Accounting for one-fifth of national health spending, Medicare plays a major role in structuring our nation’s health system.REF Like other fee-for-service (FFS) health plans over the past half-century, Medicare has failed at both cost control and integrating and coordinating benefits for retirement-age Americans. With retirees—many with multi-morbidity—set to outnumber children under 18 by 2035,REF a high importance should be placed on rethinking health care financing and delivery. The payment system behind traditional Medicare—Parts A and B—directly reimburses clinicians on the basis of the number of services delivered and is at the center of the debate on how policymakers can incentivize efficient, high-value care to beneficiaries.
Under a pay-for-volume system, an unlimited number of services could be delivered with no cost ceiling, presenting Medicare as a blank check for the health care of over 67 million Americans.REF DemocratsREF and RepublicansREF alike have questioned the sustainability of federal spending on health care programs, which is projected to steadily rise as a percentage of gross domestic product over the next 30 years.REF
This paper reviews the history of insurance design in the Medicare program, including the challenges of insurance design and subsequent application of risk-transfer tools in traditional FFS Medicare. Alongside this evolution, we characterize the introduction and growth of private plans in the Medicare marketplace, noting benefits and trade-offs for both beneficiaries and taxpayers. Finally, utilizing lessons from retirement planning, we recommend Congress auto-enroll newly eligible beneficiaries into Medicare Advantage (MA), with a default assignment into the lowest cost (i.e., zero premium) plan. Such a change would provide policymakers with a potential framework to help stabilize program budgeting by placing more beneficiaries into risk-adjusted, capitated plan products.
Insurance Design in the Medicare Program
The Medicare program consists of two primary programs: traditional Medicare (a FFS model) and MA, which is based on market-driven health plan competition. The FFS model, consisting of two-thirds of the Medicare market, is a product of insurance design dating back to its legislative birth in the 1960s, while MA emerged in the 1970s and has tracked the rise of the managed care industry. Here we briefly review the design of, periodic updates to, and challenges of each.
Traditional Medicare and the Evolution of a Publicly Funded FFS System
Originating in the Social Security Amendments Act of 1965 (H.R. 6675), Medicare began its life as a traditional FFS health plan with the aim of providing coverage to impoverished elderly Americans in the remaining few years of their life; average life expectancy at birth was 70.5 years.REF Like other FFS plans, Medicare relied on price regulation for cost control. Health economists typically describe the “health care cost equation,” in which total cost is a function of price, volume, and the intensity of service,REF or f(P, V, I). (See Figure 1.) For traditional Medicare, the Centers for Medicare and Medicare Services (CMS) administratively sets prices for physician and hospital services, while clinicians and beneficiaries jointly determine the volume and intensity of services.

With administratively set prices,REF traditional Medicare implicitly rewards clinicians on the basis of volume while intensity of care remains insufficiently addressed, a policy failure characterized by repeated congressional attempts at reform.
Recognizing the challenges of budgetary control within a FFS context,REF the Reagan Administration and Congress worked together to craft legislation to introduce prospective payment and episodic bundling for hospital care. The Diagnosis Related Group (DRG) system, introduced in 1983 as part of the Social Security Amendments,REF implemented a prospective payment system anchored by hospitalization and including associated costs (service, pharmaceuticals, devices, etc.). A patient’s principal diagnosis and up to 24 secondary diagnoses—including comorbidities or complications—determine the DRG category, which determines the base payment rate,REF an amount further adjusted for geographic variation in wages, graduate medical education, and other features such as rural location.REF
Following implementation, hospitals could no longer bill based upon incurred costs: Prospective, bundled payment initially drove efficiency gains. Over time, hospitals began to shift services to the outpatient setting, in part to escape DRG-based payment. Recognizing this, Congress—as part of the Omnibus Budget Reconciliation Act of 1990—created a “three-day payment window,” mandating inclusion of hospital outpatient services in the DRG payment bundle if provided within the three days prior to hospital admission. While areas such as hospice have retained a per diem (daily) rate,REF other components of traditional Medicare, such as home healthREF and outpatient hospital services,REF have transitioned to episodic, prospective payment systems.
