The spread of COVID-19, the disease caused by the new SARS-CoV-2 coronavirus, became a serious concern worldwide in March 2020, when on March 11, the World Health Organization (WHO) designated COVID-19 to be a pandemic.REF Now present in more than 200 countries, having infected more than 13 million people—with the Johns Hopkins Coronavirus Resource Center now reporting that over 570,000 of those coronavirus cases have ended in death—the epidemic has become the top priority of policymakers all across the globe.REF
Given that it will take time to develop a vaccine for this novel virus, and that many experts believe that the virus is still in the early stages of its progression, it is important to examine different policy approaches to combatting the epidemic. This Special Report examines the various approaches different countries have taken, as well as approaches here in the United States. The Special Report elucidates which policies have been successful so far and could potentially be adapted in other countries to save as many lives and livelihoods as possible.
Naturally, various countries began their experience with COVID-19 at slightly different times, and many varying demographic, medical, and geographic factors have affected the proliferation of the virus in different countries. Italy, for example, has a greater portion of elderly citizens than other countries, and Iceland has a much younger population. In the United States, large segments of the population suffer from pre-existing conditions, such as diabetes and obesity, both of which are linked to significantly higher rates of COVID-19 deaths than for those without comorbidities. The United States leads the world in obesity at about 33 percent of the population, while in Sweden the number is around 12 percent. Separately, some countries have a greater population in urban centers versus rural areas, facilitating greater spread of the virus.REF
While these many differences make it difficult to isolate single policies as the sole cause of varying outcomes in different countries, these comparisons are necessary to determine which factors to control for and, ultimately, which policies work best. This Special Report begins with a discussion of the situation here in the United States, and continues with a discussion of the circumstances and approaches in several other countries with varying levels of economic freedom as identified in The Heritage Foundation’s Index of Economic Freedom.REF This Special Report concludes with several recommendations for U.S. policymakers to improve outcomes related to the COVID-19 pandemic.
U.S. Analysis
The United States has a population of more than 329 million people. The first reported case of COVID-19 in the United States was on January 21, 2020, in Washington State,REF although—as is the case in other countries—the first actual case may never be pinpointed, and the virus is now known to have been circulating before this day.REF Cases and deaths quickly grew during the first few months of the year.REF As of June 27, 2020, there have been 2,467,837 confirmed COVID-19 cases (0.75 percent of the U.S. population) and 125,039 deaths attributed to the disease (about 5 percent of the confirmed cases, and 0.04 percent of the U.S. population).REF Although all 50 states have reported cases of COVID-19, the distribution has been much more heavily concentrated in some places than in others, as Maps 1-4 illustrate.
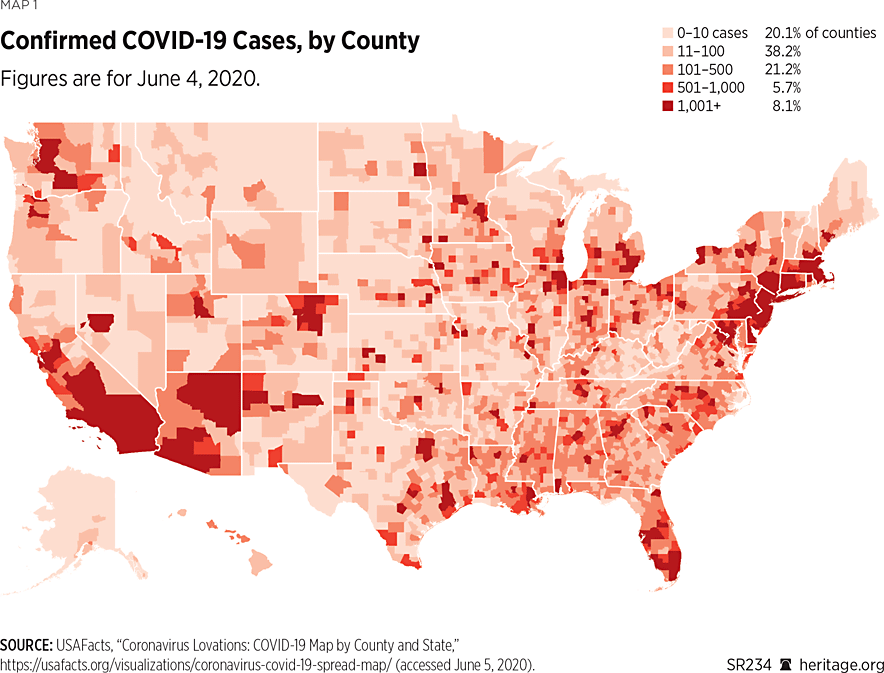
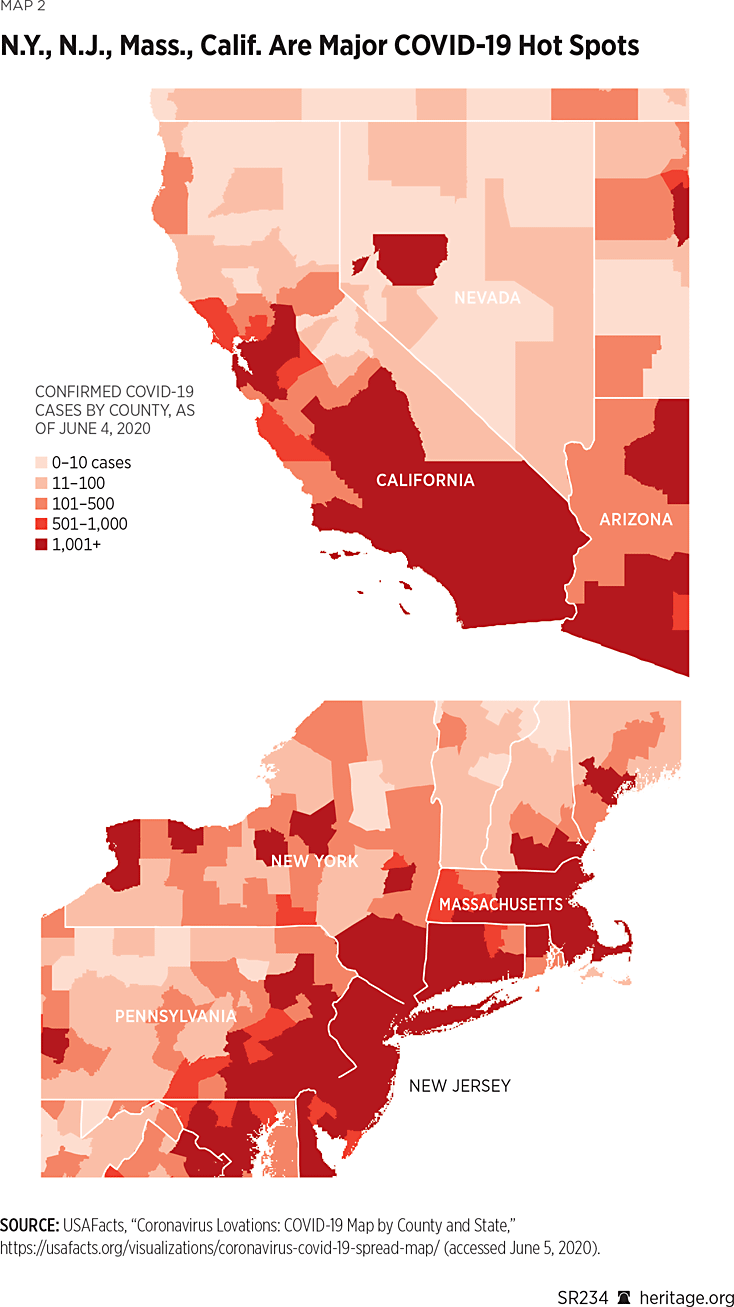
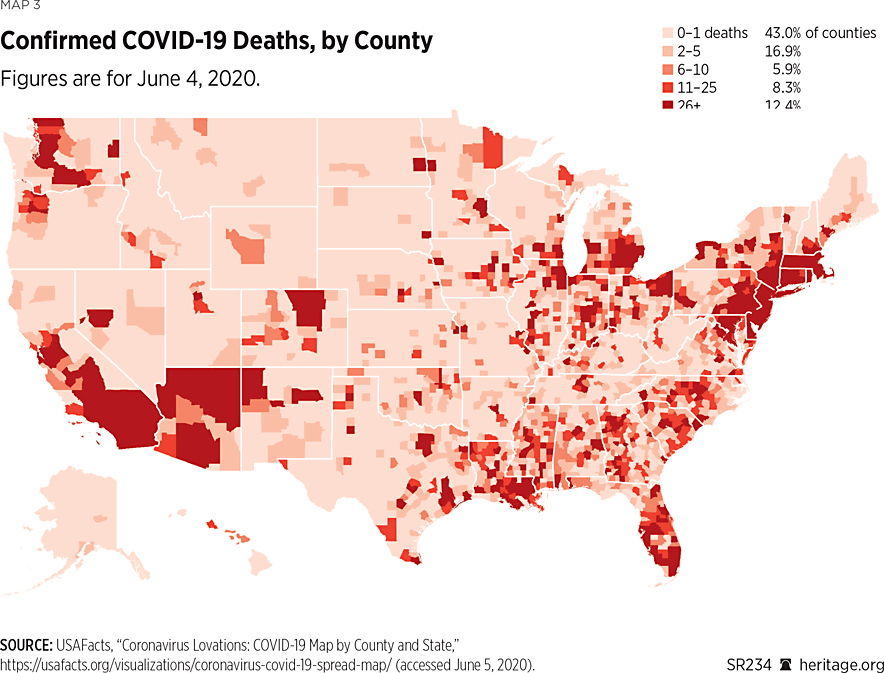
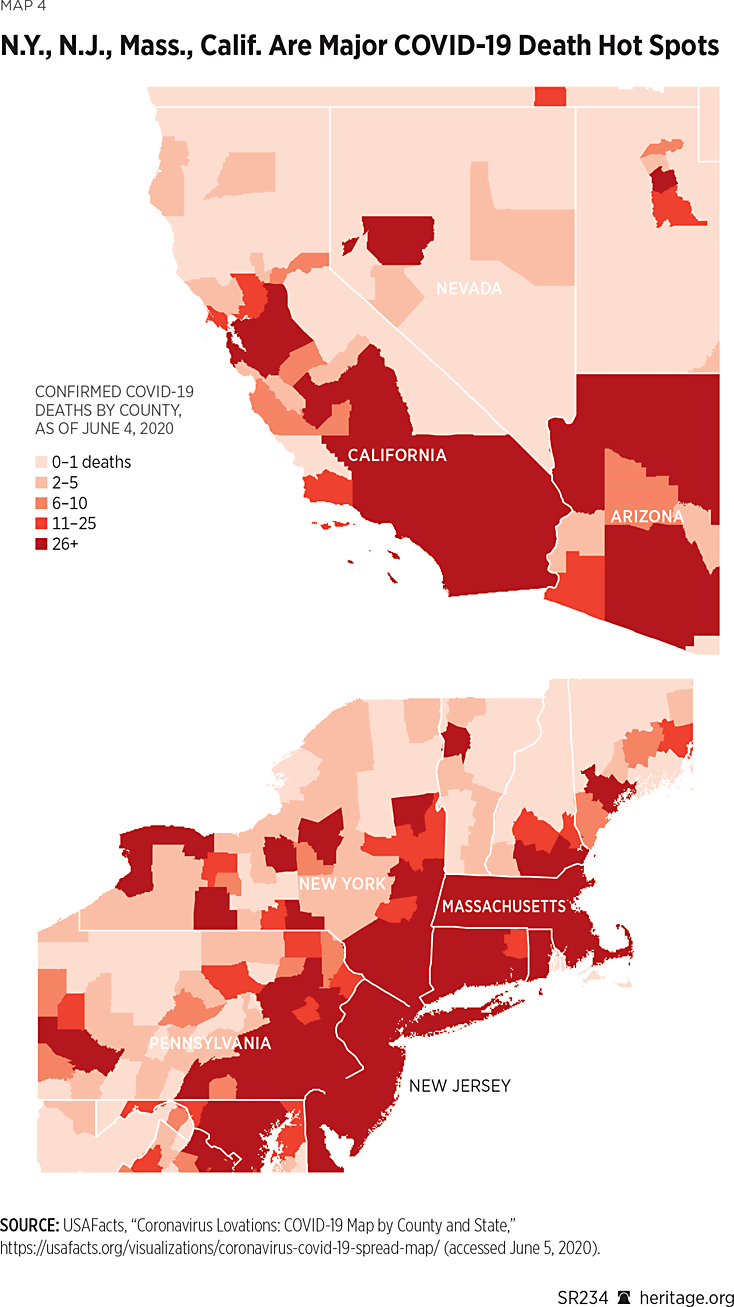
As depicted in Maps 2 and 4, as of June 4, 2020, the outbreak was predominant in a few hot spots—chiefly the densely populated areas of New York City and its surroundings along with nearby New Jersey.REF The nearby New England states—Massachusetts, Rhode Island, and Connecticut—and areas down to Washington DC, have also been hit hard by the virus.REF The Mardi Gras festival in New Orleans in February contributed to Louisiana being the sixth-most COVID-19-infected state by number of cases per one million people (as of June 28, 2020).REF Delaware, Illinois, Maryland, Arizona, and Nebraska had the seventh-most through 11th-most COVID-19 cases per million people among the 50 states (as of June 28).REF
President Donald Trump issued a ban on travelers from China to the U.S. on January 31, 2020—29 days before the first known U.S. death was to be documented.REF Travelers from Iran were banned on February 29.REF When the WHO declared COVID-19 a worldwide pandemic on March 11, President Trump imposed further travel restrictions, halting travel from mainland Europe, and on March 16 from the U.K. and Ireland as well.REF
The White House Coronavirus Task Force, federal agencies, state governments, and local governments across the country have worked together planning how to flatten the curve of COVID-19 cases. During this time, a legion of health care workers, the Armed Forces, first responders, the U.S. Army Corps of Engineers, and other Americans have been caring for the afflicted, building and providing facilities, such as temporary hospitals, and handling logistics to fight the disease.REF
