Created in 1965, Medicaid is joint federal–state program that aims to provide health care services to certain low-income individuals. The federal government sets broad rules for the program, but states are generally responsible for its administration and implementation. Eligibility, benefits, and financing vary by state, and states make use of existing flexibilities, like those offered through waivers, to tailor their own Medicaid programs. As a result, no two Medicaid programs are alike.
Looking ahead, the number of people on the program is growing; the diversity of those enrolled is expanding; the services provided to those who are enrolled are changing; and spending continues to trend upward, driving up costs at the state and federal levels. Competing beneficiary priorities, an outdated administrative structure, and a flawed financing model put the program’s future at risk.
Instead of undermining this federal–state partnership with a one-size-fits-all federal approach, as proposed under various Medicare for All proposals,REF Congress should ensure that states have the necessary flexibility to meet new and changing demands.REF In addition, Congress should take necessary steps to address the larger, more fundamental challenges that jeopardize the future of the program. Specifically, Congress should improve eligibility standards to protect the program for those who are in need, allow benefits to match the diverse makeup of enrollees more precisely, and restructure the program’s financing to target resources and dollars more effectively.
The Basics
Congress created the Medicaid program in 1965.REF The program provides federal grants to the states to provide health care services to certain low-income individuals.
The costs for providing these services are shared between the federal government and each state. States must agree to meet certain federal requirements for eligibility, benefits, and financing and have latitude within those requirements to administer their own programs. State participation in the Medicaid program is voluntary, and all states participate.REF
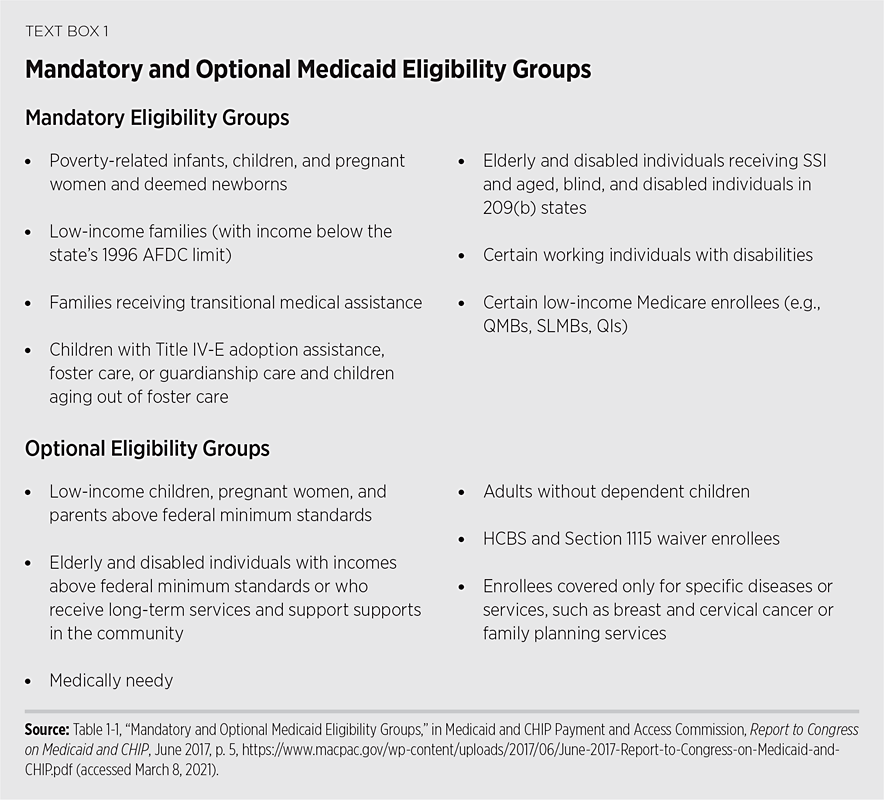
Eligibility. Federal rules outline the groups and income thresholds that states are required to adopt in order to receive federal funds for the program. These mandatory eligibility groups generally fall into one of four categories: children, pregnant women, people with disabilities, and people over the age of 65. Federal rules also outline additional groups that states can make eligible on a voluntary basis. These optional populations typically are an extension of the federal minimum mandatory standards or for disease-specific groups. (See Text Box, “Mandatory and Optional Medicaid Eligibility Groups.”)
