Mr. Chairman and Members of the committee, thank you for inviting me to testify. My name is Edmund F. Haislmaier and I am a Senior Research Fellow in Health Policy at The Heritage Foundation. The views I express in this testimony are my own, and should not be construed as representing any official position of The Heritage Foundation.
My testimony today will focus on the potential effects on market competition of three currently pending health insurance mergers, specifically: (1) Aetna’s acquisition of Humana; (2) Anthem’s acquisition of Cigna; and (3) Centene’s acquisition of Health Net.
To assess market competition in any industry one must begin by identifying the parameters of the relevant market or markets. In the case of health insurance, two key parameters are geographic presence and product line.
Geography is a relevant parameter for a couple reasons. First, because most medical services are purchased locally, the prices and quantities of those services, the size and distribution of the patient population, and the contractual arrangements of insurers and providers can all vary by location. Variations in those inputs affect the price of coverage and the extent of insurer competition available to consumers. Second, the regulation of insurance, including most anti-trust regulation, has historically been the responsibility of state governments.
Product line is also a relevant parameter because within the broader market for health insurance there exist discrete submarkets with different types of customers. Thus, the business strategy of any given insurer might range from targeting only a single subset of the broader market to seeking to serve multiple submarkets by offering a number of different product lines.
Consequently, applying these two parameters offers an appropriate framework for segmenting the broader market before analyzing the relevant data to evaluate competition within each subset.
I have limited my analysis to those submarkets for what is commonly known as “comprehensive” or “major medical” health insurance coverage—setting aside various so-called supplemental product lines, such as dental only or vision only coverage. My reasons for doing so were, first, that there is greater public interest in market competition with respect to comprehensive medical coverage, and second, that potential barriers to competition and market entry are much lower for supplemental products, and thus of rather less concern to both consumers and regulators.
I used enrollment, or the number of “covered lives,” as the basis for measuring market share. While various financial metrics are relevant to assessing whether a proposed merger is a wise business decision, those metrics would tell us little about the effects that the merger might have on the choices available to consumers.
Thus, for my analysis I used enrollment data taken from insurer regulatory filings for the end of 2014, distributed in a matrix consisting of five submarkets in each state. Those five market segments are: (1) individual coverage; (2) fully insured employer-group coverage; (3) Medicare Advantage plans; (4) self-insured employer-group plans for which insurers provide administrative services only; and (5) Medicaid managed care.
The first three submarkets—individual, fully insured group, and Medicare Advantage—are ones for which competition is most appropriately measured at the state level. Each one serves a distinct subset of customers, yet in all three markets the customers purchase coverage locally.
In contrast, the markets for self-insured group coverage and Medicaid managed care are more national in character and the customers—large employers and state governments—are more sophisticated purchasers.
The self-insured employer-coverage market consists primarily of large employers and such firms are not limited by geography when contracting with vendors to manage their plans. Indeed, a major reason that many large employers self-insure is that the arrangement enables them to offer a uniform plan to workers located in multiple states.
Similar to self-insured employer plans, Medicaid managed care typically takes the form of “bulk” contracts between state governments and insurers—though unlike self-insured employer plans, it is typically the insurer, not the plan sponsor, that bears most of the risk under a Medicaid managed-care contract. As with self-insured employer plans, there is no inherent geographic limitation to carriers bidding for Medicaid managed care contracts.
That said, while competition in these two segments may be national in scope from the customer perspective, these arrangements do affect the competitive dynamics with respect to medical providers at the state or local level. That is because insurance carriers must still contract with local providers to fulfill those contracts. Thus, as a practical matter, the extent of a given insurer’s provider contracting in a particular state will affect its ability to compete for the business of self-insured employers and state Medicaid agencies. Also, from the provider perspective, the total number of covered lives across all of a given insurer’s product lines can affect the relative bargaining positions of providers and insurers. In other words, it is possible for either competitive extreme to exist: a locally dominant provider system with near-monopolistic leverage over insurers, or a locally dominant insurer with near-monopsonistic leverage over providers.
With that as background, let me turn to offering specific data and comments about each of the three pending mergers.
Aetna’s Proposed Acquisition of Humana
Because Humana’s principle business line is Medicare Advantage plans—accounting for 40 percent of the company’s total enrollment nationwide—Aetna’s acquisition of Humana largely represents an expansion of Aetna’s presence in that submarket. Nationally, as of the end of 2014, Humana was the second largest Medicare Advantage carrier while Aetna was the fourth largest. Combining the two companies would position Aetna as the largest Medicare Advantage carrier, though it would still have less than 25 percent (24.6 percent) of the total national market for that product line.
