Executive Summary
The United States is at a fiscal tipping point—mostly due to the explosive growth in federal entitlement spending, especially on Medicare. The long-term unfunded liability of the Medicare program—promised benefits that are not financed—is almost $37 trillion, and it is relentlessly generating annual deficits. Medicare’s hospital insurance (HI) trust fund faces a shortfall of $31.8 billion in 2012. The Congressional Budget Office (CBO) estimates that Medicare spending will jump from $560 billion in 2012 to $1.041 trillion in 2022. Each year of delay makes reform that much harder.
To preserve Medicare for the next generation of retirees, The Heritage Foundation has developed a Medicare premium support plan as part of its comprehensive budget reform, Saving the American Dream. With premium support, the government makes a fixed payment (a defined contribution) to a health plan chosen by an enrollee. If an enrollee wants to purchase a plan that is more expensive than the government payment, the enrollee may do so, paying the additional cost. If an enrollee wants to buy a less expensive plan, the enrollee may also do so, and keep the savings.
Health plans would compete directly with each other for market share. Their ability to retain or expand their enrollment would depend solely on their ability to provide the best package of benefits and the highest quality of care at the most competitive price. The American Enterprise Institute, the Cato Institute, the National Center for Policy Analysis, and the Progressive Policy Institute have all endorsed this general approach to comprehensive Medicare reform.
A Powerful Consensus. Representative Paul Ryan (R–WI), chairman of the House Budget Committee, has been a leading champion of premium support. The House Budget Resolution is the most recent version of his Medicare proposal. Representative Ryan also joined Senator Ron Wyden (D–OR) in offering an updated premium support proposal. Likewise, Senators Richard Burr (R–NC) and Tom Coburn (R–OK) have offered a robust premium support plan, as have Dr. Alice Rivlin, former Director of the Congressional Budget Office, and former Senator Pete Domenici (R–NM). Senator Joseph Lieberman (I–CT), along with Senator Coburn, has also proposed a major reform of the current Medicare fee-for-service (FFS) program.
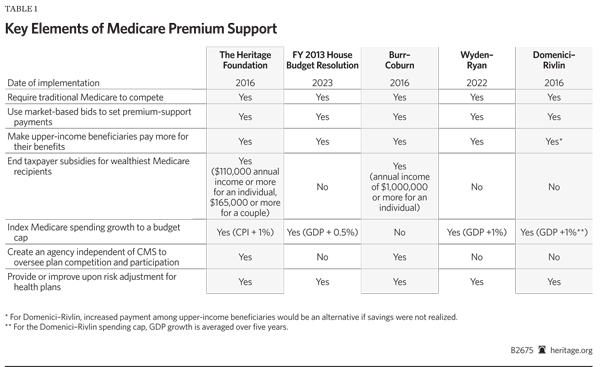
The leading Medicare premium support proposals, including The Heritage Foundation’s, have certain features in common:
- A requirement that traditional Medicare compete with private plans. Under the Heritage plan, Congress would transform the complex Medicare FFS program into a health plan with the capacity to compete with private plans chosen by enrollees. All other leading proposals would do the same.
- Market-based bids to determine government payment for health plans. Withthe Heritage proposal,the government’s contribution to a Medicare enrollee’s coverage would be based on an annual process of (regional and national) competitive bidding among health plans to provide at least the traditional Medicare benefits. Seniors choosing plans below the government contribution would receive a rebate and seniors choosing above the government contribution would pay the difference. All other leading proposals are based on similar financing.
- An adjustment of beneficiary payment or taxpayer subsidies for income. Taxpayers today directly finance between 85 percent and 90 percent of total annual Medicare costs. Under the Heritage proposal, current income thresholds for taxpayer subsidies would be tightened, and phased out entirely for the wealthiest cohort of retirees. All other leading proposals retain or expand the application of income-based subsidies for Medicare benefits.
- An authorization of an agency to oversee the competitive program and guarantee strong consumer protections. A federal agency should enforce uniform rules for health insurance and rules for consumer protection, such as marketing rules and fiscal solvency requirements, and administer a risk-adjustment program. In the Heritage plan, the existing Center for Drug and Health Plan Choice would fulfill that role, but would be independent of the Centers for Medicare and Medicaid Services (CMS), which runs traditional Medicare. All other leading proposals put in place a mechanism to enforce rules for market competition and guarantee strong consumer protection.
- A provision for, or improvement of, risk adjustment for health plans. With patient choice among a wide array of competing plans, the affordability and continuity of coverage can be disrupted by adverse selection (the concentration of older and sicker beneficiaries in certain plans) thus pushing up costs and driving out plans. To cope with adverse selection and stabilize the market, the Heritage plan improves upon the risk-adjustment mechanisms of current law. All other leading proposals adopt risk-adjustment systems for insurance.
New Incentives. Premium support would be transformational. New and powerful economic incentives unleashed by the free-market forces of patient choice and health plan competition would not only improve quality, but also control costs and reverse Medicare’s current rush toward disastrous debt.
No major proposal has yet been committed to legislative language, and each differs in degree and level of detail. Heritage, for instance, would put Medicare on an annual budget, but not all proposals do so. Heritage would also build a clear wall of separation between CMS and the administration of the new competitive system, but not all proposals do so.
While all proposals provide protection from catastrophic illness, they differ on cost sharing and subsidy levels based on income. Differences in detail are important, but they are of secondary importance to the economic impact of expanded premium support payment for Medicare benefits. This is a fundamental structural change in total Medicare financing.
Abstract: Medicare is central to the debate on federal entitlement spending. A failure to reform Medicare, and thus control entitlement spending, will rob Americans of a fleeting opportunity to escape ruinous debt, crushing taxation, or severe austerity measures. Medicare’s long-term unfunded liability is almost $37 trillion, and it is relentlessly generating annual deficits. Medicare’s hospital insurance trust fund faces a shortfall of $31.8 billion in 2012. The Congressional Budget Office estimates that Medicare spending will jump from $560 billion in 2012 to $1.041 trillion in 2022. Each year of delay makes reform that much harder. This Heritage Foundation Backgrounder compares the Heritage reform plan, advanced in Saving the American Dream, with five other reform plans. They differ in detail, but their main features are similar. Congress should build on this powerful consensus and craft a comprehensive reform of the Medicare program.
