Obamacare imposes a tax on health insurance premiums[REF] that will increase individual and small group health insurance premiums by an additional 2 percent to 3 percent in 2018.
After the 2017s moratorium ends,[REF] this tax will once again be imposed in 2018 and thereafter. The tax is projected to increase individual and small group health insurance premiums by an additional 2 percent to 3 percent in 2018. The tax will have an adverse impact on consumers and reduce employment but have little effect on large employers and their employees because large firms usually self-insure. The tax is hidden from consumers, and directly increases the cost of health insurance. Like the other Obamacare taxes, it should be repealed.[REF]
How the Health Insurance Tax Works
The Internal Revenue Service (IRS) calls the excise tax a “Health Insurance Provider Fee.”[REF] Opponents call it the health insurance tax (HIT).[REF]
The HIT is not imposed at a specified rate; rather, the effective rate is set annually by the Department of the Treasury to raise an amount of revenue specified by law.[REF] The amount of revenue that the Congressional Budget Office projects that the tax will raise is shown in Table 1.
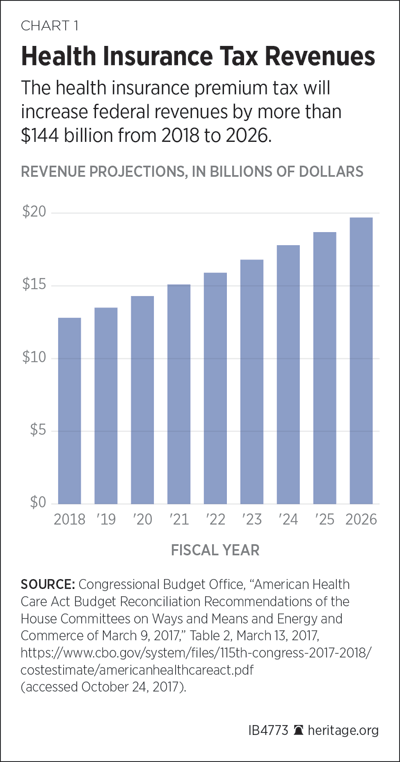
The amount of tax revenue raised will increase substantially over time. In 2026, the HIT is projected to raise 54 percent more revenue than it did in 2018.
The HIT is imposed on net health insurance premiums for any U.S. health risk to the extent that the insurer’s premiums exceed $50 million annually.[REF] The tax is not tax deductible, which raises its effective tax rate by 54 percent.[REF]
Most Large Employers and Their Employees Are Exempt
Employers that self-insure are explicitly exempted from the HIT.[REF] Most large employers self-insure, while most small employers do not. Thus, the HIT will affect almost exclusively small businesses and individual consumers. In 2015, 80.4 percent of employers with 500 or more employees were in self-insured plans; 30.1 percent of employers with 100–499 employees self-insured; and 14.2 percent of employers with fewer than 100 employees self-insured.[REF]
In general, with self-insured plans, the employer establishes and contributes money to a trust. Employee health care costs are paid in accordance with the trust or plan document. The employer will often use a third party to administer the health care plan. The plan usually uses a preferred provider network or other network of health care providers to contain costs. Small or mid-size employers that self-insure usually purchase stop-loss insurance that limits either their aggregate or per person losses or both. In all of these cases, self-insurers are exempt from the HIT.
The table below summarizes the findings of four studies of the impact of the HIT on health insurance premiums. Each study is clear that the HIT imposes more costs on consumers. However, the results vary to some degree because they:
- Consider different time periods;
- Use different data sources and estimates about the amount of health insurance premium revenue that insurance companies will have; and
- Employ different estimates about how many firms will move toward self-insurance rather than buying health insurance over time.
It is generally agreed that the economic incidence of the HIT will fall primarily on consumers and small employers.[REF] The higher costs that small employers face will tend to reduce employment. A study by the National Federal of Independent Business Research Foundation found that the health insurance tax will reduce private-sector employment by as little as 152,000 jobs and as much as 286,000 jobs in 2023.[REF]
Because of the HIT, the health insurance underwriting restrictions in Obamacare (notably the age bands limiting the ratio of the premiums for the oldest workers to no more than three times those for the youngest workers) and the Essential Health Benefits requirements for health insurance, an increasing number of employers will find self-insurance to be an attractive option under Obamacare. This effect will be particularly pronounced for employers with relatively young and healthy employee populations.
In fact, since Obamacare was enacted, the percentage of private-sector enrollees in self-insured plans has increased from 57.5 percent in 2010 to 60 percent in 2015.[REF] The proportion of small and medium-sized firms that self-insure has increased as well.[REF] Similarly, enrollment in fully insured employer group plans dropped by 8.6 million individuals, from 60.6 million at the end of 2013 to 52 million at the end of 2016 and the number of individuals in self-insured plans increased from 100.6 million in 2013 to 105.6 million in 2016.[REF] These effects would probably be larger but because the repeal of Obamacare seemed likely, some firms deferred moving toward an unfamiliar means of providing health benefits.
To the extent this movement toward self-insurance occurs, it will reduce the amount of premiums underwritten (i.e., the size of the taxable base for the HIT) and increase the required health insurance effective tax rate to raise the set dollar amounts that must be raised. The higher effective tax rate will increase the percentage by which premiums must increase in subsequent years.
A Hidden Tax
Because the HIT is collected from insurance companies, it is effectively hidden from health insurance buyers, including both individual consumers and small employers. However, because the HIT is functionally an excise tax, it directly increases premiums. Current estimates are that when the tax goes back into effect in 2018 it will increase premiums by an average of 2 to 3 percent. Even worse, that tax rate will further increase as more employers shift to self-insuring their plans, thus shrinking the tax base for the health insurance tax (which is applied only to policies purchased from commercial health insurers). That is because the law requires the IRS to extract fixed amounts of revenue from that tax base.
Those effects make the health insurance tax one of Obamacare’s more damaging taxes. As with the other Obamacare taxes, it should be repealed.
—David R. Burton is Senior Fellow in Economic Policy in the Thomas A. Roe Institute for Economic Policy Studies, of the Institute for Economic Freedom, at The Heritage Foundation.


