Plan year 2023 is the 10th year of operation for the health insurance exchanges created by the Affordable Care Act (ACA) known as Obamacare. At both the state and county levels, insurer choice and competition in the Obamacare exchanges for 2023 is roughly back to where it was in 2015—before large and escalating losses prompted numerous insurers to exit the exchanges. Despite this stabilization, insurance exchanges are still 24 percent less competitive than markets were before Obamacare was enacted in 2010. New regulations by the Biden Administration and legislation by Congress may spark renewed insurance exits in the coming years and shift more costs on to taxpayers.
State-Level Insurer Competition in the Exchanges
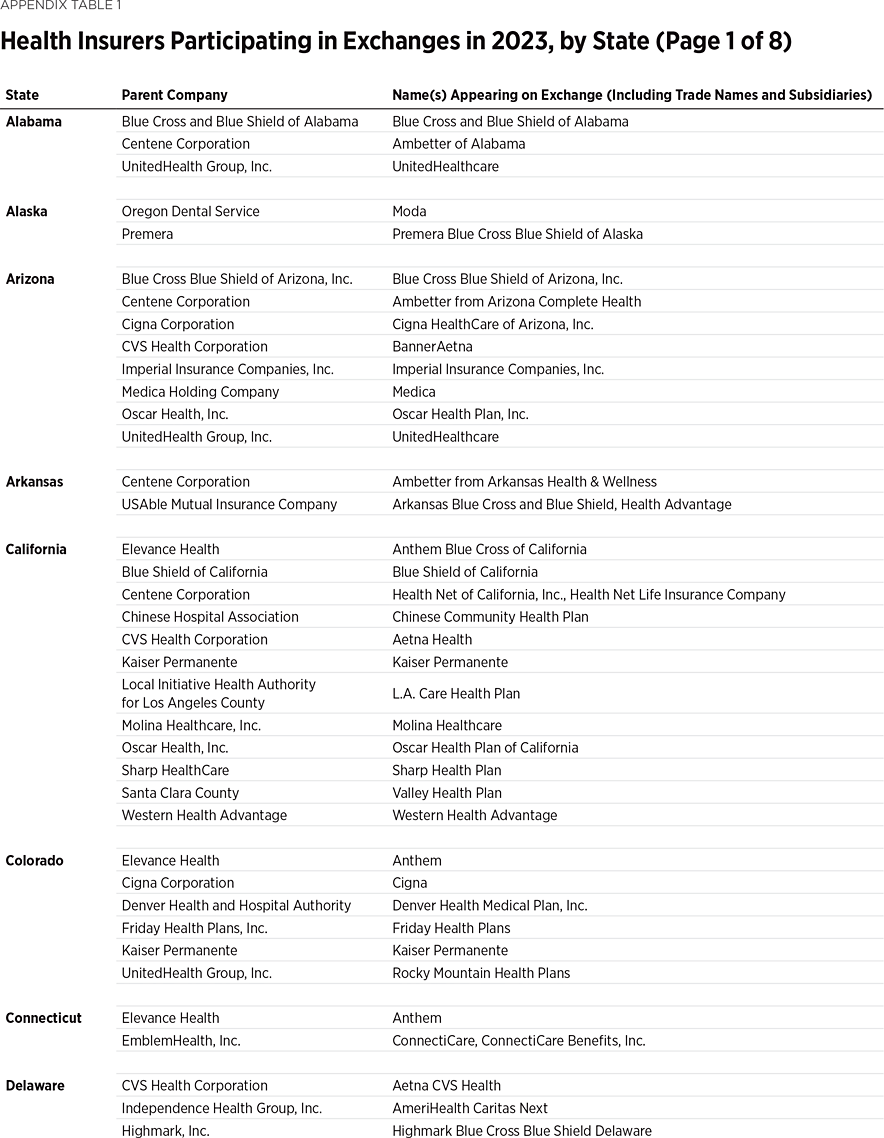
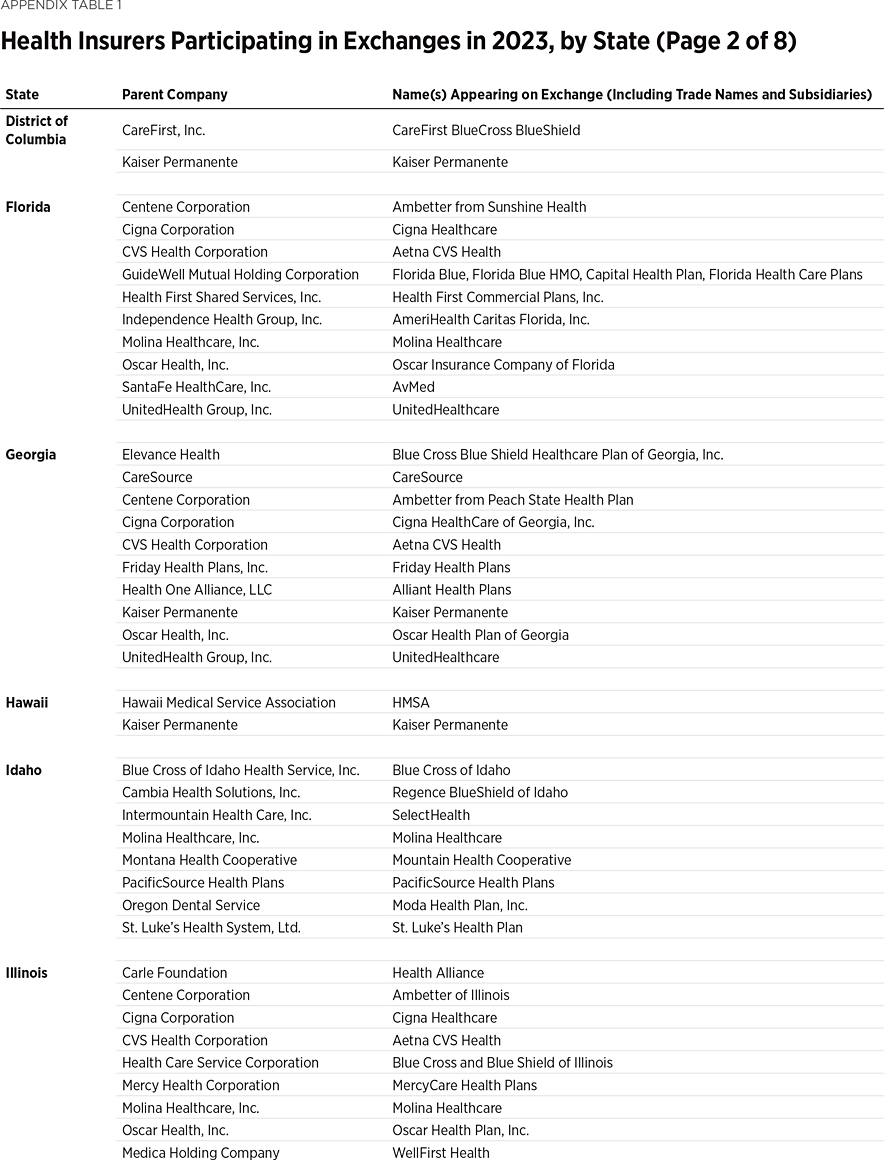
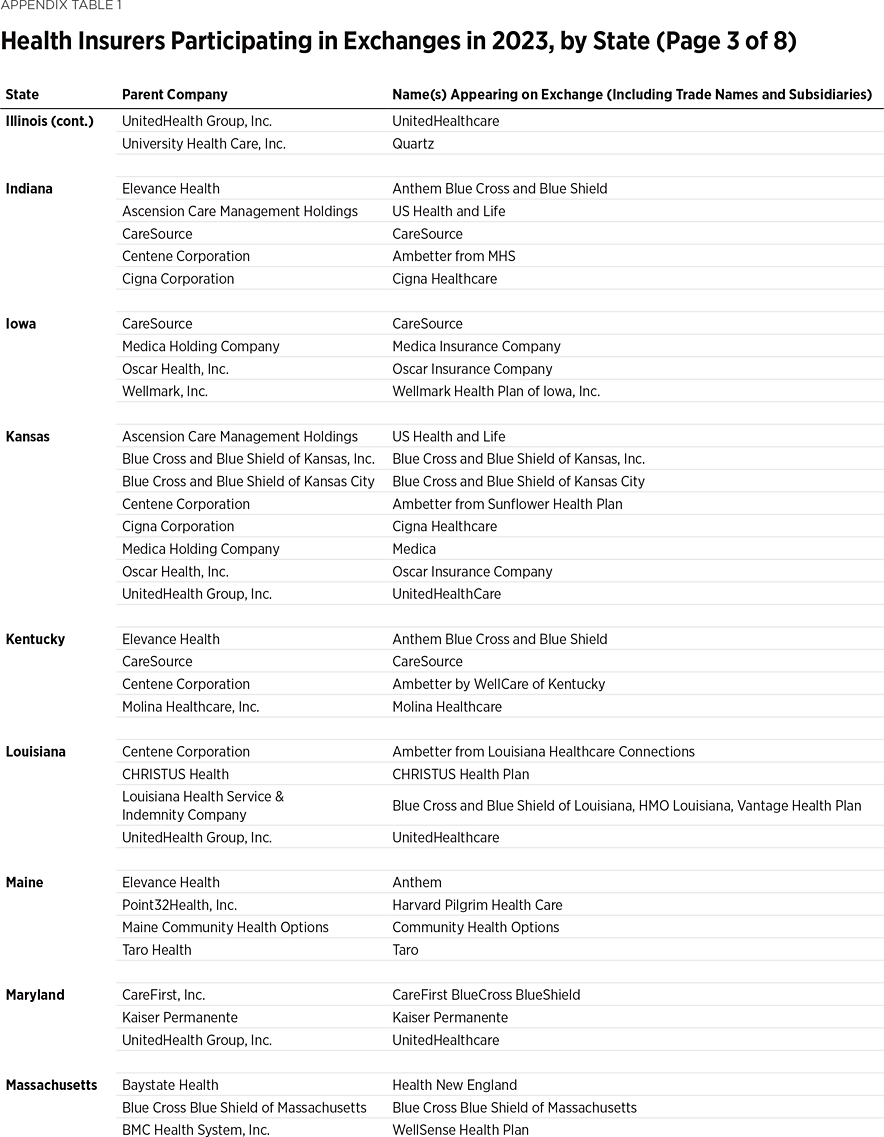
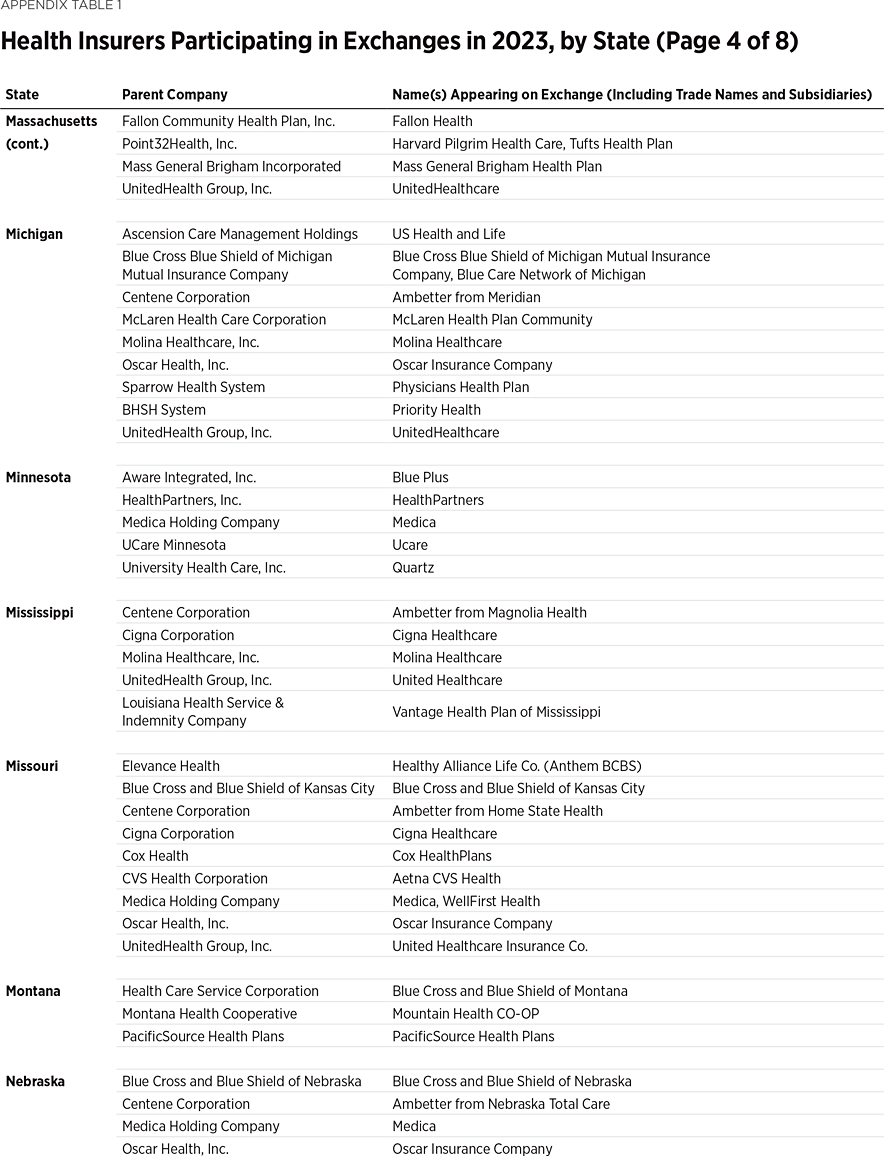
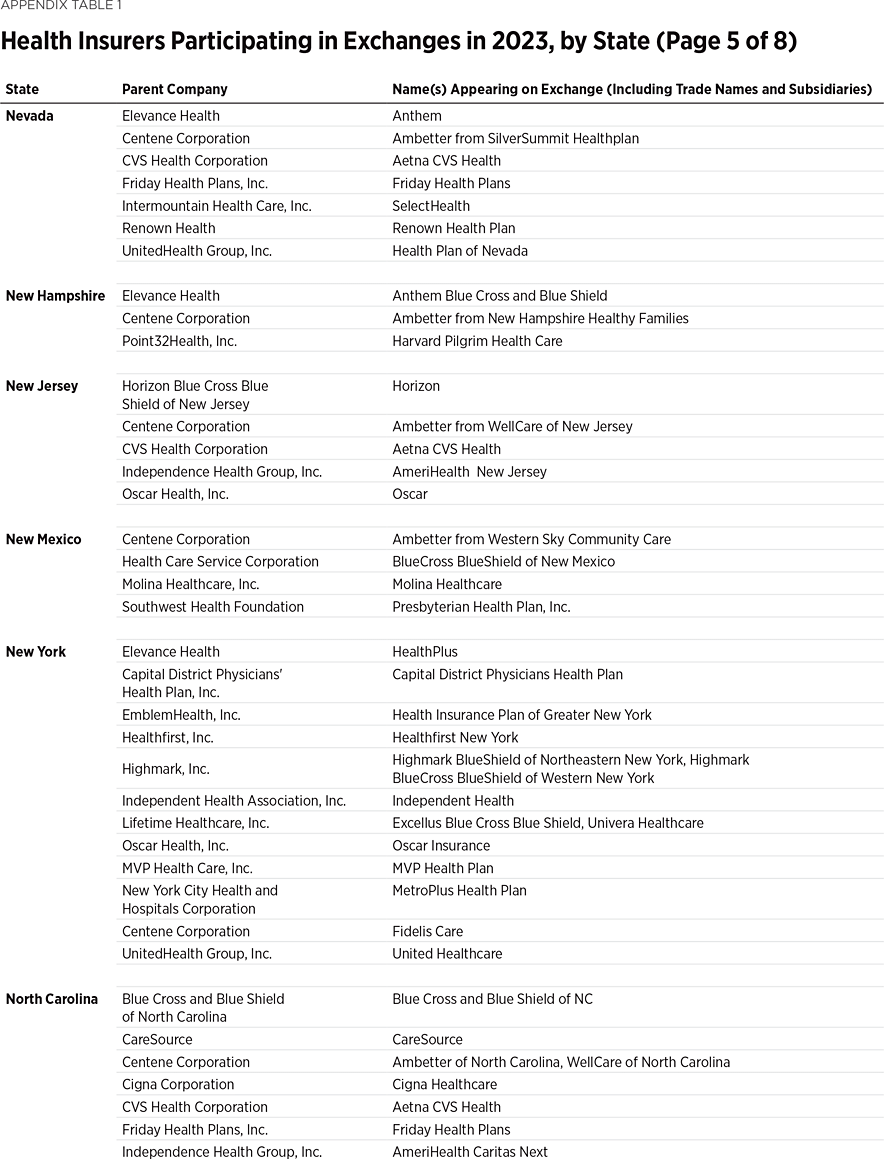
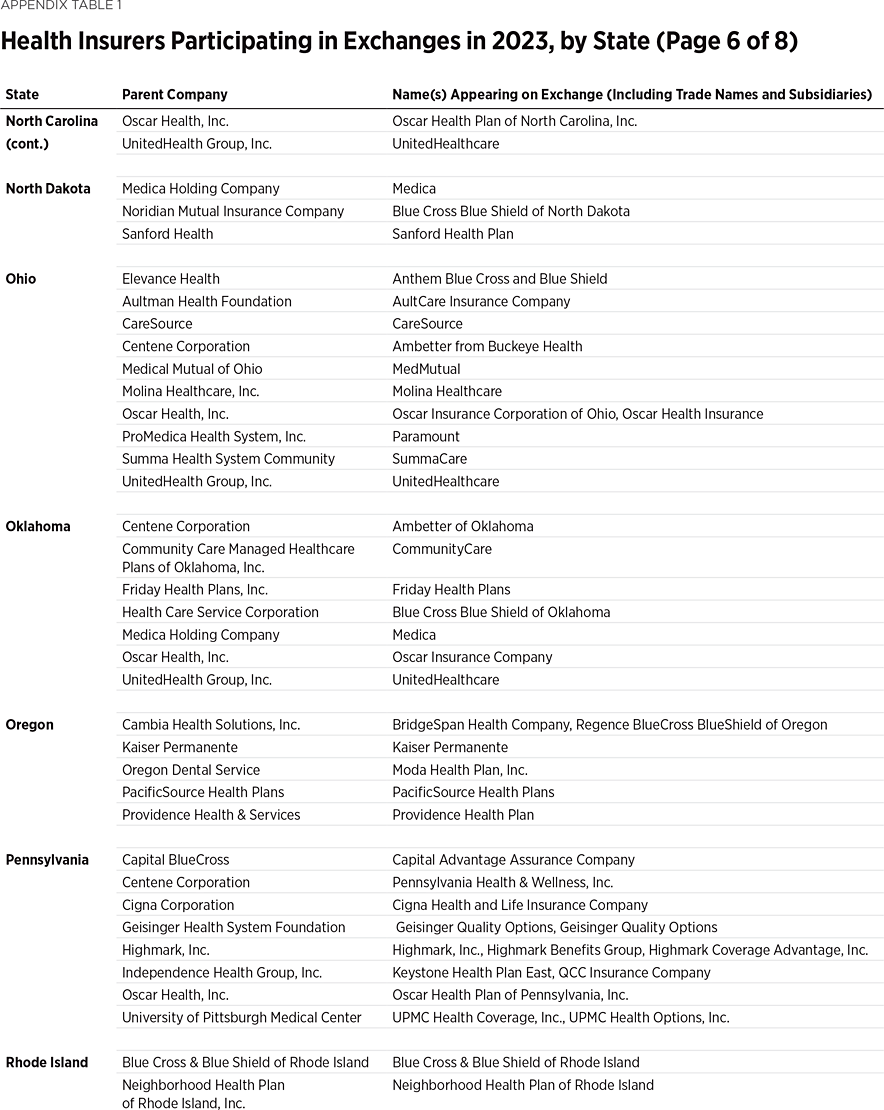
