Among the consequences of the Affordable Care Act (ACA or Obamacare) are its effects on insurer competition, particularly in the law’s new government-run exchanges. By several different measures, insurer participation in the ACA exchanges declined in 2016.
Measuring Competition
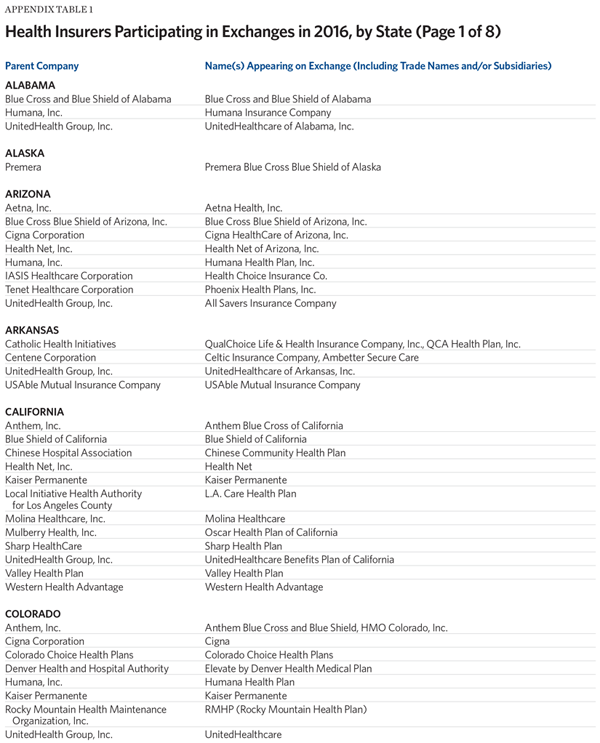
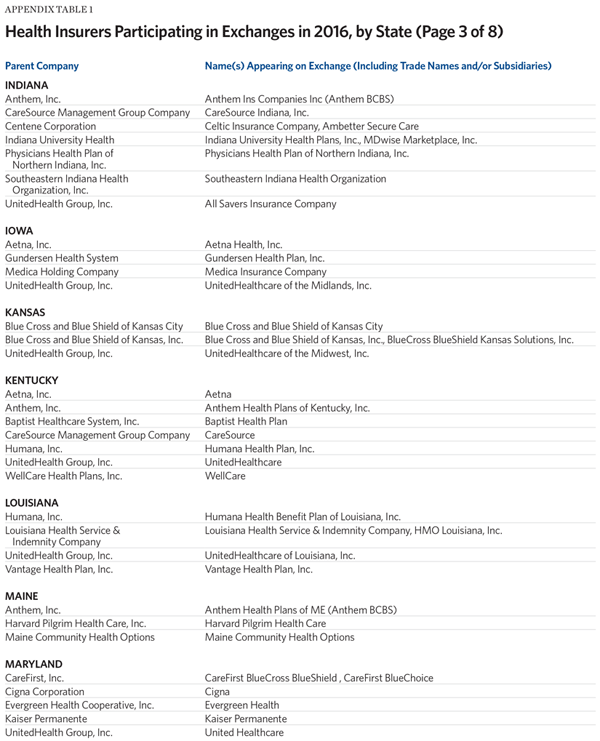
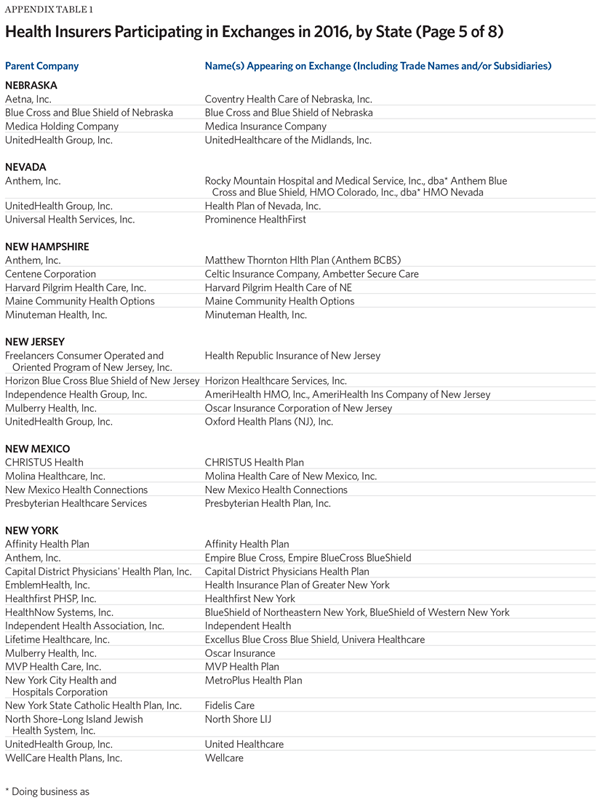
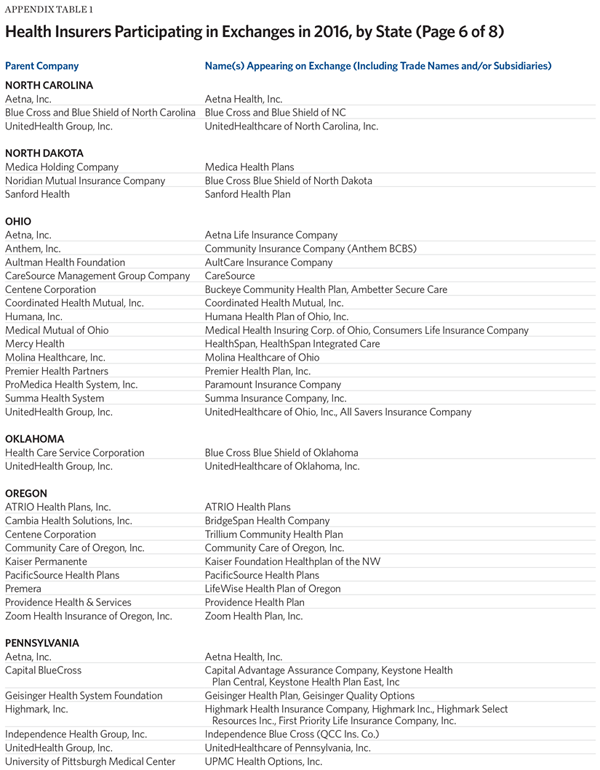
One measure for the level of competition is the number of insurers offering exchange coverage in the 50 states and the District of Columbia. For this metric, insurers that offer exchange coverage through more than one subsidiary