The Social Security Disability Insurance (SSDI) program is functionally and financially broken. With average wait times approaching 600 days, too many individuals die while awaiting their benefits. As the system denies benefits for some individuals with rather apparent disabilities, almost half of all benefit awards stem from non-medical factors, such as age, education, and work experience. Furthermore, despite the program’s intent to provide benefits only while workers are disabled, the SSDI program fails to conduct sufficient continuing disability reviews (CDRs). Moreover, fraud and abuse contribute to a lack of integrity and accountability.
All told, SSDI fails to meet the needs of individuals with disabilities and fails to use workers’ payroll taxes efficiently. By approving excessive disability insurance benefits, failing to provide any type of meaningful return-to-work assistance, and neglecting to perform meaningful CDRs, the program costs workers far more in taxes than needed to provide well-functioning disability insurance.
Policymakers should transform the dysfunctional SSDI program into one that meets the needs of individuals with disabilities in a timely and effective manner, that ensures the integrity of the program to meet its intended purposes, and that respects workers’ tax dollars through efficient program administration.
Size and Costs
When SSDI first began 62 years ago, it cost taxpayers 0.5 percent of their paychecks. Today, that tax has more than tripled to 1.8 percent, and even that level is not enough to fully fund the program. Over the past three years, Congress re-allocated about $150 billion from Social Security’s retirement program to the disability insurance program in order to paper over program deficits, yet the disability insurance program is still projected to run out of funds beginning in 2032.
SSDI’s excessive and unexpected cost growth stems from multiple factors, including loosening of eligibility standards, an expansion of the eligible population, growth in real benefit levels, inconsistent and often lax benefit determinations, and failure to help or encourage individuals to recover and return to work.
Fixing these problems would create a better functioning and more targeted disability insurance program. Heritage Foundation analysts estimate that an innovative transformation of the disability insurance program could reduce its costs by 54 percent in the long term, from 2.06 percent of payroll to 0.94 percent of payroll.REF Correspondingly, the payroll tax could eventually be lowered from 1.80 percent to 0.94 percent, and the program would still remain solvent. These changes would protect and improve the program for individuals with disabilities and reduce the burden of the program for taxpayers.
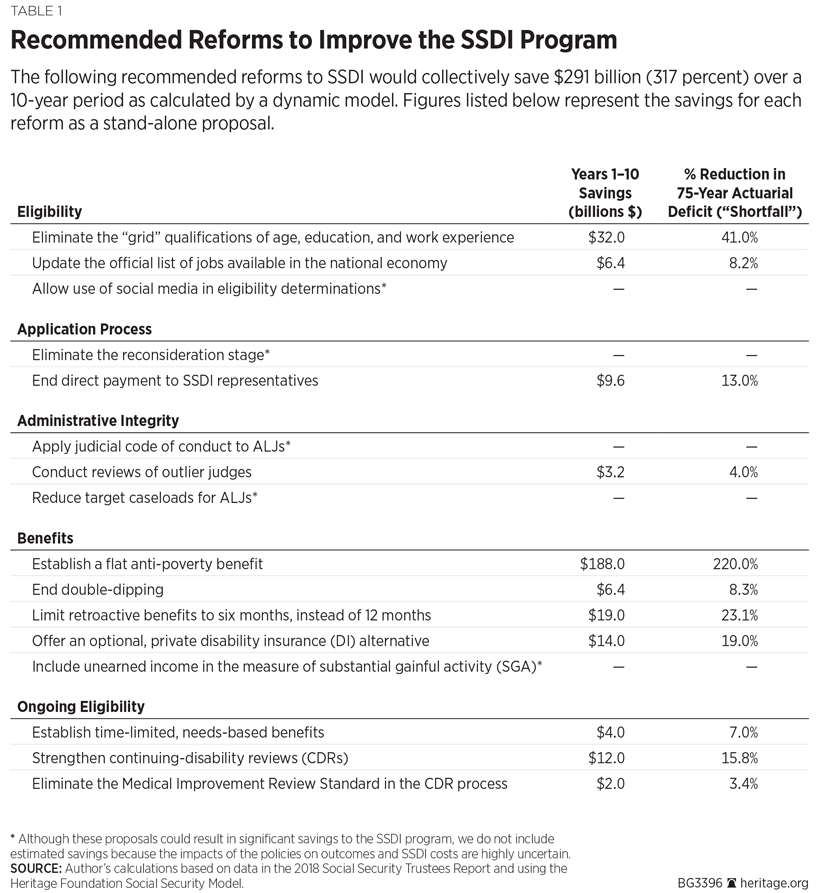
Recommended Reforms for Improving SSDI
The Social Security Disability Insurance Program provides benefits to more than 10 million individualsREF at an annual cost of $146 billion.REF Given the SSDI’s pervasive problems, creating a better functioning system for both individuals with disabilities and taxpayers requires a comprehensive set of reforms addressing each facet of the SSDI program.
