Distribution of COVID-19 Cases: Summary
Although all U.S. states have reported cases of COVID-19, the distribution is currently heavily concentrated in a small number of states, and among a small number of counties within those states. For instance, as of April 14, the State of New York accounts for 34 percent of all reported U.S. cases, of which 45 percent are in New York and New Jersey.REF Table 1 also demonstrates that just 10 states account for 75 percent of all U.S. cases, of which 90 percent are found in just 20 states. Likewise, 54 percent of the total COVID-19 deaths are in New York and New Jersey, and two-thirds are in just five states—New York, New Jersey, Michigan, California, and Louisiana. Given the overall level of case concentration across the states, it is not surprising that 80 percent of the total COVID-19 deaths are in just 10 states, and 93 percent are in 20 states. (See Table 1.)
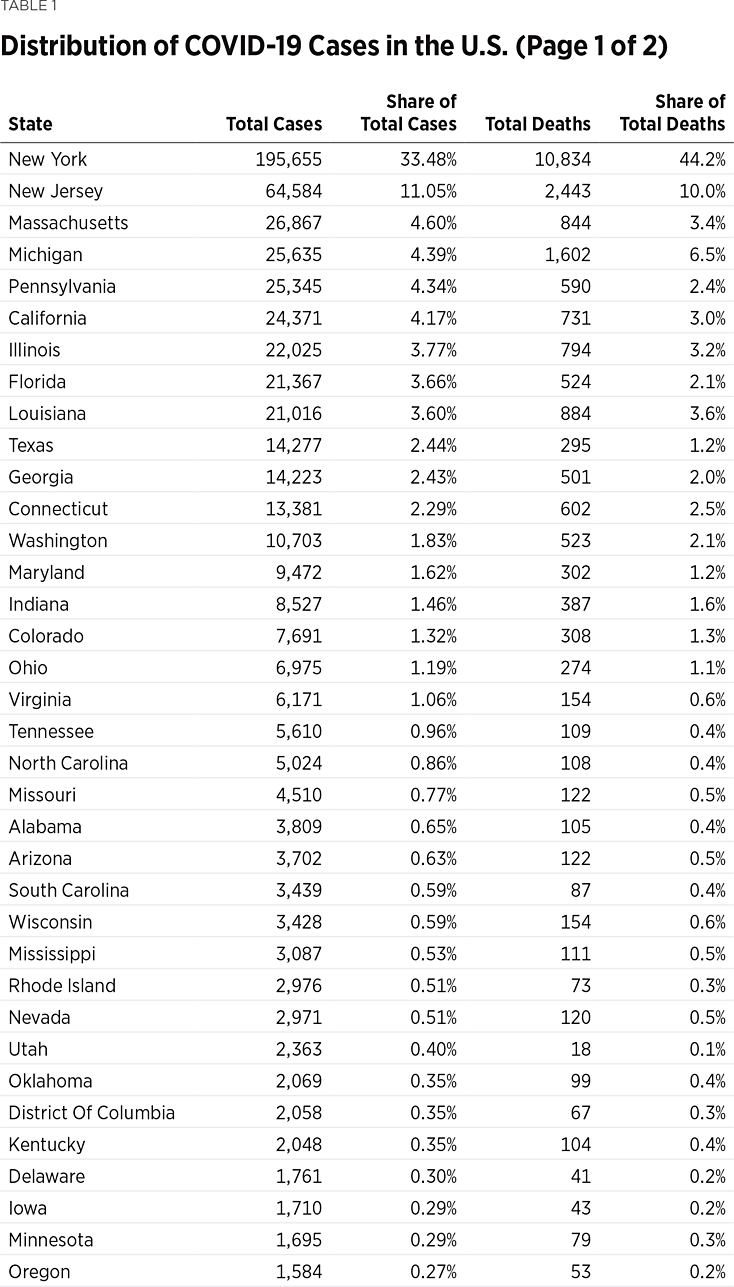
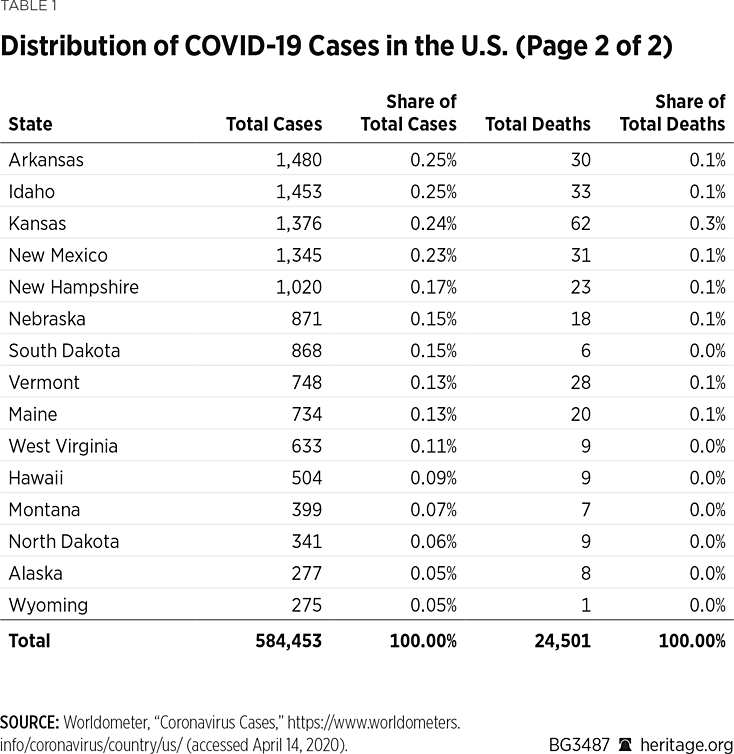
The data are similarly concentrated within states (see Map 1), meaning that a relatively small number of counties account for the majority of COVID-19 cases and deaths. In Washington, for example, 68 percent of the cases (and 75 percent of the deaths) are in just three out of the state’s 39 counties (41 percent in King County, 9 percent in Pierce County, and 18 percent in Snohomish County).REF Five of the counties in Washington report one or no cases, and 8 percent of the total cases have not yet been allocated to a county.
