 percent difference. This range in premiums still offers more than 10 times as much choice as the range she would face were U.S. policymakers to import the Dutch system to the United States.
Oligopoly and Market Power. The government of the Netherlands has repeatedly stated that competition is a guiding principle of its reform. The theory has been that competition will create a sense of value, which in turn will drive down health care costs. This focus on value is in line with research such as that from McKinsey & Company, which has found that in combination with an irrational supply of health care—such as the administration of unnecessary medical tests—the failure of the American system to “provide sufficient incentives to patients and consumers to be value-conscious in their demand decisions” is “the overriding cause of high U.S. health care costs.”[29]
Despite the Dutch government’s intention to curb costs by creating a competitive market in which consumers demand value, the market that has emerged is by definition an oligopoly. The nearly 88 percent market share captured by the four largest insurance companies since the reform is well in excess of the baseline concentration ratio for an oligopoly, which economists put as low as 40 percent and as high as 60 percent. Even the most forgiving economist would consider the Dutch market highly uncompetitive.
More definitively, the Dutch system’s Herfindahl–Hirschman Index (HHI), which is used by the United States Department of Justice and Federal Trade Commission to calculate market concentration, places Dutch health care in the category of least competitive markets.
The HHI is calculated by adding together the square of each firm’s market share. For example, the HHI of a market shared by two firms would be 5,000 (50*50 plus 50*50).
The maximum HHI is therefore 10,000 (100 x 100), in the case of a pure monopoly. As competition increases, the HHI approaches zero. Markets with an HHI score below 1,000 are considered unconcentrated, meaning that market power does not lie in the hands of any individual firm. Markets between 1,000 and 1,800 are considered moderately concentrated, and markets with a score above 1,800 are considered concentrated.[30]
Based on the most recent figures available, the Dutch health care system has an HHI of 2,111. (See Chart 2.) This level of concentration not only precludes Dutch consumers from seeking the value that will drive down costs, but it also suggests that supporters of the Dutch system would wish to import to the United States a health care market structure that the U.S. Department of Justice would deem uncompetitive. It is also important to note that the HHI score is now higher than it was before the reform. In other words, managed competition has thus far meant less competition.
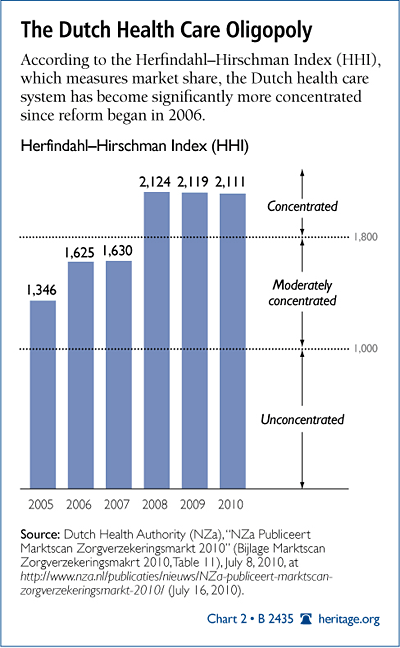
Indeed, supporters of the Dutch system frequently extol the virtues of competition in one breath but then admit a lack of competition in the next. For example, two authors claim that the Dutch reform “has led to fierce price competition.” But in the very next paragraph, the authors allow that “price competition has declined over the years, as the health insurance sector has consolidated through mergers and takeovers.”[31] This trajectory of fierce competition to oligopoly took place in a mere two years.
The trouble with an oligopolistic market is not only that consumers have limited choice and thus are unlikely to find the kinds of values that will drive down health care costs. An additional problem is the risk that firms will collude to set prices.
Since 2008, this risk has increased given that insurance companies now have the power to decide which pharmaceuticals to reimburse. Insurers may force pharmacists to exchange pharmaceuticals that the doctor prescribed to ones that are “about the same” and “therapeutically interchangeable.” This “policy of preference” has proven to be effective in driving down the macro costs as insurers choose generics to replace more expensive, innovative drugs.
But as a researcher at the financial services firm ING warned, the power of insurers could lead to cartels:
If they [insurers] all put the same generic drugs on their preference list, it may be considered as “coordinated and uniform action” which is against the law. Health insurers will aim at the cheapest products available to put in the reimbursement package. There is not a lot of choice in “the cheapest medicines.” All patients will be treated uniformly, regardless what their doctor has to say.[32]
The Dutch association of producers of generic drugs (BOGIN) has also filed a complaint with the Netherlands Competition Authority. As BOGIN chairman Frank Bongers explained, “The preference policy drives out all competition as the big four control the market. Besides, the government’s intention was to make insurance premiums more affordable this way, but the insurance companies have not modified their prices accordingly.”[33]
Instead, health insurance costs continue to increase every year. According to the insurance companies, this is due to higher health care workforce incomes, an aging population, and increased treatments for chronic diseases, such as diabetes and obesity. In 2009, the government prevented a premium increase for consumers by means of a financial injection. This measure “saved” Dutch patients €60 ($75) each that year. “That amount will indisputably be added to the premiums next year,” a spokesman for CZ, one of Holland’s major health insurance companies, declared in De Telegraaf newspaper.
