EXECUTIVE SUMMARY
The Second Stage of Medicare Reform: Moving to a Premium-Support Program
Medicare is in deep financial trouble. The right way to make it available and affordable for future generations is not through price controls and regulation, but through a bipartisan approach, as outlined in The Heritage Foundation’s Saving the American Dream, that achieves prudent budget targets while protecting seniors from financial risk. Properly designed, premium support can do that.
A Bipartisan Tradition. Of all Medicare changes advanced over the past three decades, only premium support—a variant of defined-contribution financing—has inspired bipartisan leadership for comprehensive structural reform. Building on the successful experience of existing premium-support systems, such as Medicare Part D and the Federal Employees Health Benefits Program (FEHBP), Congress therefore should:
- Simplify traditional Medicare. Congress should create a uniform Medicare fee-for-service (FFS) plan, combining the benefits of Parts A, B, and D with a catastrophic benefit. For beneficiaries choosing traditional Medicare, the cost for a single stated premium sufficient to finance the combined FFS benefits would be offset by the government’s premium support. Beneficiaries would pay one premium, minus the government contribution, and one set of co-payments for a traditional FFS plan.
- Establish a defined-contribution payment system. The government’s contribution to enrollee coverage would be based on regional competitive bidding among health plans, including Medicare FFS. Regional bidding (using existing Medicare Advantage or Part D regions) would be based on the provision of Medicare Parts A, B, and D benefits, or an actuarial equivalent, plus catastrophic coverage. After an initial five-year period, during which it would pay each health plan an amount equal to 88 percent of the total cost based on the weighted average premium for competing plans in that region, the government would pay its contribution based on the bid of the lowest-cost plan or the average of the three lowest-cost plans.
- Allow wide-open competition. During an initial two- or three-year transition period, Congress should allow new retirees to keep their current health plans (assuming that they provide catastrophic protection) as “deemed automatically eligible” for participation in Medicare premium support. The new market would be open to employment-based, individual, small-group, large-group, managed-care, Medicare Advantage, FEHBP, and state-employee health plans. Retirees with health saving accounts would also be able to bring them into retirement.
- Reduce the government’s defined contribution for upper-income Americans and eliminate it for the wealthiest enrollees. Congress should tighten current income thresholds for future government premium-support contributions, index these thresholds to inflation, and phase out subsidies for the wealthiest cohort of retirees (about 3.5 percent of the Medicare population). All retirees should be able to enroll in Medicare, pay premiums at competitive rates, and take advantage of guaranteed-issue, community-rated health insurance in large national and regional pools.
- Put Medicare on a true budget. Congress should put Medicare on a long-term budget, like most government programs. It should cap annual Medicare spending at the rate of inflation, measured by the CPI, plus 1 percent and, if needed to stay under this cap, adjust plan payments accordingly to restrain medical inflation.
- Establish fair administration and a level playing field. Medicare premium support should be administered by Medicare’s Center for Drug and Health Plan Choice to ensure a level playing field for market competition among diverse health plans while enforcing rules for consumer protection, just as the Office of Personnel Management does in administering the FEHBP. To prevent any conflict of interest, Congress must also separate supervision of the competitive system from administration of traditional Medicare.
- Retain Medicare insurance rules. Congress should retain Medicare’s community rating (the same premiums for all enrollees based on the characteristics of the entire pool rather than separate premiums based on individual characteristics); guaranteed issue (policies are available to enrollees regardless of health status or pre-existing conditions); and guaranteed renewability (enrollees have the right to continue the policy as long as they make premium payments). Seniors’ right to keep their current plans or enroll in a better one would be guaranteed through an annual open season, just as it is today in Medicare Advantage.
- Establish an effective risk adjustment for insurance. Congress should allow private plans a high degree of freedom in managing health risks while providing a generous government contribution. Improving on the FEHBP model, Congress could keep the prospective risk-adjustment models already in place for Medicare Advantage and Part D and improve upon them. Alternatively, it could establish a national risk-transfer pool and require plan membership in the pool.
A Better Medicare Future. Medicare premium support offers many advantages. As in the FEHBP, patients would have better choices and broader access to quality care through a variety of health plans, benefit options, physicians, and specialists on both the regional and national levels. It would foster greater innovation in health care delivery, harness technology more efficiently and safely, and secure higher value at lower cost—an estimated savings of $702 billion over the initial 10 years. It would also reduce the bureaucracy, red tape, waste, fraud, and politicization that characterize today’s program and compromise care for retirees.
—Robert E. Moffit Ph.D., is a Senior Fellow in the Center for Policy Innovation at The Heritage Foundation.
The Second Stage of Medicare Reform: Moving to a Premium-Support Program
Abstract: Medicare is in deep trouble. Major change is inevitable. But major Medicare reform must address the needs of a huge and diverse generation of new retirees, not merely enhance the power of the federal bureaucracy or protect the narrow interests of politically connected providers. The Heritage Foundation has developed such a reform—a variant of defined-contribution financing commonly called “premium support”—in its comprehensive budget proposal, Saving the American Dream. The Heritage proposal not only restores Medicare solvency, it also achieves a balanced budget in 10 years, and maintains it, without raising taxes.
“We all agree that the Medicare benefits package could and should be better than it is. The 1965 model we’re running Medicare under today needs to be updated and modernized for the 21st century and adapted to conform to modern notions of health care delivery. I believe that a premium-support approach is the best way to do that.”
—Senator John Breaux (D–LA), 1999, former co-chairman of the
National Bipartisan Commission on the Future of Medicare
One thing is certain: Regardless of congressional action or inaction, Medicare beneficiaries, especially baby boomers, will pay more for their benefits and government will pay less.[1] Under the Patient Protection and Affordable Care Act of 2010 (PPACA), for example, Medicare beneficiaries face major premium increases, higher drug costs, and guaranteed reductions in access to care resulting from payment reductions to hospitals, home health agencies, nursing homes, even hospice care.[2] Deeply flawed Medicare payment systems are also on automatic pilot to cut reimbursements to physicians. Medicare provider payments are on a downward slope toward Medicaid reimbursement levels, meaning that many Medicare patients, just like Medicaid patients today, will have serious trouble finding providers who will take care of them.[3]
Concentrated Power. More ominously, the PPACA created a powerful 15-member Independent Payment Advisory Board (IPAB) charged with making “detailed and specific” recommendations, subject to neither administrative nor judicial review, for further Medicare payment cuts to doctors and other medical professionals to meet hard spending targets.[4] Unless Congress enacts alternative and equal savings, IPAB’s recommendations are automatically executed. Remarkably, President Obama wants to enhance IPAB’s power. Some of the President’s allies in the health policy community even want to extend that power over doctors and hospitals in the private sector.[5] This is tantamount to rationing through price regulation.