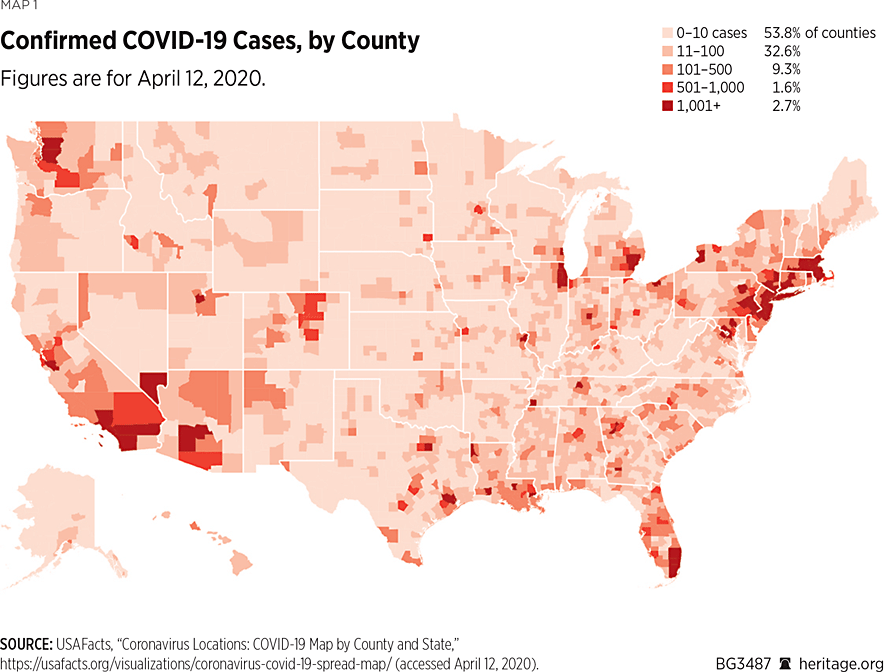
In New York, 77 percent of the reported cases (and 90 percent of deaths in the state) are in the New York City area, in six surrounding counties.REF In California, 54 percent of the cases (and 57 percent of total deaths) are in three counties (Los Angeles County, Santa Clara County, and San Diego County), each in geographically distant locations across the state. These three areas account for nearly 40 percent of the population in California.REF Of 59 counties in California, 15 have reported five or fewer cases. In Michigan, two adjacent counties (Wayne and Oakland Counties) report 66 percent of the state’s cases, and 70 percent of deaths, while 18 percent of the state’s counties report one or no cases.REF In Louisiana, 52 percent of the cases (and 50 percent of the deaths) are in two adjacent parishes (Jefferson and Orleans), and 10 of 64 parishes report 10 or fewer cases.REF
The concentration levels are similar even in states with fewer cases. In Virginia, for instance, 45 percent of the total (5,077) cases are in six counties, with 19 percent of the cases in Fairfax County (a population 1.148 million people with 946 cases).REF The ratios of cases to population are similar for Arlington, Prince William, and Loudoun Counties, all of which are located near Washington, DC. The lone outlier is James City County (2.5 percent of the cases), which includes the popular tourist destination of historic Williamsburg. In Virginia, 22 percent of the counties report one or no cases.