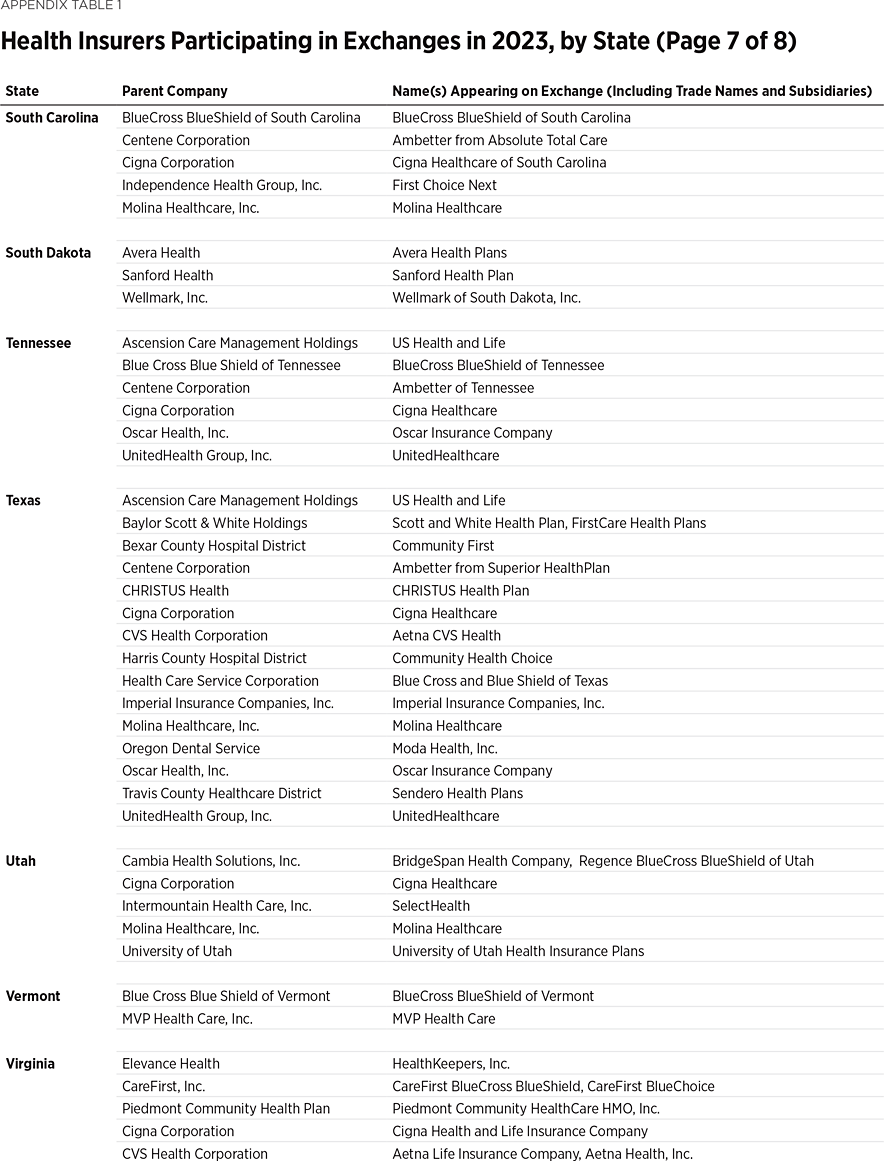
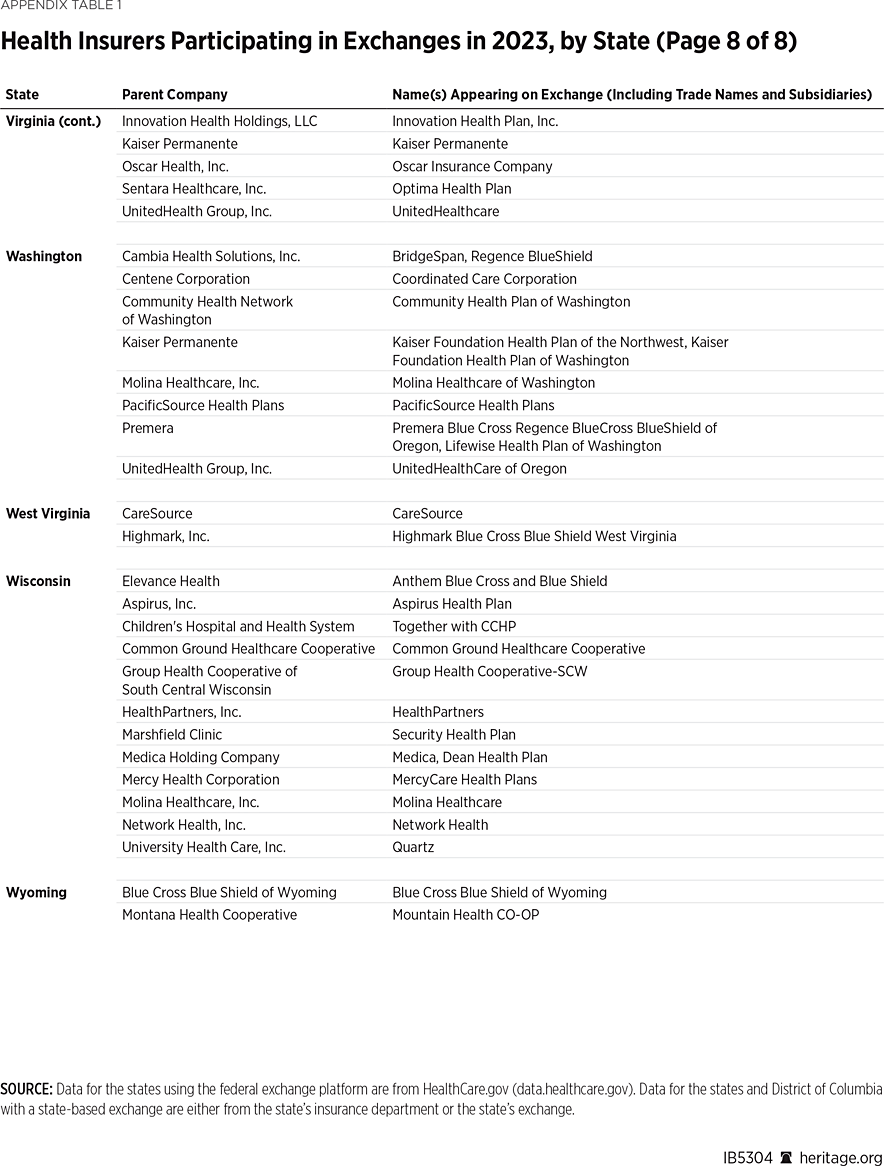
One way to measure insurer competition is to assess insurer participation on a state-by-state basis. That analysis, summarized in Table 1, shows the number of carriers in each state and the District of Columbia in the individual market in 2013, as well as in the exchanges each year since they began in 2014. Insurers that offer exchange coverage through more than one subsidiary in a state are counted as one carrier (the parent company), while insurers that offer coverage in more than one state are counted for each state (as exchange participation is a state-level decision).
