The House Committee on Oversight and Government Reform recently considered the Postal Service Reform Act (H.R. 5714). The bill proposes shifting postal retirees’ primary health care coverage from the Federal Employees Health Benefits Program (FEHBP) to Medicare. Proponents call this a consensus proposal for integrating the FEHBP with Medicare. It is not. The proposal’s impact on postal retirees and taxpayers alike could be substantial.
For taxpayers, the House bill would shift unfunded postal obligations to Medicare’s unfunded long-term obligations. Today, Medicare is burdened by an enormous 75-year unfunded obligation that ranges from $32.4 trillion to $43.5 trillion, depending on the assumptions.[1] The bill also perpetuates 100 percent wraparound, supplemental insurance, which provides “first dollar” coverage and “free” medical care. This arrangement drives excessive Medicare use, and thus imposes ever higher costs on both Medicare beneficiaries and taxpayers alike.[2]
For postal annuitants, the bill would result in these retirees facing either a significant reduction in retirement income because of additional premium costs, or a loss of existing benefits offered through the FEHBP. Under the proposal, postal annuitants would be forced to enroll in Medicare Part B, required to pay the premiums for Part B, and continued premium payments in the FEHBP if they want to maintain any FEHBP benefits or choice among FEHBP plans. Paying two premiums instead of one is an unforeseen and unbudgeted cost to these retirees.
A Better Policy. The emergence of this legislation, though focused specifically on postal employees and retirees, highlights, once again, the central underlying problems of the federal health care status quo in both the FEHBP and Medicare. Specifically, it points to a need for fundamental reform in the interaction between federal employee and annuitant health insurance in the FEHBP and Medicare.
Congressional leaders should understand that current difficulties in postal and federal retiree health coverage are a direct result of past mistakes in the design of the FEHBP. It is those mistakes, not some piecemeal postal carve-out, that need urgent attention. Congress can accomplish this task by reforming certain structural defects of the FEHBP, such as changing federal tax policy governing FEHBP plans, improving the FEHBP payment formula, and adding a risk-adjustment mechanism. Moreover, Congress should make additional changes to resolve the problems related to federal retirees who voluntarily switch to Medicare, including replacing the costly wraparound coverage that drives excessive Medicare costs.
These proposed changes would resolve crucial problems in the interaction between the FEHBP and Medicare in the provision of retiree coverage, addressing the dysfunctional relationship between Medicare and existing supplemental retiree coverage that drive costs up for enrollees and taxpayers alike. These changes would also begin to address long-standing structural problems within the Medicare program by taking a modest step toward a more rational defined-contribution financing system for Medicare.
The Postal “Reform” Proposals
There have been a number of proposals in recent years to “reform” health insurance for postal employees and annuitants. Postal employees constitute about one-fifth of all federal employees, a substantial reduction from previous decades due to postal downsizing. Postal annuitants ages 65 or above are one-fourth of all federal annuitants, reflecting previous postal employment levels. Hence, it is obvious that any change affecting postal employees or annuitants has potentially very large effects on the entire FEHBP program.
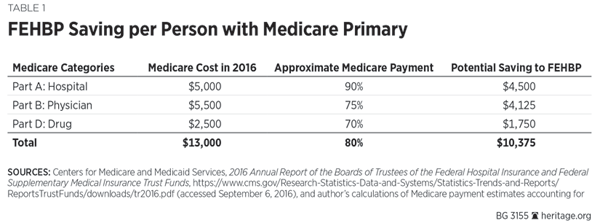
With close to 100 percent of all 65-plus postal and other federal annuitants who have retired in recent decades enrolled in Medicare Part A hospital benefits, the FEHBP already benefits from a Medicare subsidy of about $4,500 a year for almost all of these annuitants. Current proposals to reform health insurance for postal employees and annuitants would further shift costs to Medicare. (See Table 1.)
In 2012, Congress considered a set of reform proposals that would have completely withdrawn postal employees and annuitants from the FEHBP program, and enrolled them in new health plans at a massive but unacknowledged cost to postal employees. But these proposed insurance changes were just a fig leaf for the underlying proposal to mandate enrollment in Medicare Part B.[3] Today that proposal is no longer hidden but at the core of the reforms.