Social distancing, mask wearing, stay-at-home orders, and business-closure regulations have varied over time and from state to state during the pandemic, with some of the strictest orders taking place in California, Michigan, and Washington State.REF Michigan’s governor recently faced a public backlash for what many residents saw as draconian orders, including that all public and private gatherings of any size be banned, and that visiting a friend’s or relative’s home other than to provide care for them or their pets was not allowed.REF Several sheriffs in Michigan and Washington State announced that they would not enforce their governors’ stay-at-home orders.REF Some states have imposed travel restrictions as well. For example, the State of Florida required incoming travelers from certain COVID-19 hotspots to self-quarantine for 14 days or until they left the state.REF Also, while Florida required COVID-19 screening for staff at long-term care facilities to protect elderly residents, New York State, New Jersey, and Michigan initially required hospitals to return all COVID-19 patients from nursing homes to the facilities from which they came.REF
The trajectory of COVID-19 cases and deaths have varied from state to state and from city to city, with the largest death counts thus far mounting in New York and New Jersey, as well as Massachusetts, Illinois, Pennsylvania, Michigan, Connecticut, California, and Florida,REF whereas Wyoming and Alaska have experienced 14 and 20 deaths, respectively (as of June 28), since the pandemic began.REF Americans, in many regards, have cooperated well and voluntarily followed social-distancing guidelines and other measures intended to mitigate the proliferation of COVID-19. For instance, a report from the Centers for Disease Control and Prevention that looked at four U.S. metropolitan areas from February 26 to April 1 found that in each area people were already increasingly limiting their movements outside their homes before their state or local government issued a stay-at-home order.REF
As of May 4, 2020, the daily number of deaths, new cases, and COVID-19-related hospitalizations in New York City, as well as many other areas of the country, were falling.REF While any loss of life is truly devastating, the conscientious efforts of millions of Americans engaging in better hygiene practices and adherence to social-distancing guidelines have prevented additional deaths than would have otherwise occurred over that same period of time.REF
On April 16, President Trump announced guidelines to re-open the economy, which encouraged states to make data-based decisions for opening segments of their economies in three phases.REF Georgia was the first state to announce plans to enter phase one, and did so on April 24, relaxing its stay-at-home orders while allowing some kinds of businesses to re-open. Oklahoma and Alaska joined Georgia in loosening their restrictions that same day, with Tennessee, Mississippi, and Montana following a few days later. By May 18, most states had partially re-opened their economies and had set dates to open them further.REF
The battle against the coronavirus in the U.S. is far from over, and policymakers should focus their efforts on fighting localized outbreaks, while continuing to execute a comprehensive strategy that makes good use of finite local and federal resources. As the National Coronavirus Recovery Commission has recommended, “governors and local leaders should work with their local private-sector institutions (including businesses and core representatives of civil society like churches and community organizations) to take the lead on restarting economic and core social activities, and they should do so as quickly as possible.”REF
International Analysis
In the subsequent sections, we discuss the management and the outcomes of COVID-19 in other countries. Table 1 provides a list of several basic COVID-19-related statistics for the countries examined in this Special Report.
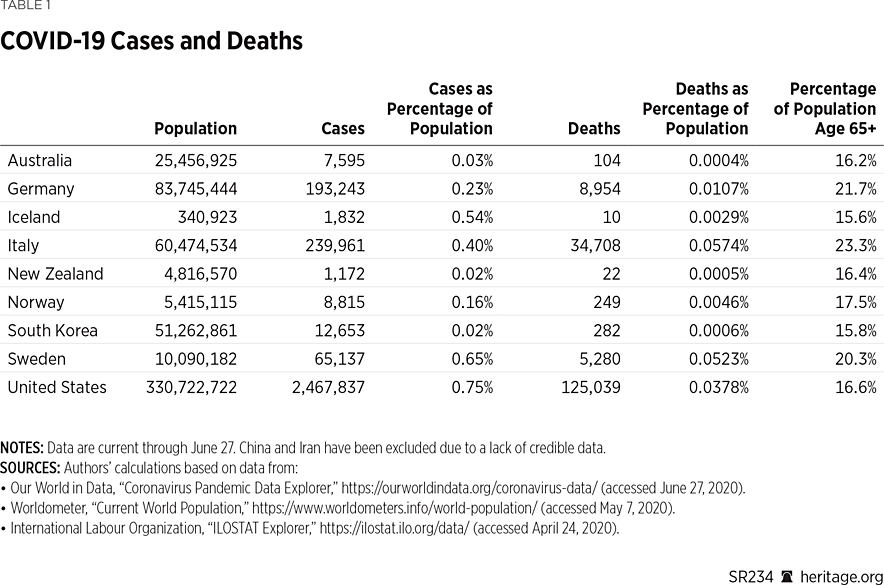
Tables 2 and 3 and Chart 1 depict the differences amongst the various countries in confirmed cases and deaths of the countries considered in this study.

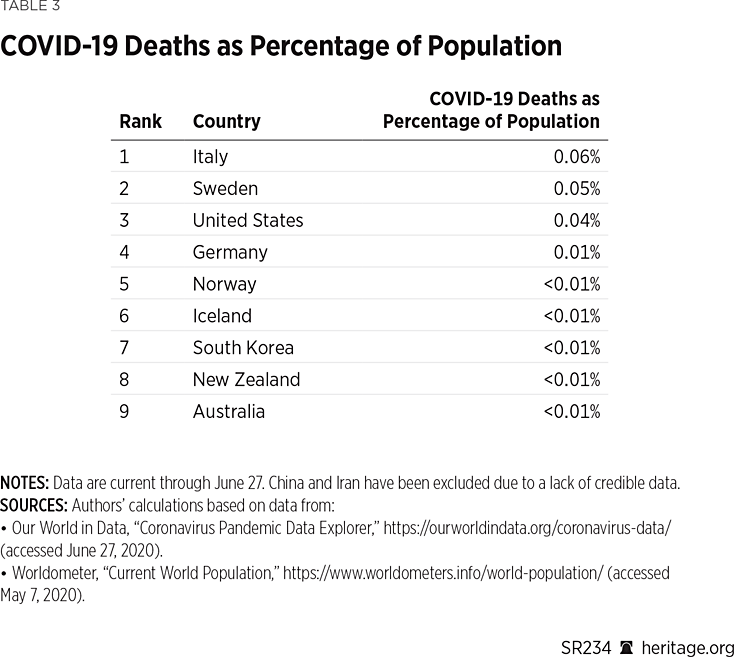
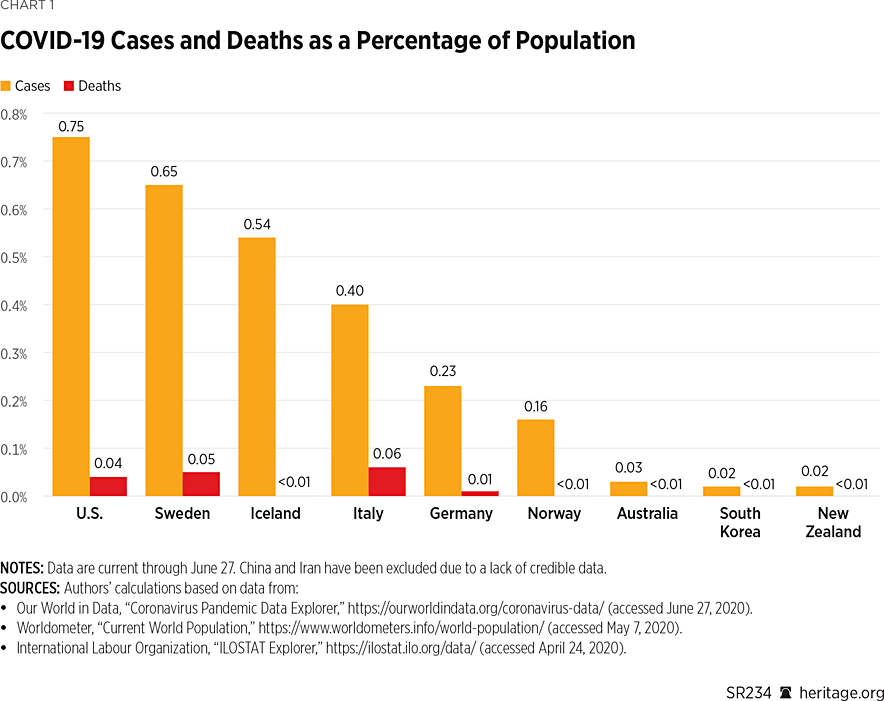
As Chart 1 shows, the United States has the most confirmed COVID-19 cases as a percentage of its population of the countries considered in this report. Sweden has the second-largest percentage, followed by Iceland, Italy, Germany, Norway, Australia, South Korea, and New Zealand, respectively. (China and Iran are known to have suffered a significant number of cases and deaths, but reliable statistics are not available for those two countries.) Regarding deaths, however, the story is quite different. Of the countries considered here, Italy has the most deaths as a percentage of its population, followed by Sweden, the United States, Germany, Norway, Iceland, South Korea, New Zealand, and Australia. Note, however, that none of these countries exceeds 0.8 percent of its population in terms of confirmed cases, and none exceeds 0.1 percent of its population in terms of deaths.
In the following sections we discuss the different approaches these countries have taken to combat the spread of the virus.