Eligibility. The biggest reason for excess growth in the disability insurance program is that the system allows many individuals who are capable of work to receive benefits. The program’s definition of disability is quite strict: To receive benefits, individuals must have a physical or mental impairment that prevents them from earning substantial gainful activity (income of $1,180 or more per month in 2018) through any job in the national economy.
In reality, however, individuals who can earn substantial gainful activity nonetheless qualify for, and receive, disability insurance benefits based on flaws in the existing system. To protect the program for individuals who have truly work-prohibiting disabilities, Congress should implement the following 16 reforms:
1. Eliminate the “grid” qualifications of age, education, and work experience. Physical and mental capabilities should be the sole basis for disability determinations. Instead, almost half—48 percent—of all disability determinations in 2016 relied on non-medical factors, such as age, education, and work experience.REF This means that if a 45-year-old man who can only perform sedentary work and who claims to not speak English comes before an administrative law judge (ALJ), that judge must grant him disability insurance benefits based on him meeting non-medical grid qualifications.
Although work capacity—particularly for physically demanding jobs—may decline with age and lack of education or experience can limit the number of jobs that individuals can obtain, the grid factors of age, education, and experience do not and cannot cause workers to be disabled from performing all work. An analysis commissioned by the Social Security Administration (SSA) confirmed this, concluding that the study “found no rigorous evidence of the independent effects of age, education, and work experience on the ability to perform new work.”REF
Only physical and mental conditions can prevent individuals from performing work, and only physical and mental conditions should qualify individuals to receive disability insurance benefits. The Secretary of Health and Human ServicesREF can and should eliminate the grids through regulation and base disability determinations solely on medical conditions. Alternatively, Congress could eliminate the grids through statute.
Savings: This proposal saves an estimated $32 billion over the next 10 years and would reduce the program’s 75-year shortfall by 41 percent.REF
2. Update the official list of available jobs in the national economy. Last updated in 1991, the list of jobs that exist in the national economy fails to recognize significant work opportunities that exist for individuals with disabilities. While telegram messenger, mule driver, and seal killer (a practice outlawed in 1972) are all listed as potential jobs for workers applying for SSDI, Internet-based and gig-economy jobs are not included on the official jobs list.REF
Many of the new jobs missing from the outdated listing are particularly amenable to individuals with disabilities. For example, there has been a shift to more service-oriented and sedentary jobs. Some of these jobs can be done remotely, allowing individuals to work from home without having to navigate what may be a physically or mentally challenging commute and workplace environment. Moreover, gig-economy platforms such as Uber, Upwork, and Etsy allow people to decide how much or how little they want to work, and they typically allow workers to perform jobs remotely, often from their own homes. If these jobs were included in the job listing, fewer individuals would qualify to receive disability insurance benefits.
Either through administrative regulation or congressional statute, policymakers should require the SSA to update the official list of jobs available in the national economy at least every three years.
Savings: This proposal saves an estimated $6.35 billion over the next 10 years and would reduce the program’s 75-year shortfall by 8.2 percent.REF
3. Allow use of social media in eligibility determinations. Social media can provide valuable evidence to support or deny individuals’ disability insurance applications, and courts regularly admit social media content as evidence in non-SSDI court cases. According to a 2014 report by the Office of the Inspector General,
social media played a critical role in the New York disability fraud investigation, as disability claimants were seen in photos on their personal accounts, riding on jet skis, performing physical stunts in karate studios, and driving motorcycles…. SSA does not allow its employees or DDS [Disability Determination Services] employees to consult this information during adjudication of a claim.REF
While social media should not be the primary means of deciding a disability case, information available on social media should not be excluded from the SSDI determination process.