The United States is at a fiscal tipping point—mostly due to the explosive growth in federal entitlement spending, especially on Medicare. The Congressional Budget Office (CBO) estimates that Medicare spending will jump from $560 billion in 2012 to $1.041 trillion in 2022.[1]
A Powerful Consensus. The good news is that some Members of Congress are forging a powerful consensus on reforming Medicare. Senators Richard Burr (R–NC) and Tom Coburn (R–OK), and Representative Paul Ryan (R–WI), chairman of the House Budget Committee, and Senator Ron Wyden (D–OR) would improve upon the experience of defined-contribution (“premium support”) financing that today characterizes the competitive private plan program in Medicare Part C and the Medicare drug program in Medicare Part D. In other words, the expansion of a system of financing that already provides benefits for the vast majority of retirees would be the least disruptive of all changes, particularly the deep Medicare payment cuts mandated by current law.[2] By harnessing free-market forces of choice and competition, already serving the vast majority of Medicare beneficiaries, these Members of Congress would create a better Medicare program for future retirees. Meanwhile, Senator Joseph Lieberman (I–CT) and Senator Tom Coburn would fix certain broken features of the existing Medicare program that drive perverse economic incentives, which, in turn, contribute to escalating costs and compromise the quality of care.
The Heart of Reform. Premium support is at the heart of major Medicare reform proposals. It is a system of defined-contribution financing, where the government makes a direct and fixed payment to a health plan chosen by an enrollee. If an enrollee wants to purchase a plan that costs more than the government payment covers, the enrollee may do so, paying the additional cost. If an enrollee wants to buy a less expensive plan, the enrollee can do that as well, and keep the savings. Beneficiaries would choose health plans within an intense competitive environment, where plans would compete directly with each other for market share. Their success would depend on their ability to provide the best package of benefits and the highest quality of care at the most competitive price.
Beyond a growing band of congressional leaders, premium support is backed by such public policy organizations as the American Enterprise Institute, Bipartisan Policy Center, the CATO Institute, National Center for Policy Analysis, and the Progressive Policy Institute.[3]
Common Features. The Heritage Foundation’s Medicare premium support plan is among the most detailed of such proposals, though all plans have certain features in common:
- A requirement that traditional Medicare compete with private plans. Under the Heritage plan, Congress would transform the complex Medicare FFS program into a health plan with the capacity to compete with private plans chosen by enrollees. All other leading proposals would do the same.
- Market-based bids to determine government payment for health plans. With the Heritage proposal, the government’s contribution to a Medicare enrollee’s coverage would be based on an annual process of (regional and national) competitive bidding among health plans to provide at least the traditional Medicare benefits. Seniors choosing plans below the government contribution would receive a rebate and seniors choosing above the government contribution would pay the difference. All other leading proposals are based on similar financing.
- An adjustment of beneficiary payment or taxpayer subsidies for income. Taxpayers today directly finance between 85 percent and 90 percent of total annual Medicare costs. Under the Heritage proposal, current income thresholds for taxpayer subsidies would be tightened, and phased out entirely for the wealthiest cohort of retirees. All other leading proposals retain or expand the application of income-based subsidies for Medicare benefits.
- An authorization of an agency to oversee the competitive program and guarantee strong consumer protections. A federal agency should enforce uniform rules for health insurance and rules for consumer protection, such as marketing rules and fiscal solvency requirements, and administer a risk-adjustment program. In the Heritage plan, the existing Center for Drug and Health Plan Choice would fulfill that role, but would be independent of the Centers for Medicare and Medicaid Services (CMS), which runs traditional Medicare. All other leading proposals put in place a mechanism to enforce rules for market competition and guarantee strong consumer protection.
-
A provision for, or improvement of, risk adjustment for health plans. With patient choice among a wide array of competing plans, the affordability and continuity of coverage can be disrupted by adverse selection (the concentration of older and sicker beneficiaries in certain plans) thus pushing up costs and driving out plans. To cope with adverse selection and stabilize the market, the Heritage plan improves upon the risk-adjustment mechanisms of current law. All other leading proposals adopt risk-adjustment systems for insurance.
The features of these plans differ in details. For example, while all proposals provide catastrophic protection, they differ on the level of out-of-pocket exposure or cost sharing. But in almost all cases, the differences in detail are of secondary importance to the transformational impact of new and powerful economic incentives unleashed by the free-market forces of patient choice and health plan competition in a premium support program.
A Better Future. Today, Medicare faces a long-term unfunded liability—benefits promised to retirees that are not financed—of almost $37 trillion. The rapidly accelerating spending, projected by the CBO, is generating continuing and substantial annual deficits; Medicare’s hospitalization (HI) trust fund, already threatened with insolvency, faces a shortfall of $31.8 billion in 2012.[4]
Today’s Medicare problems are a direct result of its outdated, centralized structure and the perverse economic incentives that it generates and sustains. Traditional Medicare pays doctors and other medical professionals a price-controlled fee for each of the thousands of medical treatments and procedures available to Medicare patients, and medical professionals respond to price controls by increasing the volume of medical services. Meanwhile, positive market-based incentives that would otherwise control costs, and drive rapid innovation in the delivery of efficient, high-quality care, are largely absent.
Premium support would realign the economic incentives of patients, plans, and providers. Within a competitive environment of competing plans on a level playing field, health plans would be compelled to deliver value for health care dollars. Competition would stir innovation, and greater innovation in health care delivery would increase productivity, as well as control costs for taxpayers and retirees alike. That is a Medicare future compatible with the American dream.
The Heritage Foundation’s Comprehensive Plan
As outlined in Saving the American Dream,[5] The Heritage Foundation prescribes a two-stage comprehensive reform of the Medicare entitlement. The first stage, beginning immediately (2012), would make a series of changes to the traditional Medicare Program.[6] The second stage, beginning in 2016, would be a robust structural reform, transforming Medicare into a premium support program.[7]
Changing Traditional Medicare. The Heritage plan adds a new Medicare catastrophic benefit. This benefit would be of tremendous value to beneficiaries, giving them peace of mind about the financial devastation of major illness or accident. The new benefit would also obviate the need for today’s Medigap supplemental coverage, which provides “first dollar” coverage and fuels greater use and higher premiums. Addition of the catastrophic benefit would be combined with streamlining Medicare deductibles and co-payments for Medicare physician and hospitalization services.
In this first stage of reform, Medicare solvency would be guaranteed through the addition of a new Part A premium to eliminate annual deficits in the hospitalization trust fund,[8] as well as a 10 percent co-payment for home health services.[9] The standard beneficiary portion of total premiums for Part B (physician services) and Part D (drug coverage) would be gradually increased from 25 percent to 35 percent,[10] while “hold harmless” protections for retirees in current law would be retained.[11]
The current income thresholds that require larger premium payments for wealthy retirees enrolled in Medicare Parts B and D would be lowered. But the reduction in subsidies for these retirees would be more gradual than current law, and, in contrast to the Affordable Care Act, the income thresholds for higher premium payments would be indexed to inflation for the next 10 years and beyond.[12] For upper-income retirees—defined as individuals with annual incomes in excess of $55,000, and couples with incomes in excess of $110,000 (about 9 percent of all retirees)—there would be a gradual reduction (1.8 percent decrease in subsidy per $1,000 increase in income) of taxpayer subsidies for their premiums. The wealthiest retirees, about 3.5 percent of the total, would pay the full cost of their Medicare premiums.[13]
The normal age of eligibility would be gradually increased (two months annually) from 65 to 68 over 10 years, and thereafter indexed to increases in life expectancy.