Italy. Italy, which ranks as “moderately free” in The Heritage Foundation’s Index of Economic Freedom,REF has a population of slightly more than 60 million people. Parts of the country have been hit particularly hard by COVID-19. One reason appears to be that Italy has an older population than the rest of the countries in this study, with more than 23 percent of the population above the age of 65—1.6 percent percentage points above Germany, the country in this study with the second-oldest population. Italy’s first COVID-19 case was on January 31 from a couple visiting Rome, and afterwards the virus quickly spread throughout the country.REF As of June 27, 2020, the country has 239,961 cases and more than 34,708 deaths (0.4 percent and 0.06 percent of the population, respectively).REF
Italy has 20 distinct regions. The virus is present throughout the country and is now most heavily prevalent in the regions of Lombardy, Emilia Romagna, and Piedmont, the three of which together comprise over 60 percent of the country’s cases. The region of Lombardy, where the first case occurred, as of June 23 carries 93,173 cases (39 percent of the country’s cases) and 16,579 deaths (47 percent of the country’s deaths)—the most of all of Italian regions.REF Early on, the region focused only on testing symptomatic cases. On February 23, 2020, after the virus had proliferated significantly, the Italian government implemented “red zones” in 11 municipalities within the Lombardy region that had at least one COVID-19 case, permitting people to exit their homes only for essential activities, such as going to the grocery store or pharmacy. Cases and deaths, however, continued to grow, and, two weeks later, on March 8, 2020, the entire region of Lombardy, as well as five additional regions, implemented similar lockdown measures.REF Two days later, Prime Minister Giuseppe Conte announced a nationwide lockdown.REF Seven days later, the country issued quarantine orders requiring all people entering the country to self-quarantine for 14 days either at home or in a hotel.REF
Despite the nationwide lockdown, some regions within Italy handled the virus in a markedly different manner from the approach taken in Lombardy. For example, the neighboring northern region of Veneto pursued widespread testing of symptomatic and asymptomatic cases early on during the pandemic. The region also engaged in proactively tracing contacts and other potential positive cases. If a particular individual tested positive for COVID-19, then everyone in the associated household as well as all neighbors were tested, or self-quarantined if testing kits were unavailable. The region also strongly emphasized at-home care, and whenever possible, samples were collected from a patient’s home before being sent to local labs.REF The small town of Vo within Veneto tested all 3,000 of its inhabitants, 3 percent of whom were deemed to have the virus. All of those testing positive were quarantined, and the epidemic was extinguished from the region quickly thereafter.REF
The differences between the approaches and outcomes in Lombardy and Veneto are profound. As Chart 2 illustrates, Lombardy has more than double the number of cases on a per capita basis than Veneto, with four times the number of deaths.REF
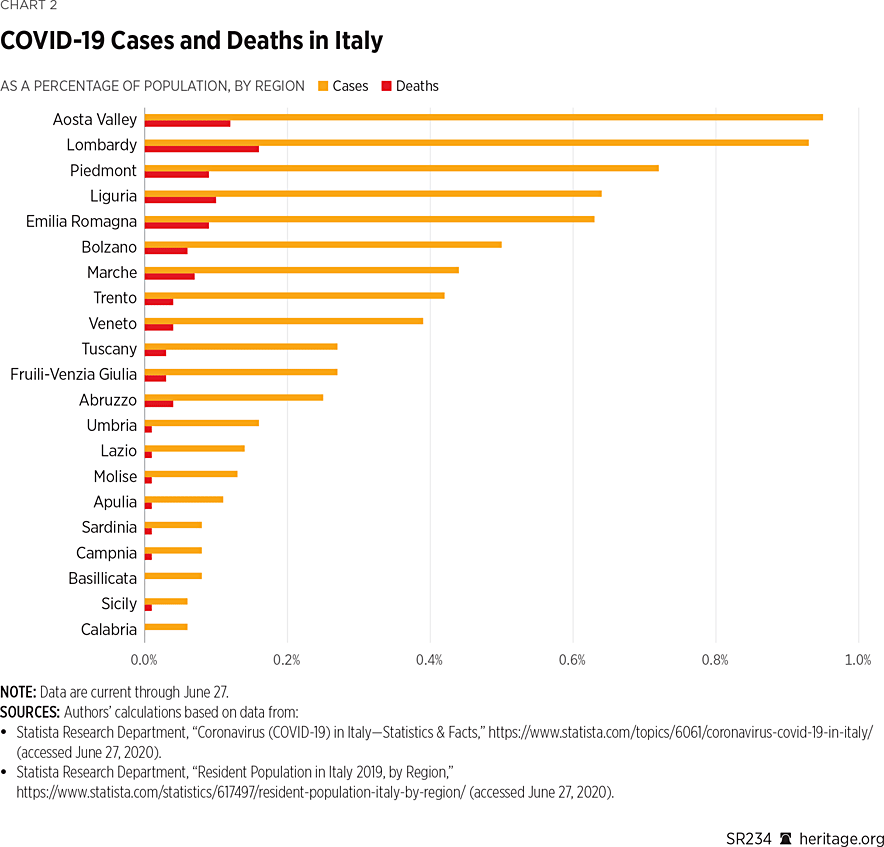
In Lombardy, the hospital system had become overwhelmed, with doctors lamenting that they were not able to provide adequate care to patients.REF Two other regions of Italy—Emilia Romagna and Tuscany—followed Veneto’s approach to implement more aggressive testing. Both regions have noted significantly fewer cases and deaths on per capita basis than Lombardy, as Chart 2 illustrates.REF
Although the cases and deaths in Italy have declined substantially, the country is still consistently reporting new cases and deaths. In particular, from June 1 to June 27, fewer than 600 new cases have been reported per day and fewer than 90 people have died per day as a result of COVID-19.REF As of April 24, the country had begun to ease its lockdown restrictions, and, as of June 3, the country began to ease travel restrictions as well.REF Throughout the spring, the Italian government sought the implementation of a smartphone app to track movements of COVID-19 carriers to aid with contact tracing. Many Italians appear to be setting aside privacy concerns, however, and the app, called Immuni, was released in June 2020 and had more than two million downloads in the first 10 days of its release.REF
South Korea. South Korea has a population of 51 million inhabitants and ranks “mostly free” in The Heritage Foundation’s Index of Economic Freedom.REF Given the country’s geographic location, it has a significant amount of interaction with China both economically and politically.REF In fact, China is the country’s number one trade partner.REF South Korea confirmed its first case of COVID-19 on January 20, 2020.REF On March 21, the South Korean government implemented a strict social-distancing policy and banned religious and sporting events. The beginning of the school year, which typically starts in March, was repeatedly postponed.REF Despite these policies, COVID-19 cases grew in the ensuing weeks, and as of June 27, there were 12,653 confirmed cases and 282 deaths, less than 0.03 percent and 0.0006 percent of the country’s population, respectively.REF All people arriving in South Korea from abroad are required to quarantine for 14 days upon arrival, either at their own local residence or, if they do not have one, a government-designated isolation center, and are required to download a contact-tracing app on their smartphone.REF
After the outbreak of Middle East Respiratory Syndrome (MERS) in South Korea in 2015, the South Korean government implemented a number of reforms to enable the country to handle disease outbreaks better. In fact, just one week after the country’s first official COVID-19 case, South Korean medical officials met with representatives from a number of private medical companies to develop and rapidly expand testing capability. As a result, within weeks of the outbreak in China, four Korean companies had manufactured tests based on recommendations from the WHO, and Korea was able to issue more than 90 times as many tests on a per capita basis than the United States did during the week of March 8, 2020.REF Given that over 35 people died in Korea during the MERS outbreak of 2015, both public and private officials had a vested interest in developing and approving high-quality tests.REF
In South Korea, people are advised to call a national public health hotline when they first show symptoms of COVID-19. Hotline staffers assess symptoms and decide if the patient is suspected of infection. Those suspected of being infected are directed to a COVID-19 testing site. Those who test positive are treated in an isolated setting—either in a hospital or a government-sponsored isolation center, depending on severity and location—to stop further infection.REF This approach has allowed many of South Korea’s retail shops, restaurants, and businesses to remain open during the crisis, with significant precautions and closures in certain areas deemed necessary.REF Private entities, such as hotels, offices, and large organizations, use thermal cameras to identify people with fevers. Restaurants check people’s temperatures before admitting them.REF
Additionally, South Korea also engages in detailed contact tracing. If an individual tests positive for COVID-19, government health authorities use phone records, car-GPS records, bank transactions, credit card records, and CCTV footage to trace their paths, identify contacts, and advise them to get tested.REF Smartphone apps are available that have the ability to warn users if they are within a particular vicinity of areas where people who tested positive for COVID-19 have been.REF Public officials also actively disinfect areas where the virus is suspected to have spread.REF Authorities send regional text alerts, notifying people living near others who have tested positive for COVID-19. Although names are not shared in these text messages, they do contain a link to a website containing information about the person’s age group and places he or she recently visited.REF This approach is consistent with long-used manual contact tracing. Regardless, some have argued that the use of technology to engage in contact tracing results in an overly intrusive approach that risks invasion of privacy.REF
In May, South Korea experienced a small resurgence in cases in Seoul, and as a result, bars and clubs in the capital were temporarily shut down.REF Over 200 schools were also closed shortly after re-opening, given the increase in cases.REF Regardless, South Korea’s measures are curbing the spread of COVID-19 better than the measures of many other countries. Specifically, in May and June, the number of daily new cases declined to fewer than 80. (In February and March, the country sometimes incurred more than 500 new cases per day.) Additionally, since June, the country has incurred fewer than two COVID-19 deaths per day.REF
Iceland. With 364,000 inhabitants, Iceland has the smallest population of all the countries examined here and ranks “mostly free” in The Heritage Foundation’s Index of Economic Freedom.REF Iceland did not impose a nationwide lockdown and, like in South Korea, many shops and businesses remained open, with the exception of those in the Húnaþing Vestra municipality.REF The country did, however, prohibit gatherings of more than 20 people, and closed secondary schools as well as universities.REF Citizens were also asked to engage in social distancing of two meters.REF The country had its first COVID-19 case on February 29, 2020, and as of June 27, the country had a total of 1,832 cases and ten deaths, less than 0.54 percent and 0.003 percent of the nation’s population, respectively.REF From March 20 on, entry was prohibited for non-essential travelers from outside the European Union, the European Economic Area, the European Free Trade Association, and the United Kingdom, and as of April 24, the Icelandic government has required that those arriving into the country from abroad be quarantined for 14 days.REF
Two big factors that differentiate Iceland from other countries are its massive testing and the fact that its authorities engage in strict digital contact tracing via an app called Rkning C-19. Once downloaded, the app garners data from other phones in the area that make it easier to trace contacts of those infected.REF Iceland’s COVID-19 contact-tracing team uses data from the app as well as manual methods to determine who might have come in contact with COVID-19-positive individuals.REF
As of April 25, 2020, Iceland had tested more than 10 percent of its population for the virus, far more than other countries.REF Working with the Icelandic biopharmaceutical company deCODE genetics, Iceland has engaged in large-scale testing to understand the prevalence of COVID-19 amongst various demographics throughout its society. The process has found some very interesting results, including that about 50 percent of COVID-19 positive people in Iceland were asymptomatic at the time of testing, and that there are at least 40 different mutations of the coronavirus.REF
A recent study published in the New England Journal of Medicine indicates that the measures the Icelandic government took may have contained the virus.REF Iceland appears to be turning the corner with fewer than six new cases a day since May 1 (as of June 27, 2020), a 90 percent drop since late March. During the entire pandemic there have been 10 deaths as of June 27, 2020 (less than 0.03 percent of the entire country’s population) due to COVID-19, with the most recent death occurring on April 20, 2020.REF As of June 15, the country began to ease COVID-19-related restrictions, including for tourists, and test visitors for COVID-19 upon arrival.REF
