Medicare Advantage (MA), a system of competing private health plans, is the major alternative to traditional Medicare for America’s large and growing cohort of seniors. Since its creation in 2003, the program has enjoyed an accelerating enrollment of highly satisfied Medicare beneficiaries, now estimated at more than 30 million, which is above 46 percent of total Medicare enrollment.REF
The MA program provides beneficiaries with a wide range of competitive health plan choices that offer a richer set of benefits than traditional Medicare, at a reasonable cost. Equally as important, the MA program has been registering consistently high marks for superior performance in delivering high-quality care.
Over the past several years, the accumulated comparative data in professional literature has shown that MA has been outperforming traditional Medicare in delivering quality care. More recent data related to COVID-19 also show that MA enrollees experienced fewer hospitalizations, fewer deaths, greater ability to receive diagnostics and treatments for ongoing medical conditions, more access to telehealth services, and more compliance with preventive health recommendations than enrollees in traditional Medicare.REF
Room for Improvement
Even though MA has outperformed traditional Medicare in several areas, critical reforms are still needed to strengthen and improve the program for the long term. Most notably, the MA payment system, tethered to traditional Medicare government-set payment rates, is overly complex and weakens the benefits of intense competitive pricing.
For decades, traditional fee-for-service (FFS) Medicare has been plagued with “improper payments”—payments that are in violation of the standard coding of services for reimbursement or other statutory or administrative payment rules.REF In 2020, for example, the Centers for Medicare and Medicaid Services (CMS), the agency that runs the Medicare program, reported that traditional Medicare had improper payments totaling $25.7 billion (a rate of 6.27 percent) and MA had improper payments amounting to $16.2 billion (a rate of 6.78 percent).REF In the case of MA (Medicare Part C), the CMS observes:
The Part C improper payment estimate measures improper payments resulting from errors in beneficiary risk scores. The primary component of most beneficiary risk scores is based on clinical diagnoses submitted by plans for risk-adjusted payment. If medical records do not support the diagnoses submitted to CMS, the risk scores may be inaccurate and result in payment errors.REF
The MA risk-adjustment system, though it has significantly improved over the years, has still not resolved the excess costs attributable to the flawed assessment of the health status of enrollees, and thus insufficiently protected taxpayers from excess costs incurred by insurers gaming the system. As reporters for The New York Times observed, government and independent audits found that some of the “major health insurers exploited the program to inflate their profits by billions of dollars.”REF Beyond these issues, MA enrollees are burdened by certain benefit and regulatory restrictions that limit their access to services.
