Governors and state legislators have important roles in managing the eventual wind down of the federal COVID-19 public health emergency (PHE). It is critical that state leaders are prepared to restore their conventional authority over the Medicaid program. After the official federal PHE ends—currently expected on June 30, 2023—and the enhanced federal funding expires, states will have up to 12 months to resume normal eligibility and enrollment operations. This is referred to as the “wind down” period. It is in the states’ budgetary interest to complete this wind down in as short a time as possible.
Enrollment in Medicaid and the state Children’s Health Insurance Program (CHIP) has increased by approximately 18 million people since March 2020, and now totals nearly 90 million individuals at a total cost of approximately $800 billion. The federal regulations that require eligibility to be redetermined once every 12 months have been suspended for more than two years in almost all cases except for death or proof that an individual has moved out of state.
Just as new governors take office and new state legislatures convene in January 2023, forecasting a state’s Medicaid budget will be a challenging task as three factors converge. First, more than $50 billion in extra funding from the federal government through Medicaid will likely end at some point next year.REF The PHE-enhanced match rate for Medicaid was always intended to be temporary. Accordingly, states, Medicaid health plans, and providers should have been planning and preparing for that day. Poor planning cannot be an acceptable excuse for delays in implementing the state’s wind-down procedures.
Second, Medicaid non-general fund accounts (such as from provider taxes and interagency transfers), which are larger today due to higher utilization during the COVID-19 pandemic, will also be on the decline. It is important that executive branch agencies and legislative branch committees with oversight of Medicaid spending not be lulled into a false sense of security based on how flush those accounts appear today. As these funding levels dissipate, health care providers and plans will likely push legislatures for additional funding through the rate-setting process to replace lost revenues.
Finally, the only time to know how well a state has prepared for the PHE wind down is when people are disenrolled from the program. The Centers for Medicare and Medicaid Services (CMS), the media, advocacy groups, and legal aid agencies will all be watching for cases in which individuals were allegedly improperly disenrolled. This means that each state should conduct a robust education and outreach campaign which is vital to assist those who are disenrolled from Medicaid in obtaining other available coverage, such as through employers or the individual insurance marketplace.
COVID-19 and PHE Statistics
There are many axioms in health care, but two of the most important are that (1) everything in health care inherently involves risk, and (2) almost everything in health care involves imperfect knowledge. Walking across the street or driving a car entails risk. People make decisions every day for themselves, for loved ones, or for strangers that they pass on the highway that are thousands of little acts of assessing situations and taking risks. Imperfect knowledge begs the question: “How much of our freedom does one surrender to lower the risk of catching a certain disease?” Overall, Americans have decided that the disruptions in their lives caused by further isolation is too high a price, given the risk. The American people have determined that COVID-19 is no longer a public health emergency through their own actions.
National data for tracking hospitalizations due to COVID-19 from the Centers for Disease Control and Prevention (CDC) provide further confirmation that the national public health emergency has passed.REF Table 1 shows the significant declines in hospitalization rates by age group for the week ending November 19, 2022 (the most recent week available) compared to one year ago, as well as to the highest peak in January 2022 and the second highest level in January 2021.
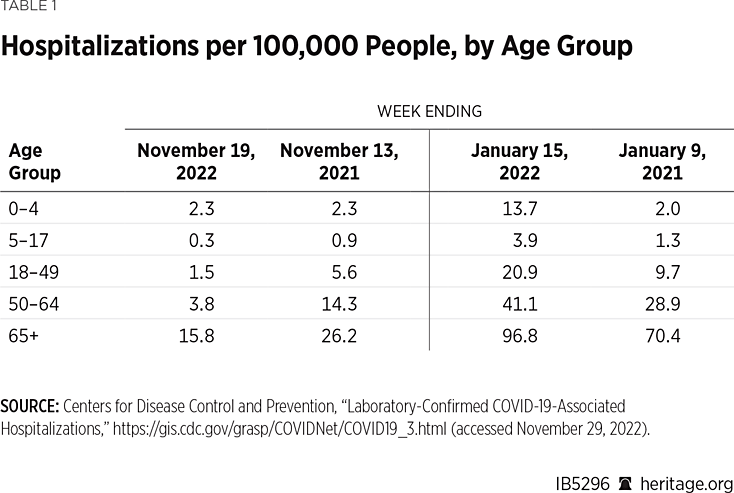
Medicaid and the Public Health Emergency
Section 6008 of the Families First Coronavirus Response ActREF offered states a 6.2-percentage-point increase in their Medicaid Federal Medical Assistance (FMAP) percentage. In return, a state would suspend its regular Medicaid eligibility redetermination process so long as the PHE is in effect. Every state accepted this federal funding option.