An analysis of enrollment based on fiscal year (FY) 2013 data found that 71.1 percent of beneficiaries enrolled in Medicaid were mandatory populations and 28.9 percent were optional populations. Children made up the largest share of mandatory enrollees (39.6 percent), and adults accounted for the largest share of optional enrollees (16.1 percent).REF
Benefits. The federal government also outlines a set of benefits that states are required to adopt in order to participate in the program. States are required to offer these mandatory benefits to both mandatory and optional populations. Mandatory benefits include services such as physician services, inpatient and outpatient hospital care, and laboratory services. As with the eligibility rules, the states may also offer additional benefits and services beyond the federal minimum requirements. These optional benefits include benefits and services such as prescription drugs, dental services, and physical and occupational services. (See Text Box, “Mandatory and Optional Medicaid Benefits.”)


An analysis of spending based on FY 2013 data found that:
- 47.4 percent of Medicaid spending was on mandatory benefits for mandatory enrollees,
- 21.1 percent was on optional benefits for mandatory enrollees,
- 16 percent was for mandatory benefits for optional enrollees, and
- 15.5 percent was for optional benefits for optional enrollees.REF
Financing. Federal and state governments share the cost of the Medicaid program. The Federal Medical Assistance Percentages (FMAP) formula calculates the federal allocation each year for the states based on each state’s income levels.REF The federal contribution levels range from a minimum of 50 percent to a maximum of 83 percent.REF For FY 2022, 12 states received the minimum federal match rate of 50 percent, and one state—Mississippi—received a 78.3 percent rate, the highest federal match rate for FY 2022.REF (See Table 1.)
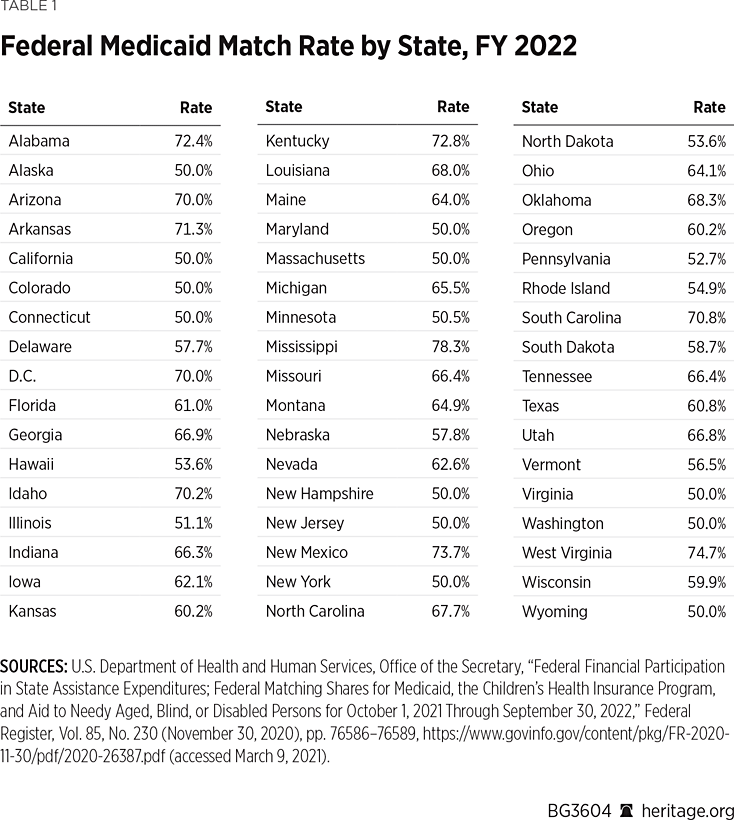
Beyond the traditional match rate, there are instances in which the federal government assumes a higher share of the costs.REF For example, states receive an “enhanced” federal contribution for enrollees in the Children’s Health Insurance Program (CHIP), for able-bodied enrollees made eligible under the Affordable Care Act, and for other stand-alone services such as breast and cervical cancer screening and family planning services. States also receive federal supplemental payments to offset other provider costs.REF
Key Trends
Enrollment, spending, and financing trends illustrate how the program has changed over time.