For physician payment, the CMS has attempted to deploy other tools of risk transfer in order to drive performance.REF The Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) created two quality performance pathways for physicians: Alternative Payment Models (APM) and the Merit-based Incentive Payment System (MIPS), with practices choosing their “path to risk.” Practices could opt to receive a 5 percent payment boost for participating in an APM through the CMS Innovation Center. Alternatively, physicians could participate in MIPS, a risk corridor with scoring in multiple areas. Summed, weighted performance across measured areas dictates payment adjustment, a risk corridor of +/- 9 percent for payment year (PY) 2020.REF
In theory, health plans can choose both the metrics and adjust the “performance bar” annually. The CMS is no exception, although it is statutorily constrained in that MACRA specified that the combination of bonuses and penalties must remain budget neutral. Based upon PY 2018 data, 97 percent of practices received a positive score and a bonus payment, with 84 percent of practices demonstrating “exceptional performance” and achieving the maximum payment adjustment of +1.68 percent,REF suggesting the metrics driving the risk corridor are inadequately anchored to performance.
The evolution of FFS Medicare reflects the application of multiple tools from policymakers’ payment policy toolkit. Risk corridors tie percentage payment adjustments to performance metrics, noting that providers can game metrics or plans can anchor performance targets too low, failing to meaningfully drive performance, as in the case of MIPS. Episodic bundles triggered by clinical events such as inpatient admission or elective surgeries capitate risk across an event or time yet are subject to other forms of gaming. For decades, under DRG-based reimbursements, hospitals have benefited from readmissions, a more recent target of CMS quality efforts.
While the Medicare FFS model of the 21st century deploys more tools of risk transfer than Medicare in its original form, it still suffers from uncontrolled cost growth.REF Unlike private plans, traditional FFS cost control mechanisms, such as prior authorization and utilization review, remain reviled by physicians and politically unfeasible. Network design is absent: Medicare represents an “any-willing provider” network,REF wherein a beneficiary can see any physician regardless of their quality or cost-effectiveness. Other tools of cost control, such as partial and full capitation, which serve to transfer both financial and clinical risk from payers to providers, remain undeployed. (See Figure 2.)
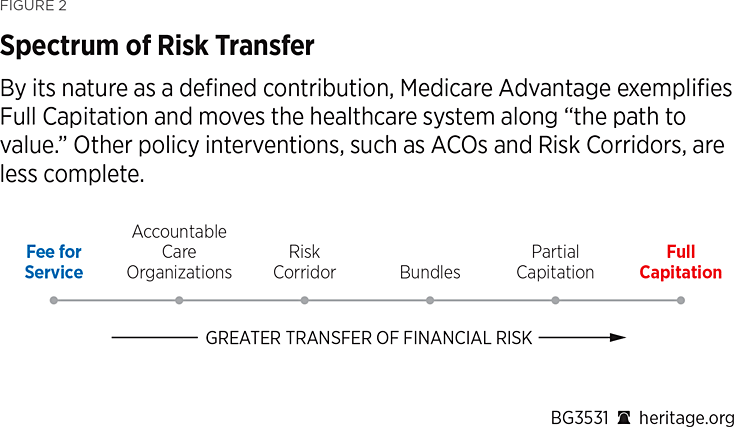
The limitations and struggles with cost growth in FFS Medicare served as the impetus for the entrance of and simultaneous development of managed care plans in Medicare.
The Role of Private Plans in the Medicare Program
While their initial involvement in the Medicare market began inauspiciously as cost contracts, through continued legislative attention and industry innovation, private plans now comprise more than one-third of Medicare’s total enrollment. Throughout the 1970s, private markets continued experimentation with health maintenance organization (HMO)–style plans, spurred by both growing costs and the HMO Act of 1973.REF The Medicare program was no exception, with the Tax Equity and Fiscal Responsibility Act of 1982 creating a pathway for HMOs in Medicare. Plans were capitated and prospectively paid 95 percent of the adjusted average capita cost, with payment adjusted for demography, disability, institutional, and Medicaid status. Enrollment lagged due to a lack of consumer familiarity with network plans and statutory limitations on plan design.
