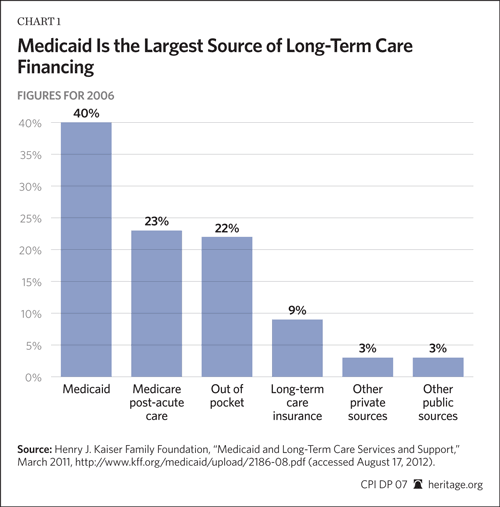
The Obama Administration’s suspension of the Community Living Assistance Services and Supports (CLASS) Act provisions of the Affordable Care Act halted a new federal entitlement program that was fiscally unsound. The repeal of the CLASS Act as part of the American Taxpayer Relief Act provides an opportunity for a necessary discussion.
The debate over the CLASS Act highlights a powerful truth. Long-term care (LTC) in the United States is in crisis. A set of interrelated financial and organizational problems in the current public and private systems will converge and reach a fiscal crescendo with the aging of the huge baby-boom generation. Already, the current system is not meeting the needs of the frail elderly and disabled populations who require assistance with tasks of daily life. The funding is a disjointed array of private funding, Medicaid, and private long-term care insurance. Public and private policymakers need to review the current state of affairs and consider possible reforms.
What Is Long-Term Care?
LTC involves the need for assistance, including prompting, with activities of daily living (ADLs). ADLs include bathing, transferring, toileting, and dressing, and incidental activities to daily living (IADLs), which include cooking, housekeeping, transportation, and managing finances.[1]
Long-term care can be provided informally or formally in a variety of settings. Options for care settings have expanded dramatically in recent decades to include expanded formal home care, aging in place communities, naturally occurring retirement communities, independent and assisted living facilities, and a continuum of care communities. Yet family and friends provide the majority of long-term care informally and without pay.[2] The hidden economic impact of this informal unpaid care, primarily on family members, includes reduced household income due to time and focus away from work and the costs that are incidental to care.[3]
Long-Term Care Users
LTC users fall into two categories: the disabled[4] and the frail elderly. Specific care needs are highly individualized and vary depending on personal circumstances, abilities, and goals. Care provided to disabled Americans typically focuses on maximizing independence and enabling them to lead long, productive, and fulfilling lives. By contrast, care for the frail elderly typically reflects the challenges of the aging process and, inevitably, end-of-life goals and issues.
The Disabled. The term “disabled” encompasses a variety of physical and cognitive impairments that limit one or more major life activity.[5] In recent decades, the disabled population has increased, partly due to improvements in medical care that have decreased mortality. However, most of this growth is due to states restructuring support services for the disabled and replacing an array of programs targeted toward specific subsets of the disabled population with care provided through the Medicaid program.[6] Not all disabled individuals require LTC support, and many may require only intermittent care.
The source and onset of the disability also heavily impacts the ability of a disabled individual or the family to self-finance care. However, current policy does not relieve the family of its responsibility to assist and support the disabled individual to a reasonable extent. Still, it is accepted that societal resources will often be required to support and complement family care and to provide care when family support is not available.