Medicare patients’ access to doctor services would be enhanced by “fixing” the sustainable growth rate (SGR) formula permanently—by ending it. During the five-year transition to a new Medicare premium support program, physician payments would be frozen, but doctors would be able to charge beneficiaries above the Medicare payment levels as long as they disclose their prices up front.[14] Meanwhile, current statutory restrictions on private contracting between doctors and Medicare patients for medical services outside Medicare and the provision of care through physician-owned specialty hospitals would be repealed. Altogether, these first-stage Medicare changes would yield savings of $298.6 billion between 2012 and 2016.[15]
Creating a Better Medicare. Under the Heritage plan a new premium support program would begin in 2016.[16] Medicare would switch from paying doctors, hospitals, and other medical professionals on a “fee-for service” (FFS) basis, according to various formulas and fee schedules, to paying health plans directly on behalf of Medicare beneficiaries. The payments, in the form of fixed amounts, would be made to competing plans offering traditional Medicare benefits, as they do today in Medicare Advantage. (Medicare Part D payments are also made in this fashion for prescription drug coverage). This payment would be a defined contribution, and is often described as a premium support; it would be made, based on the beneficiary’s choice, to either a private plan or Medicare FFS.
The government contribution (the “premium support”) to health plans would be determined by regional market bids among competing plans—competitive bidding—to provide traditional Medicare benefits, or their actuarial equivalents, plus drug and catastrophic coverage.[17] Heritage also proposes bidding for health plans marketed at the national level, just as the Federal Employees Health Benefits Plan (FEHBP) does today. Different parts of traditional Medicare would be unified into one plan, and traditional Medicare would be forced to compete with private health plans.[18]
On the basis of this market bidding during the first five years of the new program, government payment per enrollee (the premium support) would be 88 percent of the weighted average premiums of competing health plans, much like the per enrollee payment in the FEHBP.[19] After the initial five years, government payment would be tied either to the bid of the lowest cost plan or, alternatively, to the average of the three lowest regional bids.[20] Seniors choosing plans below the government contribution would receive a rebate and seniors choosing above the government contribution would pay the difference. The government payment would also be adjusted for income, based on the new income thresholds established in the first stage of the reform. Poor seniors would receive additional assistance. The wealthiest retirees (3.5 percent) would no longer qualify for taxpayer subsidies for their health care, but they would be able to enroll and secure the advantages of the large Medicare pool, its guaranteed issuance of insurance, and its variety of benefit plans and options offered at competitive prices.
For the new competitive system, the key to success is the guarantee of a level playing field among all participants. No plan would receive additional federal subsidies, taxpayer bailouts, or special regulatory or pricing advantages. In the Heritage model, there would be a wide variety of health plan and benefit options. Beyond traditional Medicare, the system would be open to Medicare Advantage plans; union plans; employer group and individual plans; and federal, state, and local government plans. Those persons with health savings accounts would be able to bring them into retirement with them.
The Medicare Center for Drug and Health Plan Choice, which today runs Medicare Parts C and D, would administer the new competitive program. It would conduct annual enrollment, oversee enforcement of fiscal solvency and insurance and marketing rules, the administration of risk adjustment, and the protection of beneficiaries from fraud and abuse. But, in the Heritage proposal, the Medicare Center would be institutionally separated from the CMS administration of traditional Medicare. It would either be given a separate line of reporting directly to the Secretary outside the CMS chain of command, or it would be transformed into an independent agency, the Medicare Patient Protection Commission, with members appointed by the President and confirmed by the Senate to ensure a wall of separation between the management of traditional Medicare and the administration of the new competitive system.[21]
While intense competition and new economic incentives will control costs, the Heritage plan also includes an overall Medicare spending cap. The growth in spending would be indexed to the Consumer Price Index (CPI) plus 1 percent. Analysts at The Heritage Foundation’s Center for Data Analysis (CDA) project that moving to a premium support system in 2016 would result in an initial 10-year savings of $702 billion. Overall, the changes to Medicare would secure total Medicare savings of $9.4 trillion by 2035.[22]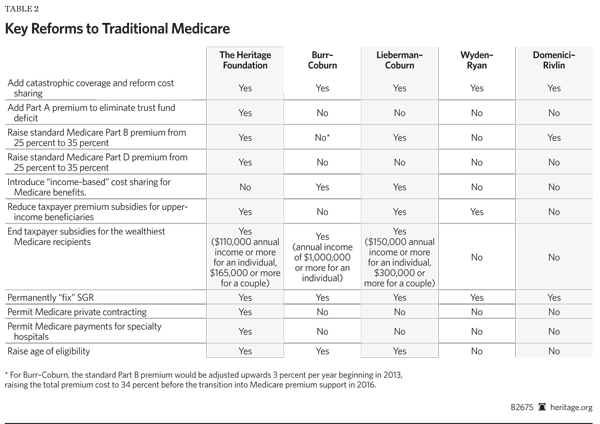
The FY 2013 House Budget Resolution (Ryan Proposal)
House Budget Committee Chairman Paul Ryan has unveiled a comprehensive FY 2013 budget proposal, including a reform of the Medicare program.[23]
Under the House Budget proposal, Medicare transitions into a premium support program. Beginning in 2023,[24] the federal government would make a defined contribution (a fixed dollar amount) to a health plan chosen by newly retiring seniors. The contribution would either “pay for or offset” the premium cost of a health plan.[25] Plan options would include both private plans and traditional Medicare FFS plans. The competition among these plans would take place through a common market called a “Medicare exchange.”
Government payment would be based on competitive bidding among plans to provide traditional Medicare benefits or their actuarial equivalents. The bid of the second-lowest cost plan (either a private plan or traditional Medicare) would be the benchmark for the annual government payment to competing health plans. If a beneficiary chose a plan that was more expensive than the benchmark payment, the beneficiary would pay the full additional cost of choosing the more expensive plan. If the beneficiary chose a plan that was less expensive than the benchmark, the beneficiary would receive the difference in the form of a rebate. All plans would be governed by insurance rules established in current law: guaranteed issue and community rating.