The Medicare Part B Mandate. The primary goal of the latest proposals in the House and Senate is to force the remaining annuitants into Medicare Part B, and thus shift most annuitant health insurance costs onto the Medicare program.[4] There are about 93,000 postal annuitants (and spouses) ages 65 and above who are currently enrolled in Medicare Part A, but who have not enrolled in Part B. Under the House bill, these postal annuitants and their dependents would be forced to enroll in Part B and pay the Part B premiums in order to keep their existing coverage, including prescription drug coverage, in the FEHBP. These annuitants would have to pay FEHBP premiums, whatever they may be on an annual basis, as well as the $1,460 per person annual premium for Part B.[5]
For all postal annuitants (65 years of age and older), the bill would reduce Part B premiums over a three-year period.[6] But thereafter, these annuitants would be required to pay the full enrollee share of the Part B premium. Thus, over a 10-year period, the average annuitant would still be out-of-pocket for more than $15,000 (twice as much for married couples) in new premium obligations. For postal annuitants, of course, this would be an amount they never anticipated, for which they never budgeted, and which was never before required of them.
The House bill would avoid at least one disaster by amending the Social Security Act to eliminate the normal premium penalty of 10 percent a year for delaying enrollment in Part B past age 65. Medicare Part B severely penalizes persons who enroll late (after age 65 or upon retirement from a job with insurance coverage, whichever is later). The penalty is 10 percent a year, or a doubled premium for someone who enrolls at age 75. By mandating enrollment into Part B, those annuitants who are already over 65 would face an additional cost if the penalty were not eliminated.
The bill would “deem” these annuitants to be enrolled so that they would not automatically lose their FEHBP coverage, but then assumes that the Social Security Administration, the Department of Health and Human Services, and the Office of Personnel Management (OPM) would locate every one of them, and by some undefined process officially force them to enroll them in Part B. For those who did not get the message, did not understand the message, or ignored the message, sorting matters out could take many years and result in many unpleasant events.[7]
Moreover, in many thousands of cases, people who had alternative employer coverage for post-65 employment (but who had still kept an inexpensive FEHBP plan legally needed to retain coverage in old age) would still be forced to pay full Part B premiums for a Part B policy that would be “secondary” and hence valueless until true retirement. In many other thousands of cases, annuitants living abroad would face a completely worthless Part B benefit, since Medicare, unlike the FEHBP, does not pay medical costs outside the United States.
The likelihood of these or other practical consequences is further complicated by the additional administrative burden it would impose on OPM. The recent failure of OPM to notify the victims of the massive hack attacks into the OPM personnel databases that stole personal information of more than 20 million federal employees and contractors illustrates this point. To date, two million victims have yet to be informed of their exposure.[8]
The Misguided Supplemental Coverage. The House bill also neglects to address one of the bigger problems underlying the proposed shift to Medicare—specifically, the costs of “first dollar” supplemental coverage. Under current practices (which this bill would legally mandate for postal annuitants), most national plans and a few local plans in the FEHBP provide to those who enroll in both Parts A and B a Medicare “wraparound” that eliminates all hospital and medical (but not prescription drug) costs, and does so for all medical services in or out of network. The actuarial value of this wraparound is approximately $750 a year in reduced cost sharing. With a Part B premium of $1,460 that means the net cost per person for Part B would be “only” about $700 a year (rising over time to $1,000 a year or more), and “only” about $8,000 over the first 10 years. Proponents argue that these postal annuitants would gain additional value under this scenario, but they would still be large net losers.
There is a robust literature demonstrating that when health care is “free” at the point of service there is a substantial increase in utilization of medically unnecessary services. This is the unfortunate effect of all supplemental plans that wrap around traditional Medicare and eliminate all or almost all cost sharing for hospital and physician services, including Medigap and employer plans (like those in the FEHBP).
In a recent report to Congress, the Government Accountability Office found a massive difference between spending by those covered only by traditional Medicare (average of $8,100), those in Medicare plus Medigap ($15,600), and those in Medicare with employer wraparound ($14,400) in 2010.[9] The best source of data is a recent report from a Medicare Payment Advisory Commission (MedPAC) contract that uses regression analysis to control for differences in health status, education, income, and other factors.[10]
Using pooled data from 2003 to 2008, the MedPAC report found that employer-sponsored wraparound coverage increased Part B spending by 28 percent compared to Medicare-only coverage.[11] Using a conservative factor of 25 percent, this is an increase of about $1,400 at present, and likely to be well over $16,000 per annuitant over 10 years. For the 93,000 postal annuitants forced into Medicare Part B coverage, this would increase total Medicare spending by about $130 million now, and $1.5 billion over a 10-year period. This would in turn require a corresponding increase in Medicare Part B premiums for all Medicare beneficiaries, to be paid by taxpayers and these elderly.
