Today’s seniors are facing higher Medicare costs. Over the next five years, current law, as amended by the Patient Protection and Affordable Care Act (PPACA, also known as Obamacare), already guarantees higher out-of-pocket costs for today’s seniors. Beyond the current law, the President’s latest budget proposal would increase seniors’ costs even more. So, notwithstanding “progressive” politicians’ rhetorical promise to “keep Medicare as we know it,” the Obama Administration is formally committed to increasing seniors’ out-of pocket costs, while the President and his allies in Congress have already enacted major Medicare payment reductions that threaten their access to care. Beyond the payment reductions to hospitals, skilled nursing facilities, and home health care agencies, many seniors will also experience a reduction in their Medicare Advantage benefits or even a loss of their existing plan.
Status Quo Hikes
The 2012 Medicare trustees report says that between 2012 and 2017, seniors’ standard Medicare Part B monthly premiums will jump from $99.90 to $128.20, while their Part B deductibles will rise from $140 to $180.[1] Seniors’ Medicare hospital deductible will increase from $1,156 to $1,336, while their daily hospital co-insurance will climb from $289 to $334. For seniors who remain in the hospital beyond 90 days (lifetime reserve days), the per diem co-insurance costs are estimated to reach $668 by 2017.[2]
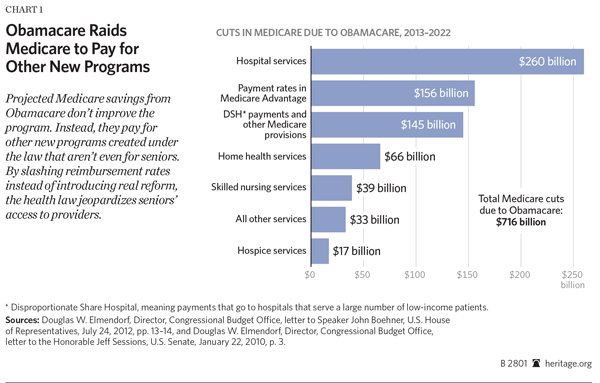
Obamacare: Impact on Access to Care. Obamacare mandates $716 billion in Medicare payment reductions over the next 10 years.[3] However, contrary to the way they are often portrayed, these cuts are not aimed at specific instances of “waste, fraud, and abuse.” Rather, they are across-the-board changes in Medicare payment formulas for hospitals, nursing homes, home health agencies, hospice agencies, and Medicare Advantage plans.
Notwithstanding the tiresome rhetoric that Medicare payment reductions affect only providers and not beneficiaries, funding cuts for Medicare services directly affect those who depend on those services. If these major reductions are implemented by Congress over the coming decade, seniors’ ability to access Medicare services will surely be compromised. In fact, the Medicare Trustees said that “[a]bsent other changes, the lower Medicare payment rates would result in negative total facility margins for an estimated 15 percent of hospitals, skilled nursing facilities, and home health agencies by 2019, and this percentage would reach roughly 25 percent in 2030 and 40 percent by 2050.”[4]
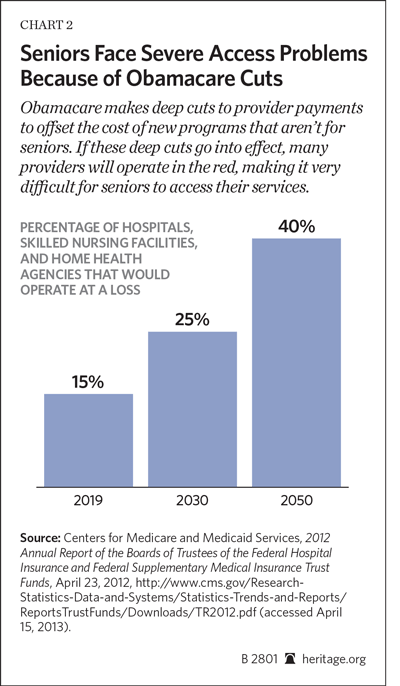
This means that seniors would have an increasingly difficult time accessing care. As the Trustees explain,
Medicare’s payments for health services would fall increasingly below providers’ costs. Providers could not sustain continuing negative margins and would have to withdraw from serving Medicare beneficiaries or (if total facility margins remained positive) shift substantial portions of Medicare costs to their non-Medicare, non-Medicaid payers. Under such circumstances, lawmakers would probably override the productivity adjustments, much as they have done to prevent reductions in physician payment rates.[5]
Moreover, these “savings” are not even reserved to enhance the solvency of the financially troubled Medicare program. Instead, the “savings” are used to finance new spending for non-Medicare coverage expansions in Obamacare.[6] Despite the simple fact that the same dollar cannot be spent twice, the Obama Administration simultaneously claims credit for extending the life of the Medicare trust fund, financing expanded health insurance coverage outside Medicare, and reducing the federal deficit.