As seen on Map 1, across the entire U.S., of more than 3,000 counties, 54 percent report 10 or fewer cases. This heavy geographic concentration across states and within states highlights how difficult it might be for a one-size-fits-all approach—from either the federal or state level—to deal with the crisis.REF At the same time, this type of concentration could help medical professionals to deal with the crisis better. At the very least, because medical care is provided locally, the concentrated distribution of the COVID-19 cases underscores the dangers of diagnosing health problems with national or even state-level data. Such data may not, for instance, adequately reveal potential hospital bed shortages.REF
U.S. Hospital Structural Capacity Compared to Other Countries: ICU Capacity
As the number of COVID-19 cases has spread in the U.S., many public officials have voiced their concerns over possible shortages of acute-care hospital beds, ICU beds, and equipment.REF Given the serious threat posed by COVID-19, such concern is certainly warranted. Still, there is good reason to believe that the U.S. health care system is in a better position than most other countries.
As Chart 1 shows, ICU-bed capacity is about two to three times higher in the U.S. than in European countries, as measured by ICU beds per 100,000 population.REF
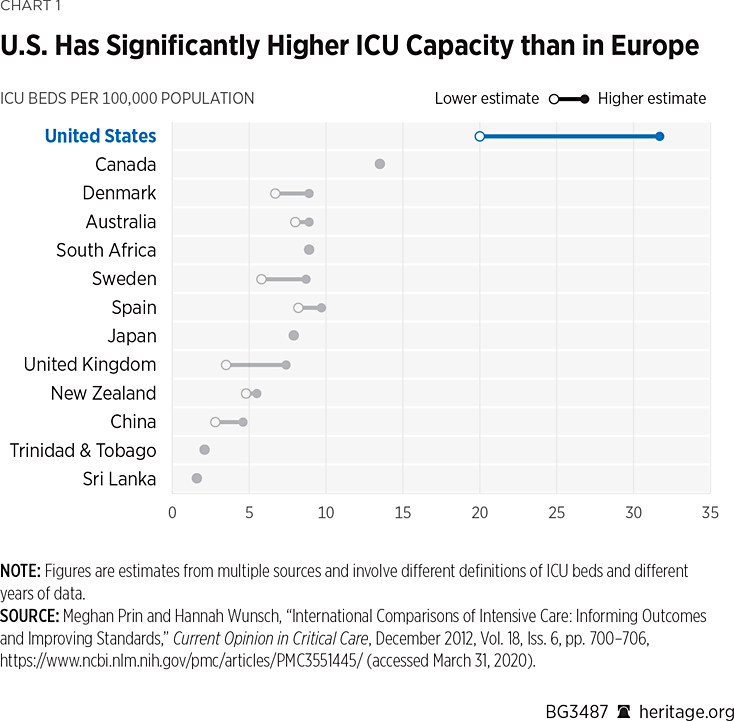
The U.S. has an estimated 20 to 31.7 ICU beds per 100,000 population. With the exception of Canada, no other country included in the study even had as many as 10 beds per 100,000. Although Italy was not included in the study, it is unlikely that its ICU capacity is materially different from that of other highly developed European countries. It is thus misleading to assume that U.S. hospitals will necessarily experience the same scale of problems that Italian hospitals have.
Moreover, Italy’s ICU-bed shortage associated with the coronavirus is concentrated in areas where the epidemic has been most acute. The Italian health ministry reports that there were just over 3,260 COVID-19 patients in ICUs on April 13.REF Of those, 35 percent (1,143) were in Lombardy, the region that has experienced the brunt of the epidemic.REF Lombardy and the three other hardest-hit regions (Emiglia–Romana, Piedmont, and Veneto) account for 64 percent (2,098) of the COVID-19 patients in ICUs. Of the remaining 17 regions, 13 reported fewer than 100 coronavirus patients (median = 41) in ICUs and only two (Tuscany and Lazio) reported 200 or more.REF That is not to say that these other regions are exempt from overburdened capacities.REF It is only to note that even in Italy, where the epidemic has hit hardest and whose ICU capacity is likely far lower than that of the U.S., the problem so far has been confined to a few regions.REF
The U.S. is vulnerable to similar surges in demand for ICU beds, as discussed later in this Backgrounder. But these shortages are neither permanent nor systemic.
Hospital Acute-Care Inpatient Capacity
Just as some have erroneously compared the ICU capacity of U.S. hospitals to that of Italy, others have argued that U.S. hospitals have fewer available acute-care inpatient beds than do other highly developed countries.REF
Those who make these assertions generally base international comparisons on acute-care hospital beds per 1,000 population. While that measurement seems reasonable, it is, in fact, a highly misleading way of estimating the capacity of U.S. hospitals to deal with a sudden influx of COVID-19 patients.
The Organization for Economic Co-operation and Development (OECD) has compiled a wealth of cross-national data on hospital capacity. Chart 2 documents the fact that the U.S. has fewer inpatient hospital beds per 1,000 population than most other developed countries.