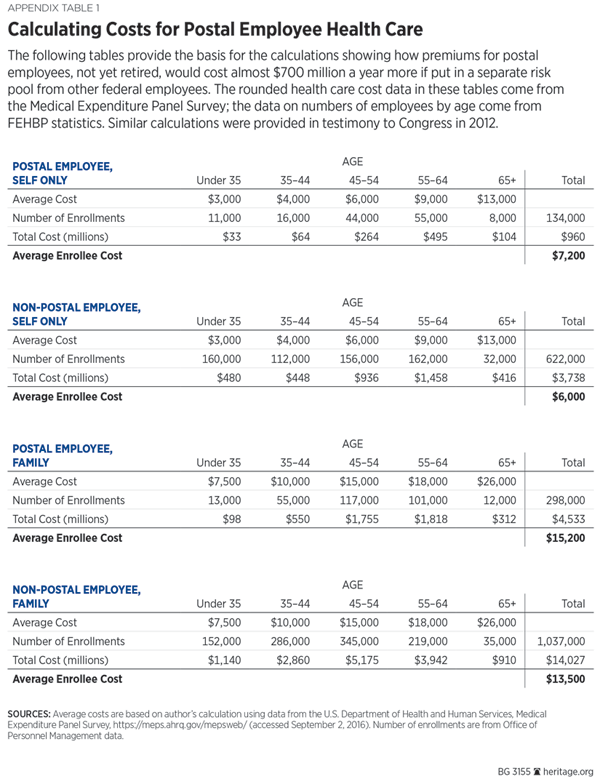
The Creation of a Costly Separate Risk Pool. The House bill would also create a separate risk pool for postal employees and annuitants who are currently in the same risk pool as all other federal employees and annuitants. The bill’s provisions would have two main effects on this new pool. First, it would appear to save approximately $500 million annually through the $4,125 shifted to Medicare taxpayers and beneficiaries per newly covered postal annuitant. But it would cost the U.S. Postal Service (USPS) almost $700 million more annually because postal employees are substantially older than other federal employees and incur much higher medical costs. (See Table 2.)
The average postal family cost is about $1,700 a year higher than the cost of non-postal families because of this age differential. Multiplying by the 298,000 postal employee families, this means an additional cost of over $500 million. Adding in self-only enrollments, the total additional cost of a separate risk pool is almost $700 million a year. Since health plans have to cover the costs of those who enroll, this translates directly into premium increases (assuming that plans do not cut back benefit levels). So the net effect from creation of a separate postal pool would be roughly a $200 million annual increase in the USPS’s combined health insurance costs for both annuitants and employees. Most of this effect would fall on the USPS as an employer, since it pays most health insurance costs, but postal employees would also be impacted through higher premiums. Of course, the USPS would also have to raise rates or find other ways to pay its almost $500 million-a-year share of this increased cost.
As a result of carving out these more expensive postal employees, the bill creates a corresponding windfall gain to other federal employees. The non-postal FEHBP premiums would decrease by that same $700 million annually spread over about 3.1 million non-postal employee and annuitant enrollments. While most of these savings would accrue to the federal government as an employer, most employees and annuitants would gain a few hundred dollars taken from postal employees.
Understanding the USPS, the FEHBP, and Medicare
Members of Congress, in seeking to craft better policy, should understand the key features of the three agencies and programs—the USPS, the FEHBP, and Medicare—and how they interact.
1. The United States Postal Service. The USPS in its modern form was created through the Postal Reorganization Act of 1970. The idea was that it should be run as a business-like enterprise, with revenues covering costs and an end to political interference in management decisions, such as deciding which post offices to open or close. This goal remains as elusive as ever.
