All modern health care systems are the products of history, politics, and culture, and require sound foundations of science, education, and economics. That is why reform of any health care system is as much a matter of social and cultural consideration as it is of organisational, business, or change management. While it would be foolish to attempt to transfer any health care system from one country to another, this does not mean that countries cannot learn from each other. Comparative analyses and the sharing of experience offer powerful aids to learning, reflection, and improvement.
It is in this spirit that this Backgrounder presents its overview of Britain’s experience with its National Health Service (NHS). Ever in search of the best health care system, the author not only acknowledges the failings of the current British and U.S. models, but, in so doing, also hopes to overcome a distracting and unhelpful “dialogue of the deaf” between these two great nations. For, just as many Britons incorrectly believe that all U.S. health care is private, many Americans no doubt assume that all British health care, not just that provided by the NHS, is socialized.
Both countries have much more mixed economies in health care than is popularly acknowledged. In fact, the U.S. spends a greater proportion of its gross domestic product (GDP) on its state health systems (Medicare, Medicaid, the Children’s Health Insurance Program, and the Veterans Health Administration) than the U.K. does on the NHS. (See Chart 1.)
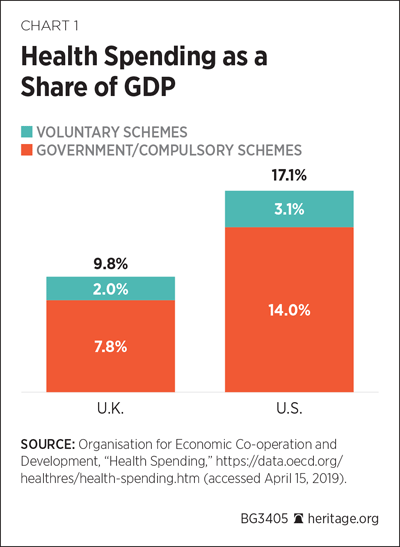
Around the world, people and electorates often take great pride in their own nation’s health arrangements, which are not always justified by performance or comparison. When it comes to practitioners and policy experts, many privately admit that if they could start over again, few would want to do it the same way.REF
Britain’s National Health Service and the Promise of “All”
In 1948, the British government delivered a leaflet to every home in the United Kingdom. In plain English, it announced the promise of the country’s new National Health Service, the NHS. Building on German Chancellor Otto von Bismarck’s official health insurance system of 1883, and Britain’s National Insurance Act of 1911,REF the leaflet heralded a new age of universal health care, funded by national insurance and general taxation, in which all health care services would be provided “free” at the point of delivery. Specifically, the leaflet promised that the NHS “will provide you with all medical, dental and nursing care. Everyone—rich or poor, man, woman or child—can use it.”REF (Emphasis added.)
The key word is “all.” The NHS promised to provide all medical, dental, and nursing care—to everyone. Now 71 years on, Britain’s NHS offers an unrivalled prism into the experience of socialized medicine and the practical reality of such a national insurance and health scheme.
On the upside, medicine and health care have evolved hugely since 1948. In Britain, people now live, on average, more than 10 years longer than they did when the NHS was created.REF
In 1948, women spent an average of 14 days in the hospital after giving birth.REF In recent years the figure is less than 1.7 days. Back in 1900, 160 babies out of in every 1,000 died before the age of one.REF Now, the figure is 3.9.REF
In 1948, there were more than 16,000 general practitioners (GPs). By 2017, this figure had risen to more than 33,000.REF In 1949, Great Britain employed 5,000 consultants and more than 125,000 nurses and midwives. Today, there are more than 45,000 consultantsREF and roughly 300,000 nurses and midwives.REF
In 1958, the NHS launched a polio and diphtheria vaccinations program, which led to dramatic reductions in these diseases. In 1988, the NHS launched a comprehensive breast-cancer and cervical-cancer screening program for women that went on to save thousands of lives.REF
Despite a gradual resurgence of private health care and increased partnerships across the public and private sectors, the founding principles of the NHS remain popular with a majority of Britons. Significantly, the polling company Ipsos MORI ranked the NHS “first” as the institution that made people “most proud to be British.”REF As a result, under electoral pressure, the NHS’s budget has grown significantly over the years. (See Chart 2.)