in a state are properly counted as only one carrier (the parent company), while insurers that offer coverage in more than one state are counted for each state (as exchange participation is a state-level decision).
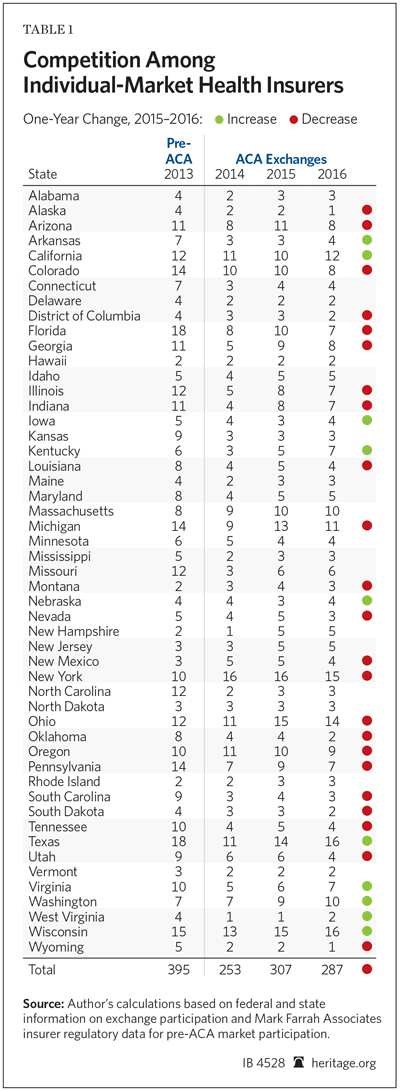
By this measure, in 2016, there are 287 exchange-participating insurers, as compared to 307 in 2015. While the participation level in 2016 is greater than the 253 insurers that offered exchange coverage in 2014, the figures for all three years are still well below the 395 insurers that offered individual-market coverage in the 50 states and the District of Columbia in 2013, just prior to the ACA taking effect.
