Senator Bernie Sanders (I–VT), along with 16 Senate Democrats, is sponsoring the Medicare for All Act of 2017 (S. 1804).[REF] The legislation would outlaw almost all private insurance and create a government health care monopoly: a single entity delivering, as well as financing, medical benefits and services. Federal officials, most notably the Secretary of the U.S. Department of Health and Human Services (HHS), would have almost total control over America’s health care financing, organization, and delivery.
Senator Sanders and his Senate colleagues are not alone. Representative John Conyers (D–MI) is sponsoring broadly similar legislation in the House with the support of 120 Representatives, more than half of the entire House Democratic membership.[REF]
The Sanders’ bill provides for a four-year transition period. At the end of that period, the federal government would run a national health plan. The new law would also expand the already formidable power of the HHS Secretary, well beyond the broad scope of authority that the Secretary already exercises under Obamacare. Unlike previous iterations of the legislation, however, the far-reaching measure contains no provisions for its financing. Instead, Senator Sanders and his colleagues have separately provided for a set of financing “options” for the measure, including a broad-based federal payroll tax, a new “premium tax,” and a series of additional taxes on private savings and investments, especially targeted at upper-income citizens.
Private monopolies exist when there are no firms producing and delivering a similar good or service. A government monopoly enjoys the same dominance, but, unlike a private firm, is armed with the coercive power of the law. In the case of the Sanders bill, the federal government would undertake a radical restructuring and consolidation of third-party payment, as well as a comprehensive control over the ways and means to reimburse and limit payment to doctors, hospitals, and other medical professionals. These payment restrictions—largely a continuation of the Medicare price-control system—are combined with practice guidelines governing how doctors and other medical professionals are to deliver medical benefits and services.
For ordinary Americans, there would be no escape. Except for a small set of benefits uncovered by the government plan, individuals and families would, ipso facto, have no health care options. Federal government officials would determine the kind of plan they get, the benefits they get, the medical procedures and treatments that would be available to them under the new government system, and under what circumstances, terms, or conditions they may receive medical services or benefits. In short, the bill would constitute a major restriction on personal and economic freedom.
If the Sanders bill becomes law, Americans can expect:
-
A prohibition of private health plans. Today, nearly 60 percent of working-age Americans get their health insurance through private, employer-sponsored health plans. Under the bill, the government would effectively outlaw almost all private health insurance, whether offered by employers or by insurers in the individual or small-group markets. Under Title VIII, Section 801, the bill language specifies, for example, that “no employee benefit plan may provide benefits that duplicate payment for any items or services for which payment may be made under the Medicare for All Act of 2017.”[REF] Employers and insurers would be able to offer non-covered benefits and services, but the sponsors of the bill intend these offerings to be minimal. The reason: The government health benefits program would be comprehensive, covering 10 major benefit and service categories, and, of course, there would be no private health plan legally permitted to offer Americans these benefits, regardless of their preferences in the matter, under different terms and conditions. In short, competition with the government health plan would be illegal.
It is worth noting that a recent NBC/ Wall Street Journal poll found that the general public favors the adoption of a “single-payer” health plan by a slim margin of 47 percent to 46 percent. When the public realizes that this would mean the elimination of employer-sponsored health insurance, however, support for the proposal falls to just 36 percent with 55 percent of the respondents opposed.[REF]
-
The absorption of existing government health programs. While the Senate legislation is popularly advertised as “Medicare for all,” ordinary Americans should understand that the bill language would not preserve “Medicare as we know it.” In fact, the bill would make major changes to the Medicare program, including the elimination of private plan options that exist today, and under Title IX of the proposed measure, Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP) would, as a matter of law, be phased out during the transition period and absorbed into the new government health plan. With Medicare, for example, “no benefits shall be available under Title XVIII of the Social Security Act for any item or service furnished beginning on or after the effective date of benefits under Section 106 (a).”[REF]
Likewise, the bill specifies that “no individual is entitled to medical assistance” from a state Medicaid plan (except for long-term care) or a state CHIP plan. However, the bill would provide a continuity of coverage for persons enrolled in those programs during the transition to the new government plan.[REF] Enrollment in the Obamacare health insurance exchanges would also end, and the bill would transition current enrollees into coverage under the new government health plan.
When fully implemented, the Senate bill would also end enrollment and the provision of health benefits for over 8 million federal employees and retirees and dependents under the popular and successful Federal Employees Health Benefits Program (FEHBP), a system of competing private plans, the largest group health insurance program in the world. Historically, notably during the 1994 debate over the proposed Clinton health plan, the threat of abolishing or eliminating the private health insurance coverage for federal workers and retirees has sparked ferocious opposition among members of the federal workforce.[REF] Beyond federal workers and retirees, the bill would also end enrollment and the provision of benefits in TRI-CARE, the special health care program for military dependents.[REF]
There are two notable exceptions to the phasing out of existing government programs: the Veterans Administration Health Program and the Indian Health Service.[REF] Both, incidentally, are classic single-payer health systems, and both have a troubled record of performance.[REF]
-
Compulsory taxpayer funding of abortion. Under most federal health programs, there is usually a statutory restriction on the use of federal taxpayer funds for abortion. In the case of the Medicaid program, for example, the Hyde Amendment only allows abortion in the case of rape, incest, or the protection of the life of the mother.
It has long been the considered judgment of Congress that American tax dollars should not be used to pay for abortions. With the enactment of the Affordable Care Act (ACA) in 2010, the Obama Administration weakened and breached the traditional wall of separation between abortion and federal taxpayer funding. With the proposed Senate legislation, the wall would disappear entirely. Under the new government health plan, federal payments for all medical benefits and services would be drawn from a newly created federal trust fund. The proposed centralized control of health care financing effectively repeals the Hyde Amendment. Title VII, Section 701 of the bill declares, “Any other provision of law in effect on the date of enactment of this Act restricting the use of federal funds for any reproductive health service shall not apply to the monies in the Trust Fund.”[REF] As Ilsye Hogue, President of NARAL Pro-Choice America, declared enthusiastically, “Senator Sanders’ healthcare bill ends the debate and makes clear that reproductive healthcare, including abortion services, is a fundamental right—not just a privilege of the wealthy.”[REF]
-
Centralization of power. The proposed Senate bill is profoundly authoritarian. A major consequence of Obamacare was the transfer of a vast field of regulatory power over health insurance from the states to the federal government. The primary decision maker in the complex system created under the ACA was, of course, the Secretary of HHS. The bill would allow a limited right of private contracting between doctors and patients, but the language would impose a draconian restriction on physicians who engaged in such a contract: the inability to treat and receive payment for all other patients (meaning those enrolled in the government plan) for a full year.