Congress should resolve a set of outstanding programmatic issues. To improve the MA program, Congress should make MA the default enrollment option; replace the complex formula-based payment model with a competitive-bidding model; reconfigure the current risk adjustment model; and remove restrictions on key benefits and services, including those related to prescription drugs, hospice care, and medical savings account (MSA) plans.
Medicare’s Future. These interim improvements would lay a solid foundation for Congress to adopt much-needed, comprehensive structural changes to the Medicare program. These changes would transform the entire Medicare program into a defined contribution (“premium support”) program, where the federal government would make a payment based on a market-based formula of competitive bidding to a health plan of the enrollee’s choice, including traditional Medicare.REF Driven by patient choice, this change would deliver more intense competition among health plans and medical professionals, control costs for enrollees and taxpayers, stimulate innovation in the delivery of care, and improve patient medical outcomes.REF
Key Features of MA’s Success
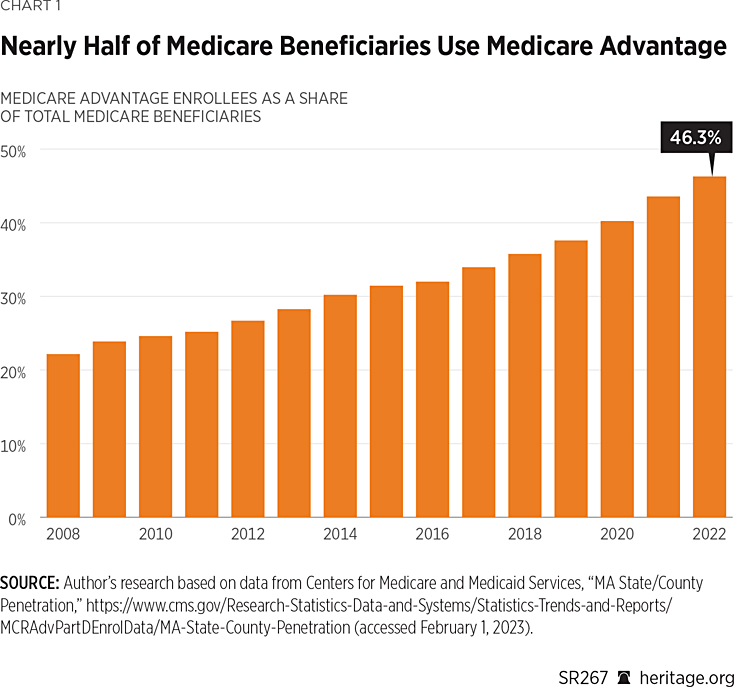
MA has been growing much faster than traditional FFS MedicareREF and has exceeded previous official projections.REF In 2020, the Medicare Trustees estimated that Medicare enrolled 62.6 million persons. Of that, more than 25 million people were enrolled in MA plans, 40.1 percent of total Medicare enrollment.REF For 2021, the Medicare Trustees estimated an enrollment of 27.4 million beneficiaries, 43 percent.REF For 2022, the MA share of total enrollment has climbed to more than 46 percent. One ambitious projection is that MA enrollment could surpass 50 percent of the entire Medicare population in 2023.REF Based on current trends, some analysts predict that enrollment in MA could reach 69 percent of Medicare by 2030.REF
These growth rates surpass official projections. In 2019, analysts at the Congressional Budget Office (CBO) projected that MA enrollment would reach a record 47 percent of the total Medicare enrollment—but not until 2029.REF The Trustees, in their 2021 report, projected that enrollment will reach 49 percent in 2030. More prescient private-sector analysts anticipated that MA penetration would reach or exceed 50 percent of total Medicare enrollment by the end of 2025.REF
Administrative actions by the Trump Administration to strengthen competition, drive down premiums, and increase choice certainly contributed to this rapid acceleration. MA enrollment increased by 44 percent between 2017 and 2020.REF
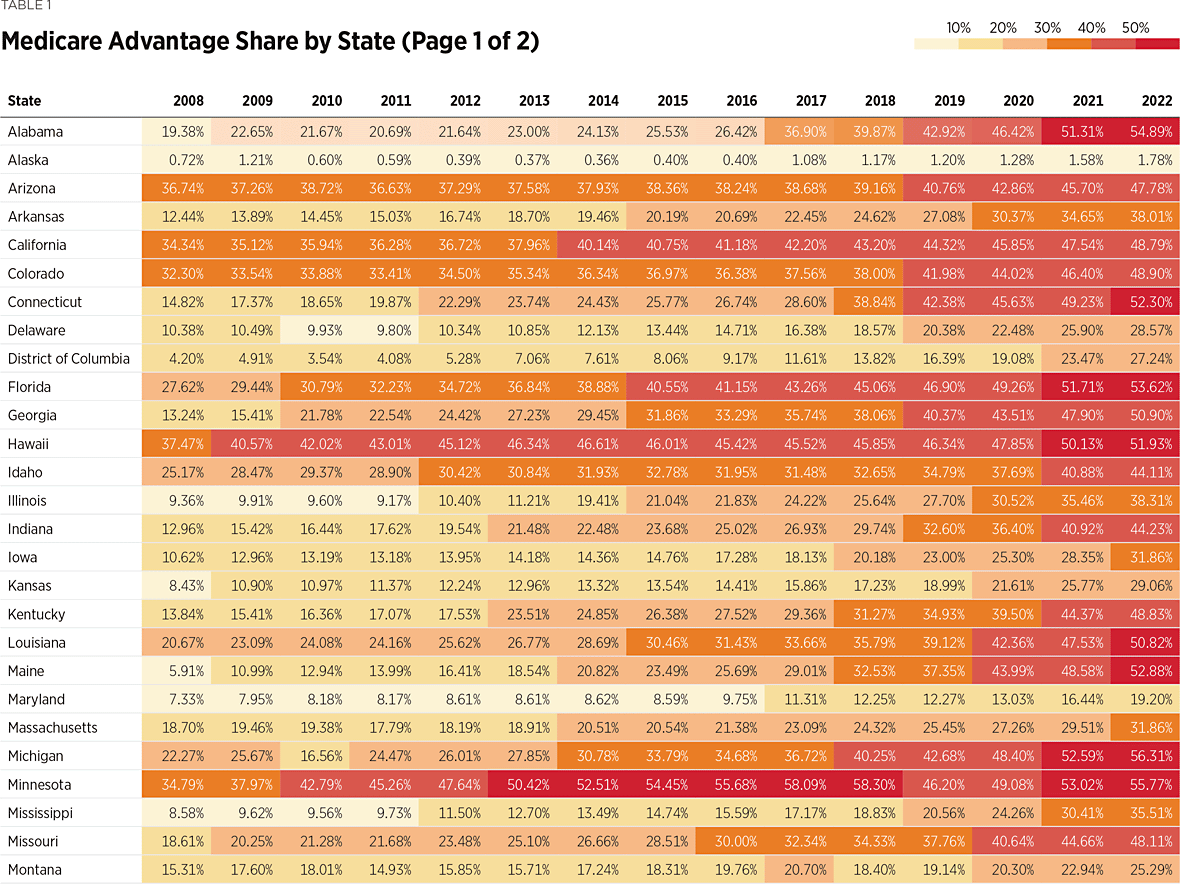
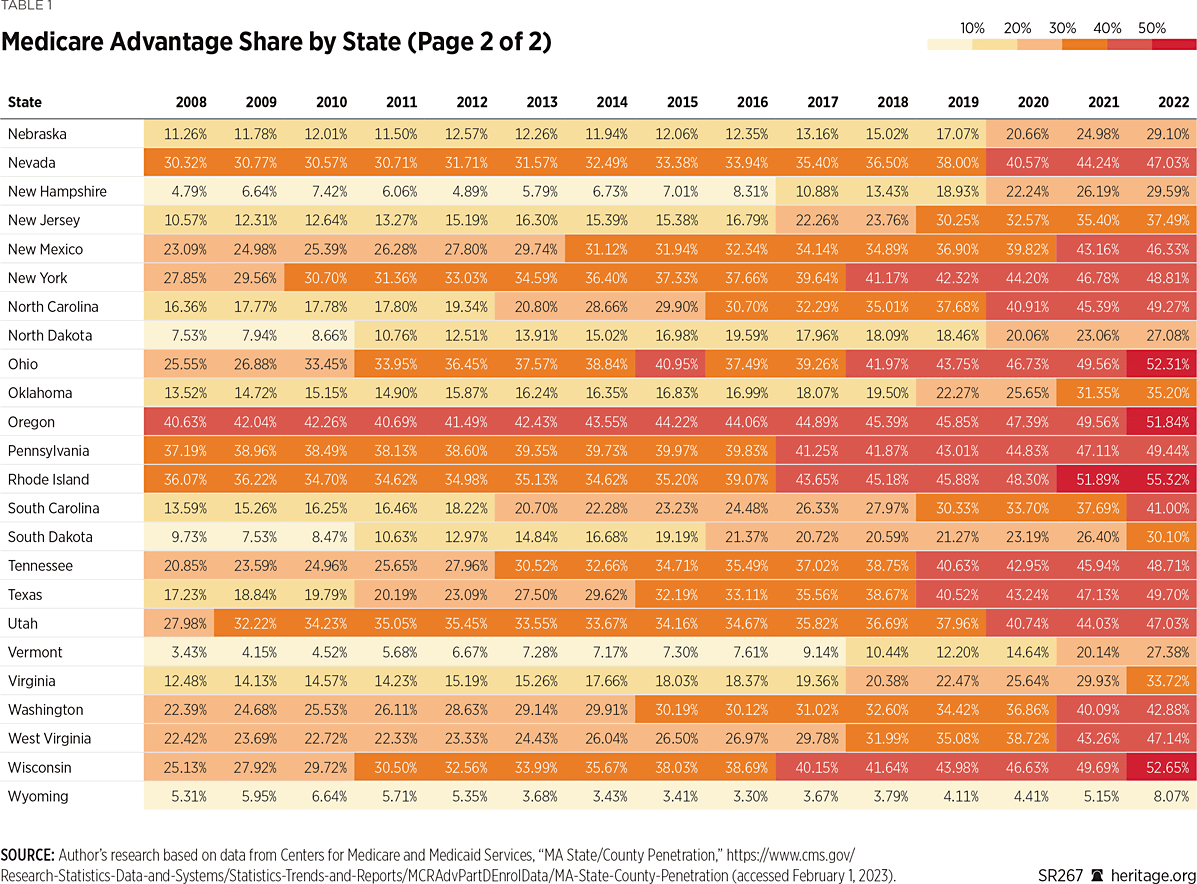
Today, MA plans are available in every state. According to Kaiser Family Foundation, “In 2022, 1 in 5 (21 percent) Medicare beneficiaries live in a county where at least 60 percent of all Medicare beneficiaries in that county are enrolled in Medicare Advantage plans (321 counties).”REF Provided that these current enrollment trends are not thwarted or reversed, MA will replace the traditional Medicare FFS program as the dominant Medicare coverage, possibly within the next two years.