Past USPS Health Policy Mistakes. In one of many key decisions, the USPS was not originally taken “off budget,” as would be the case for any real business enterprise. This decision was reversed in the Omnibus Budget Reconciliation Act of 1989, only to be partially reversed again by subsequent budget scoring laws and decisions; most notably under a 2006 statute misnamed the Postal Accountability and Enhancement Act. Today, while the $70 billion-a-year Postal Service Fund for ongoing mail-delivery services remains off budget, something called the Postal Service Retiree Health Benefits Fund (PSRHBF) is subject to complex budget “scoring” provisions.[12]
Another fateful decision kept postal employees as federal employees, entitled to the same retirement pensions and retirement health benefits as other federal employees, all guaranteed by law. Postal employees have benefited for decades from the superior cost control of the competitive FEHBP system, yet the USPS has bargained away much of the actual savings and the potential future savings, to the detriment of all federal employees, as discussed in “FEHBP Policy Mistakes” section below.
2. The Federal Employees Health Benefits Program. The FEHBP is the largest employer-based insurance system in the nation, with about 8 million enrollees and enrollee dependents. Some 250 plans participate nationally. In almost all areas, large or small, there are about two dozen plans open to all employees and annuitants.[13]
The FEHBP has an annual budget in excess of $50 billion. It was created in 1960 and was an accidental work of genius. With the federal government a latecomer to employee health insurance benefits, many union plans and health-maintenance-organization plans had been created to provide these benefits by filling this gap. When the time came to create an official, government-wide program, the plan sponsors and enrollees did not want to lose their plans. So a compromise was struck, and instead of a single government-run plan as originally proposed, several dozen plans were allowed to coexist and compete for enrollees, based on cost, service, and benefits as determined by each plan, with a uniform government subsidy.
For most federal employees, the government pays 75 percent of the cost of enrolling in any participating health plan, up to a maximum government share calculated as a percentage of the all-plan average premium cost. In the jargon of health insurance experts, this is a “premium support” system.
So manifest were the strengths of the FEHBP, that the Medicare Advantage and Medicare Part D drug programs enacted by a Republican Congress were largely modeled after it, though with some important changes to correct weaknesses in the aging FEHBP design. At the very inception of the national debate on health care reform in 2008, presidential candidate Barack Obama claimed that his proposed national health insurance exchange would function like the FEHBP.[14] Yet, key features of his original proposal, and the subsequent legislative embodiment of the government-designed health plans and health insurance exchanges in the Affordable Care Act, have little in common with the consumer-driven FEHBP.
FEHBP Policy Mistakes. The FEHBP has a solid record of superior performance including consistently outperforming Medicare in cost control.[15] Yet, wrong-headed decisions by the federal government have diluted some of this success. Most important was the decision to alter the federal tax treatment of FEHBP coverage to make it more like the costly and dysfunctional tax treatment of private employer-sponsored health insurance, which fuels over-insurance and drives up overall health care costs.
In the private sector, employers can make the employee share of premium costs non-taxable. Naturally, almost all do this because it saves employees money at taxpayer expense, with no cost to employers. But, for the federal government, there is no comparable advantage, since whatever employees save has to be paid from taxes or borrowing. Nonetheless, in the name of “consistency with private sector practice” the fateful decision to mimic private employer coverage was made first in the USPS, and then copied by OPM in 2000 for all federal employees.
This single change turned out to have massively negative effects on plan competition in the FEHBP, which depends on enrollees paying the full marginal cost of expensive plan choices. The marginal tax rate (federal, state, and Old-Age, Survivors, and Disability Insurance (OASDI)) for almost all federal employees is about 33 percent.[16] Hence, employees received a one-third discount on any expensive plan choice, and plans that previously aimed to hit the sweet spot where the 75 percent employer share ended, could now afford to increase benefits and raise premiums without losing enrollment.[17]
Yet another problem was created because of the USPS. Facing strong unions, the USPS had little to put on the table in collective bargaining except wages and the employer share of insurance premiums. As a result, while almost all non-postal employees face a maximum employer contribution of 75 percent of premium up to a maximum dollar amount, postal employees as recently as 2012 were receiving a contribution of 80 percent up to a higher maximum. (Some other agencies also provide higher premium contributions, including the Federal Deposit Insurance Corporation (FDIC) and the Federal Reserve). It is worth noting that in the private sector, the employer share of family premiums is rarely more than 75 percent.
3. The FEHBP and Medicare. In 1960, Medicare did not exist, so the federal government decided to include both current employees and federal retirees in the FEHBP with most health plans open to all. With the creation of Medicare in 1965, and over the next half century, Medicare and the FEHBP coexisted uneasily, with the design of neither program integrating in a sensible way with the design of the other.
