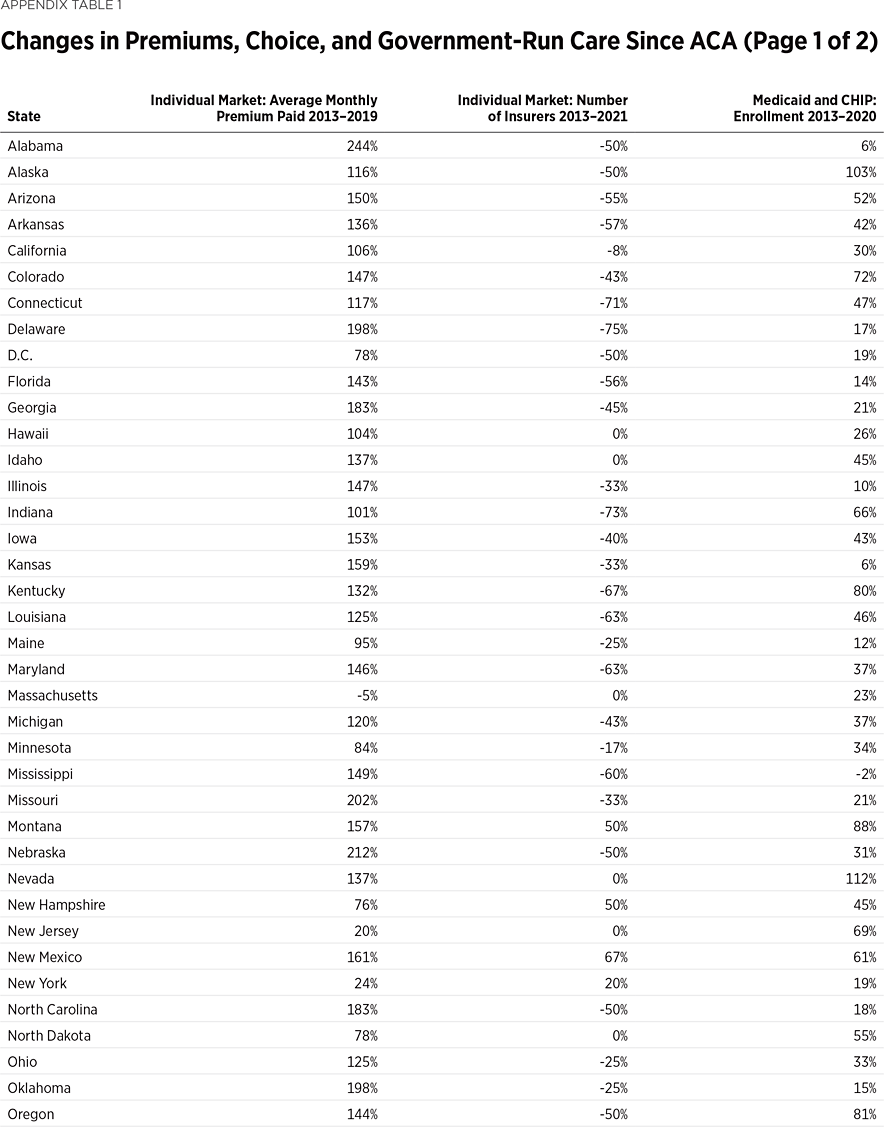
This year marks 11 years since the passage of the Affordable Care Act (ACA)—also known as Obamacare—and seven years since its key elements took effect. In that time, health insurance premiums spiked, coverage options fell, and more Americans became dependent on government-run health care. This Backgrounder examines the changes in these three areas—premiums, choice, and government-run care—and outlines ways that Congress can reverse this trend. (For a summary of changes in all three metrics, see Appendix Table 1.)