Australia. Australia has a population of about 25.2 million people and ranks “free” in The Heritage Foundation’s Index of Economic Freedom.REF The country had its first confirmed case of COVID-19 in late January 2020.REF As of June 27, 2020, there have been 7,595 confirmed COVID-19 cases (about 0.03 percent of Australia’s population), and 104 deaths attributed to the disease (0.0004 percent of the population).REF State and territorial governments in Australia work with the Australian government, sharing information and moving resources where they need to go in order to treat the afflicted and mitigate the spread of the disease. On January 29, with the number of confirmed cases at about 10 people, Australia began quarantining all passengers arriving from China’s Hubei province for 14 days upon their arrival in Australia in cooperating hotels. Beginning on February 1, all non-Australians who had been in mainland China since February 1 were not allowed to enter Australia.REF On March 20, Australia closed its borders. Only Australian citizens, legal residents, and immediate family members could travel to Australia, and must quarantine for 14 days within a government-approved facility. A number of hotels across Australia agreed to provide the appropriate facilities, and quarantine requirements are managed by state and territory governments with Australian government support.REF
The Australian government released a coronavirus-tracking cellphone app called CovidSafe on April 26, which only lets the government track those who voluntarily download and install it. Although downloading and using CovidSafe is voluntary, on May 1, Prime Minister Scott Morrison said that federal social-distancing restrictions will not be fully removed until enough Australians download CovidSafe.REF
The app uses Bluetooth signals to log if two people have been in close proximity to each other if someone tests positive for COVID-19; health officials are able to track the infected person’s past history and find who else should be tested. Many have voiced privacy concerns although using the app is voluntary, arguing that the technology used has the potential to be misused by government in the future and asking for its source code to be formally made inaccessible to law enforcement.REF Initial interest in CovidSafe soared, with over 2 million voluntary downloads occurring within the first few hours of its launch.REF
The approach of the Australian government has been to respect the freedom of the people in the country more so than in many other countries, including neighboring New Zealand.REF Policies and measures used to mitigate the virus have varied by state or locality within Australia, but all of Australia’s states and internal territories have had social-distancing restrictions in place at some level during the pandemic.REF The Australian government has encouraged schools to remain open for in-person classes as much as possible, although the decision to stay open or not is made locally and has varied a great deal within Australia.REF Restaurants and bars have been open for takeout, allowing many restaurant workers to keep their jobs. Important industries, such as construction and mining, have been allowed to continue operating, and as a result many businesses and jobs that would have been lost in a more severe economic lockdown continue to exist. By May 1, 2020, the number of new cases in Australia was holding relatively steady at around 15 new cases per day, which was down from a high of 468 on March 28.REF The end of June saw a slight uptick in the number of daily new cases, with 53 on June 28, the highest number since April 17.REF
New Zealand. New Zealand has a population of about 4.9 million people and ranks “free” in The Heritage Foundation’s Index of Economic Freedom.REF New Zealand had its first confirmed case of COVID-19 on February 28, 2020.REF As of June 27, 2020, there have been 1,172 confirmed COVID-19 cases (about 0.02 percent of the New Zealand population), and 22 deaths attributed the disease (0.0005 percent of the New Zealand population).REF
On March 28, when the number of confirmed cases was 102, New Zealand began its strictest alert level, which is COVID-19 Alert Level 4. The country remained at Level 4 through April 27, lowering its alert level to Level 3 that day. Both Levels 3 and 4 highly restrict New Zealanders’ economic freedom and travel. During this time foreigners have not been allowed to enter New Zealand. Citizens returning to New Zealand must remain isolated in a government-approved facility for 14 days. Those experiencing COVID-19 symptoms are sent to separate isolation centers. On March 29, New Zealand had its first known COVID-19-related death.REF

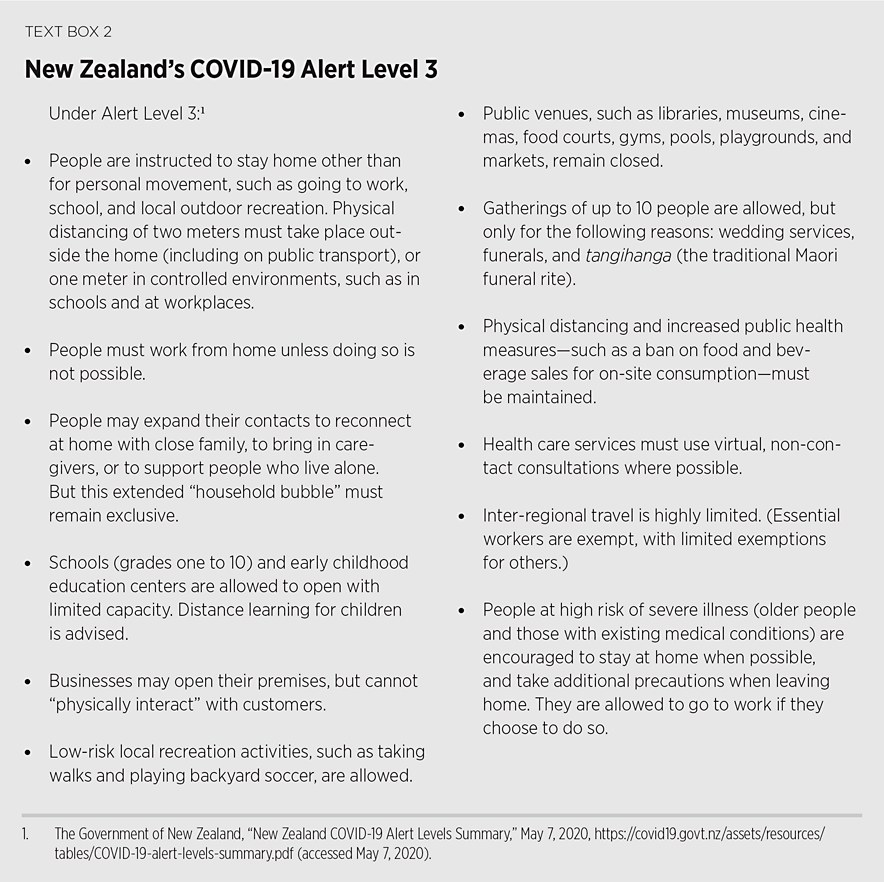
The New Zealand Ministry of Health released a digital contact-tracing app called NZ COVID Tracer earlier this year. As of June 16, 2020, more than 558,000 people have downloaded the app. To enable people to use the app, businesses and organizations are provided with an official quick response (QR) code. People who enter or exit the premises of these companies are encouraged to scan the building’s QR code to develop a log of their travels. Users can also sign up to receive alerts when a person with COVID-19 has been in the same location as they have. Users who are recognized as having a confirmed or likely case of COVID-19 are encouraged to disclose their check-ins with the Ministry of Health to assist contact tracers in identifying others who might potentially be infected.REF
Daily new cases and deaths have declined in recent weeks in New Zealand, with new cases falling to single digits and no reported deaths in June (through June 27).REF However, New Zealand’s period of lockdown enacted a heavy toll on its economy. Its strong fiscal position and government budget surpluses it has had in recent years have helped it to pay out billions of dollars in temporary wage subsidies to prevent mass unemployment, and over half the nation’s workforce relied on government transfers during the lockdown.REF However, businesses in New Zealand are now in a precarious situation. Greg Harford, of Retail NZ, an advocate for retailers, explained it this way recently to a New Zealand newspaper:
Sales across the sector have collapsed and, even online trading, which has been permitted since last Monday, is not delivering sales that will allow retailers to recover from the economic carnage of the last few weeks…. The Covid-19 restrictions will mean that the survival of many retail businesses is on a knife-edge. The wage subsidy has effectively kept many people employed in retail, but it is likely that we will see a wave of redundancies across the sector when that subsidy runs out.REF
New Zealand had been on Alert Level 1 since June 8. At Alert Level 1, New Zealanders can return to work and school, play sports and engage in domestic travel without restrictions, and can gather in groups with no size limitations. The borders of New Zealand remain closed to almost all travelers.REF
China. China has a population of 1.4 billion people and ranks “mostly unfree” in The Heritage Foundation’s Index of Economic Freedom.REF The first human cases of COVID-19 were in the Hubei province of China, in the city of Wuhan (population, about 9.8 million), in December 2019.REF Subsequent work has traced back the origin of the virus in humans to as early as November 17.REF As of June 28, 2020, there had been 84,745 official COVID-19 cases in China (about 0.006 percent of the population of China), and 4,641 officially reported deaths from the disease (about 0.0003 percent of the population of China).REF
China first alerted the WHO of 41 cases of what are now known to have been COVID-19 on December 30, 2019,REF although the virus had been circulating for at least several weeks prior. On January 11, 2020, China had its first known COVID-19-related death.REF Then, on January 23,REF with the number of confirmed cases at 571REF (revised higher since), the city of Wuhan was placed under strict quarantine. The rest of the Hubei province entered quarantine days later.
Decisions made by the Chinese government indicate that it did not prioritize preventing the virus from spreading across its borders. As a result, international travelers from China would ultimately spread the coronavirus across the globe. In particular, Wuhan’s former mayor stated that five million people left Wuhan before the lockdown there went into effect. The number of five million has been questioned by Derek Scissors, a China expert at the American Enterprise Institute,REF as that number is significantly higher than the number of people who left Wuhan in previous years during the period. Regardless, it is safe to say that millions traveled from Wuhan to other places in China, and tens of thousands to destinations outside China.REF After the quarantine of Hubei went into effect, domestic flights within China were greatly limited,REF but China complained when Italy, the U.S., and Australia banned flights from China.
As Bloomberg reports: “Vice Foreign Minister Qin Gang met with Italy’s ambassador on Feb. 6 to protest the halt to flights, and the Foreign Ministry later said in a statement that China is ‘strongly dissatisfied with the overreaction and restrictions of the Italian side.’”REF
Rome was one of just three European cities that had direct flights from Wuhan before Italy halted themREF (the other two are Paris and London), and it has a large population of Chinese workersREF and others who would make their way from Wuhan to Italy before the flights were grounded on January 23.REF The lockdown on Wuhan was lifted on April 8.REF
The Chinese communist government has a long history of human rights violations. It should therefore not come as a surprise to anyone that during the Wuhan quarantine, entire apartment buildings where the virus was thought to have been present were sometimes welded shutREF with families and pets inside them. Additionally, American journalists have been expelledREF from China for reporting on the authoritarian regime’s suppression and cover-ups during its response to the virus, and Chinese citizens who said what the government did not want them to say have disappeared.REF Still others were censored, such as Dr. Li Wenliang, who was forced by Communist Party of China disciplinary officials to write a statement criticizing himself for spreading rumors because he spoke publicly about the existence of the virus in its early days. Dr. Li later became infected with COVID-19 from one of his patients, and subsequently died from the disease.REF
China’s COVID-19 statistics should be viewed cautiously due to the government’s long-standing lack of transparency.REF In fact, one well-respected expert on China calculates that the Chinese government has underreported the number of COVID-19 cases outside of Hubei province by more than 2,900,000 cases—a factor of more than 100.REF If reported, the additional 2,900,000 cases would change the percentage of people in China who have had the virus from 0.006 percent of the population to 0.2 percent, which, if the case fatality ratio is the same as reported for Hubei province (6.62 percent as of June 28),REF would indicate that at least 191,980 more Chinese have died from the virus, which future historians will need to verify.