The Medicare Coordination Policy Mistakes. Until 1982, any career federal employee who did not have 40 quarters of Social Security coverage (the great majority of federal employees, including postal) was not covered by Medicare Part A (hospital benefits) without paying a prohibitive premium for that benefit. However, as a result of legislation enacted in 1982, all federal employees became eligible for “free” Part A coverage.[18]
Because Medicare was the “primary” source of coverage for retirees over age 65 who enrolled in Medicare while retaining private employer post-retirement coverage, it was soon apparent to both the OPM and FEHBP plan executives that the FEHBP could save large sums of money, and the plans could lower their premium costs, if federal annuitants could be enticed into joining both Medicare Part A and Part B (physician services) and thus shifting most costs to Medicare.
Hence, a fatefully wrong decision was made by OPM: Those retirees who had both Parts A and B of Medicare as primary coverage, and one of the national FEHBP plans as secondary coverage, would receive a wraparound benefit and pay zero for hospital care, zero for physician care and medical tests and equipment, and enjoy this unlimited free care not only using network providers, but also using any other providers participating in Medicare. This “integration” decision has cost both programs—especially Medicare—tens of billions of dollars through unnecessary and wasteful overuse of care due to the effects of full wraparound supplemental coverage.
Originally, few federal employees had Part A coverage. But as a result of the 1982 change, “free” Part A coverage became almost universal among annuitants upon turning 65 (the exceptions are mostly aged widows whose late husbands retired before 1983, and those still working for other employers). In addition, about 75 percent of annuitants voluntarily sign up for Part B upon turning 65 (or in some cases later, if still working). The 75 percent with both Parts A and B has not changed appreciably in the last decade.
Amazingly, both the Postmaster General and other witnesses at recent Senate and House hearings have incorrectly stated or implied that there are large numbers of 65-year-old postal annuitants who have paid $29 billion in Medicare taxes and who are not receiving Medicare coverage for which they have paid.[19] Medicare Part A eligibility and enrollment is, in fact, independent of eligibility or enrollment in Medicare Part B, and vice versa: “If you aren’t eligible for free Part A, you can buy Part B without having to buy Part A, if you’re age 65 or older.”[20] Since Part A is free for post-1983 annuitants (but very expensive for most who retired earlier), it is doubtful that more than a handful who are eligible for free Part A coverage have not signed up for it. If there are, the PSRHBF could be augmented by a nudge, such as paying any such persons a few hundred dollars to sign up for this “free” benefit. Of course, the resulting saving to the FEHBP is a cost to Medicare, and hence is a transfer from one taxpayer pocket to another (leaving aside the induced wasteful spending discussed in “The Supplemental Coverage Mistake” section below). But Medicare taxes paid by or on behalf of postal annuitants while they were still working were Part A taxes and have nothing to do with Part B or its premium. Such statements are obviously made in ignorance, or are intended to obscure the point that these bills would force annuitants to purchase Part B insurance that they have not already paid toward, do not need, and do not want.[21]
The Supplemental Coverage Mistake. From Medicare’s inception, federal officials have not only allowed but also encouraged supplementary insurance in the Medicare program. The Department of Health and Human Services fully recognized that with no coverage of prescription drugs, and no maximum out-of-pocket limit on enrollee costs, Medicare had by the 1980s fallen far behind standard practice in private insurance.
One early accommodation was to embrace wraparound Medigap plans. These plans not only provided needed catastrophic coverage, they also provided coverage for all or almost all out-of-pocket costs, resulting in “first-dollar” coverage for Medicare beneficiaries. In most versions, these supplemental plans provided the same almost 100 percent “free” hospital and physician coverage offered by many employer plans, including almost all national FEHBP plans.
Most prominent health policy experts, regardless of their political persuasion, now agree that the current arrangement of Medigap plans and other forms of supplemental coverage is a major cost-driver in the Medicare program.[22] Taxpayers, as well as beneficiaries, pay dearly for this “double” coverage. Thus, as a matter of sound policy, these supplemental plans, Medigap or employer wraparound plans, like the FEHBP, should be discouraged or prohibited.