Outdated Structure. Medicare was originally designed as the foundation of national health insurance.[6] Even though it is based on central planning and price controls, the program is run by private contractors, doctors, and hospitals. This arrangement spawned a massive and growing federal regulatory regime.[7]
With the Balanced Budget Act of 1997, the Medicare Modernization Act of 2003, and the PPACA of 2010—all three adding hundreds of provisions to the Medicare statute—the Medicare bureaucracy has become a regulatory gusher, compounding the transactional costs of doctors and hospitals and other medical providers already struggling with reams of government red tape and paperwork. Patients suffer as a result. Says Douglas Perednia, M.D., formerly a principal investigator on computer imaging for the National Cancer Institute,
A wide range of state and federal rules suck up enormous amounts of provider time and overhead. As time is the only inventory clinicians have, more time spent on administration means that less time will be spent on providing services to patients. Less time with patients yields fewer services and lower total bills. The de facto result is a rationing of care.[8]
Medicare, which processes 4.5 million claims per day, is also plagued by the triple threat of waste, fraud, and abuse. While honest medical professionals try to abide by the voluminous rules and avoid audits, investigations, and fines and penalties, the sheer complexity of the system and its regulatory regime creates a cluttered environment in which clever and dishonest providers flourish at taxpayers’ expense.[9]
Meanwhile, Medicare’s decisions are subject not only to intense bureaucratic infighting, but also to detailed congressional micromanagement. The result: Medicare has evolved into a great arena for special-interest politics and income redistribution, the battleground of the “Medicare Industrial Complex,” as described by Bruce Vladeck.[10] Armies of lawyers, lobbyists, and consultants for medical specialty organizations, providers, and beneficiary groups engage in an annual fight to increase federal payments; change reimbursement rules; add benefits or medical treatments to Medicare coverage; and obstruct new ideas and innovations, even promising demonstration projects.
A Better Program. Congress should reform Medicare with a focus on improving the program’s financial condition.[11] But this initial reform should be undertaken as preparation for restructuring Medicare and changing it into a premium-support program, where the federal government would make a defined contribution to the cost of enrollees’ chosen coverage. A Medicare premium-support program would provide comprehensive coverage and increase patient satisfaction, while controlling costs and securing better value for patients. For more than five decades, the Federal Employees Health Benefits Program (FEHBP), serving federal workers and retirees, has been a popular and successful premium-support program. Based on competitive bidding among private health plans, the government makes a defined contribution to the health plan of the enrollee’s choice. There are a wide variety of plans and benefit options at local and national levels. All plans must meet standards for fiscal solvency and consumer protection; no plans may exclude enrollees for pre-existing medical conditions. Congress should build upon the best features of the FEHBP as a working model for Medicare reform.[12]
Walton Francis, a former official at the Department of Health and Human Services (HHS) and a prominent Washington-based health care economist, has examined decades of comparative data and concluded that
For over most of its fifty years, the FEHBP has outperformed original Medicare in every dimension of performance. It has better benefits, better service, catastrophic limits on what enrollees must pay, and far better premium cost control, despite covering a federal workforce that rapidly aged throughout this period and a retiree population that rapidly grew—both major causes of higher health care costs. Fraud is rampant in Medicare and almost non-existent in the FEHBP. Medicare is low hanging fruit for “rent seeking” private interests who leverage billions of dollars through their lobbying activities and the congressional bounty they obtain; the FEHBP has been virtually immune to such assaults.[13]
Premium Support: A Bipartisan Remedy for Medicare’s Ills
The phrase “premium support” was initially coined by Henry Aaron of the Brookings Institution and Robert Reischauer of the Urban Institute as a description of their 1995 proposal for Medicare reform,[14] but the basic approach has had a long and distinguished history of bipartisan support. While there are crucial differences in the details among different proposals, premium support is a variant of defined-contribution funding for health insurance: The government makes a direct contribution, in an amount determined by a formula, to an enrollee’s chosen health plan.[15]
In 1980, Representatives Richard Gephardt (D–MO) and David Stockman (R–MI) proposed the National Health Reform Act, which contained a defined contribution for Medicare, and President Ronald Reagan also offered a defined contribution for Medicare in his fiscal year (FY) 1981 budget proposal.[16] In 1983, Gephardt and Stockman re-introduced their comprehensive National Health Reform Act (H.R. 850), which would have provided Medicare beneficiaries with a defined contribution equal to “the average health care expenditure” in a geographic area.[17] In 1995, Congress enacted the Balanced Budget Act of 1995, which also contained a premium-support provision, with a government contribution based on competitive bidding; it would have enabled beneficiaries to remain in traditional Medicare or enroll in a private plan of their choice.[18] President Bill Clinton vetoed the bill.
The Balanced Budget Act of 1997 created the 17-member National Bipartisan Commission on the Future of Medicare, chaired by Senator John Breaux (D–LA) and Representative Bill Thomas (R–CA). The commission’s majority supported a premium-support proposal, but fell one vote shy of meeting the statutory condition for a formal recommendation to Congress. The product of more than 18 months of detailed analysis and deliberations, the Breaux–Thomas proposal, modeled after the FEHBP, provided a generous government contribution to health plans, adjusted for age and income, and was based on geographic competitive bidding; a unification of Parts A and B into one plan with one trust fund, run by the government with new managerial flexibility; an increase in the normal retirement age from 65 to 67; the addition of catastrophic and drug coverage; and an independent board to administer the competitive system. The Breaux–Thomas proposal was a template for subsequent legislation.[19]
Premium support, in various forms, has also been endorsed by some of the nation’s most prominent health policy specialists, including Alice Rivlin of the Brookings Institution, Alain Enthoven of Stanford University, Mark Pauly of the University of Pennsylvania, Bryan Dowd and Roger Feldman of the University of Minnesota, and former Medicare administrators Gail Wilensky and Mark McClellan. Analysts with the American Medical Association, the American Enterprise Institute, the Cato Institute, the National Center for Policy Analysis, the Progressive Policy Institute, as well as The Heritage Foundation, have promoted or developed premium-support reforms.