Given that virtually the entire American population would be subject to the government plan, the bill would greatly expand the scope of the Secretary’s power. The language is very broad: “The Secretary shall develop policies, procedures, guidelines and requirements to carry out the Act.”[REF] The specified areas for the Secretary’s administrative actions include: standards for plan enrollment, health benefits, eligibility for benefits, insurance premiums and cost sharing, medical practice guidelines and rules for provider participation, levels of funding, methods for determining payment, coverage determinations, determination of medical necessity and appropriateness of procedures, planning for capital expenditures and professional education funding, actions to encourage states to develop “regional planning mechanisms” and “any other regulation necessary to carry out the purpose of this Act.”[REF]
Senator Sanders insists that such centralization, modeled on the traditional Medicare program, would reduce administrative costs.[REF] The Senator also claims that it would simplify the American health care system.[REF] In fact, such centralization is almost certain to generate even greater bureaucratic complexity, economic inefficiency, more intense politicization of health care decision making in Congress, and the same kind of organizational sluggishness that has long burdened the Medicare program. As Dana Goldman, a senior fellow at the Brookings Institution and professor of economics at the University of Southern California, observes:
People also forget that Medicare is a hidebound system. It took Congress more than 40 years to offer a prescription drug benefit, for example. Physicians are paid using an arcane system developed decades ago and that has now ballooned to more than 140,000 procedure codes, all of which is supervised (and gamed) by physicians themselves. Standard private sector cost saving measures, like competitive bidding for routine services, are rarely used.[REF]
-
Large and unknown costs. The Senate bill provides no financing provisions, and, of course, no Congressional Budget Office (CBO) score.[REF] This is a curious omission, as both health care spending and costs are the most important, if not the most urgent, issues in the nation’s ongoing health care debate. Compared to current and projected future costs, it is routine for single-payer advocates to insist that the new program would be more economically efficient and usher in an era of unprecedented health care savings. It is worth noting, however, that in the area of health care costs, the experience, beginning with Medicare itself, has been that the real costs of government health programs almost invariably exceed, often far exceed, their initial projected costs.[REF]
History is likely to repeat itself. Jodi Liu, a research analyst with the Rand Corporation, doubts that the Senate bill would necessarily result in savings over the status quo, and further warns: “The spending required for a single payer system depends on the price of care and services used. When health care is free, people tend to use more health care services, some of which is beneficial and some is not. Under Sanders’ Medicare for All plan, the use of health care services would almost certainly increase.”[REF]
Independent analyses of a 2016 version of the Sanders proposal indicated that the real costs of the proposal would far exceed the initial projections. For example, Kenneth Thorpe, a professor of health economics at Emory University, projected the 10-year costs at $24.7 trillion. Likewise, scholars at the Urban Institute, a liberal leaning think tank, estimated that the government health plan would cost $32 trillion over 10 years.
Meanwhile, as noted, neither the CBO nor independent analysts have completed the tax and spending estimates for the most recent version of Senator Sanders’ bill. The costs and the taxes to sustain it are doubtless going to be very large. For perspective, consider that the federal government spent a total of $3.9 trillion in 2016. According to the Urban Institute estimates, Senator Sanders’ government health plan would require a stunning $3.2 trillion in spending annually, while Professor Thorpe’s analysis indicates that the yearly cost of the program would amount to $2.6 trillion.[REF]
Polling on Senator Sanders’ concept has been generally positive. The political viability of the proposal, however, depends on public acceptance of the necessary trade-offs, especially its additional costs to the taxpayer. In this context, it is worth noting that the T. H. Chan School of Public Health at Harvard University and Politico recently conducted an in-depth survey of American voters on the topic. These researchers found that Americans are generally favorable to replacing the current insurance arrangement with a taxpayer-funded “Medicare-like” plan by a stunning margin of 66 percent, reflecting the popularity of the Medicare program itself. The Harvard–Politico survey, however, required respondents to consider the desirability of key policy options by clarifying the necessary or likely trade-offs that must accompany these public choices. Thus, they found that support for the “Medicare-like” plan proposal drops to 44 percent if adopting it meant that their “own taxes” would increase. When the pollsters describe the national health insurance program as a “single-payer” health plan, combined with the tax increases imposed on respondents necessary to sustain it, popular support for the proposal falls from 45 percent to 31 percent.[REF]
The Next Debate. American health care is a huge sector of the economy, where roughly half of all health care spending is government spending. Senator Sanders’ bill would expand that government payment to close to 100 percent. Current arrangements are governed by a diverse set of third-party payment arrangements in both the public and the private sectors, including employer-sponsored health insurance. The Sanders bill would simplify coverage by consolidating third-party payment in the federal government and by outlawing almost all private insurance, including the employment-based insurance that covers the vast majority of Americans under the age of 65.
Current government regulation and an inequitable and inefficient federal tax treatment of health insurance distort current private health insurance arrangements. Senator Sanders’ bill would solve that problem by consolidating regulation in the hands of the Secretary of HHS and abolishing all private insurance—logically eliminating all of the federal and state tax breaks that offset its cost. The result would be a large influx of additional tax revenue into federal coffers to fund the new government plan, along with the fresh federal revenues from a new set of heavy federal taxes on employers, individuals, and citizens’ investment income.
