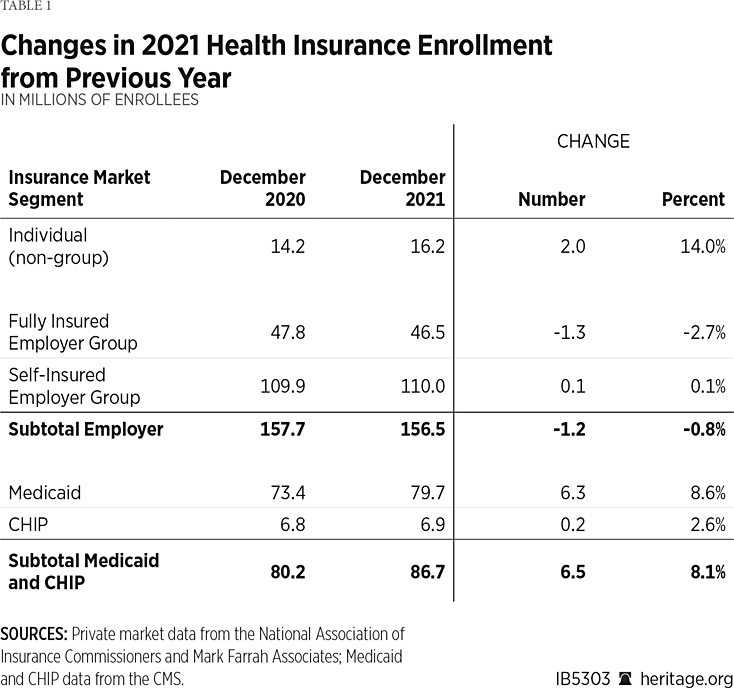
In 2021, the most recent year for which complete data are available, enrollment in employment-based group coverage declined by 1.2 million individuals (1 percent) while enrollment in individual-market (non-group) plans increased by 2 million individuals (14 percent) and public program coverage through Medicaid and the Children’s Health Insurance Program (CHIP) expanded by 6.5 million individuals (8 percent).REF (See Table 1.)
The Role of Government COVID-19 Responses
The enrollment changes in 2021 appear to have largely been the continuing results of government policies implemented in response to the COVID-19 pandemic. Specifically, the Families First Coronavirus Response Act provided states with a 6.2 percentage point increase in their Federal Medical Assistance Percentage on the condition that they maintain eligibility for all individuals enrolled in their programs on or after the date of enactment (March 18, 2020) until the end of the quarter in which the COVID-19 public health emergency (PHE) terminates.REF
The Coronavirus Aid, Relief, and Economic Security (CARES) Act, enacted on March 27, 2020, temporarily increased unemployment-compensation payments and specified that the additional payments were not to be counted as income for purposes of determining Medicaid or CHIP eligibility.REF
Also, the American Rescue Plan enacted in March 2021 temporarily increased ACA premium subsidies at all income levels and lifted the 400 percent of the federal poverty level (FPL) cap on subsidy eligibility for the years 2021 and 2022.REF
Table 2 provides further perspective on the effects of government responses to COVID-19 by comparing enrollment data for the two years prior to the onset of COVID-19 (2018 and 2019) with the two years of the COVID-19 response period (2020 and 2021).