Enrollment Trends. According to the Office of the Actuary at the Centers for Medicare and Medicaid Services (CMS), total Medicaid enrollment has grown from 34.5 million in 2000 to an estimated 73.4 million in 2017 and a projected enrollment of over 82 million by 2027.REF In 2000, low-income children accounted for 16.1 million, adults accounted for 6.9 million, individuals with disability accounted for 6.9 million, and elderly individuals accounted for 3.6 million enrollees. (See Chart 1.)
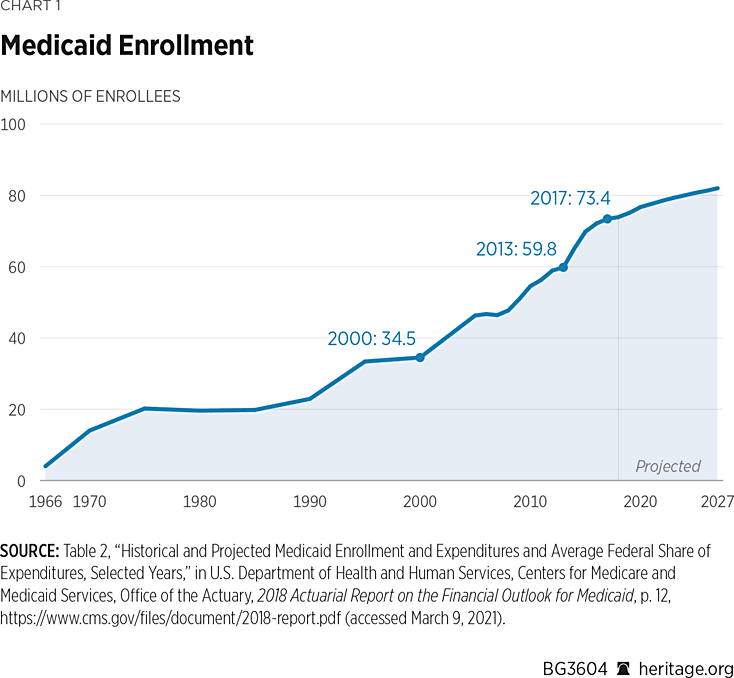
Enrollment surged among able-bodied adults after passage of the Affordable Care Act (ACA)REF when states were given the optionREF and additional federal fundingREF to add a new eligibility group—able-bodied childless adults with income levels below 138 percent of the federal poverty level (FPL)—to their programs. Enrollment for this new group grew from 4.3 million in its initial year to an estimated 13.2 million in 2020.REF By 2027, enrollment of adults (including the ACA expansion groups) will nearly match the enrollment of children: 29.9 million to 31 million, respectively.REF
Spending Trends. As with enrollment, spending on the Medicaid program has climbed sharply. According to the CMS Office of the Actuary, total spending (federal and state) was $206.2 billion in 2000 ($117 billion federal and $89.2 billion state); estimated at $600 billion in 2017 ($370 billion federal and $229.9 billion state); and projected to reach $1 trillion by 2027 ($624.8 billion federal and $383 billion state).REF (See Chart 2.)