Iran. Iran, a country of 82.4 million people, ranks as repressed” in The Heritage Foundation’s Index of Economic Freedom.REF The country reported its first two casesREF of COVID-19, and also the first two deaths from the disease, on February 19, 2020. By June 28, there were 222,669 reported cases (0.27 percent of Iran’s population), and 10,508 deaths (0.013 percent of the people in Iran, and 4.7 percent of reported cases).REF Researchers have estimated, however, that Iran’s government had probably underreported cases by 2 million cases as early as March 9 (roughly 2.4 percent of all of the people in Iran), and have argued that the undercount by that date may plausibly have been as many as 6.4 million cases (about 7.8 percent of Iranians).REF
Initially, Iran’s government downplayed and hid the extent of COVID-19’s death and destruction; Iran’s totalitarian rulers contributed to the virus spreading in the country because—as Heritage Foundation experts have explained—of their desire to, “project total control and invincibility, and to avoid damaging the regime’s political, ideological, and economic interests.”REF The representative of Iranian Supreme Leader Ayatollah Ali Khamenei in the city of Qom, for example, continued to urge pilgrimsREF from around the world to flock to Qom’s religious shrines, which many visitors believe have healing powers and have been known to lick the walls of, even though the Iranian regime already knew that Qom was the epicenter of the COVID-19 outbreak. In fact, two days after the government announced the first two deaths from COVID-19 on February 19, mass graves in Qom the size of a 100-yard football field could already be seen in satellite imagery.REF
It was not until March 17, 2020,REF when the number of reported cases was 16,169REF (though the real number was probably much higher),REF that Iran’s government changed course and shuttered the city of Qom’s shrines, moved universities across Iran to online education, closed major shopping malls, shut down subway service in some cities, and took other measures to inhibit the spread of the disease.REF
The Iranian regime regularly accusesREF the United States and Israel of bringing COVID-19 to Iran as an “ethnic weapon” targeting Iranians based on their genetics, and appears in its overall response to be at least as concerned with assigning false blame for the disease as in doing things to prevent it from continuing.
Norway. Norway has a population of approximately 5.4 million and ranks “mostly free” in The Heritage Foundation’s Index of Economic Freedom.REF The country had its first confirmed COVID case on February 26, 2020, and as of June 27, has had 8,815 cases (0.16 percent of its population) and 249 deaths (0.0046 percent of its population), respectively.REF
Norway enacted a country-wide lockdown on March 12, approximately two weeks after the first reported case (on February 26), when a Norwegian returned from China. Airports and seaports were shut down to foreigners as of March 16. The lockdown includes the nationwide closure of schools, universities, restaurants, gyms, resorts, and cultural centers.REF The Norwegian government also enlisted Home Guard soldiers to help control the border with Finland and the inner and outer Schengen area.REF After February 27, all foreign arrivals were required to undergo a 14-day quarantine.REF
The government reports that most confirmed cases during the early days of the outbreak within the country had been the result of Norwegians travelling abroad or those in close contact with travelers.REF About 60 percent of the country’s cases are in the capital, Oslo, and neighboring Viken County as of June 27, 2020. Each of Norway’s 11 counties has recorded at least 100 positive test results.REF
On April 6, Health Minister Bent Høie declared the country has the virus under control and that “every person infected with the coronavirus most likely is now infecting 0.7 other people.”REF Subsequently, Prime Minister Solberg began recommending that all citizens use an app, Smittestopp, to help trace cases and further quell the spread of the virus. By April 24, it was reported that 1.4 million people had downloaded Smittestopp, despite serious concerns over data privacy in the tracing software.REF On June 12, however, Norway’s data-protection agency announced that Smittestopp would be suspended due to the privacy questions and low numbers of active users. As of June 15, The Guardian reported that only 600,000 Norwegians out of the country’s 5.4 million inhabitants were using the app.REF
The Norwegian government enacted an economic stimulus (starting March 13) to fight the negative effects of COVID-19 and the shutdown measures.REF The stimulus includes compensation schemes for failing businesses, reductions in some taxes, and extensions for unemployment benefits.REF The stimulus is reported to be worth $10 billion, which equals approximately slightly over $1,800 per capita.REF
From a public health perspective, Norway’s situation appears to be improving, with daily new cases having dropped by over 90 percent from the beginning of April through June 27, 2020. and with daily deaths now appearing in the single digits, down from a high of 13 on April 15.REF Prime Minister Solberg announced the easing of restrictions on some schools and businesses to take effect April 20.REF The 14-day quarantine period for foreign arrivals has been recently reduced to 10 days for people entering from certain countries.REF
In early May, the Norwegian public health authority released a report that concludes that the virus was not initially spreading as fast in Norway as had been feared, and that the lockdown was actually ordered after the virus had already been waning.REF According to Camilla Stoltenberg, the director of Norway’s public health agency, “Our assessment now, and I find that there is a broad consensus in relation to the reopening, was that one could probably achieve the same effect—and avoid part of the unfortunate repercussions—by not closing. But, instead, staying open with precautions to stop the spread.”REF
Sweden. Sweden has a population of about 10.3 million and ranks “mostly free” in The Heritage Foundation’s Index of Economic Freedom.REF Sweden’s first confirmed case of COVID-19 was on January 31 in a woman in Jönköping County who was tested for COVID-19 after returning from Wuhan on January 24. She initially reported being symptom-free upon her return to Sweden, kept herself quarantined due to the news at the time, and ultimately developed symptoms.REF It was not until February 26 that a second case was confirmed after an asymptomatic man returned from a trip to Italy.REF The rate of infections rose quickly, hitting 1,000 by March 16 and 10,000 by April 12. As of June 27, Sweden has reported 65,137 infections and 5,280 deaths, 0.65 percent and 0.05 percent of the country’s population, respectively.REF While Sweden does have a higher percentage of deaths than Norway and Finland, for example, the country also has a lower rate than many Western European countries, such as Belgium, Italy, the U.K., and Spain, all of which practiced more severe lockdown measures.REF
Sweden has faced mixed responses of international derision and praise for a comparatively hands-off approach to mitigating COVID-19 infections. Although the Swedish government did ban large public gatherings, visits to elderly care homes, and some travel into the country in late March, most businesses and travel remain open and available.REF Still, travel and mobility has been reduced by as much as 75 percent or more in some areas by overwhelmingly voluntary means.REF Sweden has faced some criticism because its death rate per capita is higher than that of any other Scandinavian country. However, over 50 percent of the nation’s cases come from Stockholm and Västra Götaland Counties.REF As of May 14 according to the Swedish Public Health Agency, over 48 percent of the country’s deaths were in nursing homes.REF
The strategist behind the response is Sweden’s head epidemiologist, Anders Tegnell. Instead of mandating the closure of schools, recreation facilities, and restaurants, the government is recommending that its citizens follow safety guidelines that include social distancing and protection for the elderly.REF Tegnell says the current approach aims to slow the spread of infection so that health services are not overwhelmed while decreasing the likelihood of a subsequent wave of infection.REF One of the top epidemiologists in the world has argued that Sweden has chosen the right path to mitigate potential disaster.REF
Tegnell has also suggested that lockdown measures are not the right approach for a long-term solution. In an interview on April 28, Tegnell said that
… up to 25% of people in Stockholm have been exposed to coronavirus and are possibly immune. A recent survey from one of our hospitals in Stockholm found that 27% of staff there are immune…. Coronavirus is not something that is just going to go away. Any country that believes it can keep it out will most likely be proven wrong at some stage. We need to learn to live with this disease.REF
The Swedish government also hopes to mitigate as much economic fallout as possible over the longer term.REF Many other countries are coming to terms with the worst self-imposed economic damage in history as a result of broadly enforced lockdowns to deal with COVID-19. If successful, Sweden’s strategy will put the country in a better position to rebound economically.REF
Governmental policies are currently in the works to alleviate business impacts and cushion the blow to separated workers. For instance, the Swedish government will cover up to 50 percent of failing businesses’ wage costs to allow them to retain their employees.REF Other measures include deferments on value-added taxes.REF Additionally, Swedish mandatory social security contributions have been reduced for both businesses and employers. The government is also covering temporary sick-leave costs usually covered by employers. Extra funding for job training and job-matching services, as well as overall increases in public-services spending to match demand throughout the country are among the main focuses for emergency spending.REF
Germany. Like Sweden, Germany ranks “mostly free” in The Heritage Foundation’s Index of Economic Freedom.REF With a population of 83.7 million, Germany began early tracking of COVID-19 cases, which has helped to keep the fatality rate low through tracing the contacts of carriers. Early widespread testing was also implemented, including that of asymptomatic individuals.REF Although some argue that this approach is a leading reason for Germany’s low fatality rate and lessened stress on the health care system, the head of Germany’s disease center has urged leaders to stop the testing of asymptomatic cases to avoid a shortage of supplies.REF The country had its first confirmed case on January 27, 2020, and as of June 27, Germany has reported 193,243 cases and 8,954 deaths (0.23 percent and 0.01 percent of the country’s population respectively).REF These statistics correspond to roughly 11 deaths per 100,000 people compared to approximately 52 in Sweden, 65 in the U.K., and 46 in France.REF
These methods determined that many early transmissions occurred among young vacationers in Austrian and northern Italian ski resorts (frequented heavily by German tourists).REF The first peer-to-peer transmission in Germany was traced to an auto-plant worker from the Webasto Group in January, spreading the virus to co-workers in Stockdorf after returning from China.REF Early on, each of Germany’s 16 states was itself responsible for deciding on their lockdown measures, although the nationwide social-distancing policies were mandated by Chancellor Angela Merkel on March 22.REF Each German state enacted some form of assembly restriction and various business restrictions.REF Most schools were shut down in March and some states, such as Bavaria and the Saarland, did pursue state-wide lockdown measures.REF Germany began restricting travel in mid-March and started slowly reopening to travelers on June 15.REF
During the early months of the pandemic, German officials used manual contact-tracing methods, via phone calls by public health officials, advising people who have been in contact with COVID-19 positive people to self-quarantine and, if they develop symptoms, to get tested.REF Despite most Germans supporting a gradual re-opening of the economy as of April 24, government officials had warned that the virus was here to stay and they must not lower their guard. Fifty-three percent of German citizens approve of the partial re-opening of schools, and 94 percent agreed that large events should be banned until August, according to a ZDF poll in late April.REF
Germany passed a stimulus package in late March to offset economic disruptions caused by the pandemic. The measures total almost $1.1 trillion and include liquidity payments for small companies and simplified avenues for unemployment benefits.REF Like many European nations, Germany has worked to build a smartphone app designed to trace and report COVID-19 infections, although privacy concerns made a centralized approach to the app unlikely to please Germans. Many argued that too much information in the hands of German authorities could be used after the national emergency for unclear purposes.REF Despite these concerns, on June 16, the German government unveiled the Corona-Warn App.REF As of June 25, 12 million Germans downloaded the tracker, more than any other country in Europe.REF
Amongst the country’s 16 states, the states of Bavaria, North-Rhine Westphalia, and Baden-Wurttemberg constitute over 65 percent of the country’s cases and 68 percent of the country’s deaths (as of June 27, 2020).REF However, the country’s situation is improving, and by June 27 a reduction in daily cases by more than 70 percent, and a reduction in daily deaths of over 95 percent since April 15 had been achieved.REF
Analysis of Policies from Abroad
Table 4 provides a list of several additional COVID-19-related statistics that allow comparison across countries. In particular, these figures permit readers to assess COVID-19 cases and deaths per 100,000 people and per 1 million people across international borders with respect to population density.
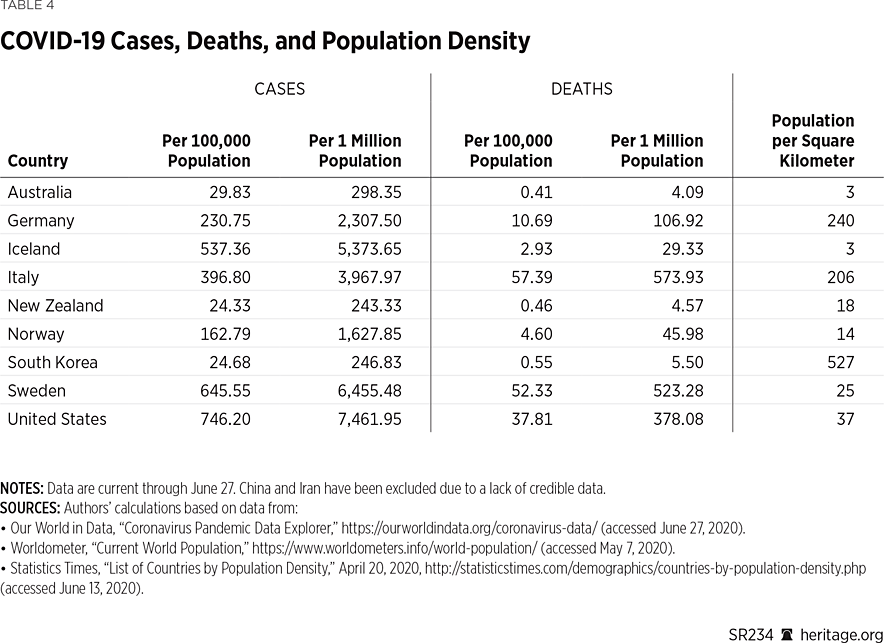
As the statistics in Table 4 show, the number of confirmed cases, on a per capita basis, is 88 percent higher in the U.S. than Italy. Italy, however, which has a relatively large share of elderly in its population, has a higher per capita death total at 0.06 percent of its population. This rate is more than 1.5 times higher than the per capita death total in the U.S.
