The response to the new coronavirus in the U.S. included severe social distancing measures, such as stay-at-home orders, broad-based school closures, and the closing of businesses deemed non-essential. The idea was to “flatten the curve,” thus spreading out infections over a longer period of time to prevent the hospital system from being overwhelmed. Put differently, this approach was designed to slow down the rate at which the epidemic spread, not to eradicate the disease or necessarily decrease the overall number of infections.REF
Virtually nothing was known about the virus at the onset of the outbreak, so this strategy was intended to help buy time for public health officials to prepare for an influx of patients. While much about the virus remains to be discovered, public officials are now in a much better position to formulate more-effective interventions. Unfortunately, instead of adapting their public health strategies to new knowledge about the disease, government officials have adapted their expectations of social distancing, increasingly viewing it as a solution, rather than a mere expedient.
Nearly five months have passed since the first known COVID-19 case was reported,REF and policymakers can now make much better decisions based on the weight of the existing evidence. This evidence does not provide policymakers with complete certainty, but such a standard is unattainable in virtually all scientific fields.
The evidence now shows that:
- The pandemic remains geographically concentrated,
- COVID-19 is primarily a threat to the elderly,
- Those with comorbidities face higher risks,
- Public officials are failing to protect those in nursing homes,
- The case fatality rate appears to be less than initially feared,
- U.S. hospital capacity has so far proven robust, and
- Widespread curbs on non-emergent care are ill-advised.
None of these facts should be used to trivialize the severity of the contagion or the number of lives that COVID-19 has claimed. This novel virus causes a lethal, highly contagious disease for which there is no vaccine or cure. It has so far claimed the lives of nearly 100,000 Americans, a death toll not seen since the Hong Kong flu (H3N2 virus) pandemic resulted in an estimated 100,000 U.S. deaths in 1968.REF But it is important to keep these overall figures in their proper context.
This Backgrounder provides an in-depth look at the evidence currently at the disposal of public health officials to deal with the coronavirus crisis, and recommends that, in light of these facts, policymakers should adapt their strategies to information that was not available to them when they instituted widespread lockdowns. The data show that policymakers should take the following actions:
- Replace widespread stay-at-home orders that treat all counties in a state the same with an approach that tailors policies to local circumstances;
- Implement enhanced, more traditional public health interventions in communities where infection rates are high—voluntary isolation facilities for the sick, contact tracing, testing, and some travel restrictions.
- Protect those who are at greatest risk—the elderly and those with underlying medical conditions;
- Protect those in nursing homes; and
- End statewide bans on non-emergent care.
Basic Virus Facts
There are 219 species of viruses that are known to be capable of infecting humans, and a large pool of unknown species is likely to exist.REF Ebola, measles, poliomyelitis (polio), yellow fever, and smallpox are all dangerous viruses, and smallpox alone killed approximately 300 million people in the 20th century.REF The 1918–1919 influenza (flu) pandemic infected an estimated 500 million people worldwide and killed approximately 50 million people, with 675,000 of those deaths occurring in the U.S.REF Overall, respiratory viruses are a serious health risk and they are “the most frequent causative agents of disease in humans.”REF
Nine known respiratory viruses, including the flu, commonly circulate among humans.REF During the past two decades, several new respiratory viruses, such as the severe acute respiratory syndrome (SARS) coronavirus (SARS-CoV), the avian influenza virus H5N1, and a novel influenza type A (the H1N1 “swine flu” virus), have also infected humans.REF In fact, the emergence of several novel influenza (type A) viruses resulted in four flu pandemics during the 20th and 21st centuries (in 1918, 1957, 1968, and 2009).REF Although there are currently four Food and Drug Administration (FDA) approved anti-viral drugs for influenza, the Centers for Disease Control and Prevention (CDC) warns that these drugs typically only lessen the severity of flu symptoms and shorten the length of illness by one day, provided that treatment is started within two days of getting sick.REF The development of anti-viral drugs for other respiratory diseases has been even less successful.REF
Viruses are parasitic. They cannot multiply unless they invade a living cell.REF Though scientists have learned much about viruses, a great deal remains to be discovered.REF It is not certain, for instance, where the measles virus originated, although it appears that either a canine or sheep virus crossed species and mutated to become the measles virus.REF More broadly, it remains unclear precisely what drives the emergence of new viruses.REF Regardless, at least 14 new virus species were reported between 2005 and 2009.REF Some of the most dangerous diseases known to medical science are viral (rather than bacterial) in origin,REF but the body is not defenseless against all viruses.
Humans develop immunity to viruses in the sense that the body has an immune response that can provide long-term protection from developing the disease associated with a virus.REF The proteins in viruses that trigger this immune response are referred to as antigens, and the vaccination against a disease works with the body’s immune system: The vaccine introduces a pathogen (such as a virus) that primes the immune system to deal with future exposures to similar pathogens.REF A healthy immune system evolves and provides protection against many viruses (and bacteria) and, ultimately, determines a person’s ability to survive.REF This strong immune response prevents transmission of a virus because it can no longer survive in its host (the body of an immune person).
In any given geographic location, when a large portion of people build immunity to a virus—whether through vaccination or naturally acquiring it by being infected—fewer people can develop the disease. (The incidence of infection declines.)REF This concept, which refers to the community-wide resistance to the spread of a disease when a large percentage of the community is immune, is often referred to as herd immunity.REF The portion of a population that must acquire immunity in order to achieve herd immunity is related to the level of infectiousness of a disease, but it is generally quite large.REF For instance, two separate groups of researchers estimate that approximately two-thirds of the population would have to be infected to achieve herd immunity for SARS-CoV-2, the virus that causes COVID-19.REF
Of course, depending on its characteristics, a viable strategy for dealing with a novel virus could be to achieve partial herd immunity by allowing low-risk individuals to become infected while simultaneously protecting those most vulnerable to the disease.REF Some epidemiologists have, in fact, suggested that such a strategy would be viable for dealing with COVID-19. Several have even argued that the suppression techniques employed in many countries—although they might be beneficial in some ways—are counterproductive because they inhibit the development of herd immunity.REF It is critical, therefore, that public officials have a good understanding of the risks that COVID-19 poses to the population.
What to Learn from the Evidence
While much remains to be learned about SARS-CoV-2, the virus that causes COVID-19, medical science is a never-ending pursuit of knowledge that rarely develops absolute certainty. Similarly, it is impossible to protect all human beings from getting sick.REF It is necessary, therefore, to weigh the bulk of the evidence to develop the best strategies for dealing with COVID-19.
Fortunately, after dealing with the virus for several months, in many different countries, there is a wealth of data to help understand how best to deal with COVID-19. It is very clear, for instance, that while COVID-19 is a deadly pathogen for which there is neither a vaccine nor a cure, and which has claimed more lives in the U.S. than severe seasonal influenza outbreaks, COVID-19 cases and deaths are highly concentrated in a small number of U.S. counties. The evidence also shows that COVID-19 poses relatively little risk of serious illness for younger people in good health.REF Data continue to pile up showing that COVID-19 was more widespread than originally thought, and that it is much less lethal than originally feared.REF Finally, while social distancing has some utility, it is inadequate to protect the most vulnerable populations,REF particularly those in nursing homes. While social distancing can slow down the rate at which the contagion spreads, it cannot defeat the pandemic in areas where infection rates are high.
Cases Are Highly Concentrated Geographically. Although all U.S. states have reported cases of COVID-19, the distribution of cases and deaths has remained heavily concentrated in a small number of states, and among a small number of counties within all states. For instance, as of May 11, just 10 states accounted for nearly 70 percent of all U.S. cases and 75 percent of all deaths (higher than their 52 percent share of the U.S. population).REF Together, New York and New Jersey accounted for 35 percent of all cases, and 44 percent of total COVID-19 deaths (roughly four to five times their population share of 9 percent).REF As of May 19, just five states—New York, New Jersey, Massachusetts, Illinois, and California—account for 50 percent of all of the confirmed cases in the U.S. and 57 percent of all COVID-19 deaths (approximately twice their 27 percent share of the population).REF These state-level figures do not, however, adequately describe the concentrated nature of the spread of COVID-19.