Higher Medicare Taxes. The PPACA will also increase Medicare taxes. The law raises the standard Medicare payroll tax, which funds the hospital insurance (HI) trust fund, on high-income earners (individuals with an annual income of $200,000 and couples with an annual income of $250,000) from 2.9 percent to 3.8 percent and also extends the 3.8 percent Medicare tax to investment income. Together, this is the largest tax increase in Obamacare, costing taxpayers almost $318 billion between 2013 and 2022.[7]
Once again, however, the new Medicare payroll tax revenue is double-counted: It is paying for new spending, while also extending the life of the trust fund.[8] As for the new Medicare tax on investment income, Medicare trustee Charles Blahous explains that “[t]hough termed an ‘Unearned Income Medicare Contribution’ (UIMC) under the law, this revenue would not come from Medicare’s traditional contribution base and it would not be allocated to a Medicare Trust Fund.”[9] (Emphasis added.)
Obamacare: Impact on Seniors’ Medicare Advantage Coverage. Currently, 27 percent of all Medicare beneficiaries are enrolled in Medicare Advantage (MA) plans. MA plans are attractive to beneficiaries because they offer more comprehensive coverage than traditional Medicare. Most notably, unlike traditional Medicare, MA plans cap out-of-pocket costs, which eliminates the need for beneficiaries to pay extra and purchase separate supplemental insurance, and these plans also routinely offer drug coverage. Further, since 2007, between 85 percent and 94 percent of participating seniors have had the option of enrolling in these private plans while paying no premium other than the standard Medicare Part B premium.[10]
The PPACA reduces payments in the MA program by $156 billion between 2013 and 2022. When the law was enacted in 2010, the Medicare actuary projected the impact of these cuts: “We estimate that in 2017, when the MA provisions will be fully phased in, enrollment in MA plans will be lower by about 50 percent (from its projected level of 14.8 million under the prior law to 7.4 million under the new law).”[11]
According to the Medicare actuary, then, an estimated 7 million seniors will leave Medicare Advantage over the next four years, but that means that they will have to re-enroll in the less generous traditional Medicare program.[12] Not only will these seniors face the loss of their existing comprehensive health plan, they will somehow have to fill big gaps in their Medicare benefits—which would mean substantial increases in their out-of-pocket costs. To compensate for gaps in traditional Medicare coverage, nearly all seniors enrolled in traditional Medicare purchase separate drug coverage and supplemental health insurance coverage, which are projected to cost on average $42 a month and $230 a month, respectively, in 2017.[13]
An analysis by health care economists Robert Book and James Capretta shows, “By 2017, Medicare beneficiaries who would have enrolled in Medicare Advantage under prior law will lose an average of $1,841 due to the MA changes alone and $3,714 when the effects of the entire bill, including the FFS [fee-for-service] cuts, are considered.”[14]
But those seniors who remain in MA will also face increased out-of-pocket costs because of other features of the President’s health care law. Obamacare imposes a special “fee” (a tax) on all health insurance plans beginning in 2014, including MA plans. Of course, as with all taxes on firms in any market, the costs of the tax increases are routinely passed on to consumers in the form of higher prices or, in the case of insurance, higher premiums. In this particular case, Oliver Wyman, a leading benefits consulting firm, has estimated, “In the Medicare market, the premium tax would increase the expected cost of MA coverage per enrollee by $3,604 over the ten-year period.”[15]