More recently, the House Budget Resolution of 2011 authorized premium support, based on the proposal of Representative Paul Ryan (R–WI).[20] Premium support is also embodied in recommendations by the Bipartisan Policy Center’s Debt Reduction Task Force, and the Committee for a Responsible Federal Budget. Premium support is even offered as a potential cost-control option by the President’s National Commission on Fiscal Responsibility and Reform (the Bowles–Simpson Commission).[21]
Steps to Premium Support
Building on this large body of policy work, Congress can take decisive steps to create a premium-support program:
1) Simplify Traditional Medicare. As outlined in Saving the American Dream,[22] Congress should create a uniform Medicare fee-for-service (FFS) plan, combining the benefits of Parts A, B, and D, with the addition of a catastrophic benefit.[23] In other words, beneficiaries would pay a single stated premium, at an amount that would finance the combined FFS benefits, and the cost of that premium would be offset by the government’s premium support. So, beneficiaries would pay one premium and one set of co-payments for one plan. Beneficiary and taxpayer funds would be deposited in one Medicare FFS trust fund. By unifying Medicare this way, Congress would take a big step toward premium support, allowing a modernized Medicare FFS plan to compete on a level playing field with private health plans.[24]
Medicare today is organized into four parts, each with different sources and methods of financing. Part A, the Hospitalization Insurance (HI) program, is funded by a federal payroll tax on today’s workers and deposited in a trust fund that finances today’s retirees. Part B, the Supplementary Medical Insurance (SMI) program, pays doctors, funds outpatient medical services, covers payment for a certain class of drugs, and is financed by a combination of beneficiary premiums and automatic draw downs on general revenues from federal income and business taxes. Part C, Medicare Advantage, is a system of private health plans financed by a combination of premiums and federal payments, though payment to these plans is “benchmarked” to Medicare’s existing administrative payment. Part D, the prescription drug program, is also financed by a combination of beneficiary premiums and taxpayer subsidies. Part D, however, operates on a premium-support basis similar to that of the FEHBP.
The division of Medicare into different parts with radically different funding streams is mostly a reflection of short-term political responses rather than a product of deliberate policy,[25] and it contributes to unnecessary complexity. As Aaron and Reischauer observed in 1995, “Whatever rationale may once have existed for the distinction between services in Parts A and B, medical technology, the development of new forms of service delivery, and new payment structures have rendered it obsolete.”[26] The policy to unify traditional Medicare has also been suggested by the Bipartisan Policy Center, the National Commission on Fiscal Responsibility and Reform, and the American Enterprise Institute. The idea is also embodied in the Coburn–Lieberman proposal.[27]
2) Establish a Defined-Contribution Payment System. As outlined in Saving the American Dream, the government’s contribution to enrollee health coverage would be based on a regional competitive bidding process among health plans, including Medicare FFS. The bidding process would take place in geographically defined regions throughout the country.[28] Regional bidding would be based on the provision of Medicare Parts A, B, and D benefits, plus catastrophic coverage.[29] Congress should also allow health plans to compete on a nationwide as well as a regional basis.
On the basis of these regional market bids, the government would annually calculate the weighted average premium in any given region. During the first five years of the new premium-support system, the government would pay each health plan an amount equal to 88 percent of the total cost, based on the weighted average premium for competing plans in that region.[30] After that initial five-year period, the government would then pay 88 percent of the contribution based on the bid of the lowest-cost plan.[31] The Congressional Budget Office reports that in using the lowest-cost-plan bid as the payment benchmark, Medicare spending could be reduced by 8 percent to 11 percent.[32]
Using the lowest-cost-plan bid to secure consequential program savings should be compatible with the goal of assuring adequate coverage for beneficiaries. But there is more than one way to accomplish that objective. Picking just one low-cost plan is the simplest way to achieve savings, but it might give too much weight to an outlier, a plan with a stringent or very small network of providers. Another approach might be to base the government payment on the average of the three or five lowest-plan bids in a region. This could also achieve the objective of a low-cost benchmark for government payment.
The contribution amount of 88 percent was embodied in the Breaux–Thomas proposal, and endorsed in 1999 by the majority of the National Bipartisan Commission on the Future of Medicare. Though varying slightly from year to year, Medicare beneficiaries’ share of Part B premiums have historically averaged about 12 percent of the total program costs.[33] While the percentage contribution would be the same in each region, the actual dollar amounts would vary depending on the diverse market conditions in different parts of the country. In Miami, for example, the dollar amount might be larger than that of geographically less expensive service delivery in, say, Minneapolis. Given a fixed-dollar contribution, regardless of the plan that the beneficiary chooses, the beneficiary would pay the full amount above that government contribution. In other words, if a Medicare beneficiary wished to buy a regional or national plan that is more expensive than the defined contribution, he could do so, and pay extra out of pocket.[34] If a beneficiary wished to buy coverage that is less expensive than that amount, he would pocket the savings.
As noted, the FEHBP is a working model of a premium-support program. With the FEHBP, the government contribution is to be 72 percent of the weighted average premium of plans competing nationally. While the proposed Medicare contribution in the Heritage proposal would be larger, it is more precise in reflecting the impact of costs on persons at different income levels, as well as real differences in health care costs and delivery in different parts of the United States.
Congress should also encourage personal savings for Medicare beneficiaries wherever possible. In Medicare Part C, the government payment to Medicare Advantage plans is “benchmarked” at the cost of traditional Medicare FFS and capped at a level equal to the average amount in a local area. In Part D, the Medicare prescription drug program, the payment is capped on a national average of competing plans only. There is no Medicare FFS “benchmark” for the government payment in the drug program. Today, the beneficiary who buys a Part D plan receives 100 percent of the savings. But a Medicare beneficiary secures only 75 percent of the savings in Medicare Advantage program. By law, if a plan’s bid is under the government benchmark payment, the plan must rebate 75 percent of the savings to the beneficiary in the form of lower premiums or richer benefits; the remaining 25 percent of the savings is retained by the federal government.
More Savings. An even more intense market competition among plans holds the promise of ever greater savings and even better value for beneficiaries. It would be ideal if consumers could secure 100 percent of the savings resulting from their personal choices. One way to achieve that, and secure even greater savings for taxpayers and beneficiaries alike, is for Congress to authorize payment of 100 percent instead of 88 percent of the premium of the lowest-cost health plan. By removing the 88 percent cap on the lowest-cost plan, it might initially appear that taxpayer costs would be higher. But the removal of the cap would give competing plans even stronger incentives to offer benefit options—within the statutory benefit requirements—that are at or below the government’s defined contribution. This would intensify price competition in the Medicare market, which would, in turn, help to restrain overall premium increases on which the government’s payment is based.[35]
3) Allow Wide Open Competition. During the first two or three years of transition to the new premium-support program, Congress should allow new retirees to keep their current health plans as “deemed automatically eligible” for participation—assuming they provide catastrophic protection. Premium support would thus be available to employment-based plans, individual plans, small and large group plans, managed-care plans, FEHBP plans, and state-employee health plans. The new system would also be open to Medicare Advantage plans as well as to new health care delivery options. Those with health saving accounts would also be able to bring them into retirement, and likewise secure the standard government contribution.