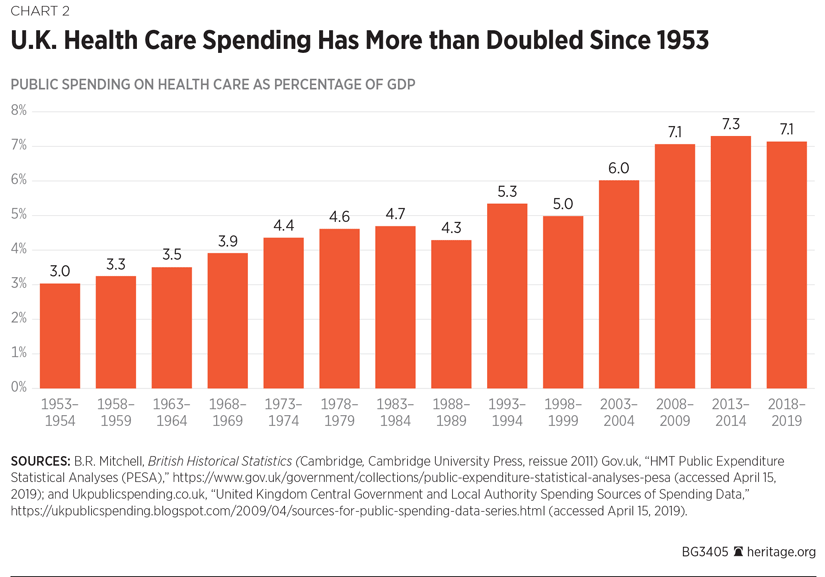
By 2024, the NHS is projected to account for 38 percent of all U.K. government spending, making it the largest item of state expenditure. (See Chart 3.)
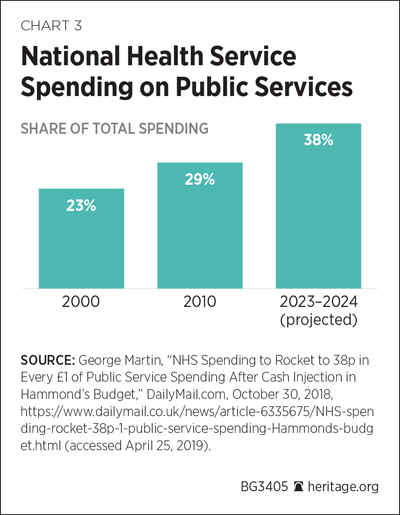
While it remains to be seen whether such a trajectory is politically sustainable over the longer term, public affection for the NHS cannot disguise the service’s ongoing problems and challenges.
Reality and Experience
Despite the promises of 1948, one downside of the NHS experience has been that checks on demand have always involved the rationing of supply, not through price, but scarcity. It was not long before the imposition of cash limits turned doctors into allocators of scarce resources and for a long time “more than minimal care was denied to cases where there was little chance of successful recovery, particularly to young children or the elderly with serious conditions.”REF The supply of NHS health care is also rationed through wait times. Crowded waiting rooms in many general practices and hospital outpatient departments are common. Lengthy waiting times are also a reality for many inpatients, who often wait several days even for those procedures deemed a priority.REF
Against the popular view that the NHS provides free and unlimited health care, history demonstrates that the supply of NHS services has always been limited in significant ways. Experience shows that people have never had an absolute right to free and equal treatment on demand:
What they have had instead is an unlimited right of access to a waiting list from which (with a few exceptions) they will not be excluded. This right of access is not equivalent to a right to treatment, as any notional right to treatment has little value in practice if it is available only at the end of a two-year waiting time. The right to healthcare is unlimited in the long term but is strictly limited in the short term when healthcare is actually required, at the very least, to relieve pain or discomfort.REF
Today, many hundreds of thousands of people are on NHS waiting lists, and countless tens of thousands are trying to get on a list. After decades of reforms and extra tens of billions of pounds invested, out of four million patients admitted to NHS hospitals for routine treatment in 2007, more than half still had to wait at home more than 18 weeks before receiving that treatment.REF While government ministers frequently shy away from talking about the parlous realities of waiting times, figures indicate that 12 percent—almost half a million people—waited more than a year for their treatment and care during 2006 and 2007.REF Nationally, while 6.4 percent of NHS patients pick up infections and illnesses that they did not have prior to being admitted to the hospital, in some hospitals, this figure is above 10 percent.REF Similarly, it was not that long ago when, according to the Malnutrition Advisory Group, more than 50 percent of NHS hospital patients were under-nourished during inpatient stays.REF
While the number of people on NHS waiting lists dropped between 2008 and 2011, not least because greater collaboration with private hospitals enabled greater responsiveness, the waiting list for NHS treatment has grown since 2012. In summer 2018, the figure stood at 4.12 million people on waiting lists, up 3 percent from the year before, and up 59 percent from 2.42 million at the end of March 2010. According to research by the House of Commons Library, “Once estimates for missing data are included the waiting list is currently thought to be at 4.31 million—up 7% year-on-year and 42% over five years.”REF
It is increasingly difficult for people to get a timely appointment with an NHS GP or even find an NHS dentist. As a consequence, many are turning to private GP services,REF with a majority of dentists offering private treatment alongside the NHS.REF