Obama’s FY 2014 Budget: Higher Seniors’ Premiums. In his fiscal year (FY) 2014 budget proposal, President Obama has proposed additional Medicare changes that would also increase costs for seniors.[16]
For Medicare Parts B and D, the President’s budget plan would expand “means testing” in the Medicare program for upper-income seniors, resulting over time in a total of 25 percent of all Medicare beneficiaries paying an income-adjusted premium. Under current law, there are four income-adjusted brackets; seniors in these income brackets pay progressively higher premiums, ranging from 35 percent to 80 percent of total Medicare program costs. In his latest budget proposal, President Obama expands the number of brackets from four to nine, requiring seniors to pay from 40 percent to 90 percent of total Medicare premium costs. For the lowest bracket, an individual with an income of $85,000 to $92,333 who is enrolled in Part B and Part D would have a combined premium increase of about $401.76 in 2017, compared to what he would pay under current law. For an individual with an annual income between $178,000 and $196,000, his combined premium increase would be an estimated $1,615 in 2017 (at 85.5 percent of total costs).
Reduction of taxpayer subsidies for high-income Medicare recipients is sound policy. There is indeed a large and growing bipartisan consensus among a variety of analysts on the need to expand the scope of Medicare “means testing.” While it makes sense to gradually reduce taxpayer subsidies for an expanded pool of upper-income seniors, it is not necessary to require one out of every four Medicare beneficiaries to pay more than the standard Medicare premiums.[17]
Obama’s Budget: New Fees
President Obama’s FY 2014 budget would also impose new fees on baby boomers joining Medicare beginning in 2017. His 2014 budget proposal introduces a $25 increase in the Part B deductible for new beneficiaries in 2017, 2019, and 2021, a $75 total increase by 2021, plus a $100 co-payment for home health services in certain cases.
Traditional Medicare incurs excessive costs resulting from “first-dollar” coverage by Medigap and other supplemental insurance. This first-dollar coverage increases utilization of medical services and drives up Medicare costs for seniors and taxpayers alike.
President Obama is right to address the need to curb the first-dollar coverage that drives up Medicare costs. His solution, however, is hardly the best available option. The President proposes a premium surcharge—a kind of “premium tax”—for new beneficiaries who choose a Medigap plan with first-dollar or near-first-dollar coverage. This approach would affect a majority of new beneficiaries in Medigap.[18] The surcharge would be equivalent to 15 percent of the average Medigap premium, adding an estimated $413.60 a year to these seniors’ premium costs.[19] While there is general agreement that supplemental coverage drives up overall Medicare costs, a much better approach would be to restructure Medicare’s cost-sharing arrangements, instead of imposing yet another federal “tax” on seniors.[20]
Obamacare and Obama’s Budget: New Prescription Drug Costs
The Obama Administration’s proposed new out-of-pocket costs will be coupled with a general increase in premiums for beneficiaries enrolled in Medicare Part D, the Medicare drug program.
The PPACA designates an estimated $48 billion to reduce out-of-pocket costs for Medicare beneficiaries, particularly those who find themselves faced with a gap in coverage for their drug costs, commonly referred to as the “donut hole.” The President’s policy is to close this Medicare Part D donut hole.[21] Under the law, the donut hole is slated to close by 2020.