While details vary, there are three major proposals that attempt to address this mistake more broadly worthy of note. First, the Obama Administration has proposed legislation to financially penalize 100 percent wraparound Medigap policies, a proposal estimated to save $7 billion over 10 years even without reaching employer wraparound plans.[23] Second, the Congressional Budget Office (CBO) presented a more aggressive policy change that would, in essence, convert all Medigap plans to catastrophic protection, and save $58 billion over 10 years.[24] Third, the recent Congressional Republican health care White Paper prepared under House Speaker Paul Ryan contains a brief summary proposal that appears to be quite similar to the CBO proposal.[25]
FEHBP and Medicare Advantage. There is a promising option for federal retirees, including postal retirees, who wish to voluntarily join Medicare. Under the Medicare Modernization Act of 2003, Medicare Advantage (MA) plans now enroll more than 30 percent of all Medicare beneficiaries. MA plans are very similar in design to most FEHBP plans and include similar benefit structures and cost-sharing provisions, and many are sponsored by most of the same insurance carriers that participate in the FEHBP. Moreover, the comprehensive design removes the necessity for supplemental coverage.
MA plan premiums that include Part D drug benefits generally cost not much more than the Part B premium, and are similar to the premiums in lower-cost FEHBP plans (around $1,200 to $1,800 annually for self only). They also all contain guarantees as to maximum out-of-pocket spending, generally around $4,000 for hospital and medical care, plus another $4,850 for prescription drugs.
OPM, to its credit, allows federal annuitants to “suspend” FEHBP enrollment and enroll in MA plans, paying only one premium and preserving the flexibility to return to the FEHBP in a future open season. However, because OPM does not provide annuitants detailed plan choice information by mail, and buries this option on its website, as a practical matter few annuitants even know it exists.
Solving the Postal Service Health Care Problem
There are a number of solutions for the problems facing the USPS that include righting the wrongs of past policy mistakes, such as moving the USPS entirely off budget and both allowing it and forcing it to function like a real business enterprise and removing postal employees from the federal employee designation.
But in the area of postal health coverage, the best single option would be to pursue serious reforms in the FEHBP; reforms that focus on the entire FEHBP, not just postal annuitants. These reforms would not only address the problem of postal employee and annuitant coverage, but would also reduce future costs for covering all federal employees and annuitants, and substantially reduce costs in the overall FEHBP program.
Fixing the FEHBP. The FEHBP has several structural features that substantially increase its present and future costs. The following reforms would help to address these underlying cost problems.
- End the premium cost-sharing exceptions. As noted, some federal agencies, including the USPS, do not follow the statutory formula for premium cost sharing, and provide a more generous premium contribution than received by most employees and all annuitants. Banning this practice would create immediate budgetary savings of several hundred million dollars a year and strengthen incentives for enrollees to choose less costly plans over time.
-
Remove the pre-tax premium subsidy. Employer premium contributions to employee health coverage are automatically tax free, but whether the employees’ premium contributions are tax free is a matter of employer determination. Throughout most of its history, FEHBP employee premium contributions were, as a matter of policy, not tax free. In 2000, OPM changed the policy, and, for the first time, federal employees and retirees were able to shield their share of FEHBP premium payments from taxation. This “premium conversion” tax subsidy for the employee share of premiums has greatly weakened the incentive structure of the FEHBP that controlled costs. Instead of enrollees paying the entire cost of their more expensive plan choices, they pay only about two-thirds. Not surprisingly, the price for this misguided tax policy is higher overall health costs for employees and taxpayers alike.[26]
The fiscal year 2017 budget for the FEHBP is $53 billion; enrollees pay on average about one-third of premiums; and the federal income and OASDI tax losses are on average about 30 percent of premiums. Hence, elimination of this 2000 tax subsidy to employees would generate federal revenues of over $2.5 billion a year.[27] An offsetting increase in federal employee pay or government share of premiums for lower-cost plans (see “Change the Payment Formula” section below) could reduce this cost for enrollees, or even eliminate it. As a fiscal matter, any increase in revenues from this policy change can be offset by lowering taxes elsewhere. Importantly, if this change led over time to as little as a 1 percent reduction in FEHBP costs through enrollee migration to lower-cost plans, it would generate additional real savings of $500 million a year, and because these savings would compound over time, likely a great deal more.