Current payment for doctors, hospitals, and medical professionals is based on multiple billing from private insurers and federal and state government programs. Senator Sanders would eliminate these multiple billings and establish a universal provider payment system directly based on an updated version of Medicare’s complex payment formulas. Such changes would guarantee cuts to providers’ revenues, and end provider cost-shifting to the private sector—because there would be no more private-sector plans. At the same time, the establishment of the federal government as the sole payer would virtually eliminate physician and hospital “market power” in negotiation with private payers because those private payers would no longer exist as parties to any such market negotiation.
Today, consumers and patients operate in a complex and bureaucratic mixed health care economy with distorted markets variously plagued by perverse economic incentives. Senator Sanders’ bill would eliminate that problem by eliminating market incentives altogether. Government would decide which plans, benefits, and medical procedures patients receive. Government would control the health care dollars, and, in so doing, would control the nature and scope of personal health care decisions. In such a world, personal choice, personal wants, or personal preferences would be ultimately irrelevant. Personal freedom in health care would itself be irrelevant.
Establishing the Universal System
Title I, Section 102 of the Senate bill sets out a declaration of universal entitlement: “Every individual who is a resident of the United States is entitled to benefits for health care services under this Act. The Secretary shall promulgate a rule that provides criteria for determining residency for eligibility purposes under this Act.”[REF]
The provision is remarkable since it defines “residency” rather than “citizenship” as a condition for eligibility to the new federal entitlement, and reserves to the Secretary of HHS, rather than Congress, the plenary authority to define that eligibility in regulation rather than legislation. The bill further authorizes the Secretary of HHS to establish a process of automatic enrollment for all persons at “the time of birth in the United States and at the time of immigration into the United States or other acquisition of qualified resident status in the United States.”[REF] The federal government would provide every resident with a “Universal Medicare Card” for processing claims. Curiously, the language reads: “The card shall not include an individual’s Social Security number.”[REF] In short, the bill would cover illegal aliens.
The Senate bill would also enact a broad non-discrimination provision: “No person shall, on the basis of race, color, national origin, age, disability, or sex, including sex stereotyping, gender identity, sexual orientation and pregnancy and related medical conditions (including termination of pregnancy), be excluded from participation in, be denied the benefits of, or be subjected to discrimination by any participating provider as defined in section 301, or any entity conducting, administering, or funding a health program or activity, including contracts of insurance, pursuant to this Act.”[REF]

The bill language is similar to that embodied in Section 1557 of the ACA, which had generated a regulatory scheme that undermines conscience protections in health care delivery.[REF] The bill’s language, however, is broader and more direct.[REF] It provides HHS with broad authority to change or modify the national benefits package. In the absence of conscience protections—combined with a reigning assumption that federal officials’ “government-approved” morality automatically trumps the moral, ethical, or religious convictions of physicians and patients- the provision invites even greater cultural and political polarization. It is reasonable to assume that the government health plan could require medical professionals to participate in a number of practices to which they would have profound moral or religious objections, including abortion, the provision of abortifacients, gender-reassignment surgeries, and even physician-assisted suicide, which is being aggressively promoted as an appropriate approach to end-of-life care.[REF] As with Section 1557, a broad interpretation of the language, either through regulation or adjudication, could expand the meaning of disability, for example, to include medical conditions and thus additional mandatory treatments.[REF]
The bill also authorizes the Secretary of HHS to establish “a procedure for adjudication of administrative complaints” alleging a violation of this non-discrimination clause. It also provides a cause of action in federal courts for persons claiming discrimination based on this provision to get “compensatory and punitive damages, declaratory relief, injunctive relief, attorneys’ fees and costs, or other relief as appears appropriate.”[REF] The provision is likely to generate a flood of litigation, particularly suits against religiously affiliated doctors and hospitals or medical institutions.
Benefits. Under the bill, the government health plan would provide medical benefits and services, effective on January 1 of the fourth calendar year after its enactment.[REF] At that time, the government would literally outlaw any private health insurer or any employer that provides health insurance benefits that “duplicate” any of the benefits that are authorized in the federal government’s comprehensive health plan.[REF]
On a “regular basis,” the Secretary of HHS can change (“improve or adjust”) the government health benefits package in response to changes or developments in “health science” and make recommendations to Congress.[REF] Congress, in other words, would retain the ultimate authority over which medical benefits or services are to be available to Americans, and which benefits and services will not be available to them in the government health plan.[REF] States, however, may provide “additional” benefits for their own citizens, at their own citizens’ expense.
Medical benefits are to be tightly controlled. In general, according to the Senate bill, “benefits” for services are not available under the act unless the services meet the standards in Section 201(a), as defined by the Secretary.”[REF] (Emphasis added.) The Secretary of HHS “shall” make coverage decisions with experimental services, and patients can appeal those coverage decisions based on a process that shall, “as much as is feasible,” follow the current Medicare appeals process.[REF]
Government benefit setting is political process. It is also worth noting, in this context, that government benefit setting, based on the 50 years of experience, will surely replicate the intense and frenzied lobbying that characterizes the provision of new benefits or changes in the Medicare program. Congress is often beholden to the “Medicare industrial complex” of powerful provider and other medical groups, and Medicare today is a big arena for special interest group lobbying.[REF] Meanwhile, Medicare’s benefits and services often lag behind the provision of benefits and services in the private sector. Moreover, in the adjudication of claims for benefits or services coverage, the current Medicare program has a record of being more stringent than the private sector, and the appeals process in Medicare is complex, cumbersome, and painfully time consuming.[REF]
No Cost Sharing. The bill provides that government plans’ medical benefits and services will be “free” at the point of service. It thus forbids any “cost sharing,” such as the payment of deductibles, copayments, or coinsurance.[REF] Cost sharing for prescription drugs and “biological products” would be the major exception. For these categories of medical services, cost sharing would be permitted for the government plan’s drug benefits as long as the use of the drug is “evidence-based,” encourages generic substitution, does not apply to “preventive drugs,” and the amount is limited to $200 per person annually (adjusted for inflation).[REF] The government would also forbid doctors (or other medical professionals) to charge patients any amount above the set government payment for medical benefits and services.[REF] In short, no “balance billing.”
