Medicare, enacted along with Medicaid in 1965, is 50 years old.[1] The program, which provides health care services to seniors and some disabled, has successfully provided its enrollees core hospital and physicians’ coverage and a strong measure of financial security. However, fiscal and demographic problems that are inherent in its outdated structure threaten seniors’ future access to quality care and impose massive burdens on taxpayers.
Nothing is inevitable, but Congress will need to tackle these issues head-on if Medicare is to endure for another 50 years. Congress should look to the successful competitive models in Medicare to move toward a future that will ensure security for seniors while also protecting taxpayers.
Fiscal Problems
-
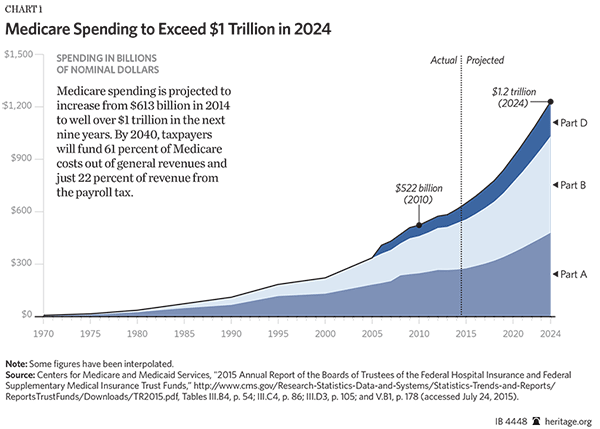
Heavier Taxpayer Burdens. Total Medicare spending will jump from $613 billion in 2014 to more than $1.2 trillion by 2024.[2] As a share of the general economy, Medicare spending will increase from 3.5 percent of GDP in 2015 to 6.3 percent by 2040.[3] Today, seniors’ premiums account for just 13 percent of total Medicare funding. By 2040, seniors’ premiums will increase to 17 percent of total funding, with taxpayers funding 22 percent of the cost out of their payroll taxes and almost 61 percent out of general revenues.[4]
-
Massive debt. Based on their most recent 75-year projection, the staff at the Office of the Actuary at the Centers for Medicare and Medicaid Services (CMS) estimates that Medicare’s stunning unfunded liability—the dollar value of promised benefits that are not paid for—will range between $28 trillion and $37 trillion, depending on the assumptions.[5]
-
Inefficient payment. Since 1966, Congress has tried to slow Medicare costs by cutting payments to doctors and hospitals. In the 1980s, Congress created complex administrative payment formulas combined with payment caps and price controls. The results were predictable: cost shifting, underpayment and overpayment for medical services, and levels of complexity that undercut the program’s efficiency. In his 2003 Senate testimony, former Medicare Administrator Thomas Scully summarized his agency’s work: “[M]y agency fundamentally spends most of its time trying to figure out what the right price is to fix for family physicians in Anchorage or hospitals in Portland.”[6] Scully also agreed that Medicare pricing was inflexible, unable to foster innovation or reward performance, and characterized by huge geographical disparities in payments for the same services.
With the Affordable Care Act (ACA), Congress enacted massive payment cuts and authorized new “value-based” payment systems to secure quality of care. Policymakers expect their cuts to continue Medicare’s recently slower spending growth and hope that their “delivery reforms” will have better results than previous experiments in achieving programmatic savings.[7]
-
Waste, fraud, and abuse. Medicare annually pays more than 1 billion claims.[8] In 2014, the Government Accountability Office (GAO) reported that Medicare’s “improper” payments—incorrect or erroneous payments—amounted to $60 billion.[9] Former U.S. Attorney General Eric Holder indicated in 2012 that Medicare fraud alone ranged between $60 billion and $90 billion annually.[10]
Federal authorities have been auditing, investigating, and prosecuting Medicare fraud for years while also trying mightily to stop wasteful Medicare spending. The problem is seemingly intractable, partly because of Medicare’s sheer size and complexity, as GAO officials have stated repeatedly.[11]
Demographic Problems
-
Flooding Baby Boomer retirement. The 77 million Baby Boomers—those born between 1946 and 1964 after the conclusion of World War II—are nearing retirement age. This will result in a significant jump in Medicare enrollment. The Congressional Budget Office (CBO) projects that the number of Americans aged 65 and older will increase by 76 percent by 2040.[12]
-
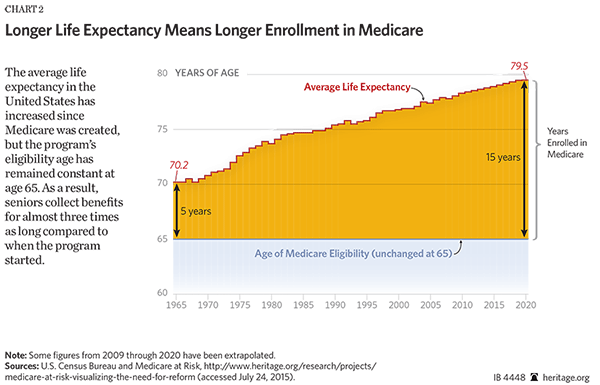
Longer dependence and fewer workers. In 1965, when Medicare was created, the average American life span was a little over 70 years of age, but in 2030, it is projected to reach almost 81 years.[13] In 1965, there were four workers for every retiree.[14] Today, there are roughly three workers for each Medicare beneficiary, and by 2030, that will decline to 2.3 workers for each beneficiary.[15] Americans are living longer and longer in retirement but are supported by fewer and fewer working taxpayers.