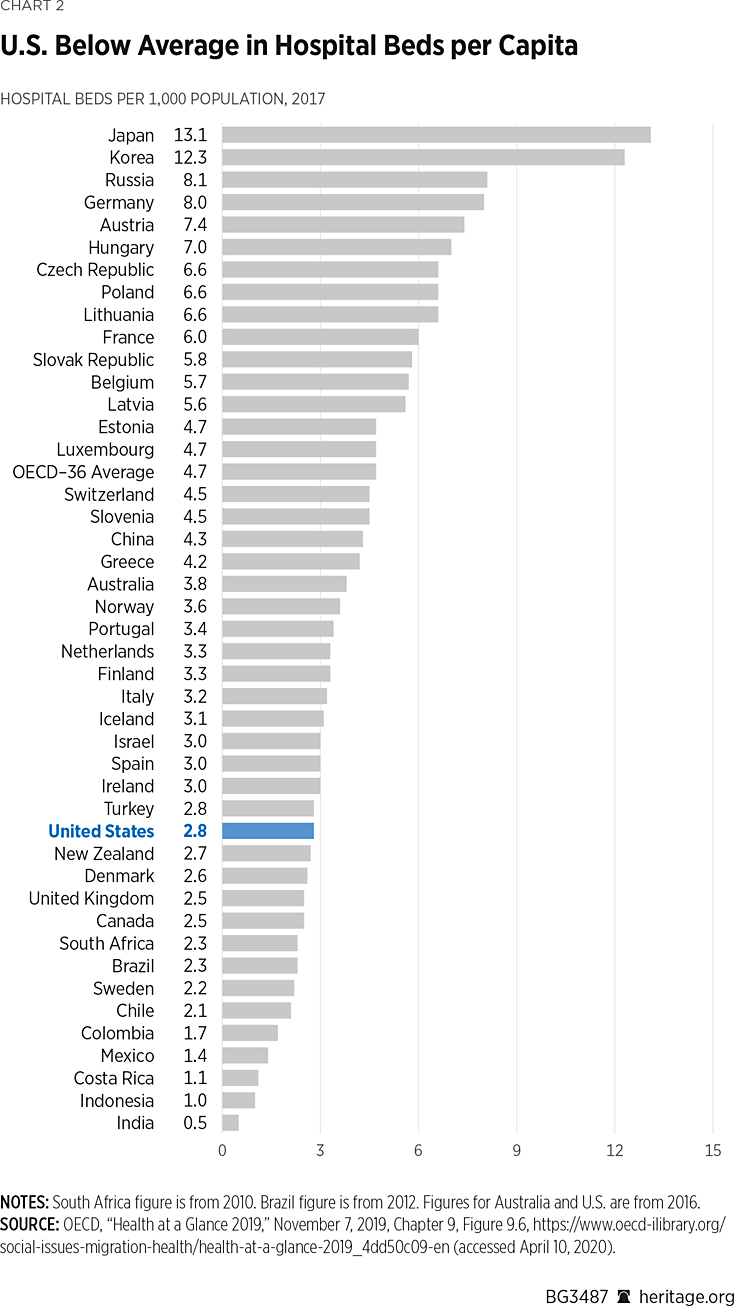
At 2.8 beds per 1,000 population, the U.S. ranks in the bottom third of OECD countries, about 40 percent below the OECD average of 4.7 per 1,000. It also ranks below Italy (3.2 per 1,000), Korea (12.3 per 1,000), and Spain (3.0 per 1,000) all of whom have faced COVID-19 challenges to their health care systems. This would suggest that U.S. hospitals are systemically less well prepared to deal with a large influx of COVID-19 patients.
Excess capacity, however, is not best measured by comparing the number of beds to the population. The more accurate way to measure excess capacity is to look at the percentage of beds that are available to accommodate patients as a percentage of total beds. Having more beds on a population basis does not help if those beds are filled. Hospital occupancy rates are a more appropriate measure of excess capacity. Chart 3 compares occupancy rates across countries.
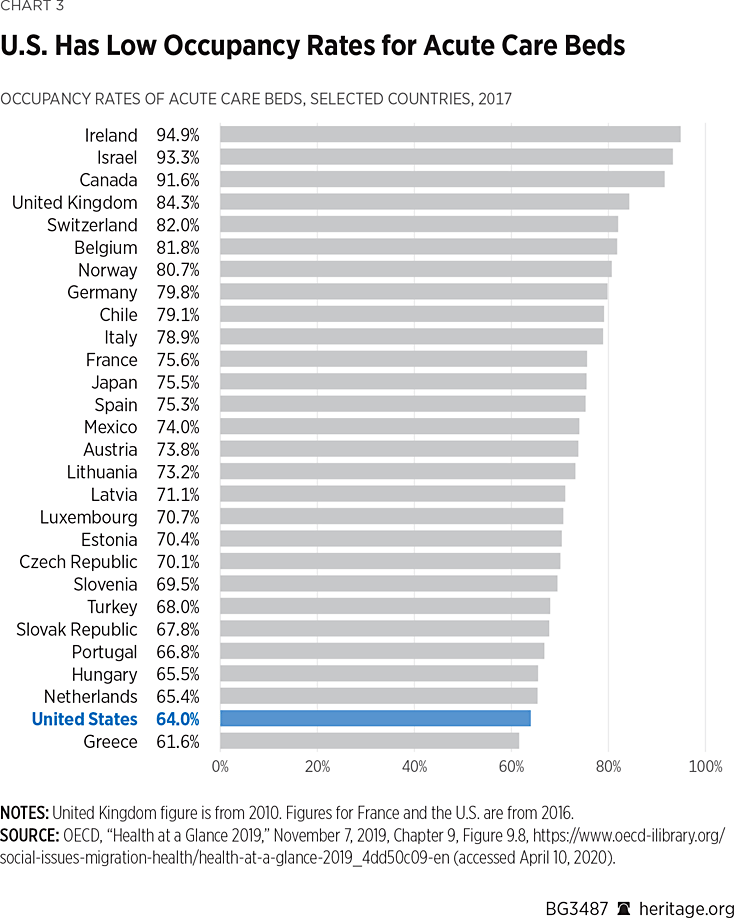
With the exception of Greece, U.S. patients occupy a smaller percentage of acute-care beds than any other country in the OECD study. Its occupancy rate is just 64 percent, well below the OECD average of 75.2 percent. Put another way, more than one-third of acute-care beds in the U.S. are unoccupied and available to receive new patients.