A variety of factors are likely contributing to this rapid shift to MA. The following are five key features that stand out:
1. Choice. A key factor behind MA’s growing popularity is its broad choice of plans. In 2021, the program attracted a record number 3,834 plans nationwide, and the average Medicare beneficiary had access to 39 health plans.REF
The program allows diverse types of private health plans to compete on regional as well as local or county levels.REF In its annual report to Congress, the Medicare Payment Advisory Commission (MedPAC) emphasizes:
In 2022, 99 percent of Medicare beneficiaries have an HMO [health maintenance organization] or local PPO [preferred provider organization] plan (both are considered local CCPs [comprehensive care partnerships]) operating in their county of residence, nearly the same as in 2021. Regional PPOs are available to 74 percent of eligible beneficiaries, like 2021. PFFS [private FFS] plans are available to 35 percent of beneficiaries, nearly the same as in 2021.REF
By making choice and competition a priority, the Trump Administration made significant strides in expanding access to MA plans. From 2017 to 2020 alone, beneficiaries’ health plan choices grew by 78.5 percent.REF
While all MA plans must cover the traditional Medicare benefits, the plans’ benefit designs are “very different.”REF MA plans provide a variety of specialized offerings, such as eyeglasses and vision and hearing care, case management services, disease management programs, nurse help hotlines, and a variety of preventive services and tests.
By enrolling in MA, almost all beneficiaries can also receive Medicare Part D standardized prescription-drug coverage.REF Roughly nine of 10 MA plans routinely offer prescription-drug coverage at no additional cost.
The Trump Administration gave MA plans even greater regulatory flexibility over its benefit offerings, including extending supplemental benefits for primary health benefits, targeted care benefits, and benefits for chronic care.REF As a result, in 2020, about 500 plans expanded services for primary-health-related services, 300 plans expanded access to enrollees with certain chronic conditions, and, in conjunction with legislative action, about half of all MA plans offered telehealth services.REF
Today, overall, more than 99 percent of MA plans offer some level of supplemental benefits to their enrollees.REF
2. Catastrophic Protections. MA plan coverage encompasses not only standard Medicare benefits, but also protection from the financial devastation of catastrophic illness. In 2022, for example, MA beneficiaries’ out-of-pocket costs were capped at an annual level of $7,550 for in-network, and $11,300 for out-of-network, benefits and services.REF Traditional Medicare provides no such protection.
In contrast, since Medicare FFS does not provide any catastrophic protection, most beneficiaries pay extra—in addition to the standard premium—for supplemental coverage outside traditional Medicare to fill crucial gaps in coverage, such as drug coverage and catastrophic protection. Using the most complete data then available, Kaiser Family Foundation analysts reported that in 2018, for example, 34 percent purchased private, MedigapREF coverage and 18 percent purchased retiree coverage through their former employer.REF
Beyond crucial gaps in coverage, beneficiaries must navigate a traditional Medicare FFS design that imposes a more complicated and confusing set of cost-sharing requirements for Parts A and B medical services than MA. That is why most enroll in supplementary coverage and usually pay an additional premium to cover the FFS cost-sharing bills and fill in coverage gaps. When enrolling in a MA plan, the beneficiary simply pays the standard monthly Part B premium for a comprehensive, integrated health plan of his choice, with flexible cost-sharing options (within limits), plus, as noted, catastrophic protection. If an enrollee chooses a plan with a premium above the standard Part B premium, the enrollee pays the difference.
As Urban Institute analysts observe,
Medicare Advantage is competing against a disjointed benefit structure that includes separate prescription drug plans and supplemental coverage options, so the simplicity of getting Part A, Part B, Part D, and supplemental coverage all in one insurance plan through Medicare Advantage is attractive to enrollees, even before considering premiums, benefits, and out-of-pocket costs. In short, the competition in Medicare Advantage is not purely premium-based because both plans and enrollees offer other incentives.REF
3. Cost. Lower costs for beneficiaries are also a contributing factor to MA’s popularity. As Kaiser Health News reporter Phil Galewitz observed, “Many private plans save seniors money because their premiums, deductibles, and other patient cost sharing are lower than what beneficiaries pay with original Medicare.”REF In fact, in 2022, 69 percent of MA enrollees paid no additional premium for enrollment in their MA plan, including for prescription-drug coverage, beyond the standard Part B premium.REF
In traditional Medicare, for 2022, the standard monthly Part B premium was $170.10, with an annual deductible of $233, a standard Part D premium of $33.37, and no out-of-pocket cap.REF As noted, to cover crucial gaps in coverage, roughly nine of 10 enrollees in traditional Medicare must secure supplemental coverage either by purchasing supplemental coverage or enrolling in Medicaid if their income level is low enough to qualify. In 2022, the average monthly premium for supplemental coverage through Medigap was $163 per month, almost doubling the beneficiaries’ total premium cost.REF
In contrast, MA premiums have seen significant reductions. Under the Trump Administration, between 2017 and 2021, the average MA monthly premium for those plans with premiums above the standard Part B premium decreased by 34.2 percent, resulting in nearly $1.5 billion in beneficiary premium cost savings over that four-year period.REF
4. Performance. The quality and performance of the private plans compared to traditional Medicare is another key advantage. Writing in a 2014 edition of The Milbank Quarterly, Joseph Newhouse and Thomas McGuire of Harvard University concluded: “The available measures, while limited, suggest that, on average, MA plans offer care of equal or higher quality and for less cost than traditional Medicare (TM). In counties, greater MA penetration appears to improve TM’s performance.”REF
Since that time, there has been a rich and growing literature on the comparative quality of MA and traditional Medicare in delivering medical services and securing positive medical outcomes. In a comprehensive review of the literature, a team of researchers writing in Health Affairs reported :
Evidence from forty-eight studies showed that in most or all comparisons, Medicare Advantage was associated with more preventive care visits, fewer hospital admissions and emergency department visits, shorter hospital and skilled nursing facility lengths of stay, and lower health care spending. Medicare Advantage outperformed traditional Medicare in most studies comparing quality of care metrics.REF
Furthermore, early evidence also suggests that MA outperformed the traditional Medicare program during the COVID-19 pandemic. Seniors enrolled in MA had fewer hospitalizations and fewer deaths, as well as a greater ability to receive treatment for routine medical conditions.REF
5. Minority Outcomes. MA has been particularly attractive to ethnic and racial minorities, especially Hispanic enrollees. Minorities generally suffer higher rates of chronic illness, and MA’s emphasis on case management and care coordination helps in dealing with these conditions.