What U.S. Policymakers Should Know
As noted, the 2006 Dutch reforms were specifically based on the theory of managed competition. Initially championed in the United States by Professor Alain Enthoven of Stanford University, the theory of managed competition rests on the belief that insurance companies should compete on price and the quality of care delivery, not benefits.
Other Examples of Managed Competition. A number of working models approach Enthoven’s vision of managed competition, though they differ in crucial details and in most respects fall short of Enthoven’s clear prescriptions. Perhaps the best example of a working program that comes closest to the theory of “managed competition” is the Federal Employees Health Benefits Program (FEHBP). In the case of the FEHBP, health plans are subject to guaranteed issue and community-rating rules. But there is no government standardized benefits package. In fact, there are a variety of benefit options, ranging from fee-for-service and managed care to health savings account plans. Nor is there an individual mandate or any government designed risk-adjustment mechanism to cope with the problem of adverse selection. In fact, curiously enough, the FEHBP, though it is a pluralistic system of private plans that responds to the personal choices of millions of consumers, has no risk-adjustment mechanism at all.
Another health initiative that closely approaches the managed competition model is the Commonwealth Care program, an essential feature of the 2006 Massachusetts health care reform. This program has just five managed care plans, with the same comprehensive standardized health benefits package, that enroll persons eligible for government subsidies for insurance coverage. Like the Dutch system, the Massachusetts program imposes an individual mandate for the purchase of coverage. However, the Massachusetts state officials did not significantly alter the benefit mandates or other regulations that help to drive up health care costs in that state; nor did they put a meaningful break on the continued taxpayer subsidization of key players in the hospital sector. Despite whatever successes Massachusetts can claim in reducing the numbers of the uninsured, cost reduction is not one of them.
The Nature of the Controversy. Some analysts see the Dutch model of managed competition as an ideological compromise, a “third way” between the existing employment-based system of insurance that characterizes American health care and a single-payer model, like that in Canada or Great Britain. Others are more skeptical.
Critics note that the United States is too large, diverse, and varied in its health care financing and delivery to import the compact system used in the Netherlands, a country of 16 million people living on a land area smaller than West Virginia. The broad acceptance and compliance with the individual mandate and differences in risk tolerance in the Netherlands highlight important cultural differences between the Netherlands and the United States. With the enactment of America’s massive new health care law, there is already evidence that the individual mandate, now accumulating legal challenges as to its constitutionality, will be difficult to enforce in the United States.[34]
But more importantly, beyond the vast demographic and geographic differences between the United States and the Netherlands, the theory of managed competition itself holds its own unique challenges.
With regard to insurance itself, the generally risk-averse Dutch will often buy insurance for their bicycles, a sharp contrast with the roughly 15 percent of Americans who do not even comply with mandated automobile insurance. While the individual mandate to purchase health insurance is now U.S. law by virtue of the enactment of the Patient Protection and Affordable Care Act of 2010, the idea had not previously gained much political traction at the state level as a means of expanding health insurance coverage. The notable exception was the state of Massachusetts, which enacted an individual mandate as part of its comprehensive health reform in 2006. Predictably, the recent federal enactment of the individual mandate has resulted in an explosion of controversy and litigation, with 21 states filing suit to challenge its constitutionality. The mandated policy and its penalties remain enormously controversial. According to a recent Kaiser Family Foundation survey, only 34 percent of Americans have a “favorable” view of the individual mandate.[35]
Mandates without penalties are meaningless. Universal insurance through such a mandate is much easier in European countries such as the Netherlands, where notions of social solidarity are simply more highly valued than individual freedom. Americans’ preference for personal liberty, central to American political culture, would suggest the adoption of less coercive policies based on positive incentives and personal responsibility, rather than mandates, to achieve universal or near universal health insurance coverage.[36]
Another important cultural issue involves the tolerance of “poverty traps,” which exist when low-income subsidies undermine incentives to work and increase income. Even if tailored well, subsidies to purchase health insurance may have negative consequences for upward mobility and economic growth. As Enthoven explains in an article co-written with Professor van de Ven of the Netherlands, in the Dutch model, “a high percentage of each extra euro earned reduces the earner’s subsidy, leaving people with little incentive to earn more money.”[37]
In the United States, fine-tuning is required in areas such as Social Security benefits, child tax credits, and earned income credits in order to avoid situations in which individuals have a disincentive to reach higher levels of income. Inflection points at which marginal tax rates increase significantly undercut the economic incentives of individuals to improve their economic positions.
