With the rapid spread of COVID-19, a deadly and novel coronavirus, the American people are in the midst of a major public health crisis.
The COVID-19 caseload is growing exponentially. According to the Centers for Disease Control and Prevention (CDC), on January 22, 2020, there was just one American case of the coronavirus. By February 22, there were 15 cases; by March 22, 33,404; by March 29, 140,904; and by April 1, 213,144.REF The CDC reports that, as of April 6, there were 374,329 cases nationwide, and 12,064 deaths. By far, New York has consistently had the largest number of cases, followed by New Jersey and Michigan.REF Projections of infection and mortality have been wide ranging, impacted by rapid changes on the ground, and highly uncertain.
In battling this virus, success will depend on strong federal–state cooperation—and even more so on the capacity and competence of governors and state public health authorities to fashion policies appropriate to the conditions on the ground.
A Federalist Approach to COVID-19
Advantages of Federalism. Fighting this disease requires presidential leadership combined with the rich arsenal of federal medical expertise in support of the states and local communities—the front lines of the response. Obviously, not all states face identical risks or have the same needs. Nor are the risks evenly distributed within states. As of April 4, as hospitals in New York City and surrounding counties braced for a surge in hospital admissions, most counties in the state reported fewer than 50 cases, and only Albany, Erie, and Monroe Counties reported more than 300 infections.REF
Because of the radically disparate impact of this epidemic on states and communities, decentralized power works better and more efficiently than centralized power. Innovative state public health policies can be quickly replicated by the governors of other states. Likewise, the damage of poorly conceived or executed policies can be confined within state boundaries, and policymakers can learn the lessons of misguided measures.
Under the U.S. Constitution, the police powers of the states, independent of the federal government, are enormous. In No. 45 of The Federalist, James Madison observes, “The powers delegated by the proposed Constitution to the Federal Government are few and defined.REF Those which are to remain in the State Governments are numerous and indefinite.” Writing in the National Review, Michael Brendan Dougherty observes:
The President doesn’t have the authority to shut down your local gin joint. Your state governor does have this power in extraordinary circumstances. That so many governors have done so, often responding to popular demand for shutdowns, demonstrates America’s genuine practice of federalism—a system that is allowing us to respond to this crisis even faster than the states of Europe that have a more monarchical or centralized system of authority for a crisis.REF
Governors and state public health officials have a broad range of options, ranging from public education and exhortations, mild guidance to practice social distancing, the avoidance of crowds and the practice of commonsense personal hygiene, to aggressive testing, statewide travel restrictions, stay-at-home rules, business closures, school closures, isolation of infected persons, and mandatory quarantines. Options are changing and policy is shifting as state policymakers respond to federal regulatory relief and assistance, providing new tools—such as diagnostics and anti-body testing—to become widely available. States have broad powers, giving them the flexibility to adapt to changing conditions on the ground.
The Federal Role. COVID-19 originated in Wuhan, China. President Donald Trump responded by quickly imposing restrictions on travel to the U.S. from China, as well as from Iran and Italy, where contagion had spread rapidly. He followed this by imposing further restrictions on European travel. In pursuing this public health strategy, the President also assembled a special task force headed by Vice President Mike Pence, including Dr. Anthony Fauci, Director of the National Institute for Allergy and Infectious Diseases and Dr. Deborah Birx, an infectious-disease specialist. As of March 23, 2020, the President had taken a total of 74 administrative and regulatory actions to combat the virus.REF His most far-reaching actions so far have been:
- Declaration of a public health emergency. Secretary of the Department of Health and Human Services (HHS) Alex Azar declared a public health emergency on January 31, 2020.REF The emergency declaration gave state, tribal, and local health departments more flexibility to request that the HHS authorize them to temporarily re-assign state, local, and tribal personnel to respond to COVID-19 if their salaries normally are funded in whole or in part by Public Health Service Act programs. These personnel can assist with public health information campaigns and other response activities. The emergency declaration also triggered statutory provisions that permit the U.S. Food and Drug Administration (FDA) to issue Emergency Use Authorizations for drugs, devices, and other medical products that can help address the emergency, even if an item has not yet received, or does not fully comply with, the law’s standard approval and marketing requirements.REF
- Declaration of a national emergency. Under current law, the President’s action enables the Federal Emergency Management Administration (FEMA) to deploy $43 billion for state and local health authorities. Since March 29, 2020, alone, FEMA has coordinated air delivery of 80 tons of medical equipment, including 130,000 respirators, 1.8 million protective masks, 10.3 million gloves, and “thousands” of thermometers for New York, New Jersey, and Connecticut, with more flights scheduled for Illinois and Ohio.REF The declaration also opened up a new set of deregulatory options at the HHS, which helped, for example, to accelerate access to telemedicine in Medicare.