While out-of-pocket costs for Medicare Part D will be reduced, the changes enacted under the new health law will only come at a higher premium price for seniors. According to the Congressional Budget Office’s 2010 estimate, “enacting those changes would lead to an average increase in premiums for Part D beneficiaries of about 4 percent in 2011, rising to about 9 percent in 2019.”[22]
These Medicare prescription drug premium increases must be understood in terms of how the Part D donut hole actually affects today’s seniors. While the average premiums of all Part D beneficiaries will increase, of all 48.6 million Medicare enrollees in 2011, only 3.6 million actually fell into the donut hole.[23] Moreover, approximately 11 million enrollees receive low-income subsidies for drug coverage, including coverage in the donut hole. Today, most private health plans already provide additional coverage for beneficiaries who might find themselves in the donut hole. For 2012, 52 percent of all plans provide generic or some generic and some brand-name drug coverage in the donut hole.[24]
The President’s FY 2014 budget proposal would close the Part D coverage gap for brand-name drugs in 2015, five years sooner than under current law. For the small minority of seniors who fall into the donut hole annually, that would be a welcome development; but most seniors should also realize that while assisting the small number of seniors who fall into it, the President’s proposal makes the drug benefit more expensive and thus will result in a general increase in seniors’ Part D premiums.
A Backdoor Tax on Seniors. Today in Medicare Part D, private plans and drug manufacturers negotiate a discounted price; it is a market price. The government is not involved at all in these negotiations. The result: Market efficiencies have been dramatically successful in controlling Medicare drug costs and stabilizing the growth in seniors’ premiums.
The President’s recent budget proposal, however, would require drug companies to pay the government the difference between the privately negotiated Medicare price and the price (the “rebate”) the government sets for the sale of drugs in the Medicaid program for low-income Medicare beneficiaries. These seniors today receive subsidies, and they account for about 30 percent of all Medicare Part D enrollees.
The President’s proposed Medicare “rebate” would act as a tax on the drug companies doing business with the federal government, but it would also function as a price control on Medicare drugs. In other words, the new rebate policy would distort the Part D market by fixing artificially low prices for one group of beneficiaries, and creating powerful incentives for the companies to try to make up the revenue losses by charging higher prices in other sectors of the Medicare market. This means that most seniors would experience increased premiums. Analysts with the American Action Forum estimate that a Medicaid-style rebate for Part D would increase beneficiary premiums by anywhere between 20 percent and 40 percent.[25]
Out of Options
President Obama’s latest budgetary scheme is not a serious prescription for long-term Medicare reform. While it tweaks Medicare’s administrative payment systems, it simply retains the current structure and provides for more cost shifting to seniors.
The President’s budget is another indication that the Administration and its allies on Capitol Hill are running out of consequential options. They have already cut Medicare Part A and Medicare Advantage provider-reimbursement rates to levels that even government actuaries have stated, in print, to be unrealistic. They have instituted a new Medicare tax on the “unearned” income of upper-income Americans (such as investment income) that will not even be exclusively used to enhance the solvency of Medicare. The vaunted Medicare “savings” from Medicare provider payment reductions and other changes enacted through the PPACA will also finance health insurance coverage mandated by Obamacare.[26]
America needs a sound Medicare policy. The Obama Administration’s agenda for increased costs for Medicare beneficiaries, plus the latest budget tweaks to administrative payments, will not reverse the troubled program’s unsustainable course.[27]
Americans differ on Medicare reform. They may disagree on the right future for Medicare. But one thing is certain: Under the Obama agenda, seniors will pay more—much more—and they will pay this steep price in many different ways, including a loss of access to care resulting from demoralized doctors and other medical professionals cutting back on Medicare practice or, in some cases dropping out of Medicare practice altogether. Doctors and other medical professionals are facing a bleak future of continued reimbursement reductions and the higher administrative costs of complying with an even larger set of increasingly complex rules and reporting requirements.
The bottom line: Medicare “as we know it” is already a thing of the past and the only way to preserve Medicare for current and future retirees is through major, market-based structural reform.[28]
—Robert E. Moffit, PhD, is Senior Fellow, and Alyene Senger is Research Assistant, in the Center for Health Policy Studies at The Heritage Foundation.