Americans should ignore false promises to keep “Medicare as we know it”—the program is already changing. Under the misnamed Patient Protection and Affordable Care Act of 2010, Congress and President Barack Obama have already enacted big reductions in Medicare funding (amounting to $716 billion over the next 10 years[1]), as well as complex new rules governing federal reimbursements to doctors and hospitals. But beyond the changes wrought by the new health care law, Medicare is facing enormous demographic changes: The first wave of the massive baby boom generation—the 77 million people born between 1946 and 1964—is now becoming eligible for Medicare enrollment.
The sheer number of beneficiaries is projected to grow from 50.7 million in 2012 to 81 million in 2030.[2] This will create an unprecedented demand for technologically advancing medical services in the 21st century. Current taxpayers already pay almost nine out of every 10 dollars in total Medicare costs in any given year, and general revenues will account for an increasingly larger share of Medicare spending [3] In other words, current and future taxpayers are being saddled with enormous obligations.
In the near term, Congress and the Administration should undertake a series of changes to the current program that would alleviate the fiscal impact of these demographic pressures. Such initiatives would include (1) gradually raising the age of eligibility for Medicare (and Social Security) to 68; (2) repealing existing penalties for late enrollment in Medicare for those who remain in private, employer-based coverage; and (3) tax relief for employees (and their employers) for those workers who continue to work beyond the standard retirement age.
The long-term solution to the demographic challenge is a full transition of Medicare to a program based on defined-contribution (“premium support”) financing. The per-capita government payment to health plans, including traditional Medicare, would be centered on a market-based bidding for the provision of traditional Medicare benefits. Plans and providers would thus compete to provide the best package of guaranteed benefits at the most competitive price. This would not only spur innovation in the delivery of medical services, but would also secure value for the Medicare dollars. Intense competition would slow the growth of Medicare spending, and secure program savings that would, over time, benefit Medicare recipients and taxpayers alike.
Demographic Impact on Medicare Spending
Medicare spending is projected to rise significantly over the next 25 years as the baby boomers enroll in the program. Under the most realistic scenario, the Medicare Trustees project that Medicare spending will rise from 3.7 percent of gross domestic product (GDP) in 2011 to 7 percent of GDP in 2040, and 10.3 percent of GDP in 2085.[4]
A major reason for the future growth in health care programs’ spending is the aging population. While the costs per beneficiary are rising, it is the sheer number of eligible beneficiaries that is driving Medicare costs up so dramatically. The Congressional Budget Office (CBO) states that “[t]hrough 2022, the aging of the population will cause spending on the major health care programs and Social Security to rise significantly.... In fact, during that period, almost all of the projected growth in such spending as a share of GDP is effectively the result of aging.”[5]
Through 2037, under the alternative fiscal scenario, which uses more realistic assumptions, the CBO attributes 52 percent of the reason for projected growth of this magnitude to the aging population, with the other 48 percent attributed to excess health care cost growth. Under the budget scenario that reflects current law, the CBO holds aging responsible for 60 percent of the cause in spending growth.[6]
The massive projected increase in Medicare spending and enrollment is contributing to financing shortfalls. The hospital insurance trust fund, which funds Medicare Part A, has been running deficits each year since 2008 and is projected to be exhausted by 2024.[7] Moreover, under a more realistic scenario, Medicare has a long-term unfunded obligation of $37 trillion; in other words, Medicare will have promised seniors and disabled citizens $37 trillion worth of unpaid benefits.[8] Once again, this means that taxpayers are faced with increasing burdens, the sheer size of which they can barely imagine.
An Aging Population
Today’s Medicare eligibility standards are rooted in the entitlement policies of the 1930s and the 1960s. When Social Security was enacted in 1935, the average American life span was 62 years, but Congress and President Franklin D. Roosevelt set the retirement age at 65. In 1961, Congress and President John F. Kennedy established an early retirement eligibility at age 62, allowing early retirees to collect a reduced Social Security benefit.
Labor force participation among older workers changed in part due to the introduction of the Social Security entitlement. In 1930, 60 percent of men aged 65 and above who could work did so; and virtually everyone in the 1940s and 1950s who left the workforce did so because of necessity, that is, a job loss, or unemployment related to poor health or incapacity.[9] By the 1960s and 1970s, between 20 percent and 30 percent of American workers said that they retired because they wanted to do so.[10] Since the 1960s, the number of men who are 65 or older and still in the workforce has shrunk to one out of six.[11]
In 1965, when Congress and President Lyndon B. Johnson enacted Medicare, they retained Social Security’s standard retirement age of 65 as the age of eligibility for Medicare. By 1965, however, the average life expectancy had increased to 70.2 years. By 2008, the average life span was 77.8 years, and is projected to reach 81.5 years by 2030.[12] In 2009, Americans had already exceeded the life expectancy that the Medicare Trustees had projected for 2025.[13]
Meanwhile, fewer children have been born to support America’s much larger and older retired population. Between 1973 and 1988, the U.S. fertility rate stabilized at 1.8 to 1.9 births per woman, compared to the 2.1 lifetime births per woman required to maintain a constant population.[14] In other words, the baby boomers did not replace themselves.