In 2009, just six years into the life of the program, 33 percent of all Hispanic Medicare beneficiaries enrolled in an MA plan. By 2018, 48 percent had enrolled in these plans, an increase of 43 percent.REF By 2021, almost 50 percent of black and 53 percent of Hispanic Medicare beneficiaries were enrolled in MA.REF
A major 2020 CMS study of seven categories of patient experiences in MA found that Hispanic patients reported experiences that were the same as those of white patients on five of these measures, and worse than those of white patients on two.REF In 2021, the CMS studied 23 clinical measures and found that Hispanics had worse results than white patients for 16 clinical-care measures, comparable results for 17 measures, and better results than white patients on six measures.REF
During the COVID-19 pandemic, black and Hispanic MA enrollees were more likely to report engaging in various disease prevention behaviors than black and Hispanic enrollees in traditional Medicare.REF
Beyond the pandemic, there is evidence that the MA program has routinely outperformed traditional Medicare in preventive medicine, such as for blood pressure and cholesterol screenings, flu vaccinations, and mammograms. Breast cancer, for example, is a leading cause of death among Hispanic women, but MA has a better record than traditional Medicare in preventing this deadly disease. According to researchers writing in the Journal of the National Cancer Institute, the rates of mammography screenings in MA plans (for both HMOs and PPOs) were higher than in traditional Medicare. Thus, the authors conclude: “Given their higher rates of mammography, Medicare HMOs may be more effective than traditional Medicare in eliminating racial and ethnic disparities in this service.”REF
Room for Improvement: Rethinking Government Payment, Risk Assessment, and Benefit-Design Options
For taxpayers, MA cost is a mixed bag and highlights a clear need for further reforms. Shortly after the enactment of the Medicare Modernization Act of 2003, the law that created the MA program, independent and government analysts alike estimated that, on a per capita basis, MA was costing taxpayers more than Medicare FFS.
In 2009, for example, MedPAC, the agency that advises Congress on Medicare reimbursement, estimated that the federal government paid MA plans an amount equal to 114 percent of traditional Medicare payment per enrollee.REF The additional payment represented additional benefits.
In recent years, however, this disparity in government payment has sharply declined. As The New York Times reported in 2020, “Since the Affordable Care Act was passed in 2010, the government’s per patient reimbursement rates for Medicare Advantage plans have been roughly equal to those in the original program.”REF While the program has grown dramatically and benefits have been further enriched and plans are awarded higher payments for higher quality ratings, there has nonetheless been a decline in the average MA bids for offering standard Medicare benefits. In 2022, for example, MA plan bids came in below the cost of traditional Medicare and averaged 85 percent of Medicare FFS spending.REF Meanwhile, there has been a progressive narrowing of the overall gap between MA and traditional Medicare costs.
Both Milliman, a private consulting firm, and MedPAC have detailed these changes. Based on 2021 data, for example, Milliman estimated that while traditional Medicare cost the government $949 per member, per month, MA cost $943 per member, per month.REF That same year, MedPAC estimated that government payment to MA plans averaged 104 percent of traditional Medicare spending; and of that 4 percent increase over traditional Medicare, three percentage points were attributable to “uncorrected coding intensity.”REF
The continuing controversy over comparative costs can be resolved not only through an improvement in MA’s payment system, but also through improving the metrics to achieve more accurate comparisons of cost performance between MA and traditional Medicare. Policymakers should consider at least two ways to improve comparative analysis.
First, policymakers should change the current measure of beneficiary FFS spending. Today, Medicare officials base MA payment benchmarks on the level of Medicare spending for beneficiaries enrolled in either Medicare Part A (for hospital insurance) or Medicare Part B (the Supplementary Medical Insurance program for physician and outpatient services). However, about 7.5 percent of traditional Medicare beneficiaries are enrolled in Part A only,REF thus lowering the cost of traditional Medicare in comparison with MA, which, by law, must cover all Medicare Part A and Part B benefits and services.
MedPAC recommends that, for purposes of MA payment, the spending measures should only include traditional Medicare beneficiaries who are enrolled in both Part A and Part B to ensure stability in payment as well as comparability between the two programs.REF By basing MA benchmark payments on FFS spending data for beneficiaries with Part A and Part B, thus enforcing an “apples to apples” comparison in basic spending, policymakers would achieve a more accurate cost comparison between the two programs.
Second, policymakers should also account for the fact that MA plans must cap beneficiaries’ out-of-pocket spending and pay the full cost of medical services over an annually designated amount ($7,550 in 2022). Traditional Medicare provides no such financial protection for beneficiaries and is thus spared that additional spending requirement. This, of course, undercuts an accurate cost comparison. In an econometric analysis conducted for America’s Health Insurance Plans (AHIP), Wakely, a benefits consulting firm, concluded that if traditional Medicare were required to impose MA’s annual maximum out-of-pocket spending cap, traditional Medicare’s overall costs would then be 3.5 percent higher. Furthermore, they observe, if, for purposes of comparison, one were to include FFS beneficiaries with both Parts A and B (as MedPAC recommends), that adjustment would add another 5.9 percent to traditional Medicare’s true total cost, which would then amount to 9.4 percent.REF
Before Congress adopts reforms for plan payment or risk adjustment in MA, it should authorize demonstrations of these changes. These systems are interrelated, and it is crucial that the government contribution and the system of risk adjustment ensure affordable coverage for beneficiaries and market stability for competing private plans with the least possible disruption.
Plan Payment. For each calendar year, the CMS establishes a Medicare FFS “benchmark” payment that provides the basis for private health plan competition and plan payment. This administratively determined benchmark is based on a CMS estimate of the cost of providing Medicare beneficiaries with the traditional Medicare Parts A and B benefits—based on the government-set, administrative price of those benefits and services—in the 3,143 counties throughout the nation. Under current law, the government contribution to private MA health plans is set between 95 percent and 115 percent of the FFS cost for the standard beneficiary in any given county.
Based on the FFS benchmark, private health insurers submit “bids” to the CMS reflecting their estimate of the cost to provide the traditional Medicare benefits at the county level, including their administrative costs and anticipated profit. Plans’ premiums, based on these bids, will determine their revenues, and their revenues minus costs (including administrative costs) will determine their profits. Also, under current law, MA plans must operate under a medical loss ratio (MLR) standard of 85 percent, meaning that 85 percent of plan revenues must be allocated to payment of medical claims, and no more than 15 percent can be reserved for plan administrative costs or profit.
It turns out that MA plans incur administrative costs of about 10 percent, and annual MA profits amount to approximately 4.5 percent.REF Though traditional Medicare reaps nothing like private-sector profits, nor incurs anything comparable to private-sector administrative costs, it still incurs real loss for the taxpayer through its continuing contribution to annual federal deficits. MA plans, which enjoy profits and must also incur marketing and administrative costs, can still deliver traditional Medicare benefits at lower costs than Medicare itself.REF
Compared to the CMS benchmark, if a health plan offers a bid that is higher than the benchmark for providing traditional Medicare benefits and services, then the plan can charge beneficiaries a premium (above the standard Part B premium that all beneficiaries pay) that is equal to the difference between the CMS benchmark and the plan bid. If, on the other hand, the health plan’s bid is lower than the benchmark, the plan must offer a rebate ranging from 50 percent to 70 percent of the difference to the beneficiaries in the form of lower Part B premiums, lower cost sharing, or richer health benefits (benefits that are not available in traditional Medicare). The federal government retains between 50 percent and 30 percent of the difference between the benchmark and the plan bid. The evidence is that most plans respond to the rebate by offering richer benefits.REF This includes supplemental benefits, a reduction in Part B or Part D premiums, or a reduction in cost sharing.
