In 2003, the Medicare Modernization Act added a publicly funded prescription drug benefit to Medicare. Known as Part D, the program was a major expansion of Medicare. Economists Gary Engelhardt of Syracuse University and Jonathan Gruber of the Massachusetts Institute of Technology have examined the degree to which the new and subsidized drug coverage replaced existing private drug coverage, and the degree to which public spending replaced the costs previously borne by seniors. The Heritage Foundation’s Center for Policy Innovation distills the research findings.
Medicare Part D significantly changed the mechanism and scale of public subsidies for prescription drugs. The introduction of Part D had equally significant consequences for the private market for drug coverage, seniors’ out-of-pocket spending for medications, and the demand for prescription drugs. In an important new paper, economists Gary Engelhardt of Syracuse University and Jonathan Gruber of the Massachusetts Institute of Technology examine the magnitude of these effects and include a preliminary calculation of the added “welfare”[1] for seniors resulting from Part D drug coverage.[2]
The Medicare Prescription Drug, Improvement, and Modernization Act of 2003 amended the universal public insurance program for seniors to include prescription drug benefits, widely referred to as Part D. When Medicare Part D was enacted, it was heralded as one of the most significant expansions of public insurance in over a generation. Seniors spend considerably more on prescription drugs than the rest of the population. Nearly 30 percent of seniors enrolled in Medicare paid out of pocket for their prescriptions before Part D. The more than 70 percent of Medicare seniors with prescription drug coverage (about half of the elderly population) were covered by private plans, mostly through their current or former workplaces. The rest, mainly low-income seniors, were covered predominantly by Medicaid.
Engelhardt and Gruber explore several consequences of Part D, including the increase in the number of seniors with drug coverage, a reduction in average out-of-pocket spending, and an increase in average public expenditures for prescription drugs. By comparing those just under age 65 to those 65 and over, Engelhardt and Gruber estimate that Part D was responsible for increasing prescription drug coverage among seniors by 10 percentage points. But this increase accounts for only a quarter of the new population with public drug coverage, suggesting that the remaining 75 percent of those who are newly publicly insured were covered by private drug coverage before Part D.
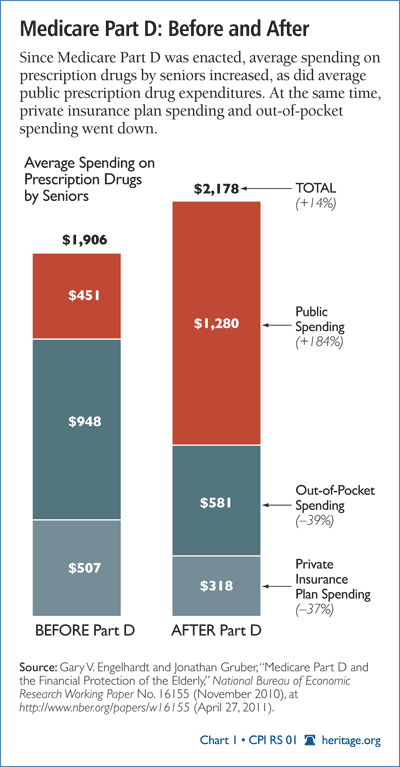
Engelhardt and Gruber find similar levels of “crowding out” of private spending by public spending. They note that although seniors spent an average of $525 more per year on drugs after implementation of Part D, average public expenditures went up by about $2,100. According to the authors, this means that “each dollar of public expenditure raises total expenditure by roughly 25 cents or that there is about a 75% crowd-out.”[3] Most of the crowd-out is the result of lower privately insured prescription drug spending, while every dollar increase in public spending is associated with a fall of about 42 percent in private spending. The rest of the crowd-out—more than 30 cents for every public dollar spent on prescription drugs—is associated with less out-of-pocket spending.
Another important finding of the study is that the level of crowd-out has been larger for those who are more likely to have private drug coverage (determined by their income and other demographic characteristics) than for those who are unlikely to have private drug coverage. In fact, those with a lower likelihood of private drug coverage (less than a 50 percent probability) are estimated to experience only 50 percent crowd-out, whereas those with a higher probability of having private drug coverage (greater than or equal to a 50 percent probability) are more likely to be crowded out by public insurance. Such differences in the elasticities and crowd-out effects of various populations are essential to analysts interested in simulating the effects of future public insurance coverage expansions.[4]
With the magnitude of private spending crowd-out being so high, Engelhardt and Gruber conclude their paper by asking how the deadweight loss of financing Medicare Part D with tax revenue compares to the gain in welfare among Medicare enrollees.[5] The authors argue convincingly that it is easy to imagine a situation where the welfare of Medicare beneficiaries is increased by Part D—even when subjected to the high level of crowd-out—since so much of the crowd-out is driven by a reduction in out-of-pocket spending, thus implying a reduction in the financial uncertainty faced by beneficiaries. Furthermore, according to the authors, if the increase in average spending by seniors after Part D reflects a tendency for Medicare beneficiaries to buy necessary prescription drugs that in the past they had typically avoided purchasing, one might well expect the group’s welfare to improve.
The authors estimate the impact that Part D had on the welfare of Medicare beneficiaries by calculating the change in the risk premium associated with lower out-of-pocket spending. This risk premium is ultimately derived as a function of individual income, the amount of out-of-pocket spending, and the level of risk aversion.
Although the authors estimate the median additional welfare to be about $170 for those who signed up for Part D coverage, the average welfare gain was nearly $450, indicating that those with high out-of-pocket costs benefited a great deal from Part D. In fact, the study estimates that seniors with out-of-pocket costs in the top 10 percent of the out-of-pocket distribution with Part D benefited so much in terms of additional welfare that the aggregate welfare gained is likely equivalent to the deadweight loss of financing Part D. The authors note that these calculations do not include potential health benefits accrued from increased prescription drug use. Engelhardt and Gruber conclude that Medicare Part D is at worst a wash—at least in terms of economic efficiency.
Summary of Findings
- Medicare Part D crowds out private prescription drug coverage and expenditures for seniors by 75 percent.
- Medicare Part D increased overall spending on prescription drugs by seniors but also reduced their out-of-pocket spending.
- Part D reduced the average out-of-pocket spending risk for seniors by about $450 for those with public drug coverage. However, seniors with expenses in the top 10 percent of the out-of-pocket distribution gained a great deal more from Part D coverage than was gained by seniors with lower drug expenses.
- The deadweight loss from taxes used to finance Part D coverage and the benefits to seniors from Part D are likely close equivalents.
—Paul L. Winfree is a Senior Policy Analyst in the Center for Data Analysis at The Heritage Foundation.