Theoretically, the NHS exists to treat people of all social classes in an equitable manner according to need. In reality, this has never been practiced.REF Analyses of GP consultations have repeatedly shown that patients from higher social classes invariably receive more and better explanations and details of their treatment than lower-class patients, and that middle-class patients spend more time on average with their GP than those from working-class backgrounds.
Julian Le Grand of the London School of Economics demonstrated that, relative to need, patients in professional and managerial jobs have long received at least 40 percent more NHS spending per illness episode than those with semi-skilled or unskilled jobs.
The NHS at 71
At 71, the NHS is internationally below average when it comes to preventing deaths from heart attacks, strokes, and cancer.REF NHS waiting lists for patients in excruciating pain or with life-threatening conditions, including lung cancer and bowel disease, have reportedly doubled since 2010.REF Waiting lists for patients awaiting treatment from a specialist for lung diseases (the U.K.’s third-largest killer) have risen by more than 120 percent since 2011 to almost 100,000 patients.REF Again, since 2011, NHS waiting lists have ballooned from 2.6 million to more than 4 million people.REF
To mark the NHS’s 70th birthday in 2018, the British Broadcasting Corporation (BBC) commissioned independent analyses from several think tanks to identify the service’s performance by international comparison across the developed world.REF The think tanks analyzed the NHS’s performance on 12 of the most common causes of death. The analysts found that the NHS performed worse than average for eight diseases or health emergencies: (1) breast cancer, (2) colorectal cancer, (3) lung cancer, (4) pancreatic cancer, (5) lung disease, (6) respiratory infections (such as pneumonia), (7) stroke, and (8) heart attacks.REF
At its seven-decade anniversary, the NHS has one of the lowest numbers of practicing doctors per population (including GPs and hospital doctors) in the European Union.REF Although the number of nurses is around the EU average, it is lower than comparable countries, such as France, Germany, and The Netherlands.REF Significantly, the NHS has fewer CT scanners (eight scanners per million of population, compared to the EU average of 21.4 scanners), and fewer MRI scanners (6.1 scanners per million compared to an EU average of 15.4 scanners) than most other European countries.REF
Despite huge improvements in medicine, technology, and the NHS budget, approximately 6.8 million people (10.6 percent of the British population) are now covered by private medical insurance; 3.7 million people (5.8 percent of the population) have private health cash plansREF; and a further 3.3 million people (5.2 percent of the population) have private dental coverage.REF More than an additional million people are covered by private discretionary health care plans, such as Benenden Healthcare,REF and hundreds of thousands more pay out of pocket for acute surgery and treatment annually.REF
These figures demonstrate that U.K. health care is already a world away from 1948, when, in order to establish the NHS, the government took into public ownership more than 3,100 private, charitable, or local-authority hospitals, clinics, and nursing homes. Today, not only do varying types of private health care annually touch the lives of many millions of people, there are, once again, hundreds of private hospitals, thousands of private nursing and assisted-living homes, and a growing plethora of private-sector providers that cover everything from eye glasses, dentistry, and acute mental health care to complex surgery, brain injury rehabilitation, and a broad range of general practice services. There are also many independent charities dedicated to supporting patients—as well as their families and friends—with specific progressive conditions, such as Parkinson’s, Alzheimer’s, or multiple sclerosis.