Simply put, poverty traps can mean that policy leading to one step forward also results in two steps back. The Obama Administration came up against the reality when its stimulus plan granted 25 additional dollars of unemployment insurance per week. The result for one man in Georgia was that while he gained about $100 in insurance payments for the month, he lost $300 in food stamps.[38]
One of the signal triumphs of recent social policy was the Welfare Reform Act of 1996, which managed to move millions of Americans off traditional welfare programs and into work, thus reducing poverty. Designing low-income assistance is a delicate task, and American policymakers should be properly concerned that they not devise a system of premium assistance that would discourage work or hamper economic advancement for low-income persons.
As for managed competition, its dependence on a regulatory regime can undermine competition itself. While it is true that a free market cannot flourish outside of the rule of law, there is a real difference between a highly regulated insurance market as envisioned in the managed competition model and a market that is flexible in response to consumer demand governed by a common and limited set of rules, including rules to cope with the problem of adverse selection.
Moreover, the widespread establishment of a managed competition model could easily result in the expansion of government influence through the multiplication of ever prescriptive regulations, particularly over health benefits. Such a development would undermine consumer choice and prevent patients from getting the specific kinds of care options that they want, which is the major point of consumer choice in the first place. The Dutch reform certainly bears out these drawbacks. In the United States, with the full-fledged federal control of health insurance markets beginning in 2014, unless there is a repeal of the new law, Americans will probably have a similar experience.
In addition, the Dutch experience highlights the trouble that managed competition faces in properly equalizing risk. No matter how good the ex ante adjustments, actual costs incurred by insurers will differ from projected costs. In fact, the extent to which this problem will vex any model of managed competition has been quantified by health policy expert Joseph Newhouse, who found that one can accurately predict only about 25 percent of the variation in health spending per individual.[39]
It is for this reason that the Dutch have not abandoned retrospective risk equalization, the use of which creates a dilemma: Should insurers be reimbursed based on the actual costs of providing care to the patient, or based on the average cost of treating the patient’s diagnosed condition?
Reimbursement based on actual cost eliminates the incentive to provide efficient care—also known as “value”—thus driving up overall health expenditures. Some critics fear that the importation of such a reimbursement into the United States would be a step backward, as the move to prospective payment and away from retrospective payment was a key development in American health care financing in the latter part of the 20th century.
The alternative is to tie ex post reimbursement to diagnosis codes, compensating insurers based on the average cost of treatment. But that would leave insurers without a financial incentive to provide care beyond the amount for which they will be reimbursed. In other words, the sickest patients will be at the highest risk of receiving less care than they need.[40]
If the function of a health care market is to secure value for the consumer as a patient, then, at the end of the day, the key decisions would be made by the consumer, including which type of health plan the consumer chooses; which kinds of health benefits the consumer wants or needs; and which kind of payment arrangements for doctors and other medical professionals the consumer thinks is best among a number of competing health plans.[41] There is, in this view of a health care market, no need for a national health board, some “supreme court of health,” or a government-standardized benefit package defining the benefits to which all citizens are entitled.
Conclusion
In 2006, the Dutch government reformed its health care system based on the theory of managed competition. The most important accomplishment of the new system is that the Dutch now have near universal coverage. But, apart from universal coverage, the system does not meet many desirable expectations. There is now, in many instances, less competition and consumer choice; it could be argued that rather than creating a new system, the government is merely sharing its supply-side influence with health insurance companies. The demand side of the health expenditure equation remains virtually unchanged.
Even though the new system is sold as free-market—or at least as competitive-market—the Dutch health reforms have entailed the adoption of significant government controls over health care and delivery. Beyond the adoption of an individual mandate, the government has created a powerful National Health Board, which sets benefits and establishes the rules for risk-adjustment among health plans financed through a special taxation. The government also imposes community-rating and guaranteed-issue rules on health insurance, and establishes benchmarks for physician and hospital payments.
Apart from that, insurance companies have been given a strong position in the health care market. They purchase health care for patients and sometimes—especially in the case of medicines—overrule doctor’s advice.
Other than greater access to insurance, there remains a question of how the reforms have benefited Dutch residents. As explained in this paper, patients in the Netherlands do not have a significant choice between health insurance companies, nor can they access sufficient information about the health system and different options. Perhaps most alarming, the system of “managed competition” has led to a market that is, on the whole, less competitive than it was before reform. After only two years, the Dutch insurance market was a clear-cut oligopoly.
The United States appears to be on a similar path. With the narrow, partisan enactment of President Obama’s health policy agenda, federal regulatory control has expanded dramatically, and the range of potential health care options will be limited. Robust competition can hardly be expected to emerge in this new legal and regulatory environment. Even though most of American health care spending today is publicly financed, there is still strong opposition among Americans to a health care system designed and run by government officials. With the expansion of government control over health care dollars, it is unlikely that an insurance system based on managed competition would serve as a workable compromise between the public-private third-party payment system that Americans have today, and a single-payer system. More likely, such a compromise would accelerate the trend toward a government-run system in which a lack of competition precludes consumer choice and enables ever greater government spending.
—Ryan Lynch is a former Health Policy Graduate Fellow at the Heritage Foundation, and Eline Altenburg-van den Broek is an independent health policy analyst from the Netherlands.