As of May 11, for example, 50 percent of all U.S. counties (with a 10 percent share of the U.S. population) had zero COVID-19 deaths, and 63 percent (representing 15 percent of the population) had no more than one. On the other hand, the 30 counties with the most COVID-19 cases account for 48 percent of all the cases in the U.S. (and 55 percent of all deaths) even though they account for just 15 percent of the U.S. population.REF So, while 1 percent of counties (mostly in the Northeast) have more than half of all COVID-19 deaths in the U.S., more than 60 percent of counties have no more than one COVID-19 death each—and both groups represent the same share of the U.S. population. (Chart 1 provides these comparisons with data as of May 19.)
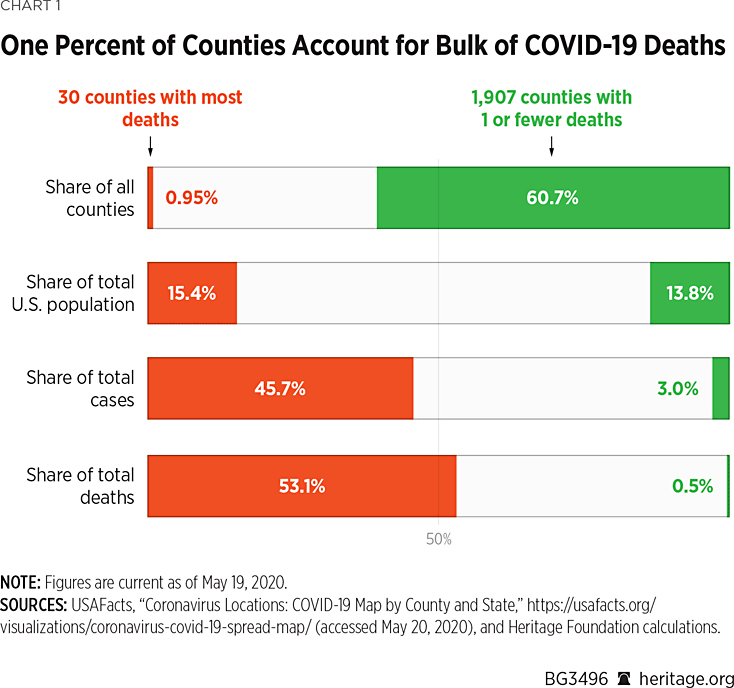
Of the 30 counties with the most COVID-19 cases, 24 are in the Northeast corridor between Philadelphia and Boston, the passageway served by a commuter railway system that runs through Manhattan. Seven of these 30 counties are among the nation’s 10-most-densely populated.REF Within almost all states, even those outside the Northeast corridor, the number of cases (and deaths) is heavily concentrated in a few counties.
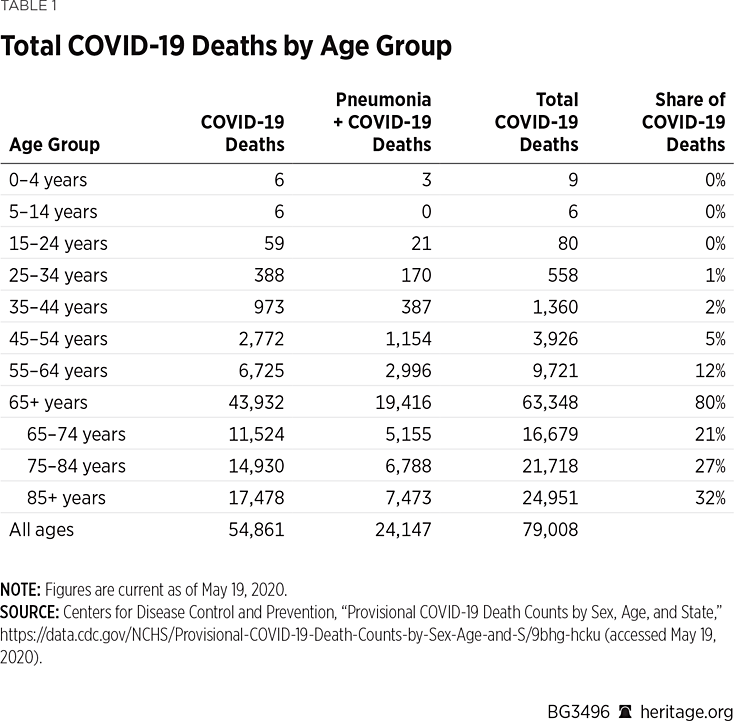
In Illinois, for instance, 70 percent of the state’s cases (as of May 11) are in just one county—the Chicago area’s Cook County, with 41 percent of the state’s population. Illinois has 102 counties, and 90 percent of the state’s cases are in just five of the counties (with a 63 percent share of the population). As Map 1 illustrates, this concentrated pattern is found in most states across the U.S. Moreover, this concentrated pattern is not a new phenomenon—it has persisted throughout the entire course of the COVID-19 epidemic.REF Thus, throughout the crisis, public health officials have dealt with very different case volumes both across states and within states.
Age and Comorbidity Statistics. The evidence shows that the overwhelming majority of COVID-19 deaths (and hospitalizations) occur among older individuals. Furthermore, the overwhelming majority of deaths and hospitalizations befall people with at least one additional underlying health problem, such as hypertension, obesity, or diabetes.
Table 1 presents CDC age-specific COVID-19 death estimates through the week ending May 19. The first column breaks out the age categories. Column 4, labeled “Total COVID-19 Deaths” represents the sum of Column 2 (labeled “COVID-19 Deaths”) and Column 3 (labeled COVID-19+Pneumonia). The final column represents the percentage of total COVID-19 deaths attributable to each age group. For example, children age five to 14 represent less than 0.01 percent of all COVID-19 deaths, while those age 25 to 34 account for 1 percent of those deaths. In all, people under 34 account for approximately 1 percent of COVID-19 deaths, while those age 54 and under account for just 8 percent of such fatalities.
Nearly 93 percent of COVID-19 deaths have so far occurred in people age 55 and older, with 80 percent of those who have died of the contagion being 65 and older. There is also some age-related stratification within this age demographic. Those age 65 to 74 account for 21.3 percent of COVID-19 deaths, those age 75 to 84 account for 27 percent, and those age 85 and older account for 31 percent of deaths.
Age and comorbidity not only are associated with COVID-19 death rates but also with severity of illness. Data from the CDC and from New York officials confirm that hospitalization rates, like mortality rates, are likely to vary with age. Table 2 presents hospitalization rates per 100,000 population by age through May 9.