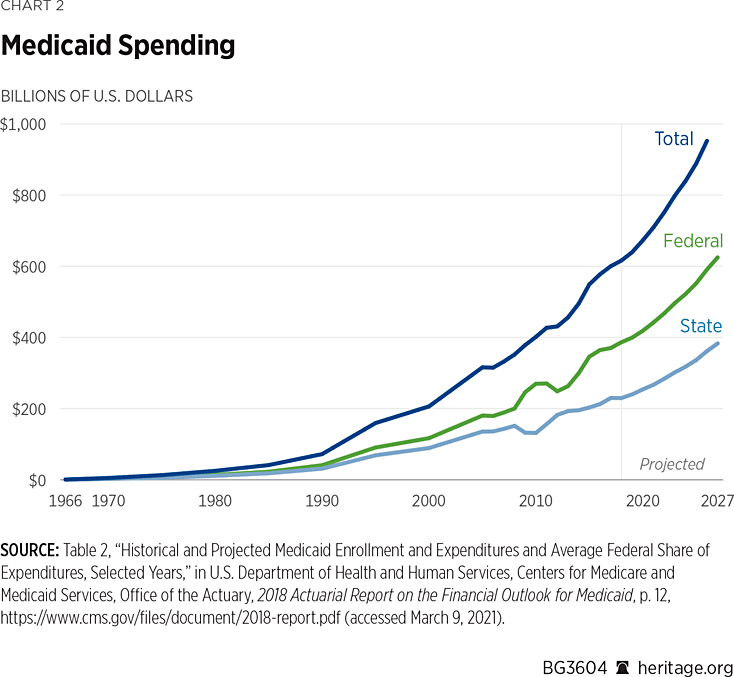
While children and adults make up the largest share of the enrollment, over half of all Medicaid spending is for services provided for the aged and disabled. In 2017, the aged and disabled made up 23 percent of total enrollment and accounted for 53 percent of spending, whereas children and adults made up 78 percent of total enrollment and accounted for 46 percent of spending.REF
Most Medicaid spending for services has shifted from fee-for-service payment to Medicaid managed care plans.REF
- In FY 2007, fee-for-service payments for acute care services such as physician services accounted for 41 percent of Medicaid expenditures, fee-for-service payments for long-term care services such as nursing homes accounted for 32 percent, capitated payments to managed care and other health plans accounted for 21 percent, and uncompensated care payments accounted for 5 percent.REF
- In FY 2017, capitated payments to managed care and other health plans accounted for 52 percent of Medicaid expenditures, fee-for-service payments for acute care services accounted for 25 percent, fee-for-service payments for long-term care services accounted for 20 percent, and uncompensated care payments accounted for 3 percent.REF
Financing Trends. With spending and enrollment trending upward, financing of the program is changing as well. Total Medicaid spending, federal and state, is expected to reach $1 trillion and 3.3 percent of GDP by 2027.REF
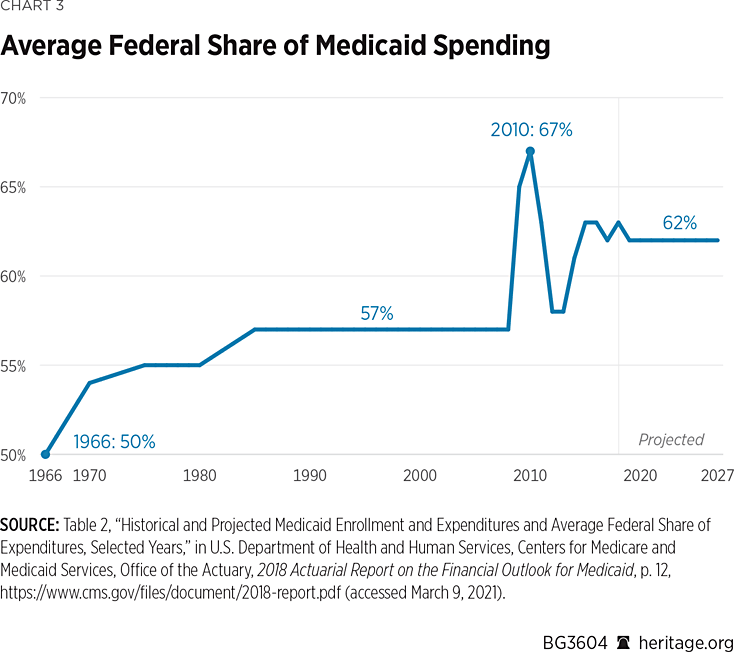
Historically, the average federal share of Medicaid spending has been 57 percent. (See Chart 3) Yet congressional intervention, most notably the ACA expansion, as well as other temporary boosts such as during economic recessions and the recent COVID response have shifted the federal share upward.REF At the same time, Congress routinely postpones the implementation of legislation requiring federal payment reductions (for example, the ongoing delay of uncompensated care cuts).
State dependence on federal resources is also growing.
