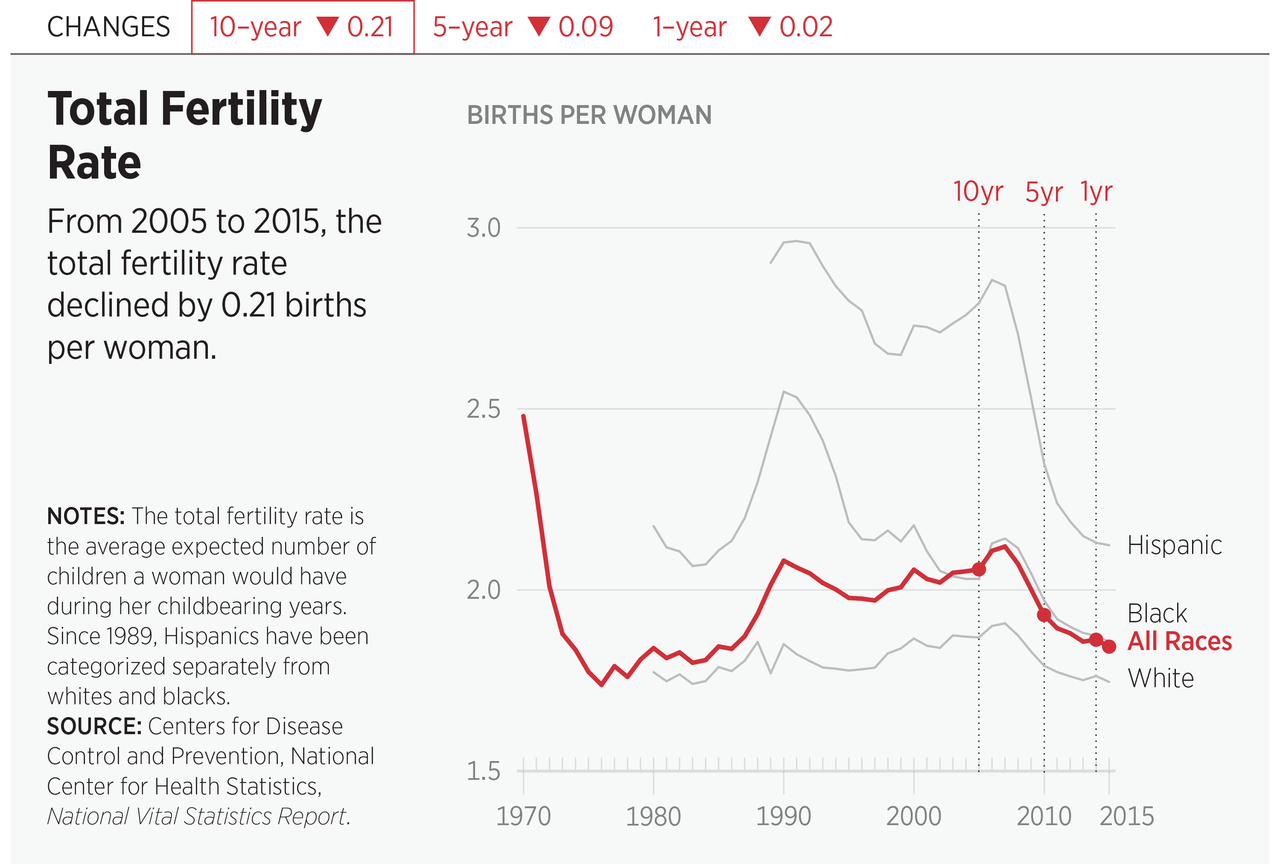
It is no news that overall fertility rates in America have been declining over the past decade. Part of this decline has to do with both men and women waiting until later to marry, and couples waiting later to begin building their families, than in the past.1 In addition, over several generations, more women have been pursuing higher education and graduate degrees and spending a large portion of their most fertile years building their careers.2
Between celebrities having children well into their 40s and companies adding “benefits” like egg-freezing technologies, women are lured into the belief that they can have children whenever they are finally ready. However, the biological clock is still alive and ticking when it comes to fertility.
In 2001, the American Society for Reproductive Medicine (ASRM) launched an educational campaign titled “Protect Your Fertility” to inform women of these dangers.3 The campaign grew out of the ASRM’s increasing awareness of the problems associated with waiting too long to begin having children and a desire to give women the facts about what happens when they postpone pregnancy and childbirth.
The truth is that for both mother and child, pregnancy is better earlier rather than later. Assisted reproductive technology and egg freezing are not magic pills to take when you are ready for a baby. Sadly, some feminist groups criticized the initiative, calling it a “scare campaign” to convince women to “hurry up and have kids.”4 This is the same feminism that misled Anne Taylor Fleming, author of Motherhood Deferred, to describe her own feeling of empowerment thusly:
Armed with my contraceptives and my fledgling feminism…with our birth control pills and the exhortations of the feminist foremothers to urge us on, what could stop us? We were the golden girls of the brave new world, ready, willing, and able to lay our contraceptively endowed bodies across the chasm between the feminine mystique and the world the feminists envisioned.5
However, this empowerment eventually left Fleming on the “baby chase.”6 What do such baby chases entail, and what are the risks and harms?
First, for the fertile woman seeking to postpone childbirth, it includes the latest scheme called egg freezing, but banking your frozen eggs does not erase the biological reality of maternal age. An ASRM report “states that live birth rates declined consistently with maternal age,” regardless of the method used to freeze eggs.7 Even if, under optimal conditions, we can freeze the eggs of a 30-year-old woman and give her a 13 percent chance of an implantation in her 40s, there is still a much higher risk of maternal morbidity and stillbirth.