A state with a regular 50/50 match rate realized a 12.4 percent increase in federal funds; a state with 60/40 received a 10.3 percent increase; and a state with a 70/30 match received an 8.9 percent increase. Although the increase did not apply to the new adult group in Medicaid, which remained at 90/10, states were required to suspend disenrollment for this population as well. The Congressional Budget Office (CBO) estimated that Section 6008 would increase federal spending by $50 billion over the 2020–2022 period.REF
As a result, enrollment in Medicaid and CHIP has increased by approximately 18 million people since March 2020. In May 2022, the CBO reported that the actual cost of Medicaid and CHIP totaled $537 billion in federal fiscal year (FY) 2021, and it projected that costs would increase to $606 billion in FY 2022 and to $619 billion in FY 2023 before falling to $552 billion in FY 2024 after the PHE expires.REF The total cost of Medicaid, counting the state share, now exceeds $800 billion annually.
The enhanced match rate is not the only CMS action tied to the PHE. If the Secretary of Health and Human Services declares an emergency under the Public Health Service Act, “CMS is empowered to temporarily modify or waive certain Medicaid, CHIP, and Medicare requirements as determined necessary by the agency under Section 1135 of the Social Security Act (the Act).”REF In addition to Section 1135, the CMS has regulatory authority to provide exceptions to several procedural actions that the state cannot carry out due to an emergency or disaster. States can also modify their section 1915(c) Home and Community Based Services through an “Appendix K” amendment.REF As a last resort, a state can submit a Section 1115 Demonstration Project.REF
At the request of states, the CMS has temporarily waived hundreds of Medicaid and CHIP rules during the PHE, which the states must decide to continue or to discontinue by filing more permanent state plan amendments (SPAs) or waiver amendments. Options for continuing the SPAs include:
- Expanding eligibility for certain optional Medicaid eligibility groups,
- Applying, temporarily, less restrictive income and resource disregards;
- Increasing the personal needs allowance under post-eligibility treatment of income;
- Suspending the waiting period for CHIP applicants;
- Determining eligibility at application based on self-attestation;
- Suspending co-payments;
- Suspending payment of premiums;
- Modifying, temporarily, provider types who are authorized to remotely monitor and treat patients;
- Expanding the use of telemedicine; and
- Extending new payment methodologies for telemedicine.
Recommendations
Since December 2020, the CMS has issued multiple forms of guidance through a series of notices, Frequently Asked Questions, and informational documents in anticipation of the end of the PHE and the subsequent “wind down” period. These documents cover dozens of technical issues and many of these documents were developed with the input of states and are part of the “toolkit” that states must review and consider.
What is clear is that states cannot simply flip a switch to return to pre-COVID-19 operations. Every eligibility decision directly affects the lives of vulnerable seniors, people with disabilities, and children and adults near or below the poverty level. Every financing decision affects not just the Medicaid budget, but the state budget as a whole.
Now is the time for states to act in order to be prepared for the end of the PHE. Here are some practical steps state leaders should consider:
-
Resist New Funding Requests. The projected $67 billion (10.8 percent) reduction in federal funding between 2023 and 2024 will create a storm of providers, health plans, and vendors pushing back against the lower level of funding. While state costs will decline as the number of Medicaid enrollees return to pre-COVID-19 levels, providers will press to increase rates to make them “whole” from any new gap between costs and revenue.
Providers will seek to replace two to three years of lost revenues with double-digit payment rate increases. Institutional providers that are dependent on “heads in beds” and cost-based reimbursement will line the halls of state capitols with dire predictions of closing their doors without a fresh source of funding. The National Association of State Budget Officers reports that the collective budget stabilization funds (“rainy day” funds) total $132.2 billion,REF but these funds can be drained very quickly during what is likely a present or impending recession.
Despite tremendous pressure to replace as many federal dollars as possible, states should resist efforts to simply approve new higher payment rates for providers. Any new funding should be linked to some type of payment reform that improves value and outcomes.
Approximately half of Medicaid expenditures go through Medicaid managed care organizations (MMCOs). Since states make capitation payments to MMCOs at the beginning of every month, disenrolling as many as 15 million ineligible people from Medicaid will have an immediate, positive financial impact on the states. Each month of delayed action costs the states money.
Tensions between payers and providers are already building. States should view the end of the PHE as an opportunity to inject reforms based on competition, transparency, and value.
-
Establish a Command Center to Coordinate an Efficient and Effective Wind Down. There must be a sense of urgency needed to accomplish this task. Each state Governor should make restoring control and authority the top task of the Cabinet-level Secretary who is responsible for the Medicaid single state agency. Medicaid is typically administered by different divisions within the state equivalent of the federal Department of Health and Human Services (HHS). Eligibility is typically processed outside Medicaid by a division that also determines eligibility for other means-tested programs. An Office of General Counsel, or even a separate office, may conduct appeals and hearings. Therefore, the command center should be headed by a senior-level official who would report directly to the respective state departmental Secretary, and who would include input from the various respective divisions.