Under the House Budget proposal, the standard government contribution would be further adjusted by income, geography, and risk. Upper-income beneficiaries would pay more than the standard premium. These higher-premium payments would track the categories established in current law for wealthy beneficiaries under Medicare Part B and Part D.[26]
Low-income persons, as defined by current law, would qualify for additional financial assistance. Low-income beneficiaries who qualify for both Medicare and Medicaid (“dual-eligibles”) would continue to receive additional assistance from Medicaid to cover their Medicare expenses as they do under current law. For those low-income beneficiaries who are ineligible for Medicaid, the government would provide “fully funded” special accounts to help offset their out-of-pocket expenses.[27]
Moreover, high-risk beneficiaries, generally those with more serious health conditions, would also secure higher government payments to offset their higher costs. The proposal is thus designed to guarantee beneficiaries access to affordable health plans, regardless of their health status or condition, and to ensure continued plan participation and market stability in the new program. To accomplish this objective, the House Budget proposal would require the CMS to “build upon” the risk-adjustment mechanisms in place today in Medicare Parts C and D.[28] Specifically, CMS would annually review the risk profiles of competing health plans (a “risk-review audit”). On the basis of that audit, CMS would charge health plans that enrolled a “higher than average” number of low-risk beneficiaries a fee, and use the monies from those fees to provide “incentive payments” to health plans covering “higher than average” numbers of high-risk beneficiaries. The fees and incentive payments would flow through a "single pool" of funding for the risk-adjustment program.[29]
Market-based pricing combined with consumer choice and competition will control Medicare costs. Nonetheless, the House Budget proposal would also put Medicare on a budget, and cap annual Medicare spending growth at gross domestic product (GDP) plus 0.5 percent. The proposed spending cap would serve as a “fallback” to assure budgetary savings, measurable by the CBO, and enhance strong incentives on the part of plans to control cost.[30] At the same time, the proposal would repeal the “Independent Payment Advisory Board” created under the PPACA. Between 2023 and 2034, the proposal would also raise the age of eligibility from 65 to 67. In sharp contrast to current law, any savings from changes in traditional Medicare would be exclusively earmarked to enhance the solvency of the Medicare program.[31]
Between 2012 and 2050, based on the Congressional Budget Office’s initial analysis, the House Budget proposal would result in a substantial reduction in federal deficits and debt, securing a balanced budget, as well as a more gradual increase in total Medicare spending compared to current law.[32]
Similarities to Heritage. Like the Heritage plan, the House Budget proposal for Medicare premium support would rely on competitive bidding for the provision of Medicare benefits (or their actuarial equivalent) to establish a market-based payment to competing health plans; compel traditional Medicare to compete with private plans; make upper-income beneficiaries pay higher premiums; retain Medicare insurance rules; put Medicare on a budget; and build and improve upon the risk-adjustment mechanisms established in current law. As recommended by Heritage, the proposal would also introduce a “back-end” risk-adjustment mechanism to protect plans in the Medicare market from adverse selection and guarantee stability of coverage for enrollees.
Differences with Heritage. While Heritage would transition to a Medicare premium support program in 2016, the House Budget proposal would not make such a transition until 2023. This is a very long delay, given the size of the baby boom generation, which has already begun to retire, and the enormity of the fiscal pressures that are building within the next 10 years. By 2023, Medicare’s annual spending would be well in excess of $1 trillion. While Heritage would raise the age of Medicare eligibility to 68, the House Budget proposal would raise it to 67. While the Heritage proposal caps Medicare spending at CPI plus 1 percent; the House Budget proposal caps it at GDP plus 0.5 percent. While Heritage would end taxpayer subsidies for Medicare premiums for the wealthiest cohort of Medicare recipients, the House Budget proposal retains them. The Heritage plan is clear on the delineation of the authority of the CMS and confines the agency to the administration of traditional Medicare; the House Budget proposal is unclear on the specific role of CMS in the administration of the new premium support program.
The Burr–Coburn Plan
Senators Burr and Coburn have also proposed a comprehensive reform of Medicare that would include changes to traditional Medicare while putting the program on a glide path to premium support.[33]
Traditional Medicare. Before Medicare transitioned fully to premium support in 2016, Burr and Coburn would make several immediate changes to the current program. First, they would provide all retirees with a Medicare catastrophic benefit, combined with a more sensible system of cost sharing and deductibles for hospitalization and physicians services. Cost sharing and deductibles in Medicare Parts A and B would be unified and restructured. There would be a single annual deductible for Parts A and B, and a 20 percent coinsurance for all services initially capped at $5,500 annually. At that amount, the coinsurance for services would be reduced from 20 percent to 5 percent, until annual out-of-pocket payments reached $7,500, the standard catastrophic cap. Medicare would then reimburse all covered expenses above $7,500.
These cost-sharing changes would be combined with Medigap reform. Under the Burr–Coburn plan, Medigap plans would not cover the first $500 of a retiree’s cost sharing in traditional Medicare, and coverage above $500 would be limited to 50 percent of retiree cost sharing.[34] Ending the current practice of using supplemental insurance to provide “first dollar” coverage of Medicare benefits would reduce both beneficiary premiums and taxpayer costs.[35]
The Burr–Coburn plan also makes several other changes to traditional Medicare. First, while it would maintain the four existing income thresholds for higher premium payments among wealthier seniors (starting with individuals who have an annual income in excess of $85,000 annually, and $170,000 for retired couples), the plan would expand “means-testing” by adding a three-tiered set of cost-sharing requirements on upper-income retirees. For the first higher income tier (individuals who earn more than $85,000; couples who earn more than $170,000), their annual out-of-pocket cap would be raised to $12,500; for the second tier (individuals at $107,000; couples at $214,000), the cap would be $17,500; for the third tier (individuals above $160,000; couples above $320,000), the cap would be $22,500. For retirees with annual incomes in excess of $1 million (about 60,000 people), the plan makes one addition: These retirees would pay full Medicare premiums.
Burr–Coburn would raise the standard Medicare Part B premiums from 25 percent to 34 percent of total premium costs over three years. The Senators say that the impact would be on the order of roughly $15 to $20 per month.[36]
Burr–Coburn would freeze the SGR for physician payments and end it in 2016 with a transition to the new Medicare premium support program. Under current law, Medicare physicians are faced (in March 2012) with a 27 percent payment cut. If Congress overrides current law and Medicare physician payment rates remain unchanged, Medicare outlays will be $316 billion higher between 2013 and 2022, estimates the CBO.[37]
Finally, the Senators would gradually raise (also by two months annually) the standard age of eligibility from 65 to 67. Under their proposal, the new normal age would be established by 2027, and it would thereafter be indexed to changes in life expectancy. The new eligibility age would not affect eligibility based on disability.[38]
During the transition to premium support, Burr–Coburn would also repeal the Independent Payment Advisory Board (IPAB), that would, govern Medicare reimbursement. And, it would add a temporary benefit: “voluntary care coordination.” The new benefit would be targeted at high-risk seniors who need special care or disease management due to chronic or debilitating conditions.