After this initial grace period, health plans would be subject to certification for participation in the new Medicare premium-support program, assuming their compliance with basic benefit requirements, most importantly the provision for protection from the financial devastation of catastrophic illness.
4) Reduce and Eliminate the Government’s Defined Contribution for the Wealthiest Enrollees. The allocation of limited Medicare dollars should be focused on the security of retirees, particularly those of limited means, and guarantee their protection from the financial devastation of catastrophic illness. Congress should tighten the current income thresholds for future government contributions—in the form of taxpayer subsidies for premiums—that already exist in Medicare Parts B and D, index these thresholds to inflation, and phase out taxpayer subsidies for the wealthiest cohort of retirees entirely.[36] This relatively small number of unsubsidized wealthy individuals and couples—about 3.5 percent of the Medicare population—would nonetheless be able to enroll in the Medicare program, pay competitive premiums, and retain existing guaranteed-issue, community-rated health insurance in a large pool.[37]
Under current law, most beneficiaries pay only 25 percent of the premium costs of Medicare Parts B and D; the remaining 75 percent of the premium cost is subsidized by the taxpayers. For upper-income beneficiaries, the income thresholds for reduced taxpayer subsidies begin at $85,000 for an individual and $170,000 for a couple. This creates big “cliff effects” in government subsidies for those upper-income beneficiaries enrolled in Medicare Parts B and D. For these and higher-income beneficiaries, premium payments are increased (thus cutting taxpayers’ subsidies) on an income scale that would require them to pay 35 percent, 50 percent, 65 percent, or 80 percent of the full premium.[38] Moreover, under the PPACA, these “high income” thresholds are locked into place over the next 10 years, meaning that they will encompass an ever-larger population of Medicare beneficiaries and generate additional savings to the federal government.
Alternatively, under the Heritage proposal in Saving the American Dream, the premium support for a beneficiary’s chosen plan would start to be reduced for an individual with an annual income of $55,000. This is roughly $12,000 above the average annual income for an American worker. The phase-out of the government contribution would be gradual, reduced at 1.8 percent per year for every additional $1,000 in income above the threshold. The government contribution would be phased out entirely for a single beneficiary with an annual income above $110,000. For couples, the income range would be $110,000 to $165,000. Couples with annual incomes in excess of $165,000 would thus receive no government contribution in a Medicare premium-support program. Unlike current law, however, the income thresholds over the next 10 years and beyond would be indexed to inflation.
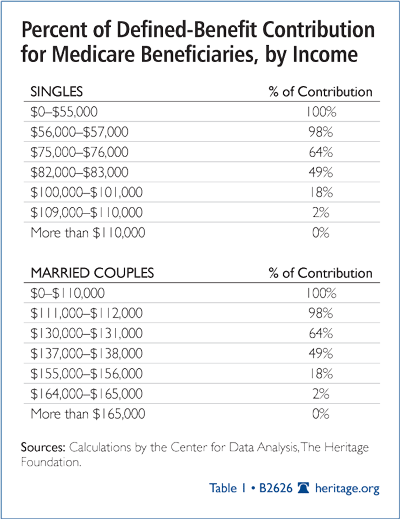
The proposed income-based subsidy system improves on current law. While the income thresholds are lowered, affecting about 9 percent of beneficiaries, the reduction in taxpayer subsidies for upper-income enrollees is not nearly as disruptive as current law; the phase-out of the government contributions is far more gradual. The new thresholds for phasing out the taxpayer subsidies are also indexed to inflation, as measured by the Consumer Price Index (CPI). Unlike the PPACA, this is a genuine structural reform, not merely a mechanism to secure “savings” for other entitlement expansions outside of program.
Income testing has been a regular feature of the Medicare program for many years. Part A hospital costs and Part B premiums and co-payments for low-income enrollees are financed through the Medicaid program. Among premium-support reforms, Senator Breaux’s 1999 proposal for the National Bipartisan Commission on the Future of Medicare included an income-related premium; low-income persons would continue to be subsidized through Medicaid, and high-income persons (with annual incomes in excess of 500 percent of the federal poverty level) would have paid a modest, additional 15 percent premium to cover health plan costs.[39] In 2011, Representative Paul Ryan, chairman of the House Budget Committee, proposed full premium support to 92 percent of Medicare beneficiaries, but would have reduced the government contributions to enrollees in the top 2 percent of income by 70 percent, and those in the next 6 percent by 50 percent.[40]
As outlined in Saving the American Dream, low-income seniors would continue to secure Medicaid subsidies, as they do today; and if they chose a private plan in the premium-support system, states would be able to use Medicaid funds to add to the federal contribution to seniors’ chosen coverage.[41]
5) Put Medicare on a Budget. As outlined in Saving the American Dream, Congress should establish a Medicare budget and cap annual Medicare spending at the rate of inflation, measured by the CPI plus 1 percent and enrollee population growth.[42]
Under the Heritage proposal, the Medicare spending cap would, of course, directly impact the share of the government contribution to health plans, including the traditional FFS option. In other words, the government share of the premium would be adjusted to ensure compliance with the spending cap. Under the Heritage proposal, the standard government contribution would be 88 percent of the plan’s premium cost. If that amount were to exceed the Medicare budget cap, the result would be a reduction of the government contribution to, say, 87 percent or 86 percent of the beneficiary’s premium cost. The payment adjustments would apply to all plans equally and all across the regions. They would also apply to national plans.