Table 1 summarizes my analysis of the state-level effects of this proposed merger. In most states the consolidation effect on the Medicare Advantage market would be fairly modest. Even in states where one of the companies already has a substantial share of the market, combining the two would, in most cases, have the marginal effect of adding only a few percentage points of market share.
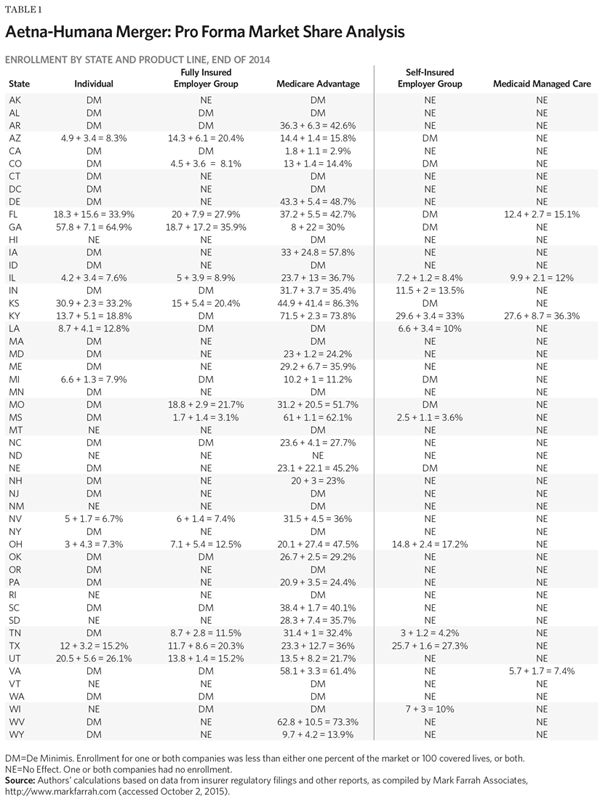
The exceptions are the handful of states where both carriers already have significant shares of the Medicare Advantage market. Most notably, in Kansas each company already has more than 40 percent of the Medicare Advantage market and the combined company would have an 86 percent share. In both Iowa and Missouri one company currently has more than 30 percent market share with the other having more than 20 percent, so that the combination would produce markets shares of almost 58 percent and 52 percent, respectively. Similarly, in both Ohio and Nebraska each company currently has more than 20 percent market share and the combination would produce market shares of 47 percent and 45 percent, respectively.
With respect to the other four market segments in this analysis, Table 1 shows that the state level consolidation effects would be modest, or even marginal, in almost all instances. The one notable exception is Georgia, where Humana already has 58 percent of the individual market—increasing to 65 percent under the proposed merger—and where the two companies each have about 18 percent of the fully insured employer-group market, yielding a post-merger 36 percent market share.
Anthem’s Proposed Acquisition of Cigna
Because Cigna’s principle business consists of providing administrative services for self-insured employer plans—accounting for 84 percent of Cigna’s total enrollment nationwide—Anthem’s acquisition of Cigna consists almost entirely of an expansion of Anthem’s presence in that submarket.
Yet, while Anthem is one of the largest carriers nationally, its geographic presence is much narrower than those of its peers. That is because Anthem is principally a collection of Blue Cross plans in 14 states. Because of their long histories, at the state level Blue Cross carriers tend to occupy dominant market positions in most or all subsets of the broader health insurance market. Thus, in the 14 states where Anthem owns a Blue Cross subsidiary, the company already has dominant market positions that are almost certain to be further expanded when it acquires any competitor, regardless of the target company’s business focus. In its basic structure, Anthem is most similar to Health Care Services Corporation, which is a nonprofit, member-owned mutual insurer comprised of Blue Cross plans in five states.
Consequently, it is not surprising that Table 2 shows that the main effect of Anthem acquiring Cigna would be to further expand Anthem’s dominance of the market for administrative services for self-insured employer plans in the 14 states where the company owns a Blue Cross carrier. The same would also hold true for the fully insured employer-group market in three of those 14 states: Indiana, Maine, and New Hampshire. However, beyond that, as Table 2 shows, this merger would have little or no market consolidation effect in other states or other market segments.