Rising Health Insurance Premiums in the Individual Market
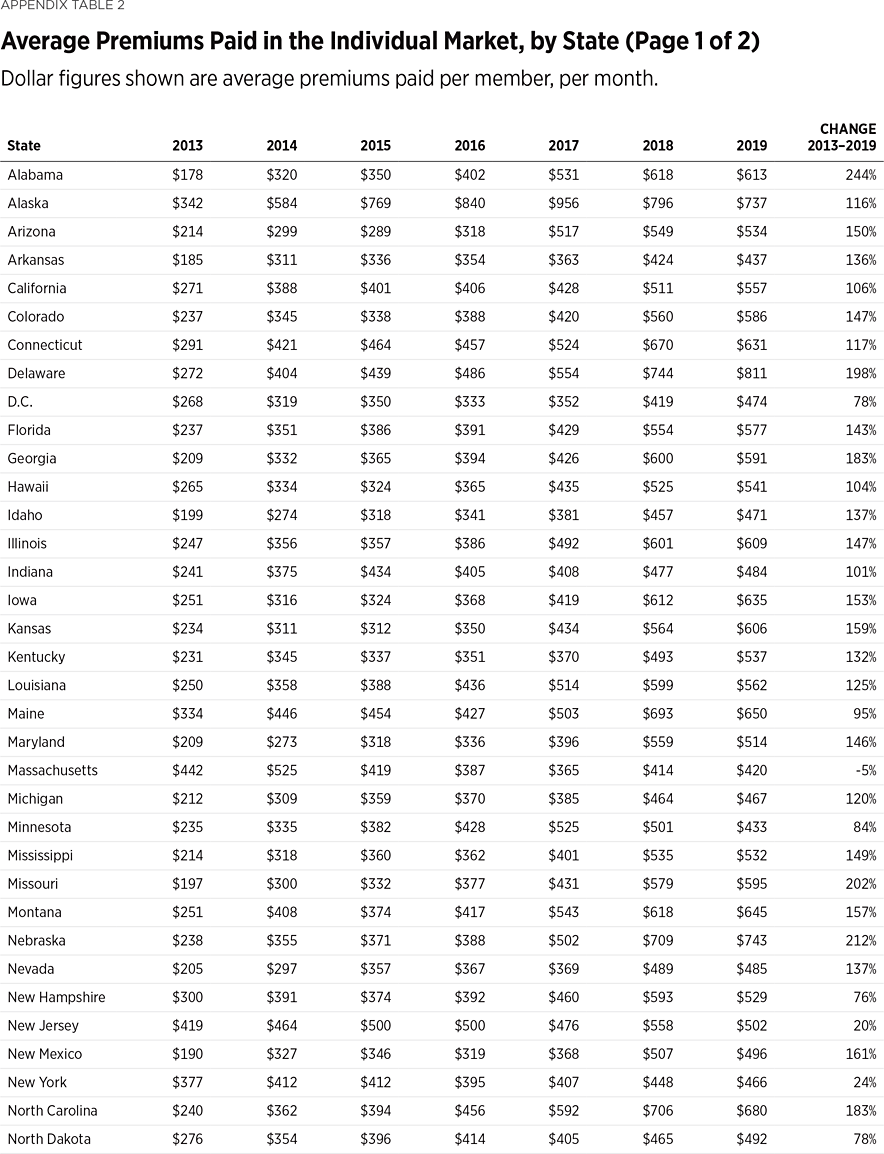
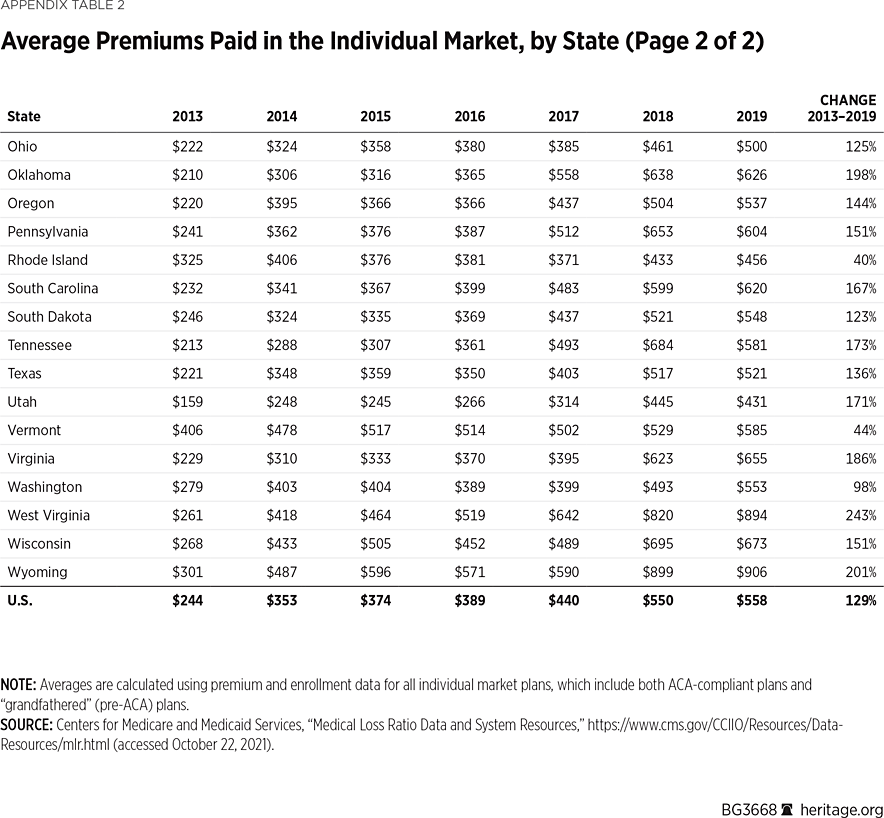
Comparing premium changes in the individual market before and after the ACA is a key measure of the law’s financial effect on consumers. In 2013, the national average premium paid in the individual (non-group) market was $244 (per member, per month).REF In 2019, the national average premium paid in the individual market was $558 (per member, per month). This is a 129 percent increase from 2013 to 2019.REF Over the same period in the large-employer market, national average premiums paid per member per month grew by only 29 percent (from $363 to $558).REF This means premiums for individual market coverage under the ACA effectively doubled between 2013 and 2019.
Premium changes varied by state. (See Appendix Table 2.) In nearly every state, consumers on average paid higher premiums under the ACA. In 40 states, the average monthly premium for individual-market coverage more than doubled by 2019—and it more than tripled in five of them (Alabama +244 percent, Nebraska +212 percent, Missouri +202 percent, West Virginia +243 percent, and Wyoming +201 percent). States with the smallest