Nevertheless, there are many important factors that are not completely apparent from these aggregate numbers. For instance, regionally between these two countries, the two worst rates of COVID-19 deaths per 100,000, are in the Lombardy region of Italy and the state of New Jersey, followed by the Aosta Valley region of Italy and New York State.REF Even within New York, it is clear that New York City is responsible for a disproportionate share of cases and deaths.REF Moreover, these aggregate figures do not shed light on the importance of age and underlying health problems. Globally, the virus is much more dangerous and deadly for older people, particularly those with serious health conditions including diabetes and hypertension.REF According to research by the International Long Term Care Policy Network, for countries that have had at least 100 COVID-19 deaths and that provide official data, COVID-related deaths among nursing home residents (as a percentage of total deaths) range from 19 percent in Hungary to 62 percent in Canada.REF Moreover, for younger healthy members of the population, particularly in the U.S., COVID-19 is much less deadly than initially feared.REF In fact, the COVID-19 pandemic—though it is clearly not over—appears to be much less lethal than one of the most deadly respiratory virus pandemics in modern history: the Spanish flu of 1918.REF
The Spanish flu lasted from early 1918 to late 1919 and infected over 500 million people worldwide. The Spanish flu was also deadly, with estimates of deaths as high as 50 million worldwide.REF The flu most likely did not originate in Spain but, like other flus, may have circulated among birds for many years before its outbreak in humans.REF In fact, according to a 2006 study, the virus is still identifiable in the ice and cold water of lakes near Siberia where large numbers of migratory birds visit.REF Chart 3 compares death rates from COVID-19 and the Spanish flu amongst the countries examined in this study.REF
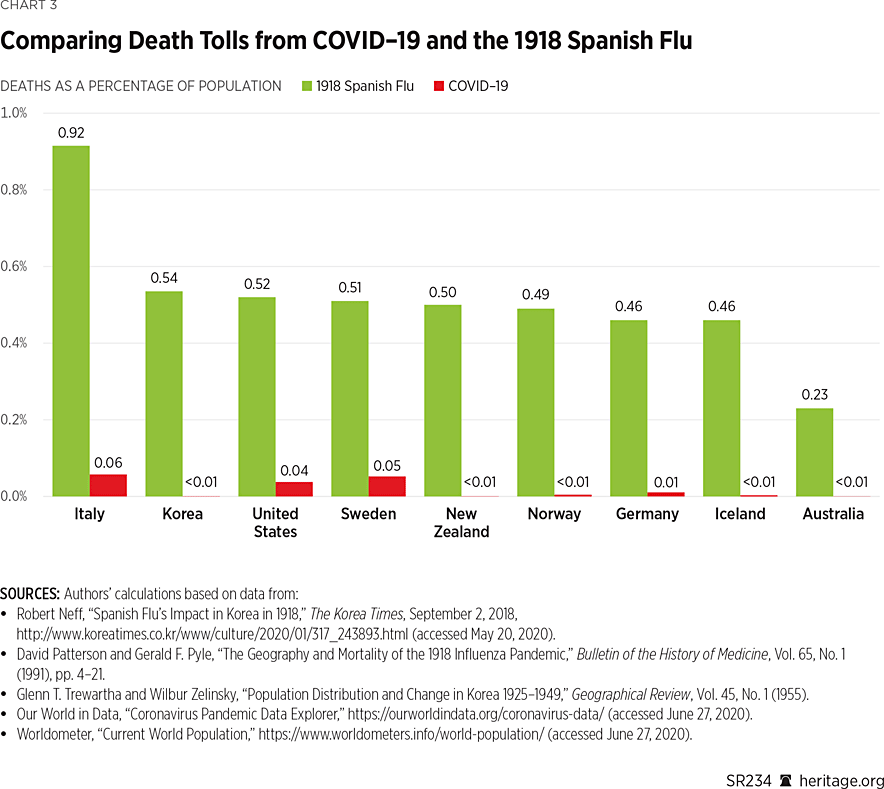
These results demonstrate how much more deadly the Spanish flu was than COVID-19 has been so far. In particular, in the United States, deaths due to Spanish flu as a percentage of the population were over 13 times higher than deaths due to COVID-19 thus far. In order for COVID-19 to kill the same fraction of the United States population as the Spanish flu did, American COVID-19 deaths would have to rise by over 1.5 million people.
In fact, in other countries, the Spanish flu killed even higher percentages of the population than COVID-19 has thus far; for example, in Iceland, the percentage of the population killed by the Spanish flu was over 150 times higher than the percentage of the population killed by COVID-19 so far. In New Zealand, the percentage of the population killed by Spanish flu was over 1,000 times that of COVID-19 as of June 27, 2020.
Although the Spanish flu and COVID-19 are two different illnesses, and although COVID-19 is still ongoing, these disparities in mortality statistics as a percentage of these countries’ populations are also a testament to how societies have evolved over the past century. In the United States, for example, over the past hundred years, life expectancy has increased more than 40 percent, and per capita real income in the U.S. has increased over 500 percent.REF It is well understood that as societies grow wealthier, they are more capable of adapting to adverse situations.REF Additionally, economic growth has resulted in improvements to medical technology and living conditions among many other factors.REF Many societies are thus much better equipped now to deal with a serious health emergency than in the past.
Comparison of COVID-19 Management Across Countries. As this analysis indicates, the different countries studied in this Special Report have taken different approaches to handling the pandemic, all with varying degrees of success. One can compare the effects of these different policies by quantitatively examining a number of important factors.REF Charts 4 and 5 depict cases and deaths (per 100,000) in the countries looked at in this study on a daily basis.
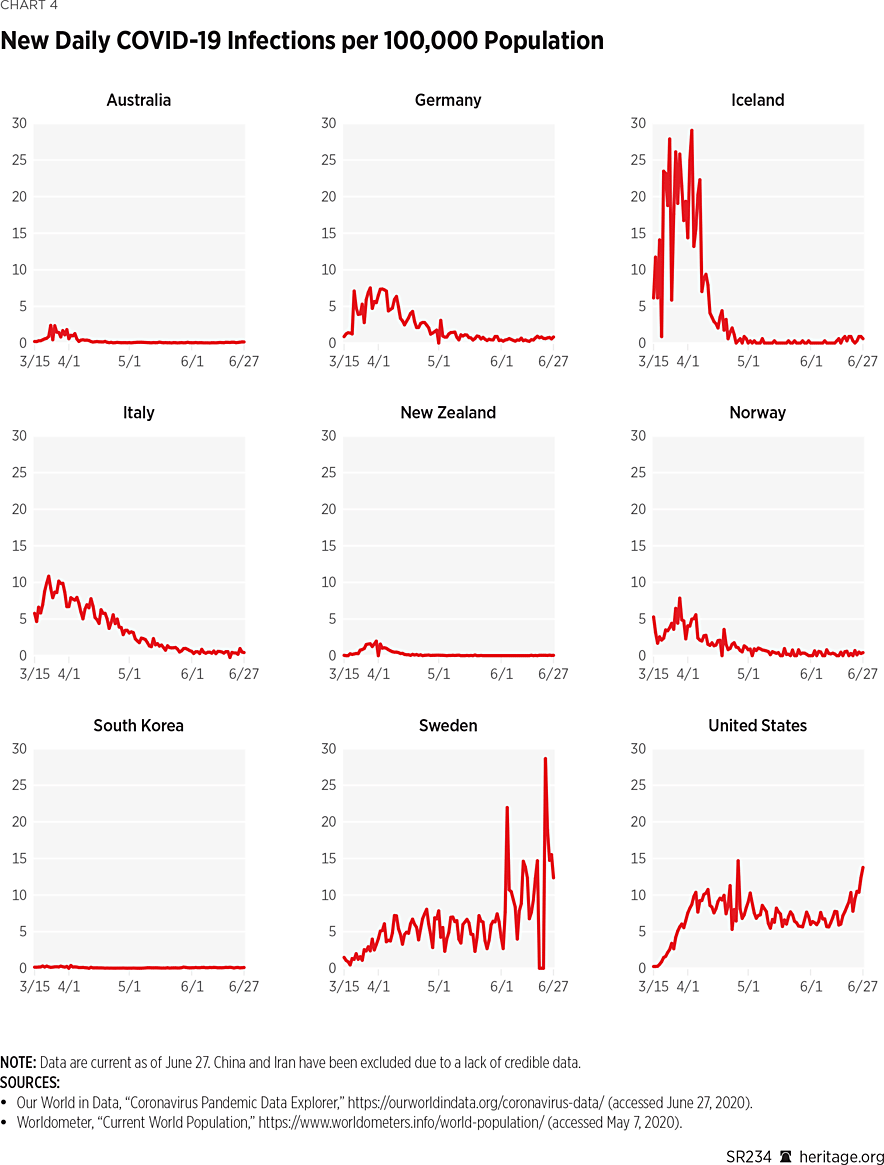
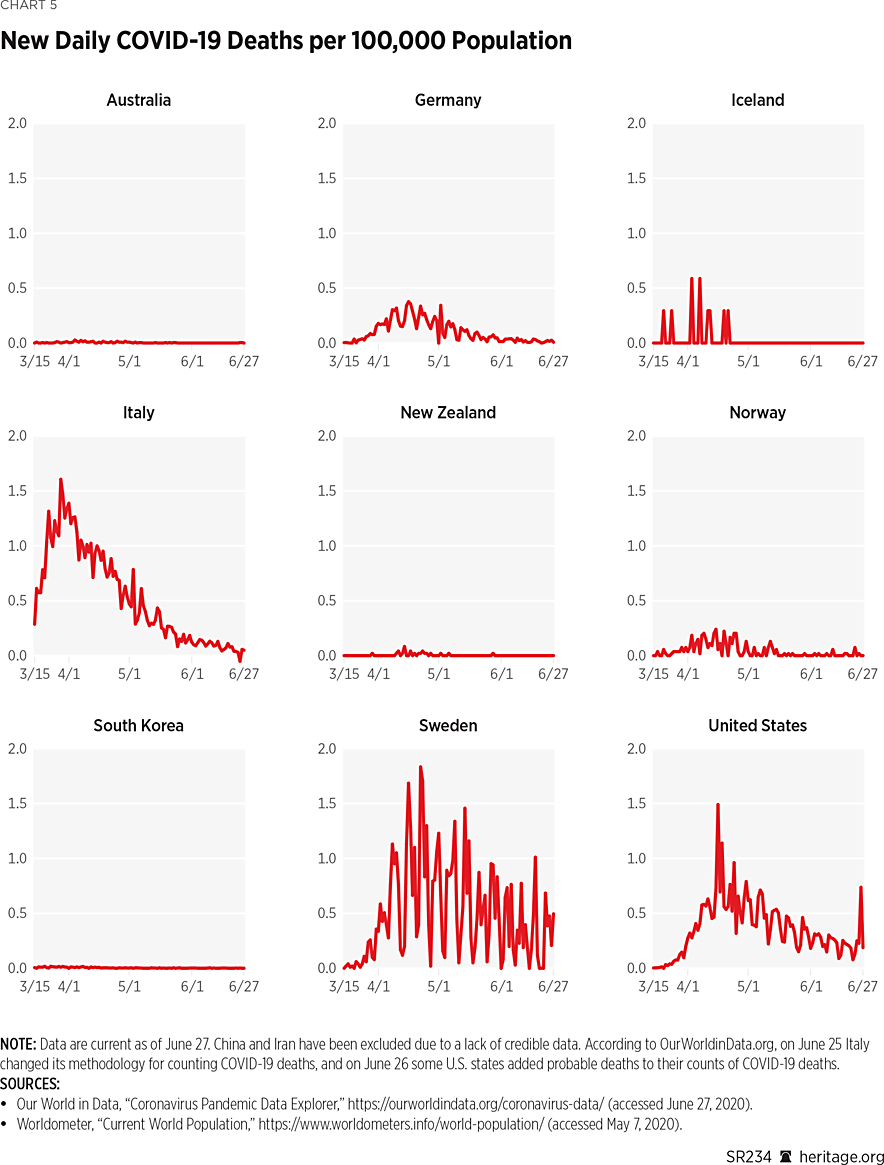
As observed in the previous section, different countries started battling COVID-19 on different dates—ranging from potentially as early as November (or even earlier) in China to late February in Iceland, New Zealand, and Norway. Furthermore, heterogeneity amongst different countries (due to date of occurrence of their first case, differences in urbanization, culture, travel patterns, geography, and population density) has likely affected the proliferation of the virus.