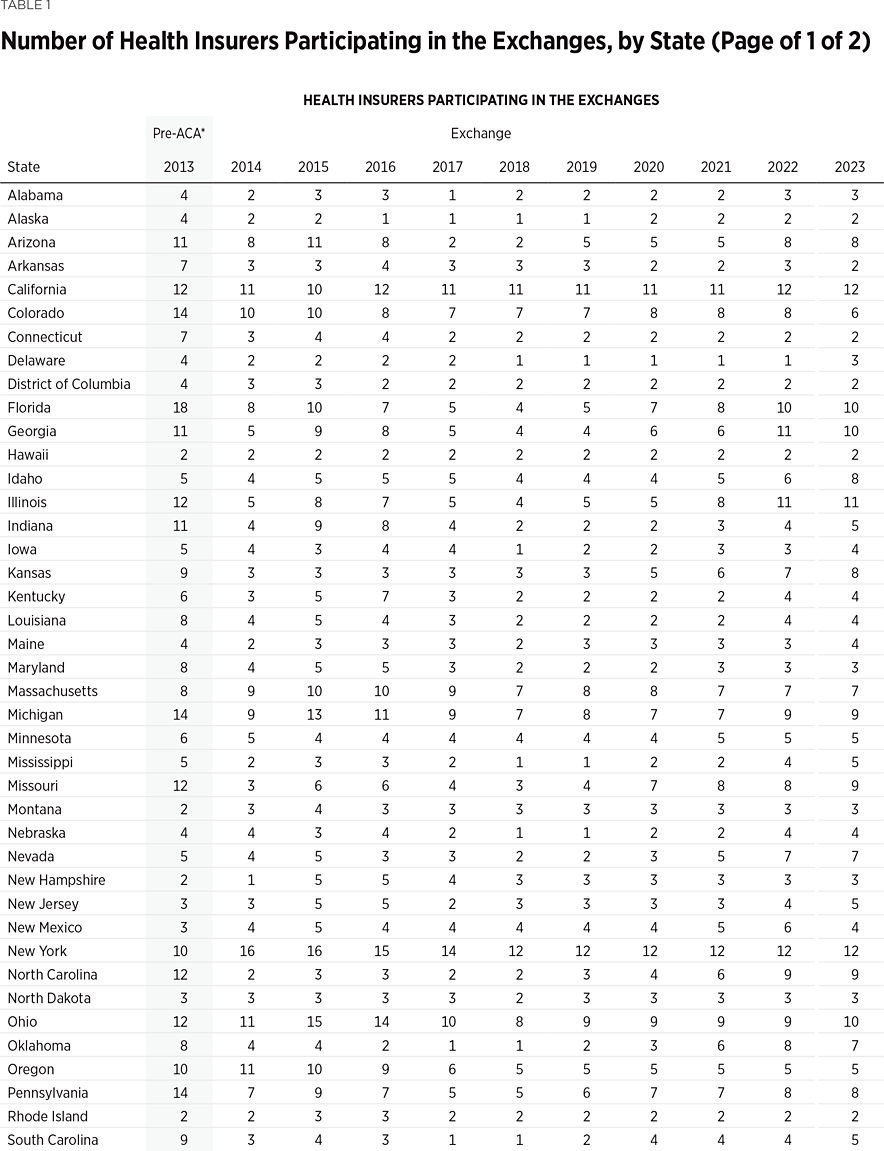
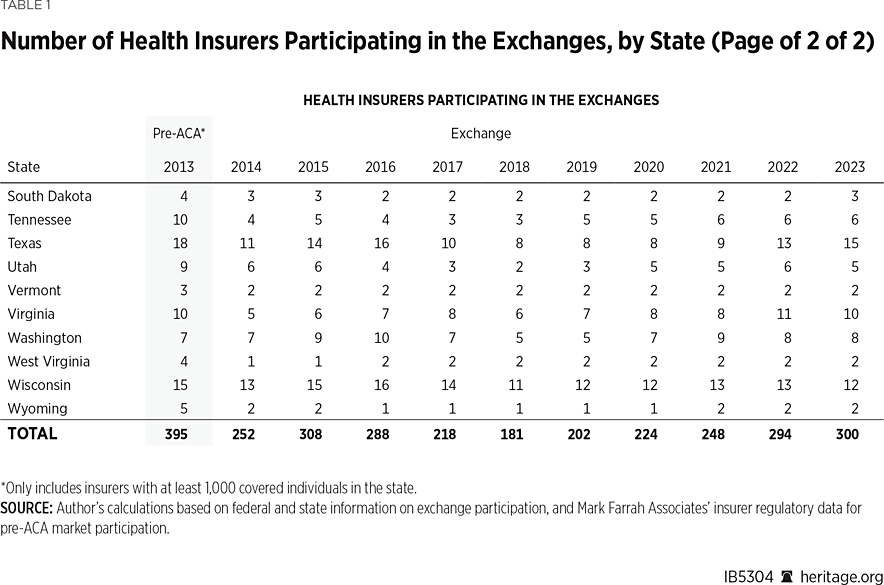
In 2013, the last year before Obamacare’s implementation, 395 insurers sold coverage in the individual market across all states and the District of Columbia. For 2023, 300 insurers offer coverage in the Obamacare exchanges. That is an increase of 119 insurers over the low of 181 in 2018, but it still leaves the 2023 exchanges 24 percent less competitive than the individual market was before the implementation of Obamacare.