- In FY 2000, state Medicaid spending accounted for 19.5 percent of state budgets,REF of which 56.7 percent was federal funds, 35.5 percent was state general funds, and 7.8 percent was from other state sources.REF
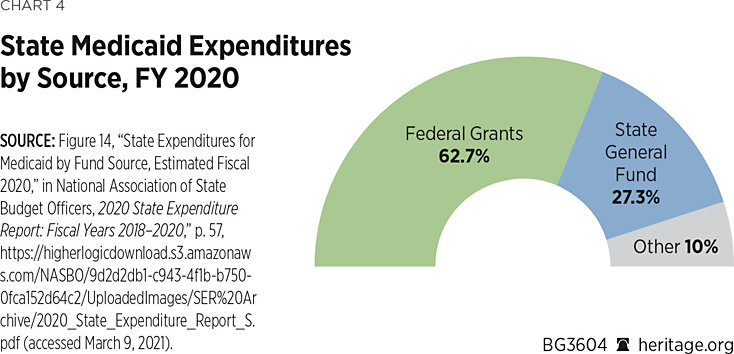
- In FY 2020, Medicaid spending made up 28.6 percent of state spending, but of that amount, 62.7 percent was the federal share, 27.3 percent was from state general funds, and 10 percent of funding for Medicaid came from other state funding mechanisms, such as taxes on Medicaid providers.REF (See Chart 4.)
The Role of Waivers
States are able to make adjustments in their Medicaid programs on an ongoing basis. The states submit their plans through state plan amendments (SPAs) to the Centers for Medicare and Medicaid Services (CMS) at the Department of Health and Human Services (HHS) for review to ensure that their plans meet the federal rules and requirements to qualify for federal matching funds.
Beyond these individualized state plans, states can also request that the Secretary of Health and Human Services waive certain Medicaid requirements. These waivers offer states additional flexibility to design and tailor their programs.
Waivers are time limited, typically approved for five years, but can be and often are renewed.REF Waivers must be budget neutral, which means that federal costs can be no more than would otherwise have been expected.REF States are also required to submit periodic evaluations and reports to CMS to ensure that their waivers are meeting the state-specific terms and conditions set forth in the agreement.
There are several types of waivers: some broad and some targeted.REF Section 1115 waivers allow the Secretary of HHS to waive a wide range of requirements and are typically viewed as the broadest waivers available to the states. States use these demonstration and research waivers to experiment with new ways of administering their Medicaid programs.
Waiver Trends. Waivers, in particular Section 1115 waivers, are used to advance a variety of initiatives at both the federal and state levels. At the federal level, Administrations use waivers to advance and emphasize their own policy goals. For example:
- The Bush Administration initiated demonstration waivers to promote private health insurance for the uninsured and to promote greater adoption of consumer-directed care models, such as cash and counseling;
- The Obama Administration used waivers to encourage eligibility and benefit expansions as well as to test new ways to deliver services; and
- The Trump Administration used waivers to encourage those who could work to work as a condition of receiving benefits and to support innovative financing arrangements such as block grants and consumer-based health accounts.
At the state level, waivers are being used to make a wide range of changes in state Medicaid programs. Based on analysis and descriptions by the Kaiser Family Foundation, as of February 25, 2021:REF
- Forty-five states had requested waivers related to behavioral health services;
- Thirty had requested waivers to make changes in targeted eligibility requirements, such as implementing more frequent eligibility verification;
- Nineteen had requested waivers for delivery system reforms;
- Nineteen had requested waivers related to work requirements;
- Sixteen had requested waivers related to eligibility and enrollment restrictions;
- Fifteen had requested waivers related to managed and long-term care;
- Fifteen had requested waivers related to benefit restrictions, copayments, and healthy behaviors; and
- Two had requested waivers related to financing of their programs.
Challenges Ahead
Given its current trajectory, the Medicaid program faces significant demographic, structural, and financial challenges. Competing beneficiary priorities, a cumbersome and outdated administrative structure, and a flawed financing model are weakening the foundation of the program.
Competing Beneficiary Priorities. Years of incremental policy changes have changed the face of the program, and Medicaid’s diverse makeup creates internal tensions within the program.