premium increases over this period—New Jersey (+20 percent), New York (+24 percent), Rhode Island (+40 percent), and Vermont (+44 percent)—were ones that had imposed costly regulations on their individual markets before the ACA and consequently already had high average premiums in 2013. Only one state, Massachusetts, saw a decline (–5 percent) in average premiums paid over this period. That was because almost all the ACA’s new mandates and regulations, along with a similar set of income-related subsidies, were already in place in the Massachusetts individual market before the ACA took effect. Massachusetts was the state with the highest average monthly premium pre-ACA ($422 in 2013).
Higher Deductibles
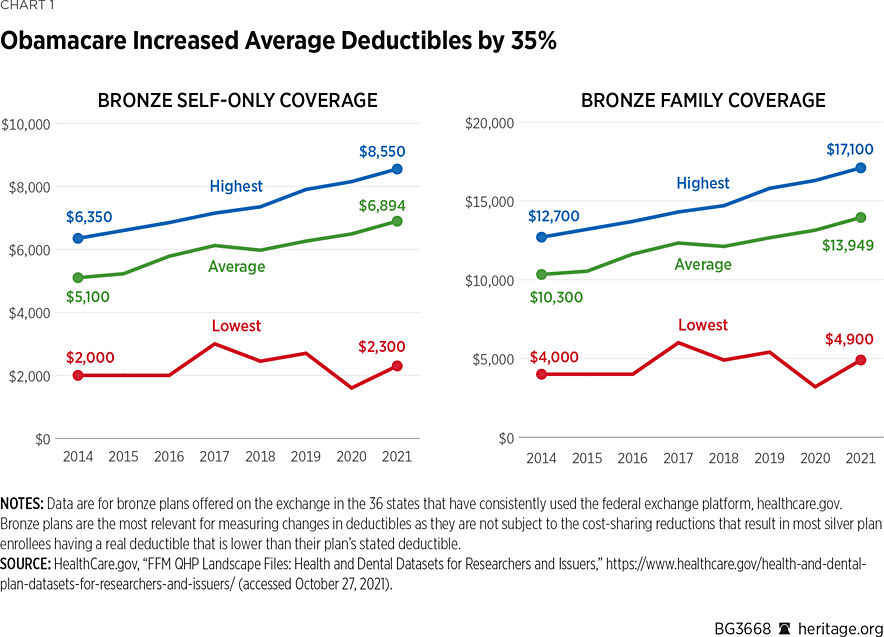
At the same time that premiums more than doubled in the individual market, deductibles for ACA-compliant coverage also significantly increased.REF Deductibles for bronze-level plans sold on the federal exchange increased by more than one-third (35 percent) under the ACA. For self-only coverage, deductibles rose from an average of $5,100 in 2014 to $6,894 in 2021, while the average deductible for family coverage increased from $10,333 in 2014 to $13,949 in 2021.REF (See Chart 1.)