In an effort as massive and far-reaching as the PHE wind down, implementation will not be perfect. The critical purpose of the command center is to identify problems as they arise and have all the right personnel working together to solve them. A beneficiary outreach team and a provider outreach team should start to work no later than mid-March 2023. No matter how well prepared, someone at some point in June (assuming disenrollment has begun) will not be able to have a prescription filled, or will have another service denied. The first call for assistance may go to Medicaid; the second call for assistance will go to Governor’s office or a state legislator. Next, especially if it involves an older person or a person with a disability, the problem will cause a firestorm on social media and will potentially result in a complaint to be filed by the individual with the HHS Office for Civil Rights or in litigation.
It will be important to track key data changes for at least three months after the end of the PHE in order to measure performance: How many complaints? How many were resolved? How many still outstanding? How long did it take to close the complaint?
-
Target Resources to IT Systems and Eligibility Staff as Needed. States have invested significant resources in their IT eligibility systems in recent years. Automation, which has enhanced the use of ex parte communications, has delivered positive results in the accuracy and timeliness of determining and redetermining eligibility. However, some states still use ex parte communications in not even half of the caseload. With the large volume of eligibility and enrollment actions to be taken during the wind down period, automation will be key to reducing the need for manual processing.
States should also assess their need for bringing in contract staff to process applications for the modified adjusted gross income (MAGI) population which is about 80 percent of the Medicaid caseload. There are vendors with eligibility experience that can contract with states within a matter of weeks to process Medicaid applications, although a public employee must still sign off on the final determination. Assigning contract staff to MAGI cases, which are virtually identical across the country, frees up state and county staff to process the more complex applications of the non-MAGI population.
-
Accelerate Household Eligibility Redeterminations. States have continued to update case files but not take final action on changes in circumstances that affect eligibility based on the composition of the household (age of individual, marriage, divorce). States have less information about changes in income. States will need to ramp up income data matching and verifications. The older a piece of information is, the less reliable it is.
Because of the volume of redeterminations (and potentially new applications as disenrollment proceeds over the months), states may consider different ways to prioritize by individual eligibility groups (such as new adult group, parent and caretaker relatives, Medicaid children, and CHIP children). To avoid processing multiple applications for each different member of the same household, the state should focus on household eligibility redeterminations rather than individual redeterminations. Every parent or caretaker relative by definition has a dependent child in the household. While there is a widespread perception that the new adult group (Medicaid expansion) includes only childless adults, a significant percentage of those adults also have a dependent child in the household.REF
-
Anticipate Litigation. The CMS certainly will exercise close scrutiny of the wind down process. Noncompliance presents financial risk in the potential loss of federal funding. In addition, legal aid service organizations are likely preparing to sue states that allegedly remove individuals improperly from Medicaid programs. If they have not done so already, state Medicaid agencies should review each and every step of their notification process with their General Counsel and Office of Hearings and Appeals, and even their state Office of Attorney General is able to withstand legal challenges. For example, states are vulnerable if notification is not clear or timely, and they are vulnerable if they do not follow their own procedures.
-
Determine Which Emergency Measures to Keep. Eligibility is the major feature for states during the PHE, but not the only focus. The CMS has provided several flexibilities to states in the administration of their Medicaid programs. The CMS “toolkit” includes flexibilities under various authorities including Section 1135, Section 1115, and the Appendix K amendment) for program administration, such as:
- Increased use of telemedicine;REF
- Expanded roles of providers (for example, permitting pharmacists to administer vaccinations);
- Directed payments from MMCOs to providers; and
- Shortcuts to procedures that are linked to eligibility, such as independent assessments, which are used to identify functional deficits.
- These temporary flexibilities are also linked to the duration of the PHE. States must determine which of these temporary changes they want to make permanent and monitor and assess them moving forward.REF To do so, states must file new SPAs, rates, and waiver changes with the CMS. For its part, the CMS must ramp up to focus almost exclusively on these state requests. This is not to say that the CMS must approve anything and everything a state submits, but rather, that the process needs to be done quickly, so that a state understands its budget situation. The CMS processes and procedures that can delay decisions half a fiscal year will be detrimental to states.
Conclusion
A narrative that allows outside groups to define the entire wind down operation as “losing Medicaid” is perilous for state elected leaders and senior executive branch appointees. A successful transition out of the PHE will require many partners. As governors and legislators take their oaths of office in the next 60 to 90 days, they will understandably want to focus on the issues on which they campaigned. How to wind down the PHE was probably not one of them. But the wind down will be one of the most important issues of the upcoming legislative session.
Dennis G. Smith, Head Coach of Medicaid Strategies, was Director of the Centers for Medicaid and State Operations in the George W. Bush Administration. Nina Owcharenko Schaefer is Director of the Center for Health and Welfare Policy at The Heritage Foundation.