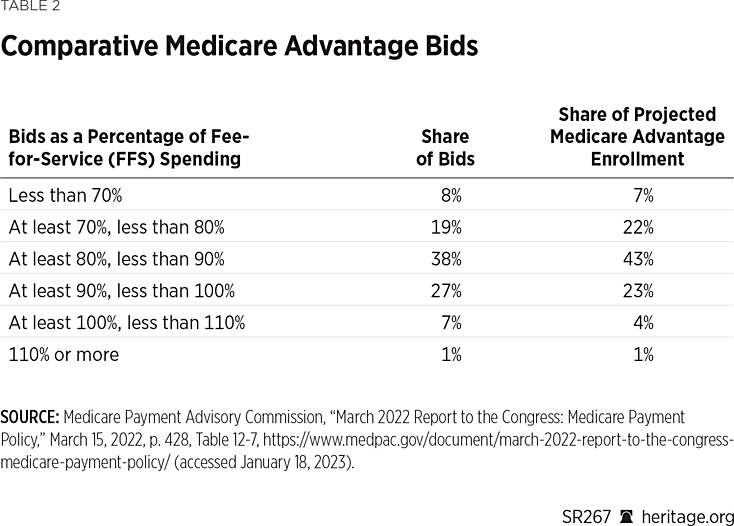
As noted, MedPAC reported in 2022 that, on average, MA plan bids were 85 percent of the Medicare FFS benchmark spending level. This performance is not new. By routinely bidding below the traditional Medicare benchmark, private MA plans demonstrate that they are, once again, generally more efficient in delivering traditional Medicare benefits than traditional Medicare itself.REF
The Problem with MA Payment Design. The existing MA payment process not only undercuts price competition, it is also outdated and fails to reflect the need for MA plans to adapt to meeting increased demand for medical services among a population with complex medical conditions.
The rebate system sabotages robust price competition because the government collects anywhere between 30 percent and 50 percent of the rebate amount when a health plan offers a bid below the CMS benchmark payment, instead of allowing the beneficiary to reap 100 percent of any savings gained by choosing a more efficient plan. Moreover, under current law, the plans can offer rebates to the beneficiaries only in the form of lower premiums, lower cost sharing, and richer benefits. In fact, the current system incentivizes the plans’ provision of richer benefits and services, which leads to higher overall program costs. If, instead of increased benefits, beneficiaries could receive 100 percent of the rebate, not only in the form of reduced premiums, but also in cash payments or deposits into a health savings or Medicare savings account, the result would intensify competition.
Beyond the distortions created by existing rebate policy, as scholars at the Brookings Institution and elsewhere have observed, the congressional decision to tie the government contribution to private health plans to the administrative costs of traditional Medicare in every county in the United States has “resulted in MA enrollment concentrating in a limited number of generally high-cost counties, leaving vast areas of the country without MA plans.”REF In short, linking payment to the traditional FFS unfairly limits plan availability and choice in certain areas of the country.
Finally, the existing payment formula is outdated and stifles the ability for MA plans—a soon to be dominant source of Medicare beneficiary coverage—to develop and adapt to new demands. As former CMS Administrator Gail Wilensky, and Drs. Rohini Chakravarthy and Brian Miller of Johns Hopkins University, note:
As the Medicare program is on a path to surpass the FFS program in size and in some markets is already the dominant model, anchoring MA around an administrative benchmark increases program costs for taxpayers and prevents full programmatic competition on the basis of price, quality, and beneficiary satisfaction.REF
Likewise, Dr. J. Michael McWilliams, a senior advisor to the Center for Medicare and Medicaid Innovation, warns that
today’s Medicare is not structured to support a dominant MA program. By statute, MA is entirely dependent on TM for establishing its payment rates. As MA grows, local FFS spending will no longer provide a reliable external benchmark. This is not a distant problem, but an impending one.REF
Risk Adjustment. To complete MA payments, the CMS must make two adjustments to the government contribution to health plans on behalf of beneficiaries: (1) The CMS must adjust the per capita government contribution to health plans based on the beneficiaries’ risk profiles, and (2) the CMS must adjust the government contribution based on a five-star rating system, which incorporates 40 categories for measuring the quality of care provided by the plan. Any plan that achieves a rating of four or five stars receives a 5 percent bonus payment. The current rating bonus system, which could also be improved, no doubt contributes to the MA’s higher performance on quality metrics relative to traditional Medicare.
In sharp contrast to traditional Medicare, the private health plans bear 100 percent of the financial risk for providing benefits. If the plans offer benefits and services at an amount below the government contribution and beneficiary premiums, they profit. If their costs of providing these benefits and services exceeds the government contribution and beneficiary premiums, they incur loss.
The focus of risk adjustment is to ensure both affordability of beneficiary coverage and market stability. Without mechanisms to adjust for differences among enrollees in health status, a competitive health insurance system could become unbalanced. In a consumer choice system with multiple competing plans, the plans that attract costlier enrollees would have to raise their premiums. That would induce healthier enrollees to leave those plans while discouraging lower-risk persons from enrolling. The market could become stratified and unstable, and in a worst-case scenario, could even collapse entirely as insurers stop participating and exit the market.