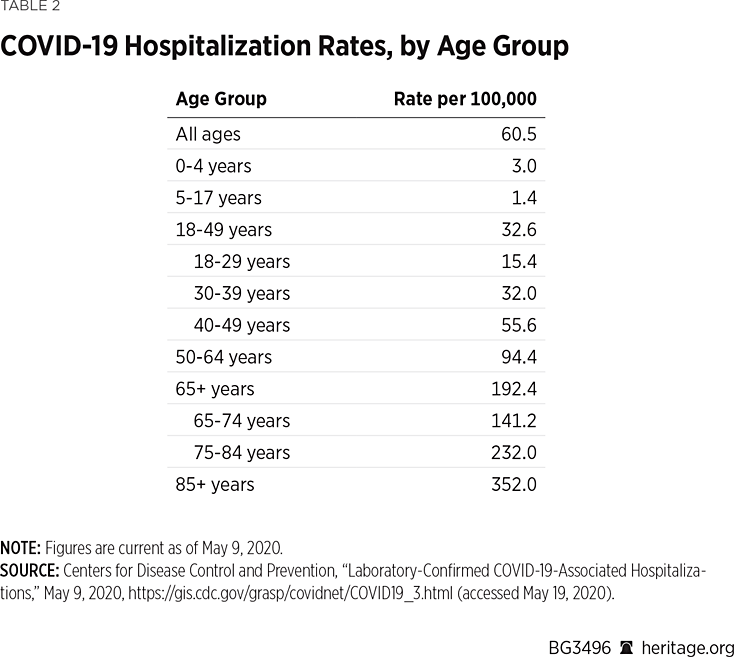
The data show that hospital resources are unlikely to be stressed by younger members of the population. As shown in Table 2, the hospitalization rates for COVID-19 patients increase with age, and the highest hospitalization rates are among those age 85 and older. (The rate for this group is nearly six times the overall rate and more than 250 times as high as for the school-age population.) The age-specific data, reported from the COVID-19–Associated Hospitalization Surveillance Network (COVID-NET), a network that covers 99 counties in 14 different states, show that (as of March 30) 75 percent of hospitalized COVID-19 patients were over the age of 50.REF
It is important to point out that COVID-NET includes data from New York, so the overall COVID-19 hospitalization rates in Table 2 are likely skewed upward relative to the rest of the country. The age-based hospitalization rates from New York City, displayed in Table 3, illustrate this point. Public health officials can likely use these figures as a worst-case scenario.
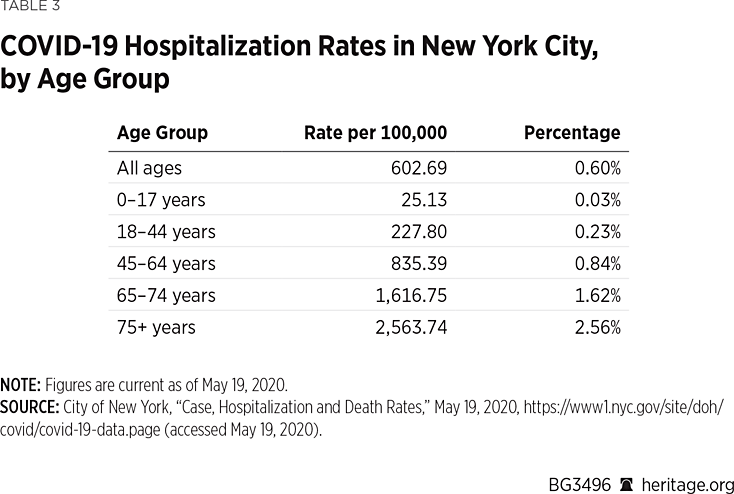
Table 3 shows that the overall COVID-19 hospitalization rate in New York city, as of May 19, was 602.69 per 100,000 people, a figure that translates into approximately one half of 1 percent of the population. For those New York City residents under 18 years, the chance of being hospitalized because of COVID-19 was less than 0.03 percent. The rate increased with age, but it was less than 1 percent for all age groups under 65. As Dr. Leora Horwitz, co-author of a large study of New York City COVID-19 patients, notes: “Age is far and away the strongest risk factor for hospitalization, dwarfing the importance of obesity. Obesity is the most important of the chronic conditions when considering all such conditions simultaneously.”REF These findings are also consistent with international data from the earliest stages of pandemic, as reported by the World Health Organization (WHO). For instance, a WHO report from March 1, 2020, stated that “illness severity is associated with age (>60 years old) and co-morbid disease.”REF
Separately, using COVID-NET data, the CDC reports that, through March, 75 percent of hospitalized COVID patients were over the age of 50, and 89 percent had at least one additional underlying condition, such as hypertension or diabetes.REF Many other studies, both in the U.S. and internationally, support the conclusion that age and comorbidities have an outsized impact on the severity of COVID-19 outcomes.REF The following list is a brief summary of the evidence on age and comorbidities:
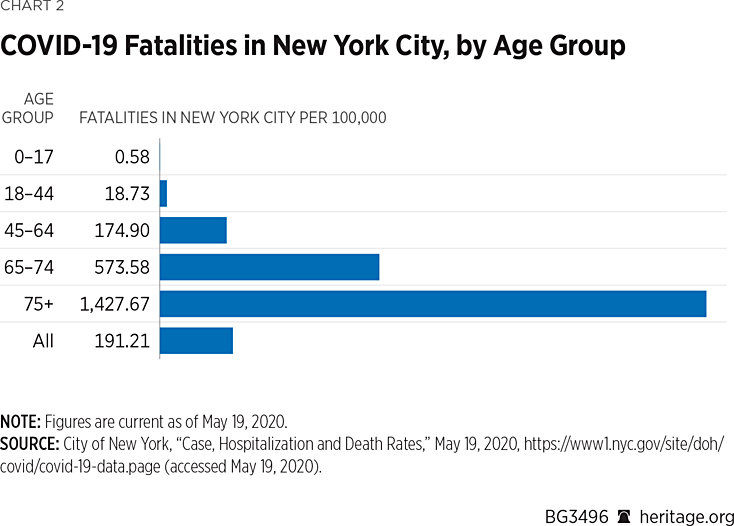
- In New York City, the rate of deaths per 100,000 people is 0.58 for those under age 18. The remaining distribution by age is as follows: 18.73 per 100,000 for those age 18 to 44 (0.019 percent); 174.9 per 100,000 for ages 45 to 64 (0.18 percent); 573.58 per 100,000 for ages 65 to 74 (0.57 percent); and 1,428 for those 75 and over (1.428 percent).REF These statistics are based solely on age, without considering the effects of comorbidities.