After slow growth in the 1990s, Congress passed the Balanced Budget Act of 1997, transforming private Medicare by expanding the choice of product offerings and—in an attempt to improve payment accuracy—requiring changes to risk-adjustment methodologies. Renamed Medicare+Choice, plans could now offer additional designs, including preferred provider organizations (PPOs), private FFS, medical savings accounts, and provider-sponsored organization plans. This expansion of beneficiary choice was, however, countered by changes in payment methodologies, driving plan exit from many county-level markets.REF
Congress responded with the 2003 Medicare Modernization and Improvement Act (MMA), creating the Medicare prescription drug benefit (Part D), authorizing Special Needs Plans (SNPs) for further plan customization, and modifying plan payment methodology. MMA implementation coincided with a wave of retirees who, both comfortable and experienced with network plans offered by their employers, enrolled in MA in droves.REF As part of implementing the 2010 Patient Protection and Affordable Care Act (ACA), the CMS enacted a final adjustment—based upon academic researchREF demonstrating overpayment of MA plans—further modifying plan payment methodology to bring MA in line with FFS spending while simultaneously tying the Stars quality program to payment bonuses,REF resulting in the MA program that exists today.
Beneficiary Trade-offs in Medicare Advantage
MA, as it exists today, represents a series of trade-offs for both beneficiaries and policymakers. Beneficiaries gain limitation on their personal financial liability along with supplemental benefits, both in exchange for some utilization and network controls for health care products and services.
In 2019, the average premium of MA plans (paid for as a separate cost to those of Part A and B) is estimated to be 7.2 percent ($4.50) cheaper than the basic Part D premium alone (which traditional Medicare beneficiaries purchase separately).REF Further, in 2019, half of MA beneficiaries had a “zero premium” plan,REF and average premiums are expected to decrease by 23 percent in 2020.REF
MA plans also set limits on out-of-pocket costs to consumers, unlike its FFS alternative. For HMOs that cover in-network services, this limit averaged $5,059 for 2019 and could not exceed $6,700. PPOs, which offer coverage for both in-network and out-of-network providers, must have a combined limit on out-of-pocket costs of $10,000 or less, though this averaged $8,818 in 2019.REF
Competition among MA plans has historically fueled the inclusion of various supplemental services not covered under traditional Medicare. For example, in 1986, a survey of Medicare HMO beneficiaries revealed that 84.7 percent had prescription drug coverage,REF a benefit added to the traditional Medicare program by Congress 17 years later.
Private-sector innovation has allowed for health plans to experiment with new benefits, evaluating both satisfaction and cost-effectiveness while focusing on functional areas core to independence. The story here is similar to prescription drugs, with research from 2016 demonstrating that an estimated 62 percent of MA beneficiaries had dental benefits while 67 percent had vision benefits. In contrast, among beneficiaries enrolled in traditional Medicare, 96 percent lacked vision insurance and 79 percent lacked dental coverage.REF
Plans continue to experiment with other supplemental benefits, such as wheelchair ramps, bathroom grab bars, meal delivery after hospital discharge, home modifications, gym memberships, and even the Apple Watch.REF Flexibility is key, helping elderly and disabled Americans maintain their independence.REF In contrast, innovation is challenging in traditional Medicare, which requires rulemaking and frequently statutory change to redefine or expand benefit categories. Beneficiaries cover the gap, with eight in 10 beneficiaries possessing some form of supplemental insurance—aptly named Medigap policies, employer-sponsored insurance, or even Medicaid.REF
Coordinated and integrated care, largely unavailable in FFS Medicare, presents another potential boon for beneficiaries. Research on MA has demonstrated benefits, including less intense post-acute care use,REF lower readmission and preventable hospital rates,REF more appropriate health care utilization,REF and decreased intensive care unit use,REF to name a few. While researchers debate the exact benefits, MA offers the potential for integrated care, a challenge in the FFS system.
Finally, vulnerable populations—such as those living in institutions or those with both Medicare and Medicaid—face even greater challenges in managing their care and health. More than half live with at least one functional impairment in activities of daily livingREF and are almost twice as likely to self-report their health to be “fair” or “poor” when compared to other Medicare beneficiaries.REF MA provides special flexibility for these and other groups, allowing for benefit customization in the form of SNPs. Auto-enrollment would simplify the organization and coordination of health benefits for disadvantaged populations.