Savings: Although this proposal could generate savings by improving the determination process and restricting individuals who are not disabled from receiving benefits, we do not include any estimated savings for this proposed reform because the size of those savings is uncertain and may be relatively small.
Application Process. The disability insurance program’s application process is a nightmare for most people, to put it mildly. While some individuals with unambiguous disabilities who submit the proper evidence and paperwork may receive a favorable SSDI determination at the initial level within a few months,REF between a quarter and a third of individuals who apply for, and end up receiving, benefits have to go through three different levels of determinations and wait an average of 591 days before receiving a favorable determination.REF Moreover, when individuals hire representatives to help them with the process—something that many individuals opt to do after being denied at the initial and reconsideration stages—the SSA improperly intervenes in the client and representative relationship, potentially leading to worse outcomes and excessive costs for individuals with disabilities. Congress and the SSA can make the application process fairer and more efficient by enacting the following reforms:
4. Eliminate the reconsideration stage. Of the roughly 950,000 individuals who apply for disability insurance benefits, about 45 percent receive approvals at the initial DDS stage, 25 percent drop out of the process after a denial, and the remaining 30 percent bring their case to the reconsideration stage.REF At the reconsideration level, applicants wait an average of 108 days for a decision and only 11 percent receive a favorable decision, while 27 percent drop out of the process and 62 percent go on to appeal their unfavorable decisions before an ALJ.REF Approval rates are highest at the ALJ level, with about 64 percent of applicants receiving favorable determinations.
The reconsideration stage follows procedures as identical to the initial DDS stage, only with a different staff reviewing the application. While applicants can submit new evidence, they are not informed of any evidence lacking at the initial stage.REF A 10-state test of removing the reconsideration stage found that doing so resulted in more accurate decisions at the initial level and significantly shorter wait times for applicants.REF
As a highly duplicative process that adds time and resource costs, the reconsideration stage should be removed in conjunction with changes to improve the accuracy of decisions at the initial level. Some improvements to the initial stage are: better development of medical and evidentiary records, more in-person or video inquiries with the claimant, and better guidance for and coordination with treating physicians.
Savings: Although we believe that this proposal would lead to long-term savings by producing more accurate and timely decisions as well as generating administrative savings, the size of those savings is highly uncertain, so we do not include any estimated savings here.REF
5. End direct payment to SSDI representatives. In general, when individuals contract with attorneys or representatives, the two parties agree to the terms of representation and individuals do not have to pay their representatives if these do not hold up their end of the agreement. That is not the case for individuals with disabilities who hire representatives. Instead, the SSA dictates the fees for the SSDI representatives and directly takes those fees—acting as a bill collector to the tune of more than a billion dollars per year—out of beneficiaries’ initial SSDI payments.REF
This takes control away from SSDI beneficiaries, allowing representatives to receive payment without necessarily providing valuable services. Moreover, the practice causes representatives to seek out individuals to apply for SSDI benefits and it encourages representatives to delay cases. Representatives typically receive 25 percent of a beneficiary’s back payment up to $6,000 (back payments are payments for all the months between when the individual first filed a claim and when they received an award determination), and the longer the case takes to process, the higher the back payment that individuals receive and thus the higher the payment that representatives can collect.REF
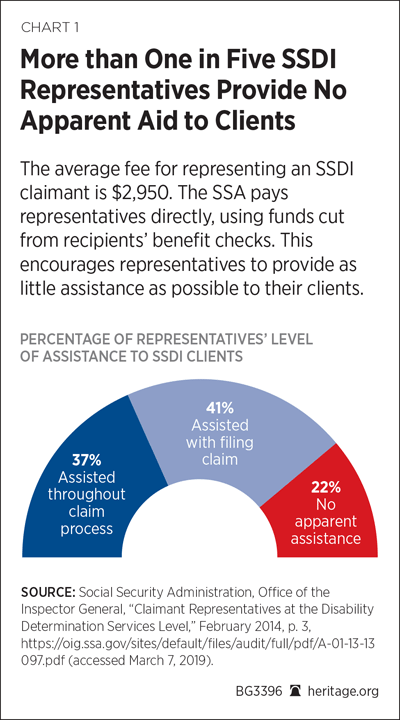
An Inspector General report found that only 37 percent of representatives assisted their clients throughout the application process, while 41 percent assisted only with the application and 22 percent provided no assistance at all; yet all received the same full payment.REF Without direct, guaranteed payment from the SSA, individuals with disabilities would likely receive better representation at potentially lower cost than what the SSA currently takes out of their benefit checks.