There is, of course, an inverse relationship between premium price and program costs and the level of cost sharing in health insurance. The higher the cost sharing, the lower the premium and program costs. In light of current practice in the traditional Medicare program, the bill’s restriction on cost sharing is a radical departure from traditional Medicare, which, in fact, imposes an array of cost-sharing requirements on benefits and services in order to dampen excess utilization and control both program and beneficiary costs. Without such cost sharing, the premium costs would be higher for both patients and taxpayers. Economists generally conclude that the existing Medigap and other supplemental coverage arrangements in the Medicare program that eliminate patient cost sharing at the point of service have contributed to significant increases in both beneficiary costs and overall Medicare program costs.[REF] The Sanders bill would also generate higher health care costs.
In the new government health plan, medical professionals would be subject to government medical-practice guidelines. Over the past five decades, federal law and regulation has progressively weakened the professional independence of Medicare physicians. Remarkably, the bill is a bold and explicit rejection of Medicare’s original statutory prohibition of government interference in the practice of medicine: “Nothing in this Title shall be construed to authorize any federal officer or employee to exercise any supervision or control over the practice of medicine or the manner in which medical services are provided.[REF]
The guideline language includes a proviso that any deviation from a practice guideline would be considered within the guideline if the medical professional deviating from it did so with “appropriate professional discretion.”[REF] Because the Senate bill is silent on the topic of medical liability or tort reform, it is unclear what impact federal medical practice guidelines will have in either encouraging or discouraging litigation. In any case, attempts to adjudicate thorny disputes in such matters will entail some complex and difficult administrative and judicial proceedings.
Long-Term Care. Beyond the provision of acute care benefits and services, the bill would also provide for expanded coverage under a revamped Medicaid program for 13 long-term-care services and supports, ranging from nursing home care and intermediate care, to home-based and community services and self-directed personal assistance services.[REF]
In financing long-term care, the federal government would make Medicaid payment to the states as long as the states do not adopt eligibility standards that are more restrictive than those in force as of May 5, 2017.[REF] Payment to the states would be based on an “expenditure floor,” and indexed annually by the Medical Consumer Price Index (M-CPI). The basic level of state spending, or the “expenditure floor,” in turn would be based on the state long-term-care spending for fiscal year 2017. This level of spending would be adjusted by a growth formula that would include the percentage increase in a state’s overall health care costs, long-term-care spending in the previous year, population increase, and the increase in the population aged 65 and older. In receiving the federal payment, the states cannot, in any way, restrict eligibility for long-term care services and supports, but the states may set “additional standards” for eligibility, benefits, and providers “consistent with the purposes” of the act.
Doctors and Medical Professionals. Under Title III, the Senate bill sets forth the terms and conditions of provider participation. No American doctor or other medical professional would be legally authorized to provide medical benefits or services under the act without entering into a “participation agreement” with the Secretary of HHS. In turn, the Secretary is to require any physician or professional participating in the government health plan to furnish services in accord with the aforementioned “non-discrimination” clause of the bill (Section 104), refrain from charging patients any more than the government payment specified for the service, and agree to abide by the Secretary’s request for information and reporting requirement, as well as cooperate with quality reviews and record-keeping requirements.[REF]
Physicians and other medical professionals can remain in good standing with the federal government if they comply with the federal regulations and the various standards prescribed by the Secretary, and they will enjoy the government’s protection if they testify in any proceeding or report to the authorities any violation of any of the provisions of the Act.[REF]
Private Contracting Restrictions. The Senate bill also provides a limited right of private contracting with patients outside the government program. This right of contract is broadly similar to the right of private contracting between doctors and patients permitted in the current Medicare program. Specifically, a doctor or other medical professional may enter into a private contract with a patient if they provide advanced notice to the patient that they will not submit a claim to the government for the service, sign an affidavit that they have entered into a private contract with the patient, submit the affidavit to the Secretary of HHS within 10 days, and refrain from providing medical services for government reimbursement to all other patients eligible for government health services for a period of one year.[REF]
This restriction on the right of doctors and patients to contract with each other privately is similar to the current restrictions in the Medicare program. Under the current Medicare law, doctors and patients who enter into a private agreement with each other, for reasons of patient privacy or any other reason that they deem appropriate, can do so. Under the Medicare statute, however, the doctor must “opt out” of the Medicare program and forego treating all other Medicare patients for a period of two full years.[REF] This unusual restriction on the doctor-patient relationship does not exist, of course, in any other American government health program, such as the FEHBP or even Medicaid. Ironically, such a restriction does not even exist in the British National Health Service, the quintessential single-payer system, where doctors freely practice in both the government program and the private sector. Throughout the 1990s, the Clinton Administration, however, was persistent in its efforts to expand federal control, and succeeded in getting the current restriction enacted through the notorious Balanced Budget Act of 1997. The law secured its intended effect: Voluntary, private agreements between doctors and patients within the Medicare program barely exist. Less than 1 percent of American physicians today “opt out” and enter into private contracts with Medicare patients.[REF] Under the Senate bill, the public can expect a similar outcome.
In real life, there are a number of legitimate reasons why patients would not want to submit a claim to a government agency to reimburse their medical treatments. It may be a strong desire for personalized medical care, a concern over the sensitivity of their medical condition, the higher quality of the personal care that they have received from a physician with whom they have enjoyed a long professional relationship, or simple privacy. While Medicare law and regulation, as well as private third-party payment contracts, have attenuated the traditional doctor-patient relationship, the Senate bill would largely complete the process, and would strongly discourage the viability of independent medical practice or the pursuit of personalized medical care.
Centralizing Federal Power
Today, the American health care sector of the economy is roughly $3.2 trillion. With the elimination of almost all private insurance and the elimination, consolidation, or transformation of almost all other federal government health programs, the Secretary of HHS, as noted, would be vested with vast administrative authority to develop “policies, procedures, guidelines and requirements” to implement the many provisions of this far-reaching legislation. With the adoption of the Senate bill, federal regulatory power would pervade virtually every aspect of the financing, organization, and delivery of medical care in a sector of the American economy larger than the GDP of France.