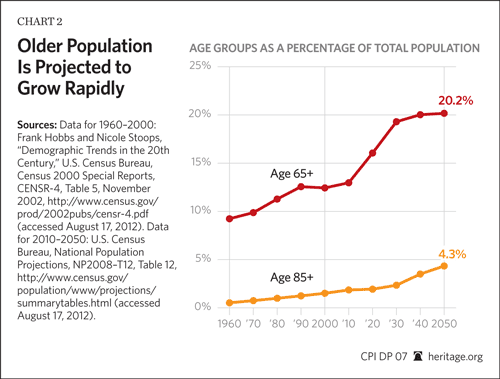
The Frail Elderly. The frail elderly are older adults with any combination of chronic conditions, including dementia, or who require assistance with daily activities due to mental or physical deterioration. Usually, “elderly” refers to those over age 65. However, those over age 85, often called the “oldest-old,” are most likely to be frail and require LTC assistance. The oldest-old population will grow dramatically in the coming years.[7] The baby-boom generation began to turn 65 in 2011 and within 20 years will double the 65+ population and increase the 80+ population by 110 percent.[8] At least 70 percent of baby boomers are expected to need some LTC services at some point, and 40 percent are projected to require nursing home care.[9] These numbers may prove conservative as medical innovations increase life expectancy even further.[10]
Other demographic patterns for the baby-boom generation indicate their sheer numbers are not the only factor likely to strain the LTC system. Compared with previous generations, the baby boomers are more likely to be divorced, have fewer children, and have female children in the workforce—all factors that make informal family care less likely and more difficult for caregivers.[11] Further compounding the problem, they have not saved enough for general retirement expenses and are especially unprepared for unplanned expenses such as LTC needs. Often, they expect cash-strapped government entitlement programs to fill the savings gaps.[12]
Financing Long-Term Care
Long-term care is expensive and becoming more expensive. Indeed, LTC costs have outpaced inflation since 2003.[13] Nationally, the median annual cost of a private room in a nursing home is $90,520.[14] Because the majority of Americans do not plan in advance to fund LTC, government programs currently account for 63 percent of LTC funding, with Medicaid paying for 40 percent and Medicare paying for 23 percent in the form of post-acute care.[15] The remaining 37 percent comes from out-of-pocket spending (22 percent),[16] LTC insurance (9 percent), other private sources (3 percent), and other public sources (3 percent).[17] Of course, this does not include the cost of unpaid care, typically provided by family members.[18]
Taxpayer Funding. Taxes are the largest source of LTC funding, with the majority of payments made through Medicaid, which is financed by state and federal taxpayers. With more middle-class Americans failing to plan for their future LTC needs, the program has effectively become the default payer rather than a safety net of last resort for the poor. The resulting strain on Medicaid threatens to undermine the original purpose of Medicaid. The strain from middle-class beneficiaries especially threatens acute-care and chronic-care medical services for the indigent. Increasing and widespread reliance by LTC users on Medicaid has helped to increase spending to unsustainable levels. With the baby boomers entering retirement and later entering the ranks of the oldest-old, even greater expenditures are on the way.
Medicare Does Not Cover LTC, but Medicaid Does. LTC generally is not really medical care, but instead assistance and support with daily tasks that an individual cannot perform due to physical or cognitive impairment.[19] Most middle-income Americans are unaware of the crucial fact that Medicare generally does not cover LTC expenses.[20] Although Medicare covers some LTC-type services for short durations after hospitalization, these “post-acute care” services[21] are provided for short time frames to help the patient to improve or to prevent further deterioration.[22]
Although baby boomers report health care as a major concern in retirement, they are largely unaware of the lack of LTC funding in Medicare, adding to worries about the future demands on Medicaid. Adult children who are conscious of the financial threat to their potential inheritance might be relieved, however, to discover that Medicaid eligibility disregards certain assets, such as an automobile and a primary residence.[23] Moreover, any stigma normally associated with welfare dependence is often eased by the growing reliance on government assistance in other areas of life. In fact, according to opinion surveys, the belief that Medicaid coverage for LTC is a “middle-class entitlement” is becoming increasingly accepted as a normal state of affairs, along with the belief that “the government has a responsibility to us.”[24]
Medicare–Medicaid Cost Shifting. The growth of Medicaid as a long-term care funding program has created some unintended incentives and financial consequences. For instance, with Medicare as the primary payer of medical services for many users of long-term care, an LTC facility has an incentive to avoid providing certain types of medical care in order to justify transferring a patient to a hospital so that the hospital covers the costly procedures. Although Medicare does not pay for LTC, it does pay for rehabilitative services after a qualifying hospital stay. However, post-acute rehabilitative care often involves many of the same services that LTC facilities would provide, with the only difference that post-acute rehabilitative services are provided for a short duration.