Regardless, as Charts 4 and 5 illustrate, some countries thus far have done much better than others in managing the proliferation of COVID-19. In particular, for every 100,000 members of the population, South Korea, Italy, Iceland, Norway, New Zealand, and Australia averaged fewer than 0.5 new COVID-19 cases per day (per 100,000 population) from June 1 to June 27.REF Over this same time horizon, Germany had an average of 0.52 new cases per day (per 100,000 population), followed by the United States, averaging 7.81 new cases per day from June 1 through June 27 (per 100,000, and then Sweden, averaging 10.29 new cases per day during this same period per 100,000). Additionally, South Korea, Italy, Iceland, Norway, New Zealand, and Australia have all averaged less than 0.1 new deaths per day (per 100,000) over the same time period.. The United States and Sweden, however, have exceeded this threshold over the same time horizon, averaging 0.23 and 0.32 new deaths per day (per 100,000), respectively.
A Comparison of Australia and New Zealand. A comparison of the approaches taken and the consequent outcomes in New Zealand and Australia is especially informative because of several key similarities between the two countries. Both Australia and New Zealand are island nations with similar climates and with similar distances to the rest of the world. Both nations closed their borders entirely to visitors from other countries at the same time (on March 19 in New Zealand and March 20 in Australia).REF Additionally, as illustrated in Table 4, both countries have lower levels of population density (nine and 18 people per square kilometer, respectively) than the other countries in this study. The first confirmed people to have the virus in both countries arrived on international flights, and had traveled through virus hotspots, Wuhan and Iran. (Australia’s first confirmed cases of coronavirus were on January 25,REF when four men, all of whom had recently traveled to Wuhan, were diagnosed with the virus. The men had arrived in Australia on separate flights in the days leading up to January 25. New Zealand’s first reported case was on February 28, when a native New Zealander returned home after visiting Iran.)REF As of May 29, Australia reported that 62.2 percent of its confirmed cases of COVID-19 were acquired overseas.REF New Zealand reported that 38 percent of its confirmed or probable cases were acquired overseas.REF Australia’s median age was reported by its census bureau to be 36.4 in 2016,REF and New Zealand’s, a similar, 37.4 in 2018.REF As of June 27, both countries have had very similar percentages of their populations test positive for COVID-19—7,595 cases in Australia (about 0.03 percent of Australia’s total population), and 1,172 cases in New Zealand (about 0.024 percent of New Zealand’s population). Both have brought the number of reported cases per day to near zero. (Australia has confirmed an average of 33 new COVID-19 cases per day for the seven days ending on June 28,REF whereas New Zealand averaged fewer than two new cases per day over that time period.)REF
While both countries have limited the health damage caused by COVID-19, Australia, unlike New Zealand, has also limited economic damage by making an effort not to infringe on the economic freedom of Australians or close their businesses when it has not been necessary to do so. For example, the Australian government has encouraged schools to remain open for in-classroom learning if possible,REF whereas the New Zealand government outlawed in-classroom learning nationwide. (With local Australian governments or individual schools making the final call, different schools within Australia have been open for in-classroom learning, or shut down with a high degree of variability by date range and school.) Similarly, Australia has allowed many businesses to operate throughout the pandemic, including mining, construction, and restaurants for takeout. New Zealand’s economic lockdown, by contrast, was more severe than Australia’s, stopping virtually all businesses from operating until very recently, for example not allowing physical interaction with customers. (See Text Box 2.)REF
Despite these differences, New Zealand and Australia appear to have mitigated the spread of COVID-19 to a similar extent. Yet, due to the New Zealand government’s harsher restrictions on business activity, its economy is expected to shrink by about twice as much in the first half of calendar year 2020 as Australia’s. The consensus forecast among major banks in New Zealand is that the economy will contract by close to 20 percent in the second quarter of 2020.REF The Reserve Bank of Australia expects the Australian economy to shrink by only 10 percent in the first and second quarters of 2020 combined, with the bulk of the decline coming in the second quarter.REF New Zealand’s government has predicted that the jobless rate in New Zealand might rise to 13.5 percent (from 4 percent at the end of 2019),REF while Australia’s central bank estimates that Australia’s unemployment rate will only about double (from the end of 2019) to 10 percent by the end of June 2020.REF
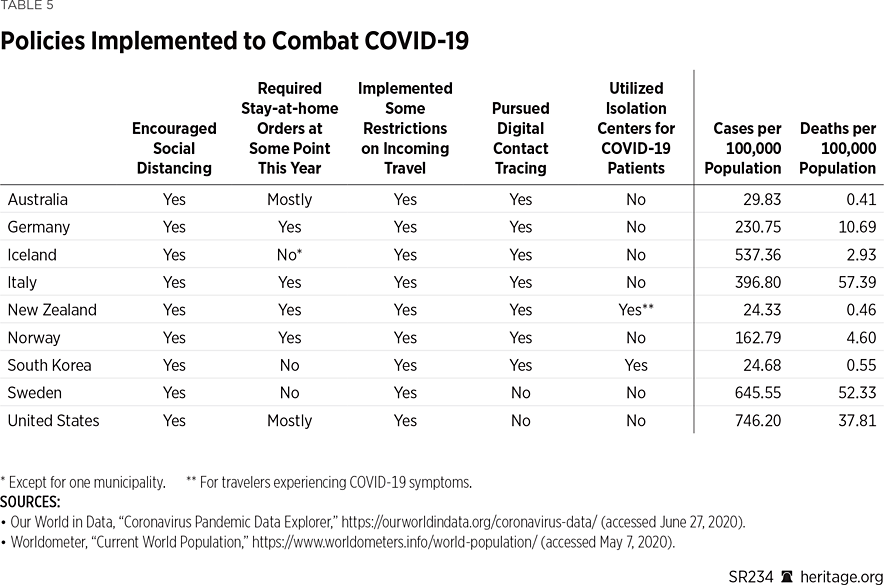
A Comparison of the United States and Other Countries. Table 5 provides a comparison of the different policies pursued by the countries in this study. As Charts 4 and 5 illustrate, since June 1, with the exception of Sweden, the United States is currently experiencing more reported cases and deaths on a per capita basis than any of the other countries considered in this study. In particular, over this time, the United States has had more than 25 times the number of average daily new known cases (per 100,000) than South Korea, New Zealand, Iceland, or Australia, and over 200 times the number of average daily new deaths (per 100,000).REF Over this same time period, the United States has had 17 times as many average known daily new cases (per 100,000) than Italy, and 2.8 times as many average daily new deaths (per 100,000).
Both the United States and Italy have also pursued similar policies in their attempts to deal with COVID-19. In particular, more than 40 of the 50 states instituted stay-at-home orders at various times during the spring.REF These policies of strict stay-at-home orders bear similarity to those of the Lombardy region of Italy, which, as discussed earlier, accounts for by far the largest share of deaths and cases in Italy. New York Governor Andrew Cuomo (D) noted that six weeks after stay-at-home orders were instituted, 66 percent of COVID-19 hospitalizations were from people adhering to those orders.REF One plausible reason for the continuing spread during lockdowns is that people with mild cases of COVID-19 (that do not involve hospitalization) isolate at home, possibly transmitting the virus to family members.REF
Regardless, none of the 50 U.S. states has implemented approaches similar to those taken in some of the other Italian regions, such as Veneto, which has also pursued mass testing and aggressive contact tracing instead of purely relying on strict lockdowns. As discussed in this Special Report, however, some countries, such as South Korea and Iceland, have pursued mass testing and aggressive contact tracing without relying on nationwide lockdowns at all. In fact, as Table 4 illustrates, South Korea, the most densely populated country of all the countries examined in this study and thus most prone to virus proliferation, has instead relied heavily on extensive testing, contact tracing, and isolating the sick. From June 1 to June 27, the country reported fewer than 70 new cases per day and single-digit deaths daily, throughout the entire population. The United States, on the other hand, during this same time has had on average 90 times as many daily cases (per 100,000) and 200 times as many daily deaths (per 100,000) than South Korea has had despite the fact that, as illustrated in Table 4, South Korea has a population density 14 times that of the United States. U.S. lawmakers would thus do well to learn from the South Korean approach, especially in those regions of the U.S. that have high population densities.
Although mass testing is a key component of successfully containing the virus, the amount of testing offered varies tremendously amongst the countries looked at in this study. (See Charts 6 and 7.)