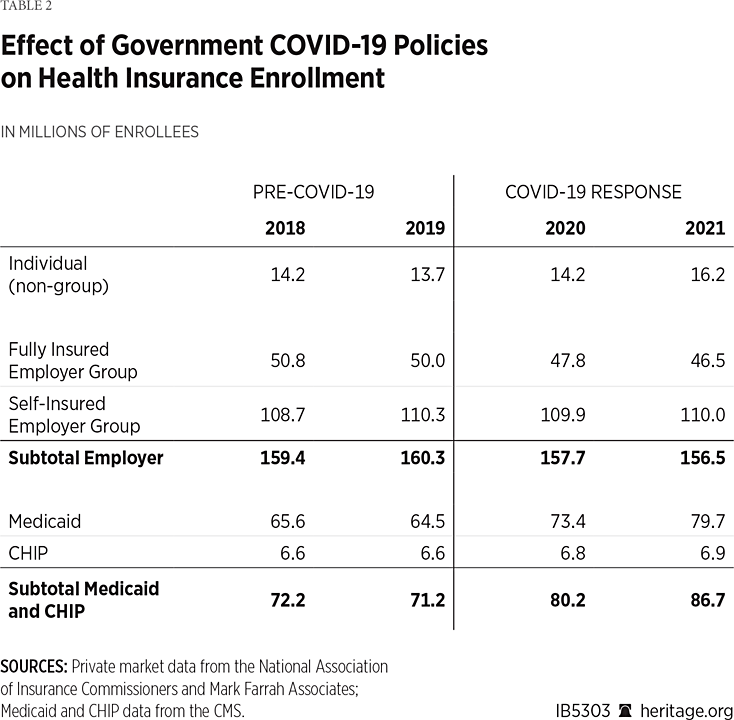
As Table 2 shows, the bulk of the coverage losses occurred in the fully insured employer-group market. Fully insured group plans are purchased primarily by small and medium-size firms, while larger businesses tend to self-insure their health plans. Enrollment in the fully insured group market dropped by 2.2 million individuals (4.5 percent) in 2020 and by a further 1.3 million individuals (2.7 percent) in 2021. Those enrollment declines were likely due to state and local government lockdowns, whose adverse economic consequences disproportionately affected small and medium-sized businesses and their workers. In contrast, the data show that there was little effect on enrollment in self-insured group plans.
The biggest enrollment gain was in Medicaid, with the individual (non-group) coverage market also experiencing increased enrollment. Enrollment in Medicaid and CHIP increased by 9 million individuals (12.6 percent) in 2020 and by a further 6.5 million (8.1 percent) in 2021. Almost all that increase was in Medicaid, with CHIP enrollment increasing only slightly.
The large increase in Medicaid enrollment reflected not only pandemic-related economic dislocation, but also the temporary program changes enacted by Congress that prevented states from discontinuing coverage when individuals cease to be eligible (often due to an increase in income).
With respect to the individual market, which encompasses both subsidized and unsubsidized customers, it is likely that much of the increased enrollment was due to the temporary expansion of premium subsidies. Enrollment in individual-market coverage grew by 600,000 (4 percent) in 2020, and then by a further 2 million individuals (14 percent) in 2021. The size and timing of those enrollment increases strongly indicates that the temporary expansion of ACA subsidies was a driver of 2021 enrollment gains in that market.
Obamacare’s Effects on Health Insurance Enrollment
The ACA created new subsidies for individual-market coverage purchased through the exchanges and incentivized states to expand their Medicaid programs to cover all able-bodied, non-elderly adults below 138 percent of the FPL by providing a very high federal match rate (90 percent) for those enrollees. Both changes took effect in 2014. Table 3 widens the perspective by reporting enrollment changes in the subsequent years.
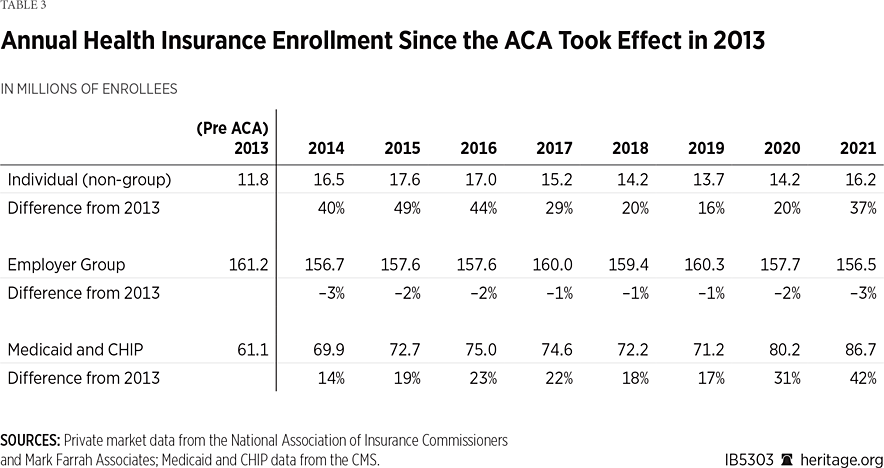
During the eight-year period of 2014 through 2021, individual-market enrollment was, on average, about 30 percent higher than before the implementation of the ACA, average Medicaid enrollment was about 20 percent higher, and average enrollment in employment-based group coverage was about 2 percent lower.