If health plan bids came in below the Medicare budget target, Congress could allow rebates to beneficiaries as direct deposits to their savings accounts, or authorize more generous benefits or premium reductions for beneficiaries, as is the case today with Medicare Advantage. Aaron and Reischauer suggested a variant of this approach in 1995, by allowing the difference between the amount of the government contribution and the cost of the plan to be “rebated to participants as nontaxable income or split between government and participants.”[43]
In the early 1990s, Medicare reformers, especially premium-support proponents, largely eschewed the employment of hard caps.[44] The tacit assumption was that big budget savings would follow the creation of a consumer-driven, highly competitive, market-based system: Get the structure right, get the economic incentives right, then the market forces will work, and the savings will follow. While those assumptions remain valid, the circumstances have changed. Record spending, dangerous deficits, and a national debt that is projected to surpass the size of the national economy threatens the economic safety and security of the public. Market reform requires a fallback, an external discipline that will guarantee a limitation on already unacceptably high levels of federal spending and debt.
The PPACA marks a major turning point in Medicare history by imposing a hard cap on Medicare spending. Surveying previous Medicare debates before 2003, Professor Jonathan Oberlander of the University of North Carolina notes that “Democrats widely viewed such a cap as threatening the ability of seniors to access quality medical care, and as incompatible with Medicare’s social contract and American conceptions of entitlement.”[45] In 2010, congressional Democrats reversed course and made sure that Medicare would no longer be an open-ended federal entitlement.
Even though Aaron and Reischauer did not endorse a hard external cap on Medicare spending in 1995, using indices of inflation or economic growth, they clearly outlined their goal for Medicare spending:
In the long run, the federal Medicare payment should grow at the same rate as per capita spending on health care for the non-elderly. This formula is mechanical and may require periodic adjustment, because the per capita cost of care depends on the average age of the population, the age specific gradient in health care costs, and the age bias of new medical technology. If Congress found it necessary to reduce federal support for Medicare, it could slow payment increases, thus shifting the costs to Medicare enrollees.[46]
Today, regardless of policy differences, there is a powerful bipartisan consensus that Medicare should, in some way or other, be a budgeted program.[47] Two years before the enactment of the PPACA, a variety of analysts with diverse views from the American Enterprise Institute, the Brookings Institution, the Concord Coalition, the New America Foundation, and the Urban Institute had concluded that “The first step toward establishing budget responsibility is to reform the budget decision process so that the major drivers of escalating deficits—Social Security, Medicare, and Medicaid—are no longer on autopilot.” They further recommended that “Congress and the president enact explicit long-term budgets for Medicare, Medicaid and Social Security that are sustainable, set limits on automatic spending growth, and reduce the relatively favorable budgetary treatment of these programs compared with other types of expenditures.”[48]
All caps are controversial because they set Medicare spending levels below the historical pattern of rising health care costs, but they vary in impact and timing. Holding Medicare spending growth to GDP plus 1 percent is currently the most favored option among many top health policy analysts.[49] It is embodied in the PPACA, beginning in 2018; it is endorsed by the Bipartisan Policy Center, also beginning in 2018; and the National Commission on Fiscal Responsibility and Reform, beginning in 2020. It is also a feature of the 2010 Ryan–Rivlin proposal. Analysts at the Center for American Progress are extreme; they want to limit all federal health spending, including Medicare spending, to flat GDP growth beginning in 2020. They would even extend the cost-control enforcement of the IPAB beyond Medicare to the private sector.[50]
But all caps are not the same, neither in their goals nor their functions. The PPACA cap on Medicare spending is the primary instrument to control Medicare costs. The cap is to be enforced through IPAB, which would make “detailed and specific” recommendations for provider payment cuts, i.e., price controls. This centralized process of elite decision making is the means by which scarce resources are to be allocated for officially sanctioned service reimbursements or favored care-delivery models.
The PPACA cap would function as the Medicare equivalent of a “global budget.” Such an approach has long been championed by the Left. A variant of the idea was embodied in the 1994 Clinton health plan and it has been a key feature of the British and Canadian health systems. Over time, the PPACA’s budgetary objectives would be secured through even tougher provider payment cuts, inviting rationing through reimbursement restrictions, much like national health insurance.
President Obama’s proposed cap is GDP plus one-half percent. Not only is the President’s cap tighter than current law, he is also offering it amidst a slow growth economy. Unlike the Ryan budget proposal, Obama’s stricter IPAB enforcement would, however, intensify the pressure of Medicare payment cuts already enacted under current law.[51]
In the case of the Heritage proposal, much like the Ryan proposal, the cap functions as a “fall-back” to control spending. The front line of cost control is personal choice in an intensely competitive market. This decentralized decision making among millions of beneficiaries interacting with numerous plans (and more than a million providers) in a new environment of plan and provider competition would drive plan and provider innovation and productivity and lower costs.
By capping Medicare spending at CPI plus 1 percent and enrollee population growth, the Heritage proposal would be a serious restraint on future Medicare spending. The cap would be slightly more generous than Representative Ryan’s budget proposal, which would cap the growth of Medicare spending at the CPI. Indexing spending growth to general price increases (using CPI), rather than normally higher medical prices, would serve to restrain rather than merely accommodate medical inflation.
The Heritage Foundation’s premium-support system, combined with safety valves for expanded access to care and more direct congressional control over the spending levels than under IPAB, is much more flexible and a far better option than either the President’s proposal or current law.[52]
6) Establish Fair Administration and a Level Playing Field. Medicare will remain a public program, notwithstanding overblown “privatization” rhetoric, and will require sound public administration. Medicare’s administration of a premium-support program should be vested in a federal agency or office with authority to ensure a level playing field for market competition among diverse health plans while fairly enforcing uniform rules for consumer protection. As noted in Saving the American Dream, the best candidate for such an agency already exists: Medicare’s Center for Drug and Health Plan Choice, the agency that today administers Medicare Advantage and the Part D drug program—the competitive portion of the Medicare program. Today, the Center for Drug and Health Plan Choice enforces marketing rules, and protects enrollees from marketing abuses.[53]
With Medicare premium support, the center would continue many of its current functions: enforcing a common set of rules for market competition and protecting consumers. In a new system, the center would have to certify that new plans entering into regional or national competition are duly licensed for insurance business by a state, meet federal solvency rules and reserve requirements for the payment of claims, meet the basic benefit standards established by law, and abide by the consumer-protection requirements.