Narrower Networks
While Obamacare enrollees have been paying more in premiums and out-of-pocket costs, their access to medical providers has also been shrinking. During the 2014 plan year, 44 percent of bronze plan offerings had more restrictive provider networks,REF but by 2021 that figure has increased to 84 percent. Silver plans experienced the same effect, moving from just 43 percent of the plans having more restrictive networks in 2014 to 85 percent of plan designs in 2021.REF (See Chart 2.)
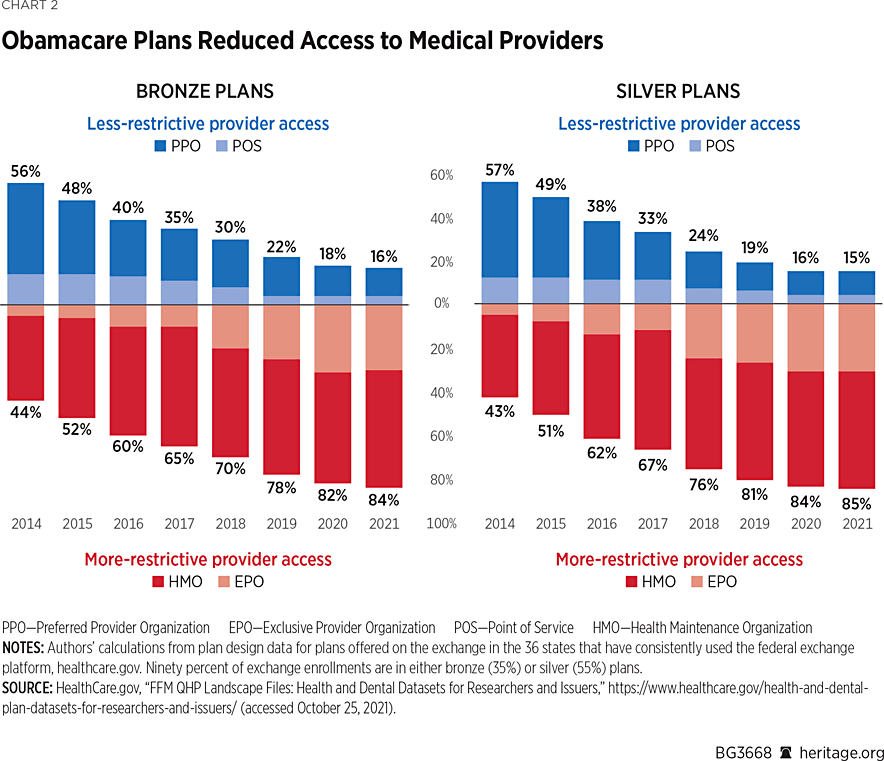
Insurers have essentially responded to the higher claims costs resulting from Obamacare’s regulations by increasing premiums and enrollee cost sharing while narrowing the networks of providers that their plans will reimburse.
The result: enrollees with Obamacare coverage have been paying more while getting less access to doctors and hospitals.
This is anomalous to both employer-group health insurance plans and the pre-ACA individual market. Prior to Obamacare, insurers generally offered—and customers generally expected—a rough trade-off in plan design to provide customers value for their purchase. Typically, plans with higher out-of-pocket costs offered a broader choice of providers, while plans with limited provider choice offered lower out-of-pocket costs. However, Obamacare has managed to force insurers into offering plans characterized by both limited provider choice and high out-of-pocket costs.