New Medicare. Beginning in 2016, the government would make its initial payment to health plans based on Medicare spending for Parts A and B in 2015. In 2017, and thereafter, the government would annually calculate its contribution based on regional, market-based bids for the provision of traditional Medicare benefits. The traditional Medicare FFS program would be forced to compete directly with private health plans. The bidding would be based on the provision of Medicare Part A and B benefits, or their actuarial equivalents, plus catastrophic coverage. Medicare Part D would remain separate.[39]
Like plan payment in the FEHBP, the government contribution, a fixed amount, would be based on the average weighted bid. Unlike the FEHBP, the government contribution would be further adjusted for income, with greater assistance for lower-income people and less for higher-income people. Also unlike the FEHBP, the government contribution would be adjusted for risk. This is the practice today in the Medicare Advantage program, modifying per capita Medicare payment to account for the varying costs attributable to health conditions among enrollees.
Finally, Burr–Coburn creates a Medicare Consumers’ Protection Agency (MCPA) to ensure a level playing field for plan competition. Modeled after the Office of Personnel Management’s (OPM) role in administering the FEHBP, the MCPA would “negotiate” with health plans, administer the bidding process and the risk-adjustment system, conduct an annual open enrollment, provide comparative information on plan offerings, and enforce rules for consumer protection. Consumer protections would include the enforcement of anti-discrimination rules in health insurance coverage, ensuring accuracy in marketing materials, and monitoring fraud and abuse.
There is, as yet, no independent econometric analysis or CBO scoring of the proposal. Powerful new economic incentives and intense competition in an environment of informed patient choice, Burr and Coburn say, will guarantee significant savings, ranging from $200 billion to $500 billion over 10 years.[40]
Similarities with Heritage. Like the Heritage proposal, Burr–Coburn changes the traditional Medicare program by adding a catastrophic benefit; reforming Medigap coverage; raising Part B premiums; expanding “means-testing” for upper-income retirees and phasing out taxpayer premium subsidies entirely for the wealthiest; imposing a freeze and then eliminating the SGR Medicare physician payment system; and raising the retirement age (to 67, instead of Heritage’s preferred 68) and indexing it to longevity.
For the new premium support system beginning in 2016, Burr–Coburn would force Medicare FFS to compete on a level playing field with private plans under uniform rules and consumer protections. Like Heritage, Burr–Coburn bases its government payment on the average weighted bid among regionally competing health plans, though Heritage moves from the average weighted bid to the lowest-cost bid or the average of the three lowest-cost bids in the second five years of the premium support program. Like Heritage, the Burr–Coburn proposal would also employ the risk-adjustment mechanisms currently established under Medicare Advantage. Heritage, however, also suggests the option of a risk-transfer pool, a “back-end” form of risk adjustment, to assure the stability of the market.[41] And, Burr–Coburn would establish a level playing field for health plan competition and consumer protection to be enforced by an independent body, the MCPA, similar to the Medicare Consumer Protection Commission recommended by Heritage, as another way to secure independence from CMS in program administration.
Differences with Heritage. Unlike Heritage, Burr–Coburn adds a new, though temporary, voluntary-care-coordination benefit to Medicare FFS. Unlike Heritage, it does not change the current income thresholds for upper-income persons who pay higher Parts B and D premiums. By expanding the scope of “means testing,” the proposal changes the form of increased payment by upper-income retirees: higher out-of pocket payments (cost sharing) by income categories, rather than by reducing taxpayer premium subsidies as prescribed in the Heritage proposal. Unlike Heritage, Burr–Coburn does not raise standard premiums for Medicare Part D to a fixed 35 percent of total premium costs, or change Part D in any way.
Unlike Heritage, the proposed MCPA charged with overseeing the competitive system, would “negotiate” with private plans, presumably the same way that OPM, as an employer, negotiates rates and benefits with private plans. In fact, Heritage specifically exempts the Medicare agency from the responsibilities that would apply to the federal government as an employer in “negotiating” the rates and benefits of health plans,[42] and would simply give the administrative agency the authority to certify plans for participation. The MCPA would also impose certain quality-reporting standards on private plans that Heritage does not require.
In contrast to Heritage and all other major Medicare-reform proposals, Burr–Coburn does not put Medicare on a budget or index its spending growth to inflation or to the general economy.
The Wyden–Ryan Plan
Senator Ron Wyden (D–OR) and Representative Paul Ryan (R–WI) have also outlined a major Medicare reform based on premium support.[43] Their plan differs in significant respects from the Ryan proposal embodied in last year’s House Budget Resolution.[44]
Traditional Medicare. Like other major proposals, the Wyden–Ryan plan calls for changes in the traditional Medicare FFS program. It would, for example, create a new catastrophic benefit and reform existing cost sharing in Medicare Parts A and B by providing for a uniform deductible. They also call for the replacement of SGR with a new physician-payment-update formula. Ryan and Wyden are not specific, however, beyond these basic descriptions.
New Medicare. Wyden and Ryan, however, are much more specific about the new Medicare program. Medicare premium support would begin in 2022.[45] In other words, there would be no change in Medicare for any person aged 55 years and above in 2012.
The Wyden–Ryan program would have other key elements.
First, Wyden–Ryan would create a Medicare exchange, a new arena for health plan competition. All health plans, including traditional Medicare, would compete within the exchange and participate in an annual process of competitive bidding—on a regional basis—to determine the dollar amount of the government contribution. Each plan would be required to cover at least the actuarial equivalent of the benefit package provided by fee-for-service Medicare. The bid of the second-least expensive plan in the region or fee-for-service, whichever is lower, would be the benchmark for the annual government per capita contribution to health plans in that region. If a retiree bought a plan with a premium cost above the benchmark, the retiree would pay the full additional premium cost. If the retiree bought a plan priced below the benchmark, the retiree would receive a rebate.[46]
The government contribution to plans in the exchange would be further adjusted for income. Wyden–Ryan would retain the same thresholds that exist today for higher premium payments for Medicare Part B and Part D benefits; and these thresholds would apply to premium payments for upper-income retirees purchasing health plans in the exchange. So, wealthier retirees would receive reduced taxpayer subsidies (a reduced government contribution) for their premiums, as they do today. Low-income retirees eligible for Medicaid would continue to have Medicaid payments of their out-of-pocket expenses, as they do today. Low-income persons who are not eligible for Medicaid would be eligible for additional federal assistance in the form of funded accounts to offset the cost of out-of-pocket expenses.[47] The government contribution would also be risk-adjusted; retirees with greater health care needs would secure higher per capita payments.