The SSA should stop interfering in the private transactions of individuals with disabilities and provide them the full benefits they are due.
Savings: This proposal would save an estimated $9.6 billion over the next 10 years and would reduce the program’s 75-year shortfall by 13 percent.REF
Administrative Integrity. Administrative law judges who decide disability cases at the third administrative appeal stage play a critical role in the SSDI program. ALJs typically receive cases with hundreds—if not more than a thousand—pages of documentation and they must play multiple roles, representing both the applicant as well as the SSA. Certain features of the administrative rules and process create perverse incentives and adverse realities for ALJs, often resulting in excessive SSDI benefit awards. The following reforms could improve the integrity, effectiveness, and fairness of the application process:
Savings: Reducing the number of cases ALJs hear each year would require additional spending to increase the number of ALJs who oversee cases, but it would likely lead to more accurate decisions, which could lead to significant savings. While we believe improved decisions would lead to fewer erroneous approvals, we do not include any estimated savings for this proposal because of uncertainty over the size of those potential savings.
6. Apply judicial code of conduct to ALJs. All judges—including ALJs who decide SSDI cases—should have a clear code of conduct, with well-defined and consistently enforced consequences for violating that code. However, ALJs currently operate under a separate, less stringent code of conduct than the judicial code of conduct that applies to all other judges. For example, the ALJ code of conduct allows ALJs to make certain political contributions otherwise prohibited by the judicial code of conduct.
Recent exposure of corruption and collusion among ALJs within the SSDI system underscores the need to enforce greater judicial accountability. Applying the judicial code of conduct to ALJs has widespread support, including from the American Bar Association, which said that making ALJs subject to and accountable under standards set forth in the judicial code of conduct would “promote fairness and public trust in administrative adjudication.”REF
Savings: Applying the judicial code of conduct to ALJs is an integrity-enhancing measure that could also lead to positive changes, such as more accurate decisions that reduce the total number of SSDI awards. However, due to the high level of uncertainty in potential financial impacts, we do not include any estimated savings for this reform.
7. Conduct reviews of outlier judges. Up until 2009, almost a third of all ALJs approved applications in more than 80 percent of cases, while less than 1 percent approved 20 percent or fewer of their cases.REF Most of the cases decided by ALJs have already been denied twice, so it seems logical that approval rates at the ALJ stage should be lower. An analysis by Mark Warshawsky of the Mercatus Center estimated the net cost of mistaken approvals and denials by high-approval-rate and low-approval-rate judges to be almost $72 billion in wrongful SSDI payments between 2005 and 2014.REF
The SSA has the authority to conduct pre-effectuation reviews, which are reviews of ALJ decisions before they are finalized and the claimant receives notice of the decision. These reviews allow the Office of Disability Adjudication and Review’s Division of Quality (DQ) to identify potential errors in ALJ decisions. However, pre-effectuation reviews are conducted at the agency’s discretion and they must be randomly assigned. To improve the effectiveness of quality reviews, the DQ should be required to perform a certain percentage of pre-effectuation reviews (as is required by statute at the DDS level), and some of those reviews should have to be targeted to cases handled by high-approval-rate and low-approval-rate judges.
Savings: This proposal would save an estimated $3.2 billion over the next 10 years, and would reduce the program’s 75-year shortfall by 4 percent. REF
8. Reduce target caseloads for ALJs. The SSA sets a benchmark for ALJs to preside over 500 to 700 case dispositions (including decisions and dismissals). This leaves very little time, on average, for ALJs to review and issue decisions. After factoring out vacation, holidays, and other required ALJ activities, the 500-to-700-cases target leaves ALJs with between 2.6 hours and 3.6 hours per case. Yet, a work analysis study commissioned by the Association of Administrative Law Judges (AALJ) concluded that the average SSDI case (655 pages in length) requires 7.1 hours of an ALJ’s time.REF While about 18 percent of cases are dismissed and a small percentage can be handled “on the record” without an actual hearing, the current caseload target nevertheless leaves very little time for judges to review cases, hold hearings, and issue well-informed decisions.
