Congress is about to set off a chain reaction that it has not planned for and will not be able to contain.
The health care legislation currently in Congress not only imposes new costs on states through expansion of the Medicaid program; it also preempts state authority in management of the program. Faced with becoming merely an agent of the federal government, states will likely take the rational and reasoned approach of simply ending the state–federal partnership known as Medicaid.
Nearly Every State Would Be Better Off
How individuals, employers, and others would react to the new health care legislation is unpredictable enough,[1] but how state governments would cope has been largely overlooked by Congress.
Also overlooked is the fact that state participation in Medicaid is entirely voluntary. Medicaid is fundamentally “a cooperative federal-state program through which the federal government provides financial assistance to states so they may furnish medical care to needy individuals. … [P]articipation in the program is voluntary.”[2] States opted into Medicaid, and they can opt out.
Congress clearly fears that with the creation of the new entitlement, states would respond by lowering Medicaid eligibility. Hence, both the House and Senate attempt to prevent such state action by imposing “maintenance of effort” (MOE) requirements on the states.
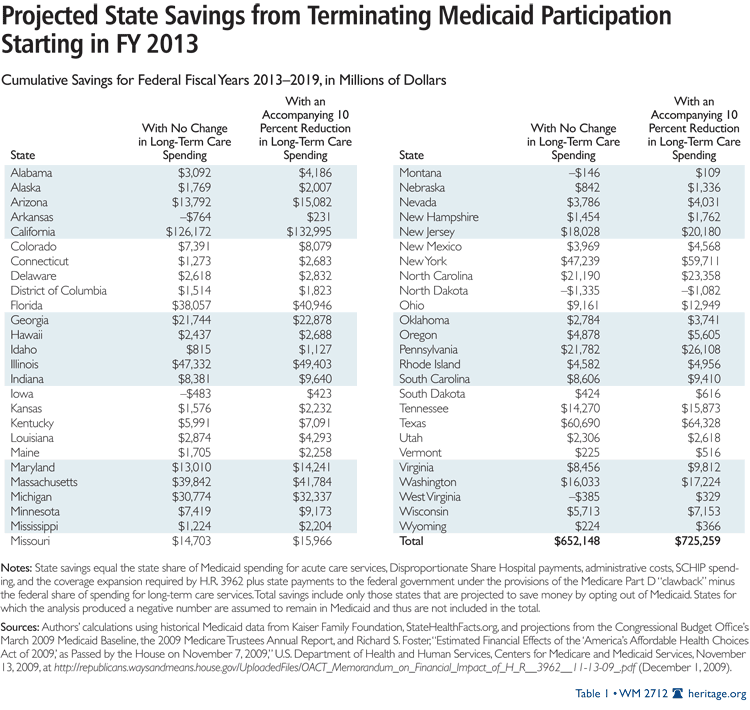
If all states withdraw from Medicaid, their collective savings would be $725 billion over the 2013–2019 period, but they would exceed $1 trillion over 10 years. This assumes that states will continue to spend at least 90 percent of what they spend now on Medicaid long-term care services with state-only dollars. On a state-by-state basis, every state except North Dakota would come out ahead financially by leaving Medicaid but continuing long-term care spending with state-only dollars. Of course, if North Dakota reduced its long-term care spending, it too would come out ahead.
The cost to the federal government to replace the state share of Medicaid, however, would be greater than $1 trillion as the entire Medicaid population would become eligible for the new, more expensive federal subsidies for premiums and cost-sharing. Moreover, the states would no longer pay for Medicare cost-sharing or the state “clawback” for Medicare prescription drugs.
The Lost Decade for States
The reasons states would seriously consider opting out of Medicaid are simple: They would no longer be able to afford Medicaid, and it is politically infeasible to have one quarter of a state’s budget controlled by Washington rather than the state capitol.
The health care legislation in both the House and Senate would require states to increase their Medicaid spending. Although the bills would provide additional federal funds for new proposed Medicaid populations, Congress does not seem to realize that states cannot afford the current Medicaid program.
Ray Scheppach, executive director of the National Governors Association, warns that “states will not fully recover from this recession until late in the next decade.”[3] To close their budget gaps, states have and will continue to cut spending for Medicaid, education, and other state priorities. Now that the federal government has committed itself to a massive new entitlement, states could solve their budget problems by simply getting out of Medicaid.