Structural Problems
-
Metastasizing bureaucracy. Over the past 50 years, the Medicare bureaucracy has generated tens of thousands of pages of rules, regulations, and guidelines governing virtually every aspect of health care financing and delivery. Medical professionals have had to comply with increasing regulatory requirements and paperwork, thereby incurring higher administrative costs. By the 1990s, the Medicare bureaucracy incurred intense hostility among medical professionals, so the Bush Administration changed the name of the Health Care Financing Administration (HCFA) to the Centers for Medicare and Medicaid Services (CMS), a more consumer-friendly name. But the agency retained its wide-ranging regulatory power. Enactment of the ACA further expanded CMS’s regulatory reach, particularly with new physician and hospital reporting and compliance requirements.
-
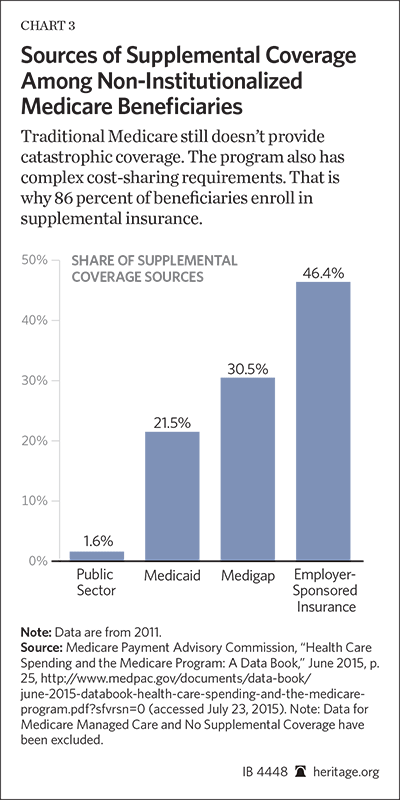
Gaps in coverage. After 50 years, traditional Medicare still does not provide protection from the financial devastation of catastrophic illness. Historically, Medicare’s adoption of medical treatments and new technologies has been sluggish; prescription drugs, for example, were not covered until 2003.[16] Medicare claims rejections have also been generally higher than rejections by private insurance. Not surprisingly, 86 percent of beneficiaries enroll in supplemental insurance, which also routinely provides “first dollar” coverage of medical services.[17] This “double coverage” arrangement, however, stimulates excessive utilization and sharply increases Medicare costs for seniors and taxpayers alike.
-
Uncertain access. The ACA imposes new layers of heavy regulation. Today, 83.7 percent of “office-based” physicians accept new Medicare patients.[18] For Medicare Part B, doctors’ responses to Medicare payment and the ACA regulatory regime will affect seniors’ access to care. For Part A, the health law’s huge payment reductions will compromise that access. According to the 2015 Medicare Trustees report, “By 2040, simulations suggest that approximately half of hospitals, 70 percent of skilled nursing facilities, and 90 percent of home health agencies would have negative total facility margins, raising the possibility of access and quality of care issues for Medicare beneficiaries.”[19]
-
Restricting personal freedom. Medicare’s original language forbids federal officials from supervising or controlling medical practice in any way.[20] In 1997, however, Congress restricted the ability of doctors and patients to contract privately outside of Medicare for Medicare-covered services, despite the fact that no Medicare claims would be submitted for reimbursement. The law says that a Medicare patient can contract privately with a physician only if the doctor signs an affidavit to that effect, submits that affidavit to the Secretary of Health and Human Services, and refrains from billing Medicare for the treatment of any other Medicare patient for two full years.[21] As Mark Pauly, professor of economics at the University of Pennsylvania, observes, “In contrast to people with private insurance, people on Medicare cannot pay with their own money for something that is more medically valuable to them than it is to the Medicare bureaucracy.”[22]
Looking Ahead
While traditional Medicare Parts A and B is the fountainhead of Medicare’s recurrent problems, Medicare Parts C and D, which are based on a competition, hold the solutions. With modernized funding of health plans and drugs, “Competitive Medicare” shows the potential of defined contribution financing to secure a comprehensive array of services at competitive pricing with high rates of patient satisfaction.[23]
Congress can build on the best features of these programs and create a modern defined contribution (“premium support”) system for the entire program.[24] Such a reform would reduce bureaucracy, eliminate centralized administrative payment, control costs through intense competition on a level playing field, ensure catastrophic protection and broader benefit options, and stimulate innovation and clinical advances in care delivery. Real reform would thus secure genuine value for Medicare dollars.
—Robert E. Moffit, PhD, is Senior Fellow in the Center for Health Policy Studies, of the Institute for Family, Community, and Opportunity at The Heritage Foundation.