-
Change the payment formula. The formula for the government share of premiums includes government payment of 75 percent of annual premium costs up to a specific dollar ceiling. The flip side of this formula is that enrollees who choose a plan below that ceiling only receive 25 percent of the savings. In contrast, when Congress created the Medicare Advantage program it wisely gave enrollees 75 percent of any savings that resulted from choosing lower-cost plans. To rectify this inequity, this author has outlined some options for changing the government payment formula in the FEHBP.[28] Such a change would move the FEHBP closer to a more rational defined-contribution model.
The key point is that the government can and should allow enrollees to retain most of the savings from choosing lower-cost plans. This would strongly improve enrollee incentives to be frugal and, over time, strengthen the plan’s competition dynamic as plans lower costs to attract more enrollees. Changes in this parameter could be used to offset some or all of the costs to enrollees from abolishing “premium conversion.”
-
Establish risk adjustment. Risk-selection problems have been a problem for the FEHBP since its inception. While these problems have not been catastrophic, they have been persistent. It is in the interest of every enrollee to join plans with the lowest proportion of high-cost annuitants. This distorts plan selection and leads to perverse results. For example, the Kaiser plans on the West Coast do an outstanding job of keeping enrollee costs low, but have a disproportionate number of annuitants who correctly understand that they do not need Medicare. This puts Kaiser at a major disadvantage since it has to cover their age-related costs.
In Medicare Advantage, Congress incorporated risk adjustment into the program to raise or lower the government share to compensate for risk selection and keep plan competition based on performance rather than enrollee health factors. The adjustment is budget neutral and invisible to enrollees. The best and easiest way to do so in the FEHBP is to focus on Medicare status, since this cost variable drives FEHBP costs far more than the details of health status. Plan premiums should receive a budget-neutral adjustment in government contribution (and hence enrollee share) based on the ratio of age-65 annuitants with or without Medicare Parts A, B, or both. This would greatly improve plan competition and plan performance in cost control over time.
FEHBP Retiree Coverage. There are also potential reforms to address the interaction between FEHBP and Medicare for those retirees who voluntarily join Medicare. The reforms would address the double-coverage cost problem, help save taxpayer money in FEHBP and Medicare, and ensure that FEHBP retiree coverage is compatible with broader reforms to Medicare.[29]
The reforms would do the following:
-
Replace the current cost-sharing Medicare wraparound for Part B enrollment. Today, FEHBP retirees who voluntarily join Part B are also provided supplemental coverage from most national plans in the FEHBP. These FEHBP plans provide wraparound coverage to eliminate the cost-sharing requirements for physician and other medical services from both Medicare Part B and the FEHBP plan. Together with the same supplementation for hospital coverage for those with Part A, these arrangements perpetuate “first-dollar,” 100 percent coverage that drives up utilization and costs. Both the CBO and this author have proposed a new policy option of having FEHBP plans subsidize Medicare Part B premiums in place of the wraparound option for both Parts A and B. If both wraparounds were removed, then, for annuitants, the FEHBP plans would be completely identical to active employee plans.[30] This change could also be accompanied by changing the Social Security Act to allow FEHBP annuitants who did not enroll in Part B at age 65 to do so in the future without penalty.
The Parts A and B wraparound is worth about $750 a year in cost savings to enrollees, and the cost shift from FEHBP plans to Medicare Part B is about $4,125. Thus, the government could make the subsidy contribution higher if it so chose. For example, enrollees could receive $1,500 a year in premium reduction for Part B but continue to pay the same cost sharing at age 65 as they had paid at age 64, for instance, $30 for a specialist visit. In effect, the Part B premium would become “free” and annuitants could not only keep their pre-retirement health plans, but also receive the significant advantage of almost unlimited provider choice.[31]
The principal advantage of this approach would be to maintain federal retirees’ voluntary option to enroll in Medicare, a major victory for personal freedom of choice, and the taxpayers would benefit because wasteful overuse of “free” medical care would be reduced in Medicare and thus yield major savings to that program. Using the MedPAC research, this author estimates that Medicare would save $1,400 per enrollee today and an average of $1,600 over each of the next 10 years in reduced overuse from this reform. Assuming that over time it attracted 90 percent participation in both Parts A and B (up from the current 75 percent), total annual Medicare savings for roughly 1.7 million annuitants and spouses 65 and up would be in the range of $2.4 billion a year. This would be a real taxpayer saving, not just shifting costs from one program to another.
This reform alone would largely or entirely eliminate the need to reduce the future cost of the PSRHBF that drives the congressional bills.