The center’s role and responsibility would be similar to, but not identical to, that of the Office of Personnel Management (OPM). OPM, for example, administers the FEHBP as an employer, not just as an umpire enforcing the uniform rules of market competition. As an employer, OPM contracts with health plans and negotiates rates and benefits on behalf of federal workers and retirees. These negotiations are confidential and largely confined to national plans, while state and local plans are more or less automatically certified for FEHBP competition if they meet the basic benefit and insurance requirements. (Benefit categories for the FEHBP are a statutory requirement, and specified by Title V, Chapter 89.) OPM is to ensure there is a “reasonable” relationship between the plans’ rates and its benefits. While OPM enforces statutory requirements, it does not standardize benefits packages. There are thus a wide variety of plans and benefit options, with very different levels of premiums and cost-sharing arrangements. Only occasionally does OPM, as an employer, get into the business of dictating detailed and specific medical treatments or procedures.[54] If the director of OPM is dissatisfied with a plan’s offerings, or if the director deems a plan too costly, regardless of whether the plan meets other criteria, he can exclude that plan from competition with other plans. The director of OPM, acting as employer, has enormous residual authority, confirmed by the courts, over the FEHBP.
In Medicare premium support, the Center for Drug and Health Plan Choice would be solely an umpire. The center would therefore continue to admit plans that meet specified standards to compete, as it does today with Medicare Advantage and Medicare Part D. But it would have no authority to negotiate rates and benefits, nor should it standardize health benefit packages among competing plans.[55] But, like OPM, the center should have authority to certify that health plans provide certain categories of benefits—such as hospitalization, physicians services, emergency and ambulatory services, drugs, and catastrophic protection—and make sure that the basic offerings are actuarially equivalent to the Medicare benefit provisions of Parts A, B, and D in the bidding process. Plan benefits and premiums are to be fully transparent. If the plans do not meet either the benefit criteria or the insurance standards, the center should have the authority to exclude them from the program.
For administering Medicare premium support, Congress should further specify that the agency could not interfere with private contracting between health plans and medical service providers or with private contracting between beneficiaries and medical professionals, and should not impose premium caps on health plans, or price controls on doctors, hospitals, or other medical institutions, goods, or services. It should reaffirm Medicare’s original statutory prohibition against federal officials’ interference with, or supervision of, medical practice.[56] It should make these prohibitions explicit.
In almost all respects, then, the governance envisioned for the new Medicare premium-support program would be similar to the administration of the FEHBP: imposing uniform insurance rules on all participating health plans, especially rules for consumer protection (including fair marketing rules, protection against fraud and misleading advertising, and plain-English requirements in sales and contracts), conducting an open season for plan enrollment, establishing a grievance process for the expeditious resolution of claims or disputes, and enforcing strong fiscal solvency and reserve requirements. As Walton Francis observes, “Despite many millions of person-years of enrollment by retired federal employees and their aged surviving spouses, there has been no documented pattern of abuse of any kind by plans in the FEHBP.”[57]
In designing a new Medicare premium-support program, the economics of a level playing field are simple enough: no subsidy or regulatory advantage for any participant in the competition; no artificial obstacles to consumer demand or provider supply; free and equal access to and exit from the market. But the political science is more complicated. Congress must protect the taxpayers and the beneficiaries from any conflict of interest: The agency that administers a competitive system cannot have a relationship, even the appearance of one, with one of the competitors; the umpire cannot have a team on the playing field.[58] The problem is that the center is part of the Centers for Medicare and Medicaid Services (CMS), and the director reports to the administrator of CMS, the agency that runs the Medicare FFS plan, which would remain a competitor in the new premium-support system.
Congress could choose a number of options to resolve this problem. None is perfect. First, Congress could require the director of the center to report directly to the Secretary of HHS rather than the director of CMS. Second, Congress could move the center out of HHS entirely and make it an independent agency that reports directly to Congress, such as the Medicare Payment Advisory Commission (MedPAC). Third, Congress could transform the center into an independent commission, say, a new Medicare Patient Protection Commission, modeled after the Consumer Product Safety Commission (CPSC), with a board appointed by the President and confirmed by the Senate and serving staggered terms. In any case, it is absolutely critical to break the institutional connection between the Center for Drug and Health Plan Choice and CMS, which runs traditional Medicare. Otherwise, taxpayers will be faced with the inherent conflict created by a “public option”: a government agency sponsoring a government plan to expand its market share against private plans in a rigged competition. Indeed, under the PPACA, this problem already exists.[59]
7) Retain Medicare Insurance Rules. As recommended in “Saving the American Dream,” Medicare’s traditional insurance rules would remain the same: community rating, which means that premiums would be the same for all enrollees based on the characteristics of the entire pool, rather than separate premiums based on individual characteristics; guaranteed issue, meaning that policies would be available to enrollees regardless of health status or pre-existing conditions; and guaranteed renewability, meaning that enrollees would have the right to continue the policy, as long as they make premium payments. In practice, the right to renew the health insurance policy would be guaranteed annually through an annual open season, where beneficiaries could keep their current plans or change to a better one. This, too, is the practice of the FEHBP.
Medicare’s population, non-working and disabled citizens, differs from the FEHBP and employment-based pools: They are older, sicker, and live on fixed incomes. The highest concentration of Medicare costs is, of course, incurred by the oldest and sickest beneficiaries. While some have proposed age-adjusted premiums, it is unnecessary. The Medicare Advantage program has prospered under the traditional rules but, unlike the FEHBP, has improved its operations through a risk-adjustment mechanism; Medicare Advantage and Part D plan premiums do not vary by age or health status.[60] Likewise, under premium-support, potential problems can also best be handled through a sound risk-adjustment mechanism.
Improving on the FEHBP’s annual open-season process, Congress may wish to allow Medicare beneficiaries to enroll in plans for two or even three years. With longer-term contracts, plans would have even stronger economic incentives to promote wellness and preventative care programs. For beneficiaries who enroll in such programs, improve their health and reduce insurance claims, insurers would be able to provide premium discounts or even bonuses.[61]
8) Establish an Effective Risk Adjustment for Insurance. Any insurance market, even if it included just two health plans, faces adverse selection; a process of risk segmentation that can destabilize and destroy it. Any one of a number of plans will attract a disproportionate share of older and sicker beneficiaries. This drives up the premium costs of the plan and encourages younger and healthier beneficiaries to drop out of the plan, driving up the costs even further and causing the plan to fail. In a pluralistic market, especially if there are liberalized rules like guaranteed issue and community rating, the process repeats itself. Plans fail, and the destabilized market collapses—a “death spiral.”
However, at least one example is incompatible with the general theory. Since its inception in 1960, the FEHBP, the oldest, the largest, and the most pluralistic consumer-driven health insurance market in the world, has never experienced anything that could be fairly described as a death spiral.[62] While adverse selection has been a persistent problem, it has been a relatively minor one. Because the FEHBP is flexible, private plans enjoy a high degree of freedom in managing health risks. But the generosity of the government contribution is also an incentive for younger enrollees to purchase more expensive plans as well as less expensive plans, since the marginal costs of doing so are relatively modest. Thus, there is a broad distribution of younger and older enrollees among all of the plans competing in the program; indeed very little risk segmentation.[63] With the even more generous government contribution in the Heritage proposal, it is reasonable to expect similar dynamics in a new Medicare program.
