Health insurance coverage appears to have so far been quite stable in the face of COVID-19’s economic dislocations.
In addition, the health system appears to have rebounded from the cancellation of non-emergency medical care back in the spring, which was instituted to free up capacity to cope with COVID-19 cases.
Because most working Americans and their dependents have health insurance through employer-sponsored plans, analysts and policymakers raised concerns that millions of Americans could lose their health insurance coverage as a result of the sudden employment dislocation due to the COVID-19 shutdown. Indeed, some analysts projected substantial coverage losses.REF
Insurance actuaries also attempted to estimate the net effect on health insurance claims from new costs for COVID-19 cases and reduced medical spending for other care.REF
While the available data for the first three quarters of 2020 is not comprehensive, it does offer some initial insights on COVID-19’s actual effects on coverage and costs. (See the Appendix for a discussion of data and methodologies.)
Enrollment Changes in 2020
Data indicate that enrollment in private insurance coverage remained fairly stable during the first three quarters of 2020.
For the individual (non-group) market, since the Affordable Care Act (ACA or Obamacare) went into effect in 2014, a new annual pattern has emerged consisting of a first-quarter enrollment surge (as coverage sign-ups during the annual open season take effect) followed by net enrollment declines over the course of the subsequent three quarters. As a result, individual market enrollment since 2014 has been highest at the beginning of each year and lowest at year-end. Consistent with that pattern, individual market enrollment increased in the first quarter of 2020, as Table 1 shows.
However, this year the expected enrollment decline during the second quarter did not occur, and there was only a slight decline (1.2 percent, or 179,000 individuals) in the third quarter. The COVID-19 outbreak and associated economic dislocation may have induced more enrollees to maintain their coverage, or the number of enrollees dropping coverage during the second and third quarters may have been largely offset by new enrollments—or both.REF
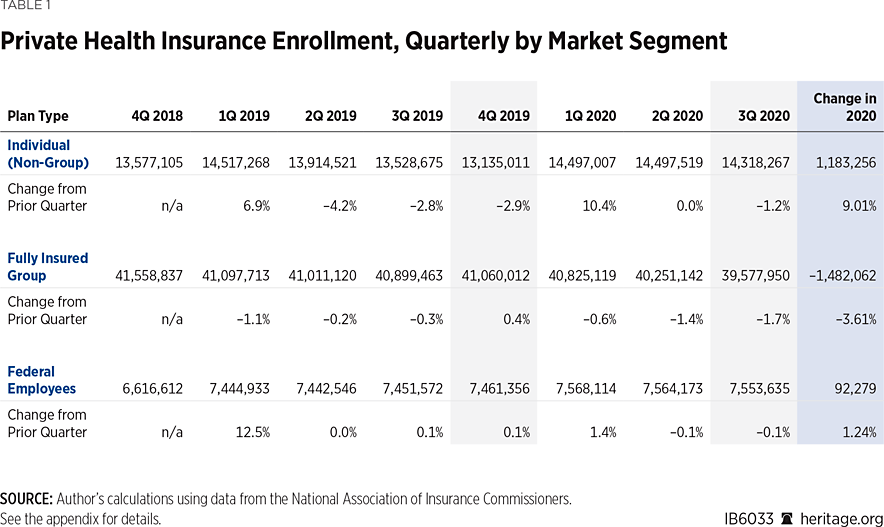
For the fully insured group market, Table 1 shows that there was a modest enrollment decline—3.6 percent—almost all of which occurred during the second and third quarters. That tracks with the time frame of COVID-19-related economic dislocation beginning in March. However, given that fully insured group plans are purchased primarily by small and medium-size firms (while larger businesses tend to self-insure their health plans), the enrollment decline among fully insured group plans was modest, even though smaller businesses generally suffered more from the lockdowns than did larger firms.
Not surprisingly, there was virtually no change this year to enrollment in the private plans offered to federal government workers through the Federal Employee Health Benefits Program.