In exchange for limitations on their financial liability and for obtaining supplemental benefits, beneficiaries are subject to some utilization and access controls. A network of providers is common among MA plans and often where concerns over the program are directed. Yet a 2017 analysis found 65 percent of enrollees to be in plans featuring either “medium” (accepted by 30 percent–69 percent of physicians in an average county) or “broad” (70 percent or more) networks.REF Consistent with this, almost two-thirds of MA participants are enrolled in HMO plans and the remainder in PPO plans.REF Given beneficiary experience with employer-sponsored insurance,REF the trade-offs between greater benefits and utilization and access controls are familiar to consumers. Consumers have voted with their feet and are leaving traditional Medicare for MA: In 2020 the FFS Medicare program, experiencing a steady annual decline since 2010, covered 60 percent of beneficiaries.REF
Medicare Advantage: A Natural Experiment in Health Plan Competition
Under MA, policymakers have set up a natural experiment in health plan competition.REF The CMS contracts with insurance companies and integrated delivery systems to design and administer health insurance plans that must meet or exceed the coverage standards of traditional Medicare. A rate filing or bid process takes place in which the CMS agrees to pay plans a fixed monthly amount per beneficiary, a method known as capitation. Capitation rates are risk-adjustedREF based on each beneficiaries’ health and eligibility statuses to best account for the total predicted future cost of their care. Health plans then assume risk and responsibility for making payment arrangements with providers and designing and administrating benefit packages for beneficiaries.
The opportunity for comprehensive quality improvement lies in the ability of MA plans to operate outside the FFS model, using this flexibility to distribute risk in more ways that both increase physician accountability and incentivize value. (See Figure 3.) As previously described, there are a number of payment arrangements these plans and providers can enter—gainsharing, risk corridors, partial capitation, private FFS, and episode bundlingREF among others—all of which have strengths and weaknesses in generating more value for the dollar.REF With 41 percent of MA spending directed through risk-transfer payment models, MA exceeds other plan markets in transferring risk to providers.
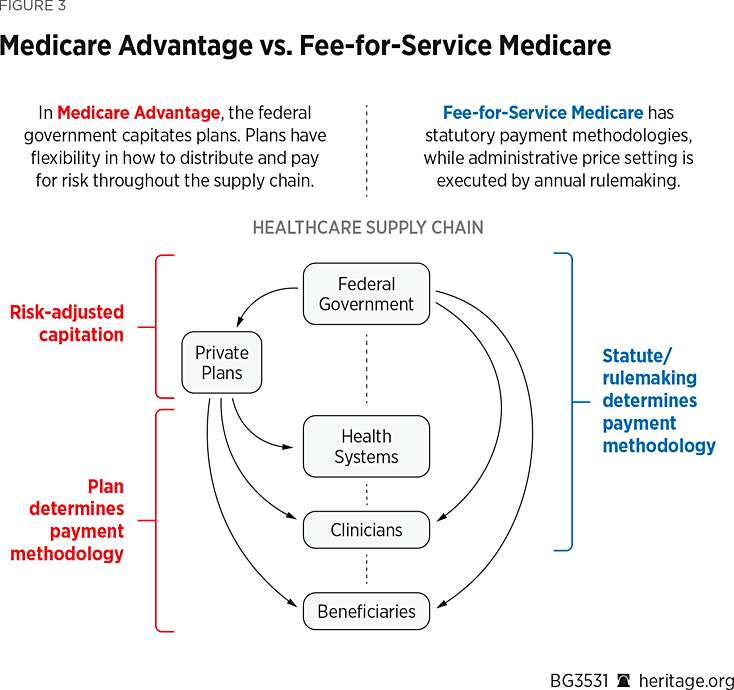
With the ability to be thoughtful in how providers are paid for services, private plans have tools to reduce the delivery system’s focus on intensity and volume of care regulation. Further, a capitated model incentivizes and empowers providers to steer consumers to appropriate care, be it in the form of increased rates of bypass surgery for patients with cardiac disease, lower utilization of emergency rooms,REF or greater utilization of preventive and screening services.REF MA plans may also tier providers, grading providers on performance. Additional cost savings are available to beneficiaries for receiving care from top-tier providers, making tiered networks a tool for steering both consumer and provider behavior towards value.REF
Responsive to the needs of beneficiaries and concerns raised by researchers, policymakers have continued to innovate in MA program design. Historically, researchers have noted that plans preferentially enrolled healthy beneficiaries while higher-cost beneficiaries disenrolled, choosing to elect FFS.REF The MMA responded with SNPs, targeting high-cost beneficiaries with better benefits customization. Further iterations in payment methodology have helped eliminate inappropriate overpayment of plans, with recent research noting that MA payments to hospitals are equivalentREF to or lowerREF than those in the FFS program. Overall spending in MA demonstrates both regional variationREF and marginally lower costsREF and is associated with positive spillover effects in FFS, decreasing county-level per capita FFS expenditures as MA penetration increases.REF
A defined budget for MA plans—based upon risk-adjusted capitation—facilitates budgetary planning on the part of policymakers and provides the CMS a more flexible tool to shape health insurance markets. In contrast, Medicare FFS, deploying administrative price setting without downstream utilization controls, leaves its payer—the CMS—with few mechanisms to budget for or manage health care expenditures on a large scale.