However, Medicare post-acute care payment rates are substantially higher than Medicaid LTC reimbursements.[25] This higher reimbursement rate creates an incentive for the LTC facility to fill as many beds with money-generating post-acute Medicare patients to compensate for often money-losing Medicaid patients receiving similar services. This incentive occurs across patient populations as well as with the same patient at different times during their stay. For instance, a patient sent for a short hospitalization can be readmitted to the same LTC facility a few days later, but at the higher Medicare rate. In addition, the LTC facility has a further incentive to transfer a sick patient to a hospital because Medicare does not reimburse the facility for additional expenses, such as isolating the patient or providing special staff. These incentives increase costs for both Medicaid and Medicare and, more importantly, result in inferior patient care.[26]
Many analysts and regulators have suggested that better coordination between payments from Medicaid and Medicare would not only reduce costs, but would greatly enhance patient outcomes.[27]
Private Financing. Private financing accounts for about 22 percent of LTC spending.[28] The main sources are insurance and direct payments from savings or borrowed funds, such as from reverse mortgages.
Long-Term Care Insurance. One way that people plan for possible LTC expenses is by buying long-term care insurance (LTCi). Currently, 8.1 million individuals have some form of LTCi protection.[29] Although the specific coverage varies based on the policy, LTCi policies cover the cost of assistance with basic daily tasks when required for an extended period of time. However, LTCi is a relatively new product, which has experienced growing pains.
In 2007, a series of stories about policyholders facing extreme difficulties in obtaining benefits and about wrongfully denied claims has caused many to question the utility of LTCi.[30] Yet a Department of Health and Human Services (HHS) study that found that insurers “erred slightly on the side of approving claims that may not meet policy contract benefit eligibility”[31] has done little to change public perceptions. Adding to the perception problems, LTCi policies are undergoing rate increases despite rate guarantees.[32] These increases are the result of actuarial assumptions that proved incorrect[33] as well as interest rates that have been below historic levels and thus have reduced insurers’ investment income.[34] To pay for future care, insurance companies rely on investment income, but investment income has fallen far short of costs at the current near-zero interest rates, requiring premium increases to cover the difference. Despite sharp rate increases, in some cases up to 90 percent, the majority of policyholders have retained coverage either by paying higher premiums or by modifying their coverage.[35] Policyholders cite the security of knowing that they can choose the type and location of care and will not be a burden on family as the major reasons for purchase and retention, although some also cite asset protection as a motive.[36]
Hurdles to LTC Insurance Enrollment. LTCi has remained a small niche market product, largely because potential buyers persuade themselves that they do not require insurance when it is affordable earlier in life.
Several reasons account for why families that would be wise to buy LTCi do not buy it. Some are psychological, such as denial about the possible need for future nursing home care. Others involve a lack of knowledge of potential LTC needs or the erroneous assumption that their other insurance or Medicare provides coverage. In addition, competing financial concerns, resistance to perceived high premiums, limited product choice, and product complexity also discourage purchase of LTCi. Private options are also burdened by crowd-out from social safety net programs.[37]
While many working Americans know parents, friends, or neighbors who receive care through Medicaid, they often fail to understand the severe limits of Medicare coverage and erroneously believe that Medicare covers LTC services. This generalized faith that the government will ultimately provide for any necessary care further encourages them to avoid the expense, complexity, and discomfort of purchasing LTCi. For about two-thirds of the wealth distribution, Medicaid replaces benefits that a private LTCi plan would pay.[38] This leads many potential enrollees to conclude that premium payments for private insurance are simply wasted on coverage already provided by the government without additional cost.[39]
The psychological obstacle is understandable. Many Americans flinch from imagining a time when they will require assistance with fundamental activities of daily life such as bathing. Misunderstanding of the potential need for care is also widespread. A baby boomer has a 70 percent chance of requiring some LTC, yet most are unaware that the probability is this high. Even those who rationally know the likelihood of needing care often convince themselves that they will somehow be in the 30 percent who will not require care. Even when the lack of knowledge and denial are addressed, a personal preference for in-home care by family may dissuade some from purchasing insurance, concerned that adult children will expect parents to use paid care if the financial incentives are eliminated.
