The economic dislocation caused by government responses to the COVID-19 pandemic last year had less of an adverse effect on health insurance coverage than was initially feared, according to data. Because most working Americans and their dependents have health insurance through employer-sponsored plans, analysts and policymakers had raised concerns last spring that millions of Americans could lose their health insurance coverage as a result of the sudden employment dislocation due to the COVID-19 shutdowns. Indeed, some analysts had projected substantial coverage losses.REF
Insurance Enrollment Changes in 2020
While enrollment in private employment-based coverage did decline somewhat in 2020, that reduction was more than offset by increases in private individual-market coverage and public program coverage through the Children’s Health Insurance Program (CHIP).REF (See Table 1.)
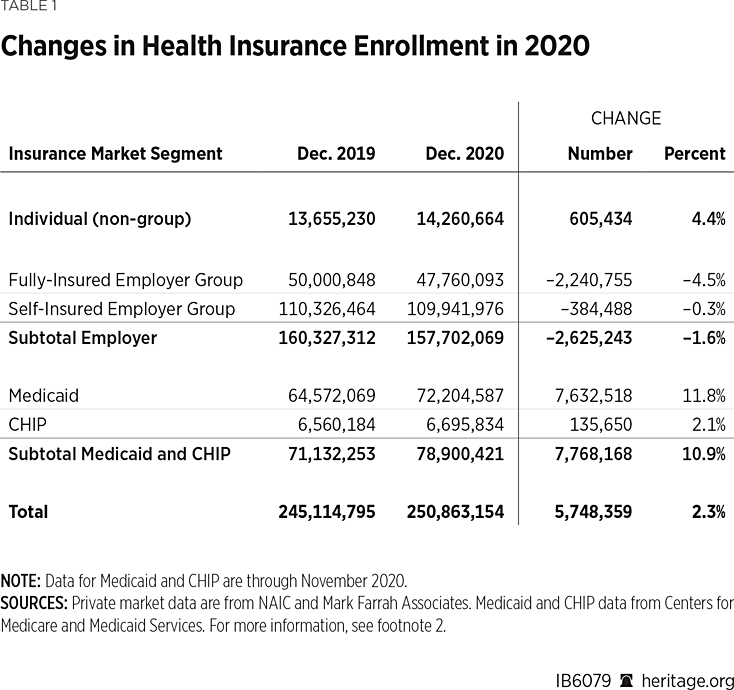
Some observations:
- The bulk of the coverage losses occurred in the fully insured employer-group market, where enrollment dropped by 2.2 million individuals, or 4.5 percent, from 50 million individuals at the end of 2019 to 47.8 million at the end of 2020.
- In the self-insured employer-group market, which is more than twice the size of the fully insured market, enrollment decreased by only 384,000 individuals (or 0.3 percenvt) from 110.3 million in 2019 to 109.9 million in 2020.
- In contrast, enrollment in individual market plans increased by 605,000 individuals (or 4.4 percent) from 13.7 million individuals at the end of 2019 to 14.3 million at the end of 2020.
- By far, the biggest change in 2020 was the substantial increase in enrollment in public programs. Enrollment in Medicaid and CHIP increased by 7.8 million individuals (or 10.9 percent) from 71.1 million in 2019 to 78.9 million in 2020. As Table 1 shows, almost all (98 percent) of that increase was in Medicaid, with CHIP enrollment increasing by only 135,000 individuals, or 2 percent.
In sum, the overall effect was that in 2020 net enrollment in private coverage (group and non-group) decreased by 2 million individuals, or 1.2 percent, while enrollment in public coverage (Medicaid and CHIP) increased by 7.8 million individuals, or 10.9 percent.
Likely Effects of Government Response to COVID-19
In the employer-group market, fully insured plans are purchased primarily by small and medium-size firms, while larger businesses tend to self-insure their health plans. Prior to 2020, enrollment in fully insured plans was gradually declining by 1 percent to 2 percent per year, while enrollment in self-insured plans was increasing at about the same pace.
Thus, at least half of the 2020 enrollment decline in fully insured employer plans was likely due to the effects of government responses to COVID-19, as smaller businesses generally suffered more from the lockdowns than did larger firms.