The re-emergence of a mixed economy in health care becomes even clearer when considering that more than 50 percent of the Trades Union Congress’s 6 million-plus members also benefit from a range of private health plans.REF According to the web site of one of the U.K.’s largest public-sector trades unions, Unison, its collective muscle enables it to offer its members private health coverage from as little as 80 pence per day.REF
It is against the backdrop of these developments, and under the rubric of public–private partnerships, that in the year 2000 the government signed an agreement with the representative body of the country’s independent health care sector (the Independent Healthcare Association) to enable NHS-funded patients to receive care and treatment in more than 200 private hospitals nationally.REF By the beginning of the millennium, much of the estate that had been removed from the private and charitable sector to create the NHS in 1948 still retained features of its pre-nationalized past. With a significant proportion of the estate predating World Wars I and II, change was required in the form of increasing private-sector capital and investment.REF
In 2001, following several years of greater private capital investment in the NHS’s stock, the government allowed the private sector to design, build, and operate a network of Independent Sector Treatment Centres (ISTCs) for NHS-funded patients.REF With the subsequent establishment of more independent and flexible NHS trusts and foundation trusts, the NHS remains the dominant funder of U.K. health care but is no longer the monopoly provider or owner of the facilities in which its services are increasingly delivered.
However, as measured by Bloomberg,REF despite years of modernization and significant increases in resources, British health care still fell 14 places and is now behind Chile, Algeria, and the Czech Republic. British health care dropped from 21st place (of 56 countries measured) in 2014 to 35th in 2015.REF This shift means it has fallen to the bottom half of the Bloomberg tables and is currently behind Mexico—with Slovakia and Peru as its peers.REF
Bloomberg’s annual analysis compares countries on the basis of life expectancy versus the percentage of spending on health care. In the U.K., the absolute cost amounts to £3,327 a year ($4,356) per head of population.REF While the U.K.’s life expectancy has remained largely unchanged in recent years, other countries have witnessed significant improvements.
Overall, Hong Kong remains at the top of the tables with life expectancy at 84.3 and just 5.7 percent of GDP spent on health care. Second is Singapore with a life expectancy of 82.7 and 4.3 percent of GDP spent on health care. By contrast, Spain and Italy have similar life expectancy rates but both spend more of their GDP on health care. While Spain spends 9.2 percent on health care, Italy spends 9.0 percent.REF
The Challenge of Bureaucratic Displacement
While such research does not account for people’s lifestyle choices and the pressures they in turn place on demand, the theory of bureaucratic displacement (Gammon’s Law) suggests that in any highly bureaucratized system, such as the NHS, “increases in expenditure will be matched by a fall in production.”REF At their worst, such systems act “rather like ‘black holes’ in the economic universe, simultaneously sucking in resources, and shrinking in terms of ‘emitted’ production.’”REF
The idea that additional resources will deliver efficiency, greater productivity, and better outcomes has long been problematic for the NHS. For example, Prime Minister Tony Blair announced in January 2000 an “unprecedented 5 per cent annual increase in NHS spending for the next five years” between 1998 and 2005, and the NHS hired an additional 307,000 people, including doctors, nurses, and administrators.REF At the time, this was the largest growth by a single employer in any country. Four years later, the NHS had taken on 52,000 more administrators, increasing its managerial payroll by more than 30 percent. Yet the additional staff did not make the NHS any more efficient or effective. Research by the Office for National Statistics revealed that staff productivity actually declined between 2001 and 2005.REF