Second, Wyden–Ryan would retain existing Medicare insurance rules, meaning guaranteed issue of coverage, renewability and community rating, and it would greatly expand coverage options. Medicare beneficiaries would also be guaranteed (the actuarial equivalence requirement) at least the same level of benefits offered in traditional Medicare, but they would also be able to purchase more expensive plans and pay the extra cost. Medicare Advantage plans, for example, would be incorporated into the new premium support program, and Ryan and Wyden envision retirees taking their employment-based plans into retirement with them.[48] Intense competition on a level playing field among health plans ensures that they will offer services at a price that is closer to the actual costs of providing those services. With competition on a level playing field, health plans would have powerful market incentives to offer a variety of benefits at the lowest possible cost.
Third, Wyden and Ryan establish an institutional framework for consumer protection and plan competition. They insist that their plan will have the “toughest consumer protections in American government.”[49] To accomplish this goal, Wyden–Ryan divide administrative and oversight responsibilities for the new competitive system between the Office of Personnel Management and the Centers for Medicare and Medicaid Services. OPM would be responsible for the administration of the Medicare exchange, and would provide retirees with comparative information on their health plan choices, conduct annual enrollment in health plans, distribute comparative information and enforce insurance rules. CMS would be responsible for review and approval of the bids, benefits, and the administration of the risk-adjustment program.[50] They also say that CMS would have the power to “weed out junk plans” and “unqualified insurers.”[51]
In administering the risk-adjustment program, CMS would review the enrollment profiles of competing health plans, thereby providing data for implementing an internal cross-subsidization of risk. Those plans with above average numbers of low-risk enrollees would subsidize health plans with above average numbers of high-risk enrollees. In other words, CMS would assess fees on low-risk plans and use those fees to offset the costs of plans with disproportionate high-risk enrollment.[52]
Finally, Medicare spending, no longer on automatic pilot, would be put on a budget, effective in 2023. Wyden and Ryan emphasize, however, that their budget cap is a “fallback” mechanism. It is designed to guarantee savings and to foster positive incentives within the new competitive system in order to secure more efficient delivery of health care.[53]
In Wyden–Ryan, the rate of growth of Medicare spending is capped at GDP plus 1 percent.[54] If Medicare expenditures exceed the growth target, Wyden–Ryan would require a variety of congressional measures to slow the growth in Medicare costs; they caution, though, that such actions should not be allowed to weaken the competitive model. In the language of their proposal, “Congress would be required to intervene and could implement policies that change provider reimbursements, program overhead, and means tested premiums.”[55] If costs rise faster than the cap, most Medicare beneficiaries will have to pay higher premiums, for example, but they will also have strong economic incentives to choose lower-cost plans and spend wisely. At the same time, Wyden–Ryan would “hold harmless” dual-eligibles from any premium increase.
As of the publication of this paper, Wyden and Ryan have not produced savings estimates for their proposal. But Professors Bryan Dowd and Roger Feldman of the University of Minnesota, and Professor Robert Coulam of the Simmons College School of Management in Boston, estimate that the Wyden–Ryan competitive bidding proposal could achieve a ten-year savings of $339 billion.”[56]
Similarities to Heritage. Like Heritage, Wyden–Ryan would make certain major changes in traditional Medicare: the creation of a catastrophic benefit, the reform of cost sharing, and reform of the SGR Medicare physician-payment-update formula. Like Heritage, Wyden–Ryan would base the government contribution in the new premium support program on market-based competitive bidding, forcing traditional Medicare to compete head-to-head with private plans. Like Heritage, Wyden–Ryan retains Medicare’s existing insurance rules: guaranteed issue, guaranteed renewability of coverage, and community rating. Like Heritage, Wyden–Ryan would also include a risk-adjustment mechanism to ensure market stability, so that enrollees who are older and sicker will be able to remain in plans of their choice, and so that those plans enrolling high-risk beneficiaries will be able to remain competitors in the market.
The Wyden–Ryan risk-adjustment mechanism (a single pool of funding with a redistribution of subsidies among the plans themselves) also broadly resembles the Heritage Foundation’s proposal for a risk-transfer pool, but, there are some crucial differences in detail. Like Heritage, Wyden–Ryan would also provide lower taxpayer subsidies to high-income beneficiaries by requiring these beneficiaries to pay higher premiums. Like the Heritage plan, the Wyden–Ryan proposal would also put Medicare on a budget, just like other government programs. As a goal and function, both Heritage and Wyden–Ryan create the Medicare budget as a “fall back,” a fail-safe mechanism to protect taxpayers, and rely primarily on the market forces of choice and competition to control program costs.
Differences with Heritage. The Heritage proposal would have Congress transition to premium support beginning in 2016; Wyden–Ryan would not begin premium support until 2022.[57] This is a major difference; the Heritage plan would encompass a much larger number of baby boomers, who present the greatest single cost and demographic challenge to the Medicare program.
While both Heritage and Wyden–Ryan would put Medicare on a budget, Heritage would index spending growth to CPI plus 1 percent; Wyden–Ryan would use GDP plus 1 percent. Heritage would also tighten the income threshold for premium differentials (lowering them) for upper-income retirees; Wyden–Ryan would simply retain the thresholds of current law. Heritage would raise the age of eligibility; Wyden–Ryan would not.
In contrast to the process of automatic spending cuts ordained by current law on the recommendations of IPAB, both Heritage and Wyden–Ryan would reaffirm direct congressional control over spending.[58] But in curtailing excessive spending, Wyden–Ryan outlines certain congressional actions, including greater means-testing, reductions in overhead, and provider reimbursement cuts. From their text, the scope of this congressional authority is unclear. It is unclear whether congressional action over provider reimbursements, for example, would be confined to the traditional Medicare plan or whether Wyden–Ryan would authorize intervention into private health plans’ contract negotiations with medical professionals or the internal management of health insurance plans. Heritage, on the other hand, is explicit: There would be no such federal interference in medical practice or pricing, and there would be no interference with market negotiations between doctors, hospitals, and health plans.[59]
While Heritage and Wyden–Ryan include a risk pool to cross-subsidize health plans with higher than average health care costs due to less healthy enrollees, Heritage would leave the governance of the pool—its premium determinations and the redistribution of risk premiums—in the hands of insurers themselves; Wyden–Ryan would delegate this risk-adjustment function to CMS. Heritage would centralize the administration and oversight in one independent agency; Wyden–Ryan would divide this responsibility between OPM and CMS. Moreover, Wyden–Ryan would give CMS the duty to approve plan bids and expel substandard plans from competition, even though CMS would presumably still manage traditional Medicare as a competitor in the exchanges. The danger of this arrangement is that it would conflate the CMS roles of umpire and player, constituting a potentially serious conflict of interest.