Benefits. The government’s role in disability insurance is intended to prevent workers who become disabled from falling into poverty while also minimizing program costs to prevent workers from having to sacrifice an undue portion of their paychecks for mandatory disability insurance. The current program does a poor job meeting these objectives in part because of its benefit structure. To better meet the needs of individuals with disabilities and to prevent extraneous and unintended use of benefits, policymakers should adopt the following recommendations:
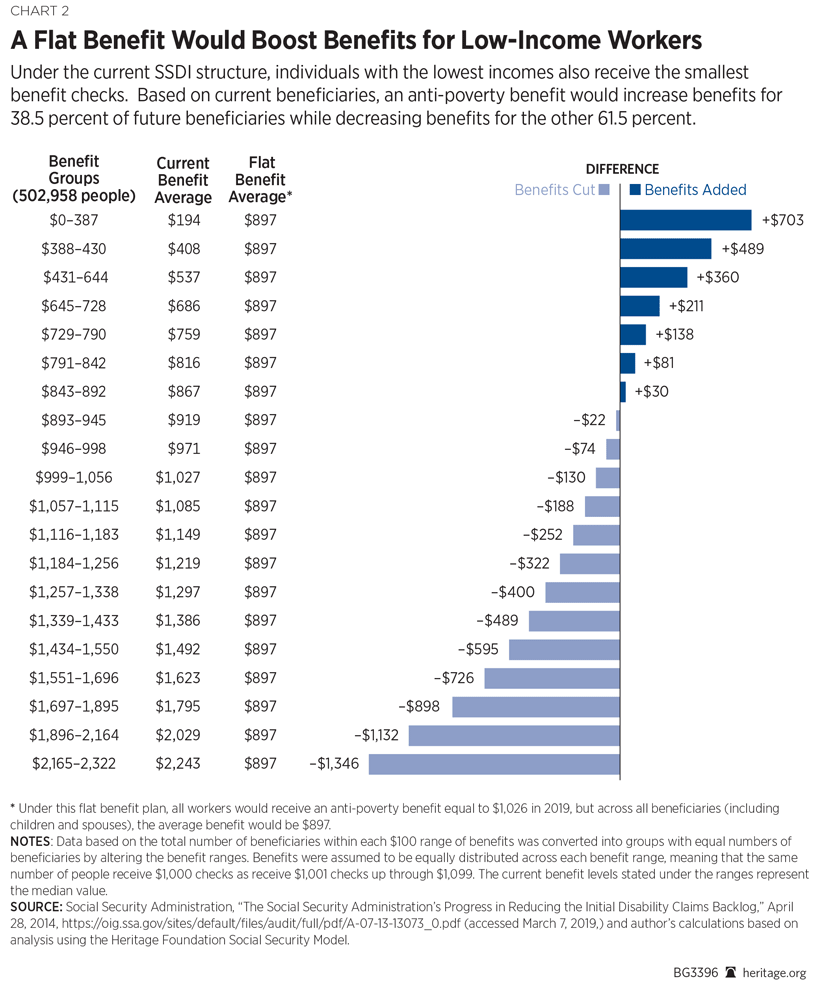
9. Establish a flat anti-poverty benefit. The disability insurance program began over six decades ago as a small-scale, anti-poverty program—not an income-replacement program. Despite its explosion in size and costs since then, the program fails to keep a significant percentage of its recipients out of poverty. Yet, it provides the highest benefits to those with the least need. Replacing the progressive benefit formula with a flat, anti-poverty benefit could lift more than a million individuals with disabilities out of poverty while also making the program financially sound over the long term, ensuring that it is there for individuals who truly need it.REF
Shifting to a flat, anti-poverty benefit would increase benefits for more than a third of new SSDI beneficiaries.REF Those who could be subject to lower SSDI benefits if they were to become disabled could purchase private disability insurance to add to the federal program’s benefits. Private disability insurance typically provides more generous coverage, higher benefits, and a more efficient determination process that takes about one-tenth of the time as SSDI.REF
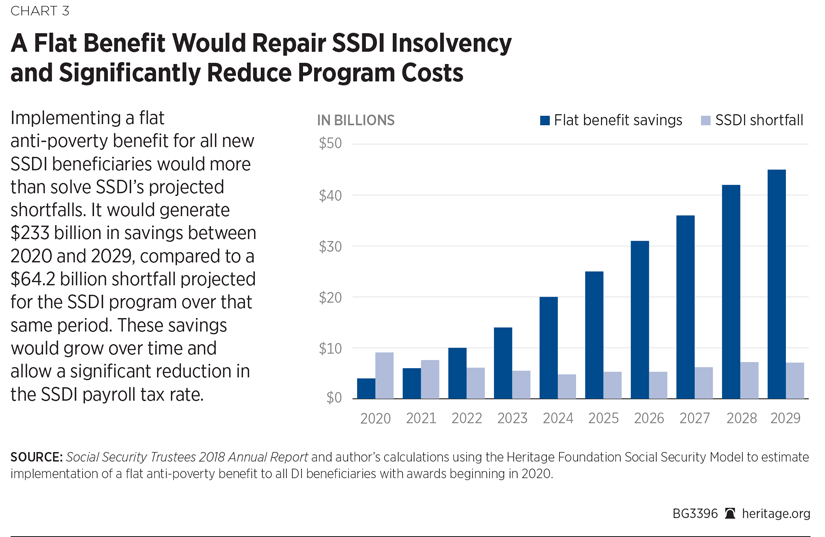
Savings: This proposal would save an estimated $188 billion over the next 10 years and would reduce the program’s 75-year shortfall by 220 percent.REF