-
Establish payment parity for the Medicare Advantage option. Today, federal annuitants who have both Medicare Parts A and B have the option of suspending FEHBP enrollment, enrolling in Part D, and then joining a Medicare Advantage plan (many of which pay the Part D premium), thereby paying premiums in only one program instead of two. This, of course, is a windfall for the FEHBP, as each enrollee in this option reduces FEHBP spending by an additional $1,750 a year by reducing FEHBP costs for drugs. (See Table 1.) To put this option on a level playing field with the usual arrangement of enrolling in both Parts A and B and the FEHBP, the government, as employer, could provide an additional contribution (such as $1,000) to a health savings account on an annual basis to any annuitant who elected this option, effectively reducing the cost of health insurance to these annuitants (who would now be paying only for Medicare, not for a supplemental FEHBP plan). Such an annual contribution could be used to help pay Medicare Advantage cost sharing, to pay for dental plan enrollment, or to save for future costs.
With enrollment in Medicare Advantage, a program of fully integrated health plans and catastrophic protection, there is, of course, no need for any annuitant to have supplemental coverage and pay extra to cover the notorious benefit gaps in traditional Medicare. Therefore, by promoting the Medicare Advantage option, policymakers would tackle directly the dysfunctional and costly relationship that exists today between traditional Medicare and supplemental health plans. By reversing these dynamics, the taxpayer savings could be substantial. Recent research suggests that as enrollment in Medicare Advantage plans increases, there are spillover effects into traditional Medicare that reduce its costs as well.[32] While the research suggests that these effects are less than 1 percent, in a program whose annual spending is over $500 billion even as “little” as 0.5 percent is massive in dollar terms.
For postal annuitants, both these changes could potentially grant the USPS the managerial flexibility to augment the subsidies with higher amounts than provided to non-postal annuitants. Importantly, these options would also have major beneficial effects on the viability and cost of the FEHBP over time by reducing adverse risk selection from the large numbers of high-cost annuitants in the program. The FEHBP, unlike most employer-sponsored health programs, enrolls a very large number of annuitants, and a relatively younger and healthier insurance pool would exert downward pressure on the program’s claims costs.
For the FEHBP and Medicare as a whole, reforming the way employer (and in this specific case, FEHBP) contributions interact with Medicare coverage is a step toward the broader policy agenda of expanding defined-contribution financing (“premium support”) in Medicare. Such a financial payment reform would transition Medicare into a single program where a variety of health plans and options, including employer and FEHBP-sponsored plans as well as a modernized traditional Medicare, would compete for retirees on a level playing field. The end result: Free-market forces of consumer choice and competition would drive down health care costs and drive up the delivery of high-quality health care.
Conclusion
The House postal-retiree health care proposal misses the underlying challenges facing the FEHBP and its uneasy co-existence with Medicare. The proposal fails to address past policy mistakes, makes the interaction between both programs worse by cementing a bad wraparound supplementation model, and puts postal annuitants in the cross hairs for a major economic penalty. For a postal-annuitant couple with an average pension of $36,000 a year,[33] being forced to pay about $3,000 for two Medicare Part B premiums to avoid losing all health insurance is not a light tap on the wallet.
It is long past time for Congress to address FEHBP issues that affect all enrollees, not single out postal annuitants. Congress needs to consider a range of options to deal with the underlying problems of (1) improving the cost-control performance of the FEHBP, and (2) intelligently integrating the interfaces between Medicare and the FEHBP to better control Medicare costs and to provide more sensible choices to annuitants. Not so coincidentally, these broader reforms would eliminate the deficit in the PSRHBF several times over, without any annuitant, postal or non-postal, being compelled to buy an unneeded and costly second health plan in order to keep his current plan, while saving taxpayers billions of dollars annually in the FEHBP and Medicare programs.
—Walton Francis is a Washington-based health care economist, who served at the Office of Management and Budget and the Department of Health and Human Services. He is the principal author of Checkbook’s Guide to Health Plans for Federal Employees.
Appendix
Appendix Table 1 provides the basis for the calculations showing how premiums for postal employees, not yet retired, would cost almost $700 million a year more if put in a separate risk pool from other federal employees. The rounded health care cost data in this table come from the Medical Expense Panel Survey (MEPS), and the data on numbers of employees by age from FEHBP statistics. Similar calculations were provided in testimony to Congress in 2012.