Chart 4 presents an international comparison of unoccupied beds per 1,000 population. This is a much more accurate indication of a country’s structural capacity to accommodate new patients, since such patients cannot be placed in beds that are already occupied by existing patients.
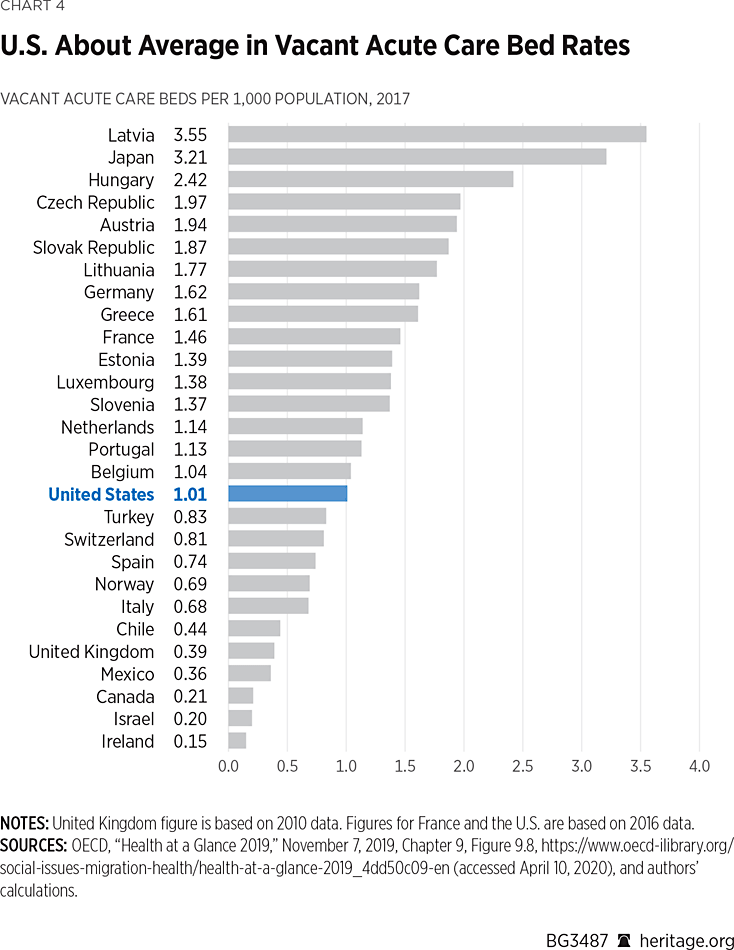
On this more precise way of expressing surge capacity, the U.S. is no longer an outlier. Its unused capacity is equivalent to that of Belgium and greater than that of Switzerland, Spain, Norway, Italy, the United Kingdom, Canada, Israel, and Ireland. Of the 17 highly developed countries for which OECD provided data, the U.S. is at the median.REF
There is no need to build a permanent excess acute-care capacity (even if one were to believe that to be a good idea) because the U.S. already has among the highest excess capacity rates in the world, and its available beds per 1,000 population places it at the median of highly developed countries. While COVID-19 may overtax the capacity of some hospitals in some areas on an episodic basis, there is no structural shortage of hospital acute-care capacity in the U.S.
Analyzing why U.S. policy has resulted in hospitals having so few beds per 1,000 population and so many empty ones is beyond the scope of this Backgrounder. One reason, however, is the fairly substantial shift from inpatient care to outpatient care. In the U.S., many procedures and treatments that once required hospital stays are performed at hospital outpatient departments, ambulatory surgical centers, and doctors’ offices. By admitting fewer patients, U.S. hospitals keep a large proportion of their beds empty. This is problematic, since empty beds impose a deadweight cost on hospitals that are likely passed through to consumers and taxpayers in the form of higher prices paid by public and private providers. This is one reason why requiring hospitals to permanently increase excess capacity is not desirable. But when measuring the structural capacity of U.S. hospitals to accommodate a surge of patients, the percentage of acute-care beds that lie empty can offer near-term advantages.