A 2004 study by the Office for National Statistics confirmed that money was being wasted on a sizeable scale. Just £35 of every additional £100 spent had produced real improvements in the previous two years. Of the remainder, £56 had fuelled inflation within the NHS, and £9 was lost through falling productivity.REF
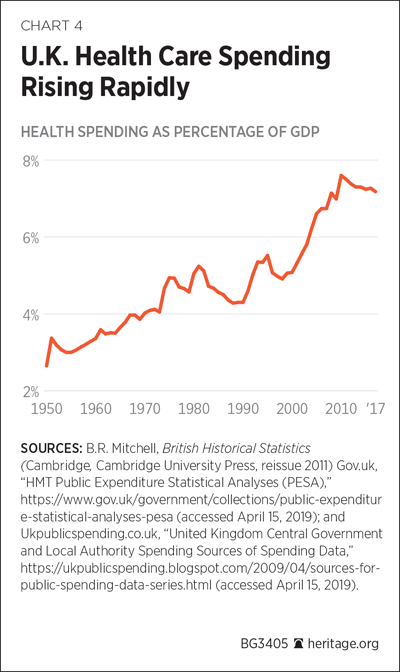
As extra sums poured into the NHS (see Chart 4), many hospital administrators and doctors were sticking to outdated practices. Even worse, half of the annual increase in the budget was spent on ever greater recruitment and higher wages. Within three years, GPs’ annual pay had doubled to more than £105,000, yet they were working fewer hours. By 2006, there were reports that some GPs were earning £250,000. As for consultants’ salaries, they went up by 27 percent to an average of more than £109,000.REF
Most of the additional £3.6 billion pledged to the NHS in 2005 was earmarked for pay increases, drugs, buildings and negligence payments. Just £475 million was actually directed towards improving the treatment and care of patients. Throughout all of this, there were reports of a 200 percent difference between the cost of the most and the least efficient NHS hospitals. Some GP surgeries were giving patients an appointment within a day, while others expected them to wait for five days or longer.REF
As Prime Minister Blair announced an NHS budget of £108 billion for 2007, deficits in many parts of the NHS were increasing. Moreover, health inequalities among the population had remained the same and in some instances were even increasing. A third more people were going to Accident and Emergency (A&E) “because 40 per cent of GPs were no longer working full-time.”REF And without proper competition, there had been no narrowing between the best-performing and worst-performing hospitals. In the best, for example, operating rooms were being used 75 percent of the time, while in the worst, the figure was as low as 35 percent.REF
Yet, ever greater amounts of money were being consumed. When Blair became Prime Minister in 1997, the NHS’s budget had been £34 billion. By 2012, it had grown to more than £120 billion.
In recent years, NHS performance has been deteriorating on a broad front: “The 18-week-to-treatment standard for planned care has not been met since February 2016, the A&E four-hour standard since July 2015 and the 62-day cancer standard for more than three years.”REF
Since 2012, the national target for elective care stated that more than 92 percent of NHS patients should start their treatment within 18 weeks from referral. While the number of patients receiving elective treatment has grown approximately from 14.2 million in 2012 to 15.7 million in 2017REF (an 11 percent increase), the total elective waiting list in April 2012 was 2.5 million. By 2017, this list had increased to an extraordinary 4.1 million people.REF Despite changes in clinical practice, including the inexorable rise of outpatient surgery, ever-mounting pressures on the service meant that its national leaders had to openly accept that it could no longer meet its targeted standards.REF While the official A&E standard is for no less than 95 percent of patients attending A&E to be admitted, transferred, or discharged within four hours, this target has been missed for the past three years.REF
When it comes to accessing cancer treatment, the most important target is that more than 85 percent of NHS patients should begin their care within 62 days of an urgent referral from their GP. While this standard was ushered in from 2009 to 2014, it has been missed every year since.REF The NHS is treating more patients every year, and key performance measures for hospital services are now being missed all year, not simply during the winter months.