Fewer Choices and Less Competition in the ACA Exchanges
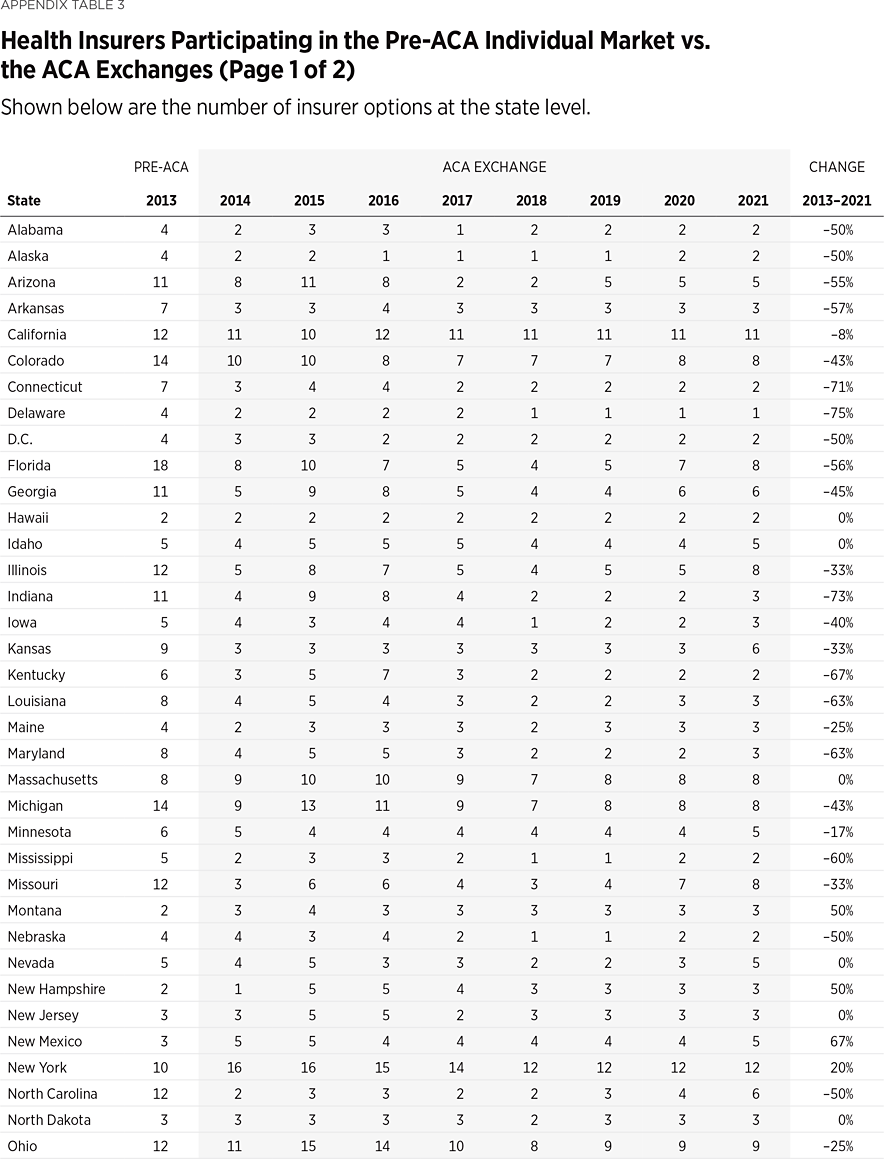
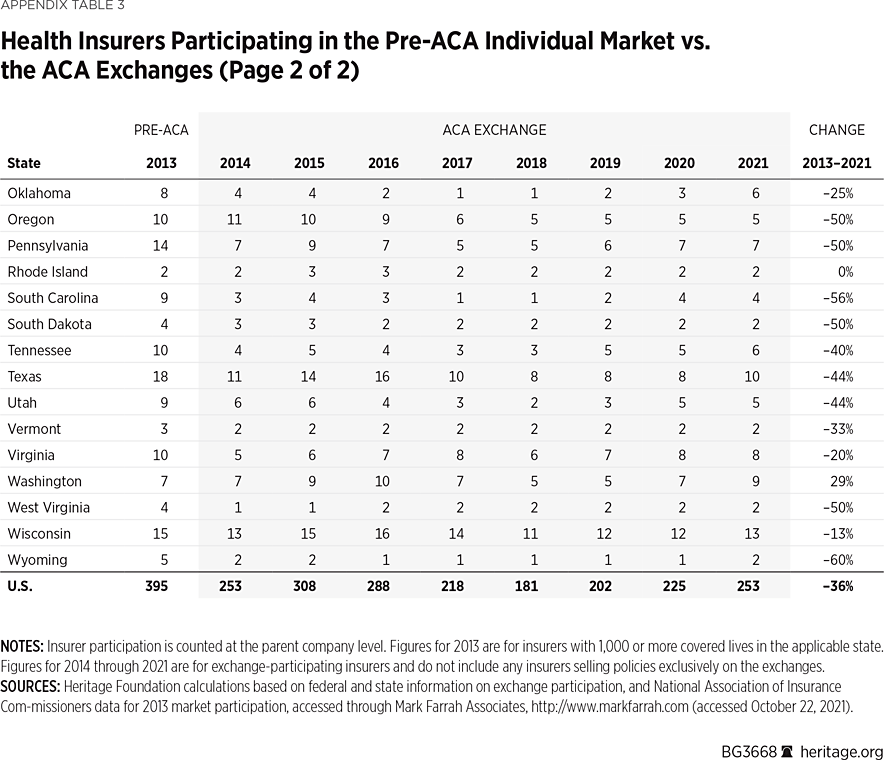
As consumers paid higher premiums and experienced narrower networks, fewer insurers offered plans on the ACA exchanges. Individual insurance markets are about one-third less competitive than they were before the ACA took effect.REF In 2013, there were 395 insurers offering coverage in the individual market at the state level. By 2018, insurer competition had fallen by more than half (54 percent), with only 181 insurers offering coverage on the Obamacare exchanges, and there were eight states in which only one insurer offered exchange coverage that year. Over the past three years, insurer competition has partially rebounded in response to steps the Trump Administration took to stabilize the market. In 2021, there are 253 insurers offering exchange coverage, though this is still 36 percent fewer than before the implementation of Obamacare.