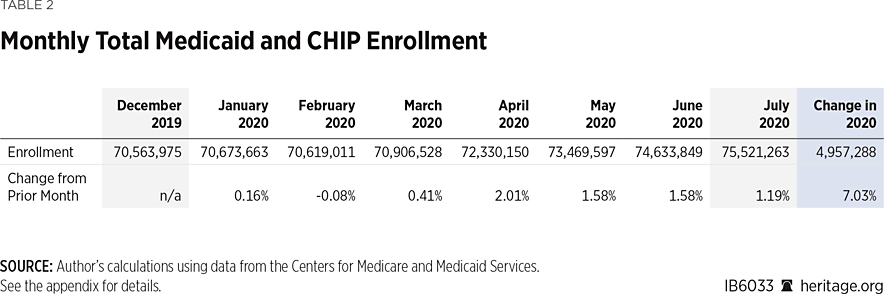
Table 2 shows that during the first six months of 2020, total enrollment in Medicaid and the Children’s Health Insurance Program (CHIP) increased by 5.77 percent, or 4 million individuals, and grew by a further 1.2 percent (another 887,000 individuals) in July. Almost all of that increased enrollment in Medicaid and CHIP took place after March, coinciding not only with the onset of COVID-19-related economic dislocation but also with two temporary program changes that Congress enacted in response to COVID-19.REF
Thus, much of the net increase in Medicaid and CHIP enrollment likely reflects the temporary retention or addition of individuals who would not have qualified for coverage under normal eligibility criteria. Also, some individuals may have become newly eligible due to COVID-19-related reductions in income, and some who were already eligible, but not enrolled, may have sought coverage in response to COVID-19.REF Researchers have long observed that a portion of the population eligible for Medicaid or CHIP at any given time are not enrolled in those programs.REF
The biggest unknown is the effect COVID-19-related economic dislocation had on enrollment in self-insured employer plans. Those plans cover about 110 million individuals, but data on their enrollment is collected and reported only on an annual basis, so data for 2020 is not yet available. However, news reports indicate that many large employers with self-insured plans enabled furloughed workers to retain their existing coverage. For instance, some employers suspended requirements that furloughed employees pay a share of their premiums to maintain coverage.
Changes in Claims Costs
Table 3 presents data on average monthly per-enrollee claim costs for commercial health insurance plans by market segment. The data indicate that, during the first half of the year, any additional claims incurred in connection with cases of COVID-19 were more than offset by reduced claims for other care.
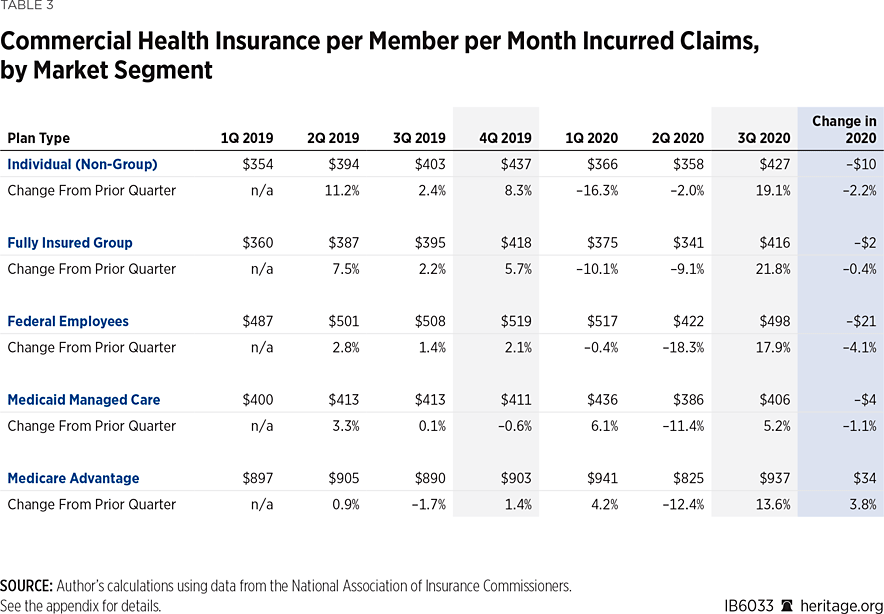
That was particularly true for the three market segments—individual, group, and federal employees—that cover workers and their dependents. Table 3 shows that the prior trend of steadily increasing claim costs reversed during the first half of the year, with each of those three market segments posting declines of around 18 percent for the first half of 2020.
In contrast, average monthly claim costs for Medicaid managed care and Medicare Advantage plans both increased somewhat in the first quarter of 2020 but then dropped (by 11 percent and 12 percent, respectively) in the second quarter.