Under the current risk-adjustment formula, the plans’ risk criteria include age, sex, and institutional or Medicaid status and health status, based on the diagnoses of the beneficiaries’ medical condition. As Donald Crane, president of America’s Physician Groups, explains, “Risk adjustment is essential in capitated models because it estimates a beneficiary’s future health care costs and aligns compensation with acuity and severity of disease.”REF
The MA Risk-Adjustment Problem. Policymakers have made some improvements to MA risk adjustment and generally maintained both market stability for health plans and affordability for Medicare beneficiaries. Between 2016 to 2021, the CMS phased in an “encounter data system,” in which the health plans submit more detailed information on Medicare patients based on their “encounters” with medical professionals, including hospital visits or stays, to improve the diagnostic data for purposes of risk adjustment.REF
The problem with MA’s current risk-adjustment design, however, is that it also creates a strong incentive on the part of participating plans to secure the highest possible set of risk scores for each individual beneficiary and thus game the system. As MedPAC vice chairman Paul Ginsburg and health policy analyst Steven Lieberman, have observed, “Although plans submit bids to CMS for a standard beneficiary, the actual monthly payments for each plan member increase or decrease based on the risk scores of those who have enrolled. As a result, generating higher risk scores for MA members increases plan revenues.”REF
There is a growing consensus among policy analysts, regardless of political persuasion, that MA’s risk-adjustment system, as well as its payment model, should be reformed. Of the two, though interrelated programs, risk adjustment is the hottest topic of controversy. Writing in Health Affairs Forefront, two prominent analysts, Richard Gilfillan and former CMS Administrator Donald Berwick, have charged that the existing plan payment and flawed risk adjustment combined are resulting in a vast overpayment to MA plans, amounting to tens of billions of dollars: “Risk score gaming creates a major transfer of wealth from taxpayers and Medicare beneficiaries to MA plans, and it lies at the heart of the business model for most MA plans.”REF
Gilfillan and Berwick identify the CMS’s hierarchical condition category (HCC), the program’s measure of health status, adopted in 2006, as the main culprit in this costly process. MA plans, they insist, have an obvious incentive to create more HCCs per beneficiary, inflate health plan per capita payments, and thus generate system-wide overpayments:
In sum, as plans code more, risk scores go up, CMS provides more subsidies, benefits and premiums get better, and buyers choose the improved plans that cost taxpayers more. This is one distorted dynamic in the MA marketplace: The costlier the plan is to the payer (CMS), the easier it is to sell it to the customer, and the greater the profit.REF
One does not have to agree with every critique of the MA program outlined by Gilfillan and Berwick, nor their extraordinary assertions that the MA program is “fundamentally flawed” and unproductive of clinical value to patients, to conclude that there remain serious deficiencies in the program’s risk-adjustment and payment systems.
That is another reason why reform of the MA risk-adjustment system should proceed in tandem with reform of the MA payment system. As noted, a new system of straight competitive bidding among competing plans in a structured market, without the current reference to traditional Medicare’s administrative pricing system, would be the best way to determine the government’s per capita contribution to health plans. As Brookings scholars and their colleagues observe,
If MA plan payments were set competitively, rather than through the current system of administrative benchmarks, the effect of “upcoding” on Medicare payments would be lessened. Under a competitive bidding system, MAO [Medicare Advantage Organizations] bids would tend to reflect their actual costs of providing coverage, including any amounts they expect to pay onto or receive from risk adjustment.REF
MA Benefit Limitations. In addition to these payment and risk-adjustment issues, other policy flaws affect beneficiary access to health care services.
Genuine health plan competition requires that law and regulation treat all health plan competitors, whether HMOs or PPOs, the same, allowing consumers to make the unbiased choice of what is best for them. That is the essence of a level playing field. Under current law, all types of MA plans are permitted to offer the standard Medicare prescription-drug coverage, except MSA plans. Because of this legal restriction on offering drug coverage, MSA plans are at a competitive disadvantage; and the program, as strong as it is, still does not have a level playing field for health plan competition. There are other benefit limitations. For example, MA plans cannot offer hospice coverage, and patients at the end of life must still depend on traditional Medicare for hospice benefits, regardless of their preferences. Medicare beneficiaries also cannot take full advantage of health savings accounts (HSAs)REF to offset their cost of care. And finally, Medicare beneficiaries are still unable to get a clear idea of the financial trade-offs between the choice of MA plans or traditional Medicare with Medigap or other supplemental insurance.
Beneficiaries should have an easier-to-understand, side-by-side comparisons of both the cost and quality of their coverage options. Writing in the American Journal of Managed Care, Brian Miller of Johns Hopkins University and his colleagues warn: “As Medicare Advantage increasingly becomes the dominant form of Medicare, meaningful and accurate comparisons with traditional fee-for-service Medicare will be increasingly important for both beneficiaries and policymakers.”REF Especially important, in this regard, are comparisons of the total projected out-of-pocket costs between MA plans and traditional Medicare combined with Medigap plans.
A Comprehensive Agenda for Medicare Advantage Reform
Congress has an opportunity to make a good program better—and, in the process, lay the foundation for more comprehensive Medicare reform that will transform the entire program into an arena of robust consumer choice and health plan and provider competition. Specifically, Congress should:
1. Make MA the Default Medicare Enrollment. Upon turning 65, a person receiving Social Security benefits is automatically enrolled in traditional Medicare (Parts A and B). Given MA’s rapid growth and superior performance, Congress should change the default enrollment from traditional Medicare to MA for newly eligible beneficiaries.
In operationalizing this default enrollment, Gail Wilensky and Brian Miller suggest that newly eligible beneficiaries should be automatically enrolled in health plans with above-average quality performance on the program’s five-star rating system (3.5 out of five stars) and, like most MA plans, with zero premium costs above the standard Part B premium. Of course, under this enrollment scenario a new Medicare beneficiary would still have the option to either pick a different MA plan or enroll in traditional Medicare.REF Furthermore, whatever the Medicare beneficiary’s eventual choice, Congress should make their benefit options and personal cost consequences more transparent.REF
2. Fix MA’s Payment System. As noted, the federal government pays health plans based on a benchmark, which itself is based on traditional Medicare benefits that are set by the government administratively for thousands of services in each geographical area. If a plan’s bids come in above the benchmark, beneficiaries enrolled in that plan pay the difference every year through a higher premium. If a plan bids below the benchmark, the plan receives a rebate, and must remit a portion of that rebate to the beneficiaries in the form of lower premiums, reduced cost sharing, or extra benefits.
Thus, the reference metric for the current MA payment system is the cost of providing the covered benefits through Medicare’s traditional FFS design under which providers are paid according to government set prices. However, analyses by health system researchers have repeatedly found instances in which Medicare’s administered pricing system either overpays or underpays providers, relative to private (non-Medicare) plan payments. While federal policymakers have tried to improve payment and delivery systems, they remain, nonetheless, far short of delivering the value that can best be supplied by a robust system of flexible market pricing. As professors Michael Porter of Harvard University and Elizabeth Teisberg of the University of Virginia, observe:
The top-down prices in the current system are not well calibrated with value…. Some are too high (so every hospital wants to provide those services), and others are too low to be attractive to providers. In the current system, there is also no incentive for an excellent provider to offer the well-reimbursed services at lower rates. The methodology of top-down price setting can be improved, but never perfected. Administered prices will never really work. Hence, preserving the current Medicare pricing structure will only perpetuate the system’s problems.REF
The better alternative is to base the government’s payments to MA plans on competing health plans submitting their pricing for the set of covered benefits, which would reflect the market-based provider contracts and rates that each insurer has negotiated independently across all its health insurance lines. The Committee for Economic Development has suggested, under a new bidding system, that plans should be allowed “to bid as low as their efficiency allows, unconstrained by the benchmark.”REF
Under such an arrangement, the CMS would still establish a standard benefit with an actuarial value equal to the traditional Parts A and B benefits package. Instead of the narrow county-based regions, under a new competitive-bidding program, a new area for plan competition should be established based on MA’s current 26 regions. This would not only expand the range of provider options, it would also reduce local payment variations that characterize the Medicare status quo.