Not only do ambitions to hold waiting lists steady for 2019 reportedly look to be “doomed,”REF but the slide is having serious socioeconomic effects. For example, while 2017 saw private-sector self-pay revenue increase by 9 percent to £1.1 billion, the independent market analysts LaingBuission recently concluded that “dissatisfaction with the NHS is now the primary driver of self-pay demand…for people seeking…diagnosis and treatment.”REF
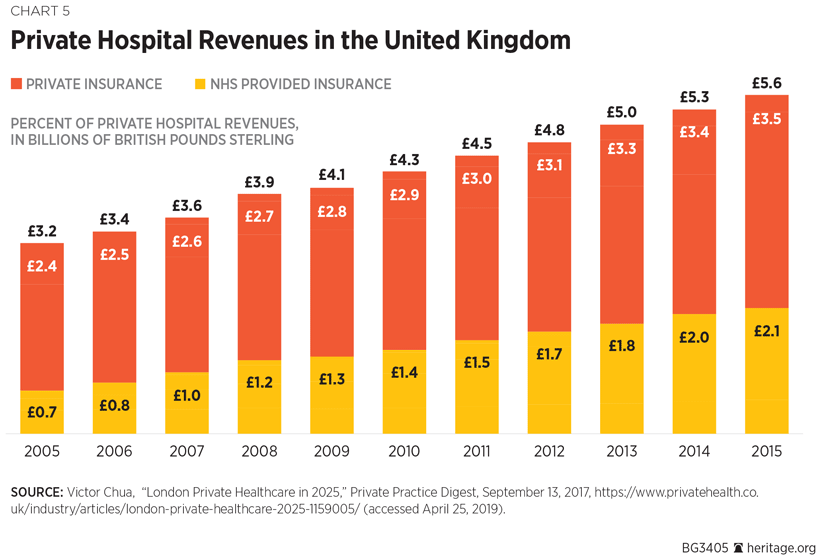
From the viewpoint of 2019, the NHS is travelling ever further away from the political promise of 1948. Experience shows that despite huge increases in funding, countless reforms, and increased partnerships with the private and charitable sectors, fundamental problems associated with rationing and bureaucratic displacement continue to abound.
Important Lessons for U.S. Policy
Overall, Britain’s experience with the NHS portends a number of lessons that American policymakers can apply as they consider the future of the U.S. health care system. Even with widespread electoral support and ever-increasing amounts of government expenditure, those who require medical treatment often end up suffering because of perpetual access problems. Although medicine and technology have advanced hugely around the world in recent decades, the British experience with socialized medicine is that it leads to comparatively poor outcomes in key areas, such as heart attacks, cancer, and stroke. Moreover, as pressures associated with bureaucratic displacement mount over time, ordinary people revert to using more-open, diverse, and market-based solutions for their health needs. The saving grace is that in an open and free society, the unintended consequence of socialized medicine is that it often helps a thriving private alternative to re-emerge.
Conclusion: London Calling
Experientially, no health system is perfect. Most have strengths and weaknesses. While all systems globally are underpinned by statutorily defined, monopoly suppliers of labor (the national equivalents of the U.K.’s General Medical Council for doctors, and the Nursing and Midwifery Council for nurses and midwives),REF most systems are riven with complex problems rooted in politics, history, and law.
The underlying institutional architecture of much of U.S. health care is a classic case in point. Dogged by an employer-based, geographically restrictive, and highly corporatist health insurance market, America’s public and private health sectors are not only costly, but the systems increasingly disport the worst elements of overly politicized monopoly markets and poorly directed government interventionism.
Seventy-one years on from its inception, the British experience with the NHS is similarly clear. The NHS remains popular with voters because it has made a clear contribution to health improvements and relieves people of the burden of having to worry about money.REF However, it also performs less well than systems in similar countries when it comes to the overall rates at which people die when more effective medical care could have saved their lives.
The NHS relies heavily on rationing, long wait times, and currently suffers poor health outputs in key areas including cancer, heart health, and stroke. Bureaucratic, inefficient, and riddled with poor productivity, it does not come close to providing the medical, dental, and nursing care that was promised in 1948.
It is these failings that have encouraged a resurgence of independent (private and charitable) medical, health, and social care in recent decades. With millions of people now using private hospitals, clinics, nursing homes, dentists, and other market-oriented health care services, a much more mixed-economy approach is becoming the norm.
—Tim Evans is Professor of Business and Political Economy at Middlesex University London, a Senior Fellow with the Adam Smith Institute, and Chairman of the Economic Policy Centre.