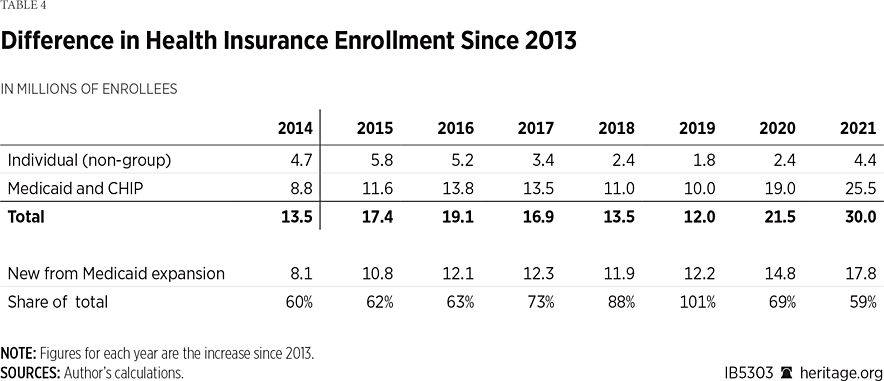
However, while the post-ACA enrollment increase for the individual market was large in percentage terms, the numerical increase was greater in Medicaid. That was because, prior to the ACA’s implementation in 2014, enrollment in Medicaid was five times larger than individual-market enrollment. Consequently, as Table 4 shows, about 80 percent of the total increase in enrollment following implementation of the ACA was attributable to the growth of Medicaid. Of those additional enrollees, some qualified under the pre-ACA eligibility criteria, but most qualified under the ACA’s expansion of eligibility to able-bodied non-elderly adults.
Policy Implications
It is likely that much of the net increase in Medicaid enrollment in 2020 and 2021 reflects the retention of individuals who will no longer qualify for coverage once the application of normal eligibility criteria resumes. On December 23, 2022, Congress enacted the Consolidated Appropriations Act of 2023, which included provisions phasing out the enhanced match and permitting states to resume Medicaid eligibility redeterminations.REF That exercise is expected to take the better part of a year and state officials would be well advised to start planning and budgeting for it now.REF
The expansion of ACA exchange subsidies for individual-market coverage was also temporary for two years (2021 and 2022), but in August 2022, Congress enacted a further three-year extension (through the end of 2025).REF Given that the basic structure of the ACA subsidies already insulated subsidized enrollees from most of the effects of increased premiums, the temporary expansion only marginally altered what most enrollees were directly paying for their coverage.REF
Indeed, Table 3 shows that even with the surge in enrollment in 2021, the number of people with individual-market coverage that year was still less than what it was in the years 2014 through 2016.
Consequently, repealing the three-year extension of the Obamacare subsidy enhancements would likely have only modest effects on enrollment, but would reduce excessive federal spending.
Conclusion
Health insurance enrollment changes in 2020 and 2021 were largely driven by government policies in response to the COVID-19 pandemic. Indeed, the temporary expansions of Medicaid and Obamacare subsidies were largely aimed at countering the negative economic and employment effects that resulted from other government responses to COVID-19, particularly lockdowns and business closures.
The reality is that current insurance market rules and the availability of alternative coverage options, including subsidized ones, are already sufficient to enable people to obtain or switch health insurance coverage when faced with changing economic circumstances.
Having enacted legislation to phase out the enhanced Medicaid funding and associated restrictions on eligibility redeterminations, Congress should now also end the increased ACA subsidies that were enacted in response to the pandemic.
Going forward, both federal and state lawmakers should refocus on the longer-term task of reducing health care costs by expanding competition, particularly through greater price transparency and the elimination of anti-competitive regulations and business practices that insulate favored medical providers from competition.
Edmund F. Haislmaier is the Preston A. Wells, Jr. Senior Research Fellow in the Center for Health and Welfare Policy at The Heritage Foundation.