Once a person is willing to consider the future need for LTC services, concerns about the insurance itself may discourage purchase. The high premiums coupled with unpredictable rate increases may make many potential buyers with fixed retirement incomes hesitate. Marketing materials focused on an asset protection component may induce some working Americans to purchase LTCi, but those without significant assets or substantial retirement savings may conclude that they do not need coverage. Many possible buyers do not enroll because they do not understand the purpose of LTCi. Some marketing materials focus on LTCi as a supplement to Medicaid, as in Partnership Program policies, whereas other companies market the insurance as a way to avoid the constraints and poor quality of Medicaid. At best, commentators send mixed messages about whether middle-class consumers should purchase LTCi.[40]
Company presentations of products inappropriate to the income and assets of consumers further impede purchase. Many potential consumers may choose not to purchase a policy when faced with unknown or confusing insurance terminology. For example, they may not understand “elimination period” or how long is appropriate for their circumstances. According to the American Health Insurance Plans, 49 percent of prospective customers chose not to purchase LTCi because of policy terminology and options that are “too confusing.”[41] In trying to simplify their options, some consumers select federally qualified plans, which may actually be more comprehensive and expensive than their circumstances justify.[42]
An additional obstacle is underwriting requirements. About 20 percent of LTCi applicants are denied coverage due to personal health or family history.[43] Still others, believing they will fail underwriting, do not even apply, or they are discouraged from applying by agents or by other family denials.[44] Coincidentally, these people are more likely to incur high LTC costs and are well positioned for Medicaid planning because they have an opportunity to plan and no alternative to self-funding.[45]
Self-Financing. As the baby-boom generation enters retirement, it has become increasingly apparent that their lack of financial planning has left them with insufficient savings for retirement.[46] Social Security provides income for basic living expenses, but is insufficient to protect against large or unexpected expenses. Average retirement savings for the boomers is around $75,000,[47] but a single year of nursing home care can cost over $80,000, and the cost of nursing home care has increased faster than inflation since 2003.[48]
401(k) Retirement Savings. Future generations and younger baby boomers are expected to rely more on their own savings as defined-benefit pension plans are declining.[49] In particular, 401(k) accounts are an option for covering some LTC costs. These accounts have been available to all Americans since 1981, although they have only been very popular since the 1990s. This means today’s retirees were not able to save in 401(k) accounts for much of their working life, and although older workers can make higher “catch-up” contributions, many do not and these contributions typically do not fully make up for the years before 401(k) availability. It will likely be another 20 years until new retirees will have had the opportunity to save in 401(k) accounts for an entire career. Only then will it be clear whether the 401(k) accounts have affected retirement savings sufficiently to significantly affect personal funding for LTC.[50] With increases in life expectancy causing future generations to reconsider how they work, save for retirement, and view government entitlement programs, the financial outlook for future generations is still unclear. Nevertheless, LTC will remain a major issue for retirement planning and saving.
Home Equity and Reverse Mortgages. Although retirees are unlikely to have extensive savings, 80 percent of older households own their home, including 78 percent of those who are 75 and older.[51] This wealth in home equity is largely exempt from Medicaid eligibility requirements, frequently leaving it untapped for LTC expenses. Some consumers are willing to spend this equity for a preferred living setting not eligible for Medicaid funding, such as assisted living.[52] Consumers frequently report their belief that these settings offer good value as the reason for liquidating housing assets.[53]
This option can open up additional care settings, and homeowners who have used reverse mortgages to pay for preferred LTC report being very happy with their decision.[54] Selling is one means of liquidating equity, but a reverse mortgage is an alternative to selling.[55] The reverse mortgage was introduced in 1960 as a means of allowing those age 62 or older to use the equity in their home. Similar to a home equity loan, it can be taken as a fixed monthly amount, a lump sum payment, or an available line of credit. However, unlike a regular home equity loan, repayment does not begin immediately. The homeowner must be living in the home and remains responsible for real estate taxes, homeowner’s insurance, and the costs of repairs. Upon the death of the homeowner or absence from the home for a year, the loan must be repaid or the home sold to repay the amount of equity used. Under federal law, if the loan amount is greater than the sale price of the home, the difference must be forgiven.