10. End double-dipping. Currently, some individuals receive both SSDI benefits as well as Unemployment Insurance (UI) benefits. Yet, by definition, an individual cannot be disabled (meaning they are unable to work) and also unemployed (meaning they are ready, able, and willing to work). Congress should stipulate that individuals should be disqualified from receiving SSDI benefits in any month in which they receive UI benefits.
Savings: This proposal would save an estimated $6.4 billion over the next 10 years and would reduce the program’s 75-year shortfall by 8.3 percent.REF
11. Limit retroactive benefits to six months, instead of 12 months. When individuals apply for and eventually receive SSDI benefits, they receive two levels of back pay. First, they receive payments for all the months between when they first filed for SSDI benefits and when their claim was eventually approved. Additionally, individuals can receive up to 12 months’ worth of “retroactive” payments dating back to their first month of disability onset. The SSDI program only requires that individuals wait five months, however, to apply for benefits after a disability onset. Thus, retroactive payments should be limited to six months to bring them in line with the program’s waiting period.
Savings: This proposal would save an estimated $19 billion over the next 10 years and would reduce the program’s 75-year shortfall by 23.1 percent.REF
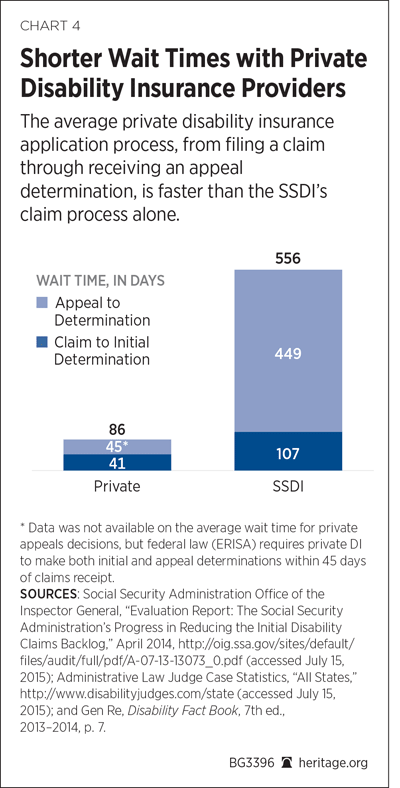
12. Offer an optional, private disability insurance (DI) alternative. Private DI has the financial incentive to provide efficient and accurate disability determinations and to help workers remain in their jobs through accommodations or to assist them in rehabilitating into new ones. While SSDI wait times often exceed 600 days, private DI determinations almost never exceed 90 days. Private DI also offers greater coverage and lower costs. Although it is not an apples-to-apples comparison, a typical private DI policy costs 0.5 percent of earnings or $250 per year while SSDI costs workers 1.8 percent of earnings or $900 per year.REF If individuals did not have to pay so much toward the federal SSDI program, they would have more money available to purchase a superior product for a lower cost from the private sector.