What’s Next? Lessons from Retirement Planning
Congress should change the default auto-assignment from traditional Medicare to MA, a reform advantageous to both beneficiaries and policymakers who desire budgetary planning. Currently, new enrollees are defaulted into traditional Medicare (with penalties for late enrollment), with MA participation requiring an elective, opt-in process. Under today’s model, about 29 percent of new enrolleesREF choose to enroll in MA annually, an increase from 22 percent in 2011.REF In this new model, newly eligible beneficiaries would—by default—be automatically enrolled in MA, with a defined period to change plans or disenroll and elect traditional Medicare should they wish to do so. Plans and programs in both Alabama and New Jersey have already begun exclusively directing coverage of retirees’ benefits to MA plans, resulting in state enrollment increases of 90,000 and 60,000 beneficiaries, respectively, over a single enrollment period.REF
Similar enrollment arrangements in other consumer marketplaces have seen dramatic success in raising participation rates. Long proposed by policy experts,REF retirement plan adoption of automatic enrollment policies drove significant increases in employee participation from 2003 to 2017. By 2017, 63 percent of new plan entrants joined via auto-enrollment, according to plan data from the Vanguard Group, a leading company in 401(k) and defined contribution retirement savings plans. By 2018, plans with an automatic enrollment feature—requiring those not interested to opt out—had a 92 percent participation rate, while those with voluntary opt-in enrollment saw a participation rate of only 57 percent,REF a finding replicated in academic research regarding 401(k) participation by workers across industries.REF
While the principles of auto-enrollment for retirement are applicable, auto-enrollment in health plan products merits special considerations, as access to health care and pharmaceuticals, choice of physicians, and obtaining hospital and emergency care when needed is sharply distinct from the economic problem of saving for retirement. Health—and health care—affects one’s ability to function in the world and is an intensely personal and important choice. Health care utilization, as opposed to retirement costs, is more varied and challenging to predict due to its numerous inputs, including the natural and constructed environment, individual choices, genetics, occupation, and other factors. Health insurance literacy, a well-recognized problem,REF presents further consumer protection challenges to be surmounted.
The Next Generation of Medicare Reform: Changing Default Enrollment
Most individuals find themselves eligible for Medicare when they turn 65 years old and either are required to activate and pay premiums for Part A hospital coverage or, if they have already received Social Security benefits for four months, are automatically enrolled in premium-free Part A coverage.REF Consumers automatically enrolled in Part A are secondarily auto-enrolled in Medicare Part B, while those paying Part A premiums have to elect Part B coverage and pay premiums.REF
Under the proposal to initiate default assignment into MA plans, the pool of individuals newly eligible for Medicare benefits would go unchanged. If new beneficiaries did not select an MA plan or elect FFS Medicare, they would be automatically assigned to an MA plan. This policy change would affect only those who become newly eligible, not those already receiving Medicare coverage. Beneficiaries would retain the ability to delay their Medicare Part B eligibility while continuing commercial coverage through their employers. Default assignment into MA would be initiated upon Part B election or Medicare auto-enrollment if eligible for Social Security. Newly eligible beneficiaries of the multiple populations that make up the Medicare program would be subject to auto-assignment, while special populations such as dual-eligibles would be auto-enrolled in the appropriate SNP.