Historically, low-income children have been the core of Medicaid and make up the bulk of the program’s enrollees. Yet changes in eligibility and funding, especially under the ACA, have resulted in a notable increase in enrollment among able-bodied adults who can work. The enhanced federal funding to the states for able-bodied adults creates a perverse financial incentive for the states to focus on enrolling newly eligible able-bodied adults at the expense of other eligibility groups.
Moreover, as noted, low-income aged and disabled individuals make up a quarter of Medicaid program enrollment but account for over half of program spending. This imbalance sets competing priorities for the states, which must decide whether to concentrate their attention on addressing the needs of the “low-cost” majority or the “high-cost” minority.
Outdated Administrative Structure. The growing dependence on waivers for administration of the Medicaid program is a clear indication that the program’s underlying administrative framework is outdated and lacks sufficient statutory flexibility.
The waiver process itself is also slow and uncertain. Despite the recent acceleration of the federal government’s review and approval process, the process for obtaining, adjusting, and maintaining a waiver is still cumbersome and time-consuming. In addition, the Biden Administration has taken the unprecedented step of reopening previously approved waivers to which the states and the federal government had mutually agreed.REF This action erodes confidence in the process and leaves states in policy limbo.
Flawed Financing Model. The Medicaid financing model is not ideal. The program’s open-ended design incentivizes states to expand the size and scope of their programs. Because there is no cap on total spending under Medicaid, the more a state spends, the more the federal government is obligated to pay the state.
Furthermore, trends in increasing the federal share create a perverse financial incentive for the states. The ACA enhanced federal funding for abled-bodied adults, for example, rewards states that enroll newly eligible able-bodied adults at the expense of other eligibility groups.
As costs grow and other state priorities such as education and public safety put pressure on state budgets, state dependence on the federal Medicaid dollars becomes much more acute. This leads states to look for ways to shift costs to the federal ledger, maximizing federal contributions and minimizing state obligations wherever possible.REF
Next Steps
Congress should understand the underlying trends and challenges and make necessary changes to ensure that the states can adjust to the growing demographic, structural, and financial challenges facing the Medicaid program. In addition, when appropriate, Congress should look to recent waivers and government audits to draw on the lessons for reform. Specifically, Congress should consider the following actions:
- Improve eligibility standards to protect those in need. As enrollment continues to grow, it is imperative that there are appropriate and accurate eligibility standards to ensure that the program remains focused on serving those in need. To this end, Congress should:
- Hold states accountable for improper eligibility determinations. The Office of the Inspector General at HHS has conducted a series of ongoing state audits and found that some states made Medicaid payments on behalf of individuals who were not eligible for the program.REF Congress should conduct better oversight of these eligibility errors and direct CMS to move more aggressively to hold states financially accountable for improper eligibility determinations.
- Roll back presumptive eligibility expansions and require more regular eligibility redeterminations. The ACA loosened certain requirements for determining Medicaid eligibility. Since then, some states have proactively requested and received federal waivers to scale back those allowances and have shifted to more frequent eligibility redeterminations in order to protect against improper enrollment. Congress should narrow federal presumptive eligibility rules and require that the states conduct more regular eligibility redeterminations to ensure that ineligible individuals are unenrolled in a more timely fashion.
- Narrow retroactive eligibility. Current law requires Medicaid to pay the costs of services provided to a newly eligible individual retroactively. Broad look-back periods are not consistent with other welfare program rules. For example, neither food stamps nor housing subsidies operate on such a retroactive basis. While states have received waivers to curb these look-back requirements, Congress should tighten the retroactive eligibility requirements statutorily.
- Strengthen asset test determinations within Medicaid. The ACA streamlined Medicaid income determination rules. This new standard, however, does not require an asset test. Stronger asset tests and enforcement would protect the program for those who need it most. Congress should add asset test requirements to its eligibility calculation and require states to enforce such tests more vigorously.
- Allow benefits to match the needs of beneficiaries more precisely. The changing makeup of the program means that the states should have the flexibility to tailor their benefits accordingly. To this end, Congress should:
- Expand premium support options for beneficiaries. Given the diverse needs of the Medicaid population, beneficiaries should be allowed to apply the dollars that otherwise would have been spent on them through the traditional Medicaid structure to a private coverage option of choice. While states currently have some flexibility to allow premium support in Medicaid, Congress should remove burdensome requirements that act as barriers to making it more widely available to enrollees.