The substantial increase in enrollment in Medicaid and CHIP reflects not only COVID-19-related economic dislocation but also two temporary program changes that Congress enacted in response to COVID-19. The Families First Coronavirus Response Act (enacted March 18, 2020) temporarily increased federal funding for state Medicaid programs but conditioned the extra funding on states continuing to cover, for the duration of the health emergency, individuals who were already on Medicaid. The CARES Act (enacted March 27, 2020) temporarily increased unemployment compensation payments and specified that the additional payments were not to be counted as income for purposes of determining Medicaid or CHIP eligibility.REF
Thus, much of the net increase in Medicaid enrollment likely reflects the temporary retention or addition of individuals who would not have qualified for coverage under normal eligibility criteria. Also, some individuals may have become newly eligible due to COVID-19-related reductions in income, and some who were already eligible, but not enrolled, may have sought coverage in response to COVID-19.REF
Policy Implications
In general, private health insurance coverage remained fairly stable in the face of COVID-19-related economic dislocations. That may have been partly the result of employers maintaining furloughed workers on their current coverage. It was also likely due to the fact that those who do lose job-based coverage have alternatives, including COBRA continuation coverage, replacement individual-market coverage, or (if they are low-income) public program coverage through Medicaid or CHIP.
The experience of 2020 indicates that there do not appear to be any significant systemic gaps or barriers to people maintaining or switching health insurance coverage in response to changing economic circumstances. Consequently, Congress increasing taxpayer subsidies for health insurance coverage is not likely to have much effect on enrollment. For instance, in the last COVID-19 bill, Congress temporarily (for 2021 and 2022) expanded eligibility and increased subsidies for those purchasing individual-market exchange coverage and also created new temporary subsidies for continuation coverage for those losing employment-based coverage.REF Yet those continuation coverage subsidies were largely unnecessary, as under Obamacare individuals eligible for unsubsidized continuation coverage already had the option of enrolling in subsidized exchange coverage instead.
Furthermore, economic research finds that many low-income uninsured individuals do not enroll in even heavily subsidized coverage unless they incur a medical condition that entails paying more than they normally do for medical care.REF In part, that is due to the widespread availability of “charity care” provided by hospitals and clinics at low or no cost to low-income individuals. Also, some public policies—such as retroactive eligibility for Medicaid coverage and the creation of numerous exceptions allowing for enrollment in subsidized exchange coverage outside of the annual open season—reinforce the tendency among low-income uninsured individuals without significant and immediate medical needs to not enroll in coverage unless and until they have to do so to avoid incurring more than nominal out-of-pocket costs for treatment.
That is consistent with what researchers have long observed about Medicaid—namely, that at any given time, a significant portion of the population eligible for Medicaid is not enrolled in the program.REF
In sum, policies that simply expand the availability of free or nearly free coverage as a strategy for covering the remaining low-income uninsured population are unlikely to have much, if any, measurable effect.
A more productive approach would include Congress reforming existing programs—which currently provided tens of billions of dollars per year to hospitals and clinics to offset their costs for treating low-income uninsured patientsREF—and allowing patients to apply subsidies from other programs (such as CHIP, Medicaid, and Obamacare) to any private coverage of their choice. Such an approach would allow needy patients to receive subsidy dollars and apply them toward the public or private coverage for which they are already eligible.
Conclusion
The data show that health insurance enrollment remained relatively stable in 2020 despite widespread economic dislocation caused by government responses to the COVID-19 pandemic.
That suggests that Congress’s health reform agenda going forward should focus on reducing costs by expanding choice and competition.
In addition, rather than simply expanding eligibility and subsidies, the better approach for addressing the residual uninsured population is through reforms that enroll them in coverage for which most are already eligible. Today, those individuals are essentially “functionally insured”—meaning that they seek and receive free medical care when and as needed—but are not “formally insured.” The main benefit of identifying and enrolling those individuals in formal coverage, particularly through private managed care plans, is that they will be more likely to get care sooner and in more appropriate settings.
Edmund F. Haislmaier is Preston A. Wells, Jr. Senior Research Fellow in Domestic Policy Studies, of the Institute for Family, Community, and Opportunity, at The Heritage Foundation.