Congressional Miscalculation
The health care legislation creates a new federal entitlement to generous health care benefits funded with generous subsidies. For individuals at the lowest income levels, these subsidies will be worth more than $20,000 for a family of four. However, those eligible for Medicaid are not eligible for the new federal subsidies. The reason? Allowing subsidies to Medicaid-eligible individuals would bust the federal budget.
This exclusion of 60 million U.S. citizens currently on Medicaid from the new program has received virtually no public attention. In addition to the current Medicaid population, the House and Senate will require states to cover another 15–20 million individuals by establishing a new minimum federal income test. The House would require states to cover all individuals at or below 150 percent of the federal poverty level (FPL), while the Senate would require coverage at or below 133 percent of FPL.
It should be noted that states already have the authority to cover millions of these individuals who are the parents or caretakers of low-income children, and some states have already extended eligibility to these Medicaid populations at their own choice.
Buying State Silence
Medicaid financing is determined by a formula based on a per-capita income of a state compared to national per-capita income. The federal government sends more money to a “poorer” state like Louisiana than a wealthier one like Illinois. States receive no less than a 50 percent match rate from the federal government and potentially could receive as high as 83 percent. On average, states fund 43 percent of the Medicaid program.
Increasing Medicaid eligibility and other costs in the program would therefore increase state spending. Faced with state opposition to increased Medicaid costs, the House and Senate have tried out various enhanced matching rates to lower state liabilities.
However, states may receive substantially less money from the federal government than they expect based on how many current eligibles enroll in Medicaid (for whom there is no enhanced match) and how the MOE requirements are interpreted through rulemaking. States have billions of dollars at stake based on the MOE. Yet there has been virtually no discussion of this critical issue during the committee and floor debates in Congress.
Greater Federal Control as Well
The legislation would not only increase federal eligibility requirements; it would also increase federal control over the states. The House bill includes more than a dozen new provisions that would substitute federal requirements for state discretion.[4]
States will not understand the full impact of the federal takeover for years to come as regulations are written and litigation ensues. Section 2101 of the Senate bill would increase the federal match rate for the State Children’s Health Insurance Program (SCHIP) but would not add more money to state allotments. States would spend the federal dollars faster, thereby running out of SCHIP funds sooner.
What happens then? Section 2101(b)(1) adds a new MOE requirement that provides, “In the event that allotments … are insufficient … a State shall establish procedures to ensure that such children are provided coverage” (emphasis added). What does this mean? The authors know full well that the allotments would be insufficient because no new federal dollars are provided. They are setting up a future fight over what ensure means. States will certainly want a limited interpretation, such as making families aware of their options. But the Administration could broaden this interpretation through rulemaking, and the courts could broaden it even further. States could one day be stunned to find out that ensure means paying the cost of coverage with state funds.
Section 2304 of the Senate bill provides a new definition of medical assistance. Why, after more than 40 years of Medicaid history, does the Senate suddenly believe a new definition is needed in the program? And what is the impact? It could mean that the federal courts would be opened more broadly to allow individuals to sue states beyond what is currently allowed. States have won a number of court cases in recent years that have limited federal review.[5]
States are not expected to create providers where they do not exist beyond what is available to the general public. Perhaps after this language appears, they will be required to do so. Medicaid pays for access; will state officials become liable for outcomes? Arguments that have enabled states to prevail in court in the past may be washed away if this language becomes law. Congress surely intends the new language to mean something, and one can reasonably assume that it means an erosion of state authority.
The Rational Choice for States
By piling billions of dollars in new costs onto states and imposing greater federal control over the states, Congress is recklessly increasing the likelihood that states will exert their own authority as sovereign units of government and end their participation in Medicaid entirely.
The savings to state budgets are so enormous that failure to leave Medicaid might be viewed as irresponsible on the part of elected state officials. The federal government, however, would be left holding a trillion-dollar-plus tab.
Dennis G. Smith is Senior Fellow and Edmund F. Haislmaier is Senior Research Fellow in the Center for Health Policy Studies at The Heritage Foundation.