With advancing maternal age, in vitro fertilization (IVF) is almost always required to achieve a pregnancy, and IVF comes with its own inherent risks and failures.8 The majority of all IVF cycles fail, meaning that a live birth is almost never achieved. Fertility drugs carry a whole host of risks to women’s short-term and long-term health.9
A pregnancy for a woman in her 40s has a rate of infant mortality second only to that of teen pregnancies.10 One study showed that “more than one fifth of all pregnancies in 35-year-old women resulted in fetal loss; for women at 42 years of age, more than half of the intended pregnancies (54.5 percent) resulted in fetal loss.”11 In short, “there is an increasing risk of fetal loss with increasing maternal age in women aged more than 30 years. Fetal loss is high in women in their late 30s or older, irrespective of reproductive history.”12
Moreover, a woman who postpones pregnancy into her 40s may need the assistance of eggs from a young, healthy, fertile woman and/or the womb of a healthy woman, each of whom are subject to health risks. Also, as IVF technologies are still fairly new, we are only now seeing that the children born out of these technologies are themselves at risk for certain types of medical problems.13
So what does all of this mean for declining fertility rates in the U.S.? It means that we need to do a much better job of educating people on the limitations of human fertility. These limits need to be discussed in light of the new novel “solutions” that lure people into thinking that we can defer motherhood to fit our own timeline. It also means that we need to stop practices that may bring harm to others: the children born from high-tech pregnancies as well as the women who are exploited for their healthy reproductive capacities.
Jennifer Lahl is Founder and President of the Center for Bioethics and Culture Network.
ENDNOTES:
1. John Fleming, “Gallup Analysis: Millennials, Marriage and Family,” Gallup Polling, May 19, 2016,
http://www.gallup.com/poll/191462/gallup-analysis-millennials-marriage-family.aspx (accessed April 25, 2017).
2. Ellie Kincaid, “Why Having Kids Later Is a Really Big Deal,” Business Insider, June 30, 2015,
http://www.businessinsider.com/why-delaying-parenthood-and-having-kids-later-is-a-big-deal-2015-6 (accessed April 21, 2017).
3. Naomi R. Cahn and June Carbone, “The Gender/Class Divide: Reproduction, Privilege, and the Workplace,” Florida International University Law Review, Vol. 8, No. 2 (2013), pp. 287–316, http://ecollections.law.fiu.edu/lawreview/vol8/iss2/6/
(accessed April 17, 2017).
4. Rebecca Leung, “The Biological Clock,” CBS News, 60 Minutes, August 14, 2003,
http://www.cbsnews.com/news/the-biological-clock/ (accessed April 25, 2017).
5. Anne Taylor Fleming, Motherhood Deferred: A Woman’s Journey (New York: G.P. Putnam’s Sons, 1994), p. 15.
6. Holly Finn, The Baby Chase: An Adventure in Fertility (San Francisco: Byliner Inc., 2011).
7. Jennifer Lahl, “Egg Freezing: Beating Biology and Buying Time, But at What Cost?” Center for Bioethics and Culture Network, June 4, 2014, http://www.cbc-network.org/2014/06/egg-freezing-beating-biology-and-buying-time-but-at-what-cost/
(accessed April 17, 2017).
8. Ibid.
9. Ibid.
10. U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System, “Infant Mortality Statistics from the 2013 Period Linked Birth/Infant Death Data Set,” National Vital Statistics Reports, Vol. 64, No. 9 (August 6, 2015), p. 14, Table 1,
https://www.cdc.gov/nchs/data/nvsr/nvsr64/nvsr64_09.pdf (accessed April 17, 2017).
11. Anne-Marie Nybo Anderson, Jan Wohlfahrt, Peter Christens, Jørn Olsen, and Mads Melbye, “Is Maternal Age an Independent Risk Factor for Fetal Loss?” Western Journal of Medicine, Vol. 173, No. 5 (November 2000), p. 331, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1071156/ (accessed April 17, 2017).
12. Ibid.
13. Marte Myhre Reigstad, Inger Kristin Larsen, Tor Åge Myklebust, Trude Eid Robsahm, Nan Birgitte Oldereid, Louise A. Brinton, and Ritsa Storeng, “Risk of Cancer in Children Conceived by Assisted Reproductive Technology,” Pediatrics, Vol. 137, No. 3 (March 2016), pp. 1–14, http://pediatrics.aappublications.org/content/pediatrics/early/2016/02/02/peds.2015-2061.full.pdf (accessed April 17, 2017); Sheree L. Boulet, Russell S. Kirby, Jennita Reefhuis, Yujia Zhang, Saswati Sunderam, Bruce Cohen, Dana Bernson, Glenn Copeland, Marie A. Bailey, Denise J. Jamieson, and Dmitry M. Kissin, “Assisted Reproductive Technology and Birth Defects Among Liveborn Infants in Florida, Massachusetts, and Michigan, 2000–2010,” JAMA Pediatrics, Vol. 170, No. 6 (June 6, 2016), pp. 1–9, http://jamanetwork.com/journals/jamapediatrics/fullarticle/2506140 (accessed April 17, 2017); and Center for Bioethics and Culture Network, “Three Things You Should Know About Third Party Assisted Reproduction,” pp. 1–2, http://www.cbc-network.org/pdfs/3_Things_You_Should_Know_About_Third_Party_Reproduction-Center_for_Bioethics_and_Culture.pdf (accessed April 17, 2017).