Data Collection. The task will require a herculean effort in central economic planning. Central planning requires the collection and organization of vast amounts of information to inform and guide regulatory initiatives. Under the bill, the Secretary of HHS would be required to create a national database. This database is to contain information on the performance of medical professionals, the costs of benefits, services, and facilities, and the quality and outcomes of the medical services being delivered by the government health plan and its contractors.[REF] This information is to be made available to federal officials, health care providers, analysts, economists, researchers, and scholars without “compromising patient privacy.”
The Secretary of HHS is required to submit an annual report to Congress on the implementation of the act, outlining the progress and the problems that it encountered in its enforcement. The bill further requires the Secretary to report on more than a dozen specific areas, ranging from enrollment and health care spending to progress in reducing ethnic and racial disparities and quality improvements. The bill also authorizes the Secretary to consult or contract with experts and conduct empirical analyses and research on health-related topics, including health care payment and delivery methods and the standards required for “evidence-based” policymaking.[REF]
Waste and Fraud. The bill requires the HHS Secretary to appoint a “Beneficiary Ombudsman” to process complaints from beneficiaries and address patient grievances, as well as identify problems in the government health plan, particularly in relation to coverage or payment policies. The bill further provides for application of the current law’s provisions to combat waste, fraud, and abuse, including the existing sanctions against guilty providers, such as the exclusion of providers from the program, the imposition of civil and monetary penalties, and the provisions that require medical professionals to disclose their ownership of medical facilities.[REF]
Medicare and Medicaid are plagued annually with tens of billions of dollars in losses from waste, fraud, and abuse. In 2015 alone, Medicaid’s improper payments amounted to $30 billion.[REF] In Medicare, improper payments reached $43.3 billion that same year.[REF] Private plans seem much better at policing and arresting these problems that are seemingly intractable in the public sector. In any event, the Sanders legislation is prescribing largely the same remedies for the same problems that have burdened Medicare and Medicaid for decades. Taxpayers can expect, given the sheer scope of the problem and the attendant costs, that under the new government health plan the losses will only substantially increase, not decrease, under the terms and conditions of the bill.
Global Budget. The HHS Secretary “shall establish” an annual “national health budget” no later than September 1 of each year. The national budget will account for the “total expenditures” for medical benefits and services provided under the government health plan. Among its categories, the budget will also outline spending for health-quality assessment, the education expenditures for health professionals, the administrative costs of the program, operating and capital expenditures related to the plan, and prevention and public health activities.[REF]
For a five-year period, beginning with the first-year implementation of the new law, the bill specifies that 1 percent of the national health budget is to be allocated for “worker assistance” for persons who lost employment because of the elimination or dislocation of existing commercial insurance arrangements, such as the elimination of private insurance plans in the individual market and those firms marketing or administering employer-based health insurance.[REF]
With an administrative payment system, as envisioned in the bill, there are ample mechanisms to ratchet down provider payments to meet spending targets set by a national health budget. The tougher challenge will be political. With the adoption of a national health budget—setting a fixed amount of dollars for health care—the key question is whether or not any Congress will really adhere to the budget. If the demand for medical services is higher than the government officials anticipated, they will face intense pressure to discard the budgetary constraints and simply increase the health care spending. In that case, the budget is meaningless.[REF] If government officials stand firm by the budget they created, in the face of rising demand, there will be a denial of access to medical services, or a more-or-less sophisticated form of government rationing, where federal officials will determine which patients receive care, when they receive it, and under which conditions they receive it.
Provider Payment. The HHS Secretary is required to establish, through regulation, fee schedules for doctors, hospitals, and other medical professionals that are consistent with Medicare payment rules and recent rules established under the Medicare Access and CHIP Reauthorization Act of 2015 as well as those under Obamacare.[REF]
The Medicare physician payment system, which sets the dollar amounts for roughly 8,000 medical services, is an administrative payment system. A complex set of formulas determine and update the annual amounts of physician payment. At the heart of this system is the resource-based relative value scale (RBRVS). With the support of the first Bush Administration, Congress enacted the Medicare RBRVS into law as part of the Omnibus Reconciliation Act of 1989. Under the RBRVS, the “value” of a physician service is equal to the resources required to deliver it. The determination of economic “value” in this case is not subject to the free-market forces of supply and demand, where consumers judge the relative value of the different commodities, goods, and services through market transactions. Instead, government officials or their agents determine, for this purpose, economic value “objectively.” They accomplish this feat through a social science measurement of the various resources that go into providing a particular medical service, including the time, labor, or level of effort, as well as practice and malpractice costs that are appropriate to the service, adjusted for geographic costs. On a regular basis, special committees of medical professionals, acting on behalf of the federal government, meet to evaluate and determine the “relative values” of medical services.
The Senate bill would also require the Secretary of HHS to establish a “standardized process” to review the “relative values” of physicians’ services, and to consult the “stakeholders” in this process. The Secretary is further required to present a “written plan” to Congress each fiscal year on physician services, the “relative value” of these services, and the rationale used for the determination of the “values” of these services. The bill’s sponsors evidently believe in the 19th-century economic theory that the value of goods and services is “objective,” based on labor or other resource inputs, beyond the perceived benefit or value to a consumer. It is quite the opposite of modern economics, which holds that the economic value of goods or services is subjective, reflecting consumer demand. Of course, in a market, suppliers of goods and services try to satisfy the personal wants, needs, or preferences. In such a large bureaucratic system, as proposed by the bill, the personal wants, needs, or preferences of individuals are usually shortchanged if not altogether irrelevant.
For compensating medical professionals, or any other class of professionals, this is a profoundly flawed approach to reimbursement; such a top-down, supply-driven process does not, as noted, account for value or benefit to the patient.[REF] The Senate bill requires that payments for drugs, medical devices, and medical equipment be “negotiated” between the manufacturers and the government annually. In the case of drugs, the Secretary would be required to establish a national drug formulary, a list of approved drugs that are to be reimbursed under the government health plan. In establishing this national formulary, the Secretary “shall promote the use of generic medications to the greatest extent possible.”
