The Affordable Care Act (ACA) put in place three separate programs designed to mitigate some of the risks assumed by health insurers participating in the markets that are most significantly affected by the health care law. The three programs are reinsurance, risk corridors, and risk adjustment.
As a result of the ACA’s inherent flaws and questionable actions taken by the U.S. Department of Health and Human Services (HHS), two of these programs (reinsurance and risk corridors) could well cost taxpayers billions of dollars. Congress should act to protect taxpayers by stopping insurer bailouts through these programs and ensuring that these programs expire as intended.
Reinsurance
The ACA’s transitional reinsurance program is a temporary program for the years 2014–2016 that provides insurers in the individual market with a reinsurance subsidy for high-cost enrollees. The reinsurance program is funded out of per-enrollee assessments imposed on all individual and group health plans, including self-insured employer and union plans. Because the employer-group market is much larger than the individual market, the net effect of the reinsurance program is to provide subsidies to about 10 percent of the total private market, with funding coming principally from the other 90 percent.
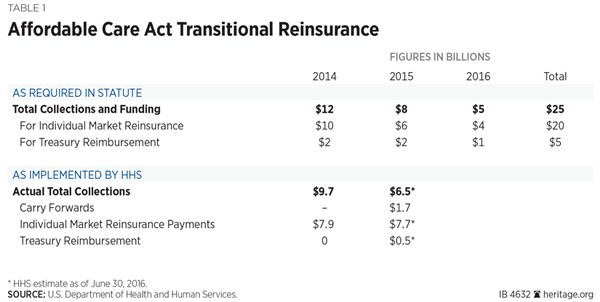
The law requires total collections of $25 billion over the three-year period for two purposes: for the reinsurance program itself and for deposits to the U.S. Treasury as an offset to the cost of the law.[1] The law specifies that collections for reinsurance shall total $10 billion for plan year 2014, $6 billion for plan year 2015, and $4 billion for plan year 2016. The law further specifies that deposits to the general fund of the U.S. Treasury shall total $2 billion for 2014, $2 billion for 2015, and $1 billion for 2016. Moreover, the statute explicitly states that this $5 billion “shall be deposited into the general fund of the Treasury of the United States and may not be used for the program established under this section.”[2]
Despite the ACA’s instruction to deposit specified amounts into the Treasury, these deposits have not been made. That is because HHS adopted a questionable regulatory interpretation in which it asserted that it has the authority to prioritize payments to insurers through the reinsurance program over payments to the Treasury.[3] The scheme devised by HHS directs that all funds collected up to the reinsurance amounts specified in statute each year will be paid to insurers for reinsurance purposes. Any additional collections are then split pro rata between the Treasury and administrative expenses.
As Table 1 shows, for 2014, HHS was supposed to collect $12 billion ($10 billion for reinsurance and $2 billion for the Treasury,).[4] However, HHS’s collection rate methodology was inaccurate, and only $9.7 billion was collected.[5] From that amount, HHS paid insurers 100 percent of their reinsurance claims (about $7.9 billion) and carried over the remaining $1.7 billion to distribute for reinsurance purposes in subsequent years.[6] The Treasury received none of the $2 billion owed as required by law for 2014.
For 2015, HHS’s collection was again about 20 percent short, totaling $6.5 billion of the statutorily required $8 billion ($6 billion for reinsurance and $2 billion for the Treasury). Of this amount, HHS intends to pay insurers $6 billion for reinsurance purposes and deposit only $500 million into the Treasury.[7] In addition, HHS intends to distribute the $1.7 billion carried over from 2014 to insurers to offset their 2015 reinsurance claims, making total reinsurance payments to insurers for 2015 $7.8 billion.[8]
Thus, for 2014 and 2015, insurers will receive a total of $15.7 billion, while taxpayers will receive only $500 million, or 12.5 percent of the $4 billion the law says they are owed.
HHS’s prioritization of funds is not authorized by the statutory text of the ACA. The Government Accountability Office (GAO), the official arbiter of appropriations law, has issued a legal opinion that:
HHS lacks authority to ignore the statute’s directive to deposit amounts from collections under the transitional reinsurance program in the Treasury and instead make deposits to the Treasury only if its collections reach the amounts for reinsurance payments specified in section 1341. This prioritization of collections for payments to issuers over payments to the Treasury is not authorized. The agency must give effect to the extent possible to all of section 1341, and, therefore, is required to collect and deposit amounts for the Treasury, regardless of whether its collections fall short of the amounts specified in statute for reinsurance payments.[9]
HHS’s unauthorized reinsurance payment scheme is already cheating the taxpayers out of $3.5 billion owed to the Treasury for 2014 and 2015, and this amount could reach $4.5 billion if HHS ignores the law for 2016 as well.