SSDI, on the other hand, is not only financially insolvent, but it fails to help individuals who are able, to recover and return to work. Losing the ability to work is a traumatic experience for most individuals, as work brings dignity and satisfaction. Most individuals who face disabling conditions would rather regain some work capacity and at least partially provide for themselves than become dependent on the government or others. Yet, the SSDI program does almost nothing to help individuals gain the capacity to work and it can even hinder their potential recovery by making individuals wait two years before they qualify for Medicare benefits.
If more workers had private DI, they would likely benefit from a more efficient disability determination process and significantly improved rates of returning to work. These benefits for individuals with disabilities would lead to lower SSDI costs. To improve both the well-being of individuals with disabilities and the efficiency and solvency of the SSDI program, Congress should allow employers and self-employed individuals to receive a payroll tax credit against their required disability insurance tax if they choose to provide their employees with qualified private DI (covering at least the first two years of disability benefits).REF
Savings: This proposal would save an estimated $14 billion over the next 10 years and would reduce the program’s 75-year shortfall by 19 percent.REF
13. Include unearned income in the measure of substantial gainful activity (SGA). Currently, only income earned through work counts toward SGA, but this allows individuals with significant unearned income from investments and other sources to receive disability insurance benefits that are intended to be for workers who do not have enough income to provide for themselves. It should not matter whether individuals receive income from work or from investment earnings. Although individuals can choose when to realize certain unearned income, this provision would at least help prevent benefits from going to those who have significant other means of income to provide for themselves.
Savings: Although this proposal would generate some savings by limiting SSDI resources to individuals with incomes below the SSDI earnings limits, the savings would be minimal because most people on SSDI do not have substantial non-earnings incomes. Thus, we do not include any estimated savings for this proposal.
Ongoing Eligibility. In addition to too many people entering the SSDI rolls, too few people ever leave the program to return to work. To better ensure that SSDI resources only go to the program’s intended population, policymakers should:
14. Establish time-limited, needs-based benefits. Disabilities vary significantly from person to person, and yet, the current system prescribes a one-size-fits-all benefit structure that fosters government dependence instead of personal autonomy and independence. The SSDI program does this by failing to set expectations that individuals will return to work upon recovery, and failing to end benefits if individuals become capable of working. Even with a significant uptick in return-to-work rates in 2016, less than 1 percent of beneficiaries exited the rolls due to medical improvement or earning above the SGA level,REF and less than 3 percent of SSDI beneficiaries ever exit the program in order to return to work.REF
Most individuals with disabilities would far rather work and support themselves, and many individuals with disabilities are capable of working in some capacity. However, the SSDI program has become an effective benefits-for-life model that does little or nothing to help and encourage individuals to get back to work if they are able.
Congress could better meet the needs of individuals with disabilities and more appropriately target program resources by implementing a needs-based benefit structure.REF Individuals who qualify for SSDI with temporary conditions that are expected to improve with time and treatment would receive a needs-based benefit for a limited time of two years, coupled with incentives to help them transition back to the labor force.REF Individuals with temporary benefits whose conditions failed to improve would be eligible to reapply for benefits via an expedited review process, within six months of their benefits expiring. Individuals with terminal or deteriorating conditions would continue to receive benefits without a time limit, as is the case today.
Savings: This proposal would save an estimated $4 billion over the next 10 years and would reduce the program’s 75-year shortfall by 7 percent.REF
15. Strengthen continuing-disability reviews (CDRs). Individuals who recover from a disability and regain the capacity to work are supposed to leave the program and return to work. Yet, virtually everyone who enters the program—about 97 percent—stays in the program. Part of this is due to the fact that SSDI does almost nothing to help individuals return to work, but a lack of sufficient enforcement by the SSA is also to blame. The SSA is supposed to conduct CDRs either every three years or when the commissioner determines them appropriate, depending on disabled workers’ initial disability determinations.