- As of April 18, out of 6,570 confirmed COVID-19 deaths in New York City, 6,520 (99.2 percent) had at least one comorbidity.REF
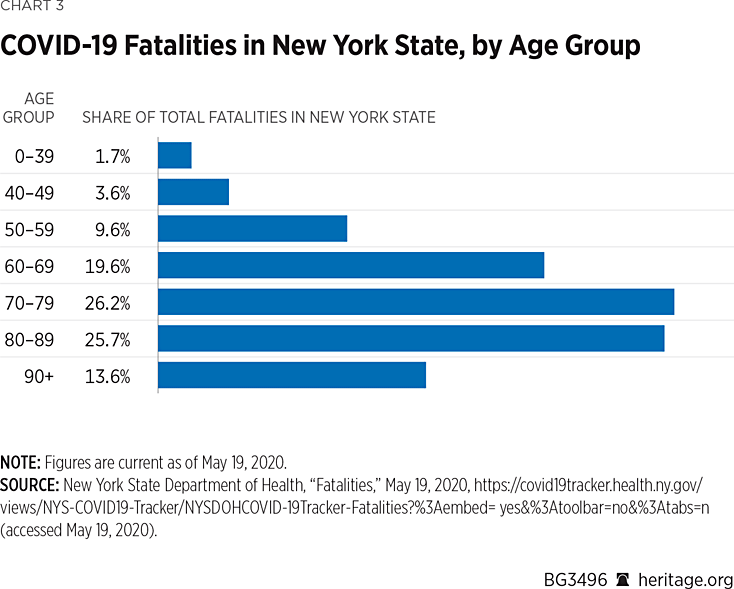
- In New York State, 90 percent of total fatalities have at least one comorbidity, and 85 percent of total deaths were people age 60 and above (with 66 percent of total deaths in patients age 70 and above).REF
- A recently published study of 5,700 patients in the New York City area revealed that, during hospitalization, 373 patients (6.5 percent) were treated in intensive care units, and those patients had a median age of 68 years.REF
- In Oakland County, Michigan, a COVID-19 hotspot, 77 percent of the coronavirus deaths are in people 70 and older.REF In Louisiana, another hotspot, 85 percent of the COVID-19 fatalities are in individuals 60 and older.REF
- A recent study published in the Journal of the American Medical Association: Pediatrics examined hospital data in the U.S. and Canada. The authors conclude: “[I]t is important to emphasize that the overall burden of COVID-19 infection in children remains relatively low compared with seasonal influenza,” and that “our data indicate that children are at far greater risk of critical illness from influenza than from COVID-19.”REF
- Consistent with several analyses of Chinese data, one study of the outbreak in China (of more than 44,000 confirmed cases) reports that 81 percent of the cases were mild. No deaths occurred in those age nine and below, but there was a case fatality rate of 8 percent for those age 70 to 79, and 15 percent for those 80 and older.REF The authors report that the case fatality rate “was elevated among those with preexisting comorbid conditions—10.5 percent for cardiovascular disease, 7.3 percent for diabetes, 6.3 percent for chronic respiratory disease, 6.0 percent for hypertension, and 5.6 percent for cancer.”REF
- A New England Journal of Medicine study reports on the early phase of the outbreak in China. The study shows that doctors categorized admitted patients’ degree of severity of COVID-19 as non-severe in 926 patients, and severe in 173 patients. Patients with severe disease were older than those with non-severe COVID-19 by a median of seven years.REF
- Authors of a paper in The Lancet studied the outbreak in China by examining data from 191 patients across two hospitals. The authors report that 48 percent of deaths occurred with patients who had at least one comorbidity, and that the odds of in-hospital death increased in older patients.REF
- A study of the outbreak in Italy notes that “COVID-19 is more lethal in older patients, so the older age distribution in Italy [23 percent of the population is 65 or older] may explain, in part, Italy’s higher case-fatality rate compared with that of other countries.”REF The study reports that “individuals aged 70 years or older represent 37.6% of cases in Italy,” and that there were zero deaths in the under 30 population.REF Out of 1,625 deaths in Italy, 52 percent were in the 80 and older population, 36 percent in those 70 to 79, and 8.6 percent in those 60 to 69.REF In a subset of Italian patients who died, “The mean number of preexisting diseases was 2.7…only 3 patients (0.8%) had no diseases, 89 (25.1%) had a single disease, 91 (25.6%) had 2 diseases, and 172 (48.5%) had 3 or more underlying diseases.”REF
- An April 7 study of COVID-19 in Italy shows that (as of March 27) 83.7 percent of the country’s 7,589 COVID deaths were among people 70 or older. The data also reveal that the most common comorbidities observed in dying COVID-19 patients were hypertension (74.7 percent) and Type 2 Diabetes (30.5 percent).REF
- In the state of Washington, across several long-term care facilities, the median age of those infected was 83, and 94 percent had a chronic underlying condition. The hospitalization rate for those infected was 55 percent, and the case fatality rate was 34 percent.REF
- According to a March 16 CDC report, an analysis of 508 U.S. patients known to have been hospitalized showed that 9 percent were 85 years or older, 36 percent were 65 to 84 years old, 17 percent were 55 to 64, and less than 1 percent were among those younger than 20. Of all cases reported in the U.S. as of March 16, “45 percent of hospitalizations, 53 percent of ICU admissions, and 80 percent of deaths occurred among adults [at least] aged 65 years with the highest percentage of severe outcomes among persons [at least] aged 85 years.”REF These results were consistent with more recent CDC data showing that people 65 and older “with or without underlying conditions were 2 to 3 times more likely to require hospitalization and admission to intensive care than were those 19 to 64 years of age.”REF
- South Korea reports that more than two-thirds of all of its “severe” and “very severe” cases were in those age 60 and older, with approximately half in the 70-to-79 age group.REF
- A study of 16,749 COVID-19 patients from 166 U.K. hospitals, from February 6 to April 18, found a median age of 72 for patients admitted with COVID-19. The data also showed that 75 percent of the patients were older than 57, and that 25 percent were older than 82. The authors report that “[i]ncreased age and comorbidities including obesity were associated with a higher probability of mortality.”REF
COVID-19 and Nursing Homes. In addition to being strongly correlated with age and underlying health conditions, COVID-19 deaths appear to be especially prevalent among residents of nursing homes. The Kaiser Family Foundation estimates that 41 percent of COVID-19 deaths in the 36 states it studied are nursing-home-related.REF A study by the Foundation for Research on Equal Opportunity estimated that approximately 40 percent of COVID-19 deaths through May 7, 2020, were nursing-home-related.REF Excluding New York State, whose reported number of nursing-home-related COVID-19 deaths appear to be an outlier, increases the overall percentage to 49 percent.REF A database compiled by Phil Kerpen of American Commitment arrives at a similar estimate.REF As of May 8, the group estimated that 52 percent of COVID-19 deaths were in nursing homes.
These figures suggest that stay-at-home orders and other policies aimed at the broader population are failing to address the group most likely to die of COVID-19: nursing home residents. Although they represent just 2.26 percent of the population, they account for an outsized percentage of the pandemic’s death toll.REF Data from across the country document that these high percentages are generally found across the states (with the exception of the anomalous New York State numbers), suggesting that neither state, local, nor federal health authorities have developed any effective response to these deaths.REF Indeed, some states, including New York, had adopted policies that exacerbate the crisis, such as ordering long-term care facilities to accept COVID-19 patients upon discharge from a hospital.REF States should consider repealing these policies and, more urgently, developing interventions that protect vulnerable nursing home residents.REF
- On May 2, in Virginia, the Alexandria Health Department reported a total of 26 COVID-19 fatalities. Of that total, 15 (58 percent) were residents of long-term care facilities.REF According to the Virginia Department of Health, approximately 54 percent of the state’s COVID-19 fatalities (660 deaths as of May 3) were residents of long-term care facilities.REF
- Louisiana health officials stopped regularly reporting case and fatality statistics for individual nursing homes, but they irregularly provide aggregated data. As of May 4, when the state was reporting 1,991 COVID-19 deaths, officials reported that 688 (35 percent) of those deaths were people who lived in nursing homes.REF The nursing homes account for 3,133 (11 percent) of the state’s 29,673 cases. The state’s other 157 residential facilities (including drug treatment centers and psychiatric facilities) account for 417 cases and 50 deaths.REF On May 19, the state released data for its 279 licensed nursing homes (omitting assisted-living homes and other residential facilities) that showed 987 COVID-19 deaths in these homes. This figure accounts for more than 40 percent of the state’s total coronavirus deaths.REF
- On May 5, more than 1,600 previously undisclosed deaths in New York were reported as nursing home residents. According to the report, as of May 3, more than 4,800 nursing home residents died from COVID-19, representing 25 percent of the state’s total coronavirus fatalities.REF According to David Grabowski, a Harvard University researcher who studies nursing homes, it is likely that nursing homes will ultimately account for half of all COVID-19 deaths in every state, as they already do in Massachusetts, New Jersey, and Pennsylvania.REF
- According to the Michigan Department of Health and Human Services, Hillsdale County, Michigan, had 137 confirmed COVID-19 cases as of May 6. The county’s outbreak has centered on a county-owned nursing home, where deaths at the facility so far have accounted for more than 80 percent of the county’s COVID-19 deaths.REF
Overall Case-Fatality Rate Lower Than First Feared. The evidence suggests that most people who become infected with COVID-19 experience relatively mild symptoms. Mounting evidence now indicates that many more people have been infected than have been reported to public health authorities.REF This finding has sometimes been mischaracterized as dangerous and as a justification for sweeping shelter-at-home orders. It is true that these data indicate that more people are potentially transmitting the virus than first thought, but it also indicates that only a small fraction of those who were infected became seriously ill or even showed any symptoms. Moreover, a higher infection rate reduces the likelihood of a large future outbreak during 2020, so long as those who develop antibodies are, in fact, immune to future infection, at least for a while.REF Finally, the more asymptomatic cases, the more important the true case-fatality rate—the percentage of all those infected who die from the disease as opposed to the crude case-fatality rate estimated as the percentage of known cases that result in death—becomes for predicting the outcomes of the epidemic.REF The following list summarizes this evidence:REF