Some portion of the first quarter increase in claims costs in private Medicare and Medicaid plans may have been attributable to COVID-19 cases. It is now well established that the elderly and those with underlying medical conditions are at much higher risk of suffering serious adverse effects from COVID-19.REF Not only are higher-risk patients more likely to be hospitalized and need more intensive (and expensive) medical care; they are also more likely to be non-workers covered by Medicare or Medicaid.
However, Table 3 also shows that the declines experienced during the first two quarters of 2020 were almost entirely reversed in the third quarter, as average monthly per-enrollee claim costs rebounded to their 2019 pre-COVID-19 levels. The timing of that effect is consistent with the health care sector returning to more normal operations in most of the country during the third quarter.
The Outlook Going Forward
During the third quarter, a number of states began to ease restrictions on business activity, and the unemployment rate has steadily declined from its lockdown-induced peak of 14.7 percent in April to 6.7 percent in November.REF To the extent that economic activity continues to rebound, there is less reason to anticipate significant future declines in employment-based health insurance coverage. However, that could still change if the recent surge in cases—and the accompanying reimposition of restrictions on businesses in many states—continue for several more months.
In general, health insurance coverage appears to have so far been quite stable in the face of COVID-19’s economic dislocations. That may partly be attributable to employers maintaining furloughed workers on their current coverage. It is likely also due to the fact that those who do lose job-based coverage have alternatives, including COBRA coverage, replacement individual market coverage, or (if they are low-income) public coverage through Medicaid or CHIP.
Also, the rebound in per-enrollee average claim costs in the third quarter indicate that the effects of suspending non-emergency medical care in the spring have largely played out.
While it is still possible that the current surge in COVID-19 cases might strain health system capacity in some locations, any repeat of the widespread suspension of non-emergency medical care now seems both unnecessary and unlikely. Consequently, the concerns that led Congress in the Coronavirus Aid, Relief, and Economic Security Act to appropriate billions of dollars in payments to medical providers to offset lost income should not be a consideration in any new COVID-19-related legislation.
Conclusion
Insurance market data for the first three quarters of 2020 show that, contrary to initial fears, the economic dislocation caused by COVID-19 did not appear to have had a significant adverse effect on health insurance coverage. In fact, indications are that health insurance enrollment has remained fairly stable this year.
Also, the data on health insurance claim costs indicate that the sharp drop in provider incomes attributable to the cancellation of non-emergency medical care in the spring was a temporary phenomenon that largely reversed in the third quarter. The rebound of average per-enrollee claim costs to pre-COVID-19 levels indicates that medical providers have now resumed most patient care.
The insights from this data, along with the current expectations for widespread COVID-19 vaccinations over the course of the first half of 2021, indicate that further COVID-19-related federal subsidies for either health insurance coverage or medical providers are not needed at this point.
Edmund F. Haislmaier is Preston A. Wells, Jr. Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.
Appendix: Data and Methodology
Enrollment Data
Data for private-market enrollment by market segment is derived from insurer regulatory filings compiled by the National Association of Insurance Commissioners (NAIC), as well as filings by companies regulated by the California Department of Managed Care, and was accessed through Mark Farrah Associates.REF
Plans that file as life insurance companies only report annually and thus were not included in the calculations of quarterly enrollment. Those plans account for about 4 percent of total individual-market enrollment and about 18 percent of total fully insured group-market enrollment.
Medicaid and CHIP enrollment figures are from the Centers for Medicare and Medicaid Services (CMS) state-level monthly enrollment reports.REF
Claims Data
Data for incurred claims and member months was also obtained from quarterly insurer regulatory filings compiled by the NAIC. Plans that file as life insurance companies and plans regulated by the California Department of Managed Care do not report that data on a quarterly basis and thus were not included. Also excluded were plans that were not in operation during all of the seven quarters on which the analysis was based, and plans identified as having missing or erroneous data. The resulting datasets used for claim cost calculations consisted of:
- Individual Market: 213 plans with 11 million enrollees;
- Fully Insured Group Market: 268 plans with 26 million enrollees;
- Federal Employee Market: 91 plans with 6 million enrollees;
- Medicare Advantage Market: 328 plans with 18 million enrollees; and
- Medicaid Managed Care Market: 160 plans with 37 million enrollees.