New Federal Trust Fund. The bill would create a “Universal Medicare Trust Fund” for all federal monies deposited or appropriated to, or transferred from, the general fund in the Treasury, as well as any “gifts and bequests.” The bill automatically appropriates monies to the Trust Fund for each fiscal year beginning on the date on which benefits first become available.[REF] In other words, like the Medicare program, the funding for the new government health plan is a permanent, indefinite appropriation, meaning that it is mandatory entitlement spending, not subject to the annual appropriations process of Congress.
In the case of existing government health programs, the bill states, “Notwithstanding any other provision of law, there are hereby appropriated to the Trust Fund for each fiscal year, beginning with the first fiscal year beginning on or after the effective date of benefits under Section 106, the amounts that would have otherwise have been appropriated to carry out the following programs.”[REF] Included in this sweeping, automatic rechanneling of appropriated funds are amounts that would have otherwise gone to fund Medicare, Medicaid, the FEHBP, TRICARE, the federal maternal child and health program, a number of Public Health Service programs, and “any other Federal program identified by the Secretary, in consultation with the Secretary of the Treasury, to the extent the programs provide for payment for health services the payment of which may be made under this Act.”[REF] As noted, the bill would provide for the transfer of funds in the existing Medicare trust fund into the new Universal Medicare Trust Fund.
Transitioning Out of the Status Quo
During the four-year period between the enactment of the legislation and its full implementation, the legislation makes a number of major changes to existing federal government health programs. As a general matter, these changes would both increase the benefits offered through these temporary programs and consolidate the federal government’s delivery of medical benefits and services.
Medicare. The Sanders bill would progressively lower the age of Medicare eligibility. The eligibility standard would include U.S. residency, including legal alien status and citizenship, or a person not otherwise eligible to benefits under Parts A and B of Medicare.
In the first year of the transition, the existing Medicare program would be open to all persons who have reached the age of 55; the second year, all those who reached the age of 45; and the third year, all of those who reached the age of 35. The Secretary would establish an enrollment period for these new Medicare enrollees, and the Secretary is required to determine their premiums. In determining the annual premiums for the new enrollees, the Secretary is to calculate the amount based on the “average per capita amount for benefits and administrative expenses” that would be payable under Parts A, B, and D, and, as applicable, Part C, for the newly enrolled persons.[REF] Persons enrolling in Parts C and D, where private plans would offer benefits, would be responsible, as they are today, for paying any additional premium amounts for these benefits.
For the transition period, the bill makes a number of other Medicare policy changes. For Medigap coverage, the supplemental private insurance that covers benefits and costs not covered or reimbursed by traditional Medicare, the bill would require Medigap insurers to offer their policies on a guaranteed-issue basis for newly enrolled individuals, meaning that they must enroll newly insured persons without underwriting or evidence of insurability.[REF]
With regard to traditional Medicare, the bill eliminates deductibles in Part A (the part of the program that pays hospitals) and Part B (the part of the program that reimburses physicians and outpatient medical services). While eliminating the Medicare deductibles, the bill also provides for annual catastrophic coverage for Medicare beneficiaries, which is the biggest coverage gap in the traditional Medicare program. In this instance, catastrophic protection would kick in after a person’s annual out-of-pocket expenses, such as coinsurance and copayment, reached $1,500.[REF] This is a relatively low threshold, and would increase taxpayer obligations. The maximum out-of-pocket limit currently required in Medicare Advantage (MA) is $6,700 annually, though most competing MA plans have annual limits of between $3,000 and $4,000.[REF]
Regarding the Medicare drug program, the Senate bill would reduce beneficiaries’ annual out-of-pocket threshold to $305, and would eliminate all beneficiary cost sharing above that threshold.[REF] The bill would also enhance the benefit package of traditional Medicare by adding coverage for dental and vision services, hearing aids, and examinations to Part B coverage.[REF] Finally, the bill would eliminate the current two-year waiting period for Medicare coverage for eligible disabled persons.[REF]
A Public Option. The Senate bill would create a “Medicare Transition Plan” that would compete with private health plans in the Obamacare health insurance exchanges throughout the nation.[REF] This is the public option. The transitional plan would comply with all of the Obamacare insurance requirements necessary to be a “qualified health plan” under current law, benefits would have a 90 percent actuarial value, and enrollment would be open to any U.S. “resident.”
Payment to doctors, hospitals, and other medical professionals would be set at Medicare fee for service rates, and payment for prescription drugs under the plan would be subject to government “negotiation.” If the administrator of the Centers for Medicare and Medicaid Services (CMS) and the drug manufacturers are unable to come to an agreement, the administrator “shall” establish a payment rate that is the lesser of drug payments under the Veterans Administration program or the drug payments for the Department of Defense and state Medicaid programs.[REF]
Physicians and other medical professionals participating in the Medicare or Medicaid programs would be required to participate as “providers” in the Medicare Transition Plan: “A health care provider that is a participating provider of services or supplier under the Medicare program under Title XVIII of the Social Security Act (42 U.S.C. 1395, et seq.) or under a State Medicaid plan under Title XIX of Such Act (42 U.S.C. 1396, et seq.) on the date of the enactment of this Act shall be a participating provider in the Medicare Transition plan.”[REF] (Emphasis added.) For the vast majority of American physicians, this provision would amount to government conscription.
The current income cap of 400 percent of the federal poverty level (FPL) for eligibility for Obamacare premium tax credits would be lifted for those enrolling in the transitional plan. The CMS administrator would determine the premium amounts for plan enrollees, and these amounts “may vary” based on family or individual coverage, age, and tobacco status, but not the “rating area”; the administrator must also take into consideration the cost-sharing reductions and premium tax credits available.[REF]
The bill also provides for special premium tax credits for the public plan for low-income persons in states that did not expand their Medicaid coverage. Premium tax credits for enrollees in the public option would be available for all those below 100 percent of the FPL.[REF] The premium tax credit would be re-adjusted so that those with annual incomes below 100 percent of the FPL would pay no more than 2 percent of their household income in premium, and those with an income at 150 percent of the FPL would pay no more than 5 percent.[REF] The bill also authorizes the HHS Secretary to set new cost-sharing rules for these enrollees.