These authors suggest auto-assignment be an option exclusive to MA plans with a star rating of 3.5 or higher,REF protecting beneficiaries from lower-quality plans while also not overly anchoring the market in favor of incumbent plans. To facilitate this policy change, health plans electing and eligible to participate in auto-assignment would be required to offer at least one zero-premium,REF basic coverage plan providing minimum Part A, B, and D benefits. These requirements would level the playing field among the health plans competing for the same beneficiaries, with the January to March open-enrollment period providing beneficiaries an opportunity to change plans. Additional criteria would need to be defined to ensure that beneficiary preferences, including provider choice, would be appropriately factored into the assignment process.REF Finally, beneficiaries who remain unsatisfied with the available choices in the MA marketplace would be able to disenroll into FFS during the existing standard annual disenrollment period from January 1 through February 14.
Several health insurance markets support this precedent. In states such as New Mexico and New York, Medicaid beneficiaries who become newly eligible for Medicare are auto-assigned to D-SNP plans, which have customized benefits for dual-eligibles. Other beneficiaries with pre-existing commercial coverage can be auto-assigned to a like-plan product (e.g., HMO to HMO or PPO to PPO) within the same parent organization, ensuring preservation of their existing provider relationships. Managed Medicaid markets also deploy auto-assignment to promote both a relationship with a primary care physician and a managed care plan, providing lessons for the MA marketplace.REF For example, Nebraska’s managed Medicaid program, Heritage Health, utilizes equitable auto-assignment, preserves primary care physician relationships, and additionally combats health insurance literacy challenges by preferentially auto-enrolling members in the same plan if a household member is already enrolled.REF
Policymakers have multiple routes for implementation. CMS Innovation Center waiver authority (Section 3021 of the ACA) would facilitate modification of the enrollment process and creation of an innovation center model with a population targeting all Medicare beneficiaries. Alternatively, Congress could enact statutory change, tying auto-enrollment in MA to the Part A auto-enrollment and Part B benefit-election processes.
Consequences of implementation are varied. Beneficiaries would gain greater financial protections along with supplementation benefits in exchange for some network access and utilization controls while still retaining the ability to elect into FFS. Uniform access to supplemental benefits would promote health plan innovation in benefit design. Health plans would gain market share in the Medicare marketplace due to auto-enrollment, further incentivizing development of care management programs. It would broaden the actuarial risk pool, as the vast majority of new Medicare beneficiaries would be enrolled in MA.REF Policymakers would obtain improved budgetary forecastingREF and new levers for budgetary control, as auto-enrollment would increase the penetration of risk-adjusted, capitated plan products in the Medicare marketplace. Thus, Congress’s and the CMS’s focus would shift to modifying future spending and adjusting capitation rates and risk-adjustment methodologies as opposed to administrative price setting of individual services as exists in FFS. Furthermore, by increasing the use of MA, policymakers would continue the healthy shift of medical necessity, formulary design, and benefits design to health plans, continuing to shift the CMS from its role as a FFS health plan operator to a market regulator.
Even without this change, participation in MA has more than doubled over the past decade: In 2020, two in five Medicare beneficiaries, comprising over 23 million individuals, enrolled in an MA plan. The Congressional Budget Office now projects that 47 percent of Medicare beneficiaries will get their coverage from MA plans by 2029, noting that the program grew 71 percent since the passage of the ACA.REF The growth of MA emphasizes the need for policy innovation and subsequent statutory change in other areas of program design, such as MA’s bidding system, which is anchored in FFS benchmarks.REF
Conclusion
The transition to value in the health care system necessitates comprehensive changes in the way care is financed and delivered. Enacting statutory change to allow auto-assignment of beneficiaries into MA plans marks the next step on the path to value. Doing so would provide policymakers with better levers for spending control while facilitating value-based development and innovation in supplemental benefit design, helping taxpayers and beneficiaries alike. Finally, by fixing financing first, policymakers can facilitate the transition of the largest health plan market—the Medicare program—to a defined contribution by way of a risk-adjusted, capitated financing model.
MA is a market-tested, federally protected, and innovative marketplace with the potential to provide better health care. It is up to Congress to deploy it to its full potential.
Brian J. Miller, MD, MBA, MPH, is a hospitalist and public health physician. Gail Wilensky, PhD, is a Senior Fellow at ProjectHope and former CMS administrator. The authors are grateful for and would like to acknowledge Jennifer M. Slota for her research and editorial assistance.