- Data from the town of Vo’ in the Veneto region of Italy suggests that between 50 percent and 75 percent of those infected with COVID-19 are completely asymptomatic.REF The researchers tested almost all 3,000 citizens of the town, and the evidence suggests that between 2.1 percent and 3.3 percent were infected with COVID-19.REF No infections were reported in children under 10, the prevalence of infection was between 1.2 percent and 1.7 percent for those up to age 50, and it was three times as high for those older than 50.REF
- According to the Japanese Ministry of Health, Labor, and Welfare, of the 621 confirmed positive cases on the Diamond Princess Cruise Ship, 322 (52 percent) showed no symptoms (were asymptomatic).REF
- In Germany, researchers tested 500 residents of the municipality of Gangelt, a town near Germany’s border with the Netherlands that was one of Germany’s hardest-hit towns. They found that 14 percent of participants tested positive—of which 22 percent were asymptomatic. The findings indicate that the true infection rate is five times higher than the official statistics for the town, and that the true fatality rate in Gangelt is approximately 0.37 percent, much lower than the (crudely estimated) 2 percent fatality rate in Germany.REF
- Between March 22 and April 4, 215 pregnant women gave birth at New York–Presbyterian Allen Hospital and Columbia University Irving Medical Center. All of the women were screened for COVID-19 when they were admitted to the hospital. Out of this group of women, 33 (15.3 percent) tested positive for COVID-19, and 29 of those 33 women (88 percent) were asymptomatic. Of the 29 women who had been asymptomatic when admitted, three (10 percent) later developed fever during their stay (the median length of stay was two days).REF Patients who tested positive were discharged 14 days later and none experienced serious medical problems.REF
- A study of 147 individuals at a Boston homeless shelter revealed that 36 percent of the participants tested positive for COVID-19, and 64 percent tested negative. Among those who tested positive, 87.8 percent were asymptomatic.REF A similar study in Los Angeles—of more than 200 people at the Union Rescue Mission in the Skid Row area—found 43 positive cases, of which 63 percent were asymptomatic.REF
- A recent study of Los Angeles County suggests that the number of infections is around 40 times as high as the number of confirmed cases. Based on results of the first round of testing, the research team estimates that approximately 2.8 percent to 5.6 percent of the county’s adult population was previously infected. (They have an antibody to the virus.) This estimate indicates that between 221,000 and 442,000 adults in Los Angeles have had the infection, roughly 28 to 55 times higher than the number of total confirmed cases (7,994 at the time of the study).REF The estimate also suggests that instead of a case-fatality rate near 5 percent, crudely estimated by dividing the number of deaths by the number of confirmed cases, the true case-fatality rate is close to 0.1 percent (similar to the case-fatality rate for the seasonal flu).
- Preliminary results from a large-scale test in Santa Clara County, California, indicate that the number of infections is much greater than the reported number of confirmed COVID-19 cases. The data implies that, as of April 1, between 48,000 and 81,000 people had been infected in Santa Clara. This estimate suggests that the number of cases in the county was actually 50 to 85 times higher than the number of confirmed cases (956) at the time of the study. This higher infection rate indicates a case-fatality rate of approximately 0.12 to 0.2 percent.REF
- Several rounds of large-scale testing in San Miguel, Colorado, indicate that between 0.55 percent (26 positive tests of 4,757 tests) and 1.5 percent of the population (70 borderline tests of 4,757) has been infected by COVID-19.REF As of April 30, San Miguel had 19 confirmed cases, but these test results indicate that between 45 and 123 people in the county were infected (between 2.5 and 6.5 times higher than the number of confirmed cases). As of April 30, San Miguel reported zero COVID-19 deaths. The cumulative test results in San Miguel remain consistent with those reported from earlier rounds of testing.REF
- On April 27, New York Governor Andrew Cuomo announced that the statewide antibody tests had expanded to 7,500, and that 15 percent of people tested positive for COVID-19 antibodies, a bit more than the previous (April 22) sample of 3,000 people indicated.REF The latest results indicate that as much as 25 percent of the population of New York City have been infected.REF Using the county populations for New York, Queens, Kings, Bronx, and Richmond, a 25 percent infection rate indicates that more than 2 million people in New York City have been infected, more than 12 times the number of confirmed cases. Using these counties’ confirmed COVID-19 deaths as of April 30 suggests a case-fatality rate of approximately 0.8 percent.REF
- On April 24, Miami-Dade County officials announced that a second round of COVID-19 antibody testing (conducted with researchers from the University of Miami Miller School of Medicine) showed that 6 percent of county residents were infected, thus affirming the results from an earlier round of testing.REF This testing program randomly sampled participants across the county’s 32 municipal statistical areas, and more than 1,800 people have participated in the testing (as of this writing). The results suggest that the actual number of COVID-19 infections in the county is possibly 16.5 times the number of officially reported infections (which numbered approximately 11,000 at the time of the April 24 release). The results indicate that the true number infected is between 123,000 (4.4 percent of the population) and 221,000 (7.9 percent population).
- An antibody study of one of the hardest-hit areas of Germany found that 14 percent of those tested had been infected. Similar to other studies, these results suggest that many more people have been infected with COVID-19 than the official records indicate. In the case of the town of Heinsberg, the results suggest a case-fatality rate for COVID-19 of about 0.37 percent.REF
- Researchers conducted a targeted testing program in Iceland that ultimately tested 6 percent of the population. The program specifically targeted those deemed most at risk for infection, but it also issued an open invitation to 10,797 people and sent 2,283 invitations randomly (response rates are not provided). A total of 1,222 of the 9,199 (13 percent) in the targeted group tested positive for COVID-19. Of those in the open invitation group, 87 (0.8 percent) tested positive, while 13 (0.6 percent) in the random group tested positive. Of all those tested, 43 percent were asymptomatic.REF
- Researchers studied 546 health care workers and 283 non-health-care workers (with no known exposure to COVID-19) in a large New Jersey university and two affiliated hospitals. The researchers report that 5 percent of the workers tested positive, and 66 percent of those study participants were asymptomatic.REF
- Recent tests conducted of inmates in several U.S. prisons showed extremely high asymptomatic infection rates. According to Reuters, “In four state prison systems—Arkansas, North Carolina, Ohio, and Virginia — 96% of 3,277 inmates who tested positive for the coronavirus were asymptomatic.”REF Although these results may not translate directly to the broader U.S. population, they are indicative of a severe undercounting problem of people infected with COVID-19.
- By February 6, a total of 565 Japanese citizens had been evacuated from Wuhan, China. These individuals were tested for COVID-19 and monitored. The tests found that 13 people (2.3 percent) tested positive, with four of those individuals asymptomatic.REF A statistical analysis estimated that the percentage of all asymptomatic Japanese evacuees was 30.8 percent. Those evacuees without symptoms were observed for a minimum of 30 days after testing; they did not develop symptoms.
Hospital Capacity Is Not a Systemic Problem. Early in the pandemic, various models forecast that the U.S. hospital system could be overwhelmed by a surge of COVID-19 patients. There was particular concern about a shortage of ventilators for those who developed severe respiratory symptoms. Some predicted that the crisis that struck some hospitals in Northern Italy, where there were insufficient numbers of available beds and ventilators to accommodate seriously ill patients, would be replicated in the U.S.REF New York City was identified as especially vulnerable.
Averting such outcomes was among the principal arguments in favor of implementing sweeping social-distancing practices (including stay-at-home orders and closures of schools and many businesses) and for prohibiting the provision of non-emergent care. A surge of unmet need now seems far less likely than it did in the early days of the pandemic, and the widespread practice of stay-at-home orders and bans on non-emergent care may have had negative consequences. Public officials must adapt these policies to this new information.