Congress should also consider several formulas for determining the specific annual contribution, such as basing plan payment on the weighted average premium of health plans (a variation on the formula used in the Federal Employees Health Benefits ProgramREF); the second lowest cost plan (the standard used in the Affordable Care Act health insurance exchanges); or the average of the three lowest cost plans.
Under any of these formulas, the process would be simpler for the health plans and better for Medicare enrollees. The key is to create incentives for beneficiaries to pick efficient health plans and to encourage them to choose the services of cost-effective medical professionals who deliver “high value” or quality care.
Congress could consider several ways to encourage stronger consumer engagement. For health plan choice, under a reformed competitive-bidding process to set plan payment, Medicare beneficiaries could get full (100 percent) rebates in the form of lower premiums, or direct cash payments, or automatic deposits in HSAs or MSAs. For incentivizing consumer choice of medical professionals, Congress could allow beneficiaries who choose a cost-effective provider to keep some portion of the savings, say 50 percent, shared with their health insurance plan. The savings potential from such a provision would be enhanced in a fully transparent market environment of price and provider performance.REF In short, Medicare beneficiaries should be able to share directly in any savings based on their personal choices of plans and providers.
Moreover, such payment changes have the potential of attracting bipartisan support. Both Presidents Bill Clinton and Barack Obama proposed straight competitive bidding among plans to improve the performance of MA and emphasized that intensifying the price competition in this fashion would also secure significant program savings.
In his June 15, 2009, speech to the American Medical Association, President Obama remarked:
Today, we are paying Medicare Advantage plans much more than we pay for traditional Medicare services. That’s a good deal for insurance companies, but not the American people. That’s why we need to introduce competitive bidding into the Medicare Advantage program, a program under which private insurance companies offer Medicare coverage. That will save $177 billion over the next decade.REF
Competitive-bidding reforms should be undertaken with a view to transforming the entire Medicare program into a comprehensive defined contribution (premium support) system; creating a glide path toward a modernized patient-centered, consumer-driven, and transparent competitive system. This should be a step-by-step process. To ensure the smoothest possible transition, as noted, Congress should first authorize a demonstration program for MA testing the different payment formulas and gradually expanding the competitive system, starting in those areas of the country where MA has already achieved the greatest geographic penetration. With default enrollment in MA—replacing the current system of default enrollment in Medicare FFS—this penetration would accelerate even more quickly.
It is worth the effort. Disentangling the MA payment system from traditional Medicare and replacing it with a market-based competitive-bidding process would more appropriately reimburse providers and achieve far better value for both beneficiaries and taxpayers.
3. Fix MA’s Risk-Adjustment System. The benefits of consumer choice in health insurance markets (such as MA) are not only that they foster value maximizing competition but also that they do a better job of meeting the diverse needs of different consumers. However, a weakness of consumer-choice markets is their potential to become unbalanced due to “selection effects” resulting from enrollees choosing plans that best suit their personal health status. In other words, it is possible for individual plan selection decisions by rationally self-interested consumers to collectively result in the segmentation and stratification of plans within the market. For instance, if a plan does a respectable job of meeting the needs of diabetic patients, it could be expected to attract more such customers, resulting in higher cost (and thus, higher premiums) relative to competing plans.
The wrong solution would be for policymakers to try to suppress those effects by standardizing coverage, creating a one-size-fits-all government plan. Doing that would not only reduce consumer choice but would also disincentivize plans from pursuing innovations in treatment and care management that could greatly benefit patients with specific medical conditions.
The better approach for policymakers is to view plan specialization as a positive, not a negative, and instead use other means to adjust for any resulting market imbalances. The basic tool for doing that is “risk adjustment.”
The CMS currently operates a version of risk adjustment for MA plans. However, the basic problem with the current design is that it attempts to predict future medical costs for each individual beneficiary. That is a nearly impossible task. So, despite years of the CMS gathering ever more clinical data and repeatedly tinkering with its payment algorithms, the system still produces suboptimal results, some of which adversely affect plan competition and Medicare spending.REF
There are reforms that could improve MA risk adjustment. Specifically, the current MA risk-adjustment design should be reconfigured into two separate and sequential components—one that is prospective and another that is retrospective.
The prospective component would consist of a formula for adjusting MA plan payments based on the following five existing demographic factors: (1) age, (2) sex, (3) geography, (4) Medicare eligibility category (aged, non-elderly disabled, or End Stage Renal Disease), and (5) institutional status (institutionalized versus non-institutionalized). These five demographic factors broadly predict most of the observed variations in total health spending among beneficiaries. It would be relatively simple for the CMS to create that formula (and to periodically update it) using aggregate data on Medicare spending patterns. Translating the results into per-beneficiary MA plan payment amounts would also be a straightforward process, consisting of simply extracting the relevant information from each beneficiary’s Medicare enrollment file.
The result would be a simpler and more consistent system for adjusting MA plan payment amounts at the beneficiary level. It would also narrow the focus of the system’s second component to addressing only the effects that might result from beneficiary plan selection decision and changes in individual health status. Those variables, and their effects, are impossible to accurately predict. Consequently, it is better to deal with them retrospectively, using real-world data.
The second retrospective component should consist of a set of MA “risk-transfer pools” operating at the regional level. Their function would be to provide a way for all participating insurers in each MA region to adjust for the effects of any significant skewing among them in the distribution of risks and costs that might arise as the result of beneficiary plan selections. Each pool would be collectively operated by its member MA plans under the supervision of the applicable state insurance departments and the pools would receive no additional funding from Medicare. Each pool would design and implement a system for calculating and transferring a portion of premium revenues among member plans to ensure that the competitive playing field remained roughly level. The objective of those transfers would be to reduce the risk of a plan becoming much more expensive relative to its competitors if it attracted a disproportionate share of costlier enrollees. The benefit of this approach is that it would not only address the current inability to accurately predict beneficiary selection behavior, but it would also enable plans to specialize in meeting the needs of beneficiaries with particular medical conditions without incurring the risk of being financially disadvantaged relative to other plans.REF
4. Allow MA-MSA Plans to Offer Drug Coverage. One type of health plan offered within the MA program is the MA-MSA plan. Just like other MA plans, MA-MSA plans must cover Parts A and B benefits, and may also offer extra benefits, such as dental, vision, and hearing services. The central features of MA-MSA plans are simple. The beneficiary pays the standard Medicare Part B premium, and those MA plans normally do not charge a premium above the standard Part B premium. The plan deposits a portion of the MA payment it receives from Medicare for the enrollee directly into the enrollee’s MSA, which the enrollee can then use to pay for medical expenses. The deposit amounts vary by plan, and enrollees can use the funds to pay for covered benefits before they reach their plan’s annual deductible, as well as any qualified medical expenses that the plan does not cover. Any money left over remains in the beneficiary’s account, and the plan adds new monies to the account for the following plan year. MA-MSA plans also have other features that many beneficiaries might find attractive: The plans normally have no provider networks, and beneficiaries are not required to get a referral to see a specialist.