Homeowners have generally been slow to embrace reverse mortgages, although they are gaining in popularity. In recent years, younger and younger borrowers are tapping their home equity for other purposes, such as paying for their children’s college tuition, so most of the equity may not be available later in life when LTC expenses occur.[56] In addition, this option is not available for residential care longer than one year because the borrowed amount becomes due after a one-year absence from the house. Any unused money from the reverse mortgage will be considered for Medicaid eligibility. Furthermore, the incentive to use home equity to pay for care is limited because the current median home sale price of $244,000 is well below the $525,000 threshold for home equity that is exempt when determining Medicaid eligibility.[57] Furthermore, as government programs expand qualified care settings, the value of these settings no longer justifies the use of housing equity, and their value may diminish as taxpayer-funded government options replace the use of personal resources.
Long-Term Care Policy Efforts
Beyond the failed and unworkable CLASS provisions in the Affordable Care Act, a variety of policies have attempted to address long-term care issues. However, these reforms have focused on the margins and have not resolved the underlying problems or provided a fiscally sound approach to funding LTC.
Medicaid and Medicare. Medicaid and Medicare are both facing growing financial strains as costs soar and demand increases. Medicaid is consuming increasing portions of state budgets, and Medicare’s long-term unfunded obligations are estimated as high as $36.9 trillion in present value dollars. Medicare has been running deficits in the Hospital Insurance Trust Fund since 2008. Medicare costs will explode with the flood of new baby-boom enrollees.[58] The programs’ rapidly increasing costs are a source of great concern and have inspired various efforts to reform them.
Previous Medicaid reforms have included closing eligibility loopholes, such as setting stricter eligibility requirements, eliminating popular Medicaid planning techniques, reducing provider payments, and attempting to eliminate fraud.[59] However, these reforms have not significantly reduced the size of the program.
Federal efforts have also required the states to establish mandatory estate recovery for Medicaid LTC expenditures.[60] Conceptually, these laws allow states to recover LTC costs from exempt assets once the recipient has died. Although seemingly an important cost-saving measure, in practice estate recovery has had minimal impact. For instance, Medicaid estate recovery programs recovered $411.1 million in 2005—just 0.61 percent of total Medicaid spending. State recovery programs vary widely, as states grapple with the appropriate role and scope of recovery.[61]
Dual Eligibles. Recent policy reforms have focused on the target population of frail elderly who qualify for both Medicaid and Medicare. “Dual eligibles” are lower-income Americans who are eligible for Medicare and are eligible for Medicaid to cover the out-of-pocket costs associated with Medicare. This population has extensive and expensive medical and LTC needs because they tend to be sicker and more likely to have cognitive limitations. In 2008, dual eligibles accounted for 31 percent of Medicare spending even though they are only 20 percent of the Medicare population and for 39 percent of Medicaid spending even though they are just 15 percent of the Medicaid population.[62]
The lack of care coordination for this population is both a fiscal issue and a problem of delivering quality care. The Centers for Medicare and Medicaid Services (CMS) is currently overseeing a care coordination demonstration project to improve the ease of navigation and the quality of care. Participating states develop programs to manage the care of dual eligibles within CMS guidelines. Currently, 38 states have expressed interest and 27 currently have plans for implementation in 2013 or 2014.[63] Although these programs are promising, their effectiveness will not be clear for some time. Even if the results are encouraging, the ability to scale-up a successful program will pose another hurdle.
