Obamacare increases enrollment in the troubled Medicaid program by over 20 million persons. However, providers are already limiting the amount of Medicaid patients they accept because of low payment rates. To entice providers to accept more Medicaid recipients, Obamacare requires that states—with federal dollars—raise primary care physician (PCP) payment rates for Medicaid to parity with Medicare rates for 2013 and 2014.
Based on estimates from the Congressional Budget Office (CBO) and the Office of the Actuary at the Centers for Medicare and Medicaid Services (CMS), the 10-year cost of raising PCP rates to Medicare levels would be between $37 billion and $68 billion. The Heritage Foundation estimates that the 10-year cost could rise to $350 billion if state reimbursement rates were to rise proportionally for all physician and clinical services.[1]
These Obamacare provisions raise potent issues for providers and policymakers: Will states raise provider rates across the board to match the PCP increase? What actions will states take when the federal funding expires and how will those actions impact doctors? Will Congress adopt a different model for Medicare payment rates than the current one, which requires temporary fixes about once a year?
Medicaid's Numerous Problems
Medicaid—the joint federal–state health insurance program for numerous categories of the poor—has significant problems. Medicaid spending growth is unsustainable, increasing over 6 percent annually (in inflation-adjusted dollars) during the past two decades.[2] Medicaid growth has resulted in three federal bailouts in the past decade, and its growth is crowding out other state priorities, such as education, transportation, and law enforcement.
At the same time, several states reimburse providers at extremely low rates. This causes many providers to refuse to treat Medicaid patients, effectively forcing Medicaid recipients to use emergency rooms for basic care. According to the Texas Health and Human Services Commission, less than a third of the state’s practicing doctors are active in Medicaid.[3]
Furthermore, Medicaid recipients likely receive a lower quality of care than privately insured patients and perhaps even the uninsured. For example, a study of nearly 900,000 major surgeries in the U.S. found that patients on Medicaid were 13 percent more likely to suffer in-hospital mortality than uninsured individuals, controlling for a plethora of factors.[4]
Obamacare Substantially Increases Medicaid
Despite Medicaid’s enormous problems, Obamacare expands it dramatically. Beginning in 2014, states are required to cover all individuals below 138 percent of the federal poverty line with Medicaid.[5] The CMS estimates that this will increase enrollment in Medicaid by 23 million individuals in 2014 at an added annual cost of over $70 billion.[6]
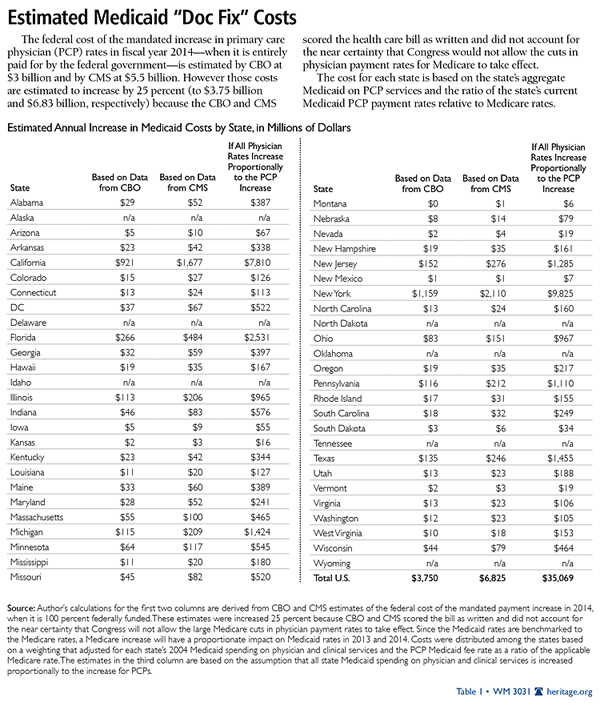
Obamacare requires that states increase Medicaid reimbursement rates for PCPs to applicable Medicare payment rates for 2013 and 2014 to encourage PCPs to treat Medicaid patients. The estimated annual cost of raising the reimbursement rates by state is provided in Table 1. However, on January 1, 2015, both the mandate and the federal funding paying for it expire.