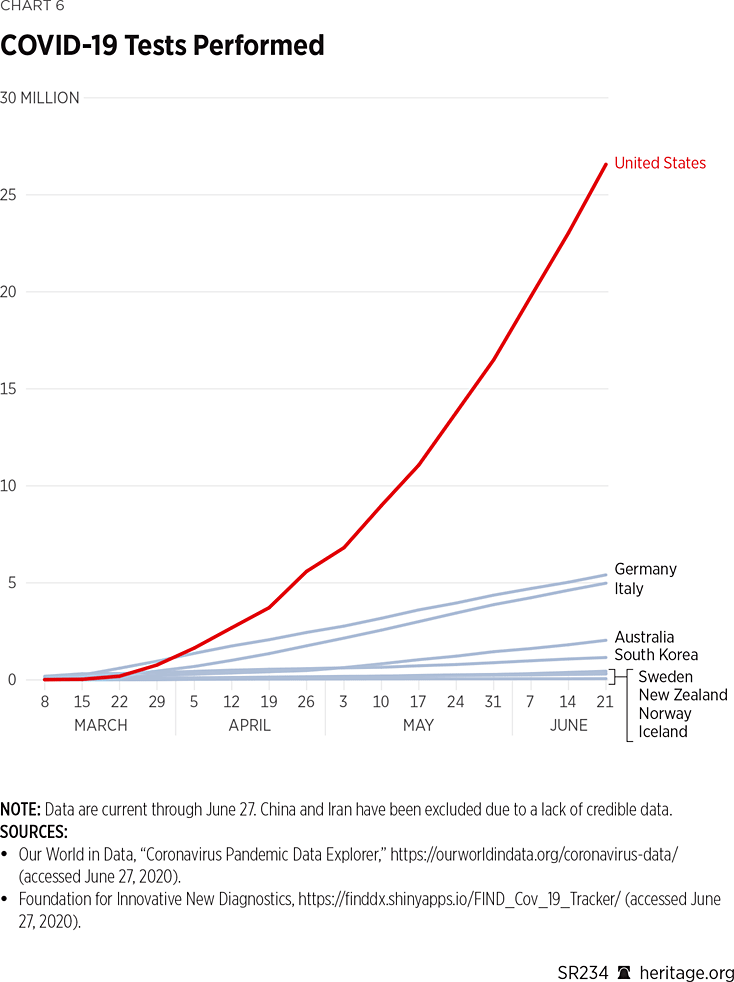
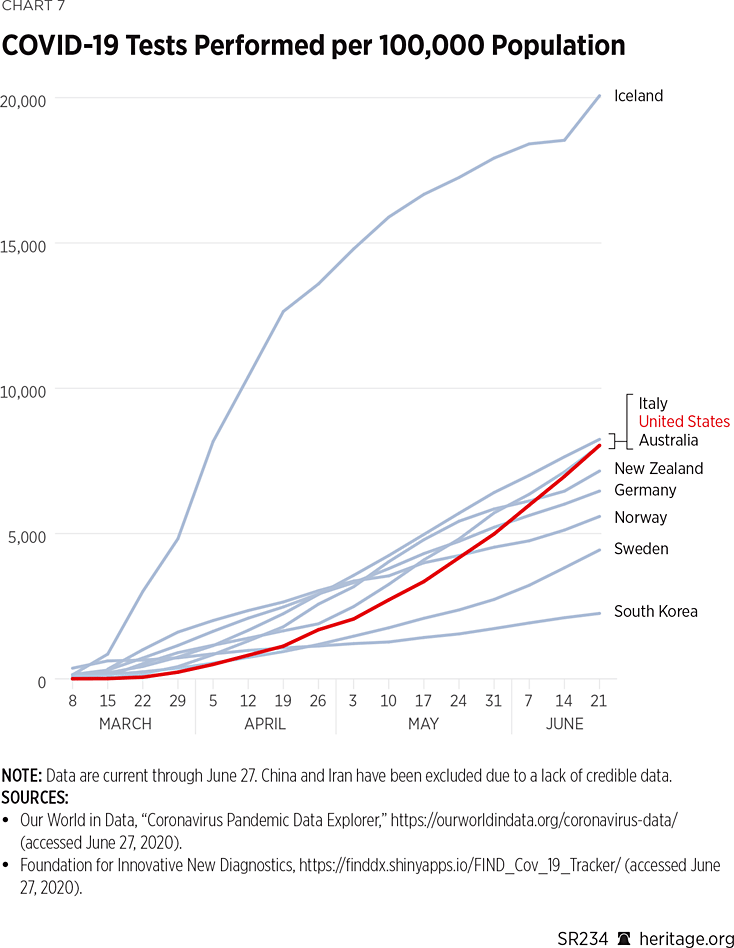
As Charts 6 and 7 illustrate, the United States leads the world in the number of COVID-19 tests given. Additionally, the United States has given more tests on a per capita basis than all of the countries looked at in this study with the exception of Iceland. In fact, Iceland is far ahead of the rest of the world with its mass testing aided by deCODE genetics, having performed over 20,000 tests per 100,000 people as of June 21, more than double that of the United States.REF
However, South Korea had performed more tests on a per capita basis earlier during the pandemic than any of the countries in this study, but it now performs less than all the other countries. This drop-off is largely due to the country’s rapidly deployed testing program at the beginning of the epidemic.REF In fact, during the week of March 8, 2020, South Korea had performed more than 90 times the number of COVID-19 tests than the United States had, and more than double that of Iceland. The aggressive approach that South Korea took early on dramatically slowed down the spread of the virus throughout the country. The tactic was so successful, in fact, that South Korea had a surplus of test kits in April, and started exporting those kits to other countries, including to the United States.REF
One of the main reasons that the United States had difficulty engaging in mass testing early on in the pandemic was that excessive regulation made it very difficult to produce a sufficient number of test kits. Specifically, the Food and Drug Administration (FDA), which has a lengthy approval process to bring any test to market, initially granted emergency use authorization (EUA) only to the Centers for Disease Control and Prevention (CDC) to develop and perform COVID-19 tests.REF Although universities and the private sector were anxious to develop tests early on, the FDA and CDC warned these entities not to perform their own testing without FDA authorization.REF Aside from the fact that the first batch of CDC test kits were faulty,REF the cumbersome process associated with getting FDA authorization prevented the U.S. from having a useable supply of tests.REF
Dr. Helen Chu of the University of Washington, for instance, developed her own tests early on in the pandemic, but both the CDC and the FDA refused to give her authorization to use them. Concerned about the spread of the virus, on February 25, she and her colleagues began performing COVID-19 tests anyway without government approval. They quickly found a positive case and informed state officials that the virus had likely been spreading in the Seattle area undetected. The CDC and FDA subsequently ordered her to stop giving these tests as they were privately developed. Only on February 29 did the FDA announce that it would begin to fast-track EUA for privately developed tests.REF
The success against the spread of COVID-19 in South Korea and Iceland, where many businesses have remained open during the pandemic and people have generally not been told to stay inside their homes, indicate that the stay-at-home orders may not necessarily mitigate the virus better than more targeted measures that include isolation of the sick, mass testing, and contact tracing. Similarly, the results in Australia and New Zealand, two countries that are similar in many ways, indicate that the most restrictive lockdown approach is not superior to one that includes less severe measures. Finally, while some have criticized Sweden’s less restrictive approach because it has more per capita deaths than some of its neighbors, Sweden’s strategy, according to state epidemiologist Tegnell, is designed for a better long-term outcome that lessens the likelihood of a subsequent wave .REF Moreover, as also discussed earlier, Sweden does have lower deaths on a per capita basis than several other Western European countries that relied on more severe lockdown measures, such as Belgium, Italy, the U.K., and Spain.
The following points are the main insights from this analysis:
- Heterogeneity amongst different countries likely contributes to differences in the spread and proliferation of COVID-19.
- The United States had significant difficulty with testing early on due to excessive regulation, preventing it from being able to implement an aggressive testing and tracing program.
- The United States currently has more confirmed cases on a per capita basis than all the other developed countries examined in this Special Report.
- Amongst the developed countries considered in this Special Report, the United States leads the world in COVID-19 tests given and ranks second to Iceland.
- On a per capita basis, the United States has given less than half the number of tests than has Iceland.
- Medical research indicates that COVID-19 deaths occur disproportionately among the elderly and those with comorbidities.
- Some countries that eschewed lockdown policies and relied on more targeted approaches, such as South Korea and Iceland, have experienced outcomes even better than those that have relied on the more severe lockdown approach.
- The United States, which has pursued state-wide lockdowns, has one-fourteenth the population density of South Korea, yet on a per capita basis, has had more than 90 times as many daily cases and more than 200 times as many daily deaths since June 1.
- Cases and deaths in the United States, however, have been highly concentrated in a few, mostly heavily populated, areas, so successful approaches to fighting the disease cannot be one-size-fits-all. What works in New York City differs from what is needed in sparsely populated regions, such as Wyoming.
- The fact that Australia and New Zealand, two similar countries, approached the COVID-19 pandemic so differently, yet had similar outcomes, suggests that alternatives to the most restrictive forms of lockdowns have merit, even in the short run.
Policy Recommendations for the United States
Maintaining a strong economy and protecting public health are not mutually exclusive policy goals. As discussed in the previous sections, a number of countries, such as South Korea and Iceland, are containing COVID-19 considerably better than the United States without shutting down their economies. In fact, many elements of the approach used in places like South Korea can be adapted within America’s borders to help the U.S. do a better job of dealing with COVID-19. In particular, the data show that policymakers and the Administration should:
- Protect those who are at greatest risk—the elderly and those with underlying medical conditions. Government measures must be both geographically targeted and demographically targeted. Seniors and those with chronic illnesses are at heightened risk from COVID-19 and public policy should urge people with these risk factors to continue to avoid exposure to the contagion. These policies should not put healthy Americans who are younger than 55 under restrictive lockdowns, except in infection hot spots.REF
- Implement enhanced public health interventions in communities where infection rates are high. Lockdown orders have been intended to buy time, not to reverse the pandemic. In heavily hit areas, officials should increase testing capacity, implement large-scale contact tracing,REF and create temporary isolation centers in which the infected can recover without endangering others. In certain situations, lawmakers can also introduce travel bans to prevent the proliferation of the virus from hotspots to other communities.
- Encourage the private sector to develop and support voluntary isolation centers. Policymakers can learn from the South Korean approach, which uses isolation centers to prevent COVID-19 patients from spreading the virus. The use of isolation centers to quarantine potential COVID-19 patients as well as those with mild symptoms on a voluntary basis has been suggested in previous Heritage Foundation research.REF Lawmakers can encourage private-sector industries that are currently suffering major setbacks to help in this process. For example, since the hotel industry has incurred significant setbacks due to the virus, one option is to encourage hotels themselves to become isolation centers.REF The cruise industry, which has also suffered major setbacks, could also provide docked cruise ships for a similar purpose.REF The Trump Administration and state governors should discuss with private insurance companies, as well as the Centers for Medicare and Medicaid Services, the idea of reimbursing patient stays in isolation centers, as they already do for many other medical treatments and procedures.REF
- Improve upon voluntary randomized testing to understand asymptomatic rates. Testing in various areas of the United States, as well several other countries, suggests that there is a non-trivial asymptomatic prevalence of the disease.REF For a variety of reasons, it is paramount to garner an accurate sense of the prevalence of asymptomatic carriers of COVID-19. First, the prevalence of asymptomatic cases enables researchers to better understand case fatality rates of COVID-19, as higher asymptomatic rates lower the overall case fatality rates of the disease.REF Second, epidemiological models, on which policymakers rely heavily, cannot make accurate forecasts without proper assumptions, including asymptomatic case rates.REF Third, and most important, asymptomatically infected individuals may unknowingly spread the disease to others, including the most vulnerable. The Trump Administration should discuss the idea of pursuing voluntary randomized testing to get a better sense of these numbers with local communities and major laboratory companies, such as Quest and LabCorp. The CDC, and even local hospital systems, should pursue such efforts with local public health departments.
- Use the Defense Production Act (DPA) to expand testing capabilities. If the Administration believes that private industry is not responding appropriately, President Trump should invoke the DPA as needed to help improve laboratory capacity to ensure adequate testing. The 1950 DPA enables the President to “invoke a broad set of authorities to influence domestic industry in the interest of national defense. The authorities can be used across the federal government to shape the domestic industrial base so that, when called upon, it is capable of providing essential materials and goods needed for the national defense.” The act was signed into law by President Harry Truman and was intended to be applied to “national defense;” however, Congress has considerably broadened the concept of national defense to apply to a variety of circumstances including national emergencies.REF Extensive testing allows the infected to be identified and isolated without having to lock down the entire country. As areas of the country begin to re-open their economies, the demand for testing will increase significantly.
Conclusion
Countries around the world have pursued a variety of policies to deal with the COVID-19 pandemic, and policymakers now have more than five months of data from which to learn. This Special Report presents a comprehensive analysis of those policies to guide policymakers as they develop better and evolving responses to the COVID-19 pandemic. The evidence suggests that, among other important findings, broad lockdown orders that fail to focus primarily on the most vulnerable members of the population—particularly the elderly—have not produced superior outcomes to less restrictive policies.
Kevin D. Dayaratna, PhD, is Principal Statistician, Data Scientist, and Research Fellow in the Center for Data Analysis, of the Institute for Economic Freedom, at The Heritage Foundation. Patrick Tyrrell is Research Coordinator in the Center for International Trade and Economics, of the Kathryn and Shelby Cullom Davis Institute for National Security and Foreign Policy, at The Heritage Foundation. Andrew Vanderplas is Special Assistant and Research Associate for the Project for Economic Growth, of the Institute for Economic Freedom.