Table 1 shows that state-level exchange competition dropped significantly over the three plan years of 2016 to 2018 but then grew again in each of the subsequent years (2019 to 2023).
For plan year 2023, there are a similar number of insurer entrances and exits, with 26 instances of insurers participating in states where they had not done so last year, offset by 20 instances of insurers exiting states where they had offered coverage in 2022. This is the first year that insurer entrances and exits have been roughly balanced, as opposed to being skewed in one direction or the other. The net effect is that, for 2023, the number of insurers offering exchange coverage increased in 13 states and decreased in eight states.
The year-to-year pattern of insurers entering and exiting the exchanges is shown in Chart 1.
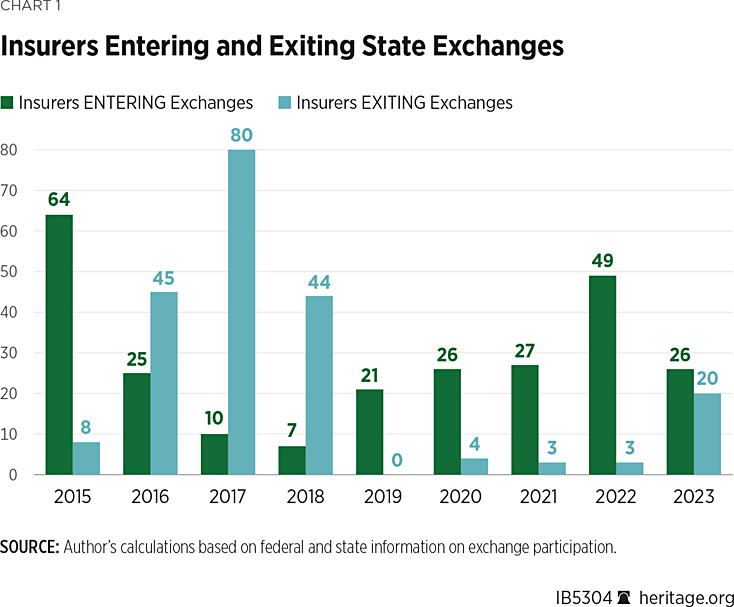
Yet, even with the increase in insurer participation over the past five years, only eight states have more insurers offering Obamacare exchange coverage in 2023 than before the ACA, while eight others have the same number, and 34 states and the District of Columbia have fewer.
2023 County-Level Insurer Competition in the Exchanges
Though state-level data are informative, the most tangible measure of competition for consumers is data at the county level. That is because health plans are offered, and priced, locally. Also, because many insurers only offer Obamacare exchange coverage in certain parts of a state, county-level data provides a more precise picture of the actual choices available to consumers.
The state-level pattern of decreasing insurer participation in the years 2016 through 2018, followed by increasing participation in the years since then, was echoed at the county level.
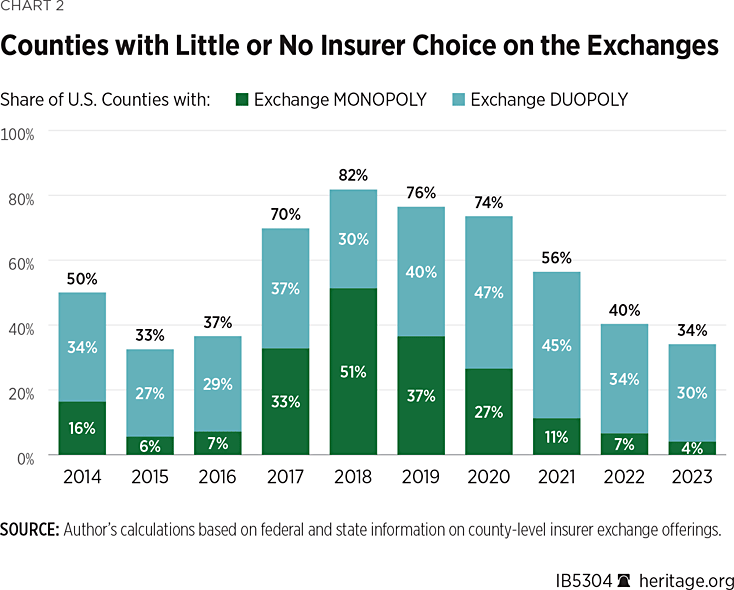
As Chart 2 shows, while the share of counties with only one insurer offering exchange coverage grew to more than half (51.3 percent) of all counties in 2018, it has since fallen to only 4 percent of counties in 2023—its lowest level yet. Chart 2 also shows that the return of insurers to the exchanges has brought the share of counties with an insurer monopoly or duopoly back down from 81.8 percent in 2018 to 34.1 percent in 2023.