The Domenici–Rivlin Plan
The Domenici–Rivlin proposal, also referred to as the Bipartisan Policy Center proposal, would change both the traditional Medicare program, as well as transition Medicare into a premium support system in 2016.[60]
Traditional Medicare. Beginning immediately, Domenici–Rivlin would raise the beneficiary share of Part B premiums, at the rate of 2 percent per year, from 25 percent to 35 percent of total Part B premium costs over five years. Existing protections for low-income beneficiaries would be retained. The existing thresholds for high-income seniors who pay Part B premiums—at levels ranging from 35 percent to 80 percent of total premium costs—would also be retained.
Domenici–Rivlin would also “modernize” traditional Medicare’s benefit and co-payment structure. This would be accomplished by adding catastrophic coverage to Medicare, adding a co-payment for home health services, increasing the cost sharing while reducing the “very high deductible” for hospitalization. Specifically, the proposal calls for a uniform deductible for Parts A and B of $560, and a uniform co-insurance rate of 20 percent on all Medicare services, and a catastrophic cap on out-of- pocket expenses of $5,250. The IPAB, created under the Patient Protection and Affordable Care Act (PPACA), would review the benefit structure every two years, and make recommendations for improvements. The authors expect that these changes will reduce retirees’ reliance on costly Medigap insurance.[61]
For Medicare Part D, the drug program, Domenici–Rivlin would alter private negotiation between drug manufacturers and private insurers on single-source drugs (drugs that are not available as generics) and impose the Medicaid-style rebates, as specified in the PPACA, requiring drug companies to kick back a certain amount to the government for participating in the program.
For Medicare Part A, Domenici–Rivlin would alter the hospital payment formulas and institute “bundling” of payments to hospitals for comprehensive treatment of patients. In other words, hospitals would receive a larger diagnosis-related group (DRG) payment for treatment of a medical condition if the hospital treatment also covers the cost of post-acute care of the patient. This payment change would reduce incentives for hospitals to discharge patients too quickly, sending them to nursing homes. Domenici and Rivlin believe this payment change would encourage coordinated care for these patients, better outcomes, and fewer re-admissions.
New Medicare. The new Medicare premium support program would commence in 2016.[62] The government payment to health plans would be based on regional bidding among health plans, including traditional Medicare, to provide traditional Medicare (A and B) benefits or their actuarial equivalents, and catastrophic coverage.[63] On the basis of that bidding, government payment would be based on the second-lowest bid in the region. That bid becomes the new benchmark bid for government payments to plans.[64] Beneficiaries who purchase a plan that is more expensive than the benchmark payment will pay the additional cost in premiums. A beneficiary who enrolls in the plan with the lowest bid will receive a full rebate equal to the difference between the benchmark and the premium cost of the plan. This would be a vast improvement over the flawed payment system that now governs Medicare Advantage.[65]
Domenici–Rivlin would also include a risk-adjustment mechanism to stabilize the competitive market and to accommodate differences in health among Medicare beneficiaries who enroll in the competing plans, including traditional Medicare. In designing a risk-adjustment system, Domenici–Rivlin calls for the creation of a single pool for participating plans, and an annual retrospective adjustment of payments to stabilize the market among a wide variety of health plans that might have enrolled an unbalanced mix of healthier and sicker individuals.
On the issue of income-based adjustment of Medicare subsidies, Domenici–Rivlin retains existing thresholds, at which upper-income retirees pay more for their health coverage: starting at $85,000 for singles and $170,000 for couples. It also freezes the indexation of these thresholds until 2020.
Like most Medicare-reform proposals, Domenici–Rivlin would put Medicare on a budget to restrain federal spending and medical inflation. Annual Medicare spending would be indexed to economic growth, GDP plus 1 percent.[66] If Medicare costs exceed that limit, Medicare eligible beneficiaries would pay higher premiums. Medicaid beneficiaries would be protected from premium increases and be guaranteed access to traditional Medicare without paying higher premiums.
Domenici–Rivlin apparently authorizes CMS[67] to create a “Medicare exchange” to administer the bidding process, oversee an annual enrollment in health plans, provide comparative information to beneficiaries on their plan options, to enforce traditional Medicare insurance rules (guaranteed issue and community rating), oversee benefit requirements, and administer the risk adjustment program. While these responsibilities are fairly standard, the CMS governance role is problematic.[68]
Based on estimates of the Bipartisan Policy Center, the Domenici–Rivlin premium support portion of their comprehensive budget reforms would result in substantial cumulative savings. Between 2016 and 2025, the reforms’ savings would amount to $409 billion; by 2030, $1.025 trillion; and by 2040, $4.05 trillion.[69]
Similarities to Heritage. The Domenici–Rivlin proposal to raise Part B premiums from 25 percent to 35 percent tracks the original CBO recommendation and is identical to that prescribed by Heritage. Like Heritage, Domenici–Rivlin also recommends the addition of catastrophic coverage and cost-sharing reforms with a view to reducing beneficiary reliance on costly Medigap.
In designing the regional competitive bidding process for Medicare premium support, benchmarking government payment to the second-lowest cost plan is broadly similar to the Heritage approach in the second five years of the implementation of Heritage’s proposed financing. But Heritage would then base the premium support payment on the lowest-cost plan, or alternatively, the average of the three lowest-cost plans.
Domenici–Rivlin would retain current insurance rules, and propose a retrospective risk-adjustment mechanism to stabilize the market; Heritage endorses the same approach, but also recommends application of an improved prospective risk-adjustment system, based on the Medicare Advantage model, as well as a back-end risk adjustment, for extra protection from adverse selection in the new health insurance market.
Differences with Heritage. While Heritage adds a special premium to reduce Part A deficits, Domenici–Rivlin proposes bundled payment to increase the efficiency of care delivery in Part A. More important, Domenici–Rivlin would favor application of the Medicaid rebate system for Part D; Heritage strongly opposes such a policy.
Heritage also favors setting Part D beneficiary premium payment at 35 percent of total premium cost; Domenici–Rivlin offers no such recommendation. While Heritage calls for tightening and indexing the income thresholds for taxpayer subsidies for Parts B and D and the new premium support system, and for phasing out taxpayers subsidies entirely for the wealthiest retirees, Domenici–Rivlin would retain existing thresholds, but temporarily suspend indexing them. While Heritage would index Medicare spending increases to inflation (CPI plus 1 percent), Domenici–Rivlin would index it to economic growth (GDP plus 1 percent).
While Heritage calls for administering the premium support program through an independent Medicare Center for Drug and Health Plan Choice, with a wall of separation between the center and the CMS’s administration of traditional Medicare, Domenici–Rivlin puts CMS in charge of running the new “Medicare exchange,” even as it still sponsors traditional Medicare. In other words, there would be no clear separation between the administration of traditional Medicare and the new competitive system—creating a potentially serious conflict of interest.