Partnership Programs. To provide an incentive to purchase LTCi, partnership policies offer Medicaid eligibility after the exhaustion of LTCi coverage even when the policyholder’s assets would otherwise make them ineligible. At its core, the incentive for the individual to purchase a partnership LTCi policy is, similar to any LTCi, to protect assets and increase personal control over care. The public policy intent is to decrease reliance on Medicaid by encouraging middle-income individuals to cover a portion of their LTC, with Medicaid providing catastrophic coverage if care needs far exceed the average. The program began as a four-state experiment, but the Deficit Reduction Act of 2005 expanded the program. As of July 2011, 40 states have such partnership programs.[64]
The goal of the partnership program is to ensure that LTC is available to those in need, while retaining Medicaid as a safety net for the indigent and those devastated by catastrophic care costs. The results have been mixed. Partnership qualified plans account for less than 9 percent of all LTCi policies in states with partnership programs.[65]
Qualified plans provide more coverage than average policies, an average lifetime benefit of $276,000 and an average premium of $2,437.[66] It is difficult to determine whether the partnership benefits have led to slight modification of existing policies or simply reward unrelated behavior.[67] Less than 1 percent of these policies have resulted in eventual reliance on Medicaid for LTC.[ 68]Partnership programs have increased policies sold with inflation protection, which ensure coverage amounts are sufficient for future care, but they have failed to increase the sale of “short and fat” policies that provide complete coverage for shorter periods of time.[69]
Another goal of partnership sales is to increase group sales with limited underwriting that allows otherwise uninsurable persons to obtain coverage. Yet this has produced meager results, with group policies representing less than 15 percent of the market.[70] Modifications of this incentive structure have been suggested, but have so far failed to garner widespread support.[71]
Tax Incentives. Tax policy, including state and federal tax credits and deductions, has also been used to encourage the purchase of LTCi. Federal tax incentives include allowing people to use health savings accounts (HSAs) to pay LTCi premiums, a tax deduction for premiums paid by employers or self-employed individuals, and a tax deduction for LTC expenses over 10 percent of income.[72] Studies examining the impact of tax subsidies have shown, at best, negligible increases in purchases of insurance.[73]
One study found that favorable tax treatment, regardless of the size of the incentive, draws attention to the importance of LTCi and increases the purchase of policies. However, it appears to have the greatest effect on higher-income individuals, who are already more likely to purchase without incentives and less likely to rely on Medicaid, even without insurance. Based on the current tax incentive designs, the study found that each dollar of lost tax revenues saves Medicaid only $0.84.[74] However, an analysis by the AARP Policy Institute suggests that properly formulated and targeted incentives may make a bigger difference.[75]
The CLASS Act. As part of the Affordable Care Act, Congress attempted to address LTC expenses through the CLASS Act, which created a voluntary government LTCi program run by the U.S. Department of Health and Human Services. It required that the premiums charged under the program make it financially sustainable and actuarially sound for at least 75 years. It was to be voluntary, self-financed, not use underwriting, and provide lifetime coverage and cash benefits. The benefits under the CLASS Act were not extravagant, just $50 to $75 per day, which typically would cover only one-fourth of the average cost of a semi-private room in a nursing home.[76] However, even at this minimal level of benefits, the Administration staff writing the regulations eventually declared that there was “no viable path forward for CLASS implementation” and suspended its implementation.[77]
The CLASS Act was doomed from the beginning. Senator Kent Conrad (D–ND) called the CLASS Act “a Ponzi scheme of the first order, the kind of thing that Bernie Madoff would be proud of.”[78] Congressional budget rules required Congress to examine the cost of only the first decade of a program. But the CLASS Act would collect 10 years of premiums, while beneficiaries would only be eligible for the last five years, creating an artificial funding surplus 10-year budgeting period.[79] However, beyond the first decade, even HHS conceded that the new entitlement would become “totally unsustainable” and “financially unsound.”[80]
To address these obstacles endemic within CLASS, Urban Institute scholar Howard Gleckman has suggested that the government could instead impose a mandate requiring everyone to purchase private LTCi insurance, similar to the individual health insurance mandate in the ACA.[81] A mandate might resolve the low participation rate and adverse selection problems in the LTCi market, but the Supreme Court’s 2012 decision on the constitutionality of the individual mandate suggests that a federal mandate to purchase long-term care insurance would need to be designed as a heavy tax for nonpurchase rather than a legal requirement. Regardless of whether such a policy would be technically desirable or wise, it would undoubtedly provoke fierce political opposition.
Emerging Market Trends in LTC Financing
As legislative efforts on LTC financing continue, the marketplace is attempting to design new options for funding future LTC needs.
New LTCi Products. Consumers unhappy with the present options have spurred the market to introduce new LTCi products. For example, consumers concerned that policy premiums are lost if care is not required can now purchase premium return riders for some policies.[82] This rider provides cash value at the end of a specified period, although it makes the policy more expensive. For consumers considering the purchase of whole life insurance, an accelerated death benefit rider is available with some policies. This means the policyholder receives a cash advance on the death benefits to pay for LTC expenses. Such policies tend to require large up-front cash payments and usually involve underwriting requirements, so they may not be attractive for many consumers. Another option, if a large up-front cash payment is possible, is an annuity with a LTCi rider to provide increased monthly cash payments in the result of LTC needs. Additional product designs will likely continue to emerge as specific needs are identified, providing the regulatory environment continues to allow such innovations.