U.S. Hospital Capacity to Withstand a Surge of COVID-19 Patients
While the U.S. has no structural shortage of ICU beds or acute-care beds, COVID-19 could overrun the capacity of hospitals in particular geographic locations for a period of time. If there is a surge of patients requiring intensive care in Brooklyn, it does no good to have empty ICU beds in Casper, Wyoming. The challenge posed by COVID-19 is not best resolved by permanently increasing national hospital capacity, but by temporarily augmenting capacity in specific localities for a short period of time.
Researchers at the University of Washington’s Institute for Health Metrics and Evaluation (IHME) used statistical modeling to help combat this problem. Their work, the most recently published comprehensive effort of its type, forecasts the strain that COVID-19 will place on the availability of hospital beds, ICU beds, and ventilators in the U.S.REF
Although elected officials should not rely on one single model, or even one single set of projections, as of April 14, 2020, the research estimated that the peak resource use for the U.S. health care system was reached on April 10, at which point there was a shortage of 3,498 inpatient beds and 7,369 ICU beds. Although the model has been criticized because the IHME team made several downward revisions to its projections, the IHME model appears to be the best available tool for forecasting state-level hospital bed and ICU bed capacity.REF
This forecast shortage, however, was neither permanent nor nationwide, and it did not, in any event materialize.REF Just one state—New York—accounted for nearly 100 percent of the predicted total-hospital-bed shortage and nearly two-thirds of the ICU-bed shortage. In earlier versions of these forecasts, the states of Colorado and Tennessee accounted for almost 15 percent of the country’s total projected bed shortage, and Tennessee alone accounted for nearly 10 percent of the predicted ICU-bed shortage for the whole country.REF Those earlier forecasts also projected that New York would be responsible for approximately 70 percent of the hospital-bed shortage for the entire country. Thus, combined, those earlier estimates suggested that 85 percent of the projected hospital-bed shortage would occur in just three states, with the majority of the problem concentrated in New York. While there is always uncertainty with these kinds of projections, the model currently predicts that there will be no shortage of beds in 29 states of the 33 states that have yet to reach their projected peak resource date.REF
The model also currently predicts a peak need of nearly 14,000 ventilators. Once again, this national figure does not indicate the varied needs of state and local regions. Based on the model’s projections, the excess demand for ventilators is predicted to be most acutely felt in certain areas, such as the New York metropolitan area, where the model shows a need of more than 5,000 ventilators at the April 8 peak.REF Other states, such as Georgia (715), South Dakota (45), Texas (577), Utah (40), and Oregon (47), are projected to need far fewer ventilators at the peak of epidemic in their respective locations.REF
Meeting the COVID-19 Challenge: The Need to Increase Capacity on a Localized and Episodic Basis
Providing the highest level of medical care to the anticipated surge of COVID-19 patients does not require building out permanent hospital capacity. It calls for something more difficult: the coordination of federal, state, and local officials to address temporary and localized crises.
This daunting challenge requires government to be nimble, adaptable, focused, and purposeful. Federal officials (some elected, some not) and an alphabet soup of agencies (including the Centers for Disease Control and Prevention (CDC), the Public Health Service, the Food and Drug Administration, the Health Resources and Services Administration, the Federal Emergency Management Agency, and other military and civilian agencies, most of which have conflicting pandemic preparedness plans in place) must formulate and execute responses that involve coordinating with one another and with similar coteries of competing state and local bureaucracies and politicians.REF
Government in its myriad manifestations is the entity charged with marshalling and directing resources where need is most acute.
That task requires temporarily increasing the supply of medical professionals, hospital capacity, and equipment in communities where needs are most acute. Doctors, nurses, paramedics, and other medical professionals in these areas are overtaxed and underresourced. They require reinforcements and personal protective equipment to carry out their heroic efforts.
Hospitals in certain areas are similarly overtaxed. Localized and episodic shortages of acute-care beds and ICU beds, as discussed above, are forecast for several metropolitan areas. Building permanent excess capacity is not only unwise policy, but it is poorly suited to the crisis at hand. By the time new hospitals are built, the pandemic will have passed. The challenge is to increase capacity on a temporary basis in the areas of greatest need.
The most severe cases of COVID-19 require intensive medical interventions. The inventory of ventilators, as discussed, is projected to fall short for limited periods of time in discrete locations. Closing this gap requires both increasing supply and assuring the delivery of ventilators to affected areas, as policymakers have begun to do.
Finally, federal, state, and local officials need to be able to adapt their strategies, tactics, and operations to changing conditions. The response to the COVID-19 pandemic is unique, not only in the U.S., but in the world. While the response of most countries to the pandemic has consisted largely of social distancing, other countries have pursued different strategies.
