Abstract: The latest projections of the size of the federal debt by the Congressional Budget Office are gloomy. The CBO estimates that by 2035, Medicare, Medicaid, and Social Security will eat up 15 percent of GDP—with Medicare alone accounting for nearly 7 percent. These levels of spending are unsustainable. Heritage Foundation health care economist Paul Winfree lays out a four-step plan that Congress can follow to move Medicare toward solvency.
In June, the Congressional Budget Office (CBO) updated its budget projections for the next 25 years, providing policymakers with some context of the size of the federal debt. The office’s conclusion: The budget outlook is “daunting.”[1]
The CBO analysts are gloomy with reason. Post-war federal spending has averaged about 20.5 percent of gross domestic product (GDP). By 2035, mandatory federal health spending (Medicare, Medicaid, and the exchange subsidies) and Social Security are estimated to be at least 15 percent of GDP, which will bring total federal spending to more than 27 percent of GDP.[2] Medicare alone is expected to account for 6.7 percent of GDP in 2035, surpassing Social Security and defense spending as the largest federal program.[3]
Unless taxes are massively increased to match this march of spending, the implied rising federal debt will have serious casualties. In fact, the CBO estimates that procrastinating just 10 years on stabilizing the debt-to-GDP ratio would reduce the “well-being of all future generations by amounts equivalent to a cut of roughly 1 percent to 3 percent of their lifetime spending.”[4] Addressing Medicare is central to stabilizing the debt-to-GDP ratio. Furthermore, ensuring Medicare’s long-run sustainability is central to guaranteeing a functioning social safety net.
This paper recommends four steps that will extend the solvency of Medicare and relieve pressure on the growing debt almost immediately, while significantly improving health care options for seniors. The first step involves a modest phase-out of the Medicare subsidy for high-income seniors. The second involves introducing a premium for Medicare’s hospital insurance (Part A) either immediately or once the health insurance (HI) trust fund reaches insolvency, which the Medicare Trustees warn will occur by 2024.[5] The third involves exempting seniors from the Social Security and Medicare payroll tax if they continue to work after becoming Medicare eligible. The fourth involves providing seniors who want to keep their existing private plans, including employment-based plans, with a risk-adjusted defined contribution.
Medicare Financing: The Basics
The traditional Medicare program is made up of three parts: (1) hospital insurance (Part A) for hospital inpatient procedures; (2) supplemental medical insurance (Part B) for doctor’s visits and outpatient procedures; and (3) prescription drug coverage (Part D). Medicare beneficiaries also have the option of buying subsidized private insurance (Part C) to replace the services covered by Parts A and B.[6]
The expenses incurred by Part A beneficiaries are paid by a 2.9 percent tax on wages and salaries of people currently working.[7] For those who have worked and paid payroll taxes for at least 10 years (or had a spouse who did so) there are no premiums for Part A. Many seniors view the taxes paid during their working life as “pre-funding” their hospital insurance. In reality, many seniors collect much more in Medicare benefits than they pay in Medicare taxes. A two-income couple—both earning average wages throughout their lifetimes—can expect to collect 3.2 times as much in Medicare benefits as they paid in taxes.[8]
Unlike Part A, Parts B and D are funded primarily through premiums paid by beneficiaries, and from the general revenues of the Treasury (income taxes, etc.).[9] For instance, just over 25 percent of Part B’s expenditures are covered by premiums. The remainder is almost entirely funded by transfers from the general revenues (that is, government debt or income tax revenue).
Each part of Medicare operates with a trust fund, though it is entirely an accounting exercise rather than an actual account accumulating income to pay to beneficiaries at a future date. In the past, Part A has brought in more revenue from the Medicare tax than has been paid out in benefits in a given year. This trend has reversed, though, as Medicare spending per beneficiary has increased and the population has aged. In fact, Part A benefits paid out have exceeded and will continue to exceed income for the foreseeable future. As Medicare outlays exceed income, Part A draws down on the balance of the trust fund to cover the difference. By 2024, Part A is projected to be permanently in deficit.
Once Part A reaches insolvency (if not before), benefit payments will be cut dramatically unless Congress steps in. Congress could decide that Part A will tap Treasury’s general fund as Parts B and D do already, thereby allowing the shortfall in Part A to drive up the budget deficit. Or, Congress can increase taxes to finance the shortfall, or it can enact specific cuts in Medicare benefits, or make other basic changes to the financing of Medicare. Tapping into the general fund is not a real option, as it does nothing to improve the sustainability of Medicare in the long run and will be disastrous for the economy. Increasing taxes is not an economically sustainable option either, as the Medicare tax would likely have to increase to 6.79 percent of GDP (from 2.9 percent) to eliminate the Part A trust fund deficit.[10] Likewise, the Centers for Medicare & Medicaid Services (CMS) estimates that benefits would need to be cut across the board by more than half to finance the Part A deficit. Benefit cuts of this scale would be difficult for many seniors who depend on Medicare.