New Care Settings. Until the 1980s, paid LTC, as opposed to care from family and friends, was almost exclusively provided in a nursing home setting. The emergence of assisted living facilities, which combine levels of nursing or other assistance in a more independent setting, has provided new options and opened doors to new and innovative methods and settings for LTC. Assisted living facilities have now developed into independent living residences, and a continuum of care facilities allow patients to stay within the same community as their care needs increase over time. These settings allow for increased independence and self-determination while providing patients with the necessary care. Many of the elderly can now join communities with mechanisms to provide support services, such as the Urban Village Movement and other age-in-place organizations, within naturally occurring retirement communities.
The Urban Village Movement began as a grassroots organization in Beacon Hill, Massachusetts, as a way to connect an aging population to the resources and services they needed to remain in their homes. The movement has spread to over 100 villages that are either active or in development.[83] A village relies on a combination of neighbors helping neighbors, volunteers, and a range of health care and other service providers. In addition to providing a sense of community, these villages offer a variety of services from transportation to changing a light bulb. Coupled with community support, new technology will allow medical and assistance providers to monitor patients better in these settings, providing promptings for those with dementia, allowing rehabilitation outside hospital or nursing home settings, and more.
Such new care environments could lead to cost savings in government programs if they are integrated into government-paid services in ways that take advantage of the lower-cost home setting. However, getting the right design for the public–private partnership is not simple. For one thing, there will be little or no cost savings to the government if individuals merely use government funds in an independent setting where they might otherwise have used their own funds. Another essential requirement is regulatory flexibility to allow these programs to grow and use funds in ways that make most sense for the individual, while still ensuring appropriate oversight. There also need to be quality metrics to ensure that the frail elderly are protected in less formal settings. Nevertheless, these opportunities for providing care may reduce costs and provide more attractive options for aging Americans. Having such settings available may also encourage younger Americans, and even some baby boomers, to overcome their reluctance to think about LTC and to prepare for their potential care needs.
However, planning is possible only if people are aware of the need to save or otherwise prepare for the possibility of needing LTC. Public education has proven difficult. Misunderstandings about LTC coverage abound. One study found that only 14 percent of middle-income pre-Medicare baby boomers were aware that Medicare does not cover LTC.[84] A lack of education about aging is a major impediment to planning. Insurance agents often report that individuals seeking out LTCi protection are those actually experiencing costly LTC episodes involving family or friends, especially parents. Thus, they only become aware when they already need LTC and by then it is usually too late to save and plan.
Trying to address this knowledge gap, the Own Your Future Campaign, a joint federal and state awareness campaign in 19 states, is attempting to raise awareness about LTC planning. The program targets households with members between the ages of 45 and 65 with a planning guide and information about obtaining additional resources.[85] Examples of private-sector responses to the education void include the “3 in 4 Need More” campaign.[86] These programs appear to be making some headway, but more will be required to turn the tide.
Conclusion
A massive wave of 77 million baby boomers is now entering retirement. Advancements in medical technology have increased the life expectancy of these Americans. Faced with a huge population that is living longer, America will experience a sizable future need for long-term care services and potentially exploding public and private costs.
As in every other phase of their lives, the baby boomers can be expected to redefine retirement and aging. For this redefinition to lead to responsible decisions rather than passing unfunded programs and personal debts onto future generations, that redefinition will require reconsidering the funding mechanisms and the process of care delivery. For a productive conversation to take place over the future of LTC, policymakers must raise awareness of these issues and reexamine how to ensure that LTC is available and affordable to the millions of Americans who will need it. This cannot be accomplished by turning first to the government and taxpayers. Without a serious plan to expand personal responsibility among Americans for their future care needs, a strong safety net for the truly needy hit with extraordinary care needs will be imperiled. Without efforts to trigger innovative new approaches to care, LTC will become increasingly unaffordable.
Policymakers need to move swiftly to reexamine the current system of long-term care as well as the financial implications of the failure to address them so far. The task is nothing less than ensuring that tomorrow’s retirees have access to the high quality care they require without bankrupting future generations.
—Diane R. Calmus is a former Research Assistant in the Center for Policy Innovation at The Heritage Foundation.