Senator Sanders’ bill thus delivers on a major Obama Administration policy objective that was scuttled during the Obamacare debate in 2010: a “robust public option”—a government health plan—that would compete against private health plans in the national health law’s insurance exchanges throughout the nation. Proponents have long argued that a “public option” would enhance market competition and, among other things, keep private insurers “honest.” The initial 2009 legislative version of what would eventually emerge as the Affordable Care Act, the House Tri-Committee bill, included a public option and provided it with special advantages, such as artificially low provider payment rates based on the Medicare payment system and a shift of financial risk to the taxpayers.[REF] The Sanders’ bill, with special rules for the transition plan, provides that advantage. In fact, the original proponents of the public-option strategy made it quite clear that the purpose of the proposal was to undercut private health plans, drive them out of the market, and create a single-payer system in the process. The Sanders’ proposal would thus accelerate the transition to the universal government health plan.
A Large and Expensive Program
As noted, the Senate bill contains no provisions for financing the new government health program. The CBO has not yet provided a tax and budget score of the legislation. Nonetheless, Senator Sanders has provided a list of “options”—new federal taxes—to finance the new government health plan along with 10-year revenue estimates.[REF] The new federal taxes would serve the dual function of funding the new government health plan and furthering a greater government redistribution of Americans’ income.
Taxing the Middle Class. Senator Sanders’ tax proposals, or some combination of them, would be the financial foundation of this program. They include a 7.5 percent income-based premium paid by employers (estimated to raise $3.9 trillion); a 4 percent income-based premium paid by all households (estimated to raise $3.5 trillion); new revenues from the abolition of existing federal tax breaks for insurance—tax expenditures—especially the federal tax exclusion for employment-sponsored insurance (estimated to raise $4.2 trillion).[REF]
Taxing the Rich. Senator Sanders has also suggested new taxes on upper-income Americans, including a set of progressively higher marginal tax rates. For example, for Americans with annual incomes of between $250,000 and $499,000, there would be a marginal income tax rate of 40 percent. For Americans with an annual income of between $500,000 and $2 million, the rate would increase to 45 percent. For those at the very top of the income scale, making more than $10 million, the marginal income tax rate would climb to 52 percent ($1.8 trillion). There would also be a special wealth tax on approximately 160,000 households with the highest incomes ($1.3 trillion).[REF]
For Americans with a household income above $250,000 annually, Senator Sanders has suggested an end to special tax breaks for capital gains and dividends, and has called for capping itemized deductions at 28 percent. He has also suggested closing certain business “loopholes” for those who run an S-Corporation—a small business.
Senator Sanders has also suggested an increase of the estate tax—replacing the existing 40 percent estate tax rate with a progressive tax rate ranging from 45 percent to 55 percent, depending on the value of the estate, with an additional 10 percent surtax on estates’ value in excess of $500 million for single individuals and $1 billion for married couples.[REF]
For those who run corporations, Senator Sanders has suggested a one-time tax on offshore profits ($767 billion), a new fee on large financial institutions ($117 billion), and the repeal of miscellaneous “corporate accounting gimmicks” ($112 billion).[REF]
Previous Independent Estimates. In 2016, independent analysts, operating with different assumptions and models, examined an earlier version of the Medicare for All Act. The bill’s financing was broadly similar to, but less robust than, the 2017 version: an employer payroll tax of 6.2 percent; an income-related premium tax of 2.2 percent for all households; the elimination of existing tax expenditures; and a series of new taxes on wealthy citizens, including increased marginal tax rates, taxes on capital gains and dividends, increased estate taxes, and new corporate taxes. Senator Sanders estimated new spending of the proposal at $13.8 trillion from 2017 to 2026.
Dr. Kenneth Thorpe, a professor at Emory University and a former health policy advisor to President Bill Clinton, basing initial estimates on the 2016 version, found that the real cost of the Sanders proposal was indeed much higher: $24.7 trillion over the period 2016 to 2024. The annual cost of the plan, according to Professor Thorpe, would be $2.5 trillion per year, creating “an average of over $1 trillion per year financing shortfall.”[REF] Because the true cost of the Sanders plan would be much higher, the funding requirements would also be much steeper. In his analysis of the plan, Thorpe concluded that the combined employer payroll and income taxes would have to increase from 8.4 percent to 20 percent. Specifically, the employer-based payroll tax would have to increase from 6.2 percent to 14.3 percent, and the income-related premium tax would have to increase from 2.2 percent to 5.7 percent: “Overall,” Thorpe concluded, “over 70 percent of the working privately-insured households would pay more under a fully funded single payer plan than they do for health insurance today.”[REF]