Nonetheless, Congress should provide added protection against market instability. Risk adjustment would accomplish that objective; in particular, it would ameliorate the problems that naturally arise from the retention of Medicare’s community rating and guarantee-issue provisions—such as higher costs for younger (generally healthier) enrollees, encouraging them to drop out of a plan increasingly populated with older (generally sicker) members paying the same premiums as younger enrollees while incurring higher expenses. There are a few options. Congress could, for example, keep the risk-adjustment mechanisms already in place for the Medicare Advantage program and Medicare Part D, and improve them if necessary.[64]
Alternatively, Congress could establish a national risk-transfer pool, and require plan enrollment as a precondition of plan participation in Medicare. This is a retrospective system of cross-subsidization of health plans. It would have some special advantages. It would be neater and cleaner; the assignment of additional subsidies or premiums would be based on hard data, and not the best guesswork of projected outcomes or costs. While all plans would be required to participate, the governance of the national risk pool, its risk-premium setting, would remain in the hands of the private insurers. At the end of the enrollment year, if any given plan ended up with the largest concentration of risks, say, an inordinate enrollment of costly diabetics or cancer patients, that plan would be made whole by the common pool.[65] At the very least, it would be worth a demonstration project.
Advantages of Premium Support
For Medicare beneficiaries and taxpayers alike, a premium-support program would offer numerous advantages:
Better Choices and Access to Care. Premium support will guarantee beneficiaries a rich menu of plan choices, as well as access to a wide range of medical specialties at competitive rates. In the FEHBP, all enrollees, including those in rural areas, have a choice of dozen or more national plans, as well as state-based health plans. Patients have access to a broad array of physicians and medical specialists, as well as a variety of benefits and services. FEHBP plans also provide coverage for those traveling abroad.[66] This level of choice and access could be duplicated for Medicare enrollees.
While it is true that an estimated 95 percent of physicians accept Medicare patients, there are dramatic provider payment cuts already underway, and access to care for newly retired persons has been a growing concern. In 2008, for instance, 45 percent of medical providers in Oregon decided against taking new Medicare patients, even as the American College of Physicians says that rapidly aging Americans will need a 40 percent increase in primary care physicians by 2020.[67] Under the PPACA, as noted, Part A Medicare reimbursements will be relentlessly reduced, even to Medicaid levels. This guarantees reduced access to care, a problem aggravated by the rapidly emerging physician shortage.
Greater Innovation in Care Delivery. CMS actuary Richard Foster says that a premium-support program, where providers compete for market share on the basis of price, could encourage medical technology companies, among others, to pursue major, market-driven improvements in care delivery, instead of minor tinkering, that would deliver patients higher value at lower cost.[68]
Historically, the Medicare program has been notoriously slow. Says Marilyn Moon, “Despite general agreement since the 1970s that the benefit structure should be improved to reflect changes in the needs of Medicare beneficiaries and the evolution of private insurance over time, a major overhaul of the benefit package did not take place until December of 2003.”[69] The main reason: Benefit decisions are legislative and regulatory decisions, which are ultimately political decisions. Thus, as Francis notes, “Public programs like Medicare require years (not months, not weeks, not days) to make decisions that in the private sector can be and are often made in hours.”[70]
Payment and delivery-system changes are not only slow, but also contentious. Much Medicare decision making focuses on tinkering with flawed administrative payment formulas, like the resource-based relative value scale (RBRVS) or the sustainable growth rate (SGR). Inadvertent testimony to the sluggishness of Medicare change is the recent creation of the Centers for Medicare and Medicaid Innovation (CMI), a new agency authorized under the PPACA to pursue breakthroughs in Medicare payment and delivery reforms.
Competition would be a tonic for traditional Medicare and the CMS staff. The Obama Administration’s vaunted delivery reforms would have a better chance of working in a bracing competitive environment. With a robust premium-support system, CMI could succeed in head-to-head competition with private-sector innovators in securing greater patient satisfaction at lower cost; something far more rewarding than merely experimenting on a captive audience.
Superior Cost Control. Medicare premium support would secure superior cost control. Based on the estimates of the Heritage Center for Data Analysis (CDA), a Medicare premium-support program would yield $702 billion in savings over ten years beginning in 2016.[71]
Competition is a powerful engine of cost control, and its impact, better value for the dollars spent, would be felt throughout the health care delivery system.[72] Medicare actuary Foster says that premium support could encourage medical technology companies to produce goods and services at a lower cost, while reducing adverse events.[73]
During the deliberations of the National Bipartisan Commission on the Future of Medicare in 1999, Senator Breaux offered an initial premium-support proposal. Then-CBO director Dan Crippen observed, “We believe that introducing competition into the Medicare program could help to reduce costs in both the short and the long run. A premium-support system that resulted in effective price competition among plans would most likely lower Medicare costs.”[74] Medicare’s Office of the Actuary concurred with CBO’s expectations of long-term cost reductions.[75] With a slower growth in program costs, commission staff projected that the original Breaux proposal would mean that beneficiary premiums would be 15 percent to 25 percent lower than projections under what was then current law.[76]
In their final 1999 report, the commission staff produced an analysis of the proposal developed by Senator Breaux and Representative Bill Thomas. In that analysis, the commission staff projected a slowing of Medicare spending by an estimated 1 percent per year, and accumulating significant savings over time.[77] This annual percentage reduction was in line with a 1998 Lewin Group finding that a competitive program, accompanied by a growth in managed care enrollment, would result in long-term Medicare spending reductions between 0.5 percent and 1.5 percent annually.[78] Beneficiaries would no longer have to rely on costly supplemental insurance, but be able to take advantage of integrated, comprehensive coverage.
According to commission staff, beneficiaries would also have stronger incentives to secure better value from sharing savings by choosing more efficient and less expensive plans. Health plans, likewise, would have powerful economic incentives to compete on price by offering coordinated and integrated health coverage.