- Broaden the application of targeted premiums and cost sharing. Not all Medicaid enrollees are the same. In some states, eligibility can exceed the federal poverty level. Several Administrations, both Republican and Democrat, have permitted states to vary premium and cost-sharing responsibilities based on group and income. Congress should make these options more readily available without the need for administrative waivers.
- Clarify the ability of states to adopt work incentives for certain eligibility groups. A number of states have requested and received approval from CMS to put in place work and community engagement requirements for certain able-bodied enrollees who can work. The principle behind this effort, which is found in other welfare programs, is that work promotes the well-being of individuals by encouraging upward mobility and self-sufficiency. Recent actions taken by the Biden Administration block these efforts. Congress should act to give states the option to put these types of work incentives in place for able-bodied adults.
- Establish a demonstration program for certain beneficiaries. In both the Obama Administration and the Trump Administration, HHS waived a series of requirements for certain eligibility groups. These changes acknowledge that there are differences between Medicaid eligibility categories. Congress should create a demonstration project that offers states a toolbox of program flexibilities to tailor benefits more appropriately to enrollees.
- Restructure the financing to target resources and dollars to beneficiaries more effectively. Medicaid’s open-ended financing structure is undermining its fiscal soundness. To keep the program fiscally sustainable and accountable, Congress should:
- End state financing loopholes. States are increasingly using loopholes to maximize the funding of their Medicaid programs. Congress should curb states’ use of loopholes related to provider taxes, upper payment limits, and budget neutrality.REF Tamping down these loopholes and cost shifting at the state level would bring greater transparency and accountability to the financing of the program.
- Reform payments to hospitals for uncompensated care. The current system to provide supplemental payments to hospitals for uncompensated care is poorly targeted and insufficiently accountable. To provide greater accuracy and transparency to this funding process, Congress should separate disproportionate share (DSH) payments from Medicaid and require that the payments be based on actual hospital claims rather than the current formula.REF
- Replace the enhanced match rate with the traditional match rate. For the newly eligible ACA expansion population, the federal government reimburses states at no less than 90 percent. However, for the traditional Medicaid population, which consists of the disabled, elderly, children, and parents, the federal government reimburses states at much lower levels that range from 50 percent to 75 percent. Congress should repeal the ACA’s enhanced federal funding for the Medicaid expansion, thereby ending the funding distortion between Medicaid populations that divert limited taxpayer resources from one group to another.REF
- Restructure basic financing and put the program on a more fiscally predictable budget. As noted, the open-ended nature of Medicaid’s financing fuels more spending, encourages cost shifting, and perpetuates inequities among the states. Restructuring Medicaid financing has gained bipartisan support in the past.REF Moreover, with the growing number of states administering their Medicaid programs through Section 1115 waivers that require the states to maintain spending under a predetermined cap, states are accustomed to the concept. Congress should revisit efforts to restructure the financing of Medicaid through either a per capita cap or a block grant based on eligibility groups.REF This could be done broadly across the entirety of the program or targeted narrowly at the ACA Medicaid expansion.REF Under either of these arrangements, the financing can be adapted to reflect Medicaid’s diverse makeup and bring greater fiscal stability, accountability, and equity to the program.
Conclusion
The Medicaid program is a health care safety net for a diverse group of low-income individuals with very diverse needs. Eligibility expansions, competing beneficiary priorities, an outdated administrative structure, and a flawed financing model are weakening the foundation of the program.
Instead of undermining this federal–state partnership with a one-size-fits-all federal approach as envisioned under various Medicare for All proposals, Congress should ensure that states have the necessary flexibility to address the changing demands on their programs.
Congress should also focus on the more fundamental challenges facing the program, including protecting eligibility for those whom the program is intended to serve, allowing benefits to match the needs of beneficiaries more precisely, and restructuring the program’s financing so that resources and dollars are targeted more effectively to those who are in need.
Nina Owcharenko Schaefer is Senior Research Fellow in Health Policy in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.