Appendix Table 3 displays the percentage change in insurer competition in the 2013 individual market and the 2021 ACA exchanges, by state. In 2013, there was no state that had fewer than two insurers offering coverage, and two states (Florida and Texas) had 18 insurers offering coverage. Despite insurers reentering the exchanges in recent years, for 2021 Delaware still has only one insurer offering exchange coverage, and 12 states and the District of Columbia still have only two insurers offering exchange coverage. Only five states have more insurers participating in their exchange in 2021 than they had offering coverage in their individual market in 2013.REF
Greater Dependence on Government Coverage
Not only did the ACA increase the cost of private coverage and reduce its availability; it also significantly expanded government-run coverage through Medicaid. Historically, Medicaid provided health care coverage to the vulnerable poor: children, pregnant women, the elderly, and people with disabilities. The ACA, however, expanded the scope of eligibility to include lower-income able-bodied adults, predominantly those without dependent children. Furthermore, the ACA offered states a much higher level of federal financing for this new population (100 percent in the first three years, eventually declining to 90 percent over subsequent years) than for their existing Medicaid populations.REF
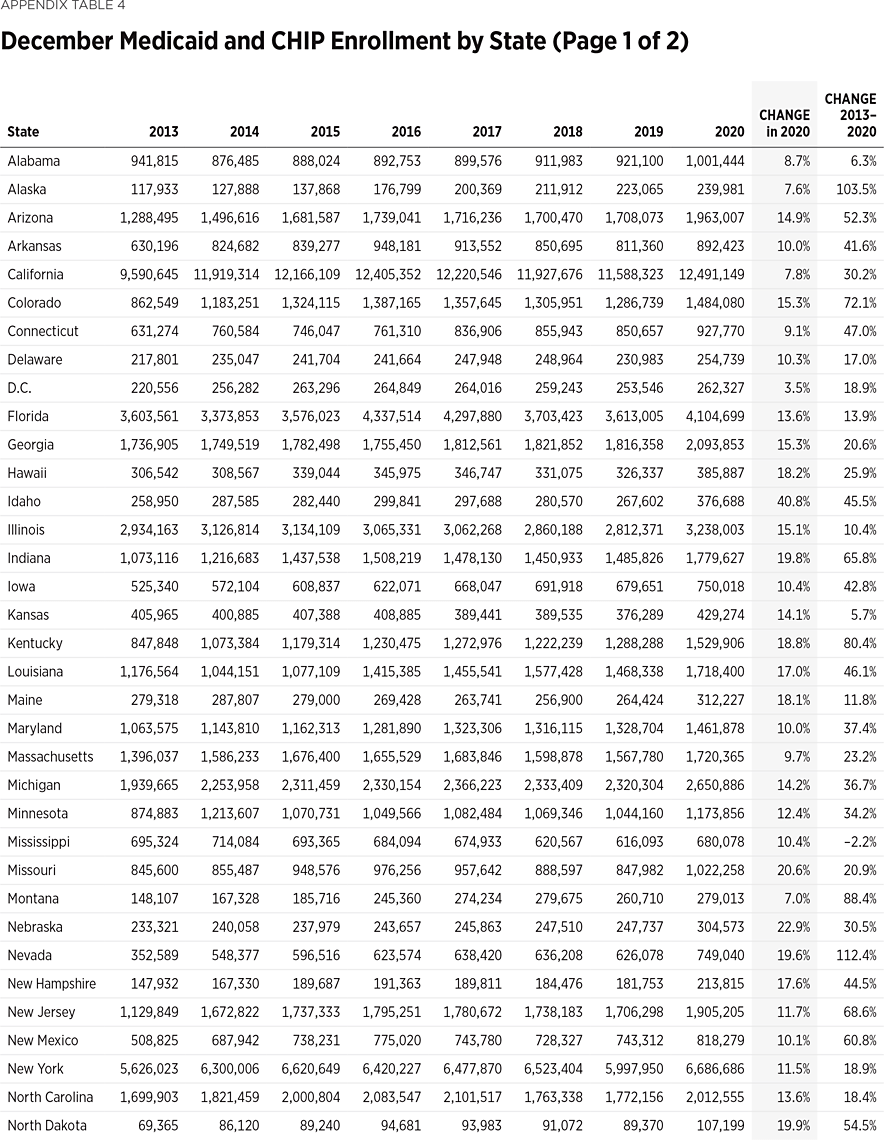
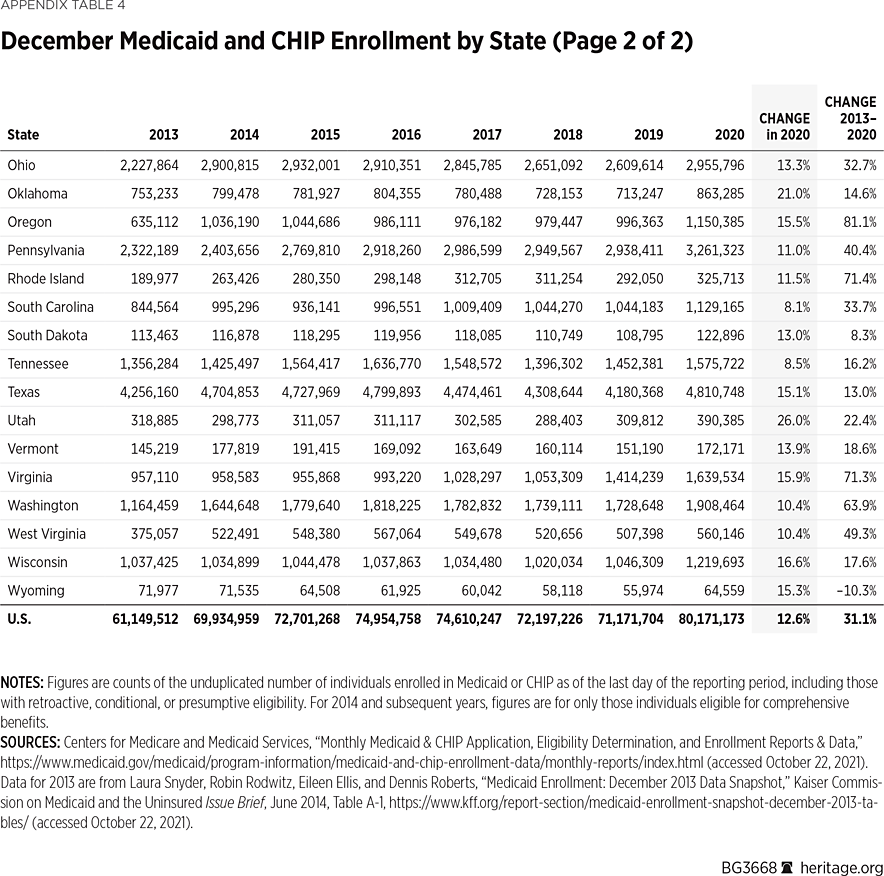
Between 2013—the last year before the ACA took full effect—and 2019, enrollment in Medicaid and the Children’s Health Insurance Program (CHIP) increased by 10 million individuals.REF Enrollment in those programs jumped by a further 9 million individuals in 2020.