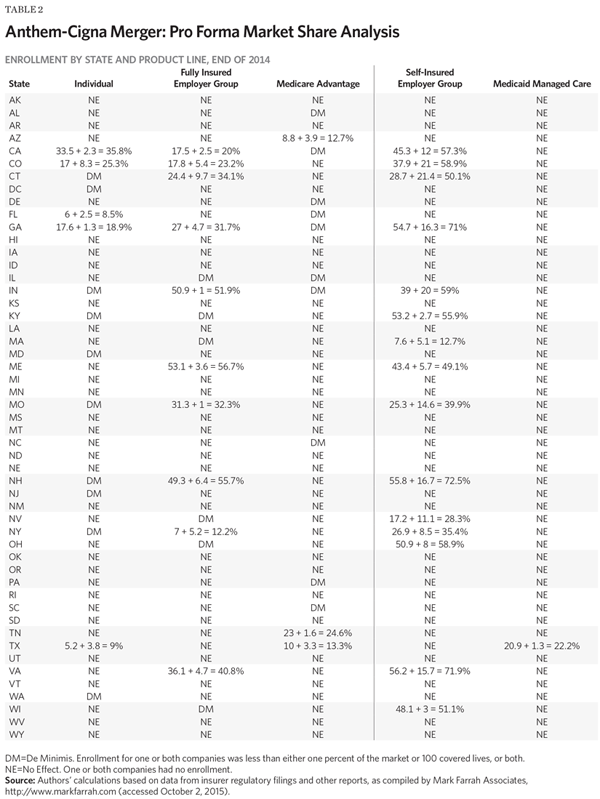
As I previously noted, the market for administrative services for self-insured employer plans is the most “national” of the five market segments and is characterized by sophisticated purchasers with few geographic constraints. Thus, state-level dominance by a single carrier is of less concern in this particular submarket, at least from the perspective of the customers for those services. However, as I also noted, such consolidation would concern medical providers to the extent that more of their patients are enrolled in plans administered by a single carrier.
Centene’s Proposed Acquisition of Health Net
Ninety percent of Centene’s total enrollment is from Medicaid managed-care contracts in 15 states. Health Net operates in only four western states: Arizona, California, Oregon, and Washington, and in two to four market segments in each state—though California is the only state where Health Net has Medicaid managed care. In contrast, Washington is the only one of those four states where Centene has a significant presence (in Medicaid managed care). Thus, this acquisition essentially consists of Centene expanding its geographic “footprint” to include Arizona, California, and Oregon. Because of the lack of overlap between the two companies, in none of the five market segments in any of those four states would this merger produce even one percentage point of market consolidation.
Additional Observations
From the perspective of a market analyst there appear to be likely rationales for each of these three proposed mergers.
Given steadily growing enrollment in Medicare Advantage plans, particularly among younger and newly eligible beneficiaries, Aetna’s decision to expand into that market by acquiring Humana makes sense. In essence, Aetna is looking to acquire more business in a segment of the market with good prospects for future growth.
The self-insured employer market is a large one that has also been growing steadily at rate of about 2 percent per year. Some provisions of the Affordable Care Act (ACA), most notably the extension—starting next year—of the law’s costly essential benefit requirements to employer groups of 100 or fewer workers, may also induce a further shift among mid-sized employers from fully insured to self-insured plans. Thus, it does not seem surprising that Anthem would want to expand further into that market by acquiring Cigna.
While Centene’s acquisition of Health Net can be viewed as an expansion of Centene’s geographic footprint, there may also be another, ACA-related, factor at work. Centene was one of two multi-state Medicaid managed-care companies (the other being Molina) that went into the ACA exchanges in those states where the companies had Medicaid managed-care contracts. Those companies recognized that the design of the ACA’s tax credits and cost-sharing subsidies were likely to produce an exchange market consisting mainly of heavily subsidized low-income customers in plans with only nominal patient cost sharing—in short, a market that looked very much like their existing Medicaid managed-care business. That has indeed proven to be the case, and may be part of the explanation for Centene’s interest in acquiring Health Net, which is already on the exchanges in Arizona and California and also has 332,000 Medicaid managed-care enrollees in California.
Mr. Chairman, this concludes my prepared testimony. I thank you for inviting me to testify today. I will be happy to answer any questions that you or the other Members may have.