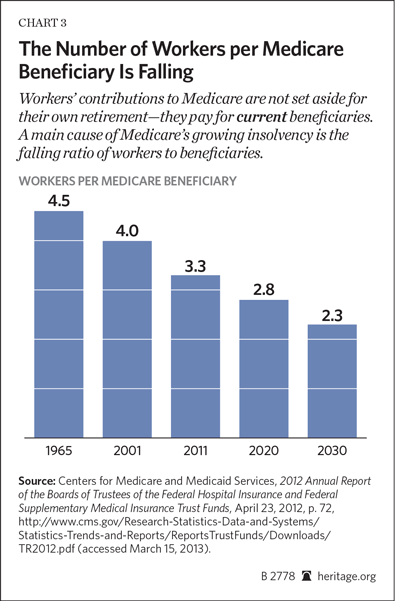
A related development is the decline in the ratio of workers to retirees, which is critically important because current workers pay for current beneficiaries through the Medicare payroll tax. When Medicare first began in 1965, there were 4.5 workers per beneficiary. The ratio has since declined, standing at 3.3 workers in 2011, and is projected to decline further to just 2.3 workers per beneficiary by 2030. For a perspective on the magnitude of this demographic shift, consider the fact that in 1950, there were 16 persons working and paying taxes to support one person drawing Social Security benefits.[15]
A Growing Bipartisan Consensus
In 1983, Congress and President Ronald Reagan, following a report from the Greenspan Commission, gradually raised the standard retirement age for Social Security from 65 to 67. Today, people born in 1937 or before retain the legal right to collect full benefits at age 65. For those born between 1943 and 1954, the retirement age is 66. For those born in 1960 or later, the retirement age is 67.
As a matter of social policy, it is worth noting that surveys show a positive relationship between work and health and happiness.[16] Congress should not ignore the potential social benefits of greater workforce participation among older Americans.
The CBO has already estimated that this limited change will increase American workforce participation for those aged 65 and above.[17] Such a policy would not only help to improve Medicare’s financing, it would also provide stronger incentives for seniors to increase their retirement savings and contribute to overall economic growth.[18]
The CBO has also projected the budgetary impact of a gradual increase in the age of Medicare eligibility from 65 to 67 for the tail end of the baby boom generation. By raising the age of eligibility by two months every year, beginning for those baby boomers born in 1949, it would reach 67 for those born in 1960. This change would save $148 billion in Medicare spending between 2012 and 2021.[19]
A bipartisan consensus is emerging on raising the age of Medicare eligibility. The Business Roundtable, an association of leading American companies, has recently proposed that Medicare’s age of eligibility should be increased to 70, while not affecting any person today who is 55 or older[20] The American Hospital Association supports gradually raising the eligibility age to 67.[21] In addition, Senator Orrin Hatch (R–UT) recently proposed raising the eligibility age to 67 in a major speech on the Senate floor, as a key entitlement reform that should be a part of any deficit reduction package.[22] Likewise, Alice Rivlin, a senior fellow at the Brookings Institution and former director of the Congressional Budget Office, and William Galston, a former adviser to President Bill Clinton, have endorsed raising the retirement age to 67. President Obama, during his 2011 discussions with congressional leaders on the debt ceiling, also agreed to raise the age of eligibility to 67.[23] It is unclear whether the White House would support such a change today.
Short-Term Reform
In keeping with the goal of comprehensive Medicare reform, Congress should take three initial steps:
- Raise the standard age of eligibility for both Medicare and Social Security to 68 over the course of 10 years, and thereafter index the eligibility age to longevity.[24] The Heritage Foundation’s Center for Data Analysis estimates that raising the Medicare eligibility age to 68 at the rate of two months per year beginning in 2012 would save $52.8 billion over five years and $243.6 billion over 10 years.[25]
- Repeal the 10 percent penalty for late enrollment in Medicare Part B for seniors who remain in employment-sponsored health plans and thus reduce Medicare costs.[26]
- Provide tax relief for those who work beyond the standard retirement age. For example, under the Heritage Saving the American Dream proposal, any person, regardless of income, who works beyond the standard retirement age would automatically qualify for an annual $10,000 tax deduction.[27]
Long-Term Reform
The best policy for coping with the retirement of the massive baby boom generation is structural Medicare reform based on a defined-contribution (“premium support”) program of financing. The Heritage Foundation has developed the components of such a reform in detail.[28]
Under such a reform, which would build upon the experience of Medicare Part D and the success of the popular Federal Employees Health Benefits Program (FEHBP), government payment to competing health plans (including traditional Medicare) would be calculated based on market-based bids to provide Medicare benefits, and beneficiaries would choose the plan that best meets their personal needs. Intense market competition among plans and providers, driven by personal choice, will not only secure better value for Medicare dollars, but will also reduce the growth in Medicare spending.
—Robert E. Moffit, PhD, is Senior Fellow in the Center for Policy Innovation at The Heritage Foundation. Alyene Senger is a Research Assistant in the Center for Health Policy Studies at The Heritage Foundation.