Some of these strategies differ markedly from those in the U.S. and have yielded more effective results.REF In preparing for localized outbreaks, public health officials should learn, not only from other U.S. cities but from around the world. This is especially true of federal public health officials, who have access to a wealth of data and can recommend policies to state and local officials bracing for a localized outbreak.
Recommendations for Policymakers
Meeting the challenge of pandemics requires increasing capacity and devising adaptable strategies. Policymakers should pursue the following four objectives:
-
Increase the Supply of Medical Professionals. COVID-19 has placed enormous stress on physicians, nurses, and other health care practitioners, who are exposing themselves and their families to contagion. While there are ongoing efforts to augment hospital capacity and to make tests, personal protective equipment, and other supplies more broadly available, these efforts cannot succeed without a sufficient number of medical professionals. States and localities are well-positioned to provide these practitioners with needed reinforcement.
In a March 24 letter to governors, Health and Human Services Secretary Alex Azar outlined how states can deploy force multipliers to enhance their COVID-19 efforts: REF
-
Allow health professionals licensed or certified in other states to practice in one’s state. Many states have licensure laws that would prevent a doctor from Massachusetts, for example, from treating patients in The Bronx. While these laws may be well-intentioned, they impede efforts to protect people in affected areas who have fallen ill due to the coronavirus. Allowing doctors from other states, either in person or through telemedicine, to assist during medical emergencies is an important way to combat the epidemic.
-
Expand telemedicine. Telemedicine not only broadens access to doctors in areas where the medical system is battling a surge of COVID-19 patients, it is also a way to get critical medical advice without interacting in an office or hospital setting with patients whom one might infect or who might infect oneself. Allowing telehealth consultations, both within a state and across state lines, by health professionals licensed in other states to deliver medicine this way during a crisis is a sensible and affordable way to expand access to care. For example, the federal government has taken steps for Medicare patients to access doctors via telemedicine regardless of where the doctor practices during the pandemic; states should follow suit by first accepting the offer from the Centers for Medicare and Medicaid Services to work with them to waive this requirement in their Medicaid program, and also reviewing laws for other barriers curtailing the use of telemedicine.REF
-
Relax scope-of-practice requirements. Most states limit medical practice to licensed physicians. Whatever value this may provide in normal circumstances, it is an impediment during a medical emergency when doctors have more than they can handle. Temporarily suspending rules that limit the care that advance practice nurses, physician assistants, and others can provide would free up doctors to deal with the patients in greatest medical need.
-
Allow malpractice insurance to travel with physicians. Some medical malpractice insurance policies do not cover physicians who provide care in other states. Governors should work with medical malpractice insurance companies to waive such limitations for physicians who travel outside the state to treat COVID-19 patients.REF
-
Allow medical students to see patients. Medical students provide another potential resource for enlarging the existing pool of medical providers. States should remove regulatory barriers that prevent students from conducting triage and treating patients, under the supervision of licensed medical staff. New York is allowing students in their last year of medical school to provide care under some circumstances.REF
-
-
Increase the Supply of Urgently Needed Equipment. In contrast to medical workforce enhancements, which generally are within the purview of states, the federal government has primary responsibility to approve, acquire, stockpile, and distribute equipment and supplies to states and localities where they are needed most. To enhance state and local response to COVID-19 outbreaks, the federal government should prioritize the following steps:
- Tests. The most telling and consequential blow to the public health battle against the coronavirus may be lack of tests.REF Those errors have made it impossible to determine the extent of the pandemic and to implement strategies to curb its expansion. Now that tests are coming available, it is up to federal public health officials to assure that they are available in areas where the need is most acute. The federal government should make every effort to prioritize these areas and to adapt these priorities as new hotspots are identified.
-
Masks. Persistent shortages of N95 masks expose medical workers and uninfected patients to heightened risk of contagion. The production shortfall of these masks has continued to hamper public efforts.REF It is critical that the federal government resolve this issue quickly and prioritize the distribution of the masks it has stockpiled to the areas of greatest need. It also should work to ramp up production of N95s by major suppliers, explore importation, prioritize use of the masks for only critical activities, and limit the use of N95 masks to specific areas of a hospital treating coronavirus patients.REF
-
Ventilators. Days after President Trump invoked the Defense Production Act to compel General Motors to begin producing ventilators, their supply still lags demand from states, including New York.REF The federal government needs to continue to drive this issue and to develop a plan to assure that the hardest hit areas have access to a sufficient number of ventilators.
- Provide Temporary Hospital Capacity. The COVID-19 pandemic has so far posed the greatest challenges in hot spots—localized areas where a spike in infection rates leads to a surge in hospital admissions. Meeting these challenges requires state and local officials to prepare for such surges in advance. Steps such officials should consider include:
-
Limiting elective procedures and non-emergent care in areas. Many states and jurisdictions already have taken this step, which relieves some of the pressure on hospitals. State and local officials that have taken these steps should monitor them closely and not leave them in place in localities where the need for beds is not acute, and should remove them from affected localities after a surge of illness has receded.