However, under current law, MA-MSA plans cannot offer integrated prescription-drug coverage. This means that beneficiaries who enroll in an MA-MSA plan have no choice but to also enroll in a separate Part D drug plan, and pay an additional premium, for their Medicare drug benefits. That restriction imposes additional costs and complexities that make MA-MSA plans a less attractive option for many beneficiaries. This is a bad policy. It undercuts robust consumer choice and creates an unlevel playing field. It should be changed.
5. Allow MA Plans to Offer Hospice Coverage. For the Medicare program, the annual cost of care for beneficiaries in the last year of life amounts to anywhere between 13 percent to 25 percent of total program costs.REF While hospital and physician care accounts for the largest share of this Medicare spending, care for the dying is also funded through nursing home, home health, and hospice care.
Writing in the American Journal of Hospice and Palliative Care, researchers find that a “more effective” use of hospice and palliative care would not only improve patient experience but would also reduce Medicare costs.REF Palliative care, often curative, focuses on providing relief from pain and discomfort; hospice care is reserved for persons who have a medical prognosis of six months or less to live. Under current law, while MA plans can and do provide palliative care for patients, they are not legally permitted to provide hospice care. Roughly half of Medicare patients take advantage of hospice services.REF
MA plans have long demonstrated that they can improve medical outcomes through careful care coordination and management, and they should be able to provide a smooth continuum of care from palliative care to hospice and improve the experience for Medicare patients and their families. Congress can accomplish this by allowing MA plans to offer hospice care as an option to enrollees.
6. Allow Medicare Beneficiaries to Use and Contribute to HSAs. Tens of millions of working Americans contribute to tax-favored accounts that they use to pay medical expenses, including health reimbursement accounts, flexible spending accounts, and health savings accounts or HSAs. Under current law, when a person reaches age 65, he or she is automatically enrolled in Medicare. Current law also specifies that individuals entitled to Medicare benefits (under Parts A or B) may no longer make contributions to their HSAs.REF However, they may continue to withdraw funds from those accounts to pay for “qualified” medical expenses and there are some exceptions to the rules governing the permissible use of funds that apply to Medicare enrollees, but not to persons under age 65. Specifically, seniors can use HSA monies to pay Medicare premiums (though not Medigap premiums), and like anyone else, they can use the account funds to pay long-term insurance costs and premiums. Also, seniors are not subject to the tax penalties for use of the funds for expenses outside of qualified medical expenses.REF
Congress can improve seniors’ access to and use of HSAs—as well as their freedom to make direct payment to physicians of their choice—in two practical ways.
First, Congress should amend the HSA statute to allow seniors who continue working past the age of Medicare eligibility to continue making contributions to their HSAs if they are covered by an HSA-compatible private health plan—the same rules that apply to other workers. Seniors enrolled in MA should have the ability to open an HSA as a “stand-alone” account, regardless of the type of MA plan in which they choose to enroll, except for an MSA plan.
Second, lawmakers should end confusion over direct payment to physicians for medical services. Under current law (Section 4507 of the Balanced Budget Act of 1997), Congress imposed statutory burdens on physicians who contract privately with patients for medical services that are also covered under traditional Medicare. The best policy, of course, would be to repeal that Clinton-era restriction altogether. At the very least, Congress should clarify that seniors enrolled in MA can use funds in their HSAs to pay directly for any legal medical service (regardless of service coverage under traditional Medicare) from a doctor of their choice, including services received through an independent contract with a physician outside of their insurance plans, such as payment for “concierge” services, or through direct primary care or direct specialty care arrangements. Seniors should be permitted to spend their own money on legal medical service from a doctor of their choice without any bureaucratic restrictions.REF
Finally, Congress should also reconsider the tax treatment of HSAs for seniors, with a view toward balancing budgetary considerations with the clear need to expand access to seniors’ personal choice of care. According to economist John Goodman, tax policy should be neutral to secure a level playing field in the market, and therefore seniors’ deposits into HSAs should be made with after-tax dollars, thus treated in the same way as their Medicare premiums.REF Under the Goodman proposal, in other words, seniors’ HSAs would be the health equivalent of Roth IRAs, where deposits are made with after-tax dollars, and interest and fund withdrawals are tax-free. Alternatively, Congress could retain the current tax-favored status of contributions, and, as James Capretta of the American Enterprise Institute has suggested, increase the tax-free contribution limits.REF
Setting a Solid Framework for Future Medicare Reform
Millions of seniors are voting with their feet. The rapid beneficiary enrollment in MA is transforming the Medicare program into a platform for consumer choice, multi-plan competition, new payment and care coordination options, and increasingly flexible benefit and service offerings. Based on current enrollment trends, MA will dominate senior coverage and care delivery, sooner rather than later, perhaps within the next two years.
From the standpoint of Medicare beneficiaries, including racial and ethnic minorities, it is obvious why they are flocking to the private plans. Not only do retirees have the security of comprehensive coverage, but the MA program offers broad choice of plans, enrollment is convenient, the benefits are relatively rich and varied, the plans guarantee protection from the financial devastation of catastrophic illness, and the plans offer high-quality coverage at affordable cost.
Nonetheless, the program suffers from certain defects that require legislative remedies. Congress should address these issuing by fixing the flawed and outdated payment formula, the defective risk-adjustment system, the odd restriction on drug coverage in MSA plans, the restriction of hospice coverage in all MA plans, the restriction on the ability of seniors to use and contribute to HSAs, and the Clinton-era law undercutting seniors’ opportunities to spend their own money directly for services provided by independent medical professionals of their choice.
Over the next 35 years, fueled by the rapidly retiring generation of baby boomers, total Medicare enrollment will double. Medicare’s financial challenges, already severe, will worsen unless Congress reforms the entire program.
Under any scenario, the taxpayers will be paying more for seniors’ medical care. The top task is not just to control federal spending, but to make sure that seniors and taxpayers get excellent value for their health care dollars. Central planning and price controls cannot achieve that objective. A well-designed consumer-driven competitive system can. That is why Congress should improve the MA program, build on its key features of defined contribution financing and flexible regulation, and then use that platform as a bridge for larger Medicare reform that would transform the entire Medicare program into a consumer-driven, patient-centered, defined contribution (“premium support”) program.REF That is what will ensure a better health care future for America’s seniors.
Robert E. Moffit, PhD, is Senior Research Fellow in the Center for Health and Welfare Policy at The Heritage Foundation.