Eliminating the long-run fiscal imbalance of Part A, reaching Medicare sustainability, and addressing Medicare’s burden on the federal budget will require significant restructuring of the program. However, there are four steps that Congress can take now that will make Part A more solvent and relieve pressure on the growing federal debt.
Step 1: Expanding the income-based phase-out of the Medicare subsidy for Parts B and D. The Medicare Modernization Act of 2003 introduced income-based phase-outs of the subsidy higher income seniors receive for Part B. The majority of individuals with incomes less than $85,000 and couples making less than $170,000 receive a subsidy that covers 75 percent of Part B program costs.[11] Medicare beneficiaries making more than these thresholds receive a smaller subsidy. The table below illustrates the percentage of the subsidy current Medicare Part B beneficiaries receive by income.
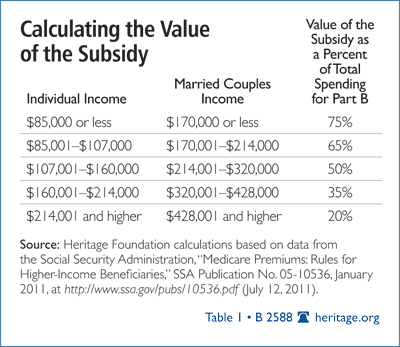
Assessing the merits of the subsidy from a perspective of both good policy and economics, there is no reason why high-income seniors should be receiving such generous subsidies.[12]
Further phasing down the subsidy for Medicare Part B can take several approaches. For instance, as Table 1 notes, the minimum share a couple earning $170,000 or less must contribute to cover the costs of Part B is 25 percent. The Congressional Budget Office estimates that increasing the minimum share of the Part B premium that seniors will have to pay from 25 percent to 35 percent could generate about $240 billion in new premiums over 10 years if implemented immediately. This could reduce pressure on the deficit, as less general revenue will be needed to offset the difference between benefits paid out and premiums paid in for Part B.
An alternative to raising the minimum share of the premium would be to reduce further, or to cut completely, the Part B and Part D subsidies for higher-income seniors. For instance, phasing out the Part B and D subsidies for individuals with incomes greater than $110,000 and couples with incomes higher than $165,000 could generate as much as an additional $58 billion in premiums over 10 years.
A third alternative, which could be pursued along with eliminating the subsidy for higher-income beneficiaries, would be to reduce the income thresholds at which the subsidies are phased down. For example, the threshold at which the subsidy rate goes from 65 percent to 50 percent could be reduced from $214,000 to $190,000. Interestingly, the Obamacare legislation took a modest step in this direction by suspending the inflation-indexing of these income points.
Step 2: Introduce a premium for Part A. The primary source of income for Part A is the Medicare payroll tax discussed earlier.[13] In 2010, payroll tax receipts for Part A were around 1.24 percent of GDP. As the economy recovers—and as the Medicare tax on high-income earners is increased by 0.9 percent as part of Obamacare while the tax is also extended for the first time to include capital income—Part A tax receipts will increase to about 1.4 or 1.5 percent of GDP by 2050.
On the other hand, Part A expenditures are expected to increase substantially, more than twice as fast as revenues. In 2010, these expenditures were about 1.7 percent of GDP. According to forecasts produced by the CMS Office of the Actuary, expenditures for Part A are expected to be 3.0 percent of GDP by 2050 and 3.9 percent by 2080.
If the growth of expenditures for Part A continues on its current trajectory, the Part A trust fund will be exhausted by 2024.[14] Absent other legislative changes, Part A will need deep, across-the-board benefit or payment cuts. The trustees estimate that the cuts would have to be 53 percent in order to eliminate the Part A trust fund deficit.[15] To cover the shortfall, Congress will either have to draw on the general fund, significantly reduce benefits directly, increase taxes, or pass some of the cost onto beneficiaries. Increasing the deficit or increasing taxes will have significant, negative consequences. Furthermore, reducing benefits to make up for the shortfall will require significant cuts in the services Medicare currently covers.[16]
Covering some of the financial shortfall through new premiums for Part A is a good option for increasing Medicare solvency for several reasons. First, as noted above, the average senior benefits much more from Medicare’s hospital insurance than he contributes in taxes to offset its cost over the course of his working life. Second, many seniors are in a much better position than younger workers to bear the burden of some of the cost. Third, beneficiaries today have no reason to be aware of the total costs of the Part A program. Paying a premium for Part A based on a percentage of program costs (similar to premiums for Part B) will provide them with some idea of the overall expense of the program.
Basing Part A premiums along the same income and contribution percentages established for Part B under the Medicare Modernization Act of 2003 is one option. In addition to the premiums beneficiaries pay for Parts B and D, the average beneficiary would be responsible for a premium of just over 25 percent of the average benefit per Part A enrollee. In 2010, the average additional annual premium would be about $1,300, with higher income seniors paying more. If such a Part A premium was introduced immediately, HI trust fund solvency would be extended by 19 years. In addition, net outlays would be reduced by as much as $890 billion between 2012 and 2021. If the premium for Part A was introduced in 2024—at the same time the Part A trust fund was scheduled for exhaustion—the Part A trust fund would remain solvent for another 14 years, or until 2038.