-
Providing auxiliary hospital capacity. This already is taking place in New York, with the repurposing of the Javits Center and the arrival in New York harbor of the USNS Comfort. As with most efforts associated with COVID-19, this one has been the subject of controversy, as some have questioned the decision by federal officials to designate the ship for non-COVID-19 patients.REF The notion of providing auxiliary hospital capacity is nonetheless a sound one in concept. States and cities anticipating patient surges should work to repurpose existing space and construct temporary hospitals. Full use also can be made of Veterans Administration facilities. By statute, the agency is required to back up the nation’s health care system and it has a surplus of beds at its 172 hospital centers, including rooms for patients with breathing disorders.REF
-
-
Enhance Efforts to Reverse the Pandemic. Public health efforts to combat COVID-19 have thus far centered on social distancing. The practice is a tactic to slow the spread of the virus, but not to reverse it. Its purpose is to “flatten the curve,” which can reduce the number of people requiring hospital care during a peak. But flattening the curve also elongates it, meaning that the epidemic will run a longer course. Consequently, one of the real costs of a sustained social distancing program that policymakers must account for is that the longer social distancing remains in effect, the deeper and longer lasting the economic damage will be. Thus, allowing states and localities to develop appropriately targeted policies that do not rely on sustained strict social distancing programs is essential for saving lives and livelihoods.
Areas of the country that are especially hard hit by the virus, as well as those areas that evidence suggests might become a new hotspot, may consider other public health strategies that, for instance, have proven effective in South Korea. Use of these tactics, combined with a much more limited version of social distancing than that practiced in most U.S. states, reversed the pandemic in a short period of time. States should consider implementing strategies that include:
-
Widespread testing. Over the next weeks, it is likely that tests will be more broadly available. States should make full use of these tests, extending them to groups at highest risk, such as seniors and people with pulmonary disease, on a widespread basis. Tests should be administered to all symptomatic people and, in areas where incidence is especially high, to asymptomatic people as well. Beyond that, states should consider conducting tests to gather samples of asymptomatic people, to gather data to inform understanding about the disease.
- Temporary isolation facilities. Testing is an important step, but it is also critical to deal appropriately with those who test positive. The standard practice in the U.S., emulating Italy and other European countries where infection rates are rising at a rapid rate, is to hospitalize those who test positive or send them home. In both cases, people shedding virus are placed in close quarters with people who are uninfected. South Korea sends such patients to temporary isolation facilities (repurposed dormitories or other similar spaces) until they test negative. Such facilities also serve as triage centers, with those exhibiting more serious symptoms being transferred to hospitals. State and local public health officials that anticipate a surge in COVID-19 cases should strongly consider acting now to prepare temporary isolation facilities. Mandatory assignment to such facilities raise civil liberty concerns, but public officials should use public education campaigns encouraging people to protect their loved ones, rather than expose them to infection. Such a voluntary campaign holds great potential for reducing the rate of infection over time, as South Korea has illustrated.
-
Enhanced contact tracing. A person who tests positive is very likely to have infected others with whom he or she has had contact. South Korea uses a phone-based app to notify people that they may have been exposed, and to encourage them to be tested. News reports suggest that technology companies are working toward a privacy-protected system now.REF
-
Travel restrictions. South Korea’s efforts were effective in part because they isolated people in the city of Daegu, where the first outbreak was identified. Placing travel restrictions on citizens is a step many state and local officials are reluctant to take. It can, however, be effective in confining infection and limiting its spread to other communities. At the federal level, the CDC on March 28 issued a domestic travel advisory urging residents of New York, New Jersey, and Connecticut to avoid non-essential travel for 14 days, but any restriction would have to be enforced by those states. Some states have acted on an ad hoc basis.REF Florida, for example, has banned residents from those three states from flying into its airports. A more focused approach by communities at risk of an outbreak, combined with other steps outlined above, might prove beneficial.
-
Conclusion
Governments are implementing, at least to some extent, many of the policy recommendations discussed above. Those efforts have so far been mixed, as one would expect. The most daunting and imminent challenge is a potential surge of patients in the New York City region, which is expected to peak sometime this month. Federal, state, and local officials are preparing for a response. Other cities, including New Orleans, also are at immediate risk.
The United States has some advantages over other countries, such as Italy, whose hospital systems in some places are not tolerating the surge in critically ill patients. The U.S. has an excess capacity of acute-care beds and more ICU beds per 100,000 population than other highly developed countries. It also does not face a nationwide outbreak, but rather localized crises that may be amenable to focused and well-coordinated public health interventions.
Policymakers should focus their efforts on forthcoming, localized outbreaks, executing a comprehensive strategy that makes full use of the methods at its disposal.
Doug Badger is Visiting Fellow for Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Norbert J. Michel, PhD, is Director of the Center for Data Analysis, of the Institute for Economic Freedom, at The Heritage Foundation.