Many Medicaid providers, who are paid on average about half of commercial rates, are skeptical of this expansion. Medicaid requires an enormous amount of paperwork, the lag time between date of service and the date of reimbursement is more than twice as long as Medicare or commercial insurance reimbursement times, and the denial rate for Medicaid claims is three times larger than for both Medicare and commercial insurance.[7] Indeed, only 10 percent of PCPs believe that new Medicaid enrollees in their area will find a suitable PCP.[8]
The Problem with Tying Rates to Medicare
Medicare’s payment rates to doctors are a central political issue nearly every year. To deal with skyrocketing Medicare costs, Congress enacted the Sustainable Growth Rate (SGR) in 1997. SGR links the increase in Medicare reimbursement rates to growth in GDP. Since medical costs historically increase at a rate more than twice GDP, the SGR reduces the real (inflation-adjusted) payments physicians receive. Congress has overruled this decrease (the so-called “doc fix”) 10 times over the past decade, with short-term boosts in Medicare rates above SGR levels.
When prices are set by government, special interests have powerful incentives to devote valuable time and money lobbying to influence those prices. This intensifies conflict among providers, policymakers, patients, and taxpayers.
Furthermore, linking Medicaid reimbursement rates to Medicare rates is unlikely to solve the Medicaid access problem. For one, Medicare rates are scheduled to be cut 23 percent in December 2010 when the latest doc fix expires. With near certainty, however, Congress will provide another temporary fix. But even if Medicare rates are not cut, they still pay only an estimated 78 percent of commercial rates.[9] Because of these facts, less than half of PCPs report they would be willing to see new Medicaid patients even if Medicaid rates reached Medicare levels.[10]
What Happens to Doctors and States When the Federal Funding Disappears?
The end of federal assistance will leave states and doctors in a precarious position. If states keep the elevated PCP reimbursement rates, they will have to make up the difference with their own funds, further adding to state Medicaid costs. But if states reduce Medicaid PCP payment rates to their previous levels when the federal funding disappears, Medicaid beneficiaries’ access to providers would be further compromised. Medicaid reimbursement rates are already quite low, particularly in states such as New York, New Jersey, and California that pay providers approximately one-third of commercial rates.
Moreover, reducing physician payment rates is typically one of the primary ways state officials control Medicaid spending. For example, 41 states and the District of Columbia cut provider reimbursements rates in 2009 or 2010, and 29 states and the District did so in both years.[11] The mandated Medicaid expansion would strip states of the ability to reduce enrollment as a cost-controlling mechanism, so reductions in Medicaid reimbursement rates seem likely to continue, especially during difficult economic periods.
In addition, setting provider rates even lower will not necessarily reduce the aggregate costs of state Medicaid programs. More Medicaid enrollees will likely seek care in hospital emergency rooms because they cannot find doctors willing to accept them, and there will be an increased incentive for providers to “up-code” their payment to maintain their incomes.
A doctor’s time is better spent serving his or her patients than lobbying politicians for payment increases. And the heavy administrative burden of Medicaid is another cost inflicted on physicians and their practices, which considerably reduces their levels of job satisfaction and the likelihood they will accept new Medicaid patients.[12]
Fundamental Reform, Not More Money
When a federal program is hemorrhaging taxpayer dollars and delivering poor results, policymakers should reform it. Fundamental Medicaid reform is desperately needed. Market-based principles should be introduced to re-align incentives of doctors and patients so that quality can increase and cost can decrease. Instead of addressing the many problems of Medicaid, Obamacare doubles down on the broken program and greatly adds to its rolls.
Based on recent experience, many states will cut provider rates when they are faced with tough budgetary decisions and the federal money goes away. Doctors will be left to rely on “fixes” at the state-level similar to what Congress does continually with Medicare rates.
A better approach: Repeal the Medicaid expansion and stop these temporary fixes that produce uncertainty, division, and socially wasteful lobbying efforts and focus instead on how to best provide a social safety net within an affordable budget.
Brian Blase is Policy Analyst in the Center for Health Policy Studies at The Heritage Foundation and is a Doctoral Candidate in Economics at George Mason University.