A second way to structure Part A premiums would be to base the new premium on the estimated deficit for Part A in 2012. Similar to the earlier option, beneficiaries would pay a new premium for Part A of about $640 per year in addition to premiums for Parts B and D. An alternative to this proposal would be to reduce the premiums for lower-income beneficiaries and subsequently increase premiums for higher-income beneficiaries. This would be in line with the income-basing of the premiums for Parts B and D. If a premium for Part A along this schedule was introduced immediately, net Medicare outlays would be reduced by $370 billion between 2012 and 2021, and the Part A trust fund would remain solvent for another seven years.
Another way of setting Part A premiums would be to credit the average lifetime Medicare payroll taxes that beneficiaries contribute toward the average benefits received for Part A, charging the difference as an additional premium. The average single man, earning an average wage, will pay about $84,000 in Medicare taxes over his lifetime.[17] He will collect about $251,000 in lifetime Medicare benefits, of which about 44 percent or $110,700 will be Medicare Part A benefits. After adjusting for a life expectancy of 15 years once a beneficiary reaches 65, the additional average annual premium would be about $1,800 in 2010. In order to insure the solvency of the Part A trust fund, the premium would have to be adjusted upward for each cohort’s expected spending and lifetime Medicare taxes paid.
Step 3: Exempt seniors who continue to work from paying the payroll tax. Liberating seniors ages 65 and older from the payroll tax is part of a broader effort to reform the growing entitlement programs. Seniors who choose to work after becoming eligible for Medicare and Social Security benefits should be freed from the burden of paying payroll taxes. At the same time, employers who are willing to hire or retain workers should be exempt from paying the employer share of the payroll tax. This option would keep many seniors, who are an essential part of the economy, in the workforce and paying income taxes until they are ready to retire.
Step 4: Allow seniors to keep their private health plans. Seniors who want to replace Medicare with a private plan should be allowed to do so and without penalty, in exchange for a risk-adjusted defined contribution. This provides an alternative for Medicare and is especially important as many seniors continue to work after the age of 65 with access to employer-sponsored insurance or another private plan. Seniors should be allowed to rejoin Medicare after opting out, but should be subject to pay a risk-adjusted premium plus a penalty payment.
Doing Nothing Is Not an Option
As Congress begins to confront the soaring national debt today and in the years to come, it will become even more obvious that fundamental Medicare reform is an essential part of that process. Though larger reforms of the Medicare program will be needed to ensure its long-run sustainability, this paper lays out several simple steps that policymakers can take now. By tightening the existing phase-out rules for Medicare Parts B and D subsidies for high-income seniors, Congress can substantially reduce the large and growing pressures Medicare creates to drive up the budget deficit. Rather than raising taxes on today’s workers, this policy would pass on some of the cost of the Medicare program to people who are in the best position to bear the burden of their own medical expenses. At the same time, introducing premiums for Part A could eliminate the threat of the insolvency of the HI trust fund. This would buy Congress, and the population close to Medicare eligibility age, additional time to adjust to the more significant and ultimately inevitable reforms of the Medicare program that Congress has yet to consider.
—Paul L. Winfree is a Senior Policy Analyst in the Center for Data Analysis at The Heritage Foundation
Methodology
To estimate the additional revenue generated by phasing out the Medicare subsidy for individuals with incomes over $110,000 and couples over $165,000, the percentage of Medicare recipients that would be affected was first calculated using individual income tax data from the 2006 Statistics of Income. Since the data is from tax returns from several years ago, the adjusted gross income of the tax filing units was adjusted to expected income in 2012 using an average growth rate for income. Since this population is already more likely to contribute amounts greater than the standard 25 percent of premiums for Part B, the same steps were repeated for the income levels currently used to set premiums for Part B to determine the additional premiums taxpayers would be responsible for paying.
For example, if a couple earned more than the 2006 equivalent of $428,000, increasing their premium to 100 percent of the cost of Part B would generate only 20 percent of the average value of the benefits for Part B, as they would already be paying 80 percent. Data from the 2011 Medicare Trustees Report was used to calculate the average benefit per enrollee for Parts B and D as well as the expected growth in average benefits to adjust the estimated average benefit per enrollee to 2012 levels.
Part A premiums based on Part B’s income-based premiums were derived by multiplying estimated total expenditures for Part A by 0.254, or the ratio of estimated income from premiums for Part B and total expenditures for Part B 2011 provided in the 2011 Medicare Trustees Report. To estimate a new expected insolvency date for the HI trust fund, the new premiums were added to the intermediate estimates for Part A income provided in the 2011 Medicare Trustees Report. The new Part A surplus or deficit was then calculated, and a new HI trust fund balance for each year.