Risk Corridors
The risk corridor program, also a temporary program in operation between 2014 and 2016, essentially establishes a range (or “corridor”) for profits or losses for insurers selling coverage on the exchanges. If an insurer’s profits are higher than expected, the government will “claw back” some of the money. Conversely, if an insurer’s losses are higher than expected, the government will pay the insurer additional subsidies to offset those losses. Thus, depending on the experience of exchange insurers, the program could generate either net receipts or net outlays for the federal government.
This gave rise to a concern that taxpayers could be left bailing out unprofitable insurers. In response, Congress inserted provisions into the annual government funding bills requiring that the risk corridor program be budget neutral for fiscal years 2015 and 2016.[10]
As Heritage had predicted,[11] far more insurers have lost money than made money on the exchanges. For 2014, risk corridor claims totaled $2.87 billion, but risk corridor charges totaled only $362 million.[12] For 2015, claims totaled more than $5.9 billion, and charges totaled about $95.4 million.[13] Thus, the risk corridor program has a cumulative funding shortfall of $8.3 billion for 2014 and 2015. If Congress had not acted to make the program budget neutral, the taxpayers would have had to pay for the funding difference. It is reasonable to expect that for 2016, the risk corridor program will experience an equivalent funding shortfall.
In response to the 2014 funding shortfall, 14 insurers are suing the federal government in an effort to obtain the balance of their risk corridor claims. HHS’s Centers for Medicare and Medicaid Services (CMS) issued a memo seemingly encouraging such suits and suggesting that the Obama Administration would likely settle with the plaintiffs.[14] However, this is in sharp contrast to the position taken by the Department of Justice (DOJ), which filed strong arguments against such suits, maintaining that the government is not obligated to pay for the risk corridor program shortfall.[15] In addition, the House of Representatives has filed a motion for leave to file an amicus brief in support of the DOJ’s argument.[16]
It has been suggested that if the government were to settle or lose the risk corridor lawsuits brought by insurers, payment could be made from the Judgment Fund, which has a permanent and unlimited appropriation from Congress and is used to settle claims made against the government. If this were to happen, it would be a backdoor bailout for insurers that could cost taxpayers up to $8.3 billion from the 2014 and 2015 shortfalls and additional amounts for any shortfall in 2016.
Risk Adjustment
The ACA’s risk adjustment program is designed to transfer money among insurers to adjust for the possibility that some carriers may get more or less than their proportionate share of costly enrollees. This program applies to the individual and small-group markets separately and is calculated separately for each market within each state. Unlike the reinsurance and risk corridors programs, the risk adjustment program is permanent.
While there are also problems with how HHS designed and implemented risk adjustment, the program does not increase the total amount of subsidies flowing to insurers, but rather reallocates premium revenues among insurers. Consequently, the program does not risk becoming a financial burden to federal taxpayers.
What Congress Should Do
To protect taxpayers and stop the insurer bailouts under the ACA, Congress should:
- Maintain risk corridor budget neutrality. The policy rider that makes the risk corridor program budget neutral should be maintained in the appropriations process for fiscal year 2017.
- Require repayment to the Treasury. Congress should require that HHS repay the $5 billion owed to the Treasury under the reinsurance program. Senator Ben Sasse (R–NE) and Representative Mark Walker (R–NC) have introduced the Taxpayers Before Insurers Act (S. 2803/H.R. 5904) to ensure that HHS puts taxpayers’ interests before those of insurers.
- Prohibit the use of settlement funds. Congress should prohibit the use of the Judgment Fund or any other federal funds to bail out insurers through risk corridor litigation. Senator Sasse has introduced legislation (S. 3481) to prohibit any funding of a backdoor insurer bailout through litigation. Representative Howard Griffith (R–VA) has introduced similar legislation (H.R. 6339).
- Prevent an extension of the reinsurance program. Some of the ACA’s proponents are calling for an extension of the reinsurance program.[17] Congress should reject such proposals and ensure that both the reinsurance and risk corridor programs expire as scheduled in 2016.
Conclusion
These three programs—reinsurance, risk corridors, and risk adjustment—expose the underlying failures of the ACA. Instead of bailing out the insurers with tax dollars through these programs, Congress should focus on repealing the regulations and provisions that are driving up the cost of coverage and creating dysfunctional health insurance markets.
—Alyene Senger is a Policy Analyst in the Institute for Family, Community, and Opportunity at The Heritage Foundation. Edmund F. Haislmaier is a Senior Research Fellow in the Institute for Family, Community, and Opportunity.