The Lieberman–Coburn Plan
Senators Lieberman and Coburn have outlined a series of major Medicare changes, though these are confined to reform of the traditional Medicare FFS program.[70]
First, they would create a Medicare catastrophic benefit combined with a simplification of Medicare cost sharing. They would impose an annual cap of $7,500 on a beneficiary’s total out-of-pocket spending, and they would streamline Medicare’s confusing set of cost-sharing arrangements. Specifically, Medicare’s current set of co-payments and deductibles would be replaced with a single deductible ($550 annually) for Medicare Parts A and B—hospital and physicians services. Medigap companies would still be able to offer supplemental coverage, but that additional coverage would be limited to 50 percent of the Medicare co-insurance up to the catastrophic cap of $7,500. Medigap would also not cover the initial $550 of a beneficiary’s cost sharing.
Second, Lieberman and Coburn would gradually increase beneficiaries’ standard Medicare Part B premiums from 25 percent to 35 percent of total premium costs. The standard premiums for physician and drug benefits would thus increase by 2 percent per year for five years. Practically, the Senators say, this would mean an extra savings of $15 to $20 per month per beneficiary; but it would also reduce the large and growing taxpayer subsidies in these voluntary parts of Medicare, which are financed by regular draw-downs of general revenues from the Treasury. Under current law, beneficiaries pay just 25 percent of their premiums, while taxpayers pick up 75 percent of the costs through general-revenue transfers. The Senators’ proposed increase of standard premiums, it should be noted, falls far short of the much stiffer requirement imposed in 1966: Medicare beneficiaries originally paid 50 percent of the costs of their Part B benefits.
Third, they would expand Medicare’s current income-related cost sharing for Parts B and D for the very wealthy. The proposal is almost identical to that embodied in Burr–Coburn. Currently, Medicare imposes higher premium requirements for upper-income beneficiaries. In 2011, for example, while the standard monthly Part B premium was $115.40, it was $369.10 for someone with an annual income of more than $214,000.The Senators would build on this policy. They would do so, however, by raising out-of-pocket caps for wealthy beneficiaries. For example, while the standard out-of-pocket cap would be $7,500 for almost all beneficiaries under their proposal, the cap would increase to $12,500 for persons with annual incomes between $85,000 and $107,000; $17,500 for persons with annual incomes between $107, 000 and $160,000; and $22,500 for persons with annual incomes between $160,000 and $213,000. These out-of-pocket caps for upper-income beneficiaries would be combined with a crucial change in premium payment. Individuals with annual incomes in excess of $150,000 and couples with annual incomes in excess of $300,000 would also pay the full cost of their Medicare Part B and Part D premiums.[71]
Fourth, the Senators would gradually increase Medicare’s age of eligibility to 67. This target age would be reached by 2025, raising the retirement age by two months every year for those born in or after 1949.
Finally, they would permanently fix the flawed SGR system, and make a number of miscellaneous program changes. The Senators propose a three-year “doc fix” financed by savings generated from the other policy changes embodied in their proposal, as well as a reduction of taxpayer subsidies to hospitals for bad debts and improvements in Medicare administration to reduce the waste, fraud, and abuse that plagues the program.
The Senators have projected 10-year savings based on recent and past CBO estimates of the particular policy changes included in their proposal. On that basis, they project that their proposal would reduce total Medicare spending by more than $600 billion, and cut the program’s 75-year unfunded liability by approximately $10 trillion.[72]
Similarities to Heritage. As policy initiatives, the addition of a catastrophic benefit, the cost-sharing and Medigap reform, the expanded application of income-related taxpayer subsidies, a gradual increase in Medicare Part B and D premiums, the elimination of taxpayer subsidies for the wealthiest beneficiaries, and the increase in the age of eligibility are all major policy prescriptions that are either identical (as in the premium increases) or broadly similar to those advanced by The Heritage Foundation.
Differences with Heritage. The differences with Heritage on reforming the existing Medicare program are confined to certain details. For example, the policy of making upper-income retirees pay more for their benefits would be based on the annual income thresholds under current law (starting at $85,000 for individuals, and $170,000 for couples), whereas the Heritage proposal would start at $55,000 for individuals and $110,000 for couples. Heritage would apply the higher payment requirement for upper-income retirees to a reduction in taxpayer subsidies for premium payments; the Senators would mostly accomplish larger upper-income payments through increases in cost sharing. As previously noted, the proposed Heritage age of eligibility is 68; the Senators set it at 67. Heritage freezes physician payment for five years; the Senators freeze it for three years.
The Senators include an ambitious program to combat waste and fraud in traditional Medicare and recover bad hospital debts; Heritage has not proposed such initiatives. There are also certain Heritage policy prescriptions absent from Lieberman–Coburn: the abolition of current restrictions on Medicare private contracting and Medicare payment for physician-owned specialty hospitals.
Conclusion
The Affordable Care Act mandates massive cuts in government funding for hospitalization and related benefits. Physicians will be subject to an unrealistic and unsustainable Medicare payment-update formula divorced from the real conditions of medical supply and demand; it is a formula that routinely threatens them with draconian payment cuts, and even more extensive Medicare payment cuts are to be implemented at the hands of the unelected IPAB, an unaccountable panel unrestrained by either administrative or judicial review. With Medicare reimbursement for doctors and hospitals controlled, and set on a downward trajectory, even dipping below the very low Medicaid payment levels, current and future retirees are guaranteed reduced access to care.
Medicare premium support is the best single alternative to an otherwise ugly Medicare future. While details differ, all major reform proposals are in accord with the Heritage Foundation plan, as outlined in Saving The American Dream, in requiring traditional Medicare to compete with private plans, using competitive bidding to determine market-based payments to health plans, requiring upper-income retirees to pay more for their benefits, providing extra assistance to lower-income enrollees, and adding a risk-adjustment mechanism to guarantee market stability and security for older and sicker retirees. The breadth of the consensus on key policy components could be the basis for a strong bipartisan agreement. As Senator Wyden has observed, “Absent a bipartisan effort to fix Medicare and protect this guarantee—if nothing is done—what the years ahead ensure is that seniors and health care providers will be getting a steady diet of cost shifting and arbitrary cuts until the Medicare guarantee is kaput.”[73]
Medicare is at the center of the debate on federal entitlement spending. A failure to reform Medicare, and thus control entitlement spending, will rob Americans of a fleeting opportunity to escape ruinous debt, crushing taxation, or severe austerity measures. Failure also guarantees a poorer future for the next generation, denying millions of young working families the chance to enjoy the same economic opportunities in a prosperous America. By taking action to avert financial and economic crises, Congress would be engaged in nothing less than a historic project to save the American dream.
—Robert E. Moffit, Ph.D., is Senior Fellow in the Center for Policy Innovation at The Heritage Foundation.