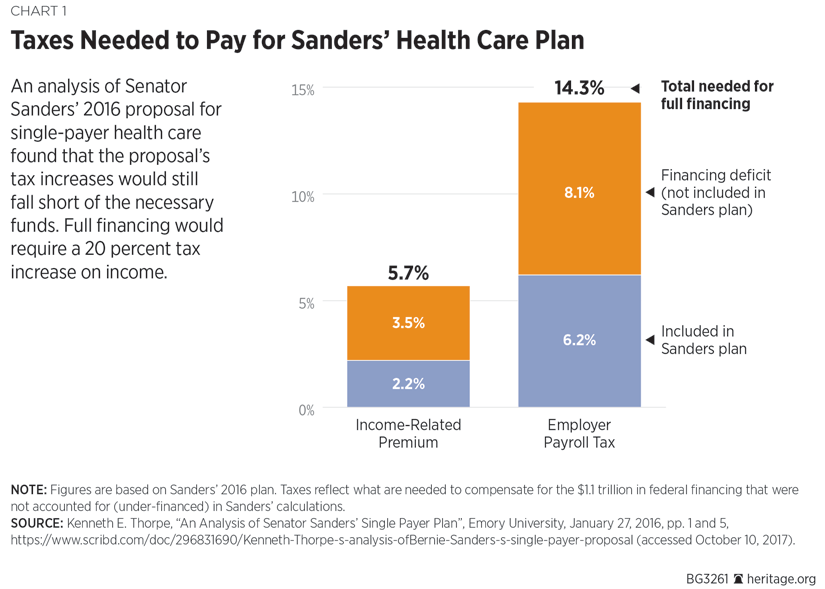
Thorpe noted that the 2016 Sanders plan would have some unpleasant distributional impacts on certain low-income populations, not just the “rich.” For example:
Medicare beneficiaries would no longer pay premiums and face no cost-sharing but would pay higher taxes. In general, small businesses that do not offer insurance today with 50 or fewer workers would face a 6.2 percent payroll tax increase. Low income populations living in poverty receiving Medicaid would pay more through the 2.2 percent income tax and the 6.2 percent reduction in wages.[REF]
Scholars at the Urban Institute, a prominent liberal-leaning think tank based in Washington, also conducted an analysis of the 2016 Sanders plan. It estimated that the total federal cost would amount to $32 trillion from 2017 to 2026.[REF] According to the Urban Institute analysts,
The increase in federal spending is so large because the federal government would absorb a substantial amount of current spending by state and local governments, employers and households. In addition, federal spending would be needed for newly covered individuals, expanded benefits and the elimination of cost-sharing for those insured under current law, and the new long-term support and services program.[REF]
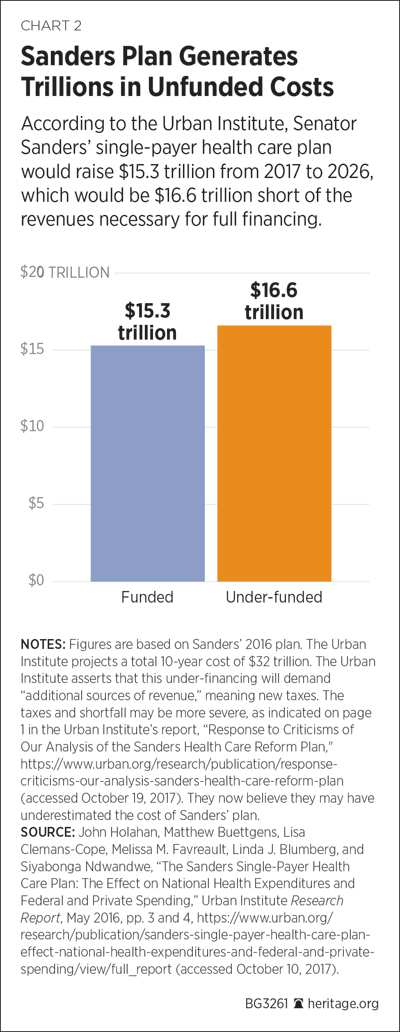
Like Thorpe, the Urban Institute analysts estimated that the true costs of the Sanders proposal would outrun the projected revenues. They estimated that from 2017 to 2026, the taxes to finance the government health plan would raise $15.3 trillion in revenue. This, the Urban Institute analysts concluded, would be “approximately $16.6 trillion less than the increased federal cost of his health plan estimated here. The discrepancy suggests that to fully finance the Sanders approach, additional sources of revenue would have to be identified; that is, the proposed taxes are much too low to fully finance the plan.”[REF]
Conclusion
The ongoing national health care debate is not simply a dispute over health care costs, access, or quality. Virtually all Americans, as well as their elected representatives, agree that there should be a dramatic expansion of health insurance coverage. They also generally believe that government should assist, in some way, those who are poor and sick. They favor policies that would restrain the growth in health care costs, or preferably reduce them. They also support policies that would improve the quality of care that Americans get from doctors, hospitals, and health plans and programs, especially public programs.
A fundamental conflict of visions is, however, at the heart of this debate. There are those for whom the provision of health care services should be a public responsibility and a federal entitlement. There are others for whom health care should be a matter of personal responsibility, and the choice of health care services should be an exercise of personal freedom. In that sense, the current debate is not just a health policy debate, but rather a quintessentially political debate over power and control. For some, government should have the power to make the key decisions in the system, and government should control the flow of health care dollars. For others, individuals and families should have the power to make the key health care decisions, and individuals and families should control the flow of health care dollars.
Americans today are struggling in a complex system that does not fully reflect either vision, though, it is clear, that the role of the federal government has greatly increased with the enactment and implementation of Obamacare, where the federal government is now exercising plenary regulatory power over the nation’s individual and small-group health insurance markets. This attempt at centralized federal regulation has proven to be a costly and painful experiment for middle-class Americans trapped in these severely damaged markets without the generous taxpayer subsidies that insulate low-income persons from the ugly reality of rapidly rising health care costs. Middle-class Americans in these markets face skyrocketing premiums and explosive deductibles, narrower provider networks, and fewer choices of health plans and providers.
Senator Sanders and his Senate colleagues have performed a valuable service in sponsoring their comprehensive legislation. They have outlined in detailed legislative text what a government-managed health care system would look like. They have made it clear that it would function as a monopoly, and that it would outlaw almost all private insurance options, including the employer-sponsored coverage that most Americans today enjoy. They have guaranteed a very large increase in taxes, along with the creation of a powerful bureaucracy that will exercise direct and detailed control over health benefits, levels of coverage, health care payments, reimbursements, and even medical practice. They have also made it clear that the personal rights of conscience, relating to sensitive moral and ethical issues, will be violated routinely, and that taxpayers, regardless of their ethical objections, will be forced to finance the destruction of innocent, unborn human life.
Senator Sanders and his colleagues have outlined clearly their vision of the future of American health care. It is long past time that the President and his congressional allies clearly outline their own vision of the future of American health care—and fight for it.
—Robert E. Moffit, PhD, is a Senior Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.