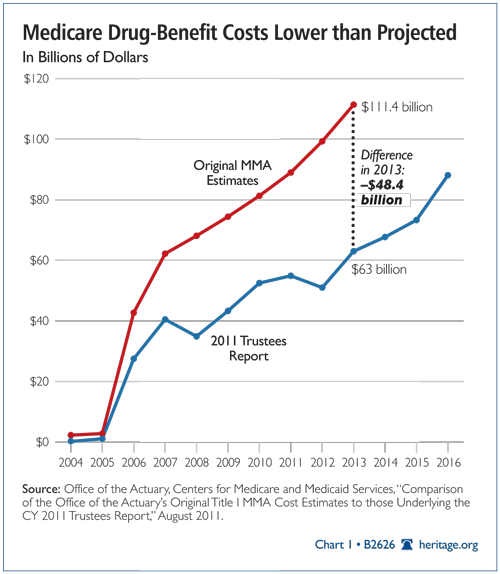
Congress today has the benefit of examining historical patterns of performance for premium-support programs.[79] In the case of Part D,[80] the program’s cost growth has come in well below the official projections. Over the period 2004 to 2013, based on the Medicare Actuary’s projections, Medicare Part D is 41.8 percent below the original cost estimate, yielding a total savings projected at $264.6 billion.[81] No other program, public or private, has shown such a dramatic performance in the health sector of the economy.
With FEHBP, the program has historically outperformed private health insurance.[82] Examining performance over a 20-year period, and adjusting for benefit improvements, notably the provision of prescription drugs, the Joint Economic Committee staff found that, in terms of average cost growth, the FEHBP also outperformed traditional Medicare on average 5.8 percent to 6.7 percent.[83]
Less Bureaucracy, Red Tape, and Politics. Traditional Medicare is a massive edifice of central planning. It is a sclerotic system governed by tens of thousands of pages of rules and regulations and guidelines, staffed by thousands of employees and thousands more contract workers. Medicare’s complex payment formulas (the RBRVS, the SGR, and diagnosis-related groups) for thousands of payments, invariably controversial in their application, also encourage routine congressional micromanagement. Because Medicare decisions are centralized, they are flashpoints in Congress and the federal bureaucracy. As Heritage Distinguished Fellow Stuart Butler has observed,
Providers included in the [benefits] package fight diligently—and usually effectively—to block serious attempts to scale back outdated coverage for their specialties. Meanwhile, talk of upgrading the Medicare benefits package unleashes an intense lobbying battle among other specialties that seek to be included in the Medicare benefits package. Invariably, the result depends as much (if not more) on shrewd lobbying than on good medical practice.[84]
The politics engendered by the outdated structure of traditional Medicare contributes directly to waste. As former Medicare administrator Bruce Vladeck observed in 1999, “There are plenty of $400 toilet seats in the Medicare program, because Medicare cannot deliver services to its beneficiaries without providers and because providers are major sources of employment, political activity and campaign contributions in every congressional district in the nation.”[85]
With a new Medicare premium-support system, the government would make one payment on behalf of a beneficiary or a couple to one plan. Its regulatory responsibilities would be confined to enforcing marketing and insurance rules, certifying plan participation, and consumer protection. Much of today’s bureaucracy and red tape would be rendered unnecessary. With a new managerial flexibility, CMS could be unleashed as an agent of innovation and patient satisfaction, experimenting with new payment and delivery reforms, while undertaking a long overdue “bottom up” review of its managerial needs. In the crucible of competition, it could enter the market and keep private health plans “honest,” while offering Medicare patients a better FFS product at a competitive price. The market share of Medicare FFS, with its combinations of premiums, co-payments, and benefits, would be determined solely by beneficiary choice.
In a consumer-driven market, with the diffusion of decision-making power among millions of enrollees, there would be a sharp decline in the influence of rent-seeking special interests, and a long overdue de-politicization of Medicare’s financing and delivery decisions. The program would function more like the market-driven FEHBP, and less like the rough political playground of the “Medicare Industrial Complex.” The FEHBP covers more than 8 million people and is administered by an OPM staff of approximately 150 civil servants, enforcing a spare statute and just 87 pages of rules published in the Code of Federal Regulations.[86]
Less Fraud and Abuse. Medicare, as noted, is plagued by scandalous levels of waste, fraud, and abuse. According to the Government Accountability Office, the annual loss amounts to $48 billion.[87] With Medicare FFS, the sheer number of transactions—government payments for roughly a billion claims annually submitted by hundreds of thousands of providers—the opportunities for this triple threat to the taxpayers are legendary.
With premium support, the government’s transactions are radically reduced to fixed and transparent annual payments to competing regional and national health plans; these plans have powerful economic incentives to police their contracts with medical providers and reduce the cost of fraud or improper payments. Losses from fraudulent or wasteful transactions directly affect their premium charges and undermine their competitive position in an intensely competitive market. Once again, Congress should carefully examine the comparative performance of the FEHBP and Medicare. As Francis has noted, “In only a relatively handful of instances in the past dozen years has the federal government lost substantial sums of money to actual fraud in or by private health plans participating in the FEHBP or Medicare Advantage….”[88]
Conclusion
In Saving the American Dream, The Heritage Foundation provides an outline of a new Medicare premium-support program. There are differences in detail compared to other proposals. But, as a policy for Medicare reform, premium support has a long history of bipartisan sponsorship. It has recently been embraced in one form or another by a wide range of analysts and institutions, including the American Enterprise Institute and the Bipartisan Policy Center Debt Reduction Task Force, and it is offered as a potential budget option by the National Commission on Fiscal Responsibility and Reform.[89]
Today, there are two working models of premium support: the FEHBP and Medicare Part D. Both have a great record of serious cost control, rich and varied benefit offerings, and high levels of patient satisfaction. Congress can replicate the success of these popular programs by transforming Medicare into an integrated plan ready to compete with private plans; establishing a defined-contribution payment system; focusing taxpayer subsidies on beneficiaries who need the most help; putting Medicare on a budget like other government programs; establishing a level playing field for open competition under uniform rules enforced by a neutral agency; and establishing an effective risk-adjustment system to cope with adverse selection.
Such a reform would improve Medicare for future retirees. It would expand their access to high quality care, and make Medicare practice far more attractive to physicians and other medical professionals. It would spur greater innovation in benefit design and care delivery, and it would reduce bureaucracy and red tape, as well as waste, fraud, and abuse. It would also end the paralyzing and unproductive politicization of crucial decision making over the provision of medical care for tens of millions of Americans. It would secure a superior and more cost-effective Medicare program for the next generation of retirees and taxpayers alike.
—Robert E. Moffit, Ph.D., is Senior Fellow in the Center for Policy Innovation at The Heritage Foundation.