Another measure is to assess changes in insurer participation on a state-by-state basis. That analysis, summarized in Table 1, finds that, relative to 2015, 45 percent of the states (22 states and the District of Columbia) have fewer insurers offering exchange coverage in 2016, while only 10 states have more insurers offering ACA exchange coverage.
Insurer competition can also be measured at the national level by counting the number of unique carriers offering exchange coverage in one or more states. By that metric, insurer exchange participation not only declined in 2016, but also is now less than in 2014. At the national level, the number of carriers offering exchange coverage in one or more states was 154 in 2014, increasing to 155 in 2015, but declining to 137 in 2016.
Understanding the Changes
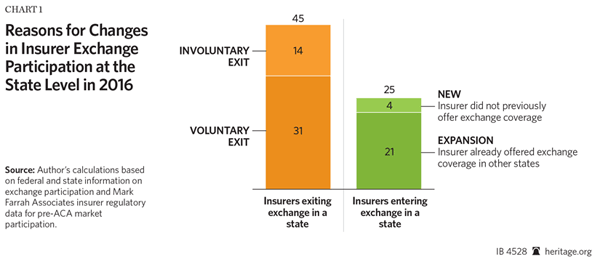
At the state level, the 20 fewer exchange participating insurers in 2016 (287 in 2016 versus 307 in 2015) was the net effect of 25 exchange entrances and 45 exchange exits by insurers, as summarized in Chart 1.
Among the 45 exchange exits, 14 can be characterized as involuntary since they resulted from state insurance regulators barring carriers deemed financially unsound from issuing new policies and renewing expiring policies. Eleven of those exits were due to the collapse of co-op insurers, created under another provision of the ACA.[1] The remaining three involuntary exits resulted from the collapse of WINhealth Partners in Wyoming and the suspension of Moda Health Plan by Alaska and Oregon insurance regulators.
Of the 31 voluntary exits, seven resulted from insurers reducing the number of states in which they offered coverage, 21 were the result of carriers withdrawing entirely from the exchange market, and three were due to acquisitions by other insurers.
Assurant was the carrier responsible for the largest number (16) of voluntary exchange exits. That company stayed off the exchanges in 2014, offered exchange coverage in 16 states in 2015, and then withdrew from all of them for 2016.
Of the three instances where insurers exited the exchanges due to acquisitions, two reduced the number of insurers offering exchange coverage, while the third had no effect as the acquiring carrier replaced the insurer that it bought on the state’s exchange.[2]
These changes also leave two states—Alaska and Wyoming—with only one insurer offering exchange coverage in each state for 2016. By comparison, there were two states in 2014 (New Hampshire and West Virginia) and one in 2015 (West Virginia) that had only one insurer offering exchange coverage.
Of the 25 exchange entrances, four were insurers that began offering exchange coverage for the first time in 2016, while the remaining 21 resulted from insurers that already offered exchange coverage in at least one state expanding their exchange presence to one or more additional states. The largest such expansion was by UnitedHealth Group, which extended its offering of exchange coverage to 11 additional states in 2016. The remaining 10 exchange entrances were the result of four carriers that each expanded into one additional state and three carriers that each expanded into two additional states.
Even Less Participation Likely for 2017
The reduction in insurer participation in the ACA exchanges in 2016 resulted from a combination of state regulators closing down financially troubled carriers and insurers voluntarily exiting markets that they found unprofitable. In light of other indicators, that experience suggests that insurer participation in the ACA exchanges is likely to further decline in 2017.
To start with, there are several pending health insurer mergers. The proposed acquisitions of Cigna by Anthem, Humana by Aetna, and Group Health Cooperative (in Washington state) by Kaiser are all likely to reduce the number of exchange participating insurers. Second, there is the possibility that still more financially precarious insurers could be forced off the market by state regulators. Third, a number of carriers, most notably UnitedHealth Group, have incurred significant losses from offering exchange coverage and have publicly stated that they are reassessing the extent to which they will continue participating in the exchanges.
Finally, the ACA’s “reinsurance” provision imposed $20 billion in assessments on health insurers and self-insured employer plans for the first three years (2014–2016) and redistributed those funds to carriers offering individual-market coverage (both on and off the exchanges). With that additional subsidy soon ending, more carriers will likely be taking a hard look at whether it remains financially feasible for them to continue offering exchange coverage.
—Edmund F. Haislmaier is Senior Research Fellow in the Center for Health Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.