While the crisis has far from passed, it appears that the U.S. is not likely to endure the dislocations experienced in Milan, Bergamo, and other Italian cities. As the authors of this Backgrounder pointed out in a previous paper, there is no systemic shortage of hospital beds or ICU capacity in the U.S.REF As reported in that paper, U.S. hospitals have among the lowest occupancy rates in the developed world, giving them a fairly robust excess capacity. It also cited data showing that the country’s ICU capacity is two to three times that of most European countries. That does not protect the U.S. from episodic and localized surges, but it does suggest that the country’s hospital bed capacity is structurally sound. Moreover, even though most of the facilities did not treat a single patient during the COVID-19 outbreak, the U.S. Army Corps of Engineers proved that it was able to construct field hospitals all over the country in a very short period of time.REF
A study by the President’s Council of Economic Advisers (CEA) similarly found that the U.S. has an ample supply of ventilators. A CEA simulation found that “existing national ventilator supply continues to be sufficient to handle total national demand—even under the most aggressive virus spread scenarios identified by the U.S. Centers for Disease Control and Prevention and before the arrival of new units produced by United States industry partners.”REF The study also concluded that the reallocation of existing supply would be sufficient to meet heightened demand without having to tap the Federal Strategic National Stockpile. As Chart 4 shows, the CDC reports daily figures on acute-care-bed and ICU-bed occupancy rates by state. Those reports continue to show very high rates of available capacity.
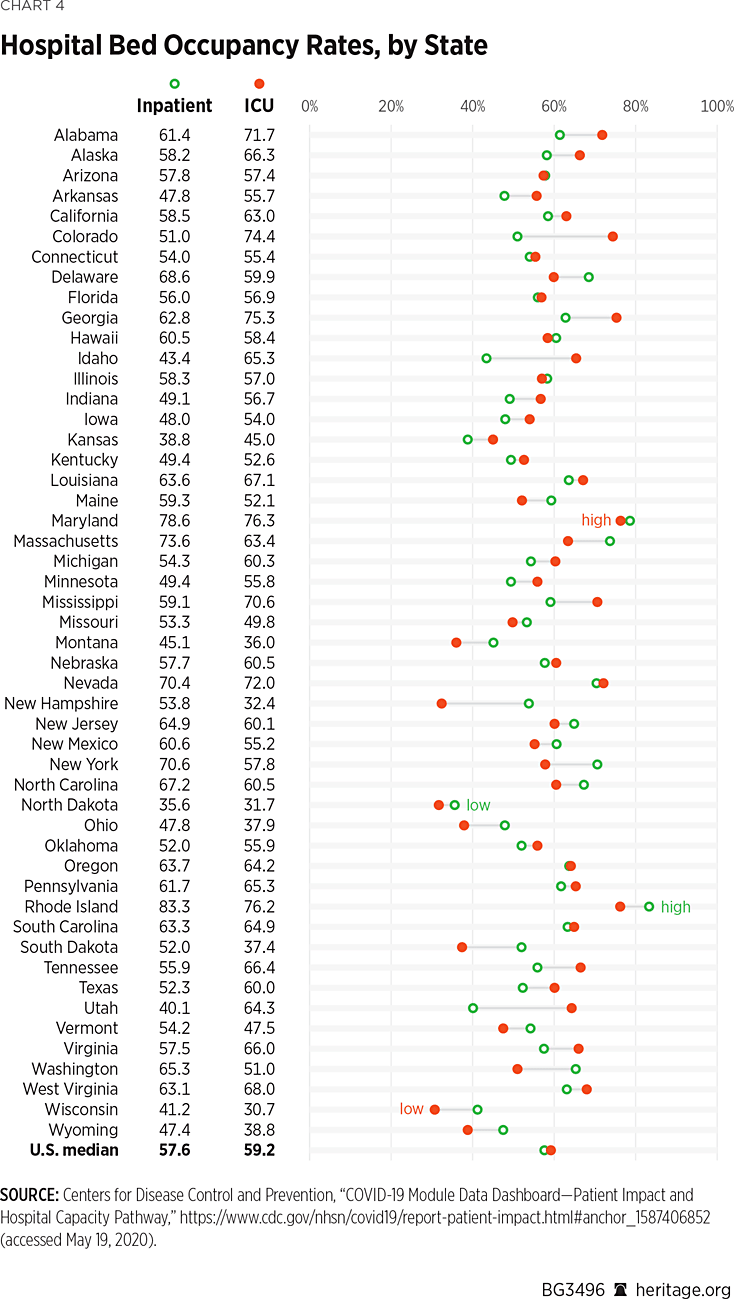
While these data are encouraging, they require cautious use. First, they provide a snapshot that changes daily, and even hourly. Second, the data are only available at the state level. Shortages are more likely to arise on a local or county basis than across an entire state. Third, the CDC collects this data from states and reporting is neither uniform nor comprehensive. Finally, these data are drawn during a period of time when many states and jurisdictions have limited the provision of non-emergent care. That policy, which is both unsustainable over a long period of time and one that should be replaced with better approaches, temporarily increases excess capacity.
The policy of banning non-emergent care carries risk for patients with chronic conditions, especially if it is kept in place indefinitely. Scheduled tests and surgery may be elective, but most also are medically necessary. This is especially relevant because, as discussed above, complications and death from COVID-19 are highly correlated with chronic illness. To the extent that bans on non-emergent care limit access to chronic disease management, it can put patients at greater risk of hospitalization and death if they contract COVID-19.
These orders to temporarily shutter medical capacity have led to layoffs of medical workers during a national health care crisis. A policy that reduces the supply of workers when they are most needed seems counterproductive. These layoffs and the reduced capacity are not merely anecdotal. In its first estimate of gross domestic product (GDP) for the first quarter of 2020, the Commerce Department estimated that the U.S. economy contracted by 4.8 percent.REF The magnitude and abruptness of that contraction is highly unusual, and especially surprising, since social distancing and lockdowns did not occur on a widespread basis until the last weeks of that quarter. More surprising, perhaps, is that the biggest decline occurred in the health care sector, which shrank by 2.25 percent on an annualized basis.
Bans on non-emergent care led to the shedding of more than 1.4 million health care jobs during the month of April, a contraction of nearly 9 percent.REF The cutback affected hospitals (job losses totaling roughly 135,000), nursing homes (113,000), physician offices (243,000), dental practices (503,000), medical and diagnostic laboratories (31,000), residential mental health facilities (27,000), and outpatient care centers (89,000).
Millions of patients have been denied access to medically necessary care, including preventive services, diagnostic tests, and treatments, as the result of these bans. Policymakers should abandon limitations on non-emergent care, except to free up bed capacity in areas identified as imminent hotspots.
Much of the concern about insufficient capacity was attributable to the inaccuracy of models that forecast shortages of beds and ventilators. These inaccurate models spurred officials to take actions to stave off a crisis that may never occur. These actions may have been prudent at the onset of the outbreak and, at least to some extent, potentially effective. Stay-at-home orders slowed down the rate of infection and therefore likely reduced peak demand for hospital services. The federal and New York State governments also took steps to provide temporary hospital capacity, most of which proved unnecessary. And the ban on non-emergent care, at least in New York City and adjacent counties, freed up hospital capacity in existing facilities.
Given the adverse consequences of inadequate preparation, government officials can hardly be criticized for overshooting expectations. But while these policies may have been useful in those circumstances, they have also produced broader and less-favorable consequences. Government officials should reconsider and adapt these policies to new information that has become available as the pandemic has matured.
Toward an Evidence-Based Public Health Response to COVID-19
Since fairly early in the pandemic, the principal public health response in the U.S. and most European countries has been widespread social distancing and stay-at-home (lockdown) orders. The initial lockdown policies—particularly in the U.S. and the U.K.—were based largely on projections from a statistical model developed at the Imperial College of London.REF In mid-March, that model predicted that an uncontrolled spread of COVID-19 would claim more than 500,000 lives in the U.K. and cause 2.2 million deaths in the U.S.REF
The model also predicted that the death toll in the U.S. would be as high as 1.2 million, even with enhanced social distancing that included special shielding of the elderly.REF Moreover, the model predicted that “the surge limits for both general ward and ICU beds would be exceeded by at least 8-fold” under the most optimistic scenario, with an increasing rate of infections and hospitalizations from April 20 through June 20.REF Hospital capacity was not exceeded to this degree anywhere in the U.S., and the seven-day moving average of new cases per day peaked (at more than 30,000) during the week of April 8 to April 15. Despite a constant ramping up of testing in the U.S., this new case average has been on a downward trend since April 26, with the average less than 23,000 per day from May 13 to May 17.REF This trend took shape while total COVID-19 deaths remained below 100,000 and states began relaxing stay-at-home orders. Thus, the Imperial model’s prediction turned out to be overly pessimistic, as did the initial forecast from the model developed by the University of Washington’s Institute for Health Metrics and Evaluation (IHME), a second model that heavily influenced the Trump Administration’s response to COVID-19.REF
Relying on these models, government officials advocated for lockdown orders. Their initial rationale was not to reverse the pandemic’s spread but to slow its pace, primarily to prevent a surge in patients from overwhelming hospital capacity. Policymakers were concerned about replicating disastrous events in northern Italy, where hospitals were overwhelmed by a surge in critically ill patients.
This has so far not happened in the U.S., despite fears that it would occur in New York City. As discussed previously, hospitals in that metropolitan area withstood the initial wave of infections, partly because of social distancing, partly because of the addition of temporary hospital capacity, and partly because the models on which public officials relied overshot estimates of demand. The threat of such a surge, to the extent it does exist, is confined to a fairly small number of localities.
Public Health Interventions Should Evolve in Light of New Data
Over time, policymakers appear to have raised their expectations of what social distancing can accomplish. Many now consider it a means to reverse the pandemic. It is not. Moreover, there is a growing perception that the current policy choice is binary: Either retain the policy of broad-based social distancing, or return to normal and risk a resurgence of the pandemic. That is a false choice.
Policymakers should acknowledge the limited value of lockdown orders and pivot toward public health interventions based on data that have emerged since those orders were set in place. Those interventions must adjust for the fact that hospitalization and death rates vary geographically and demographically, that the disease is especially lethal for the frail elderly living in congregate settings, that U.S. hospital capacity is more resilient than previously believed, and that bans on non-emergent care are counterproductive.
It is now known that the pandemic is not evenly spread across the country. In areas where there are few cases, lockdown orders inflict hardships on families and businesses without a compensating public health benefit and, to the extent that they have idled medical capacity and reduced the provision of medically necessary care, may be doing harm. Globally, for instance, the disruption of medical care for tuberculosis and malaria patients, as well as preventive measures, could lead to millions of preventable deaths.REF It is beyond the scope of this Backgrounder, but the hardships have already led to protests across the U.S. and worsened racial tensions in some communities.REF Officials should roll back the policy in those communities with few cases and low case growth, while vigilantly watching for signs of an outbreak.
In areas where the infection rate is high, lockdowns remain necessary, but by themselves, are an insufficient public health response to the pandemic. In New York City, relying primarily on social distancing means falling down the steps more slowly—infections continue to spread and people continue to die. The New York City metropolitan area still accounts for 13 percent of new cases in the U.S. and 22 percent of all deaths (several times greater than the area’s 3 percent share of the population). More effective public health interventions should be tried.
Although it is difficult to parse out the effect that various social-distancing policies had on the spread or lethality of COVID-19, some empirical (and theoretical) work does suggest that the severe social-distancing restrictions, such as the stay-at-home orders, were not effective. For instance, as two California medical professionals recently pointed out, the CDC tracking data suggest that the pace of COVID-19 infections in the San Francisco Bay area had already begun to decline in mid-March, when “the state instituted severe restrictions on social contact and personal movement.”REF In particular, the CDC data show that the highest number of hospital admissions in the Bay Area occurred between March 21 and 28, suggesting that peak infections occurred approximately 12 to 14 days prior, before the severe restrictions took effect.REF
Separately, the CDC conducted a study of how COVID-19 spread in four metro areas that were virus hot spots—Seattle, San Francisco, New York City, and New Orleans. This study closely examined the timing of all the different emergency measures that these local governments implemented, including placing limits on mass gatherings and closing schools, as well as stay-at-home orders. The results showed a significant decline in the rate of change for the number of cases after state and local emergency declarations and bans on mass gatherings. However, the results showed virtually no additional impact on case growth after stay-at-home orders were issued.REF In fact, a recent National Bureau of Economic Research (NBER) paper reports that the policy response of implementing stay-at-home orders was itself largely a response to voluntary measures that had already dramatically reduced citizens’ mobility.REF
Perhaps the most damaging evidence against the effectiveness of the current stay-at-home policies comes from New York City. On May 6, 2020, Governor Cuomo announced that preliminary data from 100 New York hospitals (covering 1,000 patients) showed that 66 percent of newly admitted COVID-19 patients were people who had been sheltering in their homes, and that 18 percent of those admitted were people living in nursing homes.REF Cuomo called the findings “shocking” and stated: “We thought maybe they were taking public transportation, and we’ve taken special precautions on public transportation, but actually no, because these people were literally at home.”REF
On April 13, Cuomo had assured New Yorkers: “If you isolate, if you take the precautions, your family won’t get infected.” That assurance, which has turned out not to be true, shows how officials modified their views on stay-at-home orders. They were introduced as a way to “flatten the curve,” making the pandemic last longer but peak at a lower level. That lower peak was meant to protect hospitals from an overwhelming surge of patients. It is likely that these measures helped to protect the New York City hospital system from a surge.
But over time, government officials came to expect results that stay-at-home orders cannot deliver: keeping people safe from infection, as Governor Cuomo suggested on April 13. That, they cannot do.REF The virus continues to spread in New York City and its environs, despite an extended period of severe social distancing.
Having promoted the practice for months, it is difficult for policymakers to pivot to other, more effective, public health interventions. Most seem locked in a dialectic between keeping lockdown orders in place or repealing them outright. Instead, they should focus their efforts on places where the risk of death is highest: nursing homes and areas like New York City, where infection rates are especially high.
A recent NBER paper by Sangmin Aum, Sang Yoon Lee, and Yongseok Shin suggests exploring a policy pathway that might prove especially effective in places where infection rates are already high. The three authors developed a quantitative model for estimating the public health and economic effects of a series of policy options.REF Their models compared outcomes of interventions practiced in the United Kingdom, which is relying primarily on social distancing, and in South Korea, which uses more extensive testing, isolation of the infected, extensive contact tracing, and travel restrictions to combat the spread of the virus.REF
Their research compared three approaches: (1) maintaining lockdowns, (2) prematurely lifting the lockdowns with no other public health interventions, and (3) adopting public health policies practiced in South Korea. They found that if the U.K. maintains its lockdown, it will reduce GDP and infections in the short term, an outcome that is preferable to prematurely ending the lockdown. However, the optimal result, the researchers found, would be to implement the public health interventions practiced in South Korea. Such policies would result in GDP losses and infections that are substantially smaller in the short and long run.
Some have suggested that the South Korean model worked because it was implemented so early in the pandemic and that it is too late for the U.K., the U.S., and other Western nations to adopt these policies. The researchers found, however, that Korea’s success was not primarily attributable to its early intervention, but “because aggressive testing and tracking more effectively reduce infections and disrupt the economy less than a blanket lock-down.”REF
The model suggests that retreating prematurely from social distancing in New York or other localities with high infection rates without introducing more effective policies would produce the worst public health and economic results over the longer term. But relying primarily on social distancing would be far less effective in those communities than instituting policies of temporary isolation of the infected, along with aggressive testing and contact tracing.REF
Another recent research project, using a different approach, reached similar conclusions. The authors report that “optimal policies differentially targeting risk/age groups significantly outperform optimal uniform policies and most of the gains can be realized by having stricter lockdown policies on the oldest group.”REF Their findings support the idea that it is more effective, both economically and in terms of minimizing COVID-19 deaths, to use protective measures targeted toward those most at risk and to isolate those who are sick.
Recommendations for Policymakers
Stay-at-home orders, blanket school closures, and the temporary shuttering of “non-essential” businesses were introduced as a public health intervention at a time when very little was known about COVID-19. This unprecedented and sweeping public policy was based on models that can produce wildly different results based on certain critical assumptions.REF Its purpose was to “flatten the curve,” avoiding a rapid spike in infections that could overwhelm hospital capacity and, in the best-case scenario, buy time until the discovery of a cure or vaccine. Over time, government officials created expectations that stay-at-home orders could somehow reverse the pandemic and that, in the words of Governor Cuomo, people who adhered to its strictures “won’t get infected.”
Social distancing undoubtedly contributed to protecting the New York City hospital system against a surge. But the pandemic continues to percolate there, despite widespread compliance with its strictures. Fortunately, much more is now known about COVID-19 than in March, when widespread lockdown orders began to take effect.
It is now known, that:
- The pandemic remains geographically concentrated. Infections are unevenly distributed in communities across the country, suggesting that policymakers should apply different policies in different contexts. Widespread lockdown orders that do not take these differences into account are counterproductive.
- COVID-19 is primarily a threat to the elderly. There are many differences between the seasonal flu and COVID-19 but they are similar in this respect: They both are more likely to cause serious illness and death in those age 65 and older. This suggests that policymakers should avoid establishing sweeping policies that fail to distinguish between the risks to seniors and the risk to children and young adults.
- Those with comorbidities face high risks. As with the seasonal flu, the vast majority of patients who suffer serious complications from COVID-19 have underlying medical conditions. Public policy should not treat those in good health the same way it treats more vulnerable people with chronic illnesses.
- Public officials are failing to protect those in nursing homes. COVID-19 is first and foremost a disease that is devastating to seniors living in congregate settings, including nursing homes, assisted-living facilities, and similar arrangements. Federal, state, and local officials should immediately develop and finance policies aimed at protecting the fragile elderly against this contagion.
- The case-fatality rate appears to be lower than initially feared. While COVID-19 is proving deadly to the elderly, those with pre-existing medical conditions, and to nursing home residents, it has proven much less lethal to the non-elderly population. Government statistics vastly understate the number of people who have been infected, as many are asymptomatic or suffer such mild symptoms that they may never seek medical care and receive a formal diagnosis. The specter of the Spanish flu appears very much exaggerated, as most non-elderly people with no comorbidities appear likely to tolerate the infection. This suggests that preventing children from attending school and working-aged adults from going to their jobs may be counterproductive in most communities.
- U.S. hospital capacity has so far proven robust. The U.S. has no structural shortage of hospital capacity. Nor has it run short of ventilators or ICU beds. That is not to suggest that it is immune to episodic and local shortages or that social distancing might not help check demand in areas of high infection. But fears that the macabre scenes from Milan will play out in American cities are decidedly less acute than they were in March.
- Widespread curbs on non-emergent care are ill-advised. Instances may arise where a governor may need to ban non-emergent care in a geographic area for some length of time, but statewide bans are temporarily shuttering hospital capacity and leading to layoffs in hospitals, medical practices, and clinical laboratories at a time of greatest need. It is also deepening the economic recession by hobbling a sector that has until now been considered recession-proof.REF Such bans were understandable during the early days of the pandemic, but are utterly wrong-headed at this stage.
The medical community still has a great deal to learn about the transmissibility, prevalence, and lethality of COVID-19. However, scientists have acquired enough knowledge about COVID-19 over the past several months to develop better responses to the pandemic than those that were initially employed. This new knowledge supports a more targeted approach that will better protect people from COVID-19 and allow them to begin the hard work of picking up the pieces of a shattered economy.
In particular, the data show that policymakers should take the following actions:
- Replace widespread stay-at-home orders that treat all counties in a state the same with an approach that tailors policies to local circumstances. A one-size-fits-all policy—from either the state or federal level—is bad public policy because it fails to take into account the highly concentrated distribution of COVID-19 in the U.S. In most communities, schools and most businesses can safely be reopened and citizens can resume most normal activities, although continued bans on large gatherings may be appropriate. Public officials also should continue and enhance surveillance efforts to identify potential outbreaks.
- Implement enhanced public health interventions in communities where infection rates are high. Lockdown orders were designed to buy time, not to reverse the pandemic. In hard-hit areas, officials should enhance testing capacity, implement extensive contact tracing, create temporary isolation facilities where people who have been infected can recover without putting others at risk and, in certain situations introduce travel bans to prevent people living in hotspots from seeding the epidemic in other communities.REF
- Protect those who are at greatest risk—the elderly and those with underlying medical conditions. Government measures must be both geographically targeted and demographically targeted. Seniors and those with chronic illnesses are at heightened risk from COVID-19 and public policy should urge people with these risk factors to continue to avoid exposure to the contagion. These policies should not put healthy Americans who are younger than 55 under restrictive lockdowns, except in infection hot spots.REF
- Protect those in nursing homes. The nursing-home-related COVID-19 death toll is a national disgrace. Protecting those in nursing homes is challenging. Seniors eat meals together, many suffer from dementia, and their frail conditions make them susceptible to a long list of diseases. It is harder for public officials to develop policies that protect nursing-home residents than it is to simply place everyone in a state under a lockdown order. But lockdown orders do nothing for those living in congregate settings. Public officials must rise to this challenge. Executive orders requiring nursing homes to admit COVID-19 patients should be withdrawn.REF Existing federal and state rules requiring cleanliness and establishing protocols against contagion should be rigorously enforced and more frequent inspections should be conducted.REF Federal, state, and local officials should target resources and personnel to protect the health and safety of nursing-home residents and staff. Texas Governor Abbott, for example, is deploying the National Guard to disinfect nursing homes to reduce the risk of contagion.REF Policymakers should consider underwriting part of the costs of paying nursing-home workers an additional sum to live at designated facilities during the contagion.REF Such facilities would protect residents by assuring that staff are not spreading contagion from their homes or by “floating” from facility to facility. Residents and staff should be tested frequently and protocols developed for managing situations in which someone tests positive for the virus.REF Other innovative approaches should be explored and implemented.
- End statewide bans on non-emergent care. These bans are shuttering hospital capacity and leading to layoffs in the medical field during a time of great need. Non-emergent care facilities can be used to supplement hospital capacity on an as-needed basis in specific geographic locations.
Conclusion
Widespread severe social-distancing policies were put into place when little was known about COVID-19, largely as a means to prevent hospitals from becoming overrun by a surge in critically ill patients. There remains much to learn about COVID-19—its transmissibility, prevalence, and lethality—and much to be done in order to protect Americans and begin the hard work of picking up the pieces of a shattered economy. However, nearly five months have passed since the first COVID-19 case was reported, and public officials can now make much better decisions based on the weight of the evidence.
It is now clear that younger adults and children with no comorbidities have a very low risk of falling seriously ill from COVID-19. On the other hand, older adults—especially those with underlying health conditions—do face a relatively high risk of serious illness and even death. The country’s most urgent policy imperative is to use this information to move beyond the widespread lockdown approach to the pandemic. Lockdowns are an expedient. Sound public policy requires solutions.
Norbert J. Michel, PhD, is Director of the Center for Data Analysis, of the Institute for Economic Freedom, at The Heritage Foundation. Doug Badger is Visiting Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.