The 2020 sharp increase was largely due to effects of the COVID-19 pandemic. When governments responded to COVID-19 by imposing restrictions on businesses and the public, the resulting adverse economic impacts fell disproportionately on industries that employ more low-wage workers, such as hospitality, personal services, and retail. Consequently, lower-income workers were more likely to suffer economic dislocation and seek assistance from safety-net programs. Also, in March 2020 Congress enacted a temporary increase in federal funding for state Medicaid programs conditioned on states continuing to cover, for the duration of the health emergency, all individuals who were already on Medicaid. In December 2013, national Medicaid and CHIP enrollment was 61.1 million. By December 2020, 80.2 million people were enrolled in Medicaid and CHIP—an increase of 31.1 percent from 2013 and of 12 percent from the end of March 2020 (the start of the widespread national COVID-19 response).REF
Due to the effects of the COVID-19 response, all states and the District of Columbia experienced increased Medicaid enrollment in 2020. (See Appendix Table 4.) While the increases varied by state, Medicaid enrollment surged in both expansion and non-expansion states. For instance, while both California and New York adopted the ACA Medicaid expansion, neither Texas nor Florida have done so. In 2020 Medicaid enrollment jumped in all four states, growing by 903,000 individuals in California; 689,000 in New York; 630,000 in Texas; and 492,000 in Florida.
Health Care Choices: A Plan to Lower Premiums, Increase Choice, and Protect the Vulnerable
The ACA led to higher premiums, fewer choices, and greater government dependence. To reverse these consequences, policymakers need to provide relief from the ACA mandates that contributed to the problem. As a start, the Trump Administration provided new flexibilities to mitigate some of these issues. A critical step included changes to regulations implementing the law’s Section 1332 waivers, which allow states to seek waivers from certain federal ACA requirements.REF The results, thus far, are encouraging.REF
Seven states had 1332 waivers in effect by 2019, and five additional states were approved to implement waivers in 2020.REF In the initial seven states, first-year premium reductions (relative to projected rates) ranged from 6 percent (Oregon) to 43.4 percent (Maryland), with an average reduction of 19.9 percent across the seven states.REF All five states with waivers taking effect in 2020 projected similar premium reductions.REF
Given the proven relief that waivers provide from high premiums, policymakers in other states should consider similar waivers.
However, more needs to be done. Congress should build on the Trump Administration’s regulatory changes and provide additional relief from the ACA’s burdensome and costly regulations.
One such approach, the Health Care Choices Proposal,REF would do just that. Under the proposal, Congress would eliminate key regulations that led to increased costs and reduced the ability of private companies to offer products people want to buy. It would also change another key aspect of Obamacare that led to higher costs and reduced choices: the current ACA subsidy structure that gives taxpayer dollars to insurance companies and increases those subsidies as insurance companies raise premiums.REF Instead, states would receive that funding in the form of grants to help the low-income and those with pre-existing conditions access coverage. Finally, unlike Obamacare (which put most subsidized individuals on Medicaid), subsidized individuals would be able to apply their subsidy dollars toward private coverage of their choice.
The Center for Health and Economy estimated that the Health Care Choices Proposal would lower premiums by as much as 24 percent and result in nearly 4 million more people purchasing insurance by 2030, with more people enrolling in private coverage versus public insurance over the same period.REF
Conclusion
Since taking effect, the ACA more than doubled premiums in the individual market while cutting the number of participating insurers by one-third. It also led insurers to raise plan deductibles and narrow their provider networks while at the same time significantly increasing the number of people dependent on government-run health care. To reverse those trends, Congress should build on promising improvements made possible by the Trump Administration’s deregulatory agenda and consider the Health Care Choices Proposal, which would lower costs, increase choices, and protect the vulnerable.
Edmund F. Haislmaier is the Preston A. Wells, Jr. Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Abigail Slagle is a Research Associate in Domestic Policy Studies.