Patterns of Insurer Exchange Participation
Smaller carriers accounted for all 20 instances of insurers exiting the exchanges for 2023. Bright Health exited all 15 states where it offered exchange plans in 2022, while Oscar Health and Friday Health Plans each dropped out of two states, and Wisconsin Physicians Service Insurance Corporation exited that state’s exchange.
National carriers either resuming or expanding their exchange offerings accounted for 12 of the 26 instances of insurers initiating exchange coverage in 2023. United returned to the exchanges in four states that it had exited back in 2017.REF Aetna (now owned by CVS) returned to two states and is offering exchange coverage for the first time in two more.REF Similarly, Cigna returned to Texas and expanded its offering of exchange plans to Indiana and South Carolina, while Medicaid managed care insurer Centene expanded into Alabama.
Also notable is that Blue Cross and Blue Shield of Nebraska returned to that state’s exchange after a six-year absence, and that Wellmark Blue Cross and Blue Shield of South Dakota is now offering exchange plans in that state for the first time.
Another trend has been the growth in exchange participation by Medicaid managed care insurers. The largest of those carriers, Centene, steadily expanded its exchange footprint from nine states in 2014 to 28 states for 2023. As a result, Centene now offers exchange coverage in more states than any other insurer and is the carrier with the largest share of exchange enrollees. Molina, another for-profit Medicaid managed care insurer, is offering 2023 exchange coverage in 14 states while two nonprofit Medicaid managed care insurers, CareSource and AmeriHealth (a subsidiary of Independence Blue Cross), offer exchange coverage in seven and six states, respectively. The net effect is that for 2023 there are 34 states in which one or more of those four Medicaid managed care insurers are offering exchange coverage.
That pattern likely reflects the fact that the ACA’s premium subsidies and reduced-cost-sharing silver plans were designed to provide nearly free coverage to individuals with incomes just above Medicaid eligibility. The result has been that such individuals now constitute a disproportionate share of the exchange market. Indeed, open enrollment data for plan year 2022 showed that 56.2 percent of enrollees had incomes below 150 percent of the federal poverty level (FPL) and 74.9 percent had incomes below 200 percent of FPL.REF
Uncertain Future
While choice and competition in the exchanges has increased in recent years, two significant policy changes in 2022 introduced new uncertainties for the exchange market. The first is a set of regulatory changes made by the Biden Administration, and the second is a set of subsidy changes enacted by Congress.
The rebound in insurer competition since 2018 was largely a response to regulatory actions taken by the Trump Administration to stabilize the exchange market. However, in May 2022, the Biden Administration promulgated a rule that reverses some of those changes and risks making the exchange market more costly and less attractive to insurers in the future.REF In particular, the new Biden Administration rule:
- Reinstates a loophole that previously enabled enrollees to skip paying premiums for the last month or two of a plan year;
- Eliminates verification requirements for many “special enrollment periods,” which could encourage more individuals to forego buying coverage until they need medical care;
- Imposes new “one-size-fits-all” rules for “network adequacy” that could make it more difficult for insurers to offer plans, in particular, in rural counties; and
- Requires insurers to offer government-designed “standard” plans.
In commenting on the rule, insurers and actuaries identified the potential adverse effects of these changes, but the Biden Administration adopted them anyway.REF Should the anticipated adverse effects materialize, they could disincentivize future insurer participation in the exchanges.
The second set of changes stem from legislation enacted in March 2021 that increased ACA premium subsidies at all income levels and lifted the 400 percent of FPL cap on subsidy eligibility for the years 2021 and 2022.REF In August 2022, Congress enacted an extension of those temporary provisions through the end of 2025.REF
How these two sets of policy changes will interact and play out over the next several years is an open question. On the one hand, the Biden Administration’s regulatory changes have the potential to make the exchange market more costly and more unpredictable for insurers—possibly sparking renewed insurer exits. On the other hand, the expanded exchange subsidies will make exchange customers less price sensitive, and thus potentially give exchange carriers more latitude to increase their premiums to compensate for higher expected losses.
Conclusion
As the Obamacare exchange market has stabilized over the past five years, more insurers have resumed, or expanded, their offering of exchange coverage. Consequently, at both the state and county levels, insurer choice and competition in the Obamacare exchanges for 2023 is roughly back to where it was in 2015—before large and escalating losses prompted numerous insurers to leave the exchanges.
Whether that will remain the case over the next several years depends on how the combination of new cost-increasing rules from the Biden Administration and Congress’s three-year extension of increased exchange subsidies plays out.
Edmund F. Haislmaier is the Preston A. Wells, Jr., Senior Research Fellow in the Center for Health and Welfare Policy at The Heritage Foundation.