- Invocation of the Defense Production Act. By invoking this law, the President enabled the federal government to secure vital medical equipment from private industry, including protective gowns, masks, gloves, and ventilators and respirators to cope with the expected massive surge in hospitalizations.
- Enlistment of assistance from major private-sector companies. The President has encouraged the private sector to join the battle in a very big way, and major companies are volunteering to help the country combat the coronavirus. For example, Ford Motor Company, the automotive giant, is transitioning certain production lines to manufacture much-needed ventilators for the severely ill, while biomedical research firms are working at breakneck speed to develop COVID tests and therapeutics to identify and reduce the contagion. On February 1, the Secretary of HHS initiated the first emergency use authorization to expand access to testing and equipment. Since then, the FDA has been working with over 200 test developers and has issued 34 Emergency Use Authorizations for diagnostic tests,REF while “several hundred” clinical trials are underway for therapeutics, including the anti-malaria drug hydroxychloroquine and the anti-viral drug Remdesivir, to ameliorate the illness.REF
- Reduction of red tape. Administration officials are providing vital relief from pre-existing and outdated federal regulations that inhibited the United States from developing and deploying the tests necessary to identify, target, and contain this dangerous virus. The initial and spectacular failure of the CDC and the FDA to approve and distribute the tests was a textbook failure of bureaucracy, resulting in a delay and denial of the ability of academic and private research centers to develop or use tests.REF Without the ability to develop and rapidly deploy vital testing, the United States fell behind other nations in this area, particularly South Korea. South Korea’s rapid testing and isolation of infected individuals was key to its indisputable success in containing the spread of the virus. The good news is that, as of March 30, 2020, the United States is recovering its testing capacity, and has conducted over a million tests, at the rate of approximately 100,000 per day.
- Support for major economic relief. In signing the Coronavirus Aid, Relief, and Economic Security (CARES) Act into law, the President allocated an unprecedented $2 trillion for a “whole government” response to the pandemic, including $100 billion for hospitals, $27 billion for research and development of vaccines and medical supplies, direct economic assistance to workers and their families, and $350 billion in loans to small businesses.REF
The Battle Against COVID-19: States and Local Governments Must Lead. The battle against COVID-19 will be won or lost on the ground. No two states or communities are the same. That is why state and local public health authorities are best able to handle this crisis. Because different states have different circumstances, they will apply different public health measures to cope, depending on the extent or threat of the contagion. Perfect solutions are, of course, non-existent.
New York City is the epicenter of the COVID-19 infection as of April 6, with the largest caseload in the United States, followed by New Jersey (mostly in counties adjacent to New York City), and Michigan. Public health crises are rapidly developing elsewhere, including San Francisco, Miami, and New Orleans. In the near term, as Dr. Fauci and others have warned, Americans will experience explosive caseloads and a rising death toll. In certain areas of the country, quarantines, of one degree or another, are going to be maintained for some time. In other areas of the country, where the infection rates are, or at least appear to be at present, relatively low, the public health strategies will be more relaxed.
Policy Options for State and Local Officials: Social Distancing vs. More Aggressive Public Health Measures. The Trump Administration has extended its “Slow the Spread” guidance for Americans beyond the initial 15 days until April 30. The President’s guidance calls on Americans to listen to, and follow, the directions of state and local authorities, while avoiding social gatherings of more than 10 persons, working from home if possible, and diligently practicing personal hygiene.REF
Consonant with the objectives of the federal initiative, state officials are also implementing a combination of strategies—many with the force of law. These include:
- Social distancing and stay-at-home rules. As of April 2, 41 states and the District of Columbia, as well as 12 Indian tribes, have issued “stay at home” orders.REF Governor Larry Hogan (R) of Maryland, for example, has issued a fairly comprehensive executive order that requires Maryland citizens to remain at home except to go to a workplace that is deemed “essential” or to go to grocery shopping, exercise, seek medical treatment, or go to the assistance of family or friends. Violation of Maryland’s emergency order carries with it a $5,000 fine or one year’s imprisonment, or both.REF The District of Columbia and the Commonwealth of Virginia have adopted similar measures.
- Aggressive testing. Testing is critical to getting control of the pandemic while allowing Americans to shift away from “stay at home” approaches and begin to resume their daily lives. Though the United States initially failed to secure the rapid and widespread testing, more COVID-19 tests are coming on line, spurred by Administration action. As of March 30, 2020, the United States has conducted approximately 1 million tests. Abbott Labs, for example, has developed a test that can detect the presence of the virus in as little as five minutes’ time. The more aggressive and widespread the testing, including the use of drive-through test sites, the greater chance that public health authorities will have of getting control of the pandemic. Testing people who are merely symptomatic is insufficient: The initial symptoms, fever, cough, or fatigue, are similar to other medical conditions, such as a seasonal flu or the Epstein–Barr virus.REF Moreover, symptoms of COVID-19 are often mild and may not show up in a patient until as many as 14 days after infection. While public health authorities cannot test everybody in a given state or community, their range of testing should be broad enough, say, through a random sample of the community, for them to get a clear picture of the extent of the prevalence of the virus.REF Finally, public health authorities not only have to identify infected persons, but trace their contacts, and track them to ensure their recovery.REF
- Self-isolation and quarantine. Depending on the prevalence of infection and the particular conditions on the ground, state public health authorities have broad authority to experiment and pursue different strategies. Quarantines are a long-used response to infectious disease. During the Ebola crisis of 2014, for example, the State of Georgia imposed a quarantine of 21 days on infected persons, checking them twice a day, while housing health care workers in separate facilities. To calm the fears of the public, Georgia assembled a strong state task force, comprising prominent physicians and nurses, who communicated effectively and regularly on the latest developments. Georgia hospitals worked closely together in sharing information and resources, including providing their ambulances with the same information for picking up and discharging patients, and distributing new patients among the hospitals in an efficient and equitable fashion.REF
The Path Forward: Emerging Lessons from Italy and South Korea
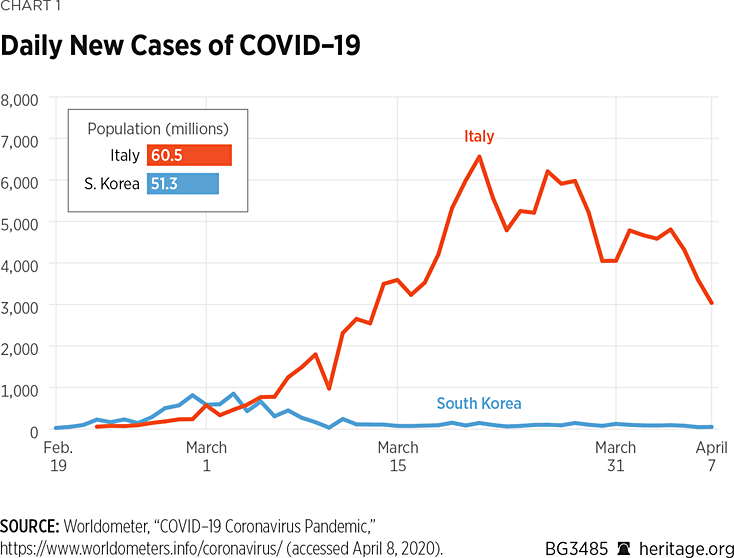
With the coronavirus, the U.S. and most European countries have generally adopted the tactic of social distancing and self-quarantine of infected people whose symptoms are mild enough not to require hospitalization. This is the practice pioneered in Italy, with less-than-satisfactory results. As Chart 1 shows, the number of new cases increased in Italy at a rate of more than 6,600 per day at its apparent peak on March 21. Over the next 10 days, the daily new case rate at one point dropped to just over 4,000 (March 30). During the first week of April, the daily number of new cases remained below 5,000. On April 7, 3,039 new cases were reported, the smallest number since March 13. Assuming that this encouraging trend holds, it will take some time for the number of active cases to decline sufficiently to give officials the confidence to relax the practice.
The Italian approach to COVID-19 involves social distancing enforced by military police and local authorities. Patients who test positive either are sent home, where family members often include grandparents, or to hospitals, which have become, in the view of physicians practicing at an overcrowded hospital in Bergamo, “the main COVID-19 carriers, as they are rapidly populated by infected patients, facilitating transmission to uninfected patients.”REF In short, infected people are placed in close quarters with uninfected fellow patients or family members. There is at least some reason to question whether this is the most effective means of limiting transmission of the pathogen or whether it may facilitate transmission.
In South Korea, officials detected the outbreak a few days before Italy began logging cases. New cases in Korea topped those in Italy through March 3. Since then, the pandemic has followed very different patterns in the two countries. The number of daily new cases in Korea declined fairly dramatically from its March 3 peak of 851, and has hovered at around 100 per day since March 12. Italy’s daily new case rate, as noted, seems to have peaked at more than 60 times that level, although it appears to have begun a gradual decline.
Korea’s COVID-19 response has vastly outperformed Italy’s (and that of every other Western country, including the U.S.) by every metric. As of April 7, COVID-19 had claimed the lives of more than 17,000 Italians, while just over 24,000 had recovered. In Korea, 6,676 people have recovered, while only 200 have died. On that same day, nearly 3,800 Italian COVID-19 patients were critically ill, compared with just 55 in Korea. The infection rate per million population was 2,243 in Italy, more than 11 times as high as Korea’s at 203 per million people.
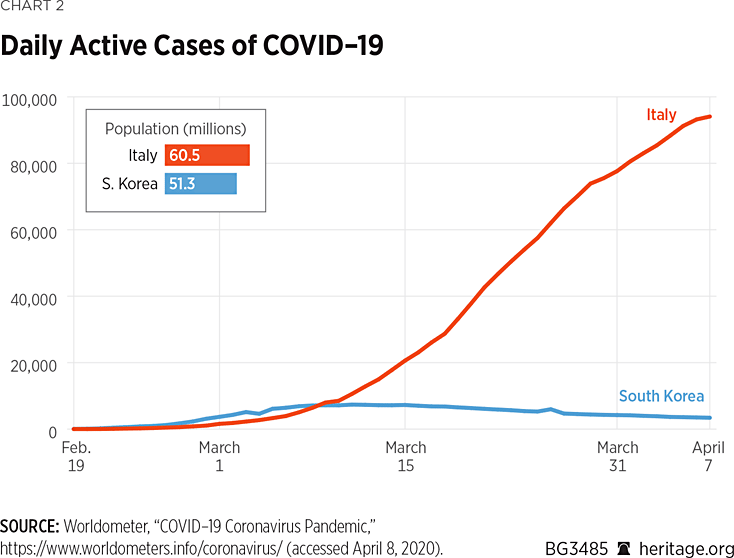
The result, as Chart 2 shows, is that active cases in Italy (total cases minus recoveries minus deaths) continues to grow in Italy (albeit at a slower rate than the week before), while active cases in Korea have been declining since March 11, when they topped 7,300. As of April 7, that figure stood at 3,408.
There are many reasons why Korea has managed to outperform every other country affected by COVID-19.REF The Korean government took a different strategy. It developed and distributed tests more quickly, imposed domestic travel restrictions to help isolate hotspots, established temporary testing centers and tested more extensively, used thermal imaging in large buildings and thermometers at restaurants to identify febrile patrons, used app-based technology to facilitate contact tracing, and transferred people who tested positive to temporary isolation facilities.REF
This has allowed South Korea to keep retail shops, bars, restaurants, and other public accommodations open, while still limiting the threat of contagion. Gyms are closed, as are public parks, but South Korea has not required highly disruptive policies that portend devastating economic damage.REF
Lessons from Italy and South Korea. It is too late to replicate the Korean results in the U.S. or elsewhere in the West where the pandemic has spread. There is no substitute for identifying an outbreak early. But with tests becoming more widely available, a broad-based testing regime is becoming more feasible in the U.S. South Korea has demonstrated the utility of widespread testing in helping to curb COVID-19 spread.
South Korea also used travel restrictions to keep the epidemic from spreading beyond an initial hotspot in the city of Daegu. The U.S. can stop the spread of infectious disease, not only from foreign countries, but also between states. While the President may not ban travel within a state, he is constitutionally empowered to ban travel between states.REF Whether the President should exercise such power is a prudential question, and dependent, once again, on his assessment of the conditions on the ground. A federal quarantine of a state would be a dramatic step. In the worsening cases of New York City and its immediate environs, however, such an action may be necessary to protect people from a devastating outbreak.REF
There are other elements of the South Korean model that could be adapted to the U.S. context. The use of smartphone apps to enhance contact tracing should be feasible. If a patient who tested positive had lunch at a particular restaurant, for example, the South Korean government uses the app-based technology to notify people in the area of the name of the establishment and the date and time when the infected person dined there. People who also were there at the time are encouraged to be tested for the virus.
Korean public health officials also have adopted a policy of keeping infected people away from uninfected people. Those who test positive for COVID-19 are housed in repurposed facilities (a dormitory, for example) until they test negative. Then they are released. This process appears to be more effective than sending infected patients home or to the hospital, where they expose others to the pathogen.
State and local officials may be reluctant to isolate patients who test positive for COVID-19. A mandatory isolation policy would raise thorny legal issues and may be regarded as inconsistent with constitutionally guaranteed civil liberties. States do, however, have broad authority reserved to them by the Tenth Amendment to impose quarantine as an exercise of the police powers within their borders. Under current law the federal government and the President himself retains significant power to protect the public.
As an alternative to mandating the isolation of people with coronavirus, government officials could create such isolation facilities and make their use voluntary for those who test positive for the virus. To be effective, this would have to be accompanied by a public education campaign, similar to the ones the federal and state governments have been using with considerable success to gain extensive public compliance with social distancing strictures. The campaign would aim to persuade people that protecting their loved ones by entering voluntary isolation is preferable to exposing them to contagion.
Federal, state, and local officials might consider testing this idea in a geographical area that is at risk of outbreak. If the effort is successful in containing spread of the virus, it could become a template for future containments.
If strategies like this are successful, they might expedite the loosening of social distancing policies. As Italy is demonstrating, these policies, once begun, are difficult to reverse. The internal logic of social distancing dictates that, as long as infected people are circulating in the community, everyone must treat everyone else as a carrier. This erodes the trust that binds communities together and enables commerce. Once a shop is closed because it is thought to pose a public health risk, the burden of proof rests with those who would pronounce it safe to re-open. At what point is it alright to allow a hair salon or a gym or a restaurant or a spa to resume operations? Social distancing offers no clear answer. The longer the closure remains in effect, the more likely that the proprietor will lack the financial means to re-open it, even if the government were to permit it. And, when it does open again, will public confidence in its safety be restored if the virus is still spreading abroad?REF
Active cases are on the rise in every country that relies primarily on social distancing as a tool to curb the epidemic.REF South Korea is an outlier, both in reversing the epidemic and in its low level of reliance on social distancing. Italy, which has had a broad policy of social distancing in place longer than other countries, has shown that adherence to the policy must persist, even where the rate of increase in new cases has begun to decline.
Flattening the Curve
The United States has experienced an exponential growth in the number of cases, and a corresponding increase in the number of deaths. With widespread testing, particularly if accompanied by one or more of the strategies discussed in the previous section, epidemiologists can assess progress in controlling the spread—state by state, and in the nation as a whole.
As the curve flattens and new cases decline, and as the number of patients who recover outpaces the number of new infections, public health authorities will know that they are winning the battle against the virus, and can start to relax the stay-at-home orders, self-isolation, and quarantines. Reaching that point as quickly as possible and avoiding economic cataclysm should be the highest priority of Congress, the White House, and state and local officials.
The longer that resolution is delayed, the greater and more lasting the economic devastation. Those effects already have begun. On March 26, 2020, the Department of Labor announced that the number of claims for unemployment insurance had set a new record that week, with 3.3 million people applying for benefits.REF The following week, that record was shattered when claims doubled to 6.6 million.REF Miguel Faria-e-Castro, an economist with the St. Louis Federal Reserve, has issued a rough estimate that the unemployment rate could rise to 32 percent during the second quarter of 2020 due to social distancing, a rate that would be nearly 10 times the February 2020 rate of 3.5 percent.REF Moody’s has estimated that gross domestic product growth on an annualized basis will contract by 30 percent over the second quarter, and by 75 percent if social distancing continues through June.REF
Conclusion
The highly contagious coronavirus, COVID-19, is on track to infect millions of Americans, and the virus, depending on the effectiveness of public health measures, will exact a large death toll. Government policy is critical to equipping medical providers to change this path.
Every state faces different challenges, and the conditions for success vary greatly, based on demography, public compliance, and the capacity of medical professionals and health workers to cope with the surge in demand for medical care. While the President and federal health officials should provide vital information, guidance, and material and technical support, the actions of state and local officials and citizens, medical professionals, and health care workers will be decisive in this effort.
As more tests become available, state officials will be able to adopt a broader variety of strategies, ranging from social distancing to mandatory isolation and quarantine, while learning from both domestic and international experience, including the comparative performance of Italy and South Korea.
Appropriate public health measures, based on state and local conditions, can arrest the rate of infection, flatten the curve, and bend it downward, so that current public health restrictions can be lifted, and Americans can soon return to a normal social and economic life.
Robert E. Moffit, PhD, is Senior Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation. Doug Badger is Visiting Fellow in Domestic Policy Studies,