Yet, often CDRs are not conducted as scheduled, and in many instances, CDRs consist of nothing more than mailing beneficiaries check-the-box postcards to ask if they are still disabled. Comprehensive CDRs are an important component to maintaining program integrity and preventing individuals who are no longer unable to work from continuing to receive benefits. Congress should require the SSA to conduct a CDR every two years for individuals with disabilities for whom improvement is expected, and every five years to seven years for all others.
Savings: This proposal would save an estimated $12 billion over the next 10 years and would reduce the program’s 75-year shortfall by 15.8 percent.REF
16. Eliminate the Medical Improvement Review Standard (MIRS) in the CDR process. When the SSA performs CDRs to determine if individuals are still unable to work, it uses an MIRS. This standard dictates that an individual remains disabled if his condition has not improved since the initial determination. Initial determinations are sometimes inaccurate, however (whether due to rubber-stamping judges or false reports), or individuals could have multiple disabling conditions and recover from some but not all. The MIRS can allow individuals who would not otherwise qualify to receive benefits to continue doing so. Congress should eliminate the MIRS and mandate that CDRs rely instead on the same disability determination standards as the original determination process.
Savings: This proposal would save $2 billion over the next 10 years and would reduce the program’s 75-year shortfall by 3.4 percent.REF
Conclusion
Following alongside strong economic growth over the past few years, fewer people are using SSDI as a long-term unemployment program. Although this has partially alleviated SSDI’s projected deficits, the program is still insolvent (it is projected to run out of money around 2032) and still in need of substantial reform. Regardless of its finances, the SSDI program suffers massive inefficiencies, it does not serve individuals with disabilities well, and it is plagued with misuse and abuse.
Comprehensive SSDI reform should emphasize recovery over dependence, focus benefits on preventing poverty rather than replacing income, correct inefficiencies and inequities in the determination process, and improve the integrity of the program to preserve benefits for those who truly need them.
Following those criteria, Congress and the SSA should: (1) eliminate the qualification “grids”; (2) update the official list of available jobs in the national economy; (3) allow use of social media in eligibility determinations; (4) eliminate the reconsideration stage; (5) end direct payment to SSDI representatives; (6) apply judicial code of conduct to ALJs; (7) conduct reviews of outlier judges; (8) reduce target caseloads for ALJs; (9) enact a flat, anti-poverty benefit; (10) end double-dipping; (11) limit retroactive benefits to six months, instead of 12 months; (12) offer an optional, private DI alternative; (13) include unearned income in the measure of SGA; (14) establish time-limited, needs-based benefits; (15) strengthen continuing disability reviews; and (16) eliminate the MIRS in the CDR process.
Each of these changes would improve the SSDI program, and together they would transform it into a vastly more effective, compassionate, and responsible program that meets the needs of individuals with disabilities at less than half the cost of the current program.
—Rachel Greszler is Research Fellow in Economics, Budget, and Entitlements in the Grover M. Hermann Center for the Federal Budget, of the Institute for Economic Freedom, at The Heritage Foundation. Drew Gonshorowski is Senior Policy Analyst for Simulations in the Center for Data Analysis, of the Institute for Economic Freedom. Romina Boccia is Director of the Hermann Center.
Appendix: About The Heritage Foundation Social Security Model
The Heritage Foundation Social Security Model includes a dynamic microsimulation model that allows for analysis of policy changes in the Social Security Disability Insurance program. This model is based on current-law policy and can simulate the individual effects of many types of reforms, ranging from small changes in eligibility to big changes in payroll taxes and benefit levels.
This model simulates the lifetime social security experience of birth cohorts based on scenarios defined by assumptions in the most recent Social Security Trustee’s report. Alternatively, the model can simulate uncertain scenarios using a Monte Carlo method. Such a method essentially runs the model hundreds, or even thousands, of times while allowing standard assumptions, such as labor force participation, birth rates, or economic growth to vary across each run. Monte Carlo simulations provide a range of outcomes as opposed to a single point estimate.
A score represents model runs that change these scenarios according to the new policy and compare it to a simulation that represents current law, or a baseline scenario. The Heritage model provides effects over the short term (annual levels) and long term (stretching up to 75 years in the future).
Policies scored in this Backgrounder tend to include changes to take-up rates, or disability incidence rates, depending on the different scenarios. Where possible, we incorporate independent and outside research to inform expectations, or